You are exhausted. Not just the “I need a nap” kind of tired that comes with growing a human being. This is a bone-deep, marrow-level fatigue where walking up a flight of stairs feels like scaling a mountain. You might find yourself chewing on ice chips uncontrollably, standing in front of the open freezer, or feeling your legs twitch and crawl the moment you finally lie down to sleep.
Table of Contents
If this sounds familiar, you are likely not just experiencing “normal” pregnancy symptoms. You may be part of the substantial percentage of pregnancies currently struggling with low hemoglobin. According to data from the Centers for Disease Control and Prevention (CDC), iron deficiency remains the most common nutritional deficiency during pregnancy, affecting millions of mothers and carrying risks that extend far beyond simple fatigue.

For decades, the standard advice given to expectant mothers has been frustratingly simple. Eat more spinach. Take a daily iron pill. Hope for the best. But medical understanding of maternal anemia has shifted significantly in recent years. We now know that “eating right” is often mathematically impossible for severe deficiencies once the baby’s demands peak. We know that generic screening guidelines often miss the mark until levels are critically low. Most importantly, breakthrough research from institutions like the Walter and Eliza Hall Institute (WEHI) suggests that the old way of treating third-trimester anemia might be putting mothers at risk of preventable complications.
This guide is not just about numbers on a lab report. It is a strategic, deep-dive breakdown of your health and your baby’s well-being. We will navigate the conflicting guidelines between medical bodies. We will compare the latest safety data on iron infusion treatments versus oral supplements. We will also detail 5 safe natural remedies to support your levels without risking your baby’s health.
The Invisible Struggle: What Is Low Hemoglobin in Pregnancy?
To fix the problem, we must first define it accurately. Low hemoglobin in pregnancy, medically known as anemia, occurs when your red blood cell count drops below specific thresholds established by the CDC and the American College of Obstetricians and Gynecologists (ACOG).
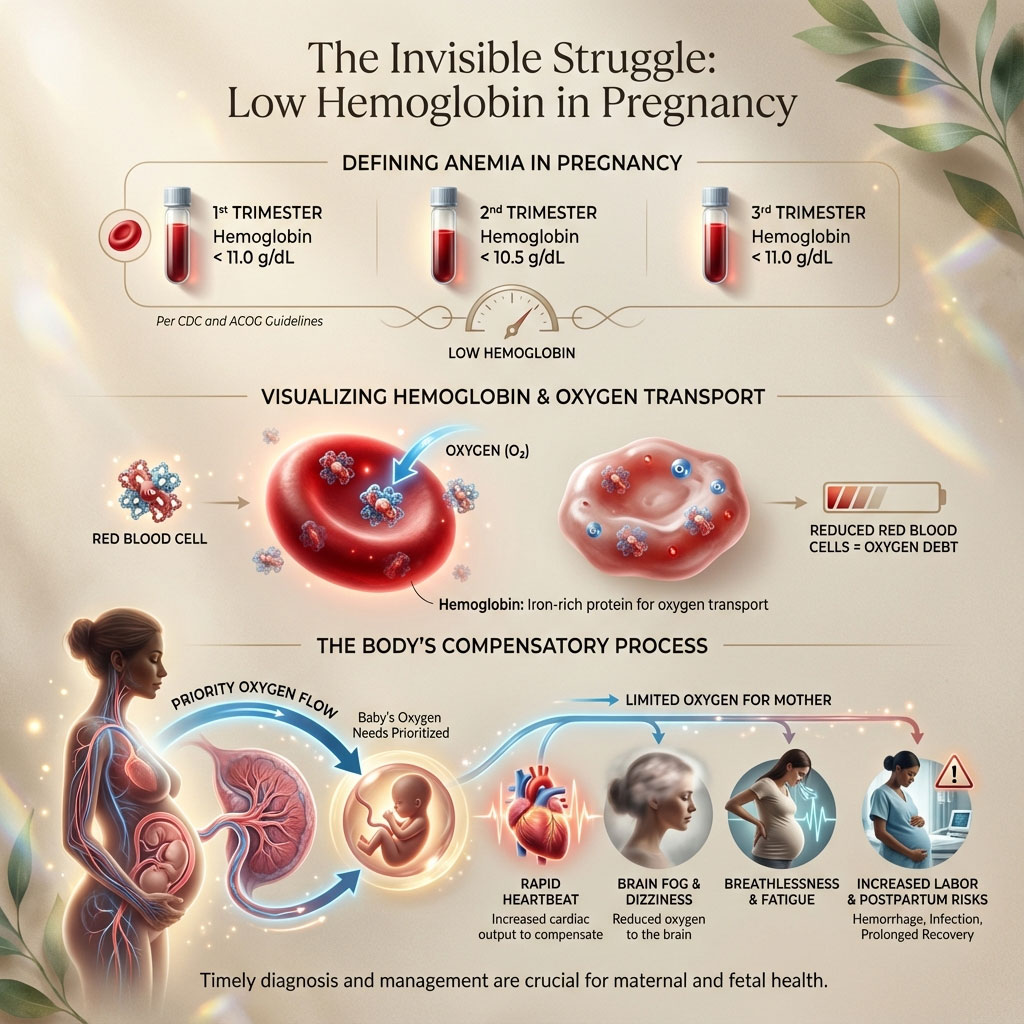
Hemoglobin is the iron-rich protein in your red blood cells. Its job is simple but vital: it carries oxygen from your lungs to the rest of your body and, crucially, to your baby through the placenta. When levels dip below 11.0 g/dL in the first or third trimesters, or 10.5 g/dL in the second trimester, your body enters a state of oxygen debt.
While mild dips are normal, true iron deficiency anemia means your body is making a difficult physiological choice. It begins prioritizing the baby’s oxygen needs at the expense of your own organs. Your heart beats faster to pump thinner blood. Your brain receives less oxygen, leading to fog and dizziness. This depletion leaves you vulnerable to complications during labor and extends your recovery time postpartum.
Core Concept: The Science of Your Blood Volume
To understand why your levels are dropping, you must understand the concept of physiologic hemodilution. This is often where the confusion begins for many patients who are told their levels are “low but normal.”
