As a board-certified gastroenterologist, there is one question I hear in my clinic almost every week. Patients constantly ask me: can dehydration cause diarrhea? The short, definitive medical answer is yes.
Table of Contents
Most people assume fluid loss is only a consequence of getting sick. They think you lose water after the stomach bug hits. But in reality, a lack of fluids in the body often acts as the primary trigger for severe bowel dysfunction, not the other way around.
Let me clear up this common misconception. Your digestive tract is a highly complex water management system. It depends on a strict internal balance to function properly. When your body runs low on water, the delicate environment inside your intestines becomes chaotic. That disruption sets off a chain of physiological failures that eventually show up as urgent, watery stools.

In this clinical guide, we will walk through the exact medical reasons behind sudden diarrhea and thirst. We will break down how systemic fluid loss forces your gut to behave erratically, look at cellular pressure shifts, explain the dangers of severe constipation, and cover the precise mechanisms behind this condition.
Quick Answer: Can Dehydration Cause Diarrhea?
Yes. When your body is severely dehydrated, electrolyte imbalances disrupt the cellular pumps in your gut. This forces water into your intestines instead of absorbing it. On top of that, chronic fluid restriction causes severe constipation, which leads to paradoxical diarrhea, where liquid stool leaks around impacted waste.
Key Clinical Statistics on Fluid Loss and Gut Health
- The human gastrointestinal tract processes approximately 9 liters of fluid every single day.
- According to the CDC, heat-related illnesses cause gastrointestinal distress in up to 30% of severe cases.
- Fecal impaction accounts for nearly 40% of paradoxical diarrhea cases in geriatric emergency room visits.
- Proper Oral Rehydration Salts (ORS) can increase intestinal water absorption by up to 400% compared to plain water.
- A drop in total body water of just 2% is enough to significantly alter gastric emptying rates.
- More than 70% of long-distance runners experience ischemic bowel symptoms due to acute fluid loss.
How Dehydration Disrupts Gut Motility
To understand the gastrointestinal effects of fluid loss, you first need to see how the gut manages liquids. Your digestive system does not just process food. It actually acts as the primary hydration controller for your entire body.
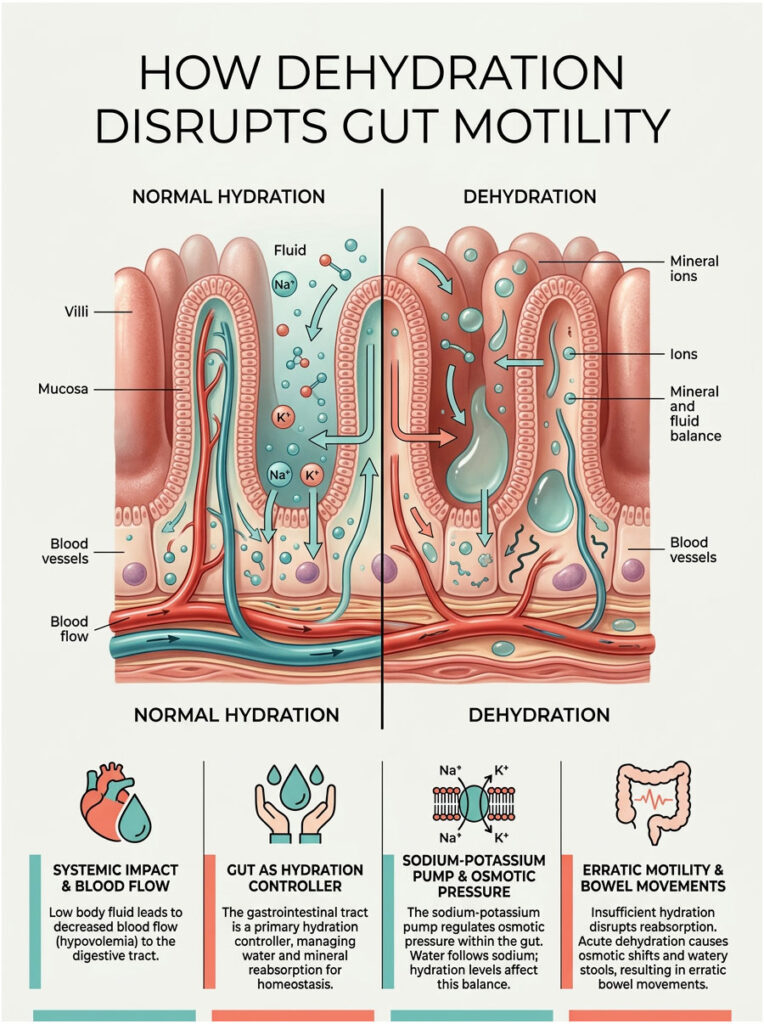
When this complex system fails, the results are immediate and uncomfortable. Your hydration status and your bowel habits are deeply intertwined. Let me explain exactly how this bidirectional relationship works.
Hypovolemia and Gastrointestinal Homeostasis
Hypovolemia is the clinical term for a decrease in blood volume circulating through your body. When you do not drink enough fluids, your total blood volume drops significantly, creating a state of systemic panic in the nervous system.
Your body immediately prioritizes blood flow to vital organs like the brain, heart, and lungs. As a direct result, it restricts blood flow to the digestive tract. This sudden disruption breaks gastrointestinal homeostasis, the perfect balance of water and minerals required for healthy digestion.
