You wake up with a splitting headache or brutal menstrual cramps. The bottle of ibuprofen is sitting right there on your nightstand. Your first instinct? Grab two tablets and swallow them before the pain takes over your entire day. But you haven’t eaten anything yet, and the thought of making breakfast while you’re hurting feels impossible.
Table of Contents
If this sounds familiar, you’re not alone. As a clinical pharmacist, I see this exact situation play out with patients all the time. People want fast relief. They don’t want to wait around to toast a bagel first.
But here’s the thing: the question of can you take ibuprofen on an empty stomach is one of the most important safety questions in over-the-counter medication. Ibuprofen is effective and widely available, but it interacts aggressively with your stomach lining. That “take with food” label on the bottle isn’t just a polite suggestion. It’s a real physiological requirement to prevent damage.
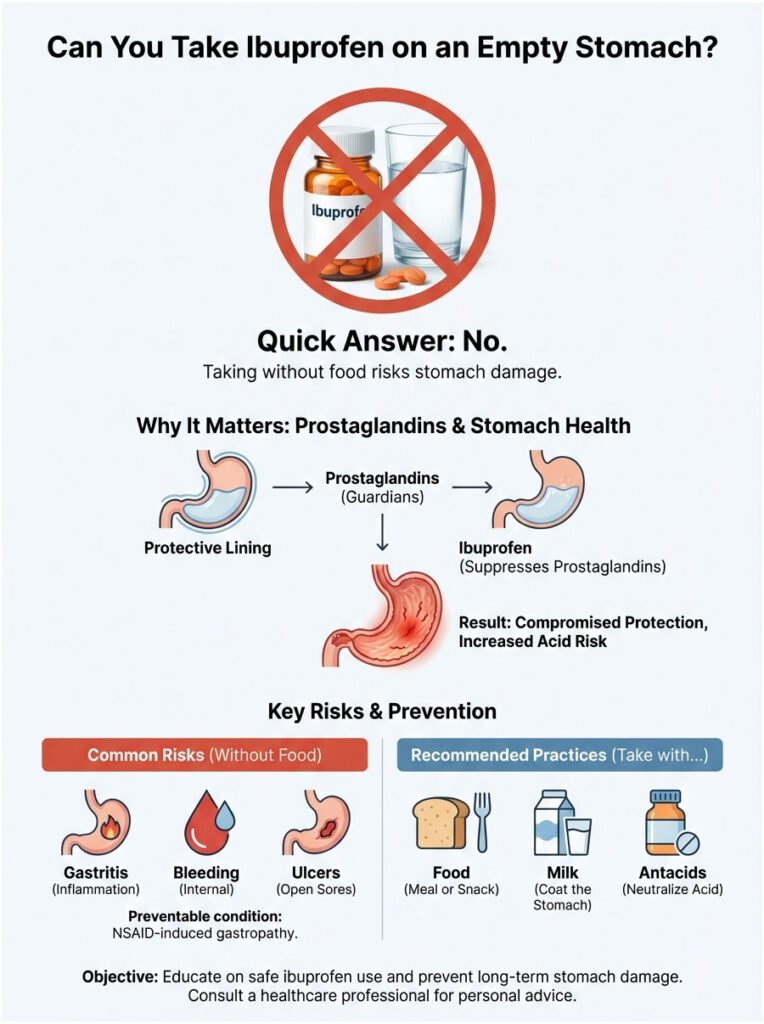
Quick Answer: Can you take ibuprofen on an empty stomach? No, it’s not recommended. Ibuprofen suppresses protective prostaglandins, leaving your stomach lining exposed to acid. This raises the risk of gastritis, bleeding, and ulcers. Even a small snack, a glass of milk, or an antacid can act as a buffer. Always take ibuprofen with food or milk to protect your stomach.
I’m Dr. Sarah J. Miller. Over years of clinical pharmacy practice, I’ve counseled countless patients dealing with NSAID-induced gastropathy, which is stomach damage caused by common painkillers like ibuprofen. Most of those cases were entirely preventable. This guide covers the science behind your stomach, explains why rushing for relief can backfire, and walks you through pharmacist-approved strategies for taking ibuprofen safely.
Why Your Stomach Needs Protection from Ibuprofen
To understand why the answer to can you take ibuprofen on an empty stomach is a firm “no,” you need to know what the drug actually does at a molecular level. Ibuprofen is a Non-Steroidal Anti-Inflammatory Drug (NSAID). Specifically, it’s a non-selective inhibitor, meaning it doesn’t pick and choose which enzymes it blocks.
