Every day, patients sit across from me asking for one pill that will fix their focus, erase their panic, or lift a heavy cloud of sadness. Before I reach for a prescription pad, I always ask them two things: how are you sleeping, and how much are you moving?
Table of Contents
People frequently ask me, how does physical health affect mental health in a real clinical setting? The honest answer is that treating the brain without looking at the body is a fundamental medical mistake.
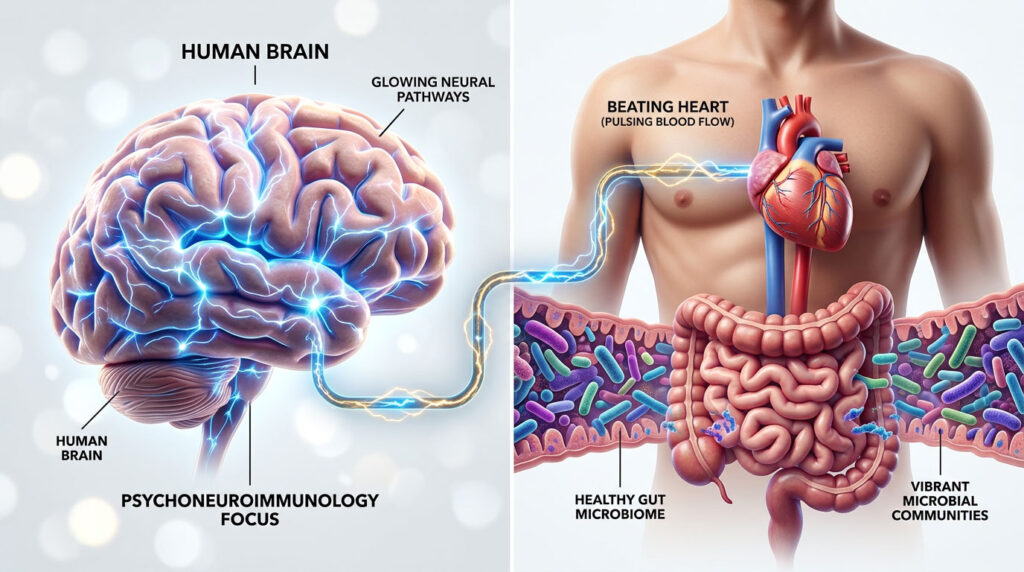
Your brain and body are not separate systems. They communicate constantly through an integrated biological circuit involving the immune system, the endocrine system, and the central nervous system. When we study this whole picture, we step into the science of psychoneuroimmunology.
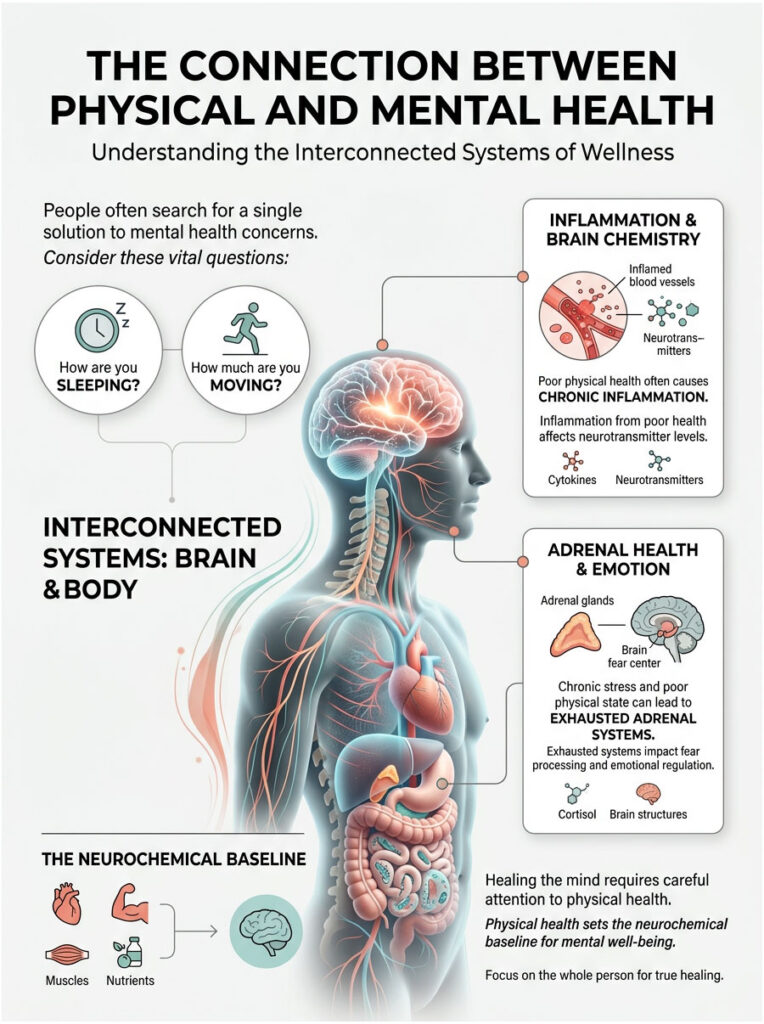
As a physician board-certified in both Internal Medicine and Psychiatry, I see this evidence every day. A spike in inflammatory cytokines from poor metabolic health directly changes neurotransmitter levels. An exhausted adrenal system reshapes how the brain processes fear. If we want to heal the mind, we need to repair the biological vessel that holds it.
Quick Answer
How does physical health affect mental health? Your physical condition sets your neurochemical baseline. Systemic inflammation, gut dysbiosis, and chronic physical stress alter brain structures and drain essential neurotransmitters like serotonin and dopamine. This biological disruption directly produces clinical symptoms of anxiety, brain fog, and severe depression.
Key Statistics on the Mind-Body Connection
- 95 percent of the body’s serotonin is produced entirely within the gastrointestinal tract. (Source: American Psychological Association, 2023)
- 150 minutes of moderate aerobic exercise per week has been shown to rival the efficacy of standard antidepressant medications. (Source: The Lancet Psychiatry, 2022)
- 30 percent higher risk of clinical depression in patients with severe metabolic syndrome. (Source: National Institutes of Health, 2021)
- 4 times the rate of severe cognitive decline in individuals with high allostatic load compared to healthy peers.
- 10 minutes of daily walking is enough to kickstart a positive dopaminergic reward loop in severely depressed patients.
