If you have ever been stuck in bed with an upset stomach, wondering what on earth you should eat, you are not alone. Figuring out what to eat when you have diarrhea can feel overwhelming, especially when your body seems to reject everything. But the right food choices can genuinely speed up your recovery, while the wrong ones can set you back hours or even days.
Table of Contents
As a clinical Registered Dietitian working in gastroenterology, I see this scenario regularly. Patients come in dehydrated, exhausted, and confused about what their gut can actually handle. The immediate priorities are always the same: slow down that overactive bowel, prevent dehydration, and protect against nutrient loss.
Choosing the best foods for fast relief is not about guesswork. It requires a focused strategy built around low-residue carbohydrates, the right electrolyte balance, and targeted soluble fibers. This guide goes well beyond the outdated advice you may have heard. It gives you a clear, evidence-based roadmap for restoring your intestinal health, from the first few hours of illness through full recovery.

Healing your gut takes patience and precision. You cannot force an inflamed digestive system to calm down overnight. But you can gently guide it back to normal with science-backed nutrition. Let me walk you through exactly how to do that, step by step.
Quick Answer: What Should You Eat for Diarrhea?
To get relief quickly, stick to a bland diet built around low-residue carbohydrates and soluble fiber. The best foods for fast relief include bananas, white rice, unsweetened applesauce, plain toast, and skinless baked chicken. Pair these with an Oral Rehydration Solution (ORS) to replace lost fluids and electrolytes. Until your bowel movements return to normal, stay away from dairy, high-fat meals, artificial sweeteners, caffeine, and insoluble fiber.
Key Statistics on Gastrointestinal Distress
- Prevalence: According to the American College of Gastroenterology (2023), adults in the USA experience an average of 4 episodes of acute diarrhea per year.
- Dehydration Risk: The Mayo Clinic reports that severe acute diarrhea can lead to a loss of up to 1 gallon of body water within 24 hours.
- Recovery Time: Clinical data shows that a targeted binding diet can reduce the duration of an acute episode by 20 to 30 percent.
- Electrolyte Depletion: Potassium and sodium levels can drop by as much as 40 percent during the first 48 hours of a severe GI infection.
- Viral Impact: The CDC notes that norovirus causes roughly 19 to 21 million cases of acute gastroenteritis each year in the United States.
- Dietary Triggers: Research indicates that 65 percent of adults have reduced ability to digest lactose after infancy, making dairy a primary trigger during gut infections.
Understanding Diarrhea: A Clinical Perspective
Before deciding what to eat for diarrhea, it helps to understand what is actually going on inside your digestive tract. Under normal conditions, your small and large intestines absorb water and nutrients smoothly from the food you eat. But when an irritant enters the picture, whether it is a virus, bacteria, or chemical trigger, that orderly process falls apart.
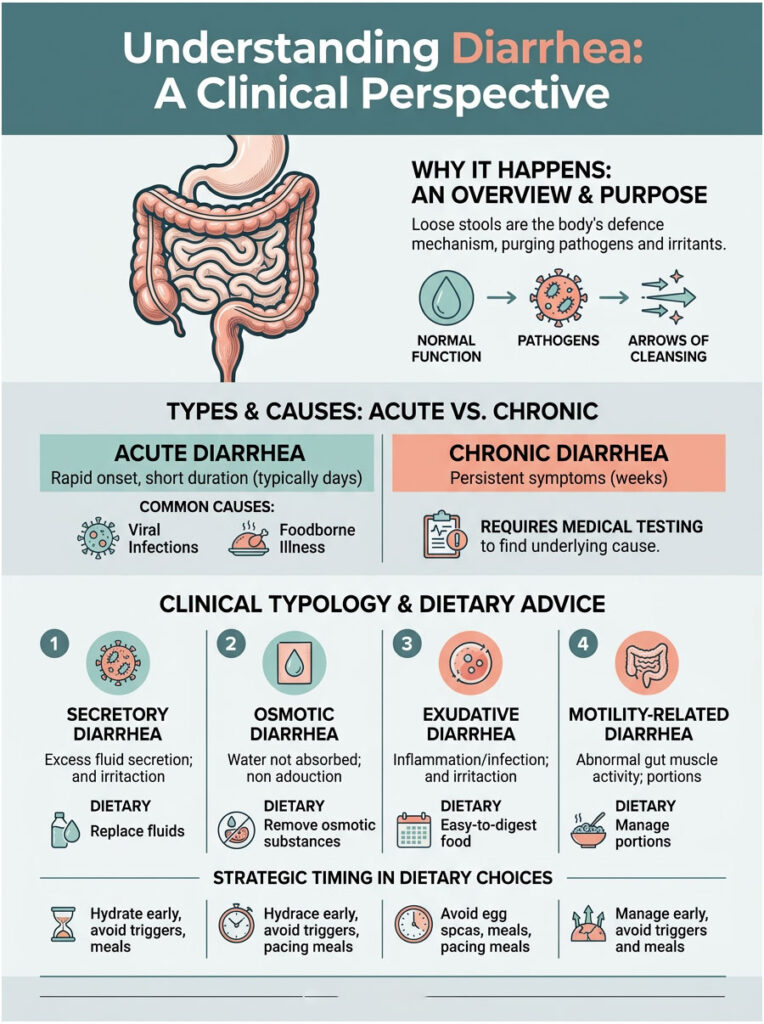
Loose stools are not just a random inconvenience. They are actually your body’s defense mechanism. Your gut is trying to flush out harmful pathogens, bacterial toxins, or chemical irritants as fast as possible. So the best foods for fast relief are the ones that support this clearing process without adding fuel to the fire, all while protecting you from dangerous nutrient and fluid loss.
In my practice, I always tell patients that treating GI distress requires strategic timing. You need to respect your body’s natural cleansing process while also preventing it from going too far. That balance is exactly why understanding what to eat for diarrhea matters so much.
