Here is something that surprises most of my patients: the burning, bloated feeling they have been blaming on too much stomach acid is often caused by too little of it. After years of working in clinical gastrointestinal practice, I can tell you this is one of the most common misdiagnoses I encounter.
Table of Contents
Learning how to increase stomach acid naturally is the real starting point for resolving chronic digestive problems. When your stomach does not produce enough hydrochloric acid, everything downstream suffers. Nutrient absorption drops, your gut microbiome shifts out of balance, and symptoms like reflux, bloating, and indigestion become a daily reality.
The widespread overuse of acid-suppressing medications only deepens the problem. These drugs shut down the entire digestive cascade, leaving the body vulnerable to infections and severe nutrient deficiencies. If you want to genuinely heal your gut, the focus needs to shift from suppressing symptoms to restoring normal stomach function using a strategic, evidence-based approach.
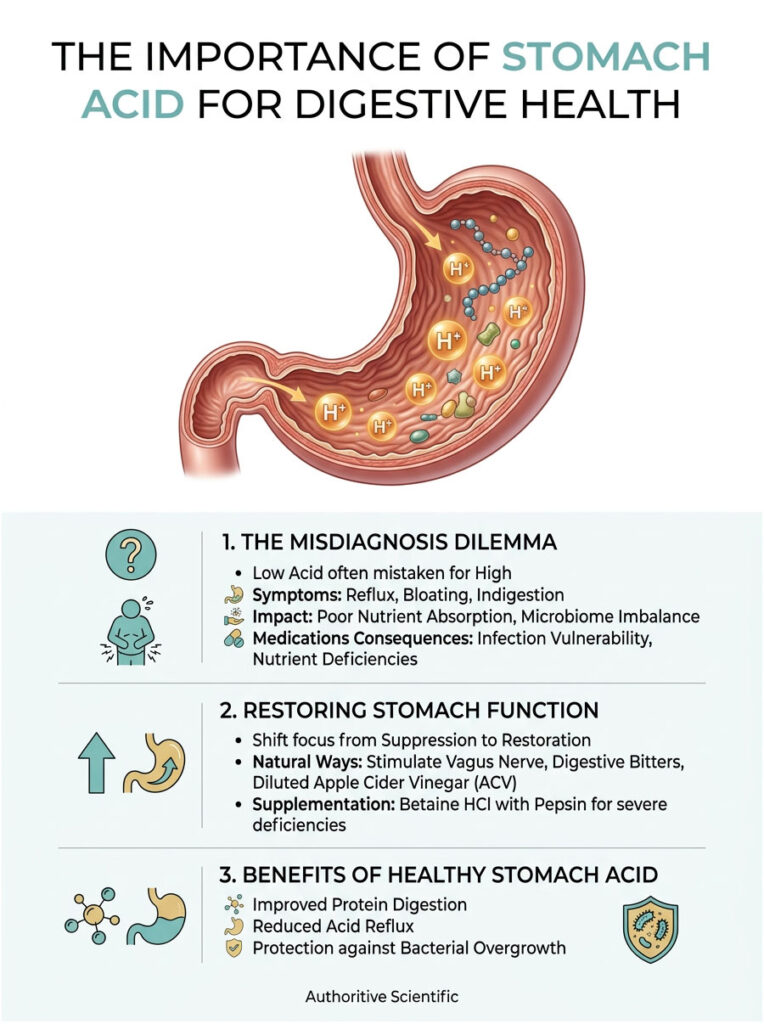
| Quick Answer: You can increase stomach acid naturally by stimulating the vagus nerve, using digestive bitters, or drinking diluted Apple Cider Vinegar before meals. For more severe deficiencies, supplementing with Betaine HCl with Pepsin can safely restore optimal gastric pH. This targeted approach improves protein digestion, helps prevent acid reflux, and protects against bacterial overgrowth. |
Key Statistics on Gastric Health
Daily acid production: According to the National Institutes of Health (NIH, 2022), a healthy adult secretes approximately 1.5 liters of gastric acid every day.
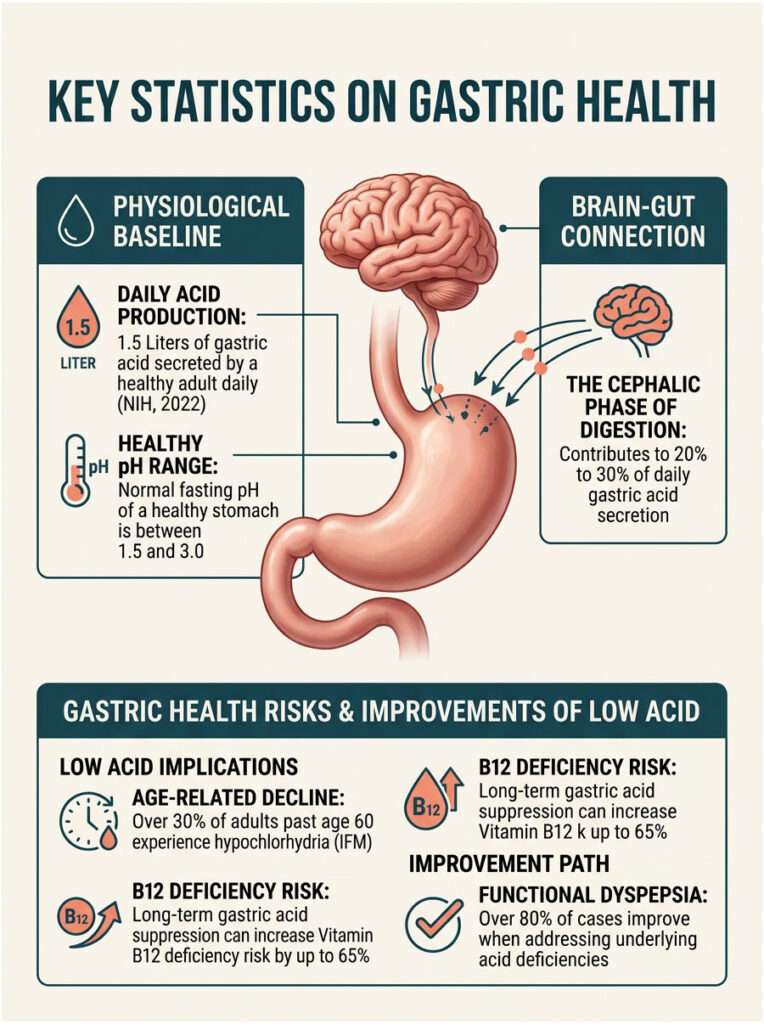
Age-related decline: Research from the Institute for Functional Medicine shows that over 30% of adults past age 60 suffer from hypochlorhydria (low stomach acid).
Healthy pH range: The normal fasting pH of a healthy stomach falls between 1.5 and 3.0.
