A patient sat in my clinic last week and asked a question I hear almost every day. She wanted to know how to maintain sexual health for women without relying on quick fixes or ignoring her body’s natural signals. As a board-certified OB-GYN with over 15 years of clinical experience, I understand that frustration completely.
Table of Contents
Female sexual wellness is not simply the absence of dysfunction or pain. It is a complex biological equilibrium involving three interconnected systems: the endocrine system, the vaginal microbiome, and pelvic floor mechanics. Based on evidence-based guidelines from the American College of Obstetricians and Gynecologists (ACOG) and the North American Menopause Society (NAMS), this guide provides a clear roadmap for protecting your intimate health.

You do not have to accept discomfort or declining desire as a normal part of aging. By understanding the science behind your body, you can take back control.
Quick Answer: How Do You Maintain Sexual Health as a Woman?
A holistic approach built on three pillars. First, support your endocrine system for proper hormonal balance. Second, protect your vaginal microbiome by maintaining an acidic pH between 3.8 and 4.5. Third, strengthen your pelvic floor mechanics to prevent pain and enhance sensation. Managing these three areas is the foundation of female sexual dysfunction prevention.
Key Statistics on Female Sexual Wellness
- 43.5% of women experience some form of sexual dysfunction during their lifetime (JAMA).
- Over 50% of postmenopausal women suffer from Genitourinary Syndrome of Menopause (GSM) silently without seeking treatment (NAMS, 2022).
- Routine douching increases the risk of Pelvic Inflammatory Disease (PID) by 73% (CDC).
- Nearly 1 in 10 women will experience Hypoactive Sexual Desire Disorder (HSDD) during their reproductive years.
- Pelvic floor physical therapy improves orgasmic function and reduces pain in 65% to 70% of compliant patients (APTA).
- Chronic stress makes women 45% more likely to report a significant decrease in sexual desire.
Redefining Female Sexual Health
For decades, medical literature and popular culture have oversimplified female sexuality, reducing it to a basic on-and-off switch. In clinical practice, maintaining sexual health for women is far more nuanced. It requires understanding how your body, environment, and mind interact every day.

Low desire is not always a psychological issue. Often, it is a physiological signal from an imbalanced system. Your body depends on a delicate network of hormones, bacteria, and muscle fibers. When one part of that network struggles, the entire system feels it.
Beyond the Simple Concept of Libido
The traditional linear model of sexual response, pioneered by Masters and Johnson in the 1960s, suggested a straightforward path from excitement to orgasm. It does not accurately reflect how most women experience arousal.
Modern gynecology relies on Dr. Rosemary Basson’s non-linear model, which shows that female arousal is cyclical. It depends heavily on emotional intimacy, physical comfort, and biological readiness. Many women experience responsive desire, meaning arousal follows physical stimulation rather than preceding it. With up to 43.5% of women experiencing some form of sexual dysfunction, this is a widespread clinical issue, not a personal failing.
The Triad of Sexual Vitality
Your intimate health rests on three interconnected pillars. Your endocrine system controls the chemical messengers driving blood flow and desire. Your vaginal microbiome keeps local tissues resilient, lubricated, and infection-free. Your pelvic floor provides the muscular control needed for comfortable penetration and orgasmic release.
A failure in one pillar almost always cascades into the others. A sharp hormonal drop can thin vaginal tissues, leading to painful intercourse (dyspareunia). That pain causes pelvic floor muscles to tense defensively, creating a cycle of discomfort and avoidance.
The Role of the Nervous System
Sexual arousal strictly requires your body to be in a parasympathetic (rest-and-digest) state. When stress keeps your sympathetic (fight-or-flight) system active, your body redirects blood away from pelvic organs and toward your limbs. You cannot achieve physical arousal if your nervous system perceives danger.
This is why relaxation is not a luxury. It is a physiological prerequisite. Deep breathing, mindfulness, and adequate sleep directly support your body’s ability to transition into an aroused state.
Hormonal Balance for Sexual Wellness
Hormones are the unseen architects of sexual vitality. They control everything from daily mood to the microscopic thickness of vaginal tissues. Achieving hormonal balance is not about chasing perfect lab numbers. It is about optimizing how those hormones interact at the cellular level.