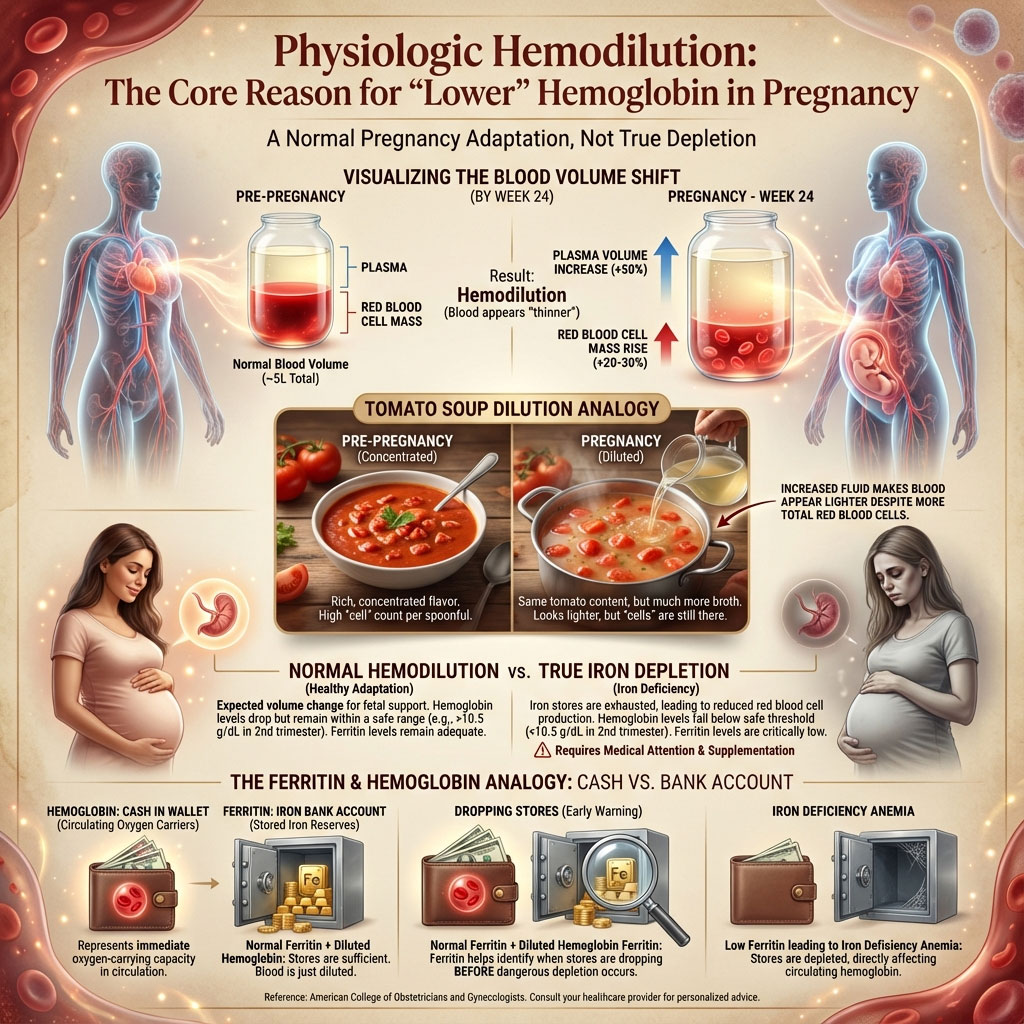
From the moment you conceive, your body begins a massive fluid construction project. By the 24th week of pregnancy, your blood plasma volume increases by nearly 50%. This additional fluid is necessary to support the placenta and prepare for blood loss during delivery. However, your red blood cell mass only increases by about 20% to 30%.
Think of this like a bowl of soup. If you add two cups of water to a bowl of tomato soup, the soup looks thinner and lighter. The actual ingredients (the red blood cells) are still there, and you have arguably more of them than before, but they are diluted in a much larger volume of liquid.
This dilution is a normal, healthy adaptation to help perfuse the placenta. It causes a natural drop in hemoglobin levels on pregnancy charts during the second trimester.
However, there is a distinct line between this healthy “watering down” and dangerous depletion. Doctors use ferritin levels to tell the difference. Ferritin is your iron storage protein. It acts as the “bank account” for iron, while hemoglobin is the “cash in your wallet.” You can have a full bank account (normal ferritin) but be low on cash (hemodilution). Or, more commonly in pregnancy, you can have an empty bank account (low ferritin) which eventually causes you to run out of cash entirely (Iron Deficiency Anemia).
The goal of modern prenatal care is to catch the problem when the bank account is getting low, not wait until you are bankrupt.
Normal Hemoglobin Ranges by Trimester
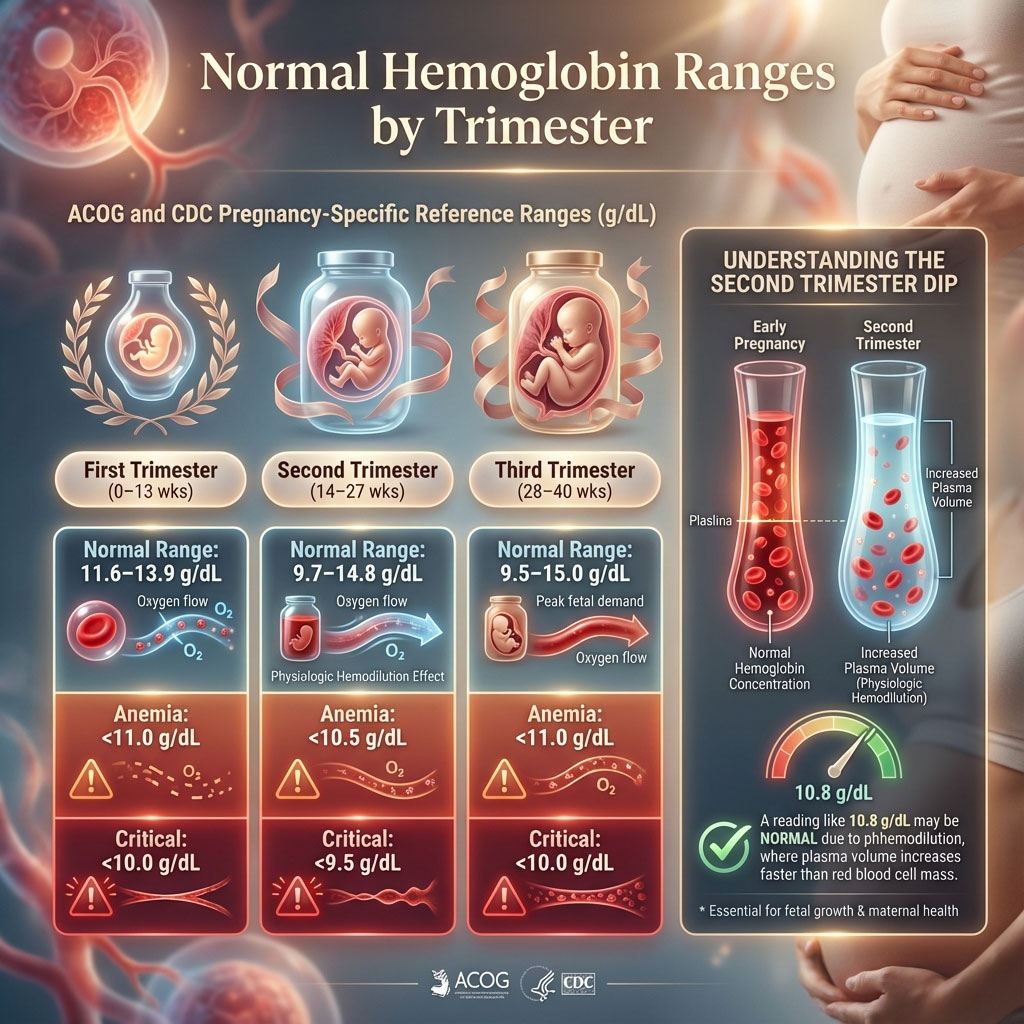
Understanding your lab results is the first step in patient advocacy. Many generic lab reports use non-pregnant reference ranges, which can flag a healthy pregnant woman as anemic or, conversely, fail to flag a borderline case. Below is the definitive chart based on ACOG Practice Bulletins and CDC criteria tailored specifically for pregnancy.
