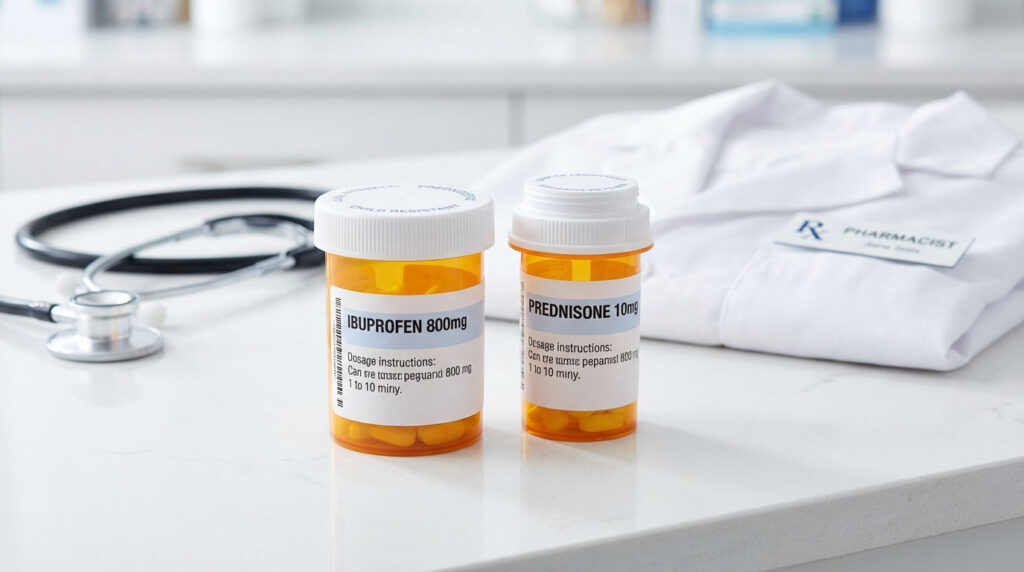
Generally, no. Taking ibuprofen and prednisone together is clinically considered unsafe due to synergistic toxicity. This combination significantly increases your risk of severe gastrointestinal bleeding, peptic ulcers, and acute kidney injury. Unless a specialist has specifically prescribed and is monitoring both medications with protective measures in place, you should avoid this combination.
Table of Contents
As a pharmacist, there’s one drug interaction alert that pops up on my screen more often than almost any other. A patient walks in to pick up a steroid pack for a bad back or a severe allergic reaction. They’re uncomfortable and looking for fast relief. Then comes the question I hear all the time: “I’m in a lot of pain. Can I take Advil with this?”
The short answer is no. While both drugs are powerful inflammation fighters, mixing ibuprofen and prednisone creates a biochemical conflict that strips your stomach of its natural defenses. This isn’t just about a stomach ache. It’s about the real risk of eroding the stomach lining to the point of a life-threatening bleed.

In this guide, I’ll walk you through exactly why this combination is dangerous, the biological mechanisms behind the damage, and the specific risk factors that make some patients more vulnerable. Most importantly, I’ll show you how to safely manage your pain using the “Tylenol Bridge” method while you’re on steroids.
Key Statistics on the Risks of Combining NSAIDs and Steroids
- 12x Risk Increase: Patients taking NSAIDs and steroids together face a substantially higher risk of peptic ulcer disease compared to taking either drug alone.
- 100,000+ Hospitalizations: GI complications from NSAIDs account for over 100,000 hospitalizations annually in the US.
- 20%+ Kidney Function Drop: Concurrent use can reduce glomerular filtration rate by over 20% in susceptible individuals within days.
- 3x Higher Risk for Seniors: Patients over 65 are three times more likely to experience a GI bleed from this combination.
- 60% Silent Damage: Approximately 60% of NSAID-induced ulcers show no symptoms until a serious bleeding event occurs.
The Pharmacological Conflict: Why Ibuprofen and Prednisone Don’t Mix
To understand why taking ibuprofen and prednisone at the same time is dangerous, you need to see what’s happening at a cellular level. Both drugs target inflammation, but they attack the same chemical pathway at different points. The result is a “double hit” to your body’s protective systems.