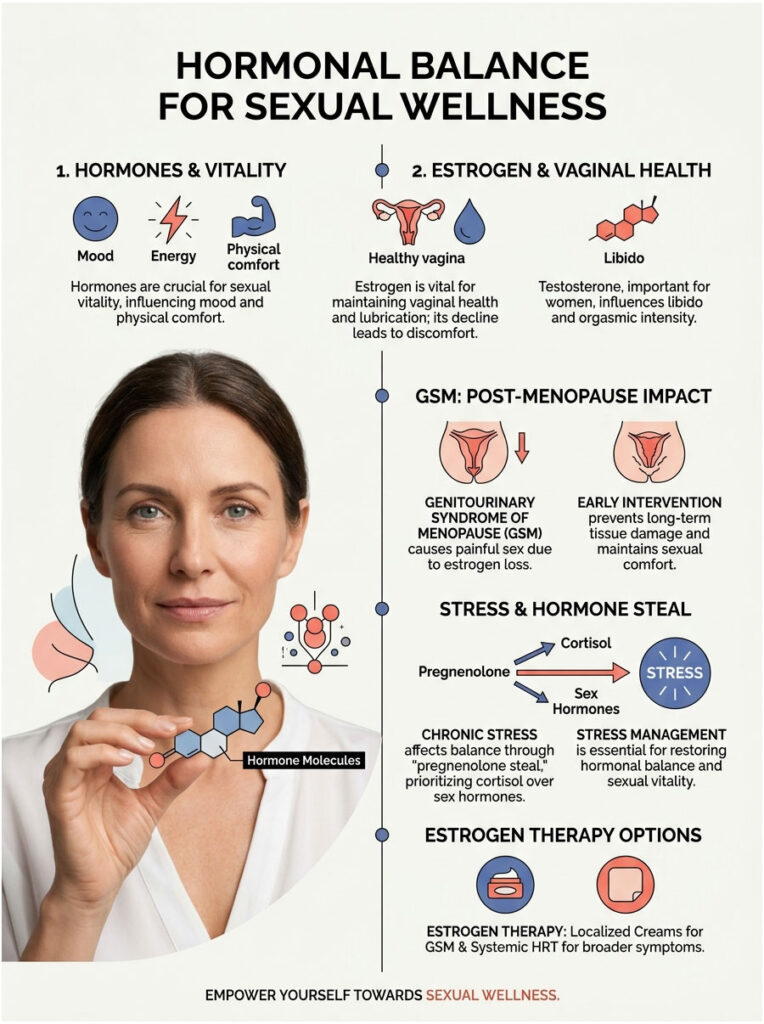
Estrogen and Sexual Function
Estrogen is the most critical hormone for female sexual comfort. It maintains the structural integrity of vulvar skin and vaginal mucosa. When estrogen is optimal, blood flow to the pelvic region increases during arousal, triggering natural lubrication.
Estrogen also drives glycogen production in vaginal walls, which feeds the healthy bacteria that protect your vaginal microbiome. Without adequate estrogen, this protective ecosystem starves and collapses.
During perimenopause and menopause, estrogen production declines sharply. Tissues become thinner, less elastic, and more prone to micro-tears during intimacy. This is why hormonal management becomes a daily priority as women age.
The Overlooked Importance of Testosterone
Testosterone is not strictly a male hormone. Women actually have higher circulating levels of testosterone than estrogen during their reproductive years. It acts directly on the brain’s desire centers, driving spontaneous sexual thoughts and maintaining the sensitivity of the clitoral nerve network.
When testosterone drops, women frequently report a complete flatlining of libido and reduced orgasmic intensity. Levels naturally peak in a woman’s twenties and decline over time, but surgical menopause or certain oral contraceptives can cause a sudden, severe drop. If you have lost desire completely, asking your doctor for a free and total testosterone panel is a smart clinical move.
Understanding Genitourinary Syndrome of Menopause (GSM)
If you experience dryness, burning, or pain during sex after menopause, you are likely dealing with GSM. NAMS defines it as a collection of symptoms caused by severe estrogen decline, affecting the labia, clitoris, vagina, urethra, and bladder.
As estrogen drops, vaginal walls lose collagen and moisture. Local pH rises, making the area more susceptible to infections. This atrophy leads to severe dyspareunia and tearing. Over 50% of postmenopausal women suffer from GSM silently, often believing painful sex is just a normal part of aging. It absolutely is not.
Clinical Tip: Do not wait for GSM symptoms to become unbearable. Early intervention with localized treatments can prevent permanent tissue changes and preserve intimate comfort for decades.