- 33 percent of patients achieved full clinical remission from depression by switching to a Mediterranean diet in the SMILES trial.
The Framework of Psychoneuroimmunology
It is time to dismantle the outdated belief that psychological problems exist only in the mind. The medical community now relies on a far more accurate and integrated model. Let me break down how this works in modern medicine.
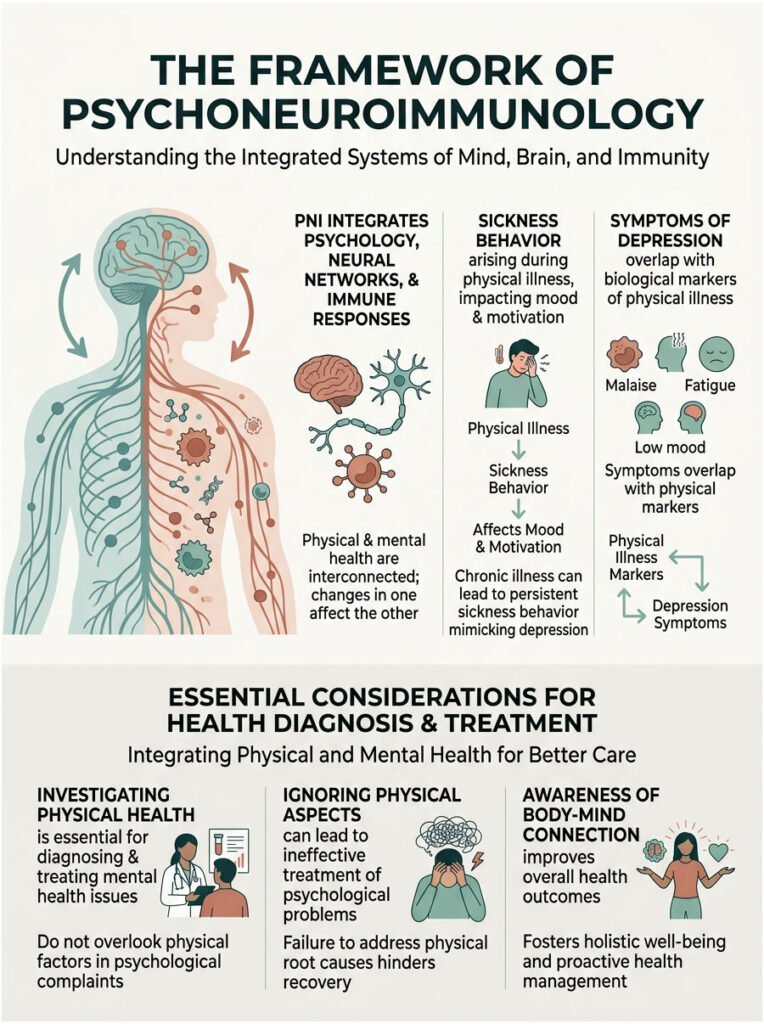
The model is called psychoneuroimmunology, the science of how your psychological states, neural networks, and immune responses are biologically intertwined. You simply cannot change one system without immediately altering the others.
When you ask a doctor how does physical health affect mental health, they should point directly to psychoneuroimmunology. This field proves that a physical infection or chronic stress creates a measurable chemical shift in your brain fluid. Your thoughts are ultimately a reflection of your underlying biology.
What Psychoneuroimmunology Means for You
The term sounds complex, but the core idea is actually very logical. Think of your body as a massive, interconnected communication grid. Your white blood cells talk to your vagus nerve. Your vagus nerve relays those messages straight to your brainstem.
When you experience a physical injury, the immune system sends aggressive alarm signals. Those chemical signals travel rapidly to the brain, which then shifts your mood to force you to rest and recover. That is psychoneuroimmunology in action.
Based on what we see in modern clinical trials, ignoring this connection leads to widespread treatment failure. You cannot out-medicate a biological system that is actively on fire. The physical flames have to be put out first.
The Sickness Behavior Phenomenon
Think about the last time you had a severe flu. You probably felt withdrawn, unmotivated, exhausted, and completely unable to enjoy anything. That emotional shift was not just in your head.
This reaction is medically known as sickness behavior. When you are physically ill, your body needs to conserve massive amounts of energy to fight infection. To do this, your immune system intentionally lowers mood and motivation.
This evolutionary survival mechanism mimics the exact clinical symptoms of major depressive disorder. Chronic physical illness traps the brain in a permanent state of sickness behavior. This is a primary reason why chronically ill patients struggle so deeply with mental health.
Where Sickness Behavior Overlaps with Depression
The diagnostic criteria for depression include fatigue, appetite changes, sleep disruption, and loss of interest. These are the exact same biological markers of systemic physical illness. In a clinical setting, the overlap is impossible to ignore.
When a patient comes to me with these symptoms, I do not just explore their childhood trauma. I look extensively at their bloodwork, checking for hidden infections, thyroid disorders, and autoimmune flare-ups.
If we ignore the physical triggers of sickness behavior, we miss the root cause of the depression entirely. Treating the mind requires a full investigation of the body.
Consider this: how many times have you felt anxious or down, only to realize later you were dehydrated or coming down with something? Your brain was interpreting physical distress as emotional pain.
The Inflammatory Link: How Systemic Health Controls Your Mood
Inflammation is the medical buzzword of the decade. But what does it actually mean for your daily mood and cognitive function? The answer lies in how the immune system interacts with your protective brain barrier.