| Trimester | Normal Range (g/dL) | Anemia Threshold (Danger Zone) | Critical Low (Action Needed) |
| First (0–13 Weeks) | 11.6 – 13.9 | Below 11.0 g/dL | Below 10.0 g/dL |
| Second (14–27 Weeks) | 9.7 – 14.8 | Below 10.5 g/dL | Below 9.5 g/dL |
| Third (28–40 Weeks) | 9.5 – 15.0 | Below 11.0 g/dL | Below 10.0 g/dL |
Table 1: Reference ranges adapted from ACOG Practice Bulletins and CDC Criteria.
The Second Trimester Dip: If your doctor tells you your level is 10.8 g/dL in week 20, you are likely experiencing normal physiologic changes. This is the nadir, or the lowest point, of the curve. However, if that same number appears in week 36, you are technically anemic and require intervention to mitigate postpartum hemorrhage risk.
The Risks: Why You Cannot “Wait and See”
There is a dangerous misconception in some wellness circles that anemia is just a minor inconvenience of pregnancy. Friends or family might tell you it is “normal” to be exhausted or that you will “bounce back” after the baby is born. Do not listen to them. Low hemoglobin during pregnancy is a systemic risk factor that alters outcomes for both you and your child.
Risks to the Mother: The Hemorrhage Connection
The most immediate danger is delivery. Childbirth, whether vaginal or Cesarean, involves blood loss. A healthy woman with a hemoglobin of 13.0 g/dL enters labor with a safety buffer. She can tolerate losing 500ml to 1,000ml of blood without reaching critical instability. A woman starting at 9.0 g/dL does not have that buffer.
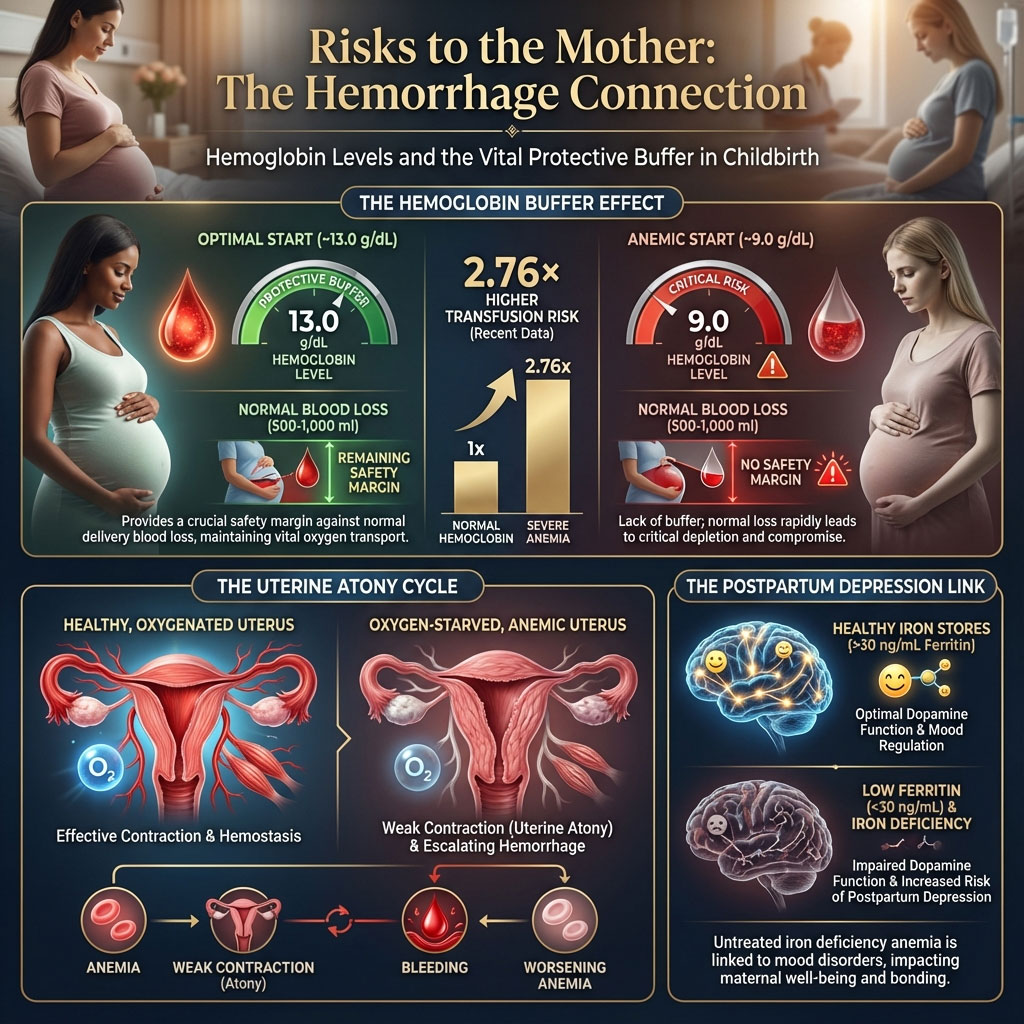
Recent data highlights this danger explicitly. Women with severe anemia face a 2.76 times higher risk of needing a blood transfusion due to postpartum hemorrhage. The mechanism here is mechanical. The uterus requires oxygenated blood to function as a muscle. After the baby is delivered, the uterus must contract violently (the “afterbirth pains”) to clamp down on the blood vessels where the placenta was attached. Anemic muscle tissue is sluggish and hypoxic (oxygen-starved). It fails to clamp down effectively, a condition called uterine atony, leading to increased and prolonged bleeding. This creates a vicious cycle where bleeding causes more anemia, and anemia prevents the bleeding from stopping.