The Four Main Types of Diarrhea
Not all stomach issues work the same way. Medical professionals recognize four distinct types based on the underlying mechanism. Secretory diarrhea happens when your body actively pumps water into the intestines, usually because of a bacterial infection like cholera or E. coli. Osmotic diarrhea occurs when unabsorbed nutrients pull excess water from your bloodstream into the bowels.
Exudative diarrhea involves blood and pus in the stool and is closely linked to inflammatory bowel diseases like Crohn’s disease or ulcerative colitis. Motility-related diarrhea happens when food moves through the digestive tract too quickly for water absorption. This rapid transit is common in conditions like hyperthyroidism or Irritable Bowel Syndrome (IBS).
Knowing your type matters for recovery. If you drank too much apple juice and triggered an osmotic shift, simply stopping the juice may fix the problem. But a secretory bacterial infection calls for a much more aggressive and carefully planned dietary response.
Acute vs. Chronic Diarrhea: Why It Matters
To build the right dietary plan, you first need to identify the timeline. Acute episodes come on suddenly and typically last three to seven days. The usual culprits are viral infections, bacterial contamination, or foodborne illness.
During an acute infection, pathogens set off a major inflammatory response in the delicate gut lining. This inflammation ramps up peristalsis, the wave-like muscle contractions that push contents through your intestines. When the gut is inflamed, these contractions become fast, intense, and unpredictable.
Chronic diarrhea, on the other hand, persists for four weeks or longer. It is usually tied to autoimmune conditions, celiac disease, or long-term post-infectious IBS. If you are dealing with chronic symptoms, you will need medical testing rather than just a quick 48-hour dietary fix.
The Dangers of Dehydration and Malabsorption
Here is the honest truth: the most immediate threat during a bout of diarrhea is not starvation. It is severe dehydration. When your transit time is drastically shortened, your small intestine simply cannot absorb the essential nutrients and fluids it normally would.
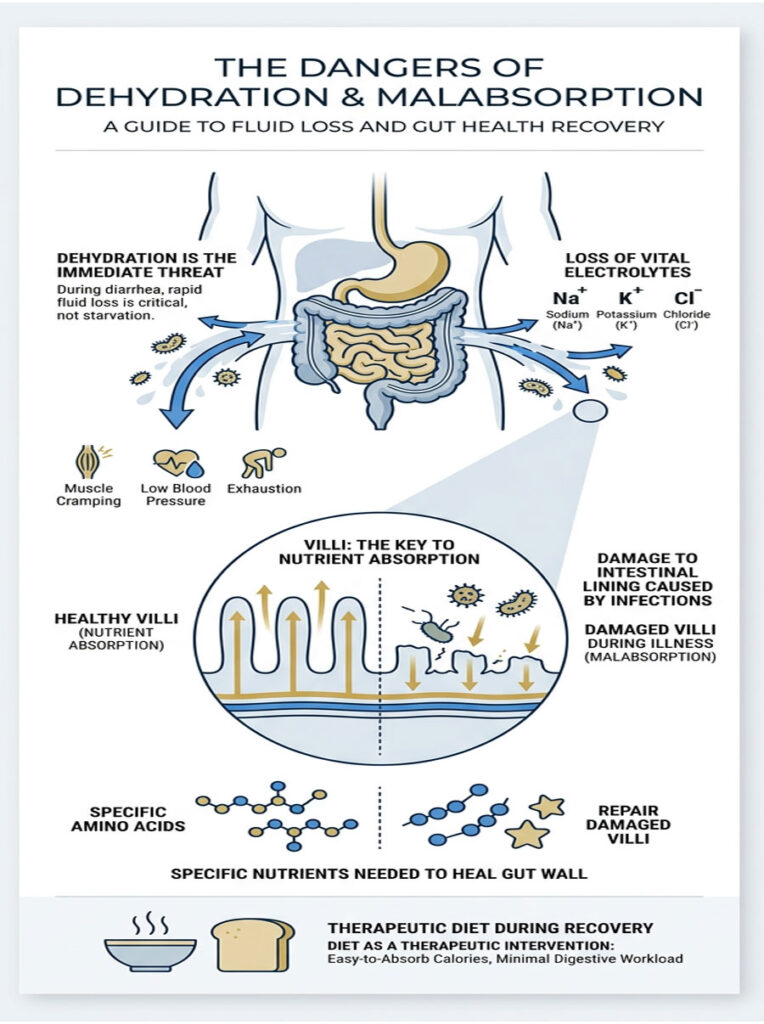
Your body depends on a precise balance of sodium, potassium, and chloride to keep your heart beating regularly and your muscles functioning. When you lose large amounts of fluid, those vital electrolytes go with it. The result is muscle cramping, dropping blood pressure, and total exhaustion.
I have seen many patients end up in the hospital simply because they tried to get by on plain tap water and regular meals. That approach only feeds the osmotic fluid shifts. To break the cycle, you need specific binding foods that actively trap the excess fluid in your bowel.
Why Your Body Needs Specific Nutrients to Heal
When an infection damages your intestinal lining, the microscopic finger-like projections called villi get blunted and worn down. These villi are responsible for absorbing all nutrients from your food. Until they heal, your digestive capacity stays severely limited. You simply cannot handle complex fats or heavy fibers during this vulnerable window.
Your gut needs specific amino acids and simple starches to rebuild those damaged villi. Without the right nutritional building blocks, healing stalls. This prolonged damage can leave you vulnerable to secondary infections and chronic food intolerances.
That is why your diet during recovery should act as a direct medical intervention. Every bite and every sip should serve a specific therapeutic purpose: supplying easy-to-absorb calories while keeping the digestive workload on your exhausted gut to an absolute minimum.
The BRAT Diet: What Has Changed and What Still Works
For decades, the go-to advice for an upset stomach was the classic BRAT diet: Bananas, Rice, Applesauce, and Toast. If you asked any pediatrician what to eat for diarrhea in the 1990s, that is exactly what they would recommend.

Nutrition science has come a long way since then. The Academy of Nutrition and Dietetics now offers a much more nuanced view. While the BRAT diet is still useful for the first 24 to 48 hours, it is no longer recommended as a prolonged plan. These four foods are very low in protein, healthy fats, and essential vitamins.