Cortisol and the Pregnenolone Steal
Chronic stress forces your body into survival mode. When this happens, a phenomenon called the “pregnenolone steal” occurs. Pregnenolone is a precursor hormone used to make both cortisol and sex hormones. Under high stress, your body prioritizes cortisol production over testosterone and estrogen, literally stealing the raw materials needed for sexual vitality.
The result: your body actively shuts down reproductive drives to focus on surviving. High cortisol blunts libido and disrupts menstrual cycles. Stress-management strategies like diaphragmatic breathing are not wellness trends. They are medical necessities for restoring hormonal balance.
Estrogen Therapy Options Comparison
| Therapy Type | How It Works | Best For | Systemic Absorption | NAMS Recommendation |
| Topical Vaginal Estrogen | Localized creams, rings, or inserts to restore tissue | GSM, severe dryness, localized dyspareunia | Very Low | First-line for genitourinary symptoms |
| Systemic HRT (Pills/Patches) | Circulates through bloodstream to elevate hormone levels | Hot flashes, systemic menopause symptoms, mood shifts | High | For moderate to severe vasomotor symptoms |
| Non-Hormonal Moisturizers | Hyaluronic acid or polycarbophil that binds water to tissues | Patients with estrogen contraindications (e.g., oncology) | None | Excellent adjunct for daily tissue hydration |
The Vaginal Microbiome and pH Balance
Your vagina is a self-regulating ecosystem that depends on a precise balance of bacteria and acidity. Maintaining vaginal microbiome health is just as important as managing circulating hormones. Disruptions in this environment lead to infections, odor, and significant discomfort during intimacy.
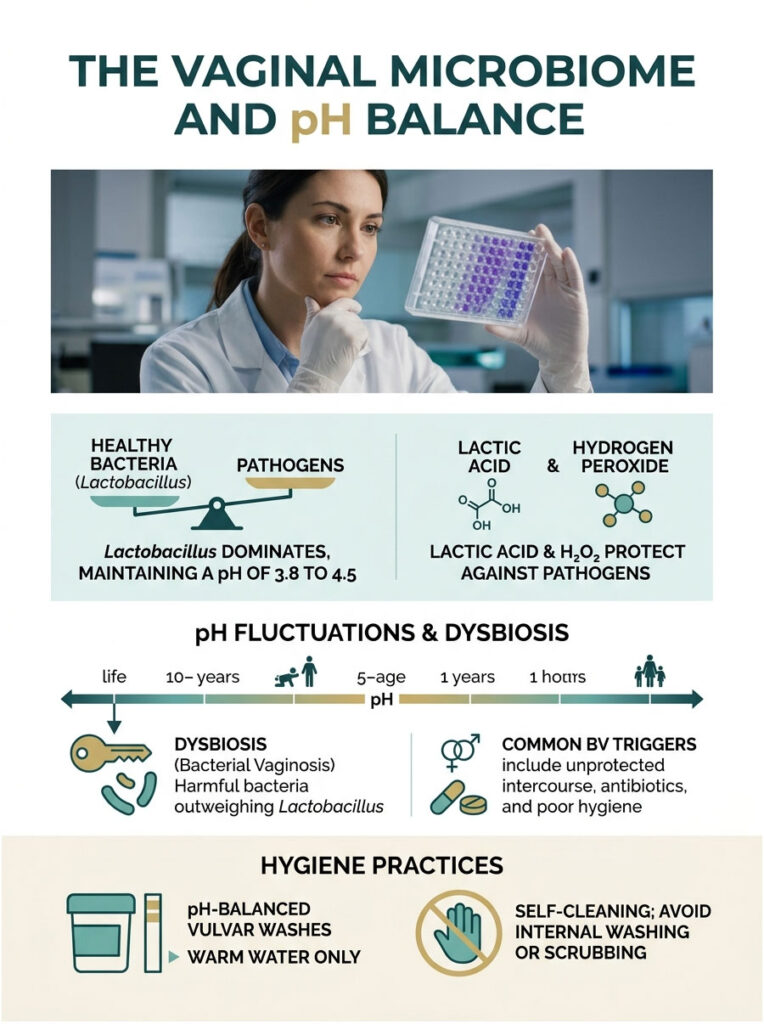
Lactobacillus and the Lactic Acid Mantle
The foundation of vaginal microbiome health is dominance by Lactobacillus species. The ideal vaginal pH sits between 3.8 and 4.5. This acidic environment is your primary biological defense against pathogens.