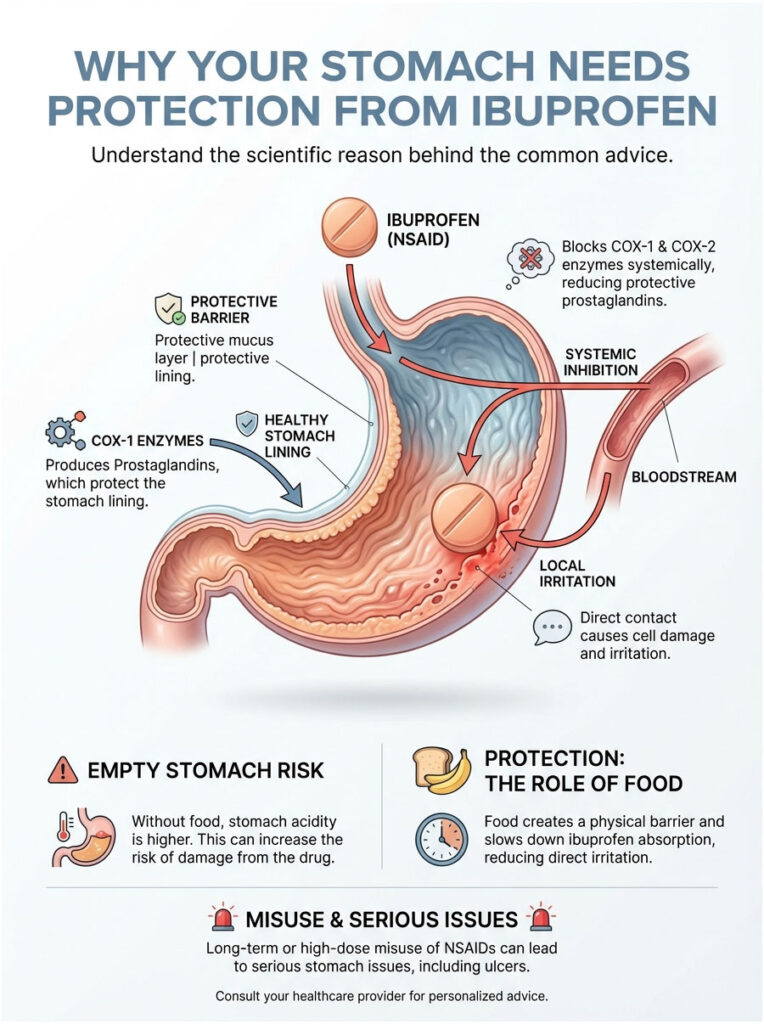
How Ibuprofen Works: The COX-1 and COX-2 Pathway
When you take ibuprofen, it blocks enzymes called cyclooxygenases (COX). Two types matter here:
- COX-2: This enzyme kicks in when there’s injury or infection. It produces chemicals that cause pain, inflammation, and fever. Blocking COX-2 is the whole point of taking ibuprofen. That’s where your relief comes from.
- COX-1: This enzyme is always active in your body, particularly in the stomach and kidneys. It handles essential “housekeeping” tasks that keep your organs running properly.
The problem? Ibuprofen is non-selective. It blocks both COX-1 and COX-2. You get the pain relief from COX-2 inhibition, but you also lose stomach protection from COX-1 inhibition. That’s the unavoidable trade-off.
The Role of Prostaglandins in Stomach Defense
COX-1 produces prostaglandins, lipid compounds that act as your stomach’s built-in shield. In a healthy stomach, prostaglandins carry out three critical functions:
- Mucus Production: They trigger the secretion of a thick mucus layer that physically coats the stomach lining.
- Bicarbonate Secretion: They signal the release of bicarbonate, a chemical base that neutralizes stomach acid close to the stomach wall.
- Blood Flow Maintenance: They keep blood flowing to the mucosal cells, allowing them to repair quickly if they get damaged.
When your stomach is empty, its pH is highly acidic, typically sitting between 1.5 and 3.5. If you take ibuprofen in that state, it shuts down prostaglandin production. Without the mucus and bicarbonate shield, the acid starts digesting the stomach wall itself.
