Every week, patients come into my office exhausted from days of frequent bathroom trips and ask one very specific question: is yogurt good for diarrhea? For decades, the standard advice was to avoid all dairy during stomach bugs and stick strictly to the BRAT diet of bananas, rice, applesauce, and toast. Modern clinical research, however, has completely changed how we approach gut recovery.
Table of Contents
As a Registered Dietitian Nutritionist specializing in Medical Nutrition Therapy, I can tell you that traditional Mexican cooking is not the only cuisine with hidden health benefits. The same is true for cultured dairy. The right type of yogurt can be a genuine healing tool, while the wrong type will make your symptoms significantly worse.
This guide will walk you through the clinical evidence behind probiotic therapy, decode the confusing dairy paradox, and give you a clear selection protocol for choosing the best yogurt when your gut needs help.

Quick Answer: Yes, specific types of plain, low-sugar yogurt are highly beneficial for diarrhea recovery. The key is live and active cultures. These beneficial bacteria help restore your compromised gut microbiome and can shorten the duration of symptoms significantly. However, you must avoid high-sugar and lactose-heavy varieties, which will actively make digestive issues worse.
Key Statistics on Gut Health and Probiotics
- Duration Reduction: Clinical studies show specific probiotics can reduce the duration of infectious diarrhea by 24 to 30 hours.
- Antibiotic Protection: Early introduction of beneficial bacteria reduces the risk of antibiotic-associated diarrhea by up to 51 percent.
- Microbiome Scale: The human gut contains over 100 trillion microbial cells that face heavy disruption during acute illness.
- Minimum CFU Threshold: Therapeutic cultured dairy must contain at least 100 million colony-forming units (CFUs) per gram to be effective.
- Post-Infectious IBS: Up to 30 percent of patients develop post-infectious IBS after a severe bout of food poisoning or viral gastroenteritis.
Not every product in the dairy aisle is created equal. Finding the right option requires understanding what is happening inside your body. Let’s start with the science behind your symptoms.
Understanding the Dairy Paradox in Gastrointestinal Distress

What Happens to Your Gut During Diarrhea?
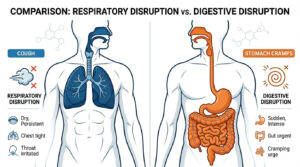
Acute gastrointestinal distress generally falls into two clinical categories. Secretory diarrhea is often caused by bacterial toxins or viral pathogens that force your body to release excess water and electrolytes directly into the bowels. Osmotic diarrhea occurs when unabsorbed nutrients draw excess water into the colon.
During an active infection, the intestinal lining becomes highly inflamed. This often leads to increased intestinal permeability, commonly called leaky gut. The tight junctions between intestinal cells loosen, allowing toxins and undigested food particles to pass into the bloodstream.
Your body responds to this breach by flushing everything out as fast as possible. This rapid flushing strips away beneficial bacteria along with pathogens, leaving your microbiome depleted and vulnerable to further infection.
Why Regular Dairy Is Contraindicated
You have probably heard that you should avoid milk when your stomach is upset. This advice is generally correct. When you have a stomach bug, the infection temporarily damages the microvilli in your small intestine.
Think of microvilli like a plush carpet lining your digestive tract. These tiny structures produce lactase, the enzyme required to digest lactose, the natural sugar in milk. When a virus damages your microvilli, lactase production drops dramatically.
If you drink regular milk in this state, the lactose remains undigested. It travels straight to the colon, where it ferments rapidly, producing excess gas, severe bloating, and painful cramping. Worse, the undigested sugar pulls massive amounts of water into the bowels, triggering osmotic diarrhea.
How Fermentation Changes the Equation
If regular milk causes such problems, why do gastroenterologists consider cultured dairy products? The answer lies in fermentation. When comparing yogurt to pasteurized liquid milk, the chemical composition is entirely different. You are essentially comparing a pre-digested food to raw ingredients.
During commercial fermentation, specific bacterial strains are added to warm milk. These bacteria consume the lactose to survive and multiply. By the time the final product reaches the store, the bacteria have already broken down the vast majority of the lactose. Your damaged microvilli do not have to do the heavy lifting.