B12 risk: Long-term suppression of gastric acid raises the risk of Vitamin B12 deficiency by up to 65%.
Brain-gut connection: The cephalic phase of digestion accounts for 20% to 30% of your total daily gastric acid secretion.
Functional dyspepsia: Over 80% of functional dyspepsia cases improve when underlying acid deficiencies are addressed.
Understanding Hypochlorhydria and How Your Stomach Actually Works
To fix a digestive problem, you first need to understand exactly what is going wrong. Low stomach acid is clinically known as hypochlorhydria. It occurs when the stomach fails to produce enough hydrochloric acid to maintain the highly acidic environment it needs to function properly.
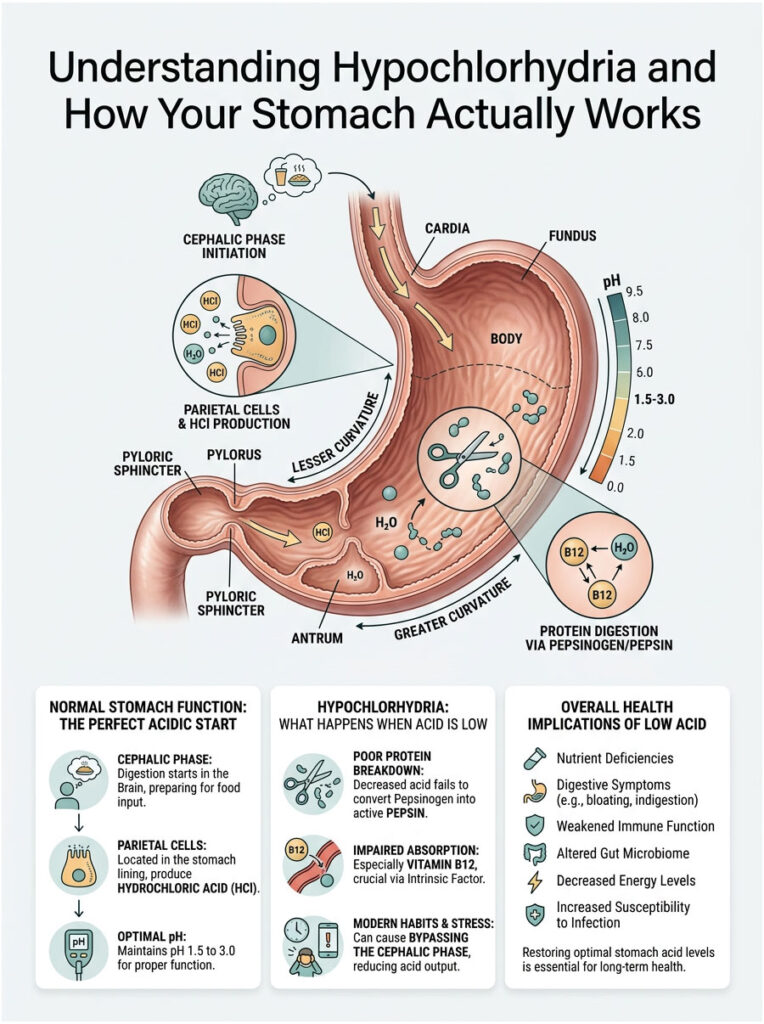
A healthy stomach must keep its pH between 1.5 and 3.0. That level of acidity is necessary to sterilize incoming food and break down complex proteins. When the pH drifts above 4.0, hypochlorhydria sets in, triggering a chain of gastrointestinal failures that can affect your entire body.
Have you ever noticed that antacids sometimes make things worse over time? The reason connects directly to how your esophagus works. Without enough acidity, the lower esophageal sphincter (LES) does not receive the chemical signal it needs to close tightly. That weakened valve allows whatever small amount of acid is present to splash upward into the esophagus. This is exactly why low stomach acid so often masquerades as excess acid reflux.
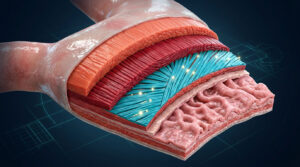
Parietal Cells and Hydrochloric Acid Production
The anatomy of your stomach lining is remarkably complex. Deep within the gastric pits sit specialized structures called parietal cells. These cells are responsible for manufacturing and secreting hydrochloric acid directly into the stomach.
Parietal cells rely on a microscopic mechanism called the proton pump, which exchanges potassium ions for hydrogen ions to create highly acidic gastric juice. When parietal cells become damaged or fatigued, acid production drops immediately. According to physiological data from the NIH, these cells require massive amounts of energy to push protons against a steep concentration gradient. If cellular energy or key micronutrients are lacking, the cells simply cannot do their job and effectively shut down.
The Cephalic Phase: Digestion Starts in Your Brain
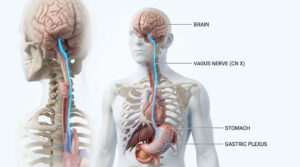
Digestion does not actually begin in your stomach. It begins in your brain. This brain-gut connection is called the cephalic phase of digestion, and it accounts for up to 30 percent of your total daily gastric acid secretion.
The cephalic phase is triggered by the sight, smell, and even the thought of food. When you anticipate a meal, your brain sends electrical signals down the vagus nerve, which then commands the parietal cells to start pumping acid before food even enters your mouth.
Here is where modern habits create real problems. If you eat while stressed, driving, or staring at a screen, you essentially bypass the cephalic phase entirely. That lack of neurological signaling is a primary driver of modern digestive dysfunction.
The Domino Effect: Pepsinogen, Pepsin, and Intrinsic Factor
Hydrochloric acid is not optional for protein digestion. Your stomach secretes an inactive enzyme called pepsinogen alongside the acid. Without a sufficiently acidic environment, pepsinogen cannot convert into its active form, pepsin. When this conversion fails, protein breakdown stalls completely. Undigested proteins pass into the small intestine where they putrefy, producing severe, foul-smelling gas.
Parietal cells also secrete a vital protein called Intrinsic Factor, which is required for Vitamin B12 absorption in the lower intestines. When hypochlorhydria compromises Intrinsic Factor secretion, patients develop pernicious anemia, a condition that causes chronic fatigue, neurological problems, and rapid cellular degradation. Restoring stomach acid is not just about fixing digestion. It is about protecting your overall systemic health.
