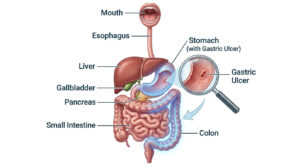
Green stool while fasting is almost always caused by rapid bile transit through an empty digestive tract. Without food to slow things down, bile salts travel from the duodenum to the rectum before gut bacteria can convert green biliverdin into brown stercobilin. This is a normal fasting adaptation in most cases. However, you should break your fast and seek medical evaluation if you notice blood in the stool, severe cramping, fever above 101°F (38.3°C), or signs of dehydration like dark urine and dizziness.
Table of Contents
A patient messaged me at 6 AM last Tuesday. She was on day three of an extended water fast and had just passed a stool that she described as “bright spinach green.” She had not eaten any green vegetables in over 72 hours. She was convinced something was seriously wrong with her liver.
This exact scenario plays out in my gastroenterology clinic multiple times a week. Green stool while fasting is one of the most visually alarming yet profoundly misunderstood digestive events in the fasting community. The vivid color triggers an immediate fear response because most people have never seen their stool look this way before.
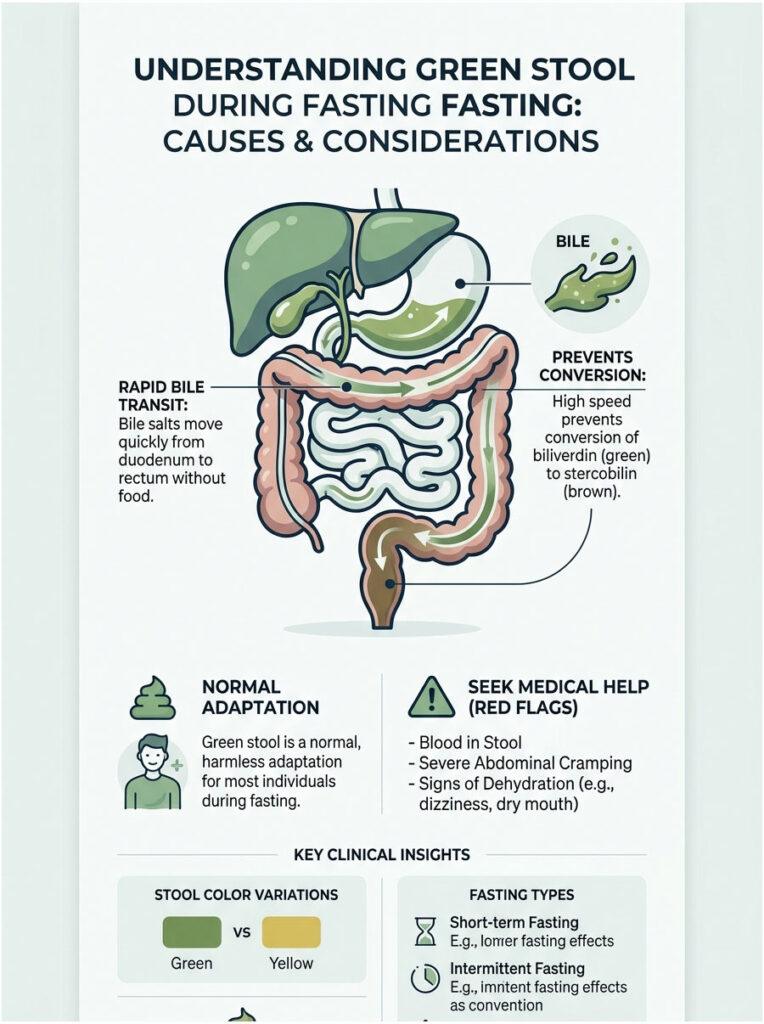
Here is the clinical reality. In the vast majority of fasting patients, green stool is a predictable and harmless consequence of bile chemistry operating without food in the system. Your liver never stops producing bile. When that bile rushes through an empty gut, the green pigments inside it do not have time to undergo their normal chemical transformation into brown. The result is stool that looks startlingly green.
But fasting is a significant metabolic stressor. There are specific situations where green stool during a fast is not harmless. In this article, I am going to walk you through the exact biochemistry of why this happens, the specific triggers unique to fasting, and the clinical red flags that demand immediate medical attention.
Explore related topics: Yellow Watery Diarrhea While Fasting: Causes, Science, and When to Worry [internal link], What Does Green Diarrhea Mean? Causes and When to Worry [internal link], Intermittent Fasting & Thyroid Health: Is It Safe for You? [internal link], and 7-Day Gallbladder Meal Plan: Pre-Surgery and After Removal Menu [internal link].
Key Clinical Statistics on Fasting and Stool Color
Daily Bile Production: The human liver produces 800 ml to 1,000 ml of bile every 24 hours, continuously, regardless of whether you are eating or fasting. This bile is inherently green due to the pigment biliverdin.