Every day, your stomach, liver, and pancreas secrete massive amounts of fluid into the digestive tract to break down food. Your intestines must then reabsorb that fluid back into the bloodstream. If you are already low on fluids, your body struggles to complete this crucial reabsorption cycle.
Clinical Note: The gut requires precise water balance to process waste efficiently. When systemic hydration drops, the intestines cannot maintain normal function. This is exactly why fluid imbalance directly leads to erratic bowel movements.
The Sodium-Potassium Pump and Osmotic Pressure Shifts
At the cellular level, your gut relies on something called the sodium-potassium pump. This vital mechanism sits in the cell membranes of your intestinal lining. It works constantly to move sodium out of cells while pulling potassium in.
Why does this matter? Because water always follows sodium in the human body. This movement creates a chemical gradient known as osmotic pressure. Under normal conditions, this gradient allows your body to pull water out of intestinal waste and back into the bloodstream, keeping stool solid and well-formed.
When you lack sufficient fluids, blood sodium levels change drastically. The sodium-potassium pump begins to fail under stress. It can no longer maintain the correct gradients needed for absorption.
Because of this mechanical failure, osmotic pressure shifts in the opposite direction. Instead of pulling water out of waste material, the altered pressure pulls water from your tissues into the intestines. This sudden, massive influx of water into the bowel causes acute, watery stools.
The Anatomy of Intestinal Water Absorption
To fully grasp how fluid deficits destroy normal digestion, we need to look at the anatomy of the gut. The human intestines are marvels of biological engineering, specifically designed to maximize water retention. When you deprive them of hydration, they malfunction in a big way.
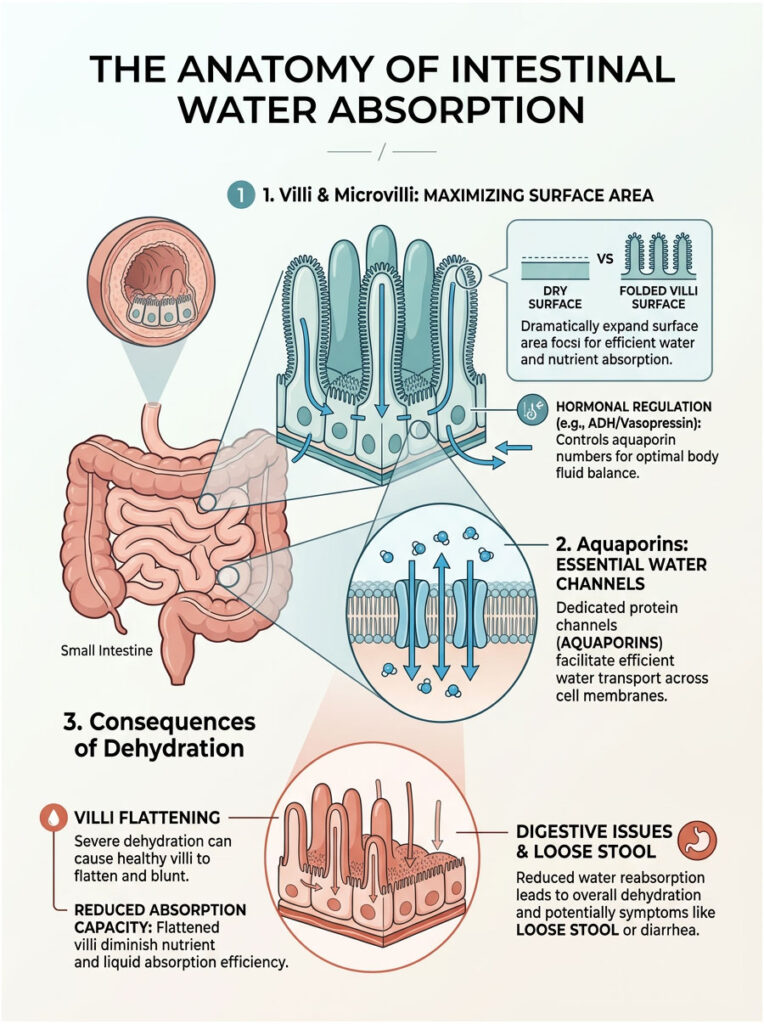
The Role of Aquaporins in the Gut
Aquaporins are specialized protein channels inside your cell membranes. Think of them as microscopic plumbing pipes. Their sole purpose is to transport water molecules quickly across the intestinal wall.
During normal digestion, these channels open and close based on your body’s hydration needs. Hormones from your brain tell the aquaporins exactly how much liquid to absorb. When you become severely dehydrated, hormonal signaling becomes frantic and confused. The brain sends panic signals that actually cause some aquaporins to shut down entirely.
Unfortunately, shutting down these channels means the water in your gut has nowhere to go. It remains trapped inside the intestinal tube, mixes with digestive waste, and results in an urgent need to use the restroom.