According to clinical guidelines from the American Gastroenterological Association, fermented dairy is generally well-tolerated during acute digestive distress. The bacteria do the digesting for you before the spoon even reaches your mouth. This fundamental chemical difference is why cultured products heal while regular milk harms.
The Clinical Evidence: Is Yogurt Good for Diarrhea Recovery?

Shortening the Duration of Infectious Diarrhea
Clinical meta-analyses have shown that introducing specific beneficial bacteria can reduce the duration of infectious diarrhea by roughly 24 to 30 hours. For a patient dealing with severe dehydration and exhaustion, saving an entire day of symptoms is a significant medical win.
The primary mechanism is called competitive exclusion. When you consume a product rich in beneficial microbes, these good bacteria travel to the intestinal mucosa and physically block pathogens from attaching to your vulnerable cell walls.
These beneficial microbes also secrete antimicrobial peptides that actively hunt and destroy harmful pathogens. This is not just soothing your stomach. It is actively fighting the infection on the front lines.
Preventing Antibiotic-Associated Diarrhea
Sometimes the medicine meant to heal you causes the most digestive damage. Broad-spectrum antibiotics kill harmful bacteria efficiently, but they do not discriminate. They wipe out beneficial flora entirely, frequently leading to antibiotic-associated diarrhea. This condition affects up to 30 percent of patients on these medications.
The sudden loss of good bacteria allows opportunistic pathogens like Clostridioides difficile to multiply rapidly. However, clinical data shows that introducing therapeutic fermented foods early in an antibiotic cycle reduces the risk of antibiotic-associated diarrhea by up to 51 percent.
Dietitian Tip: If you are taking antibiotics, never eat your fermented foods at the same time as your pill. The medication will kill the beneficial bacteria on contact. Wait at least two hours after taking your antibiotic before consuming any probiotic-rich food.
Short-Chain Fatty Acids and Stool Firming
When beneficial bacteria reach your large intestine, they ferment residual carbohydrates and dietary fibers your body could not digest on its own. The byproduct of this fermentation is Short-Chain Fatty Acids (SCFAs), the most important being butyrate.
Butyrate serves as the primary fuel for colonocytes, the specialized cells lining your colon. When colonocytes are well-fed with butyrate, they become incredibly effective at absorbing excess water and sodium from waste. More water absorption means firmer stools.
By providing your gut with the bacteria needed to produce SCFAs, you are treating the root cause of watery stools, not just masking symptoms.
Which Probiotic Strains Matter Most?

Clinical Trial Data on Key Bacterial Strains
Different bacterial strains perform vastly different jobs. To effectively treat a compromised gut, you need to know which strains have genuine clinical backing.
Lactobacillus rhamnosus GG is one of the most heavily researched strains in gastroenterology. It is proven effective against viral bugs in both pediatric and adult trials. It survives the harsh acidity of the stomach and binds tightly to intestinal walls, providing a strong barrier against rotavirus and norovirus.
Bifidobacterium lactis is naturally found in a healthy digestive tract. Clinical studies show it significantly improves gut motility and calms hyperactive immune responses. It is especially useful for patients recovering from prolonged infections.
Saccharomyces boulardii is technically a beneficial yeast rather than a bacterium. Its unique advantage is that it cannot be killed by standard antibacterial medications. This makes it the gold standard for treating antibiotic-associated diarrhea.