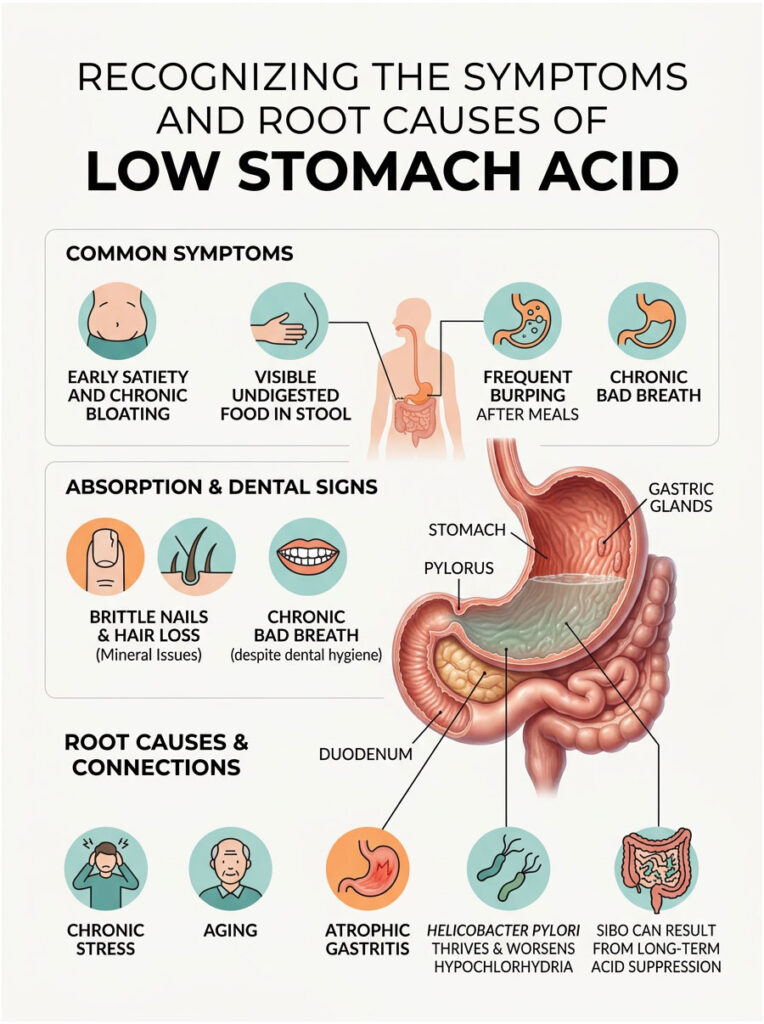
Recognizing the Symptoms and Root Causes of Low Stomach Acid
Many people suffer for years without realizing their stomach is simply underproducing acid. Because the symptoms of low stomach acid closely mimic those of excess acid, patients are often prescribed exactly the wrong treatment. Taking antacids for hypochlorhydria is like adding water to a gas tank. It completely stalls the digestive engine and creates new problems.
| Clinical Insight: If you experience heartburn that gets worse after taking antacids, or if you feel a heavy, rock-like sensation in your stomach after eating protein, you are likely dealing with low stomach acid. Excess acid rarely produces that heavy, stagnant feeling. |
Clinical Signs That Your Stomach Needs More Acid
The symptoms of low stomach acid are quite specific once you know what to look for. Early satiety, or feeling completely stuffed after just a few bites, is a classic warning sign. Chronic bloating within 30 minutes of eating is another major indicator.
Patients commonly report finding visible, undigested food particles in their stool. Because essential minerals require an acidic environment for proper absorption, brittle fingernails and sudden hair loss are also frequent symptoms. Frequent burping immediately after meals suggests food is fermenting in the stomach rather than being properly digested.
Chronic bad breath can also develop even with excellent dental hygiene. When proteins sit and putrefy in a low-acid stomach, they release foul-smelling gases that travel back up through the esophagus. Catching these subtle signs early makes a significant difference in treatment outcomes.
Root Causes: Chronic Stress, Aging, and Atrophic Gastritis
Chronic stress is one of the most overlooked inhibitors of healthy digestion. When your body is locked in sympathetic nervous system dominance (the fight-or-flight state), blood is diverted away from the gut. This actively suppresses gastrin, the primary hormone responsible for triggering acid secretion. Without adequate gastrin, your stomach stays dangerously alkaline.
Aging plays a significant role as well. The functional capacity of parietal cells naturally declines over the decades. Another severe root cause is atrophic gastritis, a condition where the stomach lining physically wastes away, destroying parietal cells in the process. When combined with long-term acid-suppressing medication use, the result can be achlorhydria, meaning zero acid production.
The link between mucosal atrophy and prolonged acid suppression is well-documented in functional medicine. True healing requires reversing this deep mucosal damage, not simply masking symptoms with more medication.
The Helicobacter Pylori and SIBO Connection
Helicobacter pylori is an opportunistic bacterial infection that thrives in a low-acid gut. To survive in the stomach, this bacterium secretes an enzyme called urease, which creates a localized ammonia cloud that neutralizes surrounding gastric acid. Over time, chronic H. pylori infection leads to severe, systemic hypochlorhydria.
When the stomach loses its protective acidity, it can no longer sterilize incoming food effectively. Harmful bacteria survive the stomach and migrate into the small intestine, causing Small Intestinal Bacterial Overgrowth (SIBO). Clinical studies have shown that long-term acid suppression directly increases your risk of developing SIBO. Treating SIBO without also addressing the underlying hypochlorhydria virtually guarantees that the bacterial overgrowth will return.
How to Test Your Stomach Acid Levels at Home and in the Clinic
Before starting any supplementation protocol, you need accurate baseline data. Guessing your gastric pH can lead to uncomfortable side effects or wasted money. Fortunately, there are several reliable ways to assess your current acid levels, both at home and through clinical testing.

The Baking Soda Test
The at-home baking soda test is a simple, inexpensive screening tool that relies on a basic chemical reaction. When baking soda meets hydrochloric acid, it produces carbon dioxide gas rapidly.
To perform this test, mix exactly one-quarter teaspoon of fresh baking soda into four ounces of cold water. Drink the solution first thing in the morning on a completely empty stomach and start a timer immediately. If you have adequate acid, the chemical reaction should cause you to burp within two to three minutes. If it takes longer than five minutes, or if you do not burp at all, it strongly suggests hypochlorhydria. This is not a perfect diagnostic tool, but it provides a useful starting point.
The Betaine HCl Challenge Protocol
The gold standard functional medicine test for low stomach acid is the Betaine HCl challenge. This method identifies your exact baseline acid needs by testing your physical response to supplemental acid during a protein-heavy meal.
Begin by taking one capsule of Betaine HCl with Pepsin midway through a meal that contains at least 20 grams of dense protein, such as chicken or beef. Monitor your body for a mild warming or burning sensation in the stomach area. If you feel nothing, repeat the challenge at your next protein meal with two capsules. Continue this careful escalation until you notice a slight warmth. Your ideal dose is exactly one capsule less than the amount that produced that sensation.
This challenge must be done carefully and methodically. It provides precise, individualized data on how much acid support your stomach currently needs.
The Heidelberg Capsule Test: Clinical Gold Standard
For patients who need definitive clinical answers, the Heidelberg Capsule Test is the most accurate diagnostic tool available. This medical procedure involves swallowing a tiny, pill-sized radio transmitter that measures the exact pH of your stomach in real time.