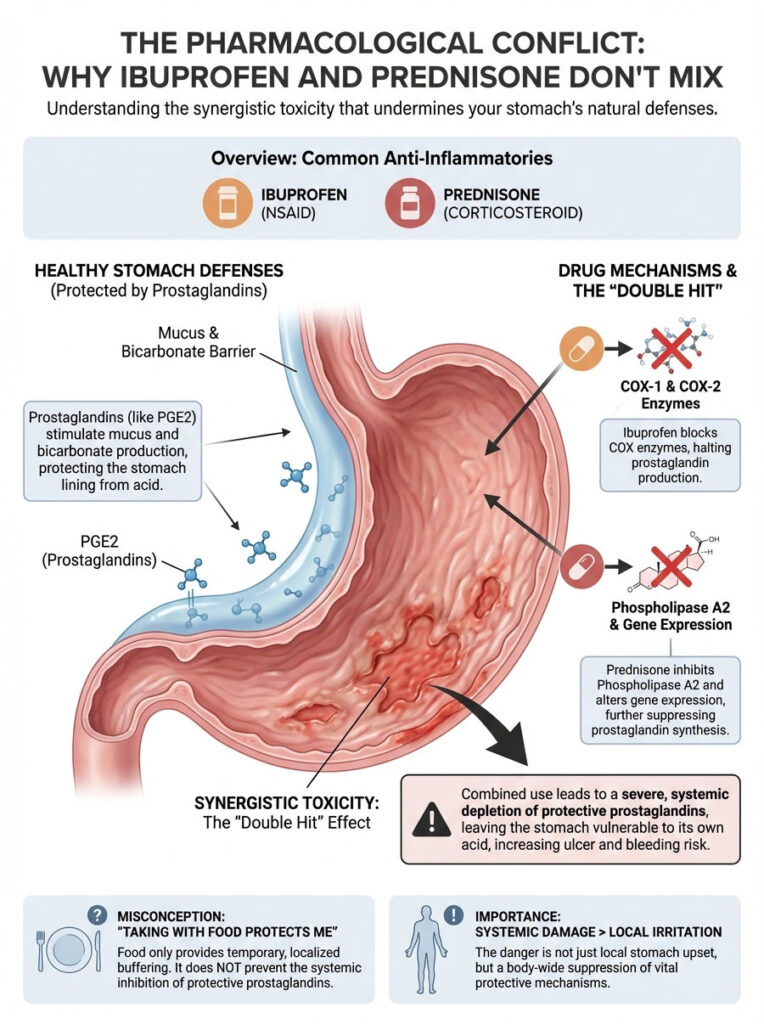
How Your Stomach Lining Protects Itself
Your stomach contains strong hydrochloric acid that’s essential for digestion. The only reason this acid doesn’t digest the stomach itself is a protective layer of mucus and bicarbonate. This layer is regulated by chemical messengers called prostaglandins, specifically prostaglandin E2 (PGE2).
Think of prostaglandins as the maintenance crew. They constantly signal the stomach wall to produce thick mucus and bicarbonate, which neutralizes acid near the lining. Without prostaglandins, the maintenance crew goes on strike and the protective wall starts crumbling.
How Ibuprofen Attacks Stomach Defenses
Ibuprofen is a Nonsteroidal Anti-Inflammatory Drug (NSAID). It works by blocking enzymes called COX-1 and COX-2:
- COX-2 drives pain and inflammation. Blocking it is the whole point, and that’s where your relief comes from.
- COX-1 maintains the stomach lining and kidney blood flow. This is the target we want to avoid hitting.
Because ibuprofen is a non-selective NSAID, it blocks both enzymes. It stops the pain, but it also shuts down the production of protective stomach mucus.
How Prednisone Weakens the Stomach from a Different Angle
Prednisone is a corticosteroid that works much higher up the biological chain. It enters the cell nucleus and changes gene expression. Specifically, it inhibits a protein called Phospholipase A2, which blocks the production of arachidonic acid. That’s the raw material your body needs to make prostaglandins in the first place.
Synergistic Toxicity: The “Double Hit” Effect
Here’s what makes this interaction so dangerous. When you take ibuprofen and prednisone together, you’re creating synergistic toxicity. The danger isn’t just additive. It’s exponential.
Prednisone weakens the structural integrity of the stomach tissue and slows its natural healing process. Ibuprofen strips away the protective mucus layer. You’re essentially removing the shield (ibuprofen) while simultaneously making the wall behind it weaker (prednisone). This leaves the gastric mucosa completely exposed to harsh stomach acid, leading to rapid erosion.
Pharmacist Insight: Many patients believe that having a “strong stomach” or taking the pills with food keeps them safe. This is a misconception. The damage is systemic, meaning it happens through the bloodstream, not just because the pill is sitting in your stomach. Food buffers the acid slightly, but it doesn’t stop the chemical inhibition of prostaglandins.
Health Risks and Complications of Combining Ibuprofen and Prednisone
The risks of mixing NSAIDs and steroids fall into three main categories: gastrointestinal injury, kidney impairment, and cardiovascular strain. Each system takes damage differently.