Staying on this restrictive diet too long can actually delay healing because of cellular malnutrition. However, as a short-term binding strategy, these foods remain some of the best foods for fast relief. Here is why each one works so well.
Bananas: The Power of Pectin
Bananas are a powerhouse when your stomach is in trouble. They are rich in potassium, which helps replace critical electrolytes lost through frequent watery stools. Even more important, bananas are loaded with pectin, a specialized fiber that acts as a natural binding agent in the gut.
Pectin absorbs excess fluid in the bowel, helping to firm up stool consistency. When choosing bananas for this purpose, go for slightly green or perfectly yellow ones. Overly ripe bananas with lots of brown spots contain higher amounts of simple sugars that can sometimes draw unwanted water into the gut.
Slightly green bananas also contain resistant starch, which bypasses the small intestine and feeds the beneficial bacteria in your colon. Those bacteria convert it into short-chain fatty acids that directly nourish and heal inflamed colon cells.
White Rice: The Go-To Low-Residue Carbohydrate
White rice is a staple of any bland recovery diet. I specifically recommend white rice, not brown rice. White rice has had the fibrous outer bran and nutrient-dense germ removed, making it a perfect low-residue carbohydrate.
Because it lacks rough fiber, white rice digests quickly and easily in the upper digestive tract. It leaves virtually no waste behind to irritate the lower colon. Think of it as a dry sponge, soaking up excess water and neutralizing harsh stomach acids.
For the best results, cook it with slightly more water than usual so it comes out extra soft. Jasmine or basmati rice work great. Skip the butter, heavy oils, or spicy seasonings, as fats will trigger unwanted colon contractions.
Unsweetened Applesauce: Gentle Soluble Fiber
Applesauce works on the same principle as bananas. Raw apples have tough, waxy skins full of insoluble fiber, which is terrible for an inflamed gut. But when apples are peeled, cooked, and mashed, the chemical structure changes completely.
The cooking process breaks down the harsh cellulose and releases a highly digestible source of pectin. This makes unsweetened applesauce one of the best foods for fast relief. It provides gentle energy without taxing your digestive enzymes.
Always make sure the applesauce is strictly unsweetened. Many commercial brands add high-fructose corn syrup or cane sugar. Those added sugars act as osmotic laxatives, pulling more water into the gut and making symptoms worse.
Plain Toast: Simple Starches for Easy Digestion
Plain white toast provides simple, easily digestible carbohydrates that your body can absorb with minimal effort. Like white rice, processed white bread has the harsh roughage removed. Toasting the bread actually changes the molecular structure of the starches slightly.
This creates dextrins, which are smaller starch molecules that are even gentler on a sensitive stomach. The dry, slightly charred texture also helps settle nausea and absorb excess gastric acid.
During the acute phase, avoid any toppings. Butter, jam, peanut butter, or cream cheese will introduce fats and sugars your gut cannot handle right now. Keep it completely plain until your stool consistency normalizes.
Soluble Fiber vs. Insoluble Fiber: Know the Difference
One of the most common mistakes people make is assuming all dietary fiber is helpful all the time. When you are looking for fast relief, understanding the difference between soluble and insoluble fiber is critical. Soluble fiber is your best friend during a flare-up. Insoluble fiber is your worst enemy.
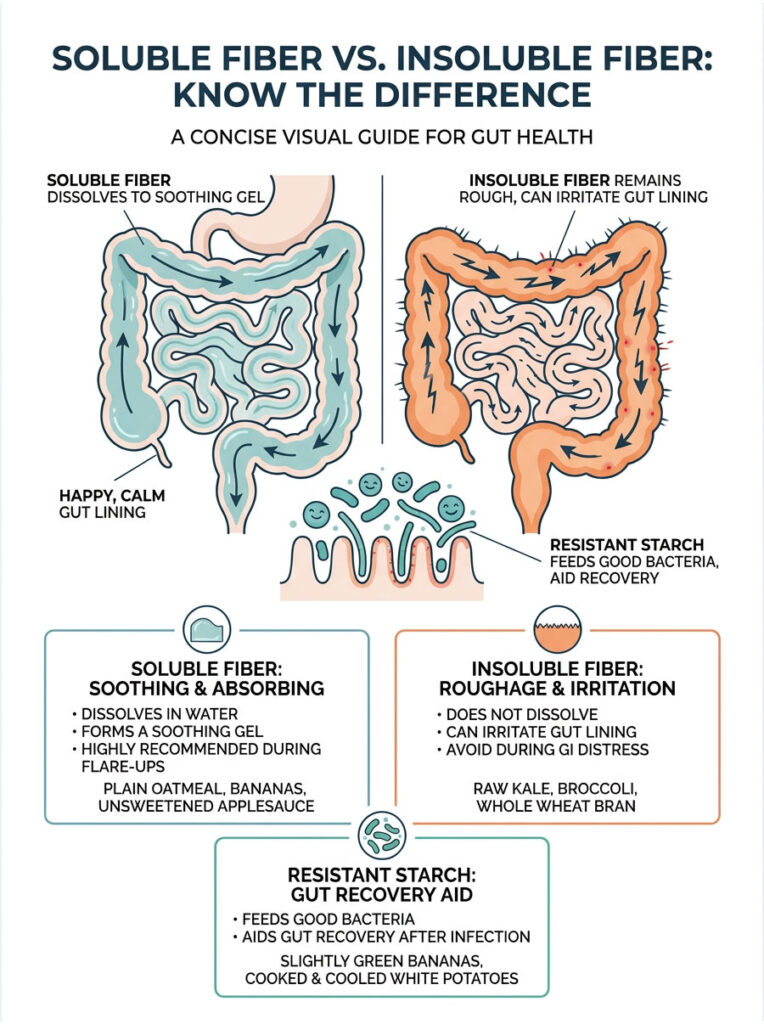
Soluble fiber dissolves in water and forms a thick, soothing, gel-like substance in the digestive tract. This gel slows down gastric emptying, traps excess fluid, and increases stool density. Foods like oatmeal, peeled potatoes, and bananas are rich in this helpful compound.