Local Irritation vs. Systemic Damage
A common misconception patients share with me goes something like this: “I washed it down with plenty of water, so the pill didn’t touch my stomach walls.” Unfortunately, water only solves half the problem.
Topical (Local) Irritation: This happens when the pill physically sits against your stomach lining while it dissolves. Ibuprofen is a weak acid. Direct contact can cause something called “ion trapping” in the mucosal cells, which leads to immediate cell damage. Food helps by creating a physical barrier between the drug and the stomach wall.
Systemic Inhibition: This is the bigger risk. Once ibuprofen is absorbed into your bloodstream, it travels back to the stomach tissue through the blood and shuts down COX-1 enzymes from the inside. This happens whether you drank water or not. It’s the reason injectable NSAIDs used in hospitals can still cause stomach ulcers, even though they never pass through the stomach at all. Food slows absorption and buffers the acid while this systemic effect takes place.
Key Statistics on NSAID Misuse
- 100,000+ estimated annual hospitalizations in the US from NSAID-related gastrointestinal complications
- 15-30% of chronic NSAID users develop peptic ulcers
- 4x higher risk of GI bleeding in regular NSAID users compared to non-users
- Age 60+: significantly higher risk of complications
- 16,500 estimated annual deaths in the US among arthritis patients from NSAID-related GI bleeding
Does Food Slow Down Pain Relief? What the Science Says
One of the main reasons people skip food is speed. And there’s a real pharmacokinetic basis for that concern. But the trade-off is almost never worth the risk.

Understanding Tmax (Speed) vs. AUC (Total Absorption)
Pharmacologists look at two key metrics when analyzing how a drug enters the body:
- Tmax: The time it takes for the drug to reach peak concentration in the blood.
- AUC (Area Under the Curve): The total amount of drug that actually gets absorbed into the bloodstream.
Clinical studies confirm that food does delay Tmax. On an empty stomach, ibuprofen typically peaks in 30 to 45 minutes. With a meal, that can stretch to 60 or 90 minutes. However, the AUC stays largely the same. That’s the important part.
In practical terms, relief may come 15 to 30 minutes later, but the drug is equally effective. You don’t lose potency. You’re simply trading a few minutes of faster onset for a meaningful safety buffer against stomach erosion.
How Food Affects Bioavailability
Interestingly, certain foods can actually help with drug absorption. While a heavy, high-fat meal might delay gastric emptying, a light snack with some protein or simple carbohydrates prevents what pharmacists call “dose dumping.” That’s when a high concentration of the drug hits the small intestine all at once. With ibuprofen, the presence of food reduces absorption variability, leading to a smoother and safer pharmacokinetic profile.
Risks of Taking Ibuprofen Without Food
When people ignore the advice about taking ibuprofen on an empty stomach, consequences can range from mild discomfort to serious medical emergencies.

Acute Symptoms from a Single Dose
Even one dose on an empty stomach can trigger acute gastritis. Symptoms typically show up within an hour:
- Dyspepsia: A gnawing, burning sensation in the upper abdomen
- Nausea: Queasiness, sometimes with vomiting
- Acid Reflux: Relaxation of the esophageal sphincter, allowing acid to rise into the throat
- Epigastric Pain: Sharp pain directly below the ribcage
Chronic Risks and the FDA Black Box Warning
The risks multiply with repeated use. The FDA requires a “Black Box Warning” on all NSAID packaging, the strictest warning available for both prescription and non-prescription drugs. It explicitly warns about serious gastrointestinal events, including bleeding, ulceration, and perforation of the stomach or intestines.
Peptic Ulcer Disease (PUD): An ulcer is an open sore on the stomach lining. NSAIDs are the second leading cause of PUD, right behind H. pylori infection. These ulcers can form without any symptoms at all.
GI Bleeding: This is the most dangerous complication, partly because it’s often painless until it reaches a critical stage. Since prostaglandins also regulate platelet aggregation, NSAIDs slightly thin the blood. If an ulcer forms and reaches a blood vessel, the body has trouble clotting the wound. This can lead to anemia or even massive hemorrhage.
Ibuprofen vs. Other Pain Relievers: Which Is Safest on an Empty Stomach?
Not all painkillers carry the same stomach risks. If you truly can’t eat due to nausea or fasting requirements, you need to consider a different medication.