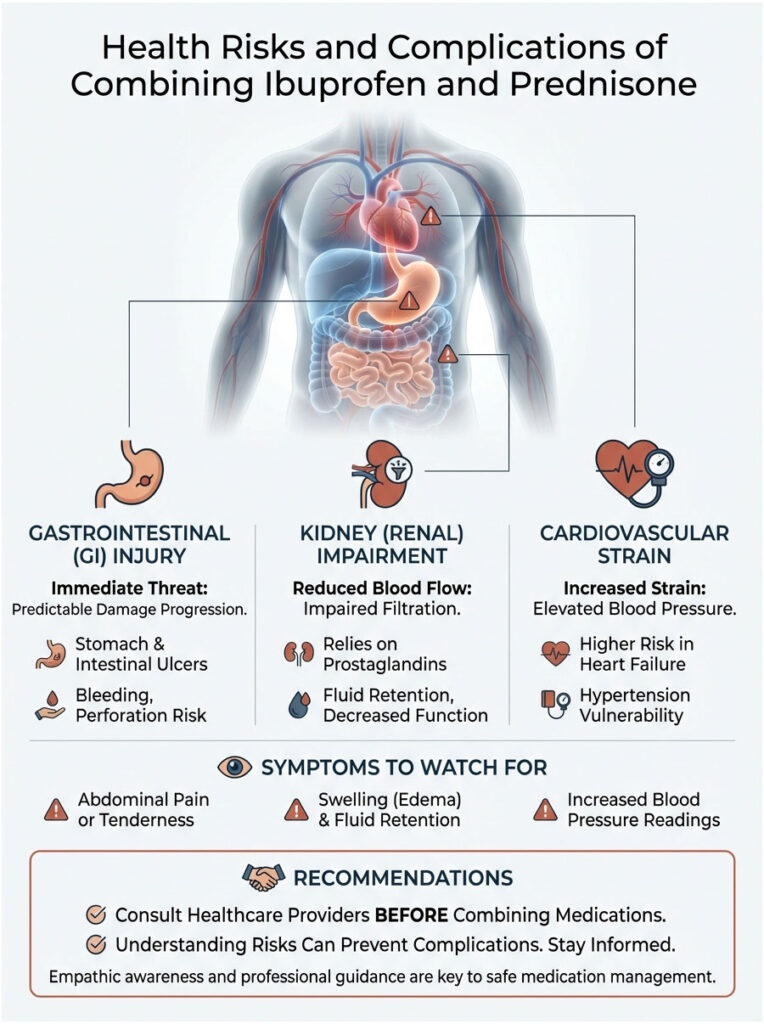
Gastrointestinal (GI) Injury
This is the most immediate and common threat. Damage can progress faster than most people expect, and it often follows a predictable pattern:
- Gastritis and Erosion: Within days of dual therapy, the stomach lining becomes inflamed. You might feel a gnawing hunger pain or persistent heartburn. This is your first warning sign.
- Peptic Ulcer Disease (PUD): As acid eats into unprotected tissue, an open sore forms. Because steroids mask pain, you may not even feel the ulcer forming. That’s the dangerous part: you lose the pain signal that would normally tell you to stop.
- GI Bleeding: If the ulcer hits a blood vessel, it creates a gastrointestinal bleed. This is a medical emergency that can lead to significant blood loss very quickly.
- GI Perforation: In severe cases, the ulcer burns a hole completely through the stomach wall. Bacteria and acid leak into the abdominal cavity, causing peritonitis and sepsis. This requires emergency surgery.
Kidney (Renal) Impairment
Your kidneys rely on prostaglandins to keep their blood vessels (afferent arterioles) dilated and open. This ensures adequate blood flow for filtration.
- Hemodynamic Effect: Ibuprofen constricts these blood vessels, like stepping on a garden hose. Prednisone causes fluid retention and disrupts electrolyte balance.
- Acute Kidney Injury (AKI): When combined, blood flow to the kidneys can drop sharply. This is especially dangerous for patients who are dehydrated, taking diuretics (water pills), or already have high blood pressure.
Cardiovascular Strain
Steroids naturally cause your body to hold onto sodium and water, which raises blood pressure. NSAIDs also raise blood pressure by altering kidney function. Combining them puts significant strain on the heart, increasing the risk of cardiovascular events in patients with a history of heart failure or hypertension.
Mechanism of Action Comparison: Ibuprofen vs. Prednisone
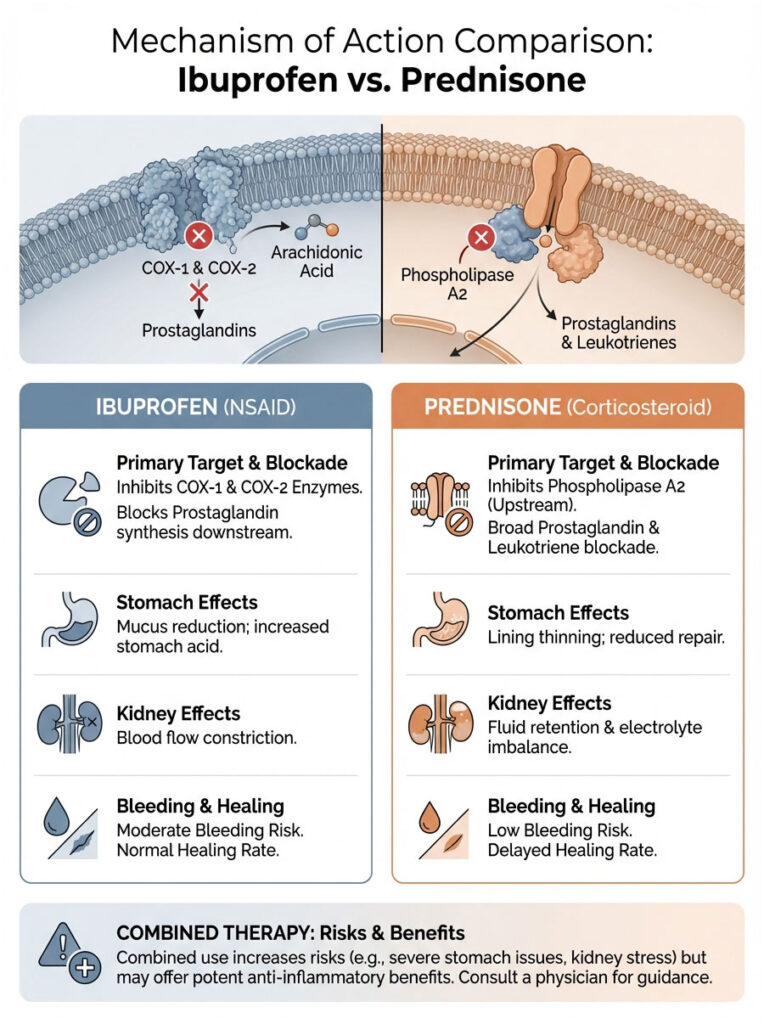
| Feature | Ibuprofen (NSAID) | Prednisone (Steroid) | Combined Therapy |
| Primary Target | COX-1 and COX-2 Enzymes | Phospholipase A2 (Gene expression) | Total Prostaglandin Blockade |
| Stomach Effect | Reduces protective mucus | Thins lining; delays healing | Rapid ulceration and bleeding |
| Kidney Effect | Constricts blood flow | Increases fluid retention | Acute renal failure risk |
| Bleeding Risk | Moderate (anti-platelet) | Low (by itself) | Severe / High |
| Healing Rate | Normal | Delayed | Severely compromised |
The “Tylenol Bridge”: A Safer Way to Manage Pain on Steroids
If you’re in pain, simply being told “don’t take Advil” isn’t helpful. You need a real strategy. That’s where the “Tylenol Bridge” comes in. It’s a method for managing breakthrough pain without putting your stomach and kidneys at risk.