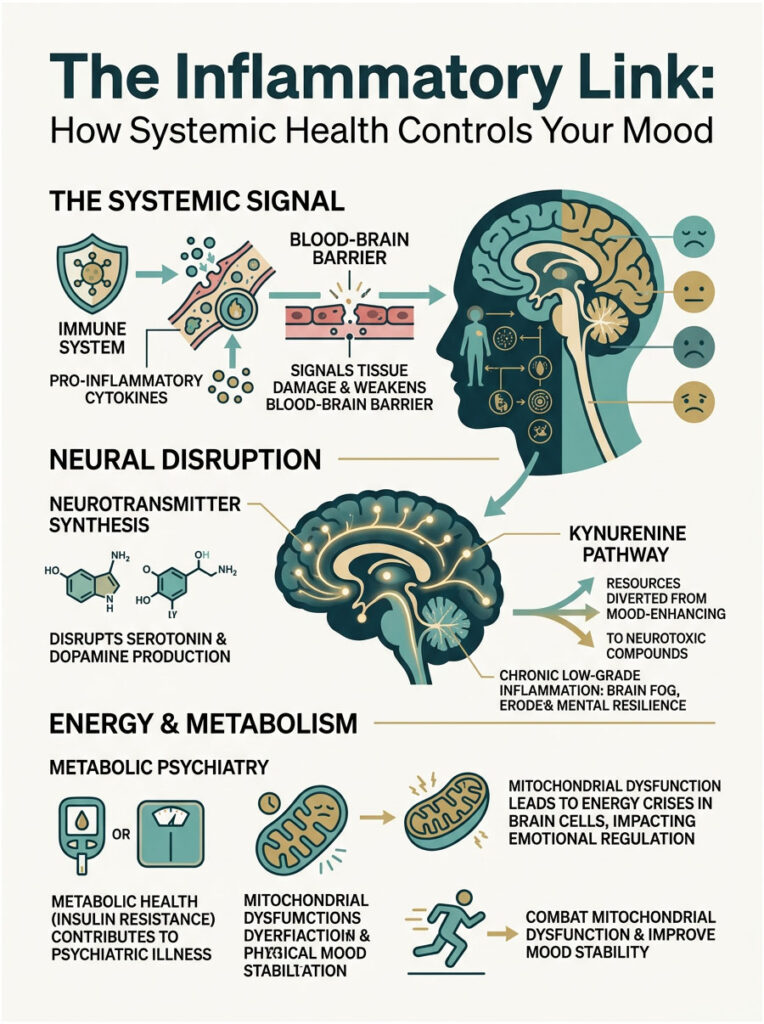
Systemic health controls mood because the brain is highly sensitive to inflammatory markers floating in the bloodstream. Poor physical health creates a constant, low-grade inflammatory response that slowly erodes mental resilience.
Cytokines and the Blood-Brain Barrier
When your body is physically stressed by a poor diet, lack of sleep, or a sedentary lifestyle, it produces pro-inflammatory cytokines. These chemical messengers signal tissue damage throughout the body, acting like biological fire alarms.
Under normal conditions, the blood-brain barrier protects sensitive neural tissue from toxins. But chronic systemic inflammation physically weakens this barrier. The pro-inflammatory cytokines cross over and enter the brain.
Once inside, they disrupt neural function by slowing down the speed at which neurons fire. This sluggish neural transmission produces what patients commonly describe as brain fog.
Expert Insight: In my practice, routine blood panels checking C-Reactive Protein (CRP) and fasting insulin are mandatory during comprehensive psychiatric evaluations. High CRP indicates systemic inflammation and correlates directly with treatment-resistant mood disorders.
Neuroinflammation and Depression: The Kynurenine Pathway
The link between neuroinflammation and depression is now undeniable in modern psychiatry. When cytokines enter the brain, they disrupt the biochemical synthesis of neurotransmitters.
Specifically, systemic inflammation diverts the precursor amino acids needed to make serotonin and dopamine. Instead of producing the chemicals that keep you feeling well, the brain uses those same building blocks to create neurotoxic compounds. This process is known as the kynurenine pathway.
This is why neuroinflammation and depression go hand in hand. Your own immune system is depleting your natural antidepressants, cannibalizing your capacity for happiness to fight a perceived physical threat.
We see this constantly in patients with untreated autoimmune diseases like lupus or rheumatoid arthritis. Their rates of severe depression are astronomically high, driven by this exact inflammatory mechanism, not just the emotional stress of being sick.
The Rise of Metabolic Psychiatry
These discoveries have sparked an entirely new medical specialty over the last five years: metabolic psychiatry. This field focuses on how metabolic health problems like insulin resistance cause severe psychiatric illness.
Metabolic psychiatry views the brain as a highly energy-demanding organ. If the body cannot process glucose correctly due to a poor diet, the brain starves for energy. This cellular energy crisis directly causes cognitive fog and severe mood instability.
By treating underlying insulin resistance through diet and physical movement, metabolic psychiatry achieves results that traditional antidepressant medications often cannot match.
Mitochondrial Dysfunction and Mood
At the cellular level, this energy crisis is known as mitochondrial dysfunction. Mitochondria are the microscopic powerhouses of your cells. When they fail, brain cells simply cannot operate efficiently.
There is a direct, measurable link between mitochondrial dysfunction and bipolar disorder, schizophrenia, and major depression. When brain cells lack energy, they cannot regulate emotions or handle daily stress, leaving the patient perpetually overwhelmed and exhausted.
To address mitochondrial dysfunction and mood issues, we prescribe physical interventions. Specific exercise protocols and nutritional changes force the body to build new mitochondria through a process called mitochondrial biogenesis.
The Gut-Brain Axis: Your Second Brain
If you truly want to know how does physical health affect mental health, look inside your digestive tract. Your gut is literally your second brain, and it shapes your emotional baseline more than most people realize.
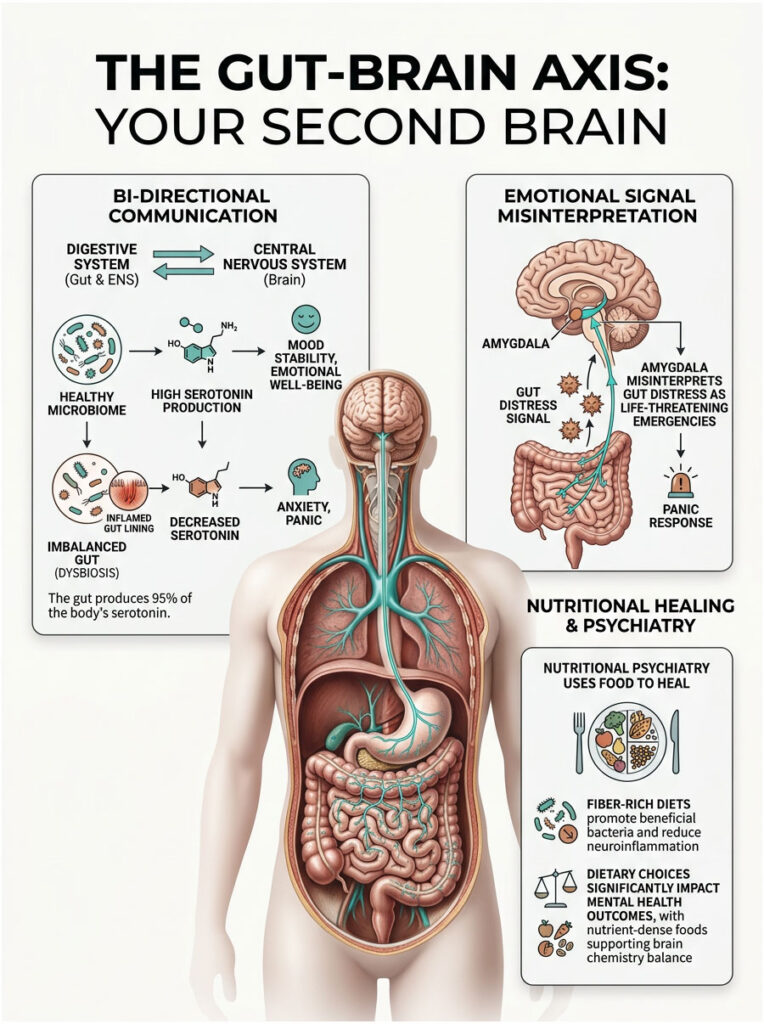
The medical term for this connection is the microbiome-gut-brain axis. It is a massive, bidirectional communication network between your gastrointestinal system and your central nervous system. They exchange messages every single second.
