Overview and Statistics
Hepatitis C is a major public health concern as it affects millions of people every year in the world. According to research done by WHO, Hepatitis C viral infection affects 58 million people with chronic infection and with 1.5 million new infections every year globally.
The Hepatitis C virus is a double-stranded RNA virus that causes inflammation of the liver leading to cirrhosis and liver cancer during chronic infection. Hepatitis C virus exists in the world in several unique forms known as genotypes. Scientists have identified seven distinct genotypes and more than sixty-seven of their subtypes. It spreads through blood contaminated with the virus from an infected person to a healthy person. Therefore, drug-addict people should be on high alert. Though there is another category of person who falls into high-risk situation and they are:
- People with HIV/AIDS
- People with Diabetes
- People who have multiple sex partners( sex workers)
- Pregnant women
What is Hepatitis C?
Hepatitis C is a viral infection that primarily affects the liver. It is caused by the hepatitis C virus (HCV) and can lead to both acute and chronic forms of the disease.
- Acute hepatitis C refers to a new infection that occurs within the first six months after exposure to the virus. During this stage, some individuals may experience mild symptoms that last for a short duration. However, for most people, acute hepatitis C progresses to the chronic stage.
- Chronic hepatitis C is a long-term infection that persists if left untreated. It can have serious health consequences, including liver damage, cirrhosis (scarring of the liver), liver cancer, and, in severe cases, even death. The infection can remain asymptomatic for many years, leading to a silent progression of liver damage.
Transmission of Hepatitis C Virus
The hepatitis C virus (HCV) is primarily transmitted through specific modes of contact with infected blood. Understanding the ways in which the virus can be transmitted is crucial for prevention and awareness. Here are the main modes of transmission:
- Medical Equipment: The reuse or inadequate sterilization of medical equipment, particularly syringes, and needles in healthcare settings, can facilitate the transmission of HCV. Strict adherence to proper sterilization protocols and the use of single-use equipment is essential for preventing infections.
- Blood Transfusion: In the past, unscreened blood and blood products were a significant source of HCV transmission. However, with the implementation of thorough screening procedures, the risk of acquiring the virus through blood transfusion has been greatly reduced.
- Injecting Drug Use: Sharing injection equipment, such as needles, syringes, or other drug paraphernalia, is a high-risk behavior for HCV transmission. Intravenous drug users should prioritize using sterile equipment and seek support for harm reduction practices.
- Mother-to-Child Transmission: While relatively less common, HCV can be passed from an infected mother to her baby during childbirth. Prenatal care and appropriate medical interventions can help minimize the risk of transmission.
Additional Considerations:
- Sexual Transmission: HCV transmission through sexual practices is possible but less common. It primarily occurs when there is exposure to blood during sexual activities. Individuals with multiple sexual partners or engaging in high-risk sexual behaviors should be cautious and practice safe sex.
- Breastfeeding, Food, Water, and Casual Contact: Hepatitis C is not spread through breast milk, food, water, or casual contact such as hugging, kissing, or sharing food and drinks with an infected person. However, maintaining general hygiene practices is always recommended.
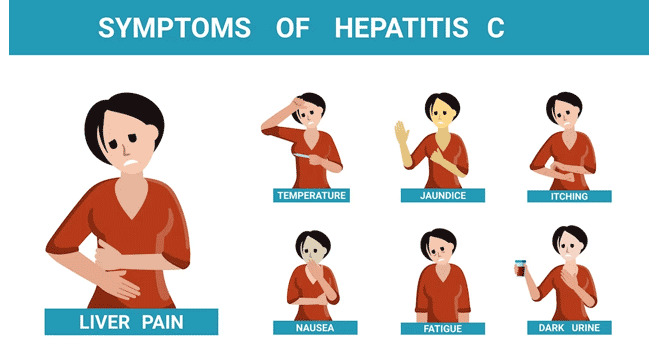
What are the symptoms of Hepatitis C?
Symptoms of Acute Hepatitis C
Symptoms of hepatitis C can vary depending on whether it is an acute or chronic infection. In many cases, individuals with acute hepatitis C may not experience any noticeable symptoms and may not even be aware of their infection. However, for those who do develop symptoms, they typically appear within 2 to 12 weeks after exposure to the virus.