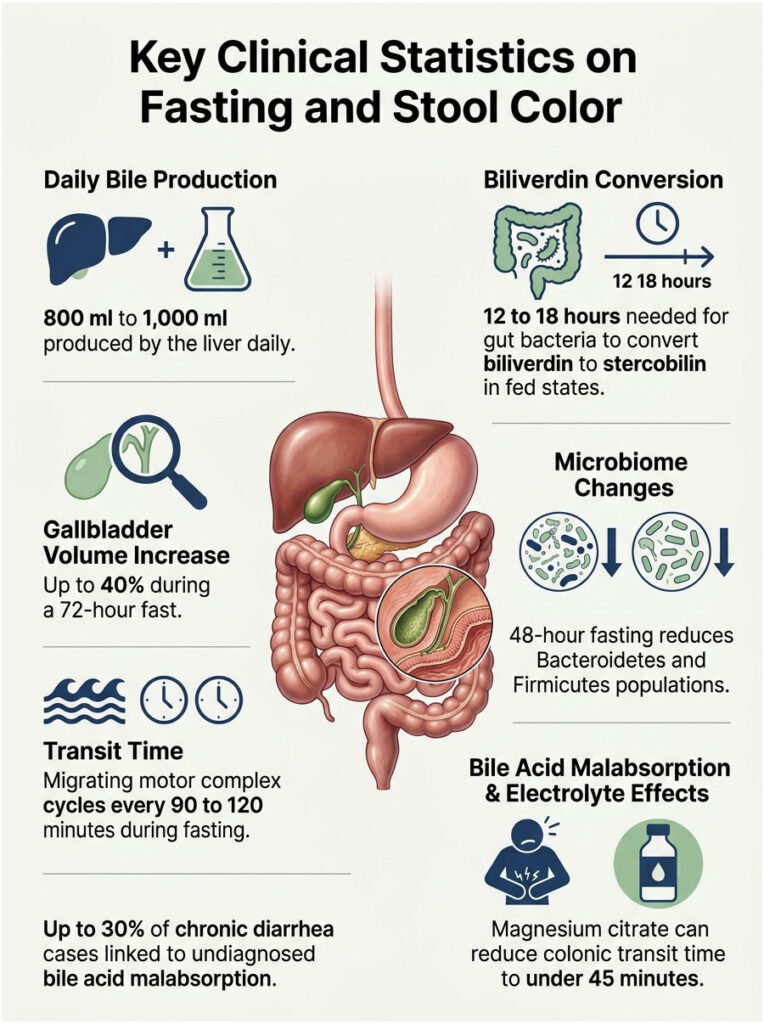
Biliverdin Half-Life: In a fed state, gut bacteria need approximately 12 to 18 hours of contact time to fully convert green biliverdin into brown stercobilin. During fasting, colonic transit can accelerate to under 4 hours, making this conversion impossible.
Gallbladder Stasis: Research published in the journal Hepatology shows that gallbladder volume increases by up to 40% during a 72-hour fast due to retained bile.
Microbiome Shift: A 2019 study in the journal Cell Reports demonstrated that just 48 hours of fasting significantly reduces populations of Bacteroidetes and Firmicutes, the bacterial phyla responsible for bile pigment metabolism.
Transit Time Acceleration: The migrating motor complex (MMC), the gut’s housekeeping wave, cycles every 90 to 120 minutes during fasting. This sweeping action moves intestinal contents far faster than during a fed state.
Bile Acid Malabsorption: The American College of Gastroenterology estimates that up to 30% of patients diagnosed with unexplained chronic diarrhea actually have undiagnosed bile acid malabsorption, a condition that fasting can unmask or worsen.
Electrolyte-Linked Motility: Magnesium citrate, a common fasting supplement, pulls water into the intestinal lumen osmotically and can reduce colonic transit time to under 45 minutes.
The Chemistry of Stool Color: Why Green Happens During a Fast
To understand green stool while fasting, you need to understand the pigment chemistry that gives stool its color in the first place. This is not a simple process. It involves your liver, your red blood cells, your gut bacteria, and the speed at which material moves through your intestines.