Furthermore, untreated iron deficiency anemia is strongly linked to postpartum depression. Research published in journals like the American Journal of Clinical Nutrition suggests that low ferritin levels (below 30 ng/mL) affect dopamine function in the brain. This makes the already difficult transition to motherhood significantly harder, affecting bonding and increasing the severity of “baby blues.”
Risks to the Baby: Development and Timing
Your baby is an incredibly efficient biological system that takes what it needs from the mother first. However, when maternal stores are completely empty, the baby suffers.
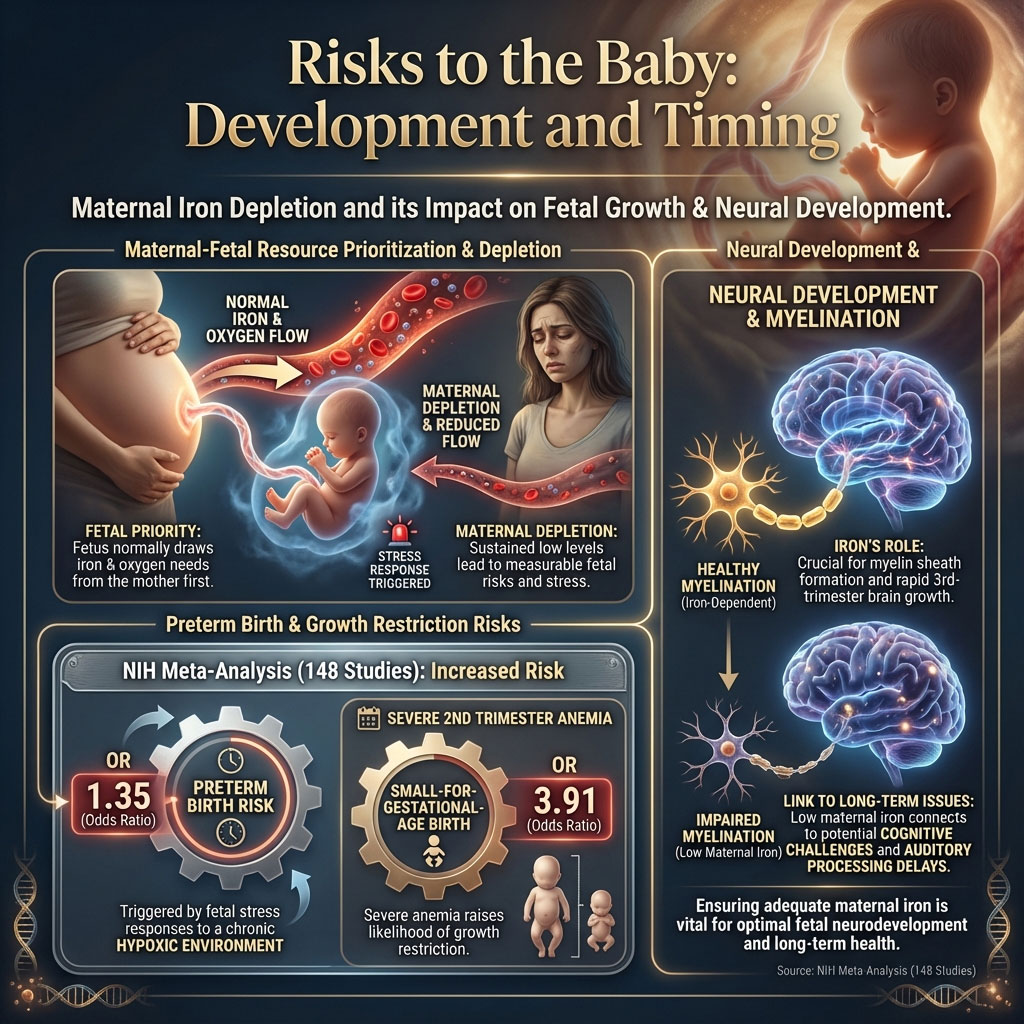
A massive 148-study meta-analysis available through the National Institutes of Health (NIH) has quantified these risks. Anemia during pregnancy raises the odds of preterm birth by 1.35 times (OR 1.35). The mechanism is believed to be related to stress hormones; the fetus detects a hypoxic environment and triggers early labor as a survival mechanism.
The data for low birth weight is even more concerning. Severe anemia in the second trimester is linked to a 3.91 times higher likelihood of the baby being born small for gestational age. Iron is critical for fetal neurodevelopment. It is a key component in the myelination of nerve fibers. A lack of iron during the rapid brain growth phases of the third trimester has been associated with long-term cognitive and behavioral issues in children, including a higher risk of auditory processing delays.