Insoluble fiber does not dissolve in water at all. It acts like a stiff broom sweeping aggressively through your intestines. Eating a raw kale salad or a bowl of bran cereal during a stomach bug will make your symptoms significantly worse.
Fiber Types in Gastrointestinal Recovery
| Fiber Category | How It Works in the Gut | Best Food Sources | Clinical Recommendation |
| Soluble Fiber | Absorbs water, forms a thick gel, slows gastric emptying, and increases stool density. | Bananas, unsweetened applesauce, plain oatmeal, peeled white potatoes. | Highly Recommended. Acts as a primary binding agent to stop symptoms fast. |
| Insoluble Fiber | Does not dissolve in water. Irritates gut lining and stimulates rapid peristalsis. | Raw kale, broccoli, whole wheat bran, seeds, tough fruit skins. | Strictly Avoid. Acts as a rough broom in the intestines, worsening symptoms. |
| Resistant Starch | Bypasses digestion to feed good bacteria, producing healing short-chain fatty acids. | Slightly green bananas, cooked and cooled white rice, cooked and cooled potatoes. | Recommended in Phase 3. Helps rebuild the gut microbiome after infection. |
Understanding these fiber categories helps you make smart choices at the grocery store. Always prioritize foods that are visually soft, easily mashed, and free of tough skins or seeds.
Hydration Science: Mastering Electrolyte Balance
When patients ask me what to eat for diarrhea, I usually redirect the conversation to what they are drinking first. Solid food is secondary to fluid resuscitation. If your cells are dehydrated, your digestive system cannot produce the enzymatic juices needed to break down solid food.

Hydration goes far beyond simply drinking eight glasses of tap water. Water does not just passively flow into your bloodstream on its own. It requires a specific biochemical mechanism to unlock the cellular gates. If you drink plain, unmineralized water during a severe bout of diarrhea, it will likely just pass straight through your system. This is where the concept of fluid osmolarity becomes essential.
How Your Body Actually Absorbs Water
In the lining of your small intestine, there are specialized proteins called sodium-glucose cotransporter 1 (SGLT1). These proteins function as tiny molecular water pumps.
For these pumps to pull water from the gut into the bloodstream, they need one molecule of sodium and one molecule of glucose present at the exact same time. When sodium and glucose bind to the SGLT1 protein together, the cellular gate opens. As the salt and sugar are pulled into the cell, water follows through a process called solvent drag.
That is the physiological secret behind clinical hydration. Plain tap water lacks sodium and glucose, so the cellular pumps stay shut. You end up excreting the water before it can actually hydrate your deeper tissues.
Why Commercial Sports Drinks Often Make Things Worse
Many people reach for bright-colored sports drinks when they are sick. In clinical practice, this habit often prolongs the illness. Sports drinks are formulated for healthy athletes sweating out salt, not for sick patients losing massive fluid volumes.
These beverages typically contain far too much sugar and not nearly enough sodium. The excess fructose overwhelms the SGLT1 pumps, sits unabsorbed in the gut, and ferments. This fermentation causes gas, painful bloating, and triggers osmotic fluid shifts that worsen bathroom trips.
For genuine fast relief, you need a precise medical ratio of salt to sugar. Always choose medical-grade hydration solutions over sugary athletic beverages.
Expert Tip: Apple juice, pear juice, and cherry juice are naturally very high in fructose and sorbitol. Giving these juices to anyone with an active stomach bug will almost certainly cause explosive osmotic diarrhea. Dilute juices by at least 50 percent with water, or better yet, avoid them entirely until symptoms resolve.
WHO Guidelines for Oral Rehydration Solution (ORS)
The global standard for rehydration is the Oral Rehydration Solution (ORS). An ORS is scientifically formulated with the exact low-osmolarity ratio of salt and sugar needed to activate those SGLT1 pumps. This makes ORS the gold standard for diarrhea recovery.
Commercial ORS products available in the USA include Pedialyte, Liquid I.V., and generic pharmacy brands. These are carefully balanced to push water directly into your bloodstream. They are essential tools for surviving the first 24 hours of illness.
The WHO formula calls for 75 mEq/L of sodium and 75 mmol/L of glucose. This specific concentration has saved millions of lives globally by preventing severe dehydration from cholera and dysentery. Keep a box of powdered ORS packets in your medicine cabinet at all times.
How to Make a Medical-Grade ORS at Home
If you cannot get to a pharmacy, you can make a medically approved ORS right in your kitchen. Start with one liter (roughly four cups) of clean, boiled, or bottled drinking water. Add exactly six level teaspoons of regular table sugar. Then add exactly one-half level teaspoon of standard table salt. Stir vigorously until everything dissolves completely. Sip slowly throughout the day to replace lost fluids.
Do not gulp the mixture quickly. A sudden, large volume of liquid can trigger the stretch receptors in your stomach wall and cause vomiting. Take small, measured sips every ten to fifteen minutes for optimal absorption.
Protein and Recovery: Rebuilding the Intestinal Lining
A major gap in traditional upset stomach advice is the complete lack of dietary protein. The classic BRAT diet focuses heavily on simple carbohydrates. While carbs are great for binding loose stool, they do nothing to repair the physical tissue damage to your intestinal walls.