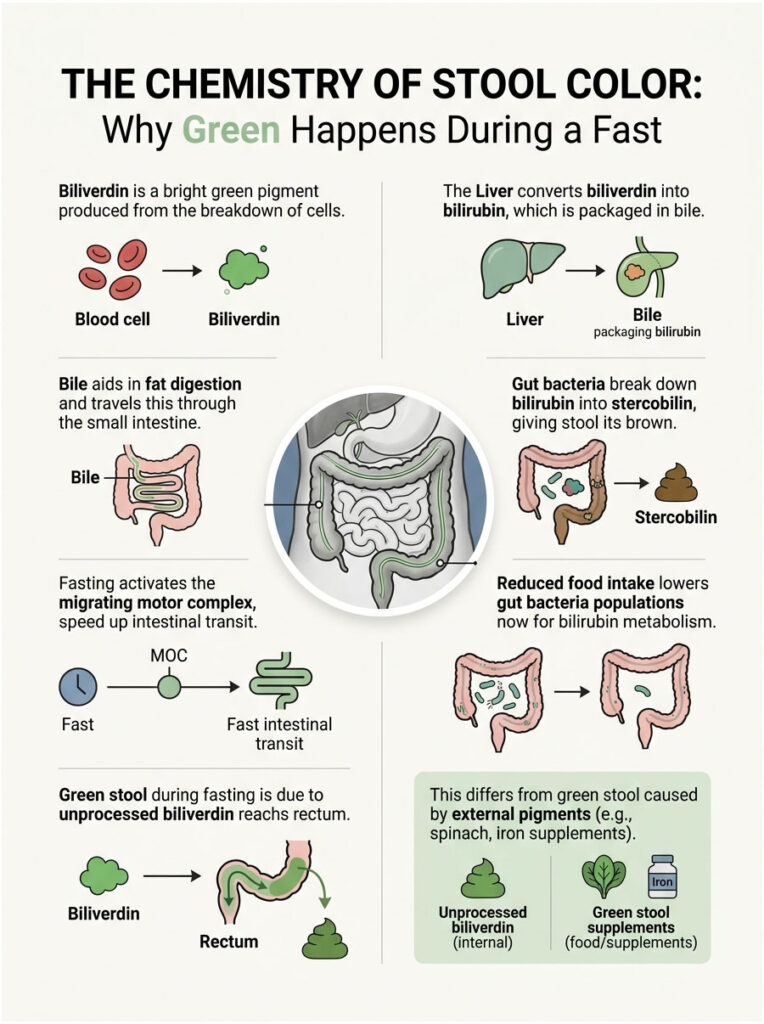
The Biliverdin-to-Stercobilin Pipeline
Every day, your body destroys approximately 200 billion old red blood cells in the spleen. The hemoglobin inside those cells gets broken down into a compound called biliverdin. Biliverdin is a bright green pigment. This is the same chemical that makes bruises turn green as they heal.
The liver converts biliverdin into bilirubin, which has a yellowish-green hue, and packages it into bile. When you eat a meal, bile gets squirted into the small intestine through the common bile duct to help digest fats.
As bile travels through the 20 feet of small intestine and into the colon, trillions of resident bacteria slowly break down bilirubin through a series of enzymatic reactions. The final product is stercobilin, a brownish pigment that gives healthy stool its characteristic color.
This entire conversion process requires two things: adequate bacterial populations and sufficient transit time. Fasting disrupts both of these requirements simultaneously.
Why Fasting Short-Circuits This Process
During a fast, the migrating motor complex becomes hyperactive. Without food to interrupt it, this rhythmic muscular contraction sweeps through the entire small intestine every 90 to 120 minutes. Each wave pushes bile-rich intestinal contents toward the colon at a much faster rate than normal.
At the same time, your gut bacteria are starving. Without the prebiotic fiber, resistant starches, and short-chain fatty acids that come from food, the bacterial species responsible for bilirubin metabolism begin to decline in population within 24 to 48 hours.
The result is a double hit. Bile moves faster than normal through a gut that has fewer bacteria available to process it. Green biliverdin arrives in the rectum essentially unchanged. What you see in the toilet is raw, chemically unprocessed bile pigment.
This is fundamentally different from green stool caused by eating spinach or taking iron supplements. In those cases, the green comes from external pigments in food. During fasting, the green comes from your own internal bile chemistry.
Seven Fasting-Specific Triggers for Green Stool
Green stool during a fast is rarely caused by a single factor. It is almost always the result of multiple physiological changes stacking on top of each other. Here are the seven most common triggers I see in my fasting patients.