The Demographic Gap in Care
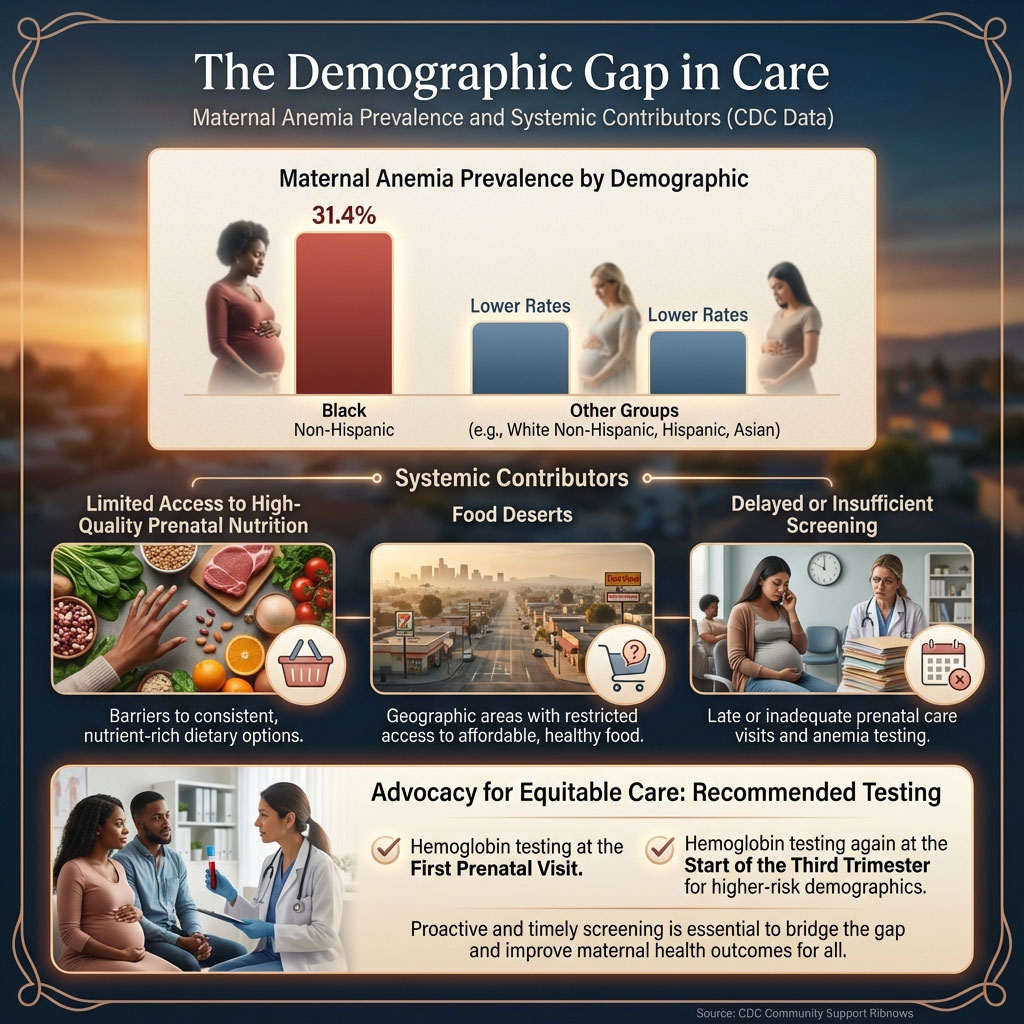
We must also address the equity gap in maternal health. CDC anemia guidelines and prevalence reports show that maternal anemia complications disproportionately affect Black non-Hispanic women, with a prevalence rate of nearly 31.4% compared to lower rates in other demographics.
This is not simply a matter of genetics. It is often a result of systemic barriers to high-quality prenatal nutrition, “food deserts” where fresh iron-rich foods are scarce, and late screening protocols. If you fall into a high-risk demographic, early advocacy is vital. Do not wait for your provider to suggest a test; request hemoglobin levels checks at your first appointment and again at the start of the third trimester.
Treatment Showdown: Oral Iron vs. Iron Infusion
For decades, the standard of care was identical for everyone. Take a ferrous sulfate pill. If that didn’t work, take two. Drink some orange juice.
In modern obstetrics, that “one size fits all” protocol is increasingly viewed as obsolete. Clinical data from WEHI and other major research bodies has revolutionized how obstetricians view treatment, particularly in the third trimester.
Oral Iron: The First Line of Defense
For mild cases diagnosed early (weeks 12-20), oral iron remains the first line of defense. The goal is to boost your intake to 60–120 mg of elemental iron daily.
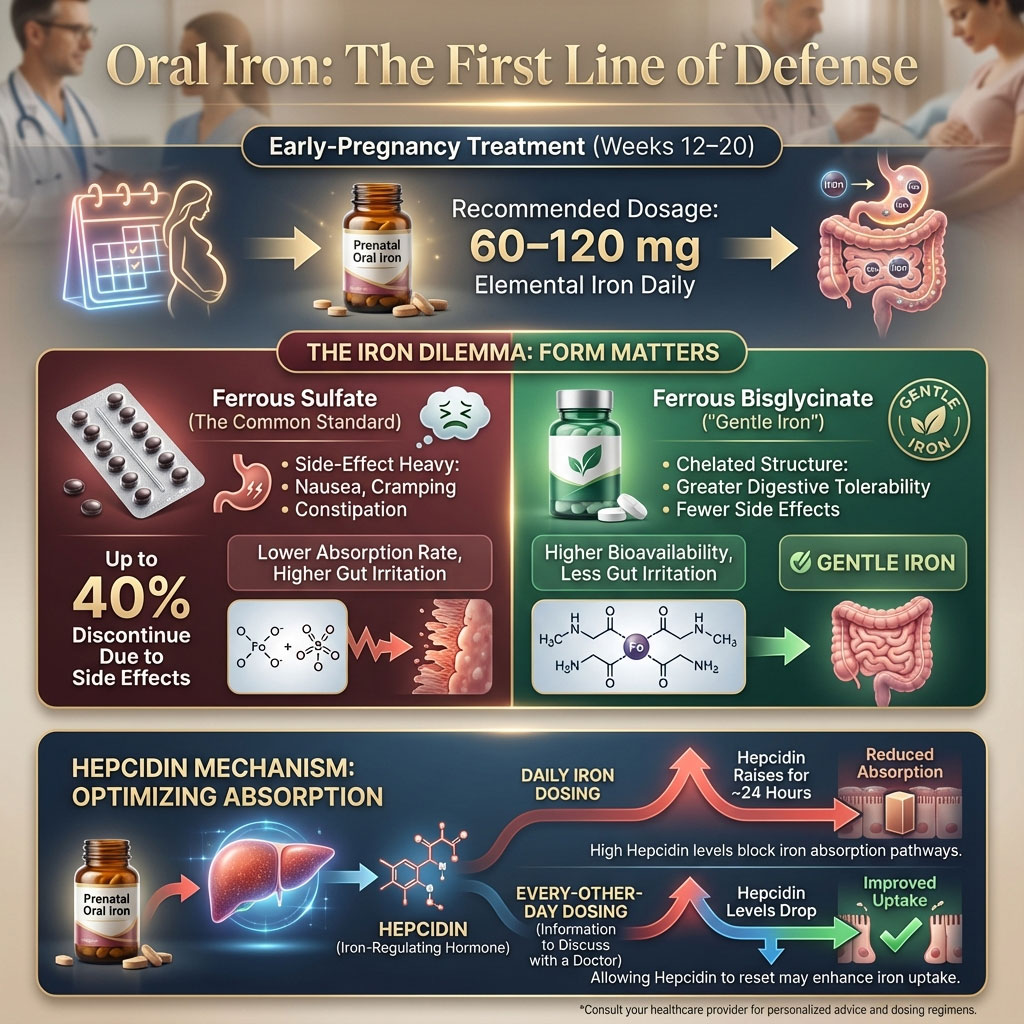
The main issue with oral iron is compliance. Ferrous Sulfate, the cheap iron found in most pharmacies and insurance formularies, is notorious for causing nausea, stomach cramps, and severe constipation. Because progesterone already slows down digestion in pregnancy, adding Ferrous Sulfate often leads to extreme discomfort. Up to 40% of pregnant women stop taking their supplements because the side effects are unbearable.