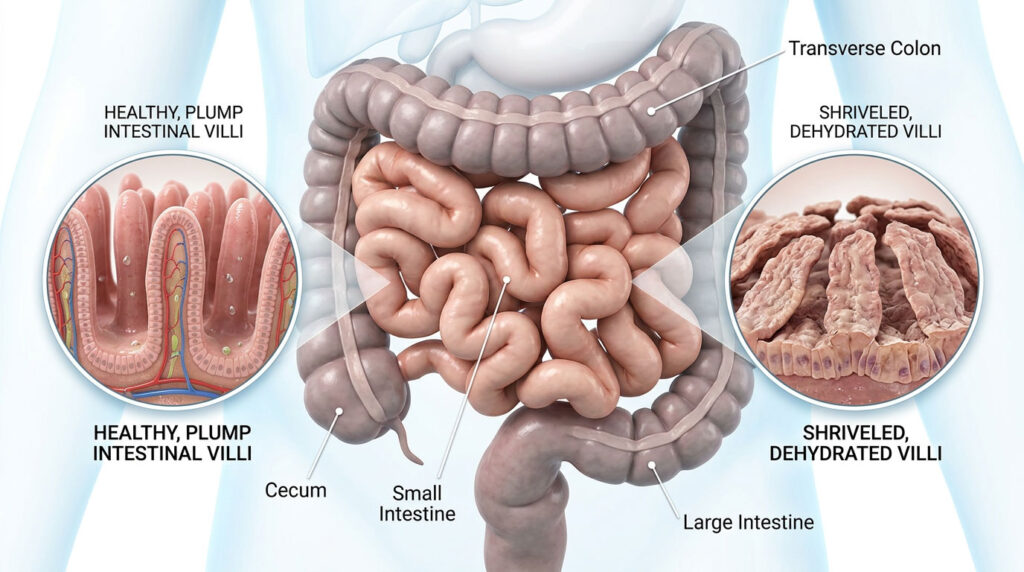
Villi and Microvilli: Why Surface Area Matters
The inside of your small intestine is not smooth like a garden hose. It is covered in millions of tiny, finger-like projections called villi. These villi are then covered in even smaller projections called microvilli.
This design increases the surface area of your gut enormously. If you flattened out all the villi in your intestines, they would cover roughly the area of a tennis court. That massive surface area is essential for absorbing nutrients and liquids efficiently.
Adequate hydration keeps these villi plump and functional. When you stop drinking enough water, they begin to shrivel and flatten out. A flattened intestinal lining cannot absorb liquids properly. The surface area shrinks drastically, leaving the gut unable to process incoming fluids. The unabsorbed liquid simply rushes past the damaged villi and exits the body as loose stool.
Clinical Mechanisms: How Fluid Loss Triggers Loose Stools
Now that we have covered the cellular and anatomical foundations, let us look at the practical triggers. How exactly does a lack of water turn into an active bowel emergency? There are three specific clinical mechanisms at play.
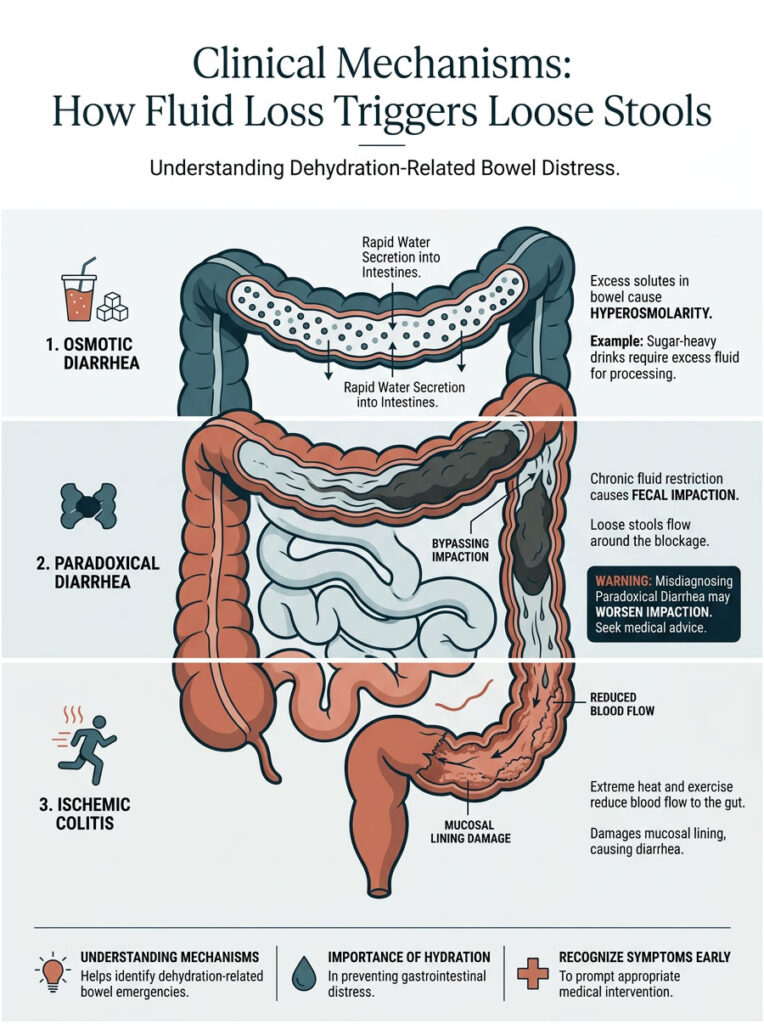
Osmotic Diarrhea and Solute Concentration
Osmotic diarrhea occurs when too many solutes, such as unabsorbed sugars, artificial sweeteners, or excess minerals, sit inside your bowel. Because your body lacks enough water to dilute these particles, the gut environment becomes hyperosmolar.
To fix this dangerous concentration, your body forcefully secretes its own water into the intestines. This floods the bowel and flushes the irritating contents out rapidly. That is a classic, textbook example of dehydration-induced diarrhea.
Consider a very common scenario. Someone feels parched on a hot day and chugs a massive, sugar-heavy soda. Because they are already low on fluids, their digestive system cannot process the heavy sugar load. The sugar sits in the gut and ferments. The altered osmotic pressure pulls even more water from surrounding tissues into the bowel. The result is an explosive bout of watery bowel movements.