- Yellow skin or eyes (jaundice)
- Loss of appetite
- Upset stomach
- Vomiting
- Abdominal pain
- Fever
- Dark urine
- Pale-colored stools
- Joint pain
- Fatigue
Symptoms of Chronic Hepatitis C
chronic hepatitis C often progresses silently without causing significant symptoms in most individuals. General symptoms such as chronic fatigue and depression may be present, but they can be easily attributed to other causes. The true extent of the infection becomes apparent when complications arise over time, such as chronic liver disease, cirrhosis (scarring of the liver), and even liver cancer.
- Chronic fatigue
- Depression
- Mild or no symptoms
- Development of chronic liver disease
- Cirrhosis (scarring of the liver)
- Liver cancer
Transmission of Hepatitis C without Symptoms
It is important to note that hepatitis C can be spread even if an infected person does not have any symptoms. This means that individuals who are unaware of their infection can unknowingly transmit the virus to others.
- Asymptomatic transmission
- Ability to spread the virus to others without symptoms
Hepatitis C Testing and Diagnosis
The Hepatitis C virus test is a combination of four types of tests that checks antibodies:
The First Stage of the HCV Testing:
In this stage, we perform a blood test to detect antibodies present in the bloodstream of the suspected patient. The test is called the HCV antibody test.
HCV Antibody Test:
This is a blood test that checks for antibodies present in the serum of the suspected individual. The test uses enzyme immunoassays (EIA) that detect antibodies for HCV. This test is done to ensure whether an individual has been exposed to the virus or not. Many of us will not show symptoms immediately after exposure to the virus. Hence, this test ensures whether you are active in the infection or not.
You will get two types of results:
- Positive: A reactive or positive antibody test means that is a potential carrier of the virus. The doctor will then recommend further tests. Sometimes, a false-positive result also comes. This happens when there is cross-reactivity with other viral antigens or the presence of immunologic disorders, such as lupus or rheumatoid arthritis.
- Negative: A non-reactive or negative HCV antibody test means you are not having HCV at present. But if think that you are exposed to the virus then you can go for a retest. Sometimes, a false-negative result comes. This happens if the test is performed during the window period after acute HCV infection but before seroconversion (when the HCV Ab converts from negative to positive).
The normal range for this assay is Not Detected.
The quantitative range of this assay is 10 – 100,000,000 IU/mL (1.0 – 8.0 log IU/mL).
A result of “Not Detected” does not rule out the presence of inhibitors in the patient specimen or hepatitis C virus RNA concentrations below the level of detection of the test. Care should be taken when interpreting any single viral load determination.
The Second Stage of the HCV Testing:
The second stage of the HCV test involves the detection of the viral genome. In this stage, we perform NAT. NAT stands for Nucleic Acid Amplification Testing and is also known as a PCR test. NAT is a highly sensitive and gold-standard method of testing the presence of viral RNA in patients whose screening test has come positive. It also reduces the window period as it is used to detect nucleic acid and not antibodies, so if there is any doubt in case of a negative screening result then this NAT test clarifies the doubt because in this test we don’t have to wait for antibodies to show its reaction.
If you are infected with the virus and the result comes positive then this test will also provide us with the amount of virus. The amount of virus present in our blood is called a viral load.
The test is performed using the PCR method and it uses two approaches:
- Qualitative test: This test is done immediately after the HCV antibody test and it tells us whether the HCV virus is present in the body or not. But, it cannot measure the viral load. To know the viral load the doctor performs a quantitative test.
- Quantitative test: This test is performed to know the exact measure of the HCV present in the blood in international units per milliliter (IU/mL). It also helps to determine whether you have a high or low viral load.
When the viral load comes down to 15 IU/mL, the amount of virus in the body is considered undetectable. In this scenario, a qualitative test is conducted to know whether you are free from the virus or if still, a small amount is present in the body.
What does the viral load range in the test tell us?
The quantitative PCR test shows the viral load range from 15 to 100,000,000 IU/mL.