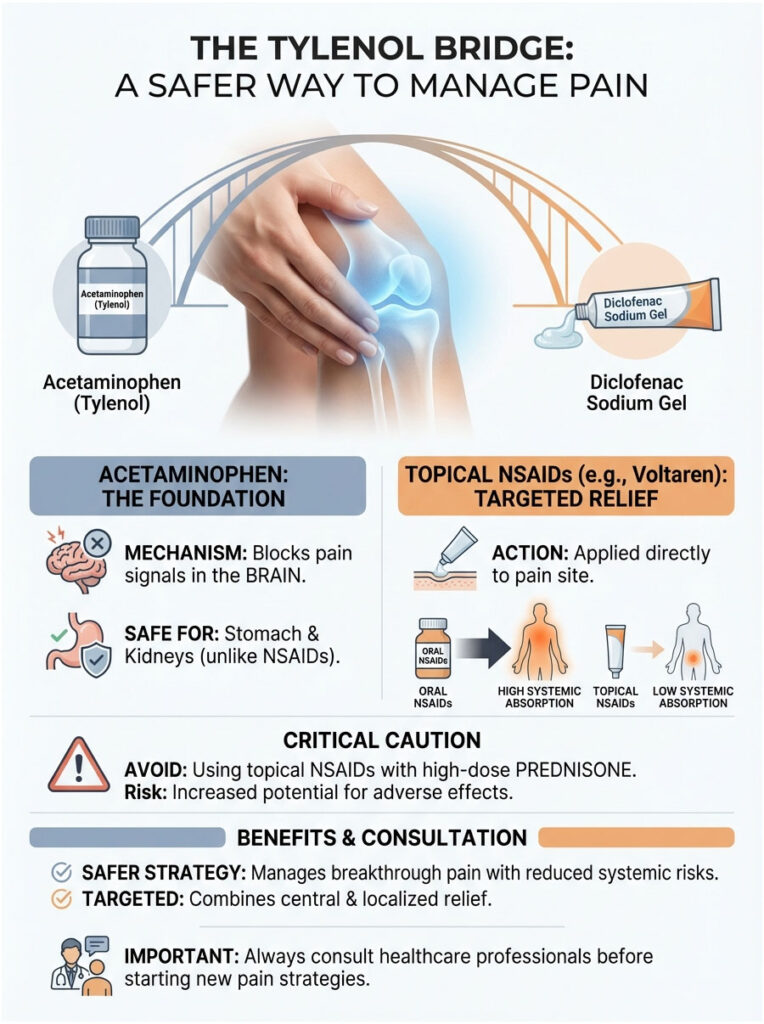
Why Acetaminophen (Tylenol) Is Different
Acetaminophen is a pain reliever and fever reducer, but it is not an NSAID. It works in the brain to block pain signals rather than attacking inflammation at the injury site. Because it has practically no effect on COX-1 enzymes in the stomach or kidneys, it doesn’t strip away your stomach lining or constrict kidney blood vessels.
The Protocol
- Stick to the Steroid Schedule: Continue your prednisone exactly as prescribed. Never skip doses or stop abruptly, as this can trigger adrenal crisis.
- Use Acetaminophen for Breakthrough Pain: Most healthy adults can take 500mg to 1,000mg of acetaminophen every 6 hours. Do not exceed 3,000mg to 4,000mg in a 24-hour period. Check with your doctor if you have any liver concerns.
- Add Non-Drug Methods: Ice packs work well for acute swelling. Heat pads help with muscle stiffness. These physical interventions complement the medication without adding chemical load to your body.
Topical NSAIDs: The Partial Exception
There is one potential workaround worth knowing about: Diclofenac Sodium Gel (Voltaren). This is a topical NSAID applied directly to the skin.
While oral NSAIDs have 100% systemic absorption, topical gels absorb at significantly lower rates, often around 6%. Most of the drug stays in the knee or joint where you applied it, so less reaches the stomach lining. However, “safer” does not mean “risk-free.” If you’re on a high dose of prednisone, clear the use of Voltaren gel with your doctor first.
When Do Doctors Actually Prescribe Both Together?