Paradoxical Diarrhea: The Overflow Phenomenon
Here is a fascinating and often misunderstood medical reality. Severe constipation is actually a primary consequence of chronic fluid restriction. When you do not drink enough water, your colon extracts every possible drop of moisture from your stool to survive.
This extreme extraction leaves behind hardened, rock-like waste that becomes stuck in the lower colon. We call this fecal impaction. But how does a solid blockage lead to loose stools?
The answer is paradoxical diarrhea, also known as overflow diarrhea. While the solid mass blocks the lower colon, your upper digestive tract continues processing new food and liquid. The new liquid waste travels down, hits the blockage, and simply bypasses it. It leaks around the edges of the impaction and exits the body rapidly.
Clinical Warning: Paradoxical diarrhea is frequently misdiagnosed at home. People assume they have a standard stomach bug and take anti-diarrheal medication. This dangerously worsens the underlying impaction by paralyzing the bowel. If you feel thirsty and have loose stools but suspect constipation, see a doctor before self-treating.
This is one of the most common medical reasons for sudden diarrhea and thirst in older adults. The symptom is loose stool, but the actual disease is profound dehydration and impacted waste.
Ischemic Colitis and Heat-Induced GI Distress
Many active patients ask me: is diarrhea a symptom of heat exhaustion? The medical community recognizes this as a definitive yes. The specific mechanism behind it is called ischemic colitis.
When you exercise or work in extreme heat, your body fights to cool you down through vasodilation at the skin surface. Blood rushes from your core to the skin to release trapped heat. But that blood has to come from somewhere. Your body initiates vasoconstriction in the splanchnic circulation, which is the primary blood supply to the gut.
This temporary, severe reduction in blood flow is called ischemia. The lack of oxygen and nutrients damages the sensitive mucosal lining of the colon. The damaged, oxygen-starved colon can no longer absorb water. It spasms violently and expels its contents. This is exactly why marathon runners and outdoor workers frequently experience dehydration-induced diarrhea during hot months.
The Impact of Specific Electrolyte Deficiencies
Water alone does not keep your gut functioning. The minerals dissolved in your body water are the true drivers of digestion. When you lose fluids, you lose these critical minerals simultaneously.

Magnesium Depletion and Gut Spasms
Magnesium is responsible for over 300 biochemical reactions in the body. One of its primary jobs is regulating smooth muscle contractions. The muscles lining your intestines rely heavily on magnesium to stay relaxed.
When you sweat heavily or fail to drink enough, serum magnesium levels plummet. Without adequate magnesium, intestinal muscles cannot relax. They twitch and spasm uncontrollably, pushing waste through the colon far too quickly. Because the waste moves so fast, the colon never gets a chance to absorb water from it. The result is an urgent, liquid bowel movement.
Chloride Channels and Secretory Diarrhea
Chloride works hand-in-hand with sodium to maintain proper fluid balance inside and outside your cells. Your gut lining has specific chloride channels that control fluid secretion.
Severe dehydration causes these chloride channels to malfunction. They become locked in an open position. When that happens, chloride pours into the intestinal cavity continuously. Because water naturally follows chloride, massive amounts of bodily fluid flood into the gut. This is what we call secretory diarrhea, where the body literally secretes its own water reserves into the bowel.
This process is incredibly dangerous because it accelerates fluid loss exponentially. It creates a vicious cycle where fluid loss causes even more fluid dumping. Breaking this cycle requires precise medical intervention.
Diagnosing Dehydration-Induced Diarrhea
When a patient arrives at my clinic with severe bowel issues, I need to perform a careful differential diagnosis. Is a virus causing the problem, or is the patient suffering from profound fluid loss? Understanding the difference is critical for proper treatment.
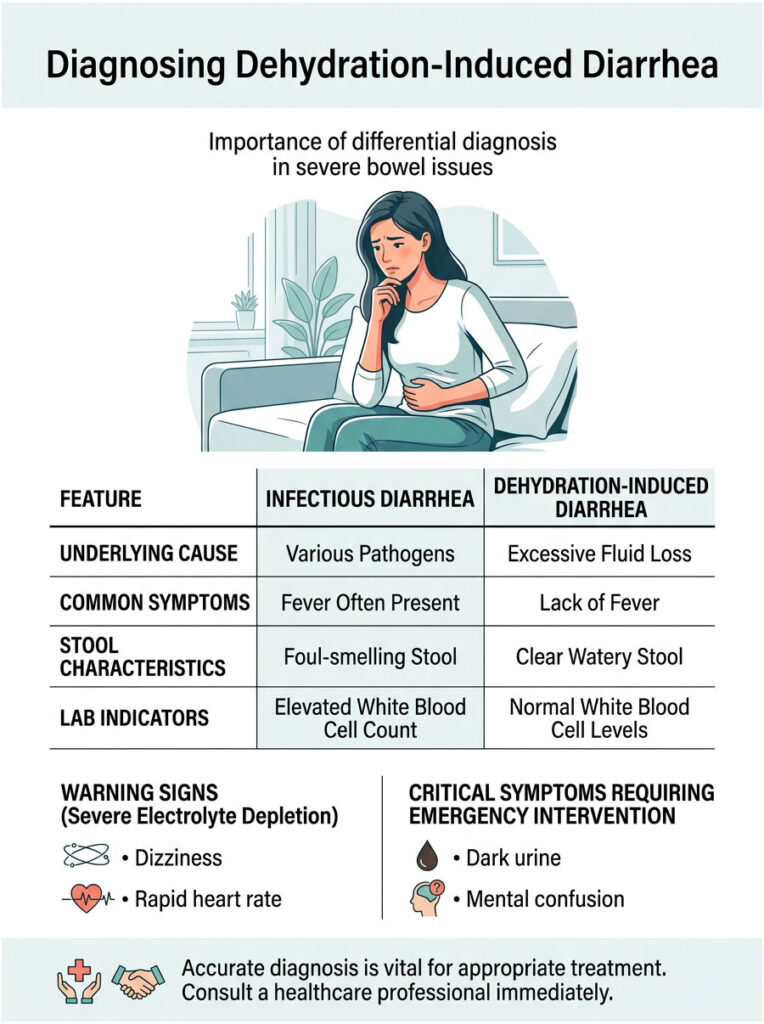
How Doctors Tell the Difference Between Infection and Fluid Imbalance
Infectious causes like norovirus or bacterial food poisoning behave very differently from a purely fluid-driven event. Pathogenic infections typically cause a high, sudden fever because the body raises its core temperature to fight the invading bacteria. Pure dehydration-induced diarrhea rarely presents with a fever, unless severe heatstroke is involved.