What you put into your stomach directly shapes the chemical environment of your mind. You are not just feeding yourself. You are feeding trillions of microscopic organisms that influence your mood.
The Enteric Nervous System
Your gut has its own independent nervous system called the enteric nervous system. It contains hundreds of millions of neurons, actually more than your entire spinal cord.
Here is the most fascinating part: the gastrointestinal tract produces roughly 95 percent of the body’s total serotonin. Serotonin is the primary neurotransmitter responsible for feelings of well-being, confidence, and emotional stability.
If your gut lining is inflamed or damaged, serotonin production plummets immediately. This is psychoneuroimmunology at work. A stomach ache is never just a stomach ache. It is a neurological event.
Dysbiosis and the Amygdala
Inside your gut live trillions of bacteria, fungi, and viruses. This complex ecosystem is your microbiome. When you eat poorly or take too many antibiotics, you kill off good bacteria and allow harmful bacteria to overgrow.
This bacterial imbalance is called dysbiosis. A compromised microbiome sends distress signals up to the brain, traveling through the gut-brain axis directly to the amygdala, the fear and panic center.
This means bad gut bacteria can physically trigger a spontaneous panic attack. The brain interprets localized gut inflammation as a life-threatening emergency. You feel anxious, but the root cause is entirely in your intestines.
Nutritional Psychiatry in Practice
Food is now used as a targeted psychiatric intervention. Nutritional psychiatry focuses on healing the gut-brain axis to address mood disorders, essentially treating the kitchen as a pharmacy.
We focus heavily on short-chain fatty acids like butyrate. When you eat dietary fiber, good bacteria ferment it into butyrate, which strengthens the gut lining and reduces systemic inflammation.
Without enough fiber, those good bacteria start eating the protective mucus lining of your stomach. This leads to leaky gut syndrome, flooding the bloodstream with toxins and triggering massive neuroinflammation.
Dietary Impact on the Gut-Brain Axis
| Dietary Pattern | Gut Impact | Effect on Brain Chemistry | Mental Health Outcome |
| Ultra-Processed / High Sugar | Induces severe gut dysbiosis and increases intestinal permeability (leaky gut). | Spikes pro-inflammatory cytokines; depletes serotonin precursors. | High risk for severe anxiety, brain fog, and treatment-resistant depression. |
| Mediterranean-Style Diet | Promotes microbial diversity and strengthens the gut lining. | Increases short-chain fatty acids; boosts BDNF levels. | Strongly associated with clinical remission of mild to moderate depressive episodes. |
| High-Fiber / Prebiotic Focus | Feeds beneficial bifidobacteria and lactobacilli strains. | Lowers systemic cortisol and normalizes the HPA axis. | Improved emotional regulation and significantly enhanced stress resilience. |
The clinical takeaway is clear. We cannot expect patients to feel mentally well if they consume a diet that actively destroys their neurochemistry. Food is biological information.
Every meal is a chance to either fight inflammation or fuel it. Choosing nutrient-dense, fiber-rich foods actively repairs the blood-brain barrier and gives the body the raw materials it needs to produce the chemicals behind focus and well-being.
Neuroplasticity and the Science of Exercise
When patients ask how does physical health affect mental health, they usually assume I will talk about a runner’s high. They picture exercise as a quick burst of good feelings, a temporary distraction from their problems.

That is a major misconception. Exercise is not about temporary symptom relief. It is about fundamentally rewiring the physical structure and volume of your brain.
This biological process is called neuroplasticity: your brain’s ability to grow new neural pathways, heal damaged circuits, and adapt to stress. Exercise is the strongest trigger for neuroplasticity that we currently have.
Beyond Endorphins: What Really Happens
Endorphins are useful, but they only last a few hours. The real benefits of exercise happen long after you leave the gym.
Physical movement triggers a cascade of genetic expressions inside brain cells. Your muscles act as an endocrine organ, releasing chemicals called myokines into the bloodstream.
These myokines travel to the brain and protect it from aging, stress, and toxic buildup. This is why daily, intentional movement is a non-negotiable prescription in my psychiatric clinic. You are literally medicating your brain with your muscles.
Brain-Derived Neurotrophic Factor (BDNF)
Let me introduce you to the most important chemical you have probably never heard of: Brain-Derived Neurotrophic Factor, or BDNF. Think of it as biological fertilizer for your brain.
When you exercise, your muscles release proteins that travel to the brain and trigger massive BDNF production. This chemical promotes intense, rapid neuroplasticity.
BDNF physically repairs neural pathways damaged by chronic stress, trauma, and inflammation. Low BDNF levels are found universally in patients with severe depression, anxiety, and Alzheimer’s disease. High BDNF creates a brain that is resilient, adaptable, and emotionally stable.
Cardiovascular Fitness and the Prefrontal Cortex
Aerobic exercise does something highly specific to brain anatomy. It dramatically increases blood volume and oxygen delivery to neural tissues through a process called angiogenesis, which means building new blood vessels.
This extra blood flow targets and strengthens the prefrontal cortex, the logical, decision-making center of the brain. When the prefrontal cortex is strong, it can quiet the emotional, reactive amygdala. You gain logical decision-making over emotional reactivity.