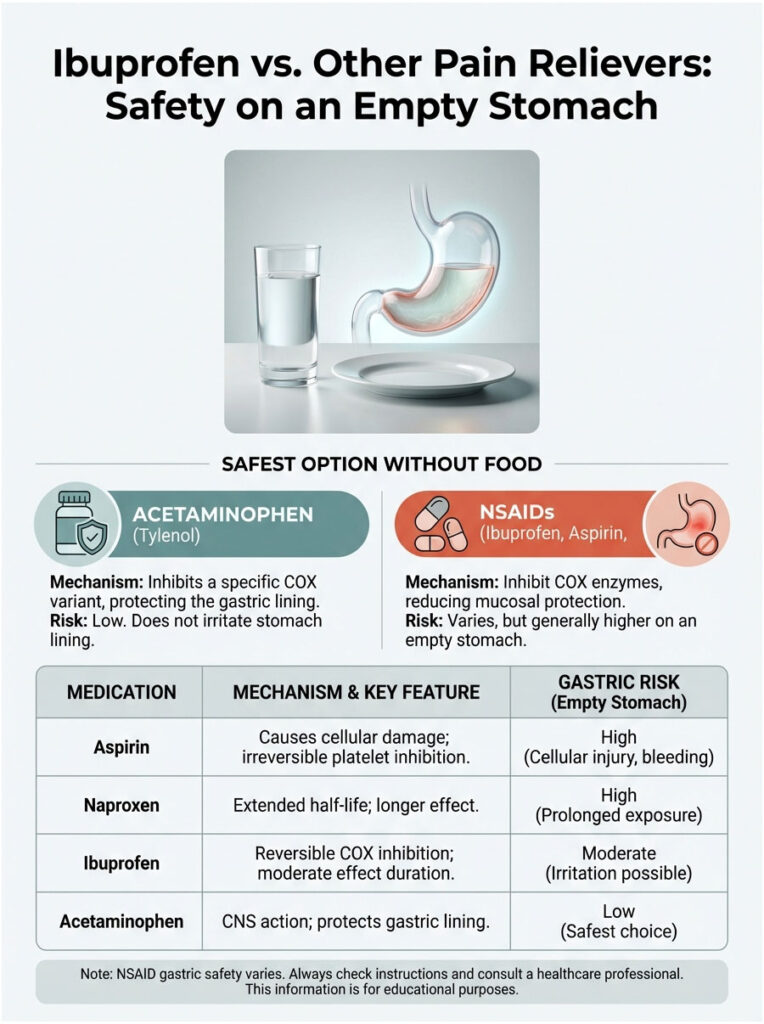
Choosing the Right Pain Reliever
Acetaminophen (Tylenol): This is the safest option when your stomach is empty. It’s not an NSAID. It works in the brain and is believed to inhibit a variant called COX-3. It does not block COX-1 in the stomach, so it doesn’t strip away the protective mucus layer.
Aspirin and Naproxen (Aleve): These tend to be harsher on the stomach than ibuprofen. Aspirin causes direct cellular damage and irreversible platelet inhibition. Naproxen has a longer half-life, meaning it stays in your system longer and suppresses prostaglandins for an extended period.
NSAID Gastric Safety Comparison Table
| Medication | Drug Class | Mechanism | Gastric Risk (Empty Stomach) | Safe on Empty Stomach? |
| Ibuprofen (Advil, Motrin) | NSAID | Non-selective COX-1 & COX-2 Inhibitor | High | NO |
| Naproxen (Aleve) | NSAID | Non-selective COX-1 & COX-2 Inhibitor | High | NO |
| Aspirin (Bayer) | NSAID (Salicylate) | Irreversible COX-1 & COX-2 Inhibitor | Very High | NO |
| Acetaminophen (Tylenol) | Non-NSAID | Central COX Inhibitor | Low | YES |
Who Faces the Highest Risk from Ibuprofen on an Empty Stomach?
While nobody should take ibuprofen without food, certain groups face especially serious consequences.