You may be thinking, “But my rheumatologist put me on both ibuprofen and prednisone.” It does happen, but only under very specific, controlled circumstances. It’s not standard practice for general pain.
The Rheumatoid Arthritis and Lupus Context
In severe autoimmune diseases like Rheumatoid Arthritis or Lupus, inflammation can be destructive enough to permanently damage joints and organs. In those cases, the benefit of aggressive inflammation control may outweigh the risks. A specialist will prescribe both to bring a massive flare-up under control quickly.
The Gastroprotection Strategy
When doctors do prescribe this combination, they almost always add a “shield” for the stomach. This typically comes in the form of a Proton Pump Inhibitor (PPI) like Omeprazole (Prilosec) or Pantoprazole (Protonix).
PPIs drastically reduce the amount of acid your stomach produces. By turning down the acid volume, the risk of acid eating through the weakened lining decreases. But this is a prescription-level strategy. You should never try to “DIY” this combination by buying over-the-counter PPIs and hoping for the best. The risk of GI bleed remains elevated even with protection.
Washout Periods: How Long to Wait Between Medications
One of the most common questions I hear is about timing: “I finished my steroid pack yesterday. Can I take ibuprofen today?” This is what we call a washout period, and it matters a lot for safety.

Switching from Prednisone to Ibuprofen
Prednisone has a biological half-life, meaning it stays in your system for a while after the last dose. More importantly, the biological effects on your stomach lining can persist even after the drug has cleared.
Recommendation: Wait at least 24 to 48 hours after your last dose of prednisone before resuming NSAIDs. This gives your body time to restart prostaglandin production and allows the mucosal barrier to begin repairing.
Tapering Note: If you’re on a taper (gradually reducing the dose over days), you are still taking the medication. Do not take ibuprofen during the taper. The risk is still present.
Switching from Ibuprofen to Prednisone
Ibuprofen has a much shorter half-life of about 2 hours. It clears the system relatively fast.
Recommendation: It’s usually considered safe to start a course of prednisone 12 to 24 hours after your last dose of ibuprofen. Since the steroid takes time to start weakening the stomach lining, ibuprofen will likely be fully eliminated before the steroid effects peak.
Emergency Symptom Checker: When to Call 911
If you’ve accidentally taken ibuprofen and prednisone together, or if you’re on a prescribed dual therapy, stay vigilant. GI bleeding can start subtly and then become catastrophic.
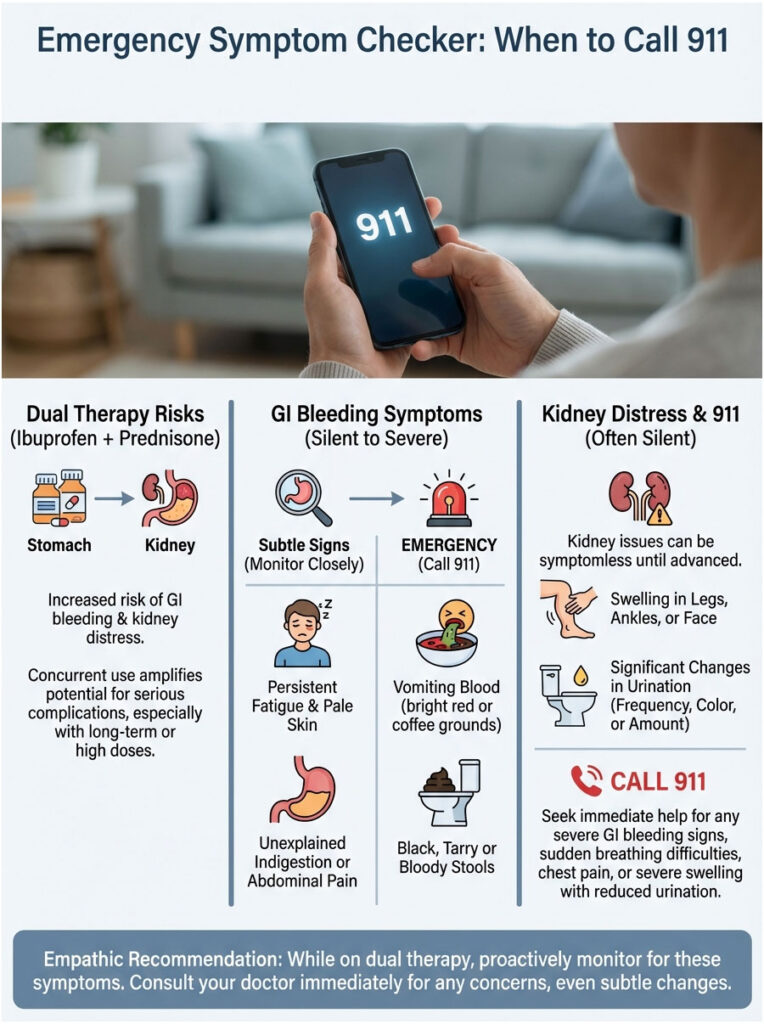
Signs of a GI Bleed
- Melena: Black, tarry, sticky stools with a distinct foul metallic smell. This indicates blood is being digested in the upper GI tract. It looks like road tar, not just dark stool.
- Hematemesis: Vomiting blood. It may look bright red (fresh blood) or resemble “coffee grounds” (older blood that has been exposed to stomach acid).