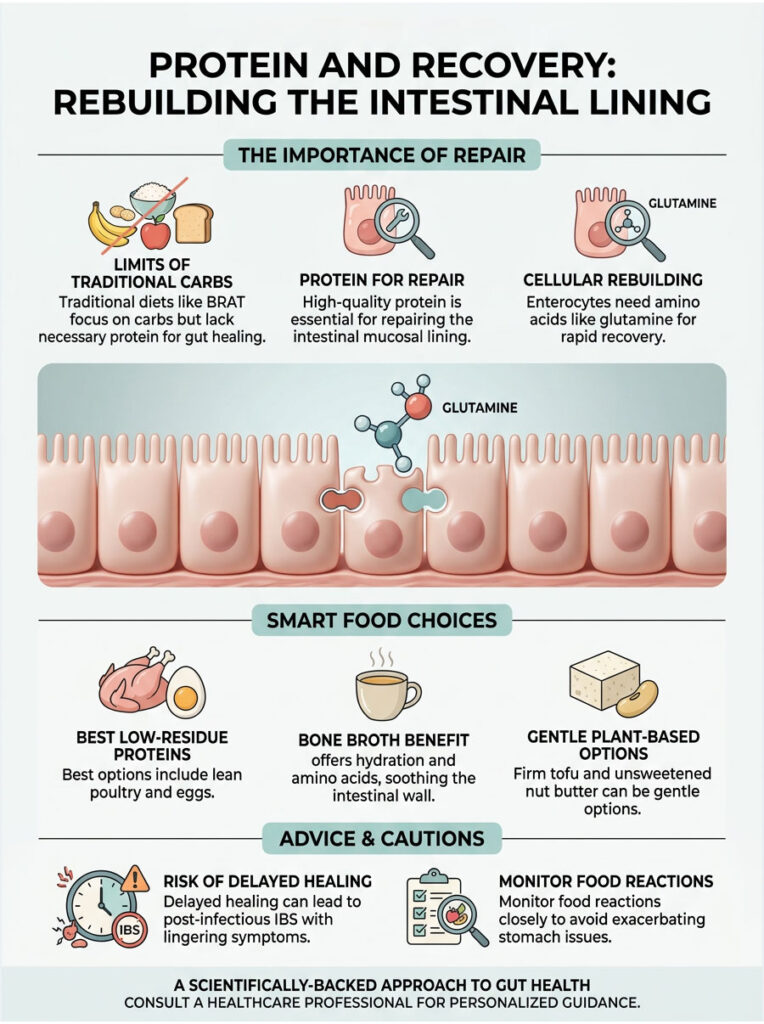
Your gut needs specific amino acids to rebuild the delicate mucosal lining damaged by infection or inflammation. By day two or three of an illness, high-quality protein must be introduced. But you cannot just eat a heavy, fatty steak. Red meat is tough to digest and sits in the stomach for hours, causing nausea.
You need proteins that require minimal digestive effort from your pancreas and gallbladder. The goal is to provide building blocks for cellular repair without triggering the gastrocolic reflex.
The Role of Enterocytes in Gut Healing
The cells lining your intestinal tract are called enterocytes. They have a rapid turnover rate, completely replacing themselves every three to five days. When a stomach bug hits, millions of these cells are destroyed.
To grow new enterocytes quickly, your body needs the amino acid glutamine. Glutamine is the primary fuel source for these intestinal cells. Without enough protein during recovery, enterocytes cannot regenerate properly.
This delayed healing is a primary cause of post-infectious IBS. Patients often experience lingering bloating and food sensitivities for months simply because their gut lining never fully repaired. Introducing gentle proteins early is the key to preventing that chronic problem.
Best Low-Residue Proteins for Easy Digestion
When selecting the best foods for fast relief, focus on lean poultry, eggs, and certain soy products. Boiled or baked skinless chicken breast is an excellent choice. It delivers high-quality protein without the saturated fat that irritates the bowel.
Scrambled eggs are another fantastic option for a recovering stomach. They are soft, easy to chew, and digest rapidly in the upper GI tract. The cooking method matters here. Avoid frying in oil, and skip the heavy butter, lard, or spicy seasonings. A simple pinch of salt is all you need.
The Healing Power of Bone Broth
If solid proteins still cause nausea, traditional bone broth is an exceptional liquid alternative. It offers a powerful dual benefit: critical hydration and vital amino acids delivered at the same time.
The slow, 24-hour simmering process extracts collagen and gelatin directly from the bones. Gelatin is incredibly soothing to the inflamed intestinal wall, acting like a liquid bandage. Bone broth is also naturally packed with the glutamine your enterocytes desperately need.
Additionally, properly made bone broth contains high amounts of sodium and trace minerals. Sipping warm, clear bone broth can calm painful stomach spasms while providing the structural nutrients needed to break the cycle of rapid bowel motility.
Plant-Based Protein Options for Sensitive Stomachs
If you follow a vegetarian or vegan lifestyle, getting gentle protein takes careful selection. Many plant-based proteins like beans and lentils are packed with insoluble fiber and gas-producing complex sugars. Those will absolutely wreck a sensitive, recovering gut.
Firm tofu is an excellent low-residue plant protein. Because it is made from pressed soy curds, the fibrous parts of the soybean have been removed. It is soft, easily absorbed, and provides a complete amino acid profile.
Smooth, unsweetened peanut butter or almond butter can also work in very small quantities. Spread a thin layer on plain white toast for a small boost of protein and calories. Monitor your body’s reaction closely, as the natural fat in nut butters can sometimes be too heavy for a very weak stomach.
Restoring the Gut Microbiome: Probiotics and Fermented Foods
Once the acute phase has passed, your digestive system is in a highly vulnerable state. The aggressive flushing action of your illness does not just remove the bad bacteria. It also washes away massive amounts of your beneficial gut flora.

This severe disruption in your microbiome is exactly why many people struggle with lingering digestive issues for weeks after a stomach bug. If you do not actively repopulate your gut with beneficial microbes, opportunistic pathogens can easily take over, leading to chronic bloating, trapped gas, and irregular bowel movements.
The Post-Infectious Microbiome Wipeout
Think of your gut microbiome as a dense, thriving forest. A severe intestinal infection acts like a massive forest fire, burning down both the weeds and the ancient trees. After the fire, the soil is barren and susceptible to invasive species.
In medical terms, this barren state is called gut dysbiosis. Without good bacteria to produce healing short-chain fatty acids, your colon environment becomes alkaline and hostile. You lose the ability to properly ferment complex carbohydrates, leading to severe gas whenever you eat normal foods.
You must actively reseed this forest with the right types of beneficial bacteria. But be careful. Introducing the wrong bacteria or heavy dairy products too soon can backfire and trigger a relapse.