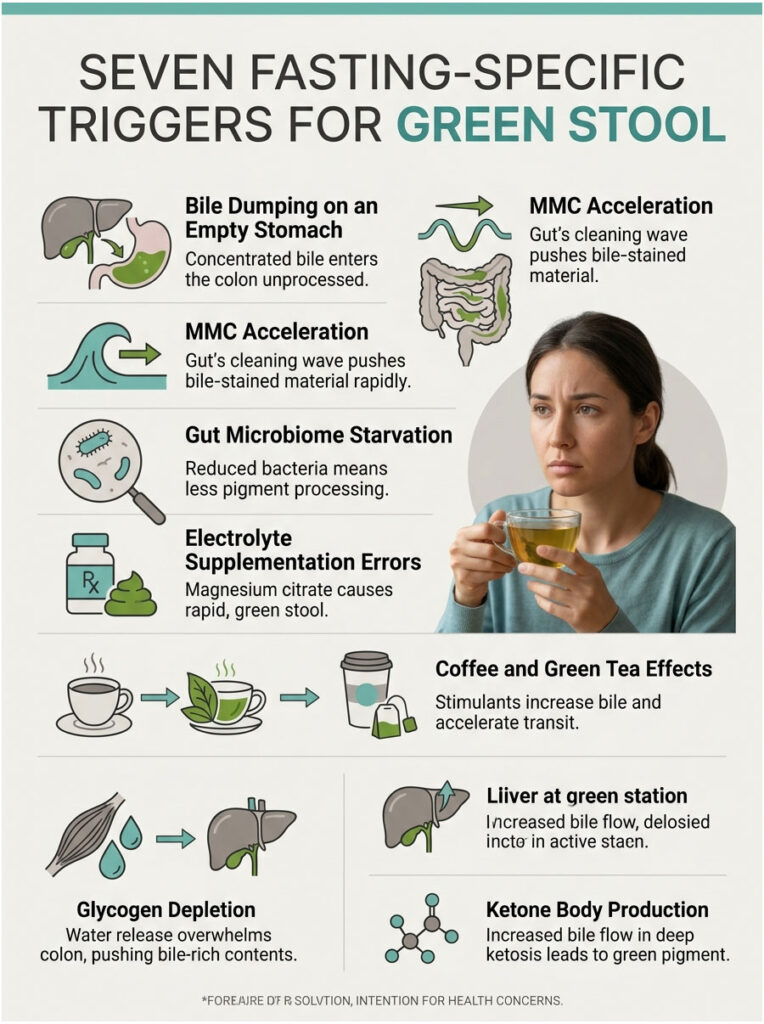
1. Bile Dumping on an Empty Stomach
Your liver produces bile continuously. In a fed state, the gallbladder stores and concentrates this bile, releasing it in controlled bursts when you eat fat. During a fast, the gallbladder becomes overfull. Internal pressure builds until a spontaneous contraction forces concentrated bile into the small intestine. With no food to bind to, this concentrated, caustic fluid travels rapidly to the colon. The green pigments inside never get a chance to be converted to brown.
2. The Migrating Motor Complex (MMC) Acceleration
The MMC is your gut’s internal cleaning wave. During eating, it gets suppressed. During fasting, it runs uninterrupted every 90 to 120 minutes. Each cycle pushes a small wave of bile-stained mucus and cellular debris through the intestines. Think of it as a dishwasher running on repeat in an empty kitchen. The more cycles it runs, the more green-tinged material reaches the colon before bacteria can process it.
3. Gut Microbiome Starvation
Your colonic bacteria depend on a steady supply of dietary fiber and undigested carbohydrates to survive. When you fast, you cut off their fuel supply entirely. Research shows significant drops in Bacteroidetes and Firmicutes populations within 48 hours of fasting. These are the exact bacterial phyla that metabolize biliverdin into brown stercobilin. Fewer bacteria means less pigment processing.
4. Electrolyte Supplementation Errors
Magnesium citrate is the single most common cause of green, watery stool in my fasting patients. It is a powerful osmotic agent that draws water into the intestines and dramatically accelerates transit time. Many popular electrolyte powders contain magnesium citrate as their primary magnesium source. Taking this on an empty stomach during a fast almost guarantees rapid, green bowel movements. Magnesium glycinate and magnesium taurate are far gentler alternatives that absorb without the laxative effect.
5. Coffee and Green Tea on an Empty Stomach
Black coffee is the unofficial drink of intermittent fasting. However, coffee is a potent stimulant of gastric acid, bile production, and colonic motility. It triggers the gastrocolic reflex, which accelerates movement through the colon. Caffeine also stimulates the gallbladder to contract. The combined effect of increased bile release and faster transit creates the perfect conditions for green stool, especially during a morning fast when the stomach has been empty for 12 or more hours.
6. Glycogen Depletion and the Water Flush
During the first 24 to 48 hours of any fast, the body burns through stored glycogen. Every gram of glycogen binds approximately 3 grams of water. As glycogen reserves deplete, the body releases up to 1.5 liters of previously bound water into the bloodstream and gastrointestinal tract. This sudden flood of fluid can overwhelm the colon’s absorptive capacity and push bile-rich contents through before bacterial processing is complete.
7. Ketone Body Production and Bile Flow Changes
As fasting progresses beyond 48 hours and the body shifts into deep ketosis, the liver dramatically increases its metabolic activity to produce ketone bodies from fatty acids. This elevated hepatic workload also increases bile production. More bile flowing through an already-empty gut means more green pigment reaching the colon. Some studies suggest that elevated ketone levels may also directly affect intestinal motility, though this research is still evolving.
Green Stool vs. Yellow Stool While Fasting: What Is the Difference?