Probiotic Strain Comparison
| Probiotic Strain | Primary Benefit | Ideal Use Case | Evidence Level |
| Lactobacillus rhamnosus GG | Reduces duration of infectious diarrhea | Viral gastroenteritis, pediatric diarrhea | High |
| Bifidobacterium lactis | Improves gut motility and immune response | Post-infectious IBS, general dysbiosis | High |
| Saccharomyces boulardii | Binds to pathogens, survives antibiotics | Antibiotic-associated diarrhea, traveler’s diarrhea | Very High |
| Lactobacillus acidophilus | Restores general flora, aids lactose digestion | Mild stomach upset, daily maintenance | Moderate |
The Selection Protocol: What to Choose at the Grocery Store
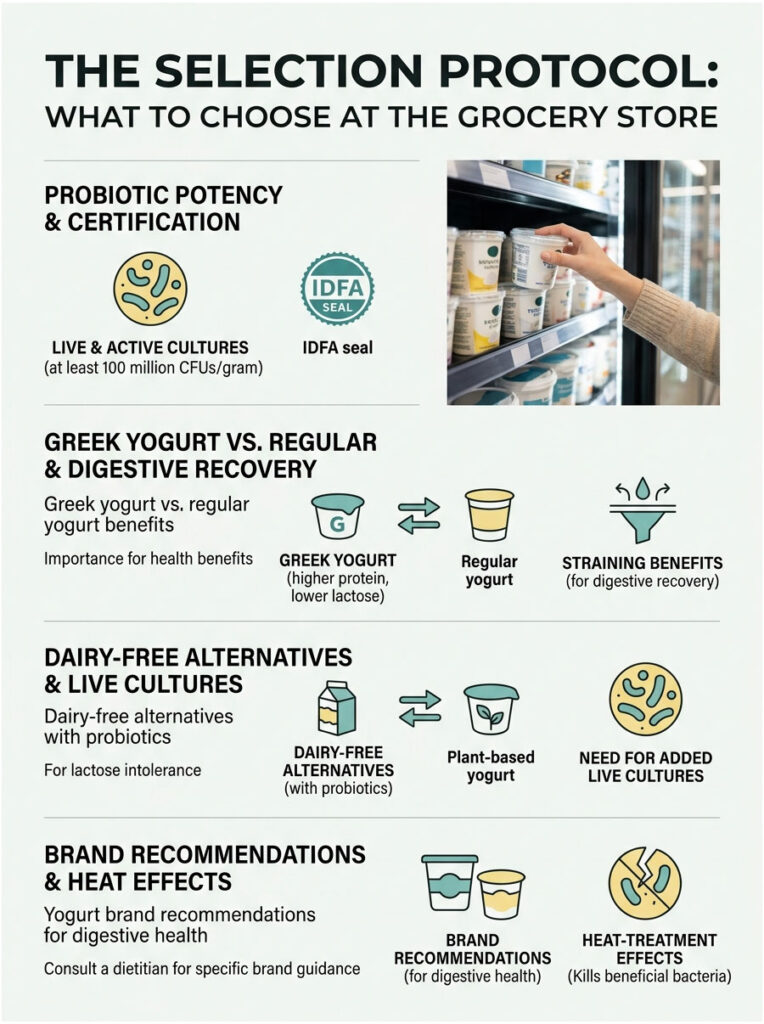
Decoding the “Live and Active Cultures” Label
The single most critical phrase to look for is “live and active cultures” on the packaging. Without living organisms, you are eating sour pudding, not medicine. The International Dairy Foods Association (IDFA) has a specific seal guaranteeing that products contain at least 100 million colony-forming units per gram at manufacture.
This high concentration is necessary to survive stomach acid. If a product has been heat-treated after fermentation, all beneficial bacteria are dead. Manufacturers sometimes heat-treat to extend shelf life and label the result as a “dairy snack” rather than a true fermented food. Always check the back of the container for specific living strains listed by their Latin names.
Greek Yogurt vs. Regular Yogurt for Digestive Recovery
Texture matters when your digestive system is compromised. Greek varieties are preferable because of the traditional straining process, which removes liquid whey multiple times. The whey holds the majority of remaining lactose, so straining it out eliminates most osmotic triggers.
This straining also concentrates protein content significantly. High-quality protein is essential for repairing damaged intestinal tissue. A standard Greek variety offers roughly double the protein of a regular cup, making it a superior choice for tissue recovery.
Dairy-Free Alternatives with Probiotics
If you are vegan or have severe baseline lactose intolerance, you can still benefit from probiotic therapy. Dairy-free alternatives made from almond, coconut, or oat milk are naturally lactose-free, eliminating the risk of dairy-induced osmotic diarrhea.