- Orthostatic Hypotension: Feeling dizzy, lightheaded, or faint when standing up quickly. This can signal internal blood loss.
Signs of Kidney Distress
Kidney injury is often silent, but you can watch for these changes:
- Noticeable decrease in urine output
- Dark, concentrated, or “cola-colored” urine
- Sudden, severe swelling (edema) in the ankles, feet, or legs
Dietary and Lifestyle Factors That Increase Risk
When managing inflammation with steroids, what you eat and drink matters. Certain substances can make stomach injury worse, while others can help reduce side effects.
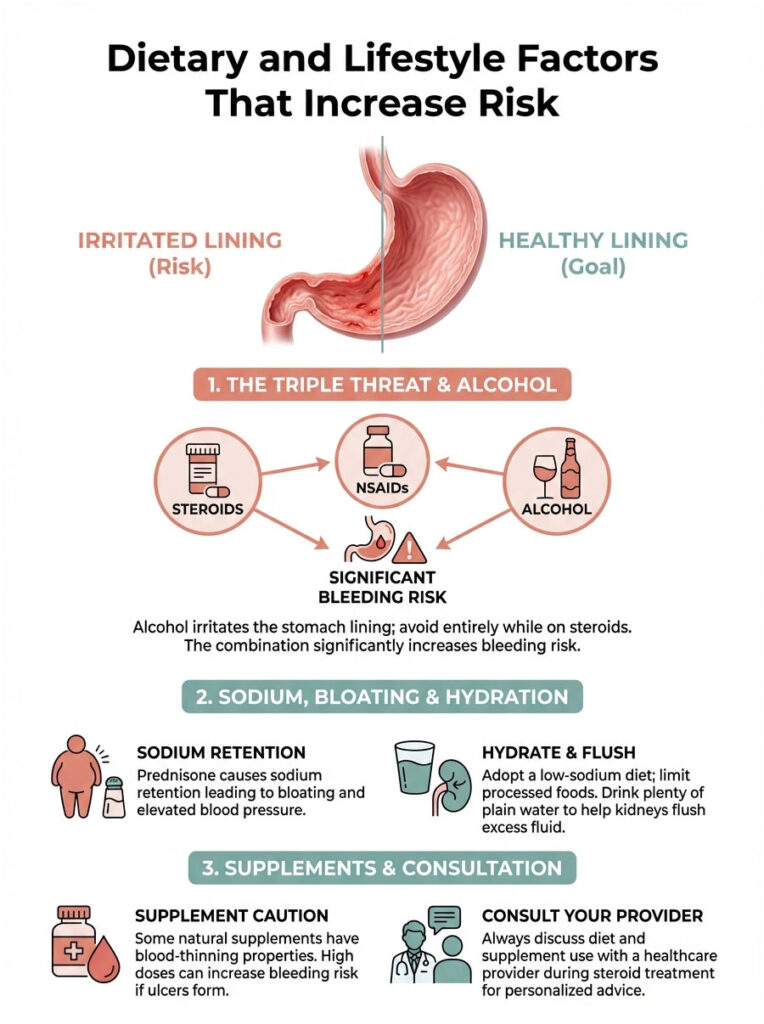
The Alcohol Danger
Alcohol directly irritates the stomach lining on contact. Combining alcohol with prednisone adds a third factor to the injury equation, sometimes called the “Triple Threat” (steroids + NSAIDs + alcohol). The bleeding risk goes through the roof. Avoid all alcohol while on a steroid course and for at least 48 hours after finishing the medication.
Salt and Fluid Retention
Prednisone causes the kidneys to hold onto sodium, and water follows sodium. This leads to bloating and elevated blood pressure. NSAIDs also cause sodium retention. To minimize this effect, adopt a low-sodium diet during treatment. Cut back on processed foods, canned soups, and salty snacks. Drink plenty of plain water to help your kidneys flush out excess fluid.
Supplements to Watch Out For
Some natural supplements have blood-thinning properties that can increase bleeding risk if an ulcer forms. Be cautious with high doses of:
- Garlic supplements
- Ginkgo Biloba
- Ginseng
- Vitamin E (in very high doses)
Frequently Asked Questions: Real Patient Scenarios
In the pharmacy, patients constantly bring up specific scenarios. Here are detailed answers to the questions I hear most often.

Can I take 200mg of ibuprofen with prednisone if I eat a big meal?
No. Eating a large meal buffers stomach acid temporarily, but it doesn’t prevent the systemic absorption of the drugs. Once ibuprofen enters your bloodstream, it inhibits COX enzymes throughout your body, shutting down protective mucus production. The risk of stomach lining damage remains even with a full stomach. Food helps with nausea, but it does not prevent ulcers.
I accidentally took one ibuprofen while on prednisone. Will I get an ulcer?
Don’t panic. A single accidental dose is rarely catastrophic in an otherwise healthy person. The risk builds with repeated doses. Stop the ibuprofen immediately and switch to acetaminophen. Monitor yourself for any stomach pain or indigestion over the next 24 hours, and drink plenty of water to help clear the medication.
Is Aleve (Naproxen) safer than ibuprofen with steroids?
Actually, it may be worse. Naproxen has a longer half-life than ibuprofen, which means it suppresses prostaglandin production for a longer duration. That prolonged suppression, combined with steroids, sustains the risk of a GI bleed. Avoid all NSAIDs while on steroids, including naproxen and high-dose aspirin.