Recent meta-analyses from The Lancet Psychiatry confirm that just 150 minutes of moderate aerobic activity per week rivals the efficacy of certain SSRI medications. This is powerful proof of how physical health shapes mental well-being.
Exercise Types and Their Neurochemical Benefits
| Exercise Type | Physiological Target | Key Neurochemical | Psychological Benefit |
| Moderate Aerobic (Zone 2) | Cardiovascular system and mitochondrial efficiency | BDNF and Endocannabinoids | Long-term neuroplasticity and reduced baseline anxiety |
| HIIT | Metabolic conditioning and lactic acid threshold | Dopamine, Norepinephrine, and Lactate | Improved focus, motivation, and executive function |
| Resistance Training | Central nervous system and musculoskeletal system | IGF-1 and Testosterone | Better self-efficacy, sleep architecture, and reduced depressive symptoms |
| Yoga / Tai Chi | Autonomic nervous system and vagal tone | GABA | Downregulation of fight-or-flight response and trauma processing |
Different forms of physical stress produce entirely different psychiatric benefits. A well-rounded physical routine is essentially a broad-spectrum psychiatric treatment that hits multiple neurochemical pathways at once.
For a patient with severe ADHD, I prescribe HIIT for the dopamine spike. For someone dealing with trauma and anxiety, we start with yoga to boost GABA. The physical movement is tailored to the specific mental health deficit.
The HPA Axis and Cortisol: Your Stress Response System
Stress is not just a fleeting feeling. It is a systemic biological event. To understand this fully, we need to look at the body’s primary alarm system.
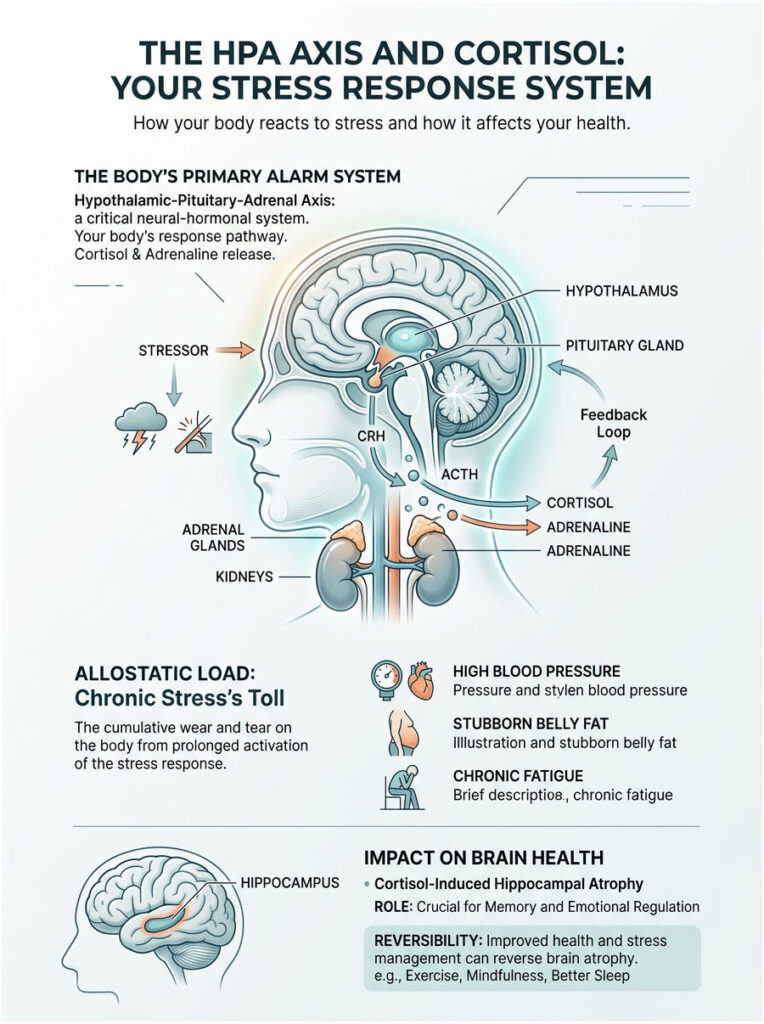
This system handles everything from a difficult email to a car accident. It mobilizes your energy resources for survival. But when it breaks down due to poor physical health, it severely damages the brain. Chronic stress is neurotoxic.
How the Stress Response Works
Your alarm system is called the Hypothalamic-Pituitary-Adrenal axis, or HPA axis. When you perceive a threat, the hypothalamus signals the pituitary gland, which tells the adrenal glands to release cortisol and adrenaline.
Here is the critical point: physical stressors trigger the exact same biological alarm as psychological stressors. Your brain cannot distinguish between a toxic relationship and a diet loaded with processed foods.
If you are constantly physically unhealthy, your HPA axis never shuts off. You get trapped in a permanent state of fight-or-flight. That constant cortisol drip slowly poisons the nervous system.
Understanding Allostatic Load
When the HPA axis fires nonstop, it creates a massive burden on the body. In clinical medicine, we call this accumulated burden allostatic load, the physiological wear and tear of modern life.
Patients with high allostatic load present with high blood pressure, stubborn belly fat, and severe chronic fatigue. Their system is entirely burned out from the inside.
Lowering allostatic load through physical interventions like better sleep and proper nutrition is mandatory. It is the only way to restore mental peace. You cannot talk your way out of a high allostatic load in a therapist’s chair alone.
Cortisol-Induced Hippocampal Atrophy
What actually happens to the brain when it is constantly flooded with stress hormones? The physical results are destructive. High cortisol literally erodes brain tissue over time.
Prolonged cortisol exposure physically shrinks the hippocampus, a condition known as cortisol-induced hippocampal atrophy. It is visible on an MRI scan.
The hippocampus is responsible for memory formation and emotional regulation. When it shrinks, you lose the ability to remember details clearly and to calm yourself down. This condition is a hallmark of chronic depression and severe PTSD.
The encouraging news: this process is reversible. By improving physical health and lowering cortisol levels, the hippocampus can physically regrow.
The Vagus Nerve: Your Built-In Anxiety Reset Button
When my patients are trapped in high anxiety, I do not just focus on their conscious thoughts. I teach them how to manually control their nervous system using their physical body. This is a vital clinical skill.