Many of my patients confuse green fasting stool with yellow fasting stool. They are related but chemically distinct. Understanding the difference helps you assess what is happening inside your gut.

| Feature | Green Stool | Yellow Stool |
| Primary Pigment | Biliverdin (unconverted) | Bilirubin (partially converted) |
| Main Cause | Ultra-fast transit; bacteria never process bile | Bile dumping; fat malabsorption |
| Typical Timing | Day 2-5 of extended fast | Day 1-3, especially first bile dump |
| Consistency | Semi-formed to loose | Watery, urgent, explosive |
| Burning Sensation | Mild or absent | Often intense (raw bile acids) |
| Common Trigger | MMC cycles, coffee, Mg citrate | Gallbladder stasis, salt flush |
| Concern Level | Low (usually harmless) | Low-moderate (monitor hydration) |
If you are experiencing yellow watery diarrhea specifically, read our complete clinical guide: Yellow Watery Diarrhea While Fasting: Causes, Science, and When to Worry [internal link to your existing blog].
The Gut Microbiome Shift: How Fasting Starves Your Pigment-Processing Bacteria
This section is critical because it explains why green stool often gets worse as a fast progresses, not better.
Your colon is home to approximately 38 trillion bacteria. These organisms are not passive residents. They perform hundreds of essential metabolic functions, including the conversion of bile pigments from green to brown.
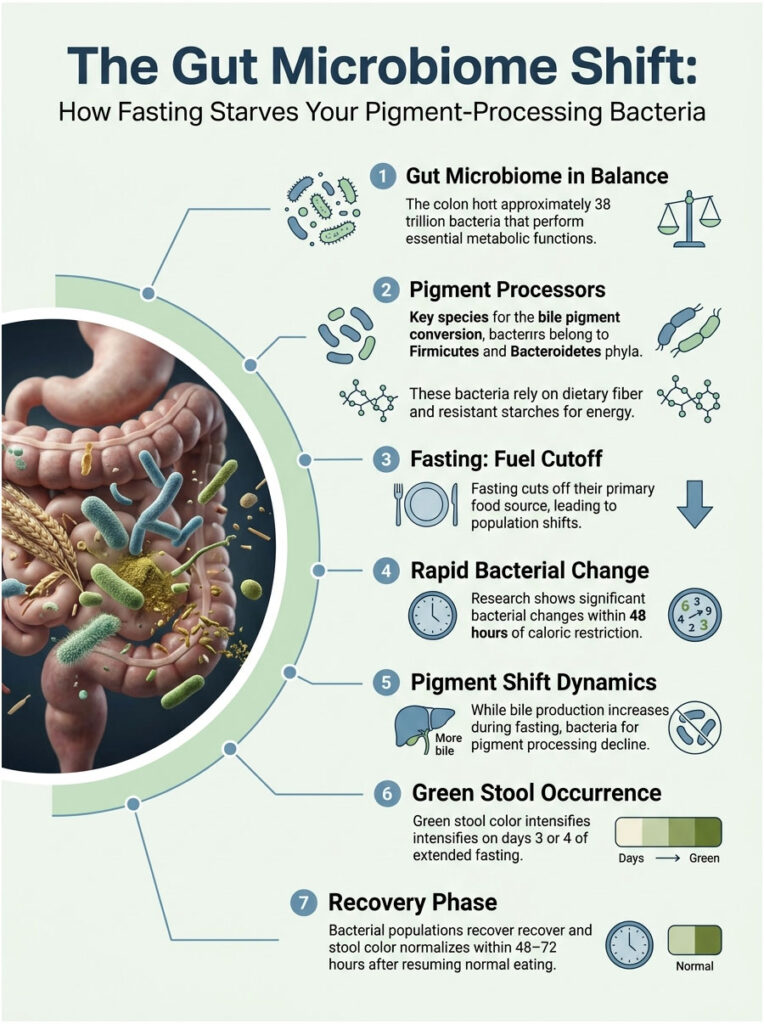
The primary bacterial species involved in this pigment conversion belong to the phyla Firmicutes and Bacteroidetes. They depend on dietary fiber, resistant starches, and other undigested food components as their primary energy source.
When you fast, you are cutting off their food supply entirely. Research published in Cell Reports has shown that significant bacterial population shifts occur within 48 hours of caloric restriction. The bacteria that process bile pigments decline in number, while certain bile-tolerant species like Bilophila wadsworthensis actually increase.
This creates a paradox. The longer you fast, the more bile your liver produces to support increased fat metabolism, and simultaneously, the fewer bacteria you have available to process that bile’s green pigments. This is why green stool tends to become more vivid on day 3 or day 4 of an extended fast, even though the initial bile dump may have happened on day 1.
The good news is that this microbiome shift is entirely reversible. Within 48 to 72 hours of resuming normal eating with adequate fiber intake, bacterial populations recover and stool color normalizes.