Can I take baby aspirin (81mg) with prednisone?
This comes up frequently with heart patients. Generally, doctors will advise you to continue your 81mg aspirin for heart protection. However, they may add a Proton Pump Inhibitor (PPI) to protect your stomach during the steroid course. Don’t stop your heart medication without consulting your doctor, but do ask whether you need stomach protection.
Does prednisone make ibuprofen stronger?
No. It doesn’t make the pain relief stronger. It makes the side effects stronger. That’s the definition of synergistic toxicity. You get zero added benefit in pain reduction. You only get added risk of harm.
Quick Reference: Safe vs. Unsafe Drug Combinations with Prednisone
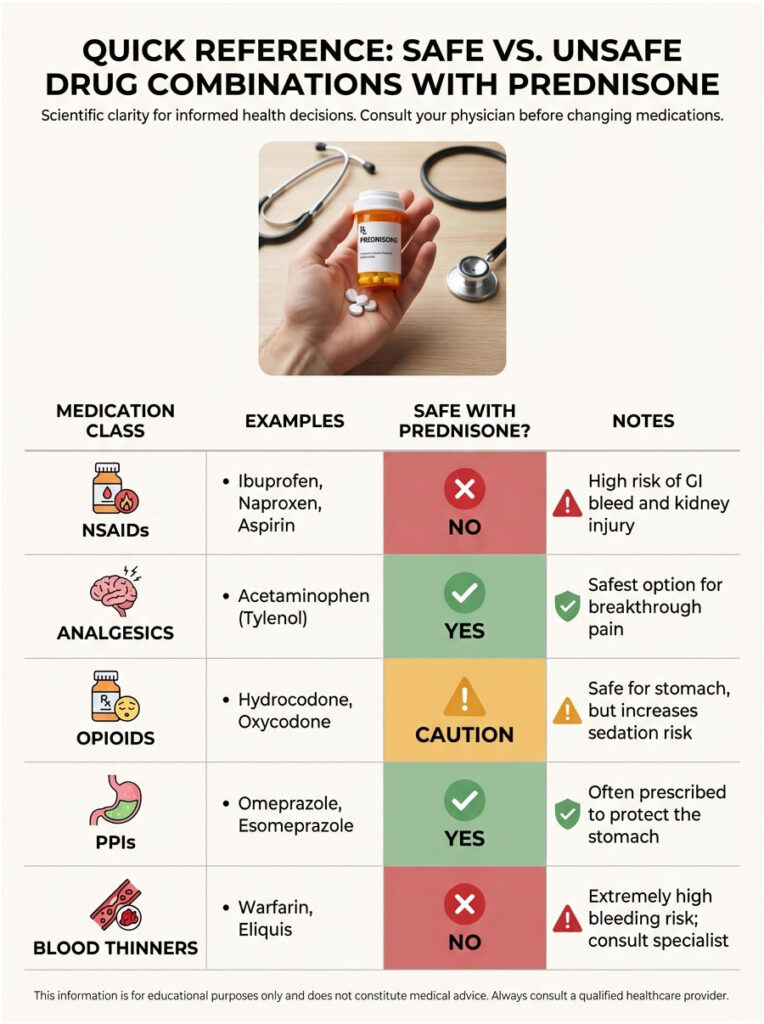
| Medication Class | Examples | Safe with Prednisone? | Notes |
| NSAIDs | Ibuprofen, Naproxen, Aspirin | NO | High risk of GI bleed and kidney injury |
| Analgesics | Acetaminophen (Tylenol) | YES | Safest option for breakthrough pain |
| Opioids | Hydrocodone, Oxycodone | CAUTION | Safe for stomach, but increases sedation risk |
| PPIs | Omeprazole, Esomeprazole | YES | Often prescribed to protect the stomach |
| Blood Thinners | Warfarin, Eliquis | NO | Extremely high bleeding risk; consult specialist |
Summary and Key Takeaways
Navigating medication interactions can be confusing. But when it comes to ibuprofen and prednisone, the rules are fairly rigid for a very good reason: the safety of your stomach and kidneys. The synergistic toxicity created by these two drugs removes your body’s natural defenses and turns a standard dose of medication into a potential medical emergency.

The Bottom Line:
- Avoid the Mix: Do not take NSAIDs (Advil, Motrin, Aleve) while on oral steroids. The bleeding risk is too high.
- Use the Bridge: Rely on Acetaminophen (Tylenol) for pain relief during your steroid course. It’s effective and safe for the stomach.
- Watch for Warning Signs: Black tarry stools or “coffee ground” vomit require immediate emergency care. Don’t wait to see if it goes away.
- Protect Your Kidneys: Stay hydrated. But know that hydration alone doesn’t eliminate the risk of kidney problems if you combine these drugs.
- Respect the Washout: Wait 24 to 48 hours after your last steroid dose before resuming ibuprofen.
Always consult your pharmacist or physician before adding any over-the-counter medication to a prescription regimen. Your safety depends on respecting the chemistry of these powerful drugs.
Frequently Asked Questions
Why is it clinically unsafe to take ibuprofen and prednisone at the same time?
Combining these medications creates synergistic toxicity, where the risk of injury is significantly higher than taking either drug alone. Prednisone weakens the structural integrity of the gastric mucosa, while ibuprofen inhibits the prostaglandins responsible for producing protective stomach mucus, leaving the lining vulnerable to severe acid erosion.