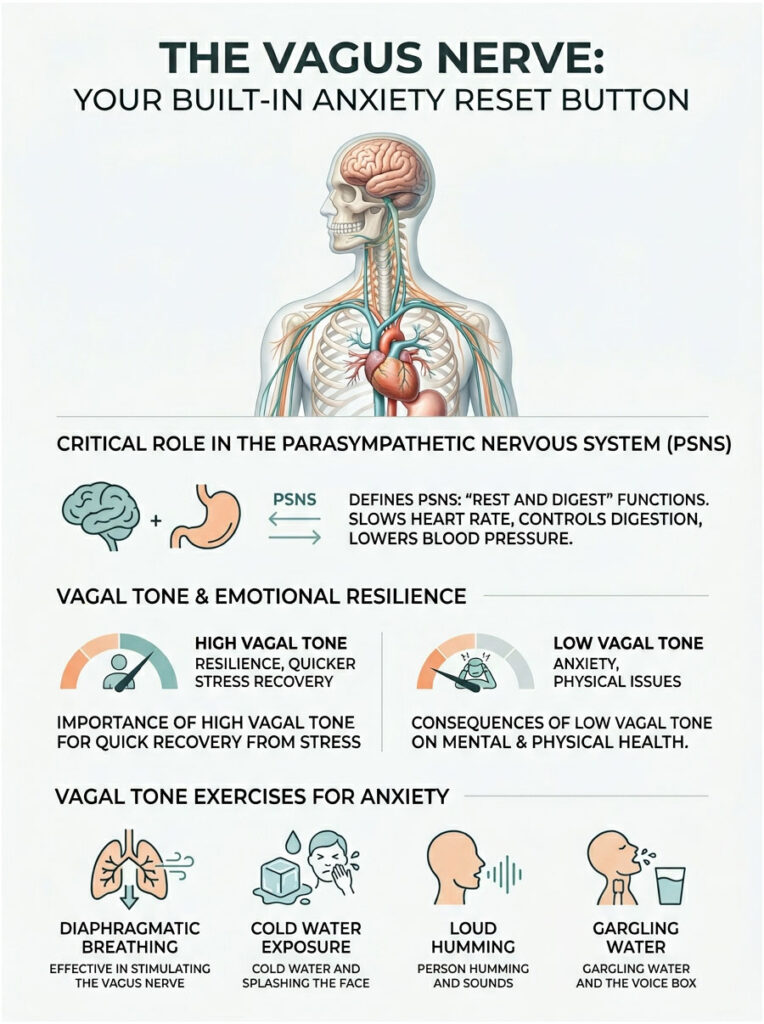
This is where the practical power of psychoneuroimmunology truly shines. We can use specific physical nerves to force the brain to calm down, bypassing the logical mind entirely.
The Parasympathetic Superhighway
The vagus nerve connects your brainstem to the heart, lungs, and digestive tract. It acts as a massive biological superhighway for emotional data.
It is the primary controller of the parasympathetic nervous system, the rest-and-digest system, which is the biological opposite of fight-or-flight.
When you physically stimulate the vagus nerve, it releases acetylcholine. This chemical forces the heart rate to slow, drops blood pressure, and tells the brain that you are safe.
Vagal Tone and Emotional Resilience
In clinical medicine, we measure the health of this nerve through vagal tone. High vagal tone means the body can quickly relax after a stressful event, acting as a built-in biological shock absorber.
People with high vagal tone recover from emotional distress much faster. They do not hold onto anger or panic for hours.
Low vagal tone is consistently linked to chronic anxiety, heart disease, and digestive disorders like IBS. If you want to understand how does physical health affect mental health, look at the measurable strength of your vagus nerve.
Vagal Tone Exercises for Anxiety
You can strengthen this nerve like a muscle. I frequently prescribe vagal tone exercises for anxiety to my patients. These are physical actions that directly stimulate the nerve fibers.
Deep, slow diaphragmatic breathing is the most effective method. When you exhale longer than you inhale, you physically massage the vagus nerve against the diaphragm, sending an immediate calming signal to the brainstem.
Other vagal tone exercises for anxiety include cold water exposure to the face, loud humming, and gargling water. These physical habits directly override the brain’s panic signals and force the body into parasympathetic dominance.
Practicing these exercises daily builds permanent physical resilience against psychological stress. You train the nervous system to default to calm instead of panic.
Sleep Hygiene and Brain Restoration
Sleep is not a luxury or a sign of laziness. It is a highly active, non-negotiable biological process. Without adequate sleep, the brain literally drowns in its own toxic waste.
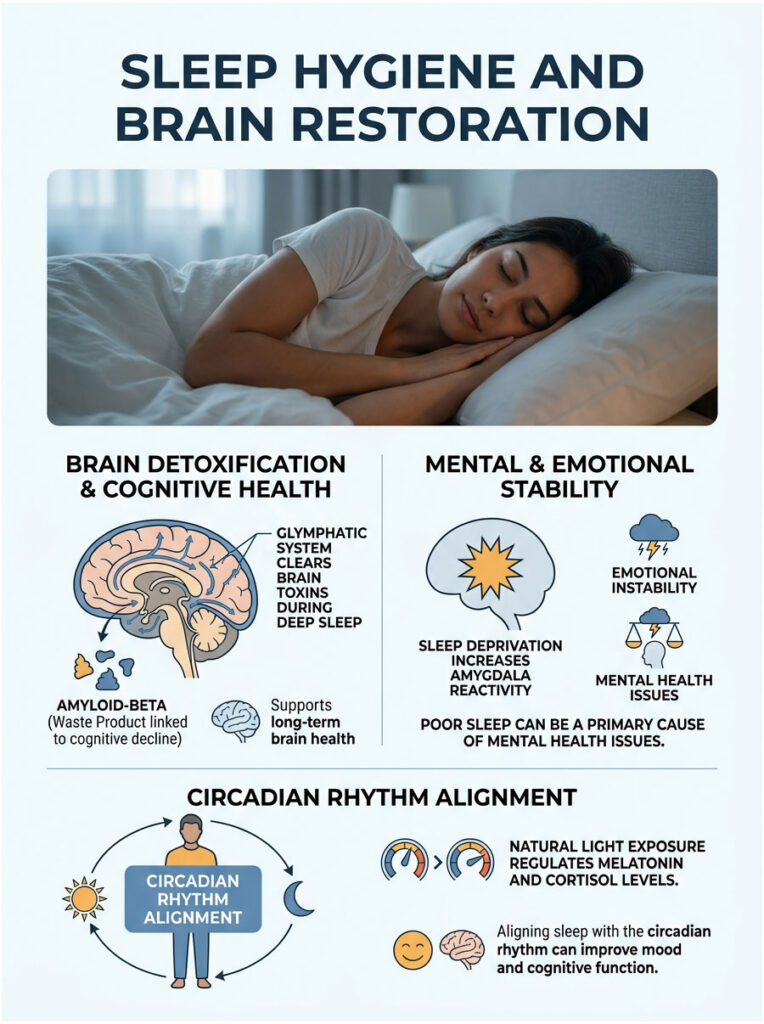
Every psychiatric evaluation must include a deep look at sleep architecture. Poor sleep is rarely just a symptom of mental illness. It is very often the primary biological cause.