Green Stool by Fasting Type: Intermittent, Extended, Ramadan, and Navratri

16:8 Intermittent Fasting
Green stool is uncommon with standard 16:8 intermittent fasting because the fasting window is short enough that bacterial populations remain largely stable. When it does occur, the most common cause is drinking black coffee on an empty stomach during the fasting window. The combination of caffeine-stimulated bile release and the gastrocolic reflex can produce a green bowel movement within 30 minutes of the first cup.
24 to 72-Hour Extended Fasts
This is where green stool becomes most common and most vivid. By the 36 to 48-hour mark, glycogen stores are depleted, the microbiome has started to shift, and the MMC is running full cycles without interruption. Green stool during this phase is nearly universal and should be expected, not feared.
Ramadan Fasting (Dawn to Sunset)
Ramadan fasting presents a unique pattern. The daily fast lasts approximately 14 to 16 hours, followed by an eating window. Green stool most commonly appears in the first week as the gut adjusts to the new schedule. It may also occur after Suhoor (the pre-dawn meal) if the meal is low in fiber and high in refined carbohydrates, which speeds transit without providing adequate substrate for bacterial pigment processing.
Navratri and Religious Fasting in India
During Navratri, many people restrict their diet to fruits, milk, and specific fasting-approved foods for 9 days. While this is not a complete fast, the dramatic reduction in dietary fiber and the shift away from normal meals can still cause microbiome changes and accelerated transit. Green stool during Navratri is common and typically resolves within 2 to 3 days after resuming a normal diet.
Medical Red Flags: When Green Stool Means Something Serious
While green stool during fasting is usually benign, there are specific clinical situations where it can indicate a genuine medical problem. Fasting does not cause infections, bleeding, or organ failure. If these symptoms appear alongside green stool, they are not caused by the fast itself and they require immediate evaluation.

Bright Red Blood in or on the Stool
This is never a normal fasting symptom. Bright red blood (hematochezia) can indicate hemorrhoids, anal fissures, or more serious conditions like colitis or colorectal polyps. If you see red blood mixed with green stool, break your fast immediately and contact a healthcare provider.
Black, Tarry, Foul-Smelling Stool (Melena)
If your stool turns black and sticky with an unusually strong odor, this may indicate bleeding in the upper gastrointestinal tract, typically from a stomach ulcer or erosive gastritis. This is a medical emergency. Extended fasting can increase gastric acid production, which may worsen a pre-existing ulcer.
Fever Above 101°F (38.3°C)
Green diarrhea combined with fever suggests an infectious cause, not a fasting adaptation. Bacterial pathogens like Salmonella, Clostridioides difficile, and Campylobacter can produce green, foul-smelling diarrhea with systemic fever. If you develop a fever during a fast, the fast must be broken and medical evaluation is necessary.
Severe Abdominal Pain That Does Not Resolve
Mild cramping during fasting is common and usually related to the MMC or bile dumping. However, severe, persistent, or localized abdominal pain, especially in the right upper quadrant, can indicate gallstone complications, pancreatitis, or cholecystitis. Fasting-induced gallbladder stasis increases the risk of biliary sludge and gallstones in susceptible individuals.
Signs of Severe Dehydration
Watch for extreme thirst combined with dry, sticky mouth, sunken eyes, dark amber urine, dizziness upon standing, and rapid heart rate. If green diarrhea becomes frequent and watery, it can quickly deplete your fluid reserves. Dehydration during a fast can spiral into a dangerous clinical state. Break the fast and begin oral rehydration immediately.