The Solution: If you are prescribed pills, ask for Ferrous Bisglycinate (often labeled as “Gentle Iron”). This form is chelated, meaning the iron molecule is bonded to amino acids (glycine). It passes through the stomach more easily and is absorbed in the small intestine with significantly fewer digestive issues.
The Hepcidin Block: New research also suggests that taking iron every other day might actually be more effective than daily dosing for some women. Iron triggers a hormone called Hepcidin, which blocks further iron absorption for about 24 hours. By dosing every other day, you allow Hepcidin levels to drop, potentially absorbing more iron overall with fewer side effects. Discuss this strategy with your doctor.
Iron Infusion: The Modern Standard for Rapid Relief
If you are 34 weeks pregnant with a hemoglobin of 9.5 g/dL, oral pills will physically not work fast enough. Oral iron takes 6 to 8 weeks to rebuild red blood cell mass significantly. You do not have 8 weeks. You have a due date.
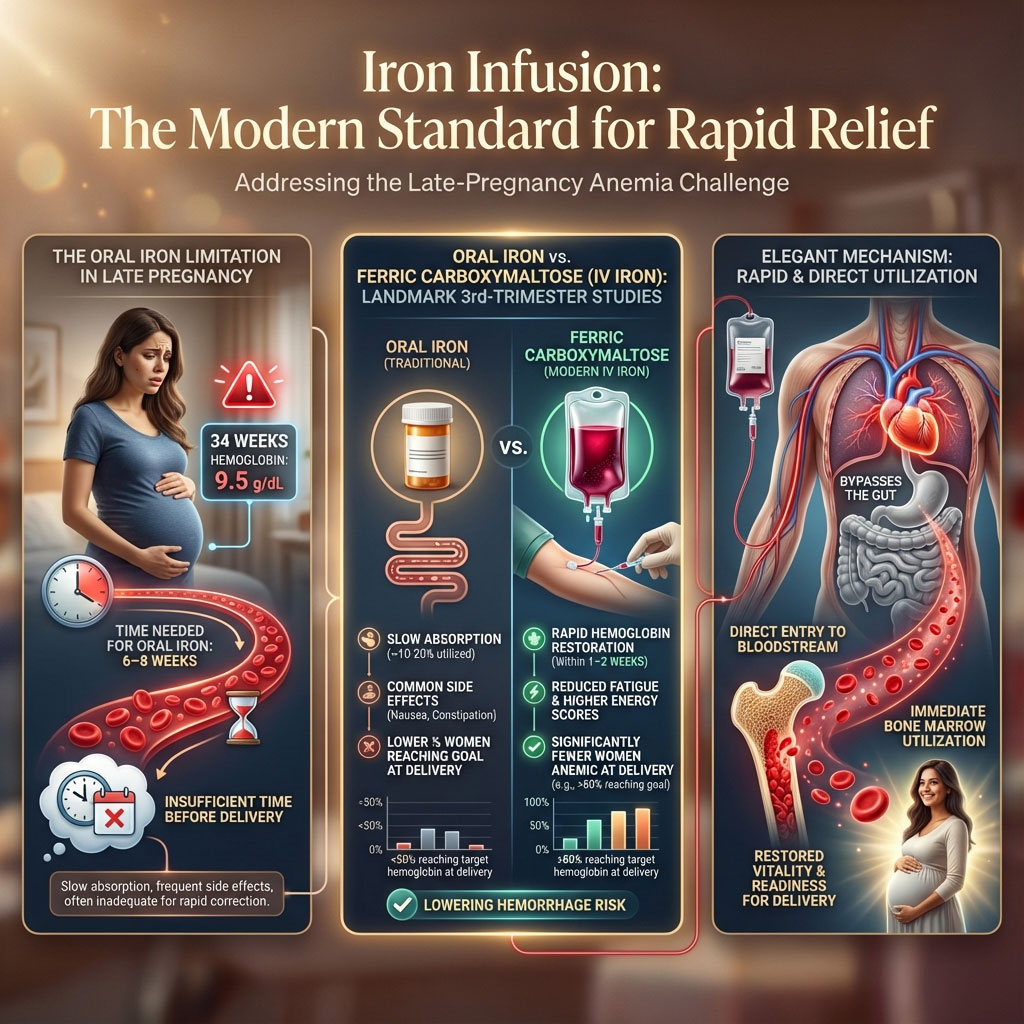
This is where the iron infusion pregnancy protocol changes the game. Landmark studies comparing women receiving standard oral care against those receiving a single dose of Ferric Carboxymaltose (IV Iron) in the third trimester have shown definitive results.
The findings are undeniable. The infusion group sees a rapid restoration of hemoglobin levels within 1 to 2 weeks. Patients report significantly less fatigue and higher physical energy scores. Most importantly, fewer women in the infusion group are anemic at the time of delivery, significantly lowering their hemorrhage risk.
Iron infusion treatments bypass the gut entirely. The iron is delivered directly into your bloodstream, where it can be immediately utilized by your bone marrow.
What Does an Infusion Feel Like?

Many women fear the idea of an “infusion.” It typically takes place in a hematology center or a labor and delivery triage unit. An IV line is placed in your arm, and the dark-colored iron solution drips in over the course of 15 to 30 minutes. Most women feel absolutely nothing during the process. Some report a metallic taste in their mouth. Modern formulations have largely eliminated the risk of serious allergic reactions that were associated with older types of iron.
Comparison: Oral Tablets vs. IV Infusion
| Feature | Oral Iron Tablets | IV Iron Infusion |
| Speed of Recovery | Slow (4–8 weeks to see change) | Rapid (1–2 weeks to full effect) |
| Digestive Side Effects | High (Nausea, Constipation) | None (Bypasses the gut) |
| Absorption Rate | Low (Blocked by food/inflammation) | 100% Bioavailability |
| Best Candidate | Early pregnancy, mild anemia | 3rd Trimester, severe anemia, or intolerance to pills |
| Cost | Low (10–10–50 per month) | High ($1,000+, usually insurance covered) |
| Safety Profile | Excellent | Excellent (Modern formulas minimize reaction risk) |
Table 2: Therapeutic comparison based on current clinical efficacy data.
5 Safe Natural Remedies to Increase Hemoglobin
Many women prefer a holistic approach or want to supplement their medical treatment with dietary strategies. While we must be clear that diet alone cannot cure severe iron deficiency anemia where stores are completely depleted, it is the foundation of prevention and maintenance. Here are 5 safe, effective ways to support your levels naturally.