Lab work also tells a clear story. A bacterial infection shows an elevated white blood cell count on blood tests. If the issue is strictly a fluid and mineral imbalance, white blood cells usually remain normal.
We also evaluate the stool itself. Pathogenic stools are often extremely foul-smelling and may contain visible mucus or blood. Stools resulting from a disrupted sodium-potassium pump tend to be clear, watery, and lack significant odor.
Warning Signs of Severe Electrolyte Depletion
It is vital to recognize when a simple fluid deficit becomes a true medical emergency. Electrolyte depletion happens incredibly fast when the bowel continuously flushes out vital minerals.
What are the signs of severe dehydration in adults with diarrhea? Watch for extreme dizziness upon standing, a rapid resting heart rate, and very poor skin turgor. If you pinch the skin on the back of your hand and it stays tented upward, you are dangerously dry.
Dark, tea-colored urine is another major warning sign that your kidneys are struggling. Severe electrolyte depletion also leads to mental confusion, profound lethargy, and painful muscle cramping. These symptoms require immediate emergency medical intervention.
Differential Diagnosis: Infection vs. Dehydration
| Clinical Feature | Infectious Diarrhea | Dehydration-Induced Diarrhea |
| Primary Trigger | Viral, bacterial, or parasitic infection | Severe fluid loss, heatstroke, or fecal impaction |
| Fever | Frequently present and often high | Typically absent (unless heatstroke is involved) |
| Stool Characteristics | Often foul-smelling, may contain mucus or blood | Watery, clear, or liquid leaking around solid stool |
| Other Symptoms | Nausea, vomiting, body aches, chills | Extreme thirst, dry mouth, dark urine, muscle cramps |
| Onset Speed | Rapid, usually 12 to 48 hours after exposure | Gradual onset following prolonged fluid restriction |
Medications That Can Worsen Dehydration and Diarrhea
Sometimes, the root cause of fluid loss is sitting right in your medicine cabinet. Many common prescription drugs actively strip water from your body. When combined with poor drinking habits, these medications can guarantee bowel dysfunction.

Diuretics and Blood Pressure Medications
Millions of people take diuretics, often called water pills, to manage high blood pressure or heart failure. These drugs intentionally force your kidneys to excrete excess sodium and water into urine.
While excellent for your heart, they can be rough on your gut. If you take a strong diuretic and fail to drink enough replacement fluids, your blood volume drops. Your body responds by pulling water away from the colon. This triggers the same ischemic responses discussed earlier. The colon spasms, osmotic pressure reverses, and you experience sudden loose stools.
Patients on blood pressure medications need to be especially careful about daily water intake.
Laxative Abuse and the Rebound Effect
This is a frustrating cycle I see regularly in my gastroenterology clinic. A patient becomes slightly constipated due to mild dehydration. Instead of drinking more water, they take a powerful stimulant laxative.
The laxative forces the bowel to dump massive amounts of water to clear the stool. This artificially induced diarrhea leaves the patient profoundly dehydrated. The colon is now completely empty and dry. Because they are now severely dehydrated, the body locks down all remaining fluids, causing an immediate rebound constipation that is much worse than the original problem.
The patient takes another laxative, and the destructive cycle continues. You cannot cure dehydration-induced constipation with a pill. You must fix the underlying fluid deficit first. Stimulant laxatives only mask the true problem while making cellular damage worse.
Recent Research on Dehydration and Gut Health
The field of gastroenterology is constantly evolving. In recent years, researchers have uncovered much deeper connections between systemic hydration and cellular gut health. The gastrointestinal effects of fluid loss go far beyond simple water movement. The actual structural integrity of your gut is compromised when you dry out.