The Glymphatic System
Throughout the day, brain cells produce metabolic byproducts as they consume energy. One of these waste proteins is amyloid-beta.
During deep sleep, the brain activates its overnight waste clearance system, the glymphatic system. Brain cells physically shrink by up to 60 percent, allowing cerebrospinal fluid to rush in and wash away toxic buildup.
Without enough deep sleep, these toxins accumulate rapidly, causing brain fog, memory loss, and massive mood instability. Over decades, this buildup contributes directly to Alzheimer’s disease.
Sleep Deprivation and Amygdala Hijack
The clinical reality of acute sleep loss is alarming. Just one night of poor sleep severs the neural connection between the logical prefrontal cortex and the emotional amygdala.
Without the prefrontal cortex keeping it in check, the amygdala becomes up to 60 percent more reactive. Everything starts to feel like a life-threatening emergency.
This is why you are so irritable, emotional, and anxious after a bad night of sleep. The brain has physically lost its emotional braking system. You are operating on primal fear and reactivity.
Circadian Rhythm Alignment
To fix sleep, you have to fix your biological clock first. Your circadian rhythm is controlled by light exposure entering the eyes.
Viewing natural morning sunlight regulates melatonin production for the upcoming evening and provides an immediate healthy cortisol spike to wake you up. It sets a roughly 14-hour timer for sleep onset.
Aligning physical habits with the natural light cycle stabilizes daily mood fluctuations. It is a simple, free, and highly effective intervention. Proper light exposure is just as important as proper nutrition.
Practical Strategies: Clinical Protocols That Change Brain Chemistry
Understanding the science is only the first step. The real value comes from applying these principles daily. Knowledge without action is useless in medicine.

When patients ask how does physical health affect mental health, I give them specific, measurable protocols. We do not guess. We implement strict, evidence-based physical habits.
Micro-Movements for Dopamine
For severely depressed patients, the idea of going to a gym feels impossible. Their allostatic load is simply too high. So we start with tiny micro-movements to build momentum.
I recommend a simple 10-minute walk outside in the morning. This small physical action is enough to kickstart a dopaminergic reward loop in the brain and prove that action is possible.
Over time, those 10 minutes compound. They slowly raise baseline levels of Brain-Derived Neurotrophic Factor and prepare the patient for harder workouts.
Daily Vagal Tone Exercises for Anxiety Relief
When a severe panic attack strikes, logic fails completely. You need a physical intervention to stop the spiral. I teach patients the 4-7-8 breathing protocol for immediate relief.
Inhale quietly through the nose for 4 seconds. Hold for 7 seconds. Exhale completely through the mouth for 8 seconds. This ratio is one of the most powerful vagal tone exercises for anxiety available.
It forces the heart rate down manually and switches the nervous system from sympathetic panic to parasympathetic calm in under two minutes. I recommend doing this four times a day as preventative medicine.
Anti-Inflammatory Nutrition Steps
To combat neuroinflammation and depression, we must change the fuel source. I advise patients to increase their intake of Omega-3 fatty acids, specifically EPA and DHA.
Omega-3s found in wild-caught salmon and walnuts physically cross the blood-brain barrier. Once inside, they suppress inflammatory cytokines and act as brain armor against systemic stress.
Incorporating polyphenol-rich foods like dark berries and extra virgin olive oil is also essential. These foods feed good bacteria in the gut-brain axis, stabilizing serotonin production and preventing leaky gut.
Tracking the Cortisol Awakening Response
I also teach patients to monitor their morning energy levels carefully. This biological marker, the cortisol awakening response, reveals how well the adrenal glands are functioning.
If you wake up exhausted despite sleeping 8 hours, your HPA axis is likely dysregulated. The body is failing to produce the necessary morning cortisol spike.
By tracking this daily, we can adjust exercise timing and nutritional intake to slowly rebuild natural energy curves over several months. Healing the HPA axis requires patience and physical consistency.
Case Studies and Clinical Evidence
Modern medicine demands proof. The concepts of psychoneuroimmunology and metabolic psychiatry are backed by rigorous, peer-reviewed data and double-blind clinical trials, not just wellness theories.

Real-world case studies help us see exactly how does physical health affect mental health in measurable terms. These results are reshaping the standard of psychiatric care worldwide.
The SMILES Trial
The SMILES trial is arguably the most important study in modern nutritional psychiatry. Led by Professor Felice Jacka, researchers enrolled adults with moderate to severe clinical depression.
Instead of adjusting psychiatric medication or adding therapy, they assigned participants to a clinical dietician. Patients followed a modified Mediterranean diet rich in whole grains, lean proteins, and healthy fats.
The results were remarkable. Over 33 percent of the dietary group achieved full clinical remission of their depression. Their physical diet healed the gut-brain axis, which in turn resolved the psychological illness.
Post-Viral Fatigue and Mental Health
The negative side of this connection is visible in post-viral syndromes. When a patient recovers from a severe viral infection like Epstein-Barr or COVID, the immune system is often left completely depleted.
This immune exhaustion leads directly to severe cognitive deficits and deep, persistent depression. The body is trapped in prolonged sickness behavior for months, with the brain starved of energy and flooded with lingering cytokines.
By treating the physical immune system through targeted rest, hydration, and anti-inflammatory protocols, mental health symptoms gradually resolve. This is psychoneuroimmunology in practice: healing the mind by restoring the body.
Key Takeaways: Healing the Mind by Healing the Body
The separation of mind and body is a dangerous medical myth. Physical health is the absolute biological prerequisite for psychological healing. You cannot out-think a poor diet, a sedentary lifestyle, or chronic sleep deprivation.