How to Prevent Green Stool While Fasting: Clinical Protocols
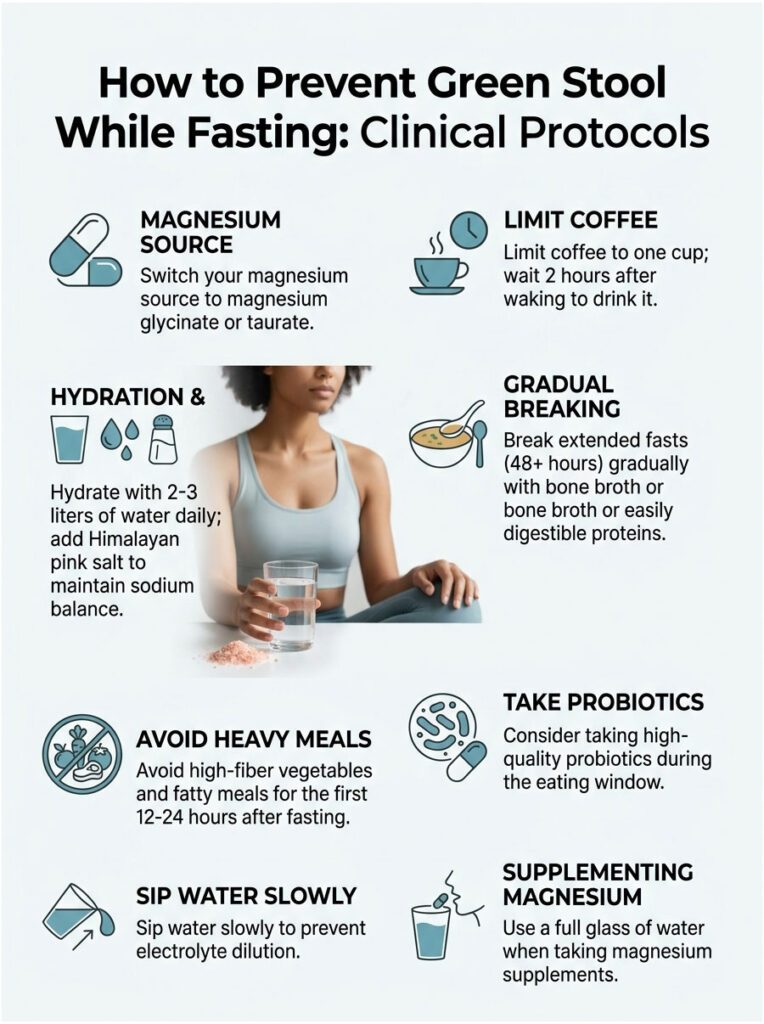
Switch Your Magnesium Source
Replace magnesium citrate with magnesium glycinate or magnesium taurate. Both forms are chelated to amino acids and absorb efficiently without the osmotic laxative effect. Take magnesium with a full glass of water rather than as a concentrated shot.
Manage Coffee Timing and Intake
If you drink coffee during your fast, limit it to one cup and do not drink it first thing in the morning on a completely empty stomach. Consider waiting at least 2 hours after waking before your first cup. Adding a small pinch of salt to your coffee can also help buffer gastric acid production.
Hydrate Strategically, Not Excessively
Overhydrating during a fast can dilute electrolytes and worsen diarrhea. Aim for 2 to 3 liters of water per day during an extended fast. Sip slowly throughout the day rather than drinking large volumes at once. Add a quarter teaspoon of Himalayan pink salt per liter to help maintain sodium balance.
Break Extended Fasts Gradually
When ending a fast of 48 hours or longer, reintroduce food slowly. Start with bone broth or a small portion of easily digestible protein like scrambled eggs. Avoid high-fiber vegetables, raw salads, and fatty meals for the first 12 to 24 hours. This gives your gut bacteria time to reactivate and your gallbladder time to resume normal emptying.
Consider Probiotics During the Eating Window
If you practice regular intermittent fasting, taking a high-quality probiotic containing Lactobacillus and Bifidobacterium strains during your eating window can help maintain bacterial diversity and support normal bile pigment metabolism.
Which Lab Tests Should You Get?
If green stool persists after you resume normal eating, or if you experience any of the red flags mentioned above, the following tests can help identify or rule out underlying conditions.

Liver Function Test (LFT): Measures SGPT, SGOT, bilirubin, alkaline phosphatase, and GGT. This test evaluates whether your liver and bile production are functioning normally. Elevated bilirubin levels can contribute to persistently abnormal stool color.
Complete Blood Count (CBC): Checks for infection markers, anemia, and inflammation. An elevated white blood cell count combined with green diarrhea may suggest a bacterial infection.
Stool Culture and Sensitivity: If infection is suspected, a stool culture identifies the specific pathogen causing green diarrhea and guides targeted antibiotic treatment.
Comprehensive Metabolic Panel (CMP): Evaluates electrolyte levels including sodium, potassium, and magnesium, which can become dangerously depleted during extended fasting.
Serum Electrolytes Test: Specifically measures sodium, potassium, chloride, and bicarbonate. Critical for anyone experiencing watery diarrhea during a fast, as electrolyte imbalances can cause heart arrhythmias.
Full Body Checkup: A comprehensive screening panel that covers liver, kidney, thyroid, blood sugar, lipid profile, and more. Recommended before starting any extended fasting protocol.
You can book any of these tests at home through HealthcareOnTime with results delivered within 24 hours. [Internal link to test booking page]
Key Takeaways
Green stool while fasting is usually harmless. It is caused by bile passing through your intestines too quickly for gut bacteria to convert its green pigments into brown. This is a normal fasting adaptation, not a disease.