Specific strains like Lactobacillus crispatus consume glycogen produced by vaginal cells and produce lactic acid and hydrogen peroxide. This lactic acid mantle creates an environment that is inhospitable to harmful bacteria and yeast. Vaginal pH fluctuates across life stages: high estrogen during reproductive years keeps it acidic, menstrual blood temporarily raises it, and menopause reduces glycogen production, leading to a dangerously alkaline shift.
Preventing Bacterial Vaginosis (BV)
When the lactic acid balance is disrupted, a condition called dysbiosis occurs. The most common result is Bacterial Vaginosis (BV), where harmful anaerobic bacteria outnumber protective Lactobacillus strains.
Common triggers include frequent unprotected intercourse (semen is alkaline, with a pH of 7.2 to 8.0), broad-spectrum antibiotics that wipe out good and bad bacteria alike, and improper hygiene practices. Untreated BV is not just a nuisance. It carries a strong clinical link to increased risk of Pelvic Inflammatory Disease.
Evidence-Based Vaginal Hygiene Practices
One of the most common mistakes involves improper intimate hygiene. The vagina is internal and entirely self-cleaning. It requires no internal washing, scrubbing, or flushing. Here are the steps to follow daily:
- Urinate within 15 to 30 minutes after intercourse to flush bacteria from the urethra and prevent UTIs.
- Wash the external vulva with warm water only. If you must use soap, choose a pH-balanced, fragrance-free cleanser for external use only.
- Never douche. ACOG and the CDC strongly warn against all douching. It washes away protective bacteria and pushes pathogens toward the cervix, increasing PID risk by 73%.
- Wear 100% cotton underwear. Synthetic fabrics trap heat and moisture, which rapidly breeds yeast and harmful bacteria.
Intimate Hygiene Product Analysis
| Product | Typical pH | Microbiome Impact | Expert Verdict |
| Traditional Bar Soaps | 9.0-10.0 (Alkaline) | Strips the protective acid mantle | Avoid completely |
| Commercial Douches | Variable | Destroys Lactobacillus, pushes bacteria upward | Strongly avoid (ACOG/CDC) |
| Scented Intimate Wipes | Variable | Introduces allergens and synthetic fragrances | Avoid (risk of contact dermatitis) |
| pH-Balanced Vulvar Washes | 4.0-5.0 (Mildly Acidic) | Respects the acid mantle if used externally | Approved for external use only |
| Warm Water Only | 7.0 (Neutral) | Safe, non-disruptive mechanical cleansing | Gold standard for daily care |
Pelvic Floor Mechanics and Sexual Function
Hormones and hygiene get most of the attention, but the physical structure supporting your reproductive organs plays a massive role in both pleasure and pain. Pelvic floor muscles must contract forcefully for orgasmic release and relax fully for comfortable, painless penetration.
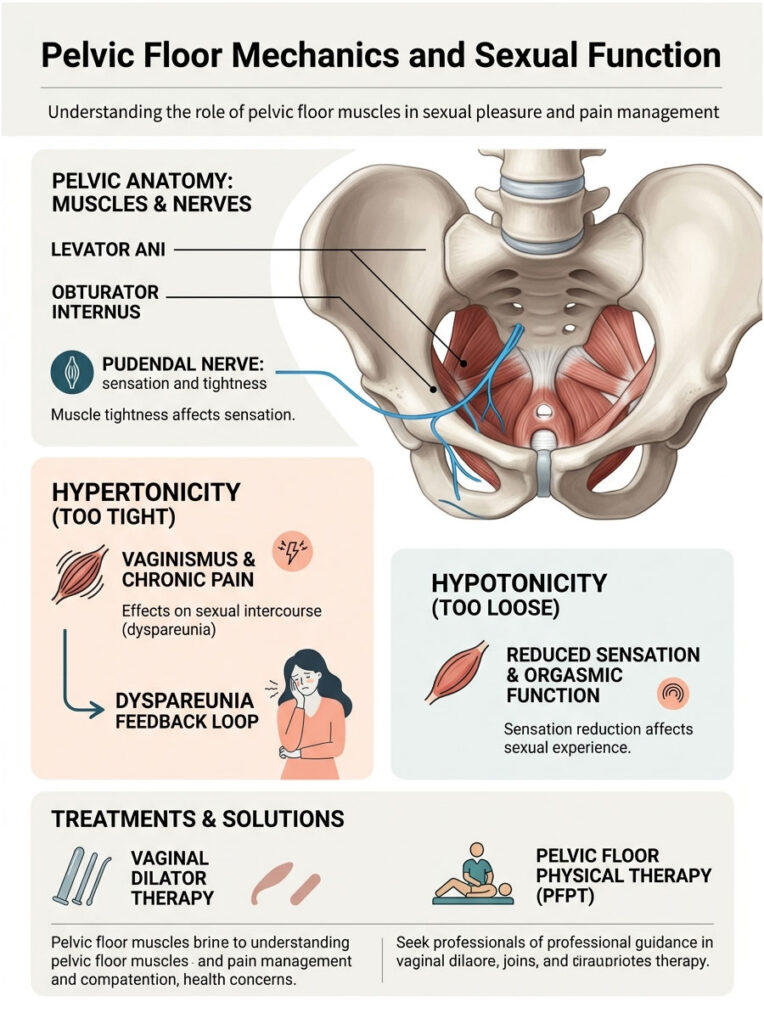
Pelvic Anatomy Basics
The pelvic floor consists of several muscle groups, including the levator ani and obturator internus. They wrap around the urethra, vagina, and rectum like a supportive sling, maintaining continence, supporting organs against gravity, and facilitating sexual function.