Once swallowed, the doctor administers a baking soda solution to temporarily neutralize your stomach acid. The capsule then records how long it takes for the stomach to re-acidify. A healthy stomach returns to a pH of 1.5 within 15 to 20 minutes. If your stomach takes over 45 minutes to re-acidify, you have a definitive clinical diagnosis of hypochlorhydria. This test removes all guesswork and allows practitioners to design highly targeted treatment plans.
Normal Gastric Function vs. Hypochlorhydria: A Clinical Comparison
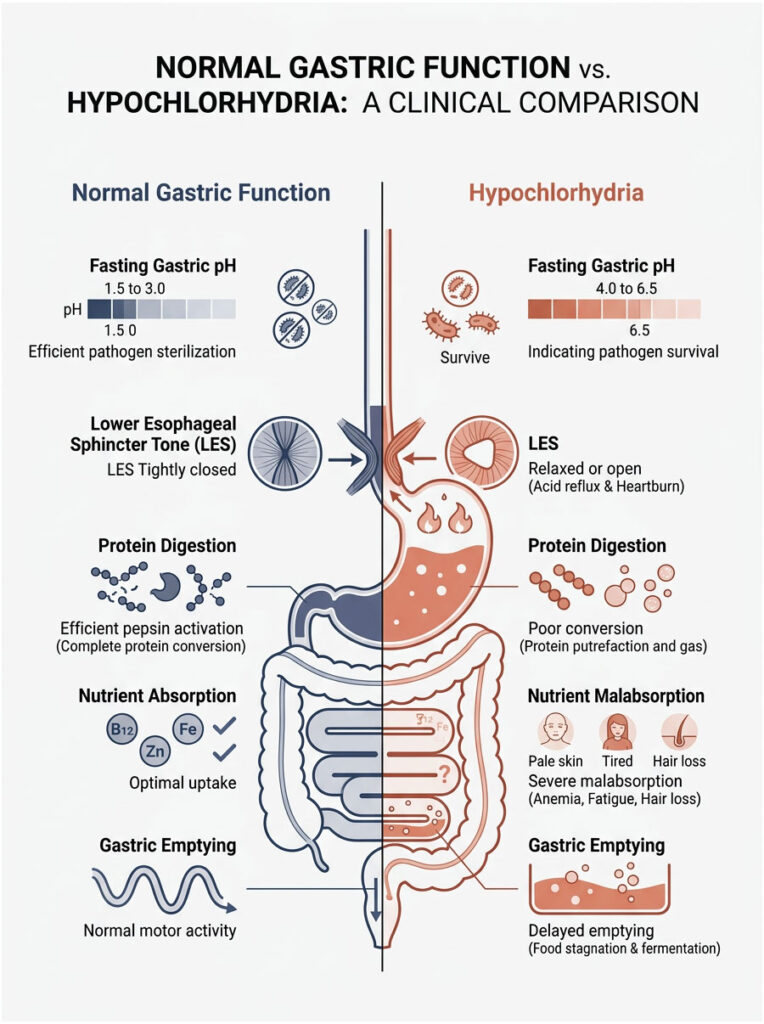
| Physiological Marker | Normal Function | Hypochlorhydria | Clinical Consequence |
| Fasting Gastric pH | 1.5 to 3.0 | 4.0 to 6.5+ | Cannot sterilize ingested pathogens |
| LES Tone | Tightly closed | Relaxed or open | Acid refluxes into esophagus, causing heartburn |
| Protein Digestion | Efficient pepsin activation | Poor pepsinogen conversion | Proteins putrefy, causing severe gas |
| Nutrient Absorption | Optimal B12, Iron, Zinc uptake | Severe malabsorption | Anemia, fatigue, and hair loss |
| Gastric Emptying | Normal motor complex activity | Delayed emptying | Food stagnates and ferments in the stomach |
Proven Natural Methods to Increase Stomach Acid
Once you have confirmed a deficiency, it is time to take action. Figuring out how to increase stomach acid naturally requires a layered approach that addresses neurological signaling, chemical pH adjustment, and targeted supplementation all at once.
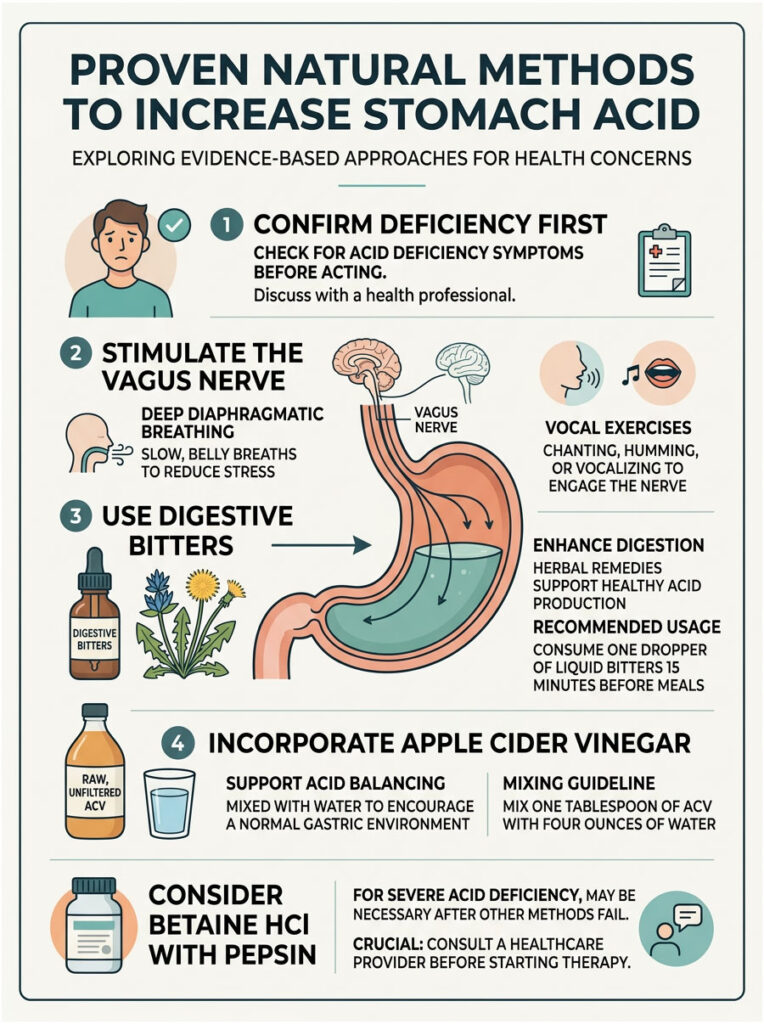
There is no single magic pill for this. You need to retrain your entire digestive system to function independently again. That means combining smart daily habits with specific, powerful clinical interventions.
