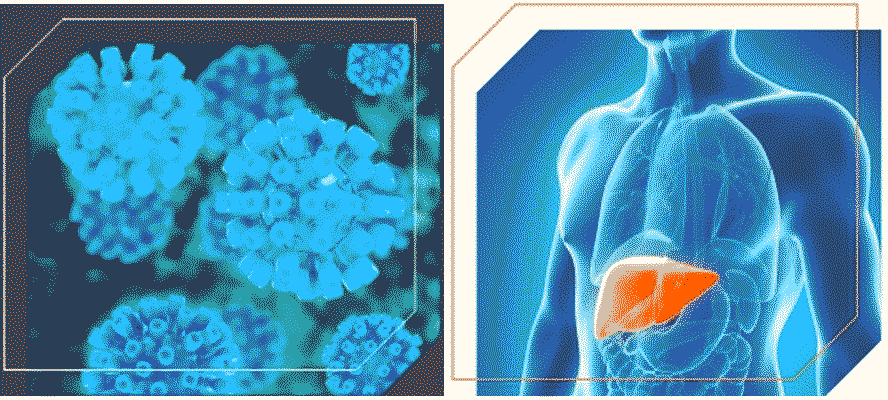
What can one say about the remarkable organ liver? That it is the largest organ in the body after the skin? That its roles are so varied as to include both digestive functions as well as immunological ones? How about the fact that the liver is the single organ in the body that has the unique ability to regenerate to a great degree and recover from injury? Despite this, liver diseases are very common in our country. Of these, some are caused due to lifestyle such as alcoholism, while some others are caused by liver infections. One such set of liver diseases are called hepatitis, which is inflammation of the liver, most typically caused by viral infection.