The pudendal nerve runs directly through this muscle group, supplying sensation to the clitoris, vulva, and perineum. If surrounding muscles are too tight, they can compress this nerve, causing numbness, shooting pains, or a persistent burning sensation during sex.
Hypertonicity vs. Hypotonicity
A hypertonic pelvic floor is chronically too tight and cannot relax enough for painless penetration. This is the primary driver behind vaginismus, where vaginal muscles spasm involuntarily. Hypertonicity is often caused by chronic stress, previous pelvic trauma, or high-impact athletic training.
Hypotonicity is the opposite: muscles that are too loose or weak, often from childbirth, chronic heavy lifting, or estrogen loss. Hypotonic muscles reduce physical sensation, limit friction during intercourse, and weaken orgasms, since orgasms are essentially rhythmic contractions of these muscles.
Breaking the Dyspareunia Cycle
Dyspareunia creates a powerful feedback loop. When sex hurts, the brain anticipates pain the next time. The nervous system commands the pelvic floor to tighten defensively, which guarantees the next experience will also be painful. Breaking this loop is essential.
Vaginal dilator therapy is a highly effective, evidence-based treatment for vaginismus. Dilators are medical devices used progressively to train pelvic floor muscles to stretch and relax without pain. Paired with diaphragmatic breathing, this therapy teaches the brain that penetration is safe, effectively rewiring the pain response over time.
Pelvic Floor Physical Therapy (PFPT)
A specialized pelvic floor physical therapist assesses muscle tone internally and externally. They do not simply hand out a generic Kegel sheet. If you have a hypertonic pelvic floor, doing Kegels will actually make your pain worse.
PFPT uses advanced manual release techniques, biofeedback, and targeted stretching to restore proper function. Clinical trials from the American Physical Therapy Association show that consistent training improves orgasmic function in roughly 65% to 70% of compliant patients.
Holistic Wellness: Nutrition, Probiotics, and Lifestyle
Your sexual organs do not operate in isolation. They are deeply connected to overall systemic health. What you eat, the supplements you take, and the environmental chemicals you are exposed to all influence intimate vitality.

Targeted Probiotics for Vaginal Health
The gut-vagina axis is a well-documented medical pathway. Oral or vaginal probiotics containing Lactobacillus crispatus, Lactobacillus rhamnosus, and Lactobacillus reuteri have been shown to migrate from the gut to the vaginal tract, where they colonize tissue and produce protective lactic acid.
Oral probiotics work well for ongoing daily maintenance. Vaginal probiotic suppositories offer a direct, rapid intervention during active dysbiosis.
Avoiding Endocrine Disruptors
Many personal care products, cosmetics, and plastic food containers contain endocrine-disrupting chemicals (EDCs). The most common offenders are phthalates, parabens, and Bisphenol A (BPA). These chemicals are structurally similar to your natural hormones and can mimic estrogen, sending false signals to cellular receptors, or block your natural estrogen from binding altogether.