If your PCR test results are:
|
Fewer than 15 IU/mL |
The virus can be detected, but the amount can’t be measured exactly. |
|
Fewer than 800,000 IU/mL |
The viral load is low. |
|
More than 800,000 IU/mL |
There is a high viral load. |
|
More than 100,000,000 IU/mL |
The virus has started infection in the body. |
Note: The quantitative PCR test does not tell how severe the infection is. To know the severity of the infection you need to go through a further test that involves a biopsy or the study of the liver tissue.
Even the qualitative test result can come positive if the viral load decreases drastically.
The Third Stage of the HCV Testing:
In this stage, the patient goes for genotype testing. As I have told you earlier in this article the hepatitis c virus has six different types of strains, so the treatment of this disease depends on the genotype. The patients need to be tested for genotype once in their lifetime because the genotype remains the same throughout infection.
Genotype testing is done by analyzing the sequences of short sections of the RNA genome which is known as restriction fragment length polymorphism (RFLP). This is followed by line probe reverse hybridization or sequence analysis. In most of the assays, they target the 5′ untranslated region (5′ UTR), as it is the most conserved region throughout the HCV genome and is most suitable for reverse transcription-polymerase chain reaction (RT-PCR) amplification.
The Fourth Stage of the HCV Testing:
This stage involves HCV Resistance Testing (RAV testing). For the treatment of this virus, doctors use DAAs (direct-acting antiviral agents) that target specific positions in the virus to stop its replication. But the virus is very intelligent. Over the years it has mutated itself and become resistant to the drug. This condition is referred to as resistance-associated variants (RAV). This scenario is seen to occur in Genotype 3 patients. Hence, it is recommended by the doctor to perform this test to ensure smooth treatment of the patient.
Why is Hepatitis C Test Done?
I will give you the best four reasons to know why you should go for an HCV test.
- You may not know that you have the infection: Sometimes, it takes months to develop the symptoms after being exposed to the virus.
- You will not spread it to other people: If you are unaware of the disease present in your body then you might spread it to a healthy person.
- The test is very quick and effective: A simple blood test is done and it gives you results within a few days. Many clinics give results within 20 to 30 minutes of the test.
- It might stop you from developing chronic infection: In the early stage of the disease, the infection is acute. But if left untreated it might develop into a chronic infection. Chronic infection can lead to liver cancer and it might prove fatal and result in death.
Prevention of Hepatitis C Infection
While there is currently no effective vaccine available for hepatitis C, preventing the transmission of the virus is crucial. By reducing the risk of exposure to the virus, particularly in high-risk populations and healthcare settings, we can significantly lower the incidence of hepatitis C infections. Here are key prevention strategies:
- Safe Healthcare Practices: Ensuring the safe and appropriate use of healthcare injections is paramount. This includes using sterile needles, syringes, and equipment for medical procedures and avoiding the reuse of needles or inadequate sterilization. Proper handling and disposal of sharps and medical waste are also essential to prevent accidental injuries and exposure.
- Harm-Reduction Services: Comprehensive harm-reduction services play a critical role in preventing hepatitis C transmission among people who inject drugs. Access to sterile needles, syringes, and drug paraphernalia, along with education on safe injection practices and support for addiction treatment, are crucial components of harm-reduction programs.
- Blood Safety: Screening donated blood for hepatitis B and C, HIV, and syphilis is essential to prevent transmission through blood transfusions. Rigorous testing protocols and quality assurance measures ensure that donated blood and blood products are safe for use.
- Training and Education: Proper training of healthcare personnel on infection control practices, including standard precautions and safe injection techniques, is vital in preventing occupational exposures and safeguarding patient and provider safety.
- Safe Sexual Practices: Preventing exposure to blood during sexual activities is important in reducing the risk of hepatitis C transmission. Safe sex practices, such as using barrier methods like condoms, can help protect against bloodborne infections. Regular testing for sexually transmitted infections (STIs) is also recommended.
By implementing these prevention strategies, we can significantly reduce the incidence of hepatitis C infections and promote overall public health. Raising awareness, providing resources, and ensuring access to comprehensive prevention services are crucial in our collective efforts to combat hepatitis C.