How does physical health affect mental health? It dictates everything. Your daily physical habits control the gut-brain axis, manage allostatic load, and determine your levels of Brain-Derived Neurotrophic Factor. By reducing systemic inflammation, you actively protect the brain from neuroinflammation and clinical depression.
As a physician, my message is empowering. You have immense daily control over your brain chemistry. View your physical habits as active, potent mental health treatments. Fix the biological vessel, and the mind will naturally follow.
Frequently Asked Questions
How does physical health affect mental health from a clinical perspective?
In clinical practice, we view the brain and body as an integrated biological circuit rather than separate entities. Your physical state dictates your neurochemical baseline; for example, systemic inflammation and metabolic dysfunction can cross the blood-brain barrier, altering neurotransmitter synthesis and directly causing symptoms of anxiety, brain fog, and clinical depression.
What is psychoneuroimmunology and why is it significant for mood disorders?
Psychoneuroimmunology is the exact science of how your psychological states, neural networks, and immune responses are biologically intertwined. It is significant because it proves that physical triggers, such as chronic inflammation or infection, create measurable chemical changes in brain fluid, often manifesting as ‘sickness behavior’ which mimics the diagnostic criteria for major depressive disorder.
How does the microbiome-gut-brain axis influence emotional stability?
The gut is often referred to as the ‘second brain’ because the gastrointestinal tract produces approximately 95 percent of the body’s serotonin. Through the microbiome-gut-brain axis, gut dysbiosis (bacterial imbalance) sends distress signals via the vagus nerve to the amygdala, which can physically trigger spontaneous panic attacks and emotional instability.
What role does Brain-Derived Neurotrophic Factor (BDNF) play in mental health?
BDNF acts as a biological fertilizer for the brain, promoting neuroplasticity—the ability to grow new neural pathways and heal damaged circuits. Low levels of BDNF are consistently found in patients with depression and Alzheimer’s, while physical exercise is the most potent way to trigger its production and repair the brain’s physical structure.
Can systemic inflammation lead to treatment-resistant depression?
Yes. Chronic systemic inflammation releases pro-inflammatory cytokines that disrupt the kynurenine pathway. Instead of using amino acids to synthesize serotonin and dopamine, the brain is forced to create neurotoxic chemicals. This biological ‘theft’ of happiness-inducing neurotransmitters is a primary cause of treatment-resistant mood disorders.
How does metabolic psychiatry address cognitive fog and mood instability?
Metabolic psychiatry focuses on how insulin resistance and mitochondrial dysfunction cause a cellular energy crisis in the brain. When brain cells cannot process glucose efficiently, they lack the energy to regulate emotions or handle stress, leading to cognitive fog. Treating the underlying metabolic health often resolves psychiatric symptoms that medication alone cannot reach.
What is the impact of chronic cortisol exposure on brain anatomy?
Prolonged exposure to high cortisol levels due to a hyperactive HPA (Hypothalamic-Pituitary-Adrenal) axis is neurotoxic. It can lead to cortisol-induced hippocampal atrophy, which is the physical shrinking of the brain region responsible for memory and emotional regulation, a hallmark sign of chronic PTSD and depression.
How can vagal tone exercises for anxiety provide immediate relief?
Vagal tone exercises, such as the 4-7-8 breathing protocol or cold water exposure, manually stimulate the vagus nerve to release acetylcholine. This chemical forces the heart rate to slow down and shifts the autonomic nervous system from a sympathetic ‘fight-or-flight’ state to a parasympathetic ‘rest-and-digest’ state, bypassing the logical mind to calm the brainstem.
Why is the glymphatic system critical for preventing ‘amygdala hijack’?
The glymphatic system is the brain’s waste clearance mechanism that operates during deep sleep to wash away neurotoxic byproducts like amyloid-beta. Without this ‘neuro-restoration,’ toxic buildup severs the connection between the logical prefrontal cortex and the reactive amygdala, leading to an ‘amygdala hijack’ where emotional responses become 60 percent more intense.
What did the SMILES trial reveal about nutritional psychiatry?
The SMILES trial provided landmark evidence that dietary intervention can be a primary treatment for mental illness. It demonstrated that 33 percent of patients with moderate to severe depression achieved full clinical remission simply by switching to a Mediterranean-style diet, which reduces neuroinflammation and strengthens the gut-brain axis.
How does ‘allostatic load’ explain the physical sensation of burnout?
Allostatic load is the physiological wear and tear that accumulates when the body is in a state of constant survival mode. High allostatic load results in a ‘burned out’ system where the HPA axis is dysregulated, leading to high blood pressure, chronic fatigue, and a depleted ability to handle even minor psychological stressors.
Which exercise modalities are most effective for specific neurochemical deficits?
In clinical protocols, we tailor movement to the deficit: HIIT (High-Intensity Interval Training) is prescribed for ADHD to spike dopamine and norepinephrine; moderate aerobic exercise is used for depression to boost BDNF; and Yoga or Resistance Training is used for anxiety to increase GABA levels and improve sleep architecture.
Disclaimer
This article is for informational purposes only and does not constitute medical advice. The biological links between physical and mental health discussed—including psychoneuroimmunology and metabolic psychiatry—are complex clinical fields. Always consult a qualified healthcare professional or psychiatrist before making changes to your medication, diet, or exercise routine, especially if you have underlying health conditions.
References
- American Psychological Association (2023) – “That gut feeling” – Explaining the 95% serotonin production within the gastrointestinal tract and the enteric nervous system.
- The Lancet Psychiatry (2022) – “Exercise as a primary treatment for depression” – Meta-analysis comparing 150 minutes of aerobic exercise to standard antidepressant efficacy.
- National Institutes of Health (2021) – “Metabolic Syndrome and Depressive Symptoms” – Statistical data regarding the 30% increased risk of depression in patients with metabolic dysfunction.
- BMC Medicine (SMILES Trial) – “A randomised controlled trial of dietary improvement for adults with major depression” – Clinical data showing 33% remission rates through Mediterranean diet intervention.
- Harvard Medical School – “Understanding the Stress Response” – Detailed breakdown of the HPA axis, cortisol, and the physiological impact of chronic stress on the hippocampus.
- Frontiers in Immunology – “Psychoneuroimmunology: Mechanisms and Clinical Implications” – Peer-reviewed overview of how cytokines cross the blood-brain barrier to affect mood.