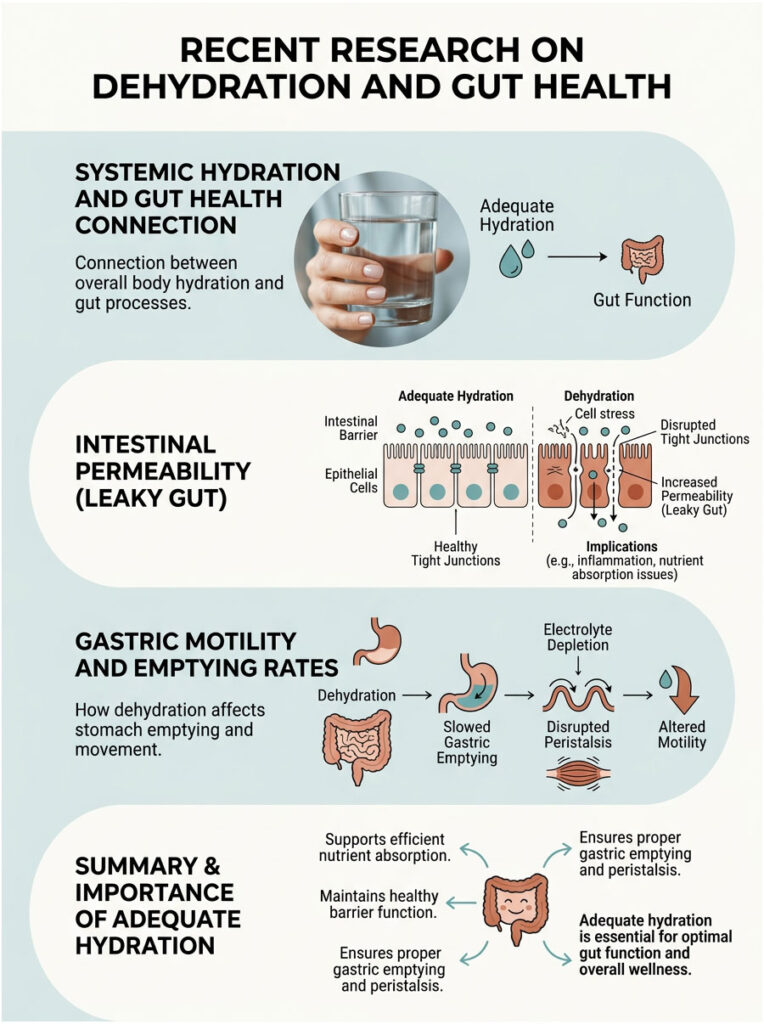
Intestinal Permeability and Leaky Gut
Recent clinical studies focus heavily on the microscopic mucosal lining of the intestines. This lining is made up of epithelial cells held together by proteins called tight junctions. These junctions act as biological security gates, controlling what enters your bloodstream.
Prolonged fluid restriction severely compromises these tight junctions. Without adequate water and stable sodium levels, epithelial cells physically shrink. As they shrink, the tight junctions pull apart. This creates increased intestinal permeability, commonly known as leaky gut.
When the gut becomes highly permeable, erratic fluid shifts occur instantly across the barrier. Water from the bloodstream leaks backward through the broken junctions into the intestinal tube. This structural failure makes loose stools absolutely inevitable.
Altered Gastric Emptying and Peristalsis Disruption
Another area of recent medical research involves gastric motility. Clinical trials consistently show that even a minor 2% drop in total body water alters gastric emptying rates.
Fluid scarcity slows stomach emptying significantly, leading to nausea and bloating. But the problems do not stop there. The lack of fluids causes profound peristalsis disruption further down the tract. Peristalsis is the rhythmic, wave-like muscle contraction that moves waste through your colon.
When severe electrolyte depletion sets in, the nervous system governing peristalsis begins to misfire. Colon muscles spasm erratically, pushing waste through too quickly. Because transit time becomes so fast, the colon completely fails at its critical water reabsorption duties.
Safe Rehydration: What to Drink and What to Avoid
If you are experiencing severe GI distress from fluid loss, you must treat it correctly. Drinking the wrong types of fluids can actually make things worse. Rehydration is a precise science, and you need to follow established clinical protocols to restore gut health safely.

The Danger of Plain Water and Hyponatremia
The most common mistake patients make is chugging massive amounts of plain water during a severe diarrheal episode. This well-intentioned action is actually dangerous.
Plain purified water contains zero electrolytes. When you flood an irritated, mineral-depleted gut with plain water, you dilute already low blood sodium levels. This rapid dilution can trigger a life-threatening condition called hyponatremia, which is dangerously low blood sodium. It causes cellular swelling, brain edema, and massive GI distress.
The gut responds to this plain water influx by flushing it out immediately. You drink water, you trigger osmotic dumping, and you experience even more watery stools. You must break this cycle with the proper mineral balance.
How Oral Rehydration Solution (ORS) Works
To fix a broken sodium-potassium pump, you need a precise medical tool. That tool is an Oral Rehydration Solution (ORS).
ORS exploits a biological mechanism called the sodium-glucose cotransport system. Your intestinal walls have cellular receptors that require both sodium and glucose to activate. When you consume the exact right ratio of sugar and salt, these receptors open up. They actively pull sodium across the intestinal wall, and water follows immediately behind it. This mechanism bypasses the damaged osmotic pressure gradients entirely.
The World Health Organization (WHO) provides the gold standard ORS formula. You can purchase packets at any pharmacy. In a pinch, you can mix a basic version at home: one liter of clean water, six teaspoons of sugar, and one-half teaspoon of salt.
Using a properly formulated ORS is the best way to resolve dehydration-induced diarrhea quickly. It restores minerals while stopping fluid loss.
When You Need IV Fluids
Sometimes, oral fluids are not enough. If a patient reaches the dangerous stage of hypovolemic shock, they need immediate emergency intervention.