This interference causes measurable hormonal imbalances, irregular cycles, lowered libido, and poor tissue elasticity. Reading labels and choosing paraben-free, phthalate-free products is essential for maintaining hormonal balance.
Nutritional Support for Hormonal Health
Your endocrine system needs healthy fats, particularly omega-3 fatty acids, to synthesize sex hormones. Omega-3s also regulate systemic inflammation, directly improving pelvic blood flow. Zinc supports healthy testosterone production, while magnesium helps relax both the nervous system and pelvic floor muscles.
Certain adaptogenic herbs show strong clinical evidence for libido support. Ashwagandha actively lowers cortisol, preventing the pregnenolone steal. Maca root has been shown in double-blind studies to support sexual desire, particularly in women with SSRI-induced dysfunction.
Clinical Interventions: When to See a Specialist
Lifestyle, hygiene, and nutrition are powerful tools, but sometimes they are not enough. Modern medicine has evolved significantly in treating female sexual dysfunction, with targeted therapies that address root causes of pain and low desire.

Screening for HSDD
It is normal for desire to fluctuate with your cycle, stress levels, or relationship dynamics. But when persistent low desire causes you significant personal distress, it crosses into clinical territory. This condition is Hypoactive Sexual Desire Disorder (HSDD), diagnosed using DSM-5 criteria. The key differentiator between a normal dry spell and HSDD is the element of profound distress. A diagnosis validates your experience as a recognized medical condition with viable treatments.
FDA-Approved Therapies
For severe GSM, prescription options like DHEA vaginal inserts (Prasterone) or oral selective estrogen receptor modulators (SERMs like Ospemifene) can rebuild vaginal tissue without exposing the entire body to systemic estrogen.
For premenopausal women with HSDD, neuromodulating medications are available. Flibanserin is a daily pill, while Bremelanotide is an as-needed auto-injector. Both work on brain neurotransmitter pathways, balancing dopamine and serotonin to restore desire. They are not magic pills, but they offer significant relief for neurologically based HSDD.
Emerging Regenerative Therapies
Fractional CO2 vaginal lasers are becoming a popular treatment for severe GSM. These painless lasers create microscopic injuries in vaginal mucosa, stimulating a healing response that produces fresh collagen and elastin.
Platelet-Rich Plasma (PRP) therapy, sometimes called the O-Shot, involves isolating growth factors from your own blood and injecting them near the clitoris and anterior vaginal wall. While large-scale data is still growing, many patients report increased sensitivity and natural lubrication.
Red Flags Requiring Immediate Medical Evaluation
- Unexplained sharp pelvic pain during or immediately after intercourse.
- Bleeding after sex (postcoital bleeding), which requires a cervical exam.
- Chronic vaginal itching, burning, or abnormal discharge that does not resolve with standard treatments.
- A sudden, distressing drop in libido that severely affects daily mental health.
- A sensation of bulging or heaviness in the vagina, which may indicate pelvic organ prolapse.
Summary and Key Takeaways
Understanding how your body functions is a lifelong journey that requires patience, education, and proactive care. You do not have to accept chronic pain or declining desire as permanent.