However, plant milks do not ferment the same way as cow’s milk. Manufacturers must add beneficial bacteria after the thickening process. Always check labels for added live cultures. Watch out for artificial thickeners like carrageenan or heavy guar gums, which can cause gastrointestinal inflammation in sensitive individuals. Choose brands with the shortest, cleanest ingredient list.
Yogurt Brand Comparison for Digestive Health
| Category / Brand | Suitability | Key Reason | Recommendation |
| Plain Greek (Chobani, Fage) | Excellent | Low lactose, high protein, active cultures | Highly Recommended |
| Icelandic Skyr (Siggi’s Plain) | Excellent | Very low lactose, minimal ingredients | Highly Recommended |
| Fruit-on-the-Bottom / Syrupy | Poor | High sugar triggers osmotic diarrhea | Avoid entirely |
| Lactose-Free (Green Valley) | Excellent | Zero lactose risk, contains beneficial flora | Best for severe sensitivity |
| Frozen Yogurt | Poor | High sugar, cultures often destroyed by freezing | Avoid entirely |
When Yogurt Makes Diarrhea Worse: The Avoid List

High Sugar Content and Osmotic Diarrhea
The biggest mistake is buying a product loaded with added refined sugar. Fruit-on-the-bottom cups, syrupy mix-ins, and sweetened vanilla varieties are strictly off-limits during gut recovery.
When you consume high amounts of refined sugar, your damaged system cannot absorb it all. The excess sugar travels to the large intestine, where it acts like a sponge. Through osmosis, sugar molecules pull massive amounts of water from surrounding tissues into the bowels. The result is explosive osmotic diarrhea. Always choose plain, unsweetened varieties.
Artificial Sweeteners: Sorbitol and Xylitol
Many people think “sugar-free” options are a smart choice. In clinical nutrition, this is a serious error. Most sugar-free dairy products are sweetened with sugar alcohols like sorbitol, xylitol, or erythritol. These are very poorly absorbed and ferment rapidly in the gut, producing excessive gas and bloating.
More importantly, they have a well-documented laxative effect. The last thing a hyperactive bowel needs is a chemical laxative. Even natural zero-calorie sweeteners like stevia can sometimes irritate a highly inflamed mucosal lining. Stick strictly to plain, unsweetened products.
High-Fat Dairy During Acute Illness
Fat is normally a healthy part of a balanced diet, but during acute gastrointestinal distress, high-fat foods become problematic. Fat is complex to digest, requiring bile acids and significant effort from the liver and pancreas.
High-fat foods accelerate gastric emptying, forcing the stomach to dump contents into inflamed intestines faster than normal. This causes severe cramping and urgency. Unabsorbed fats in the colon also undergo bacterial hydroxylation, creating compounds that stimulate the colon to secrete even more water. Stick to non-fat or low-fat plain varieties until normal stool consistency returns.
How to Incorporate Yogurt into a Recovery Diet

Dosing and Timing for Best Results
For acute recovery, aim for one to two servings daily, roughly 6 to 12 ounces of high-quality, plain Greek yogurt per day. This provides enough colony-forming units to repopulate your microbiome without overwhelming the digestive system.
Timing matters. Eat your yogurt on a relatively empty stomach, first thing in the morning or as a mid-afternoon snack. When the stomach is full of a heavy meal, it produces highly acidic gastric juice that can kill live cultures before they reach the intestines. A lighter stomach allows beneficial bacteria to pass through more safely.
Prebiotic Fiber Synergy
Probiotics are living organisms that need specific food to survive and multiply. That food is prebiotic fiber. Combining a probiotic-rich food with soluble fiber dramatically boosts bacterial multiplication and SCFA production.
During active illness, you cannot eat harsh raw vegetables or heavy grains. Instead, mash a small amount of ripe banana into your plain yogurt. Ripe bananas are gentle on the stomach and packed with soluble pectin fiber. Another option is a small spoonful of cooked, plain oatmeal.
Dietitian Tip: Do not add honey during the first 48 hours of recovery. While honey is natural and antimicrobial, it is high in fructose. Excess fructose can cause unwanted osmotic pressure in a sensitive gut. Use mashed banana for natural sweetness instead.