Evidence-Based Probiotic Strains for Recovery
Not all probiotics work for gastrointestinal distress. Walking into a supplement store and grabbing a random bottle of bacteria will likely not give you the results you want. Clinical research has identified very specific strains that effectively help stop symptoms.
The most heavily researched probiotic for this condition is Saccharomyces boulardii. Interestingly, it is not a bacteria at all, but a beneficial yeast. Because it is a yeast, antibiotics do not affect it, making it ideal for antibiotic-associated illness.
Another highly effective strain is Lactobacillus rhamnosus GG. This bacteria is known for surviving the harsh acidic environment of the stomach. Clinical trials consistently show that these specific strains can significantly shorten a stomach flu recovery timeline.
Is Yogurt Safe During Diarrhea?
One of the most common questions I hear is whether yogurt is safe during an illness. The answer requires some nuance. In general, dairy is off-limits during an acute flare-up because gut infections often cause temporary lactose intolerance.
Your inflamed intestinal lining temporarily stops producing lactase, the enzyme needed to digest milk sugars. However, fermented yogurt is a unique exception, provided you choose the right kind. Plain, low-sugar yogurt with active live cultures is actually beneficial.
During fermentation, the bacteria in yogurt consume and break down the majority of the lactose. This pre-digestion makes it safe even for those with temporary lactose sensitivity. Traditional Greek yogurt is an excellent choice for rebuilding gut flora.
Introducing Gentle Prebiotics for Long-Term Health
Probiotics are the beneficial bacteria themselves, while prebiotics are the foods that feed those bacteria. Once you have stopped the acute symptoms, you need to start feeding your new microbiome. Otherwise, the good bacteria will simply die off and leave your system.
Gentle prebiotics include cooked onions, cooked garlic, asparagus, and slightly green bananas. These contain inulin and fructooligosaccharides (FOS). Introduce them very slowly, starting with tiny portions, to avoid overwhelming your system with sudden gas production.
A great transitional meal is a small portion of white rice mixed with thoroughly cooked carrots and a tiny bit of garlic powder. This provides the perfect mix of low-residue starches and gentle prebiotics to stimulate healthy bacterial growth.
Foods to Avoid: What Triggers Osmotic Diarrhea and Peristalsis
Knowing what to eat for diarrhea is only half the battle. Knowing what to strictly avoid is arguably more important. One dietary mistake can completely reset your recovery and send you rushing back to the bathroom.

When your gut is compromised, it loses its normal ability to process complex molecules. Foods you would normally consider healthy suddenly become chemical irritants. The most common culprits fall into three categories: osmotic laxatives (excess sugars), chemical stimulants (caffeine), and heavy macronutrients (saturated fats).
Sugar Alcohols and Artificial Sweeteners
Sugar alcohols and artificial sweeteners hide in many diet sodas, sugar-free gums, and low-calorie protein bars. Ingredients ending in “-ol,” such as sorbitol, xylitol, mannitol, and erythritol, are notorious for causing digestive distress even in healthy people.
Your body cannot fully absorb these compounds. They travel intact to your large intestine, where they act as powerful osmotic laxatives, drawing massive amounts of water from the bloodstream into the bowel. The bacteria in your colon also rapidly ferment them, producing large amounts of trapped gas. The combination of excess water and expanding gas leads to explosive, watery stools and severe cramping.
The Impact of Fats and Fried Foods
High-fat meals are incredibly difficult for a compromised gut to handle. Fat delays stomach emptying, which can worsen nausea and fullness. But the real danger happens once that heavy fat reaches the intestines.
Heavy fats trigger a massive release of bile from the gallbladder and stimulate the gastrocolic reflex. This reflex causes the entire colon to contract violently, creating an immediate and urgent need to use the bathroom. Fried chicken, greasy burgers, and heavy cream are the exact opposite of what you need.
Even healthy fats like avocados, olive oil, and fatty salmon should be avoided during the first 48 hours. Your digestive system needs a complete break from producing bile and lipase enzymes. Stick to lean, fat-free proteins until you are fully stabilized.
Why Caffeine Makes Diarrhea Worse
Caffeine is a trigger that people often overlook. Many patients brew a cup of black or green tea, thinking the warm liquid will soothe their stomach. But caffeine is not just a nervous system stimulant, it is also a powerful gastrointestinal stimulant.
It artificially increases peristalsis, pushing food through the intestines much faster than normal. This rapid transit prevents the colon from absorbing water, leading to loose stools. Caffeine also acts as a mild diuretic, forcing your kidneys to excrete water and worsening dehydration.
If you want a warm beverage, choose a naturally caffeine-free herbal option. Peppermint tea contains natural antispasmodic compounds that gently relax the smooth muscles of the intestines. Chamomile tea is also soothing and helps reduce localized GI inflammation.
Dairy Products and Temporary Lactose Intolerance
As mentioned, acute gut infections frequently strip away lactase enzymes from your intestinal lining. Without lactase, your body cannot break down lactose, the primary sugar in milk. Unabsorbed lactose acts just like a sugar alcohol, triggering powerful osmotic fluid shifts.
Drinking regular cow’s milk or eating ice cream during a stomach bug is a recipe for disaster. The lactose ferments in the colon, causing severe bloating, foul-smelling gas, and painful cramping. Strictly avoid all liquid milk, soft cheeses, and heavy creams.
This temporary lactose intolerance usually resolves within a week or two as your enterocytes regenerate. Until then, use lactose-free alternatives like almond milk, or stick exclusively to fermented dairy like plain Greek yogurt.
Safe Foods vs. Trigger Foods for Acute Diarrhea
| Category | Safe Option | Trigger to Avoid | Why to Avoid the Trigger |
| Beverages | ORS, Clear Bone Broth, Peppermint Tea | Black Coffee, Caffeinated Soda, Energy Drinks | Caffeine stimulates rapid peristalsis and acts as a diuretic, worsening dehydration. |
| Carbohydrates | White Rice, Plain Toast, Saltine Crackers | Whole Wheat Bread, Bran Cereals, Brown Rice | Insoluble fiber in whole grains irritates the sensitive intestinal lining. |
| Proteins | Skinless Baked Chicken, Scrambled Eggs, Firm Tofu | Fried Chicken, Greasy Burgers, Processed Sausage | High fat delays stomach emptying but triggers rapid, violent colon contractions. |
| Fruits/Dairy | Slightly Green Bananas, Applesauce, Plain Kefir | Grapes, Berries, Ice Cream, Apple Juice | High fructose, tough fruit skins, and heavy lactose draw excess water into the gut. |
Keep this table handy during your recovery. When you are exhausted and hungry, it is easy to make a poor choice out of convenience. Stick to the safe column until you experience at least 24 hours of completely normal bowel movements.