Stimulating the Vagus Nerve for Better Digestion
The vagus nerve is the master controller of your digestive system. It serves as the primary communication highway between your brain and your gut. If the vagus nerve is dormant or suppressed by chronic stress, your parietal cells will never receive the signal to produce acid.
To activate the vagus nerve, you need to shift your body into a parasympathetic (rest-and-digest) state. I recommend practicing deep diaphragmatic breathing for three full minutes before every meal. Inhaling deeply expands the diaphragm, which physically stimulates the vagus nerve.
Other effective methods include gargling cold water vigorously, humming loudly, or singing. These specific actions activate the vocal cords, which are directly connected to the vagus nerve. Making vagus nerve stimulation a daily habit is one of the most important foundational steps in overcoming hypochlorhydria.
Digestive Bitters: An Ancient Remedy With Modern Science Behind It
Bitter herbs like gentian root, dandelion, and burdock have been used for centuries across cultures to improve sluggish digestion. When you taste something intensely bitter, it triggers a hardwired neurological reflex that is remarkably effective.
Bitter receptors on the back of your tongue send an immediate electrical signal through the vagus nerve, prompting the stomach to release the hormone gastrin. Gastrin then instructs the parietal cells to flood the stomach with acid.
For the best results, place one full dropper of liquid digestive bitters directly on your tongue about 15 minutes before eating. Do not dilute them heavily in water. You need to actually taste the bitterness to trigger the reflex properly. This simple, affordable habit can dramatically improve early-stage digestion.
Apple Cider Vinegar: A Practical, Accessible Option
If you are looking for a natural remedy that is easy to find and affordable, Apple Cider Vinegar is a solid choice. Raw, unfiltered Apple Cider Vinegar contains acetic acid, which temporarily lowers gastric pH and helps the stomach reach the critical threshold needed for proper digestion.
While Apple Cider Vinegar is nowhere near as strong as hydrochloric acid, it is quite effective for mild indigestion. It also helps tighten the lower esophageal sphincter, which can quickly reduce reflux symptoms. Additionally, it acts as a mild natural antimicrobial in the upper gut.
Here is the protocol I recommend for safety and effectiveness: mix exactly one tablespoon of raw, unfiltered Apple Cider Vinegar into four ounces of room-temperature water. Drink it about 15 minutes before your largest meals. Using a straw is highly recommended to protect your dental enamel from the vinegar’s acidity.
Betaine HCl with Pepsin: For Severe Hypochlorhydria
For patients dealing with significant acid deficiency, lifestyle adjustments alone are rarely sufficient. This is where exogenous acid replacement therapy becomes necessary. Supplementing with Betaine HCl with Pepsin provides the exact chemical compound your stomach is failing to produce on its own.
Betaine HCl drops the gastric pH to optimal levels almost immediately. The added pepsin ensures that complex protein strands are broken down efficiently, stopping the putrefaction process that causes severe bloating and foul gas.
Based on extensive clinical experience, patients often need between 500mg and 3000mg of Betaine HCl per meal, depending on the protein content of the food. These capsules must always be taken midway through a meal, never on an empty stomach.
Important safety note: Betaine HCl is strictly contraindicated for individuals with active peptic ulcers, severe gastritis, or those currently taking NSAIDs or corticosteroids. Always consult a qualified healthcare provider before beginning this therapy.
Essential Micronutrients Your Parietal Cells Need to Produce Acid
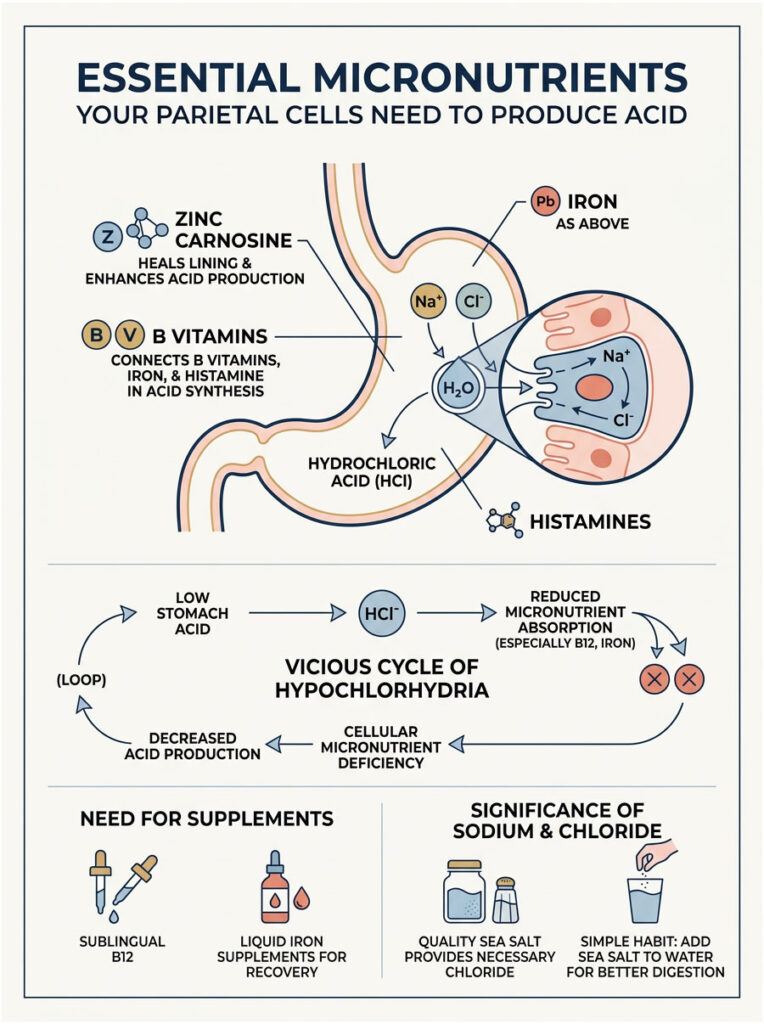
Your stomach cannot manufacture acid out of thin air. The biological machinery requires specific raw materials to function properly. If you are deficient in key micronutrients, your parietal cells will physically fail to produce adequate hydrochloric acid.
Zinc Carnosine: Healing the Stomach Lining From the Inside
Zinc is a non-negotiable cofactor for an enzyme called carbonic anhydrase, which is the specific enzyme inside parietal cells responsible for creating gastric acid from water and carbon dioxide. Without adequate zinc, acid production drops significantly.
Zinc Carnosine is a unique chelated compound that adheres directly to the stomach wall, actively healing ulcerations and reducing mucosal inflammation. It allows damaged parietal cells to recover from trauma caused by H. pylori or chronic stress. Clinical studies support taking 75mg of Zinc Carnosine twice daily, away from food, for optimal mucosal healing.