If you cannot keep any oral fluids down due to severe, continuous vomiting, you need an IV. If you exhibit signs of severe dehydration, including an inability to urinate for over eight hours, profound mental confusion, or a resting heart rate over 100 beats per minute, do not attempt to manage this at home. Get to an emergency room.
Comparing Rehydration Fluids
| Fluid Type | Electrolyte Content | Osmolality | Clinical Recommendation |
| WHO Standard ORS | Optimal (Sodium, Potassium, Chloride) | Isotonic (ideal for absorption) | Gold Standard. Best for rapid rehydration and gut recovery. |
| Sports Drinks | Low Sodium, High Potassium | Hypertonic (too much sugar) | Not Recommended. High sugar worsens osmotic diarrhea. |
| Plain Water | None | Hypotonic (dilutes blood sodium) | Use with Caution. Fine for daily maintenance, poor for acute recovery. |
| Broths and Soups | High Sodium | Variable | Acceptable. Good secondary option if ORS is unavailable. |
Real-World Clinical Scenarios
Medical theories matter most when applied to actual patient care. Based on years of clinical experience, here are two generalized scenarios that illustrate how fluid imbalance triggers bowel dysfunction in very different populations.

Geriatric Patients and Fecal Impaction
Consider an 82-year-old patient who arrives at the emergency room with sudden, uncontrollable watery stools. The family assumes a contagious stomach virus. But on examination, there is no fever and white blood cells are normal. Skin turgor is very poor, and the patient admits to drinking only one small glass of water daily.
An abdominal X-ray reveals a massive fecal impaction blocking the descending colon. This is a classic case of paradoxical diarrhea. Decreased thirst mechanisms in aging populations lead directly to chronic fluid restriction. The colon dries out the stool over weeks. New liquid waste simply leaks around the blockage.
Treatment involves manually clearing the impaction and administering IV fluids, not anti-diarrheal medication. The symptom is loose stool, but the actual disease is profound dehydration.
Athletes, Heat Exhaustion, and Acute Bowel Episodes
Now consider a different scenario. A healthy 30-year-old endurance athlete is running a marathon in 90-degree summer heat. Around mile 18, intense stomach cramps hit, followed by an acute diarrheal episode.
What happened inside the body? Heavy, continuous sweating caused massive systemic fluid loss. To prevent overheating, the body diverted blood away from the gut to the skin surface. This emergency diversion caused instant splanchnic ischemia. The sudden lack of oxygen to the bowel made the intestinal lining spasm violently, dumping remaining water into the colon.
The athlete required a strict ORS protocol to stabilize serum sodium and restore normal peristalsis. This is a textbook example of why knowing about dehydration-induced diarrhea matters for active people.
Preventing Dehydration-Induced Bowel Issues
The best way to handle dehydration-related bowel problems is to prevent them entirely. Proactive hydration is the cornerstone of excellent digestive health.

Daily Baseline Fluid Requirements
The old advice of drinking eight glasses of water a day is oversimplified. Your actual fluid needs depend on body mass, local climate, and daily activity level.
A better clinical rule of thumb is to drink half your body weight in ounces of water daily. If you weigh 160 pounds, your baseline goal should be 80 ounces. However, increase that significantly if you consume diuretics like coffee or alcohol. For every cup of coffee, add an extra glass of water. This simple math prevents the slow, creeping fluid deficit that ruins gut motility.
Dietary Adjustments for Optimal Gut Hydration
You do not have to get all your hydration from a water bottle. Roughly 20% of your daily fluid intake can come from the foods you eat. Water-rich fruits and vegetables are a fantastic way to maintain intestinal moisture. Cucumbers, watermelon, celery, and strawberries are all composed of over 90% water and provide natural electrolytes.
Also monitor your soluble fiber intake. Soluble fiber acts like a sponge in the gut, soaking up water to form soft, bulky stools. If you eat high-fiber foods without drinking enough water, you risk creating a cement-like blockage. Always pair fiber supplements or high-fiber meals with a large glass of water to keep the digestive tract lubricated and moving smoothly.
Daily Electrolyte Requirements for Gut Health
| Electrolyte | Daily Recommended Intake | Primary Gut Function |
| Sodium | 1,500 – 2,300 mg | Drives the osmotic gradient to absorb water from the intestines. |
| Potassium | 3,400 – 4,700 mg | Balances sodium to maintain the cellular sodium-potassium pump. |
| Magnesium | 310 – 420 mg | Relaxes intestinal smooth muscle to prevent rapid transit spasms. |
| Chloride | 2,300 mg | Regulates fluid secretion channels inside the intestinal lining. |
Key Takeaways: Can Dehydration Cause Diarrhea?
We have covered a substantial amount of clinical ground in this guide. The physiological link between your hydration status and your bowel habits is undeniable.

So, can dehydration cause diarrhea? Absolutely yes. It is not just a secondary symptom of being sick. It is a primary, complex physiological trigger that disrupts the entire digestive system. Here are the most important takeaways:
- Osmotic Pressure Reversal: Severe fluid loss destroys the function of the sodium-potassium pump. This reverses normal osmotic gradients, pulling water into the bowel and causing urgent, watery stools.
- Paradoxical Diarrhea: Chronic lack of water causes severe constipation, leading to overflow diarrhea where liquid waste leaks around a solid fecal impaction.
- Heat and Ischemia: Extreme heat causes blood to rush away from the gut to cool the skin. This splanchnic ischemia damages the colon and triggers immediate loose stools.