A Practical 48-Hour Meal Plan for Fast Diarrhea Relief
Theory is useful, but practical application is what actually heals you. When a patient asks me what to eat for diarrhea, I do not hand them a random list of foods. I give them a structured, phase-by-phase timeline.

Your digestive system needs a phased approach to recovery. You cannot jump from liquid stools to a full plate of chicken and rice. A proper recovery timeline is broken into specific phases that gradually test the gut’s tolerance. If symptoms return during any phase, step back to the previous phase for another 12 hours.
Phase 1: Fluid Resuscitation (Hours 0 to 12)
During the first 12 hours of acute illness, avoid solid food entirely. Your gut is severely inflamed, and any solid matter will likely be expelled immediately. This phase focuses entirely on preventing dehydration and replacing electrolyte losses.
Start with a medical-grade ORS. Sip 2 to 4 ounces every 15 to 30 minutes. Do not chug, as sudden volume expansion will trigger vomiting. If nausea is severe, suck on ice chips or freeze your ORS into small popsicles.
Phase 2: Testing Tolerance with Clear Broths (Hours 12 to 24)
If vomiting has subsided and you can keep clear liquids down, introduce savory broths. Warm, clear bone broth or simple chicken bouillon are perfect for this phase. The warmth relaxes the stomach muscles, and the sodium helps pull water into your tissues.
Continue sipping ORS alongside the broth. You can also add weak, caffeine-free peppermint tea. Still no solid food during this window. Monitor your bowel movements closely. If frequency slows and your urine turns pale yellow, you are successfully rehydrating.
Phase 3: Introducing Soluble Binders (Hours 24 to 36)
Once bowel movement frequency has significantly slowed, you can introduce tiny amounts of solid food. This is where the bland diet comes in. The goal is to use soluble fiber to form a gel in the gut and bind loose stool.
Start with half a slightly green banana or a very small bowl of unsweetened applesauce. Wait two hours and monitor your reaction. If it stays down without triggering cramps, introduce a small portion of white rice. Keep portions extremely small, eating two or three bites every few hours. No fats, proteins, or dairy during this phase.
Phase 4: Transitioning to Low-Residue Proteins (Hours 36 to 48)
If your stool consistency has visibly improved and energy is returning, it is time to rebuild the mucosal lining. Staying on the carb-heavy BRAT diet too long will deprive you of vital energy.
Introduce a single scrambled egg cooked without butter, or a small piece of boiled chicken breast. Pair it with white rice or toast. You can also add a small cup of plain Greek yogurt with live cultures to start repopulating gut flora. Continue avoiding onions, garlic, excess sugar, and raw vegetables until you feel fully recovered.
Advanced Dietary Strategies for Chronic Diarrhea
While acute infections usually resolve within a few days, some patients experience symptoms that linger for weeks or months. If that describes you, the standard 48-hour BRAT diet will not solve the problem. Chronic diarrhea requires a more sophisticated dietary investigation.
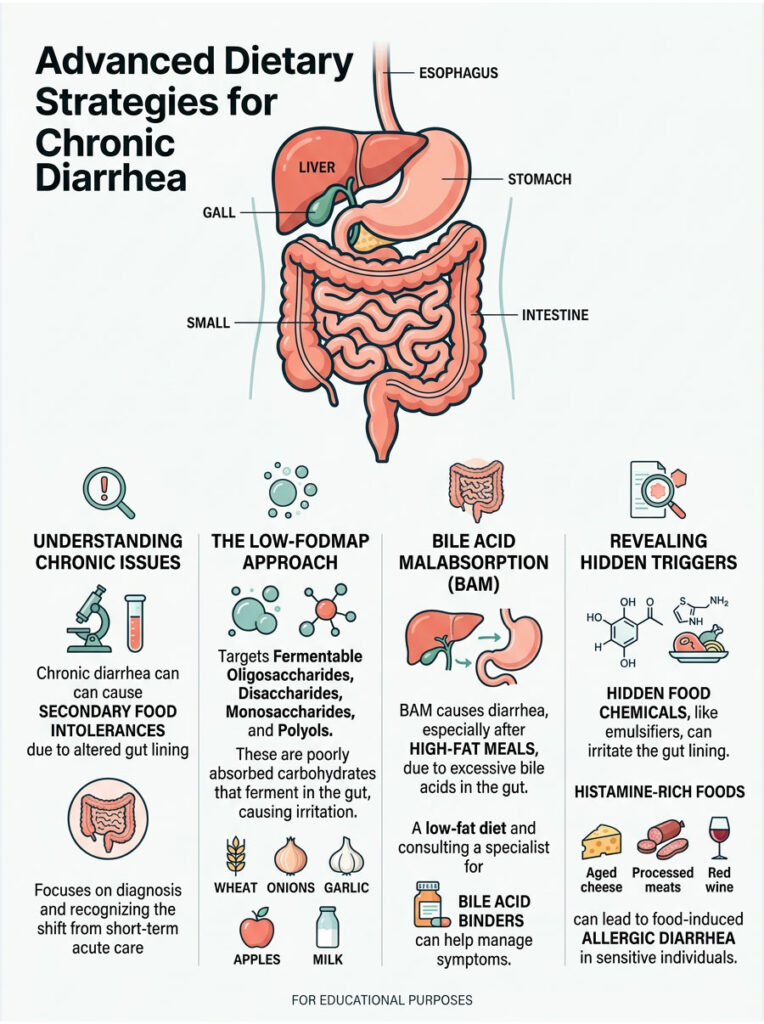
When the gut stays inflamed long-term, it often develops secondary food intolerances. Foods you have eaten your entire life suddenly cause severe bloating and urgency. Advanced clinical protocols like the low-FODMAP approach, bile acid management, and hidden food chemical sensitivities can help you reclaim your quality of life.