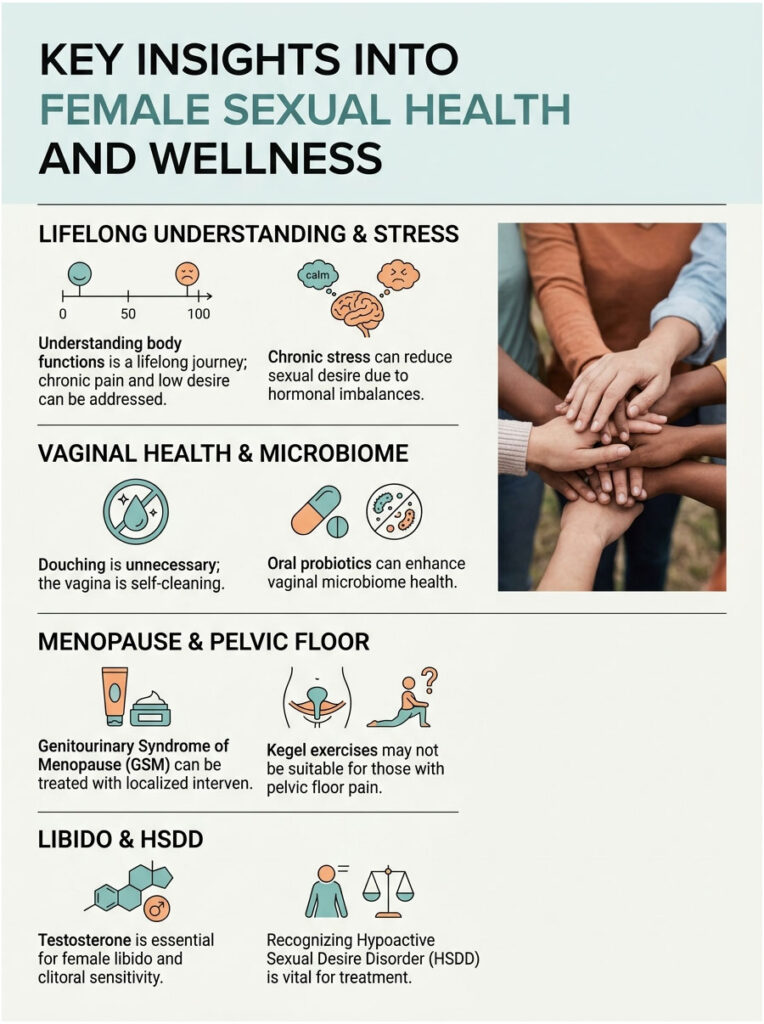
- Support Your Hormones: Hormonal balance protects tissue integrity and drives natural desire. Do not ignore early signs of GSM.
- Protect Your Microbiome: Maintain your lactic acid mantle by avoiding douching. Use gentle hygiene and targeted probiotics.
- Strengthen Your Pelvic Floor: Optimal pelvic floor mechanics prevent dyspareunia and enhance physical pleasure.
- Manage Stress: Protect your endocrine system from the cortisol steal. Keep your nervous system in a receptive, parasympathetic state.
- Seek Expert Help: If you suspect HSDD or severe tissue atrophy, consult a specialist. FDA-approved interventions are available.
Female sexual dysfunction prevention is entirely possible when you treat your body with the respect and scientific care it deserves. Prioritize your holistic health daily, and you will maintain sexual health and vitality for a lifetime.
Frequently Asked Questions
Why does chronic stress significantly decrease female sexual desire?
As an OB-GYN, I often explain this through the ‘pregnenolone steal’ phenomenon. When you are under chronic stress, your endocrine system prioritizes the production of cortisol, the primary stress hormone, over sex hormones like estrogen and testosterone. This biological survival mechanism shunts blood flow away from the pelvic organs and blunts the brain’s desire centers, making physical arousal physiologically difficult.
Is douching necessary to maintain proper vaginal hygiene?
Absolutely not. The vagina is a self-cleaning organ that relies on a delicate acidic environment. Clinical data from the CDC shows that douching increases the risk of Pelvic Inflammatory Disease (PID) by 73% because it flushes away protective Lactobacillus and forces pathogens higher into the reproductive tract. For external hygiene, warm water or a strictly pH-balanced, fragrance-free cleanser is the medical gold standard.
What is Genitourinary Syndrome of Menopause (GSM) and how is it managed?
GSM is a chronic condition caused by a decline in estrogen, leading to thinning of the vaginal walls, decreased lubrication, and urinary urgency. Unlike systemic menopause symptoms, GSM usually requires localized intervention. Treatment options include low-dose vaginal estrogen (creams, rings, or inserts), DHEA suppositories, or non-hormonal hyaluronic acid moisturizers to restore tissue integrity and comfort.
Can oral probiotics actually improve my vaginal microbiome health?
Yes, through the gut-vagina axis. Specific, clinically-backed strains such as Lactobacillus crispatus, L. rhamnosus, and L. reuteri can migrate from the digestive tract to colonize the vaginal environment. These beneficial bacteria produce lactic acid and hydrogen peroxide, which maintain an acidic pH between 3.8 and 4.5, effectively preventing dysbiosis and recurrent Bacterial Vaginosis (BV).
Should I perform Kegels if I experience pain during intercourse?
Not necessarily. If your pain is caused by a hypertonic (overly tight) pelvic floor, performing Kegels can actually exacerbate the condition by increasing muscle tension. For patients with dyspareunia or vaginismus, we typically recommend Pelvic Floor Physical Therapy (PFPT) focusing on manual release and down-training exercises rather than strengthening, to help the muscles learn to relax for comfortable penetration.