1. The Lucky Iron Fish
This is one of the most innovative safe natural remedies for anemia, particularly for vegetarians or those who struggle with pills. The Lucky Iron Fish is a cast-iron ingot shaped like a fish (or a leaf).

The science is simple chemistry. You boil the fish in 1 liter of water or broth for 10 minutes. Crucially, you must add an acid—such as a few drops of lemon juice, apple cider vinegar, or tomatoes. The acid helps release bioavailable iron from the ingot into the liquid.
When used correctly, the water is enriched with 6 to 8 mg of absorbable iron. It does not change the taste of the food. You can use this iron-enriched water to make soups, stews, oatmeal, or even herbal tea. It is safe, reusable for up to five years, and provides a gentle, consistent baseline of iron that is incredibly easy on the stomach.
2. Heme Iron Pairing (The “Red Meat & Bison” Protocol)
Not all iron is created equal. Heme vs non-heme iron is the critical distinction that many diet plans miss.

- Heme Iron: Found in animal products (blood and muscle). Your body absorbs this easily, with a rate of 15-30%.
- Non-Heme Iron: Found in plants (spinach, lentils, fortified cereals). This is much harder to absorb, with a rate of only 2-20%.
To naturally boost levels, you need to prioritize the most potent sources. While beef is standard, Bison and Elk are superior choices for pregnancy. They are leaner, often grass-fed (higher in Omega-3s), and typically contain more iron per ounce than feed-lot beef. Clams are another powerhouse, containing nearly four times the iron of beef, though they must be fully cooked to be safe for pregnancy. Dark meat chicken (thighs) also contains more iron than breast meat.
3. The Vitamin C “Lock”
You can double or triple the effectiveness of your food by understanding kitchen chemistry. Vitamin C iron absorption synergy is a real, measurable phenomenon supported by NIH dietary supplement fact sheets. Vitamin C (ascorbic acid) changes the chemical structure of non-heme (plant) iron from ferric to ferrous, making it soluble and easier for your gut to absorb.

The Strategy: Never eat iron-rich foods alone.
- The Combo: Eating a spinach and kale salad? You must add strawberries, bell peppers, or a lemon vinaigrette.
- The Breakfast: Eating iron-fortified oatmeal or bran flakes? Do not drink coffee. Drink a small glass of fresh orange juice or eat half a grapefruit.
- The Supplement: If you take an iron pill, swallow it with a Vitamin C supplement (500mg) or citrus juice. This “locks” the iron in and prevents it from passing through your system unabsorbed.
4. Cast Iron Cooking
Grandmother’s skillet was actually a medical device. Cooking acidic foods (like tomato sauce, chili, or stew) in a cast-iron skillet leaches small amounts of dietary iron into the meal.

While the dosage is inconsistent compared to supplements, every milligram counts when you are fighting low hemoglobin during pregnancy. Research shows that cooking high-moisture, high-acid foods in cast iron can increase the iron content of the final dish by up to 16%.
Tip: Do not use enamel-coated cast iron for this purpose; you need the raw, seasoned iron to be in contact with the food. Simmering a tomato-based pasta sauce for 20 minutes in a cast-iron skillet is an easy, passive way to boost the family’s intake.
5. Blackstrap Molasses & Liquid Herbs
For those who cannot tolerate pills, liquid remedies are a viable natural adjunct.

- Blackstrap Molasses: This thick, dark syrup is a byproduct of sugar refining, but unlike refined sugar, it retains all the minerals. Just one tablespoon of high-quality Blackstrap molasses contains about 20% of your daily recommended iron, along with calcium and magnesium. It can be stirred into oatmeal, smoothies, or warm water.
- Liquid Herbal Iron (Floradix): This is a popular European supplement made from yeast and herbal extracts like nettle, spinach, and fennel. Because the iron is already dissolved in liquid and paired with herbs that aid digestion, it is non-constipating and highly absorbable. While the dosage (approx 10mg) is lower than a medical tablet, it is an excellent “natural” bridge for maintenance or for women with mild deficiencies.
What to Avoid: Risky Trends & Blockers
The internet is full of “natural” advice that is either useless or dangerous. We must filter out the noise.

The Beef Liver Danger
You will often see influencers or “ancestral diet” advocates recommending large amounts of beef liver to raise levels fast. Proceed with extreme caution.
While liver is incredibly high in iron, it is also incredibly high in Preformed Vitamin A (Retinol). Unlike beta-carotene found in carrots (which is safe), high doses of Retinol are teratogenic, meaning they can cause birth defects in the developing baby. The safe upper limit is debated, but most medical experts recommend limiting liver consumption to less than 50g (about 1.5 ounces) once per week. Do not take desiccated liver pills if you are already taking a prenatal vitamin that contains Vitamin A. The cumulative effect can be toxic.
The Inhibitors: The 2-Hour Rule
You might be sabotaging your own treatment without knowing it. Certain foods block iron absorption aggressively.
- Calcium: Calcium and Iron are chemically similar enough that they compete for the same absorption receptors in the gut. Calcium usually wins. Never take your iron pill with dairy (milk, cheese, yogurt) or your calcium-heavy prenatal vitamin.
- Tannins: Coffee, black tea, green tea, and chocolate contain tannins. These compounds bind to iron in the stomach and flush it out of your system before it can be absorbed.
- Phytates: Whole grains and legumes contain phytates, which can inhibit absorption.
The Strategy: Implement a 2-hour buffer. Take your iron supplement on an empty stomach with Vitamin C. Wait two full hours before eating dairy, taking your prenatal vitamin, or drinking tea/coffee. This simple timing change can double your absorption.
Practical Strategies for Advocacy
You are the only person who lives in your body. If you feel wrong, you must advocate. Fatigue is often dismissed in pregnancy, but you know the difference between “sleepy” and “unable to function.”

Know Your Symptoms
Look for the specific signs of iron deficiency anemia that go beyond tiredness:
- Pica: Do you crave ice? This condition, called Pagophagia, is a specific craving for non-food items like ice, dirt, or laundry starch. It is a screaming red flag for anemia. The chewing of ice is thought to trigger a reflex that increases blood flow to the brain, providing temporary alertness.
- Restless Legs Syndrome (RLS): If your legs feel “crawly,” twitchy, or impossible to keep still at night, preventing sleep, check your iron. RLS is strongly correlated with low ferritin.
- Palpitations: A racing heart when standing still, or feeling winded after speaking a few sentences.
- Pallor: Check the inside of your lower eyelid or your nail beds. If they are pale pink or white instead of red, you may be anemic.
The “Guideline Conflict” Strategy
The U.S. Preventive Services Task Force (USPSTF) has stated there is “insufficient evidence” to screen asymptomatic women for anemia. However, ACOG guidelines strongly recommend screening everyone.