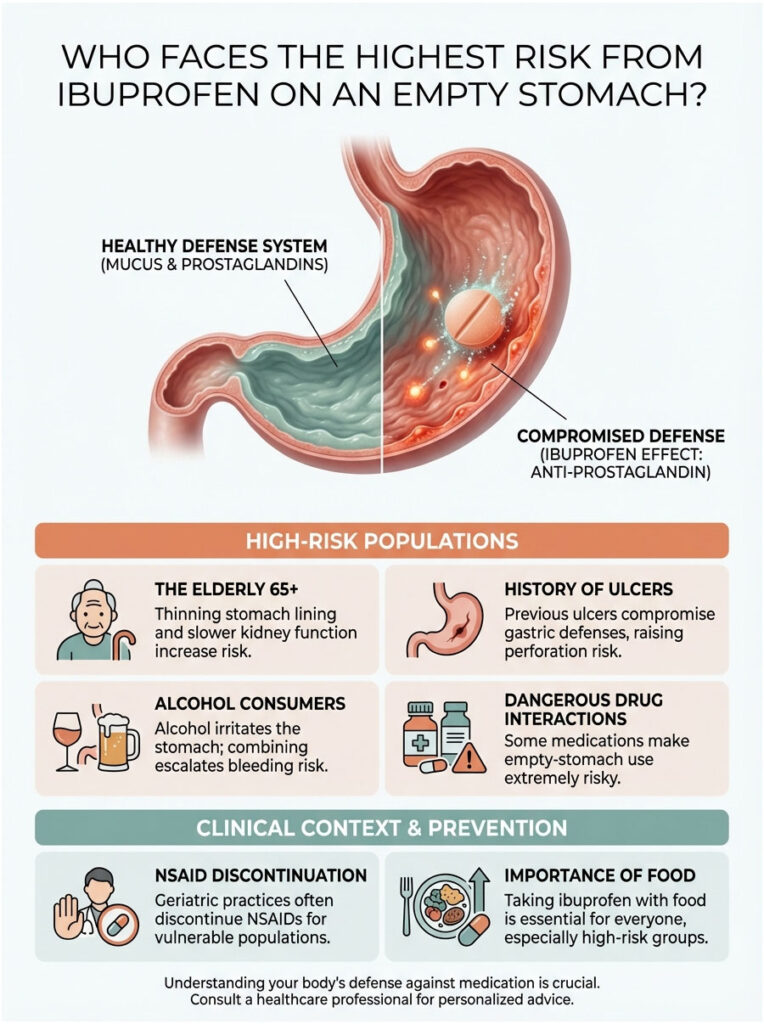
Most Vulnerable Populations
The Elderly (65+): As we age, the stomach lining naturally thins and the kidneys clear medication more slowly. The drug stays in the body longer, exerting its anti-prostaglandin effects for extended periods. In geriatric practice, we frequently discontinue NSAIDs entirely for this reason.
People with a History of Ulcers: If you’ve ever had a peptic ulcer or been diagnosed with H. pylori, your gastric defense system is already compromised. Taking NSAIDs without food can reignite the risk of perforation.
Alcohol Consumers: Alcohol directly irritates the stomach lining. Combining a hangover with ibuprofen on an empty stomach is essentially a two-pronged chemical assault on the gastric lining. This combination significantly raises the risk of acute bleeding.
Dangerous Drug Interactions (The “Triple Whammy”)
Drug interactions are a major concern. For certain prescription medications, the answer to “can you take ibuprofen on an empty stomach” shifts from “no” to “absolutely never.”
- SSRIs (Antidepressants): Drugs like Sertraline (Zoloft) or Fluoxetine (Prozac) affect platelet function. Combining them with NSAIDs can increase the risk of upper GI bleeding by up to 600%.
- Blood Thinners (Warfarin/Eliquis): This is a life-threatening combination. If ibuprofen causes even a small bleed in the stomach, the anticoagulant prevents clotting, turning a minor irritation into a medical emergency.
- Corticosteroids: Prednisone and ibuprofen both weaken the stomach lining. Taking them together increases the ulcer risk by up to 15 times compared to the general population.
How to Take Ibuprofen Safely: Practical Strategies
Knowing you need food is one thing. Knowing what to eat is another. The good news? You don’t need to prepare a full breakfast to take a pill safely.

What Counts as “Food” (You Don’t Need a Full Meal)
In pharmacy practice, we use a simple rule of thumb for buffering. You need enough substance to neutralize some acid and stimulate normal digestion. This dilutes the medication and protects the lining.
Best options:
- A glass of milk (8 oz): Often better than solid food for quick dosing. The proteins and fats coat the stomach, and milk’s near-neutral pH helps buffer acid.
- Yogurt: Provides a thick coating and beneficial probiotics.
- Crackers or toast: Simple carbohydrates that absorb excess acid effectively.