- ORS Over Plain Water: Never chug plain water to fix severe fluid loss. Use properly formulated Oral Rehydration Salts to activate the sodium-glucose cotransport mechanism and safely restore electrolyte balance.
Your gut health depends on consistent, intelligent hydration. By understanding the mechanisms behind dehydration-induced diarrhea, you can take proactive steps to protect your digestive system and avoid serious complications.
Frequently Asked Questions
Can dehydration directly cause diarrhea?
Yes. As a board-certified gastroenterologist, I can confirm that severe fluid loss disrupts the sodium-potassium pump in your intestinal lining. This failure reverses normal osmotic pressure, pulling water from your tissues into the bowel instead of absorbing it, which results in urgent, watery stools.
What is paradoxical diarrhea and how does it relate to hydration?
Paradoxical diarrhea, or overflow diarrhea, occurs when chronic fluid restriction leads to a fecal impaction—a hardened mass of waste in the colon. Liquid stool from the upper digestive tract leaks around this solid blockage, creating the illusion of diarrhea when the underlying cause is actually severe constipation and dehydration.
Why does heat exhaustion often lead to gastrointestinal distress?
During heat exhaustion, the body redirects blood flow to the skin surface to regulate temperature. This causes splanchnic ischemia, a significant reduction in blood flow to the gut. The resulting lack of oxygen damages the intestinal mucosa and triggers violent spasms, leading to acute heat-induced diarrhea.
Is it safe to drink plain water to treat dehydration-induced diarrhea?
Drinking only plain purified water during a severe episode is often counterproductive. It lacks the essential electrolytes needed to fix the osmotic balance and can lead to hyponatremia (dangerously low blood sodium). This often triggers a ‘dumping’ effect where the gut flushes the plain water out immediately, worsening the condition.
How do electrolyte deficiencies like magnesium affect bowel movements?
Magnesium is vital for regulating smooth muscle contractions in the gut. When dehydration causes magnesium levels to plummet, the intestinal muscles cannot relax and begin to spasm. these spasms push waste through the colon too quickly for water reabsorption to occur, resulting in liquid stools.
What are the clinical warning signs of severe dehydration in adults with diarrhea?
You should seek emergency medical care if you experience neurological or physical red flags such as mental confusion, a resting heart rate over 100 beats per minute, an inability to urinate for more than eight hours, or poor skin turgor where the skin stays ‘tented’ when pinched.
What is the medical benefit of using an Oral Rehydration Solution (ORS)?
An ORS is formulated to exploit the sodium-glucose cotransport mechanism. By providing a precise ratio of sugar and salt, it forces the intestinal receptors to pull sodium and water into the bloodstream, effectively bypassing the damaged osmotic gradients that plain water cannot fix.
Can blood pressure medications or diuretics cause diarrhea?
Yes. Diuretics, or ‘water pills,’ intentionally force the kidneys to excrete sodium and water. If a patient does not increase their fluid intake to compensate, the resulting hypovolemia can trigger the same ischemic gut responses and osmotic shifts that lead to sudden diarrhea.
How does dehydration affect the ‘leaky gut’ or intestinal permeability?
Prolonged fluid restriction causes the epithelial cells in the gut lining to shrink, which pulls apart the ‘tight junctions’ that maintain the intestinal barrier. This increased permeability allows water from the bloodstream to leak backward into the intestinal tube, making loose stools inevitable.
What is the role of aquaporins in dehydration-induced bowel issues?
Aquaporins are microscopic protein channels that transport water across the intestinal wall. During severe dehydration, hormonal panic signals can cause these channels to shut down or malfunction. This traps water inside the gut lumen, which then exits the body as watery diarrhea.
Why does the body secrete water into the gut when it is already dehydrated?
This is known as osmotic diarrhea. When the gut becomes hyperosmolar due to unabsorbed solutes (like sugars or minerals) and lacks sufficient water to dilute them, the body forcefully secretes its own remaining water reserves into the intestines to flush out the imbalance.
How much water should I drink daily to maintain optimal gut motility?
A clinical rule of thumb is to drink half your body weight in ounces of water daily. For example, a 160-pound individual should aim for 80 ounces of hydrating fluids. This baseline must be increased if you consume diuretics like caffeine or are active in high-heat environments.
Disclaimer
This article is for informational purposes only and does not constitute medical advice. The physiological mechanisms discussed regarding how dehydration can cause diarrhea are complex and require professional diagnosis. Always consult a board-certified gastroenterologist or qualified healthcare provider before beginning any rehydration protocol or treating gastrointestinal distress. If you are experiencing symptoms of hypovolemic shock or severe dehydration, seek emergency medical attention immediately.
References
- Centers for Disease Control and Prevention (CDC) – https://www.cdc.gov/extremeheat/warning.html – Clinical data on gastrointestinal distress related to heat-related illnesses and fluid loss.
- World Health Organization (WHO) – https://www.who.int/health-topics/diarrhoea – Standards for Oral Rehydration Salts (ORS) and management of secretory diarrhea.
- American Journal of Gastroenterology – Publication on Ischemic Colitis – Research regarding splanchnic circulation and the effects of acute hypovolemia on the colon.
- National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) – https://www.niddk.nih.gov/ – Information on fecal impaction and the mechanics of paradoxical (overflow) diarrhea.
- Journal of Clinical Investigation – Research Paper – Detailed study on the sodium-potassium pump and osmotic pressure shifts in the intestinal lumen.
- International Society of Sports Nutrition – Statistical Source – Data regarding ischemic bowel symptoms and gastric emptying rates in endurance athletes.