B Vitamins, Iron, and the Histamine Connection
There is a frustrating cyclical problem with hypochlorhydria. Low stomach acid causes poor absorption of B vitamins and dietary iron. But your body needs these exact nutrients to power the histamine H2 receptors that stimulate acid production in the first place.
You need iron and Vitamin B6 to synthesize histamine in the gut. Histamine binds to H2 receptors on parietal cells, instructing them to release acid. If you are anemic from low acid, you physically cannot produce the histamine needed to make more acid. It is a vicious cycle.
To break this loop, patients often need sublingual B12 and liquid iron supplements that bypass the compromised digestive tract and enter the bloodstream directly. This gradually restores the stomach’s ability to produce its own gastrin and acid naturally.
Sodium and Chloride: The Overlooked Building Blocks
We often forget the most basic chemistry involved in digestion. Hydrochloric acid is literally made of hydrogen and chloride. If you follow a strict low-sodium diet, you might be starving your body of the chloride it needs to manufacture stomach acid.
High-quality, unrefined sea salt is rich in natural chloride and trace minerals. Standard table salt is heavily processed and stripped of these beneficial cofactors. Swapping to Celtic sea salt or Himalayan pink salt provides the raw materials your parietal cells need.
I often advise patients to add a small pinch of quality sea salt to their morning water. This simple habit hydrates the cells and supplies an immediate dose of chloride. It is a tiny change that yields meaningful benefits for digestion.
Top Natural Interventions for Stomach Acid Support: A Comparison

| Intervention | How It Works | Ideal Timing and Dosage | Best Suited For |
| Apple Cider Vinegar | Introduces acetic acid to lower gastric pH | 1 tbsp in 4 oz water, 15 min before meals | Mild indigestion and early-stage hypochlorhydria |
| Digestive Bitters | Stimulates tongue receptors to trigger gastrin release | 1 dropper on the tongue before meals | Vagus nerve sluggishness and poor bile flow |
| Betaine HCl + Pepsin | Provides direct exogenous hydrochloric acid | 500mg to 3000mg midway through a protein meal | Severe hypochlorhydria and chronic SIBO patients |
| Zinc Carnosine | Supports carbonic anhydrase and heals gastric mucosa | 75mg twice daily, away from food | Patients recovering from H. pylori or gastritis |
Dietary and Lifestyle Strategies for Long-Term Stomach Health
Supplements are effective, but they are only one piece of a larger puzzle. How you eat matters just as much as what you eat. Long-term gastric optimization requires behavioral changes that support your body’s natural digestive rhythms.
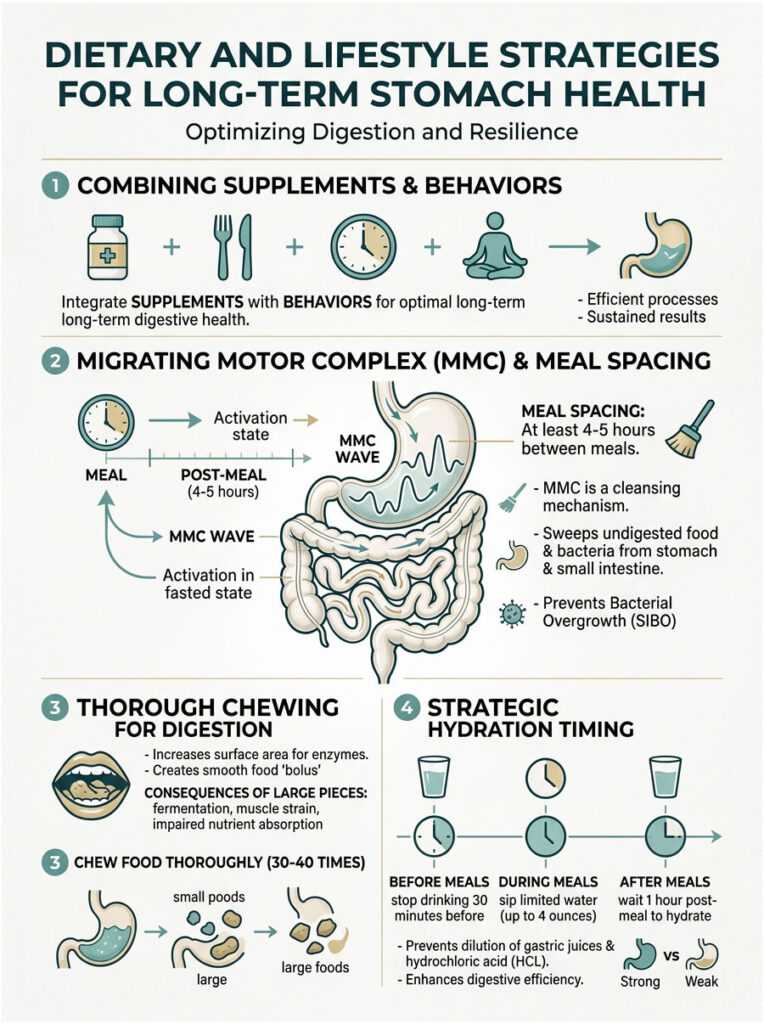
Meal Spacing and the Migrating Motor Complex
Frequent snacking is one of the worst habits for long-term gut health. Fasting between meals activates a neurological process called the Migrating Motor Complex (MMC), a sweeping wave of electrical activity that cleans out the stomach and small intestine between meals.
The MMC only activates after you have been in a fasted state for at least 90 to 120 minutes. If you eat a handful of nuts every couple of hours, you halt this cleansing wave entirely. Residual food sits stagnant, fermenting and worsening hypochlorhydria.
I strongly recommend spacing meals at least four to five hours apart. This gives your stomach time to empty completely, reset its acid levels, and prepare properly for the next meal.
Why Chewing Your Food Thoroughly Matters More Than You Think
Your stomach does not have teeth. If you swallow large, poorly chewed pieces of food, you place an enormous chemical burden on your parietal cells. Aim to chew each bite 30 to 40 times until the food becomes a warm, liquid paste.
Thorough chewing dramatically increases the total surface area of your food, allowing hydrochloric acid and pepsin to penetrate much more effectively. It also extends the cephalic phase of digestion, giving the vagus nerve more time to signal the stomach. Slowing down your meals is a powerful, completely free intervention that yields immediate results.
Hydration Timing Around Meals
Drinking large amounts of liquid during a meal is a common habit that works against anyone with low stomach acid. Chugging a tall glass of ice water with dinner actively dilutes your gastric juices and raises the stomach’s pH, making it less effective.
Ice-cold beverages also constrict blood vessels lining the stomach, reducing blood flow to the parietal cells and slowing acid production. Digestion requires heat, energy, and concentrated acid to work properly.