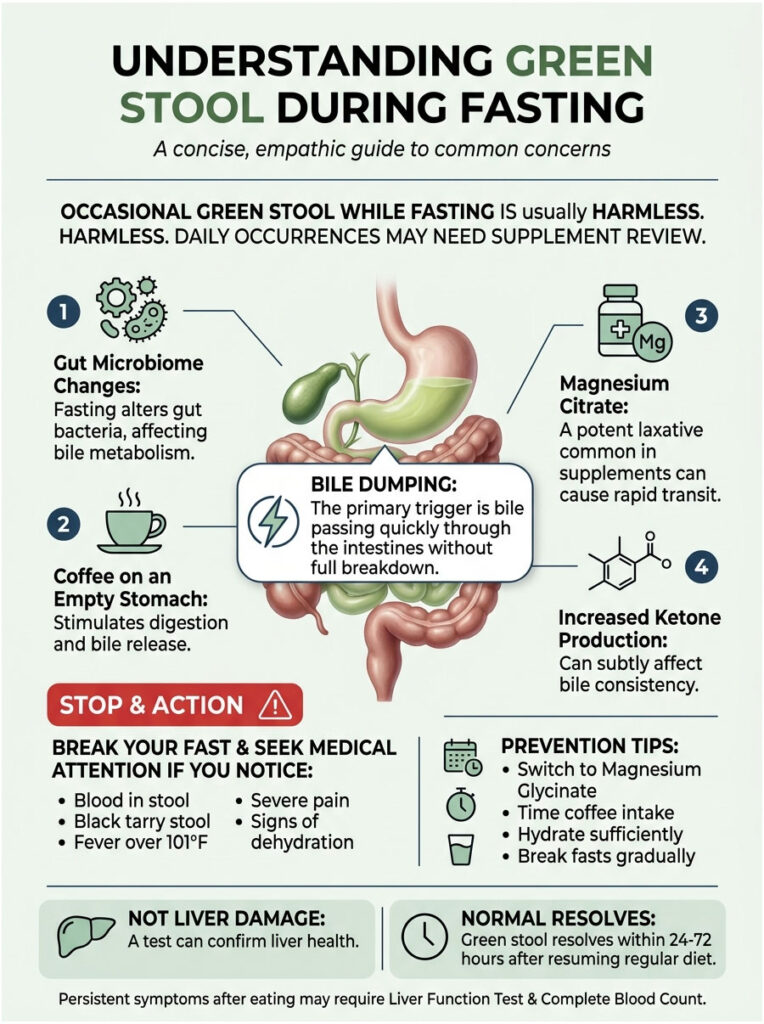
The primary triggers are: bile dumping from gallbladder stasis, migrating motor complex acceleration, gut microbiome starvation, magnesium citrate supplementation, coffee on an empty stomach, glycogen-bound water release, and increased ketone-driven bile production.
Break your fast immediately if you notice: blood in the stool, black tarry stool, fever above 101°F, severe abdominal pain, or signs of serious dehydration.
Prevention is straightforward: switch to magnesium glycinate, time your coffee intake, hydrate strategically, and break extended fasts gradually with easily digestible foods.
If symptoms persist after eating: get a Liver Function Test and Complete Blood Count to rule out underlying issues. Book an at-home test with HealthcareOnTime for results within 24 hours.
Worried about persistent green stool? Book a Liver Function Test or Full Body Checkup at home with HealthcareOnTime — sample collection at your doorstep, results within 24 hours.
Frequently Asked Questions
Is green stool while fasting normal?
Yes. In the vast majority of cases, green stool during a fast is a normal and harmless consequence of bile moving through an empty gut too quickly for bacteria to convert its green pigments into the usual brown color. It is not a sign of liver failure, infection, or poisoning.
How long does green stool last after fasting?
Green stool typically resolves within 24 to 72 hours after resuming normal food intake. Once dietary fiber reaches the colon and bacterial populations recover, stool color returns to brown. If green stool persists for more than 5 days after ending a fast, consult a gastroenterologist.
Should I stop fasting if my stool turns green?
Green stool alone is not a reason to stop fasting. However, if green stool is accompanied by blood, severe pain, fever, or signs of dehydration, you should break the fast immediately and seek medical evaluation.
Can intermittent fasting cause green poop every day?
Occasional green stool with 16:8 intermittent fasting is possible, especially if you drink coffee on an empty stomach or take magnesium citrate supplements. If it happens daily, review your supplement choices and consider switching to magnesium glycinate.
Does green stool mean my liver is damaged?
No. Green stool during fasting is a bile transit issue, not a liver problem. Your liver is actually functioning normally by continuing to produce bile. If you are concerned about liver health, a simple Liver Function Test (LFT) can give you definitive answers within 24 hours.
Why is my stool green during Ramadan?
Ramadan fasting involves a 14 to 16-hour daily fast followed by an eating window. Green stool is most common during the first week as your gut microbiome adjusts to the new meal schedule. Eating fiber-rich foods during Iftar and Suhoor can help maintain normal bacterial activity and reduce green stool episodes.
Disclaimer: This article is for educational purposes only and is not a substitute for professional medical advice. Always consult your healthcare provider for personalized diagnosis and treatment.