- Almond or soy milk: Plant-based milks also work well due to their viscosity and slightly alkaline nature.
What to avoid: Don’t use coffee, acidic fruit juices, or soda to wash down the pill. Coffee and soda are both acidic and carbonated beverages only make things worse. They’ll amplify the harsh environment ibuprofen already creates in your stomach.
Do Liquid Gels or Enteric-Coated Tablets Help?
Pharmaceutical companies have developed different formulations to reduce stomach risks. But none of them are a complete solution.
Enteric Coating: These tablets have a polymer barrier that resists stomach acid, allowing the pill to pass into the small intestine before dissolving. This reduces local irritation, but it does not prevent systemic COX inhibition. The bleeding risk remains. You may just feel less immediate stomach pain.
Liquid Gels: These contain solubilized ibuprofen and absorb faster. While the drug spends less time sitting in your stomach, the peak blood concentration hits faster too, shutting down prostaglandins more rapidly. You still need food.
Ibuprofen Formulations and GI Safety
| Formulation | Onset (Tmax) | Local Irritation | Systemic GI Risk | Best Use Case |
| Standard Tablet | 30-60 min | Moderate | High | General pain with food |
| Liquid Gel | 20-40 min | Low | High | Rapid relief (migraines) |
| Enteric-Coated | Delayed | Very Low | High | Chronic conditions |
| Chewable | Fast | High | High | Swallowing difficulty |
Expert Clinical Recommendations and Safer Alternatives
As a pharmacist, my priority is making sure you get pain relief without creating a new health problem. If you take NSAIDs regularly, follow what I call the “Gastric Shield” protocol.

The “Gastric Shield” Protocol
- Stay hydrated: Always take the medication with a full 8 oz glass of water. This helps dissolve the pill and assists with gastric emptying, moving the drug into the intestine where it’s absorbed.
- Stay upright: Remain sitting or standing for at least 15 to 30 minutes after taking the dose. Lying down right away can cause the pill to float back toward the esophagus or settle in one spot of the stomach, leading to localized burning.
- Consider co-therapy for chronic use: If you need daily NSAID therapy for conditions like arthritis, talk to your doctor. We often prescribe a Proton Pump Inhibitor (PPI) like Omeprazole or an H2 Blocker like Famotidine to reduce acid production while you’re on the medication. This is a standard protective strategy.
When to Call the Doctor
Be vigilant for red flags. Black, tarry stools (melena) indicate digested blood from the upper GI tract. Vomiting that looks like coffee grounds is another sign of internal bleeding. Persistent abdominal pain that doesn’t resolve with antacids requires immediate medical evaluation.
Also follow the “10-Day Rule.” If you need ibuprofen for more than 10 consecutive days, stop self-treating and see a healthcare provider for a proper diagnosis.
Common Mistakes People Make with Ibuprofen
Let’s walk through specific real-world scenarios where people frequently get things wrong. Recognizing these patterns can prevent accidental injury.

The “Hangover Cure” Mistake
Waking up after a night of drinking often means a pounding headache. But your stomach is already irritated by the alcohol, which strips the mucus layer in much the same way NSAIDs do. Taking ibuprofen on an empty stomach in this state compounds the irritation. It also stresses the liver and kidneys, which are already working overtime to clear alcohol toxins.
The “Morning Runner” Mistake
Athletes often pop ibuprofen before a run to preempt soreness, sometimes calling it “Vitamin I.” This is risky. During exercise, blood flow diverts away from the stomach to the muscles, creating a natural state of reduced blood flow (ischemia) that weakens the stomach lining. Adding ibuprofen to the mix, especially without breakfast, creates a perfect storm for gastric erosion.
The “Menstrual Cramp Rush” Mistake
Period pain can be debilitating, and the urge to take medication the second you wake up is strong. Ibuprofen is actually the right choice for the pain mechanism during menstruation. But taking it without food can trigger what’s called “NSAID dyspepsia,” piling nausea on top of existing cramps. A few crackers can make the difference between relief and vomiting.
Why Milk Works Better Than Water as a Buffer
I get asked all the time why water isn’t enough. The chemistry of the stomach explains it clearly.