What are the warning signs of a gastrointestinal bleed when mixing steroids and NSAIDs?
Patients should be vigilant for melena, which is the passage of black, tarry, and foul-smelling stools indicating digested blood. Other critical symptoms include hematemesis (vomiting blood or coffee-ground material) and orthostatic hypotension, which manifests as sudden dizziness or lightheadedness when standing up.
How long should I wait to take Advil after finishing a course of prednisone?
As a pharmacist, I recommend a washout period of at least 24 to 48 hours after your final dose of prednisone before resuming any NSAID like ibuprofen. This delay allows your body to restart natural prostaglandin production and ensures the steroid has sufficiently cleared your system to minimize the risk of a late-onset GI bleed.
Can I safely take Tylenol for pain relief while on a steroid pack?
Yes, we often refer to this as the “Tylenol Bridge” because acetaminophen works centrally in the brain and does not inhibit the COX-1 enzymes that protect your stomach or kidneys. It is the safest over-the-counter analgesic option for managing breakthrough pain while taking oral corticosteroids like prednisone or methylprednisolone.
Is topical diclofenac gel safer to use with oral steroids than ibuprofen pills?
Topical NSAIDs like Voltaren gel have much lower systemic absorption—typically around 6%—compared to oral tablets, which reach 100% absorption. While this makes them a lower-risk “loophole” for localized joint pain, you should still consult your physician before use, as some systemic exposure still occurs during high-dose steroid therapy.
What should I do if I accidentally took one ibuprofen while on prednisone?
A single accidental dose is rarely a medical emergency for a healthy individual, but you should immediately stop taking any further NSAIDs and switch to acetaminophen if pain relief is needed. Monitor yourself closely for indigestion, abdominal pain, or changes in stool color over the next 24 hours and stay well-hydrated to support kidney function.
Is Aleve or Naproxen a safer alternative to ibuprofen when taking steroids?
Naproxen is actually considered riskier in this context because it has a significantly longer half-life than ibuprofen, meaning it suppresses protective prostaglandins for a much longer duration. To prevent severe peptic ulcer disease, you should avoid all non-selective NSAIDs, including Aleve, Motrin, and high-dose aspirin, while on a steroid regimen.
Why would a rheumatologist prescribe both a steroid and an NSAID together?
In cases of severe autoimmune flares like Rheumatoid Arthritis or Lupus, specialists may determine that the benefit of rapid inflammation control outweighs the GI risks. In these controlled scenarios, doctors typically prescribe a “shield” such as a Proton Pump Inhibitor (PPI) like omeprazole to drastically reduce stomach acid and mitigate the risk of ulceration.
Does taking prednisone with a large meal make it safe to use ibuprofen?
No, this is a common misconception; while food can buffer acid and reduce immediate nausea, the damage caused by this drug combination is systemic. Once the medications enter your bloodstream, they chemically inhibit the enzymes that maintain your stomach lining, meaning an ulcer can still form regardless of whether your stomach was full or empty at the time of ingestion.
Can I drink alcohol while taking a combination of prednisone and NSAIDs?
Absolutely not; alcohol is a direct gastric irritant that further inflames the stomach lining, creating what we call a “triple threat” for GI bleeding. Combining alcohol with steroids and NSAIDs exponentially increases the likelihood of a life-threatening hemorrhage or perforation and should be avoided entirely during and shortly after treatment.
How does the combination of steroids and ibuprofen impact kidney health?
This combination can lead to acute kidney injury (AKI) by causing a double hit to renal hemodynamics: ibuprofen constricts the blood vessels entering the kidney while prednisone promotes fluid and sodium retention. This can result in a rapid drop in the glomerular filtration rate, especially in patients who are elderly, dehydrated, or taking blood pressure medications.
Is it safe to continue my daily baby aspirin if I am prescribed prednisone?
Patients on 81mg aspirin for cardiovascular protection should not stop their medication, but they must inform their prescribing doctor immediately. In these instances, the physician will often add a gastroprotective agent like a PPI to the regimen to shield the stomach from the combined erosive effects of the aspirin and the steroid.
Disclaimer
This article is for informational purposes only and does not constitute medical advice. The interaction between Ibuprofen and Prednisone can be life-threatening. Always consult a qualified healthcare professional or your pharmacist before combining any medications or changing your prescribed treatment plan.
References
- U.S. Food and Drug Administration (FDA) – fda.gov – Official drug labeling and safety communication regarding NSAID and corticosteroid interactions.
- Mayo Clinic – mayoclinic.org – Clinical overview of the risks associated with combining nonsteroidal anti-inflammatory drugs and oral steroids.
- The American Journal of Gastroenterology – gi.org – Peer-reviewed research on the 12-fold increase in peptic ulcer risk when using dual therapy.
- National Kidney Foundation – kidney.org – Guidance on how NSAIDs and steroids impact glomerular filtration and acute renal failure risks.
- Arthritis Foundation – arthritis.org – Patient guidelines for managing autoimmune flares and safe analgesic alternatives like the Tylenol Bridge.
- PubMed / National Center for Biotechnology Information – ncbi.nlm.nih.gov – Study on the biochemical mechanism of synergistic toxicity in the gastric mucosa.