Beyond Initial Recovery: Long-Term Gut Healing

Transitioning Back to a Normal Diet
As stool consistency improves, reintroduce complex foods slowly. Continue daily yogurt, but begin adding slightly more complex prebiotic fibers like soft cooked carrots or sweet potatoes.
During this phase, your microbiome is still fragile. The beneficial bacteria you have introduced are fighting to establish permanent colonies. If you suddenly switch to processed foods, alcohol, or greasy meals, you will disrupt this colonization process. Give your body at least a full week of clean whole foods after a severe stomach bug.
Pay close attention to how your body responds. If a specific food causes bloating or loose stools, step back immediately. Intestinal villi need time to regenerate, and lactase production may take several days to return to baseline.
Long-Term Microbiome Maintenance
A severe infection should serve as a wake-up call for overall digestive health. Once recovered, focus on building a microbiome so robust that future pathogens struggle to gain a foothold. Daily fermented foods are a cornerstone of this strategy.
You do not have to limit yourself to yogurt. Try milk kefir, water kefir, or small amounts of raw sauerkraut. Each offers different beneficial strains. Microbial diversity is the key to a strong, resilient immune system.
Ensure you consume at least 25 to 30 grams of diverse dietary fiber daily. The probiotics you eat will only stick around if you feed them consistently. A diet rich in varied plant fibers keeps your bacterial colonies thriving for years.
When to See a Doctor
Dietary interventions are powerful, but they are not a replacement for emergency medical care. Food therapy is appropriate for standard viral bugs, mild food poisoning, and antibiotic-associated upset. It is not sufficient for severe, life-threatening infections.
- Symptoms lasting beyond 48 hours without improvement require medical evaluation.
- Signs of severe dehydration (dark urine, dizziness, confusion) mean you need urgent care immediately.
- High fever, severe abdominal pain mimicking appendicitis, or bloody stools are absolute emergencies.
Always listen to your body and consult a physician when symptoms feel unmanageable.
Summary and Key Takeaways
Plain, low-sugar, probiotic-rich yogurt is a powerful, evidence-based tool for recovering from diarrhea. It provides the exact beneficial bacteria your body needs to repair damaged tissue and restore normal gut function. Here is what to remember the next time you are navigating the grocery store:
- Always choose plain and unsweetened. Avoid added sugars and artificial sweeteners to prevent osmotic diarrhea.
- Look for the IDFA seal. Verify live and active cultures on the label to ensure clinical efficacy.
- Choose Greek or Skyr varieties. Aggressive straining removes most lactose and concentrates protein.
- Mind your medications. If treating antibiotic-associated diarrhea, space yogurt intake at least two hours from your pill.
- Pair with gentle prebiotic fiber. Mashed banana or plain oatmeal boosts SCFA production and speeds recovery.
Your gut microbiome is incredibly resilient. While a stomach bug or a course of antibiotics can cause severe temporary disruption, your body knows how to heal. By providing it with the right beneficial bacteria, you give your digestive system the exact tools it needs to repair itself. The next time someone asks you, is yogurt good for diarrhea, you will know exactly how to answer.
Frequently Asked Questions
Is it safe to consume dairy like yogurt when I have a stomach bug?
As a Registered Dietitian Nutritionist, I explain this through the ‘dairy paradox.’ While liquid milk is contraindicated due to temporary lactase deficiency during infection, fermented yogurt is safe and beneficial because the live bacteria have already pre-digested the lactose, preventing the osmotic diarrhea typically caused by dairy.
What does the ‘Live and Active Cultures’ seal mean for my recovery?
The IDFA seal guarantees that the product contains at least 100 million colony-forming units (CFUs) per gram at the time of manufacture. This high concentration is clinically necessary to ensure enough beneficial bacteria survive your stomach acid to effectively repopulate your compromised gut microbiome.
Why is Greek yogurt specifically recommended over regular varieties for diarrhea?
Greek yogurt undergoes an intensive straining process that removes the liquid whey, which contains the majority of the remaining lactose sugars. This makes it much easier on a gut with damaged microvilli, while providing double the protein needed for repairing intestinal tissue and ‘leaky gut’ permeability.