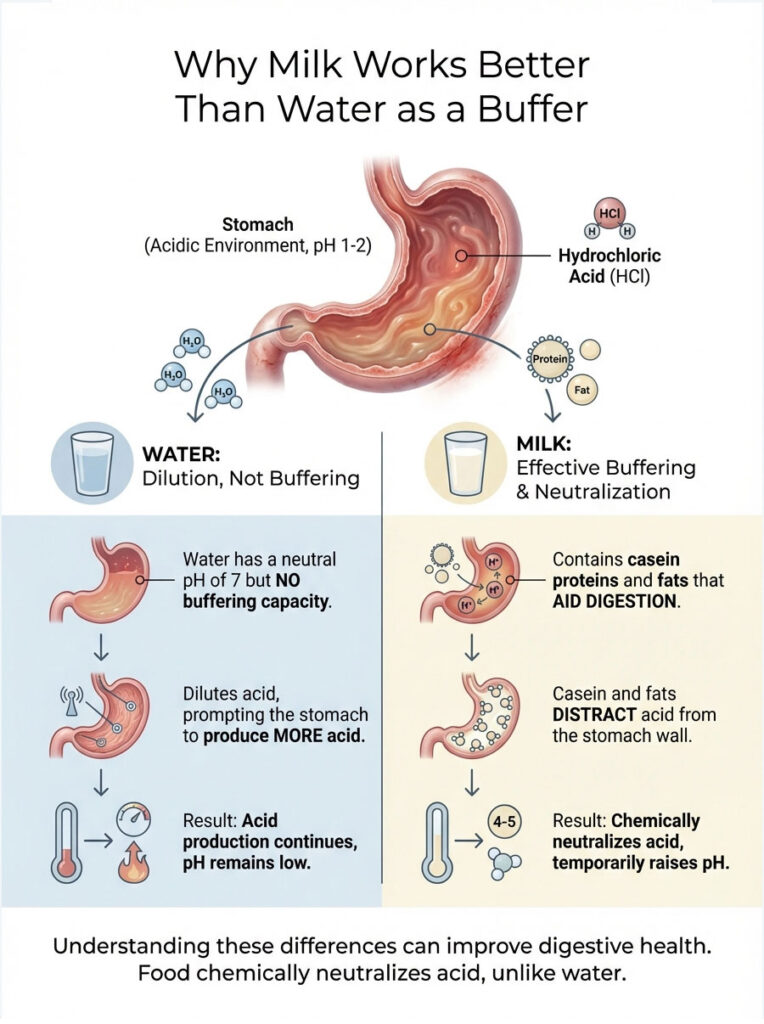
Your stomach contains hydrochloric acid (HCl). When you eat, the food acts as a buffer by binding to the hydrogen ions in the acid, which temporarily raises the pH. Milk is especially effective because of its composition. It contains casein proteins and fats that require acid for digestion. These substances effectively “distract” the acid from the stomach wall.
Water has a neutral pH of 7, but it has zero buffering capacity. It dilutes the acid slightly, but your stomach responds by pumping out more acid to compensate for the added volume. Food, on the other hand, chemically neutralizes the acid. That’s a significant difference.
Summary and Key Takeaways
So, can you take ibuprofen on an empty stomach? The clinical answer is a clear no. While ibuprofen is a powerful pain management tool, its mechanism of action makes it inherently hostile to an unprotected stomach lining. It shuts down the prostaglandins your stomach depends on for defense.

Taking ibuprofen with food isn’t an old wives’ tale. It’s a pharmacokinetic requirement for preventing gastritis and ulcers. Whether it’s a glass of milk, a piece of toast, or a cup of yogurt, providing a buffer lets the medication do its job without sacrificing your gut health.
If food is truly impossible, switch to Acetaminophen (Tylenol) or consult your pharmacist for a safer alternative.
Pharmacist’s Final Tip: Keep a small box of crackers or a shelf-stable protein shake on your nightstand. If you wake up in pain, you don’t have to drag yourself to the kitchen. Eat two crackers, drink some water, take your medication, and rest. This small habit can save you from a lifetime of stomach problems.
Frequently Asked Questions
Can I take ibuprofen on an empty stomach if I drink plenty of water?
While water helps reduce local irritation by preventing the pill from sticking to the gastric wall, it does not address systemic inhibition. Once absorbed, ibuprofen blocks the COX-1 enzymes that produce protective prostaglandins throughout the body, leaving your stomach lining vulnerable to acid regardless of how much water you drink.
How long should I wait to take ibuprofen after eating?