What role does testosterone play in female sexual wellness?
While often labeled a male hormone, testosterone is vital for women’s libido and clitoral sensitivity. It acts directly on the androgen receptors in the brain to drive spontaneous sexual thoughts and fantasies. When levels drop due to aging, surgical menopause, or certain contraceptives, women may experience a ‘flatlining’ of desire and decreased orgasmic intensity, which can sometimes be addressed through supervised androgen therapy.
How do I know if my low libido is actually Hypoactive Sexual Desire Disorder (HSDD)?
The clinical diagnosis of HSDD hinges on the presence of persistent low desire that causes significant personal or relational distress. If your lack of interest in intimacy is a source of anxiety or emotional pain, it moves beyond a ‘normal dry spell’ into a treatable medical condition. We utilize the DSM-5 criteria and tools like the Decreased Sexual Desire Questionnaire (DSDQ) to screen for this disorder.
Why is the ‘lactic acid mantle’ so important for preventing infections?
The lactic acid mantle is the primary chemical barrier of the vagina. When Lactobacillus bacteria metabolize glycogen from vaginal cells into lactic acid, they create a highly acidic environment (pH <4.5). This acidity is toxic to most pathogenic bacteria and yeast. If this mantle is disrupted by alkaline semen, antibiotics, or harsh soaps, the pH rises, allowing opportunistic infections like BV or candidiasis to take hold.
What are endocrine disruptors and how do they affect my intimate health?
Endocrine-disrupting chemicals (EDCs), such as phthalates and parabens found in many scented personal care products, are synthetic compounds that mimic or block your natural hormones. Because they can bind to estrogen receptors, they can cause hormonal imbalances that lead to irregular cycles, decreased vaginal lubrication, and lowered libido by interfering with your body’s endogenous signaling.
How does Dr. Rosemary Basson’s non-linear model change our understanding of arousal?
Unlike older linear models, Basson’s model recognizes that many women experience ‘responsive desire.’ This means they may start from a point of sexual neutrality and only experience arousal and desire after physical stimulation has begun. Understanding this model helps patients realize that a lack of spontaneous ‘hunger’ for sex isn’t a dysfunction, but a common and normal biological variation.
What are the benefits of fractional CO2 laser therapy for vaginal health?
Fractional CO2 lasers are a regenerative medical intervention used to treat severe vaginal atrophy and GSM. The laser creates microscopic thermal zones in the tissue, which triggers a natural healing response and stimulates the production of new collagen and elastin. This helps restore the thickness and elasticity of the vaginal mucosa without the need for systemic hormone replacement therapy.
When is postcoital bleeding considered a medical emergency?
While not always an emergency, any bleeding after intercourse (postcoital bleeding) must be evaluated by an OB-GYN promptly. It can be a symptom of benign issues like cervical polyps or vaginal dryness, but it is also a primary red flag for cervical dysplasia or infection. A physical exam and often a Pap smear or HPV test are required to rule out more serious underlying pathology.
Disclaimer
This article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. The "Quick Answer" and guide content are based on clinical experience and general guidelines. Always consult with a Board-Certified OB-GYN or a qualified healthcare professional before starting any new supplement, medication, or physical therapy regimen. Never disregard professional medical advice because of something you have read in this guide.
References
- The Journal of the American Medical Association (JAMA) - Prevalence of Sexual Dysfunction in Women - Source for statistics regarding the 43.5% rate of female sexual dysfunction.
- North American Menopause Society (NAMS) - 2022 Position Statement on GSM - Authoritative guidelines on Genitourinary Syndrome of Menopause and estrogen therapy.
- Centers for Disease Control and Prevention (CDC) - Vaginal Hygiene and PID Risk - Source for the 73% increased risk of Pelvic Inflammatory Disease associated with douching.
- American College of Obstetricians and Gynecologists (ACOG) - Clinical Consensus on Female Sexual Dysfunction - Evidence-based definitions of HSDD and arousal disorders.
- American Physical Therapy Association (APTA) - Pelvic Health Guidelines - Data regarding the 65-70% improvement rate in orgasmic function through physical therapy.
- Dr. Rosemary Basson - The Non-Linear Model of Sexual Response - The foundational medical model for modern female arousal and responsive desire.