Can probiotics in yogurt prevent antibiotic-associated diarrhea (AAD)?
Clinical evidence shows that introducing therapeutic fermented foods early in an antibiotic cycle can reduce the risk of AAD by up to 51%. To be effective, you must consume the yogurt at least two hours before or after your medication to prevent the antibiotic from instantly killing the beneficial microbes.
Which specific bacterial strains should I look for on the label for infectious diarrhea?
For viral gastroenteritis, look for Lactobacillus rhamnosus GG, which is highly effective at binding to intestinal walls. For general recovery and immune response, Bifidobacterium lactis is the gold standard. If you are dealing with antibiotic-associated issues, Saccharomyces boulardii is the preferred therapeutic choice.
Why does eating flavored or ‘fruit-on-the-bottom’ yogurt often worsen symptoms?
High sugar content triggers osmotic diarrhea. When your digestive system is compromised, it cannot absorb refined sugars, which then act like a sponge in the colon, drawing in massive amounts of water and leading to explosive stools and increased cramping.
Are dairy-free yogurts effective for gut recovery during illness?
Plant-based alternatives like coconut or almond yogurt are excellent lactose-free options, provided they are fortified with live and active cultures. However, ensure they do not contain artificial thickeners like carrageenan, which can further inflame a sensitive mucosal lining.
How do beneficial bacteria help firm up watery stools?
Probiotics reach the large intestine and ferment fiber into Short-Chain Fatty Acids (SCFAs), specifically butyrate. Butyrate fuels your colonocytes, making them significantly more efficient at absorbing excess water and sodium from your waste, which naturally firms the stool.
Is frozen yogurt a suitable alternative during a bout of gastroenteritis?
I strongly advise against frozen yogurt for medical recovery. It is typically loaded with refined sugars and the freezing process often kills the delicate live cultures required for therapeutic benefits, leaving you with a product that may actually prolong your symptoms.
What is the most effective time to eat yogurt for gut healing?
I recommend consuming cultured dairy on a relatively empty stomach, such as first thing in the morning. This allows the beneficial bacteria to pass through the stomach more quickly, avoiding the high levels of gastric acid produced during heavy meals that can destroy the probiotics.
How can I maximize the healing power of yogurt using ‘prebiotic synergy’?
You can create prebiotic synergy by mashing a ripe banana into plain Greek yogurt. The soluble pectin fiber in the banana acts as fuel for the probiotics, stimulating them to multiply rapidly and increase the production of healing short-chain fatty acids in your colon.
When should I stop self-treating with yogurt and seek medical attention?
While dietary therapy is powerful, you must seek medical care if symptoms persist beyond 48 hours, or if you experience clinical red flags such as high fever, bloody stools, severe abdominal pain, or signs of acute dehydration like dizziness and dark urine.
Disclaimer
This article is for informational purposes only and does not constitute medical advice. The content is based on clinical research and the professional experience of Dr. Elena Richardson, RDN. Always consult a qualified healthcare professional or your primary care physician before making significant dietary changes, especially during acute illness. If you experience signs of severe dehydration, high fever, or bloody stools, seek emergency medical attention immediately.
References
- American Gastroenterological Association – gastro.org – Clinical guidelines on the dietary management of acute gastroenteritis and probiotic use.
- National Institutes of Health (NIH) – Office of Dietary Supplements – Fact sheet on the efficacy of probiotics for infectious and antibiotic-associated diarrhea.
- Journal of Clinical Gastroenterology – “Probiotics for the Prevention of Pediatric Antibiotic-Associated Diarrhea” – Meta-analysis of Lactobacillus rhamnosus GG efficacy.
- International Dairy Foods Association (IDFA) – idfa.org – Standards and regulations for the “Live and Active Cultures” seal on fermented dairy products.
- World Gastroenterology Organisation (WGO) – Global Guidelines on Probiotics and Prebiotics – Evidence-based strain recommendations for digestive disorders.
- Cochrane Database of Systematic Reviews – “Probiotics for the prevention of Clostridium difficile-associated diarrhea” – Statistical data on the 51% reduction in AAD risk.