There is no need to wait; in fact, it is clinically recommended to take ibuprofen during or immediately after a meal. Taking the medication alongside food ensures that the buffering agents are present in the stomach simultaneously with the drug, providing immediate protection for the mucosal lining.
Is milk better than water when taking ibuprofen?
Yes, milk is often superior to water because it acts as both a physical and chemical buffer. The proteins and fats in milk coat the stomach lining, while its slightly alkaline nature helps neutralize the hydrochloric acid that becomes more damaging when ibuprofen suppresses prostaglandin production.
Does taking ibuprofen with food make it less effective or slower to work?
Food may slightly delay the Tmax, which is the time it takes for the drug to reach peak concentration in your blood, typically by 15 to 30 minutes. However, the total absorption, or Area Under the Curve (AUC), remains unchanged, meaning you receive the same level of pain relief while significantly reducing the risk of gastric erosion.
What are the early signs of stomach damage from taking NSAIDs without food?
Common early symptoms of NSAID-induced gastropathy include dyspepsia, which is a gnawing or burning sensation in the upper abdomen, and nausea. If you experience persistent epigastric pain or acid reflux after taking ibuprofen, it is a clear signal that your gastric mucosa is being irritated.
Can I take Tylenol on an empty stomach if I am unable to eat?
Yes, acetaminophen (Tylenol) is generally safe to take on an empty stomach because it is not a traditional NSAID. It works centrally in the brain and does not inhibit the COX-1 enzymes in the stomach that are responsible for maintaining the protective mucus and bicarbonate layers.
Do liquid gel ibuprofen capsules protect the stomach better than standard tablets?
Liquid gels are designed for faster absorption, which can minimize the time the drug sits in direct contact with the stomach wall, reducing local irritation. However, they still carry the same systemic risk of shutting down protective prostaglandins once they enter the bloodstream, so they must still be taken with food.
Is it safe to take ibuprofen for a hangover on an empty stomach?
This is highly discouraged because alcohol is a direct mucosal irritant that already compromises the stomach lining. Combining a hangover with ibuprofen on an empty stomach creates a synergistic effect that drastically increases the risk of acute gastritis and gastrointestinal bleeding.
Why does ibuprofen cause stomach ulcers and internal bleeding?
Ibuprofen non-selectively inhibits COX-1 enzymes, which are essential for producing prostaglandins that stimulate mucus production and regulate blood flow to the stomach wall. Without these defenses, the stomach’s own acid can digest the tissue, leading to peptic ulcers and potential hemorrhage.
Can I take ibuprofen if I am already taking an antidepressant like Zoloft or Prozac?
Combining SSRIs with NSAIDs is risky because both classes of drugs affect platelet aggregation and the integrity of the gastric lining. This combination can increase the risk of a serious upper GI bleed by up to six times, so you should always consult your healthcare provider before using them together.
Does enteric-coated ibuprofen prevent the risk of gastric ulcers?
Enteric coating allows the tablet to pass through the stomach and dissolve in the small intestine, which significantly reduces local irritation. However, it does not prevent the systemic effect of prostaglandin inhibition, meaning the risk of developing a stomach ulcer remains if used frequently without a food buffer.
What is the best small snack to eat if I need to take ibuprofen but don’t want a meal?
You don’t need a full meal to protect your stomach; a few saltine crackers, a slice of toast, or a cup of yogurt is sufficient. These foods provide enough substance to absorb excess acid and stimulate the stomach’s natural protective secretions, acting as a “gastric shield” for the medication.
Disclaimer
This article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. The biological interactions described are general clinical observations. Always consult with a qualified healthcare professional or your local pharmacist before starting or changing a medication regimen, especially if you have underlying health conditions or are taking other prescriptions.
References
- U.S. Food and Drug Administration (FDA) – www.fda.gov – Official safety labeling and Black Box Warning requirements for non-steroidal anti-inflammatory drugs (NSAIDs).
- Mayo Clinic – www.mayoclinic.org – Clinical overview of NSAID-induced Gastropathy and Peptic Ulcer Disease symptoms and prevention.
- American Journal of Gastroenterology – Journal Publication – Research data regarding the 15-30% ulcer prevalence in chronic NSAID users.
- National Institutes of Health (NIH) – PubMed Central – Detailed pharmacokinetic studies on the Tmax and AUC of ibuprofen when co-administered with food.
- Arthritis Foundation – www.arthritis.org – Statistics on annual hospitalizations and mortality rates related to NSAID gastrointestinal complications.