If your provider hesitates to test you because you “look fine,” cite the ACOG guidelines. Request a CBC (Complete Blood Count) and a Ferritin test. Remember, hemoglobin levels tell you if you are anemic today. Ferritin levels tell you if you will be anemic next month. Knowing both gives you the power to act before it becomes a crisis.
Postpartum Planning: The Fourth Trimester
Iron care does not stop when the baby is born. In fact, the postpartum period is when many women feel the crash most acutely. You have just run a marathon (labor), potentially lost blood, and are now producing breast milk, which requires significant energy and nutrients.

If you were anemic during pregnancy, continue your iron supplements for at least 6 to 12 weeks postpartum. Ask your doctor to recheck your levels at your 6-week follow-up. Restoring your iron stores is critical for preventing postpartum depression, maintaining milk supply, and having the energy to bond with your new baby.
“For more options beyond this, check out 7-Day Meal Plan to Increase Hemoglobin Fast & Naturally to support your pregnancy journey.”
Summary & Key Takeaways
Navigating low hemoglobin during pregnancy is a balance of biology and strategy. You are fighting against a body that is diluting its own blood supply while building a new human from scratch.

- Know Your Numbers: Memorize the normal hemoglobin range trimester chart. If you hit 10.5 g/dL in the second trimester, monitor it closely. If you hit 9.5 g/dL, treat it aggressively.
- Choose the Right Weapon: For mild cases, use Iron Bisglycinate paired with Vitamin C. For severe late-term cases, advocate for an iron infusion referral based on current clinical data.
- Use the 5 Safe Remedies: Integrate the Lucky Iron Fish, Cast Iron cooking, Heme proteins (Red Meat/Clams), Vitamin C pairing, and safe liquids like Molasses into your daily routine.
- Watch the Risks: Remember that treating anemia is not about vanity or just “feeling less tired.” It is about safety. It is about reducing the risk of postpartum hemorrhage and ensuring your baby reaches full term with a healthy brain development.
You have the right to feel energized, strong, and capable as you prepare for labor. Do not accept exhaustion as the status quo. With the right tools and the right timing, you can refill your tank and enter motherhood with strength.
Frequently Asked Questions (FAQ)
Is a hemoglobin level of 10.5 dangerous in the second trimester?
In the second trimester, a hemoglobin level of 10.5 g/dL is generally considered the lower limit of normal due to physiologic hemodilution (blood volume expansion). While it is not immediately dangerous, it is a warning sign. It indicates that your iron stores are being used faster than they are being replaced. You should focus on diet and supplements to prevent it from dropping further into the “anemia” range (below 10.0 g/dL).
How fast can I raise my hemoglobin before labor?
Oral iron supplements typically take 4 to 6 weeks to significantly improve hemoglobin levels because the digestive process is slow and regulated. If you are close to your due date (36+ weeks), this may be too slow to guarantee safe levels for birth. In this case, an iron infusion treatment can restore iron stores in as little as 1 to 2 weeks.
Is the Lucky Iron Fish safe to use while pregnant?
Yes, the Lucky Iron Fish is safe when used according to instructions. It releases a controlled amount of iron (6–8 mg) into your cooking water, which is well below toxicity levels. It is an excellent way to boost dietary iron intake without the digestive side effects of high-dose pills. Always ensure you add an acid (lemon/tomato) to the boiling water to activate the release.
Can I take Floradix and Prenatal vitamins together?
Yes, but check the total dosage. Floradix is a gentle, liquid iron supplement, but it contains a relatively low dose (approx. 10 mg) compared to prescribed iron pills (65 mg or more). It is great for maintenance, but if you have diagnosed anemia, Floradix alone may not be strong enough. Ensure your total daily iron intake matches your doctor’s recommendation.
Why do I crave ice during pregnancy?
Craving ice is a condition called Pagophagia, a form of Pica. It is a classic, highly specific symptom of iron deficiency anemia. Experts believe the coldness triggers a response that increases blood flow to the brain, temporarily alleviating the sluggishness caused by anemia. If you find yourself chewing ice, request an iron test immediately.
Does an iron infusion affect the baby?
Current research shows that modern iron infusions (like Ferric Carboxymaltose) are safe for the baby in the second and third trimesters. By treating the mother’s anemia effectively, the infusion actually protects the baby from risks like low birth weight and preterm delivery associated with maternal hypoxia.
How much beef liver is safe for pregnancy anemia?
You should be very careful with beef liver. It is high in Vitamin A (Retinol), which can cause birth defects in high doses. Limit consumption to no more than 1.5 ounces (approx. 50g) once a week to avoid toxicity. If possible, rely on muscle meats (steak, bison) for heme iron instead.
What are the side effects of modern iron infusions?
Modern iron infusion formulations have a very low risk of serious side effects. The most common minor side effects are temporary injection site irritation or a metallic taste in the mouth during the drip. The risk of anaphylaxis, which was a concern with older iron dextran formulas used decades ago, is extremely rare with new drugs.
Can anemia cause complications during C-section?
Yes. Cesarean sections typically involve more blood loss than vaginal births. If you have low hemoglobin, you have a lower tolerance for this blood loss. This increases the risk of needing a blood transfusion or experiencing cardiac stress and extreme fatigue during the recovery period.
Why is my iron low even though I take supplements?
You may be dealing with absorption issues. If you have Celiac disease, Crohn’s, or even an undiagnosed H. pylori infection, your gut cannot absorb iron pills effectively. Alternatively, you might be taking your pill with tea, coffee, or calcium, which blocks absorption. This “failure of oral therapy” is a primary reason doctors switch patients to infusions.
What is the difference between low iron and low hemoglobin?
Think of iron (ferritin) as your bank savings and hemoglobin as the cash in your wallet. You can have low savings (Iron Deficiency) but still have cash (Normal Hemoglobin) for a while. Eventually, if you don’t replenish the savings, you run out of cash (Anemia). You want to catch the problem at the “low savings” stage before it affects the oxygen in your blood.
Does insurance cover iron infusions for pregnancy in the USA?
Most US insurance plans cover iron infusions if you have a documented diagnosis of anemia and “failure of oral therapy.” This usually means you have tried pills and they either didn’t work or caused intolerable side effects. Always call your provider to confirm pre-authorization requirements before the appointment.
Medical Disclaimer:
The information provided in this article is for educational and informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always seek the advice of your physician, obstetrician, or other qualified health provider with any questions you may have regarding a medical condition or treatment. Never disregard professional medical advice or delay in seeking it because of something you have read in this article. If you think you may have a medical emergency, call your doctor or 911 immediately.