Stop drinking large amounts of water about 30 minutes before eating. During the meal, sip no more than four ounces of room-temperature water if needed to swallow food. Wait at least one hour after finishing your meal before resuming normal hydration.
Clinical Case Study: Restoring Stomach Acid After Years of PPI Use
In clinical practice, restoring stomach acid genuinely transforms patients’ lives. Here is a generalized case study based on real-world observations. A 45-year-old male presented with chronic acid reflux, severe daily bloating, and diagnosed iron-deficiency anemia.
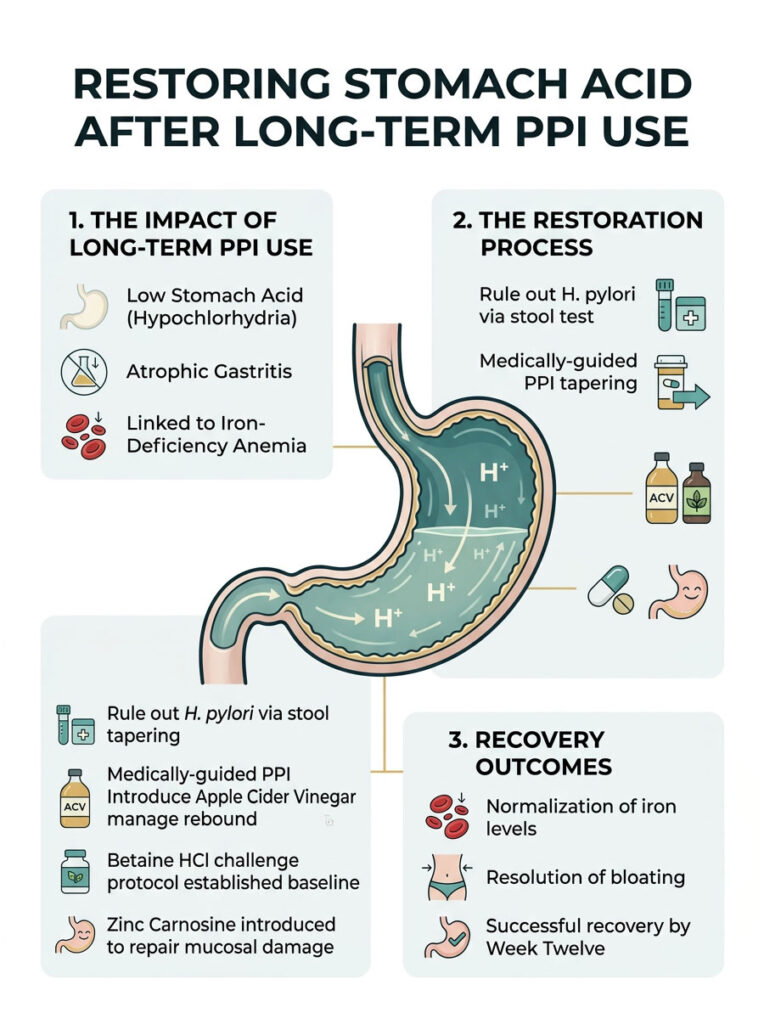
For five years, he had been taking daily Proton Pump Inhibitors (PPIs) prescribed by his primary care doctor. His symptoms were progressively worsening, and his energy levels were completely depleted. We identified that long-term atrophic gastritis combined with PPI use had essentially shut down his natural acid production.
Here is how we approached his recovery. First, we ran comprehensive stool testing to rule out active H. pylori infection. Then, we began a slow, careful tapering process off his PPI medication under close medical supervision. To manage rebound reflux, we introduced Apple Cider Vinegar and digestive bitters to gently lower his gastric pH.
In week four, we used the Betaine HCl challenge protocol to establish his baseline. He required 1500mg of Betaine HCl with Pepsin per meal to achieve normal, pain-free digestion. We also introduced 75mg of Zinc Carnosine twice daily to repair the mucosal damage caused by years of poor digestion.
By week twelve, his chronic bloating had completely resolved. His iron levels began to normalize as his stomach became acidic enough to absorb minerals again. Over six months, he successfully weaned off Betaine HCl entirely as his parietal cells regained their natural function.
This case aligns with published data from the Institute for Functional Medicine, which shows that directly addressing hypochlorhydria resolves up to 80% of functional dyspepsia cases, often without the need for lifelong medication.
Summary and Key Takeaways
Learning how to increase stomach acid naturally requires patience, clinical precision, and a multi-layered lifestyle approach. It is not about finding a single pill to suppress symptoms. It is about restoring the biological environment your entire gastrointestinal tract needs to thrive.

Prioritize stress management to optimize vagus nerve tone and parasympathetic signaling.
Use bitter herbs and Apple Cider Vinegar to enhance natural digestive reflexes and provide mild pH adjustment.
Supplement with Betaine HCl with Pepsin when clinical deficiency is confirmed, under proper guidance.
Support parietal cell health with Zinc Carnosine, quality sea salt, and bioavailable B vitamins.
Respect meal timing and chewing to give your digestive system the conditions it needs to function properly.
Do not let the symptoms of low stomach acid control your quality of life. By understanding your physiology, supporting your parietal cells with the right nutrients, and respecting the cephalic phase of digestion, you can reclaim your health. Learning how to increase stomach acid naturally means working with your body’s design rather than fighting against it.
Frequently Asked Questions
What are the most common clinical symptoms of Hypochlorhydria?
The primary clinical indicators of Hypochlorhydria, or low stomach acid, include chronic bloating within 30 minutes of eating, early satiety (feeling full quickly), and the presence of undigested food in the stool. Patients also frequently report a heavy, ‘rock-like’ sensation after consuming dense proteins, as the lack of acid prevents the activation of pepsinogen into pepsin, halting protein breakdown.
How does Apple Cider Vinegar (ACV) help increase stomach acid naturally?
Apple Cider Vinegar contains acetic acid, which possesses a lower pH than the average hypochlorhydric stomach. By consuming one tablespoon of raw ACV in four ounces of water 15 minutes before a meal, you introduce exogenous acid that helps lower the gastric pH. This temporary acidification assists in signaling the lower esophageal sphincter (LES) to close, which can prevent acid reflux symptoms caused by low acidity.
Is it safe to take Betaine HCl with Pepsin for low stomach acid?
Supplementing with Betaine HCl with Pepsin is a standard functional medicine intervention for restoring gastric pH. However, it must be used cautiously. It is strictly contraindicated for individuals with active peptic ulcers, severe gastritis, or those taking NSAIDs and corticosteroids, as these can thin the gastric mucosa. Always perform a supervised Betaine HCl challenge to determine your specific dosage needs based on meal protein content.
Can low stomach acid actually cause acid reflux and GERD?
Yes, this is a common clinical paradox. The lower esophageal sphincter (LES) is a pH-sensitive valve; it requires a highly acidic environment (pH 1.5–3.0) to receive the chemical signal to close tightly. In cases of Hypochlorhydria, the LES remains relaxed or ‘floppy,’ allowing even small amounts of weak acid to reflux into the esophagus, mimicking the symptoms of hyperacidity.
How do I perform the at-home Baking Soda Test for stomach acid?
To perform the bicarbonate screening, mix 1/4 teaspoon of baking soda in 4 ounces of cold water and drink it on an empty stomach first thing in the morning. The baking soda reacts with hydrochloric acid to produce carbon dioxide gas. If you have adequate acid levels, you should burp within 2 to 3 minutes. If it takes longer than 5 minutes, it suggests a state of Hypochlorhydria.
What role does the Vagus nerve play in gastric acid secretion?
The Vagus nerve is the primary conduit for the parasympathetic nervous system, which governs the ‘rest and digest’ response. It stimulates the Parietal cells via the Cephalic phase of digestion, which can account for up to 30% of total daily acid secretion. Stress suppresses Vagus nerve tone, preventing the brain from signaling the stomach to produce acid before food arrives.
Why is Zinc Carnosine recommended for patients with low stomach acid?
Zinc is a mandatory co-factor for the enzyme carbonic anhydrase, which Parietal cells use to manufacture hydrochloric acid. Zinc Carnosine is particularly effective because it is a chelated compound that adheres to the gastric lining, promoting mucosal repair and healing inflammation. This is critical for patients whose stomach linings have been thinned by chronic stress, H. pylori infections, or long-term PPI use.
How does H. pylori infection lead to chronic low stomach acid?
Helicobacter pylori is a highly adapted bacterium that survives the stomach’s acidic environment by secreting an enzyme called urease. Urease converts urea into ammonia, creating a localized ‘neutralizing cloud’ that raises the surrounding pH. Over time, the chronic inflammation caused by the infection can lead to atrophic gastritis, where Parietal cells are permanently damaged, resulting in long-term Hypochlorhydria.
Can low stomach acid lead to Vitamin B12 and iron deficiency?
Absolutely. Hydrochloric acid is required to cleave Vitamin B12 from food proteins and to stimulate the secretion of Intrinsic Factor from Parietal cells, which is necessary for B12 absorption in the ileum. Furthermore, iron requires an acidic environment to be converted into its absorbable ferrous form. This is why chronic Hypochlorhydria is a leading cause of pernicious anemia and iron-deficiency anemia.
What are digestive bitters and how do they stimulate acid production?
Digestive bitters are liquid herbal extracts (such as gentian or dandelion) that trigger the ‘bitter reflex’ on the tongue. This reflex sends a signal through the Vagus nerve to the stomach, prompting the release of the hormone gastrin. Gastrin then instructs the Parietal cells to secrete hydrochloric acid and the pancreas to release digestive enzymes, making bitters an excellent tool for priming the digestive cascade.
What is the ‘Cephalic Phase’ of digestion and why does it matter?
The Cephalic phase is the stage of digestion that occurs before food ever hits the stomach. It is triggered by the sight, smell, and even the thought of food. This phase activates the Vagus nerve to begin acid production in anticipation of a meal. Eating while stressed or distracted bypasses this phase, often resulting in insufficient acid levels and poor protein digestion.
How does meal timing and the Migrating Motor Complex (MMC) affect stomach acid?
The Migrating Motor Complex is a cleansing wave of electrical activity that occurs only in a fasted state, typically 90–120 minutes after eating. Constant grazing or snacking prevents the MMC from activating and keeps the stomach in a perpetual state of low-level secretion, which can exhaust Parietal cells. Spacing meals 4–5 hours apart allows the stomach to reset its pH and maintain the acidity required for the next meal.
Disclaimer:
The information provided in this article is intended for general educational and informational purposes only. It does not constitute medical advice and should not be used as a replacement for consultation with a licensed healthcare professional.
Supplementation with Betaine HCl, Zinc Carnosine, digestive bitters, Apple Cider Vinegar, or any other substance mentioned in this article should only be undertaken after consulting with a qualified healthcare provider. Self-diagnosing hypochlorhydria and beginning supplementation without professional guidance can lead to adverse effects, particularly for individuals with active peptic ulcers, gastritis, or those taking NSAIDs, corticosteroids, or other prescription medications.
The Betaine HCl challenge protocol described in this article is a functional medicine screening tool and should ideally be performed under clinical supervision. The baking soda test is a preliminary home screening method and is not a definitive diagnostic tool.
The case study presented is a generalized clinical example based on common patient presentations. It does not represent a specific individual, and results vary from patient to patient. Statistics cited from the National Institutes of Health and the Institute for Functional Medicine are based on published research and are subject to ongoing scientific review.
The author and publisher disclaim all liability for any harm, injury, or damage arising from the use or misuse of the information contained in this article. Any dietary, lifestyle, or supplement changes should be discussed with your doctor before implementation.
Never stop or modify prescription medications without direct supervision from your prescribing physician.
References:
- National Institutes of Health (NIH) – Gastric Acid Secretion and Physiology
https://www.ncbi.nlm.nih.gov/books/NBK507793/ - Institute for Functional Medicine (IFM) – Hypochlorhydria and Digestive Health
https://www.ifm.org/ - National Library of Medicine – Betaine Hydrochloride Clinical Efficacy
https://pubmed.ncbi.nlm.nih.gov/ - NIH – Proton Pump Inhibitors and Long-Term Health Risks
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4110863/ - American Journal of Gastroenterology – Impact of Gastric Acid on Nutrient Absorption
https://journals.lww.com/ajg/pages/default.aspx - NIH – Helicobacter Pylori Infection and Gastric Acid
https://www.ncbi.nlm.nih.gov/books/NBK534233/ - National Library of Medicine – Small Intestinal Bacterial Overgrowth (SIBO)
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3099351/ - NIH – Zinc Carnosine for Gastric Mucosal Protection
https://pubmed.ncbi.nlm.nih.gov/17151807/ - NIH – Vitamin B12 Deficiency and Gastric Acid Suppression
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4462725/ - NIH – The Vagus Nerve and Gastrointestinal Function
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5859128/ - Mayo Clinic – Atrophic Gastritis
https://www.mayoclinic.org/diseases-conditions/gastritis/symptoms-causes/syc-20355807 - NIH – Parietal Cell Function and Hydrochloric Acid Production
https://www.ncbi.nlm.nih.gov/books/NBK541099/ - World Gastroenterology Organisation – Cephalic Phase of Digestion
https://www.worldgastroenterology.org/ - NIH – Apple Cider Vinegar and Digestive Health
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8243436/ - NIH – Migrating Motor Complex and Interdigestive Motility
https://www.ncbi.nlm.nih.gov/books/NBK542172/ - NIDDK – Pernicious Anemia
https://www.niddk.nih.gov/health-information/blood-diseases/pernicious-anemia