Understanding the Low-FODMAP Approach
FODMAPs stands for fermentable oligosaccharides, disaccharides, monosaccharides, and polyols. These are complex carbohydrates and sugars that are poorly absorbed in the small intestine. When they reach the colon, bacteria ferment them rapidly, producing massive amounts of trapped gas.
This gas stretches the colon wall, triggering pain receptors and causing rapid bowel motility. Common high-FODMAP foods include wheat, onions, garlic, apples, milk, and certain beans. If you have chronic post-infectious IBS, a strict low-FODMAP elimination diet is worth trying.
By temporarily removing these fermentable sugars, you starve the overgrown bacteria and reduce osmotic fluid shifts in the bowel. After a few weeks of strict elimination, you slowly reintroduce them one by one to identify your personal triggers.
Bile Acid Malabsorption and Dietary Fat
Sometimes chronic diarrhea is not caused by food sensitivities at all, but by bile acid malabsorption (BAM). Your liver produces bile to digest dietary fats. Normally, this bile is reabsorbed at the end of the small intestine and recycled.
If your intestinal lining is damaged, bile escapes into the large intestine. Bile acids are extremely irritating to the colon and act as a chemical laxative, causing explosive, watery stools, especially after high-fat meals.
If you notice symptoms are worst right after eating greasy food, BAM could be the culprit. A strict low-fat diet combined with prescription bile acid binders from your gastroenterologist can provide dramatic relief.
Identifying Hidden Food Intolerances
Beyond FODMAPs and fats, modern processed foods contain hidden chemicals that can trigger severe bowel issues. Emulsifiers like carrageenan, guar gum, and polysorbate 80 are frequently added to almond milk, ice cream, and protein shakes to improve texture.
Emerging clinical research shows these emulsifiers can directly degrade the protective mucus layer of your intestines. This allows bacteria to touch the intestinal wall directly, triggering chronic inflammation and loose stools. Reading ingredient labels carefully is essential.
Also pay attention to histamine-rich foods. Fermented foods, aged cheeses, and leftover meats contain high levels of histamine. If your gut is compromised, you may lack the DAO enzyme needed to break it down, leading to food-induced allergic diarrhea.
When to Seek Immediate Medical Attention
While knowing what to eat for diarrhea resolves the majority of mild to moderate cases, dietary interventions have their limits. Sometimes, gastrointestinal distress can signal a severe infection or a dangerous structural issue. Recognizing when home remedies are no longer enough is vital.

If you are losing fluid faster than you can replace it orally, no amount of ORS or white rice will be sufficient. Intravenous (IV) fluids in a hospital setting become necessary to prevent organ damage. Do not try to push through severe symptoms at home.
Warning Signs and Red Flags
According to clinical guidelines from the Mayo Clinic and CDC, consult a doctor if symptoms persist beyond three days without visible improvement. Prolonged diarrhea may indicate a severe pathogen that your body cannot fight alone, possibly requiring targeted antibiotics.
Visual changes in your stool need immediate attention. Bright red blood in the stool, or black, tarry stool (which strongly suggests upper GI bleeding), should send you to the emergency room immediately. A high fever exceeding 102 degrees Fahrenheit is another major warning sign. Severe, localized abdominal pain that does not improve after a bowel movement could indicate appendicitis or a bowel obstruction.
Recognizing Severe Dehydration
Watch yourself and family members closely for signs of severe dehydration. Early indicators include extreme thirst, a completely dry or sticky mouth, and decreased urination. When you do urinate, the color will be dark amber rather than pale yellow.
As dehydration worsens, you may notice an inability to produce tears, deeply sunken eyes, or no urination for more than eight hours. Feeling dizzy, confused, or lightheaded upon standing points to a dangerous drop in blood pressure caused by severe fluid depletion. If you or a loved one cannot stand without fainting, call emergency services immediately.
When to Ask for Stool Testing
If you have recently traveled internationally, drank untreated water, or completed a heavy round of antibiotics, let your doctor know. These situations put you at high risk for aggressive pathogens like Giardia, Campylobacter, or Clostridioides difficile (C. diff).
In these cases, dietary changes alone will not cure the infection. Your doctor will need to order a comprehensive stool PCR test to identify the exact pathogen and prescribe the right antimicrobial therapy.
Never take over-the-counter anti-motility drugs like loperamide (Imodium) if you have a high fever or bloody stools. Stopping the diarrhea traps dangerous bacteria and toxins inside your body, which can potentially lead to toxic megacolon or sepsis.
Final Thoughts: Taking Control of Your Digestive Recovery
Recovering from gastrointestinal distress does not have to be a miserable guessing game. With a strategic, science-based approach to nutrition and hydration, you can dramatically shorten your recovery time and protect your body from serious complications.
Your first priority should always be cellular hydration through an Oral Rehydration Solution. Once you are hydrated, lean on soluble fiber as your primary tool for firming up bowel movements. The best foods for fast relief, including white rice, slightly green bananas, unsweetened applesauce, and plain toast, all require minimal digestive effort.
Remember that a bland diet is only a temporary tool, not a long-term plan. Transition to lean, low-residue proteins like boiled chicken and scrambled eggs within 36 to 48 hours to support tissue repair. Strictly avoid insoluble fiber, high-fat meals, artificial sweeteners, and caffeine until your system fully stabilizes.
By understanding the mechanics of your gut and respecting the healing timeline, you take real control of your digestive health. Knowing what to eat for diarrhea is not just about comfort. It is about preventing dehydration, supporting tissue repair, and guiding your body smoothly back to normal.
Frequently Asked Questions
What are the absolute best foods for fast relief from diarrhea?
To achieve rapid relief, focus on low-residue carbohydrates and soluble fiber. The most effective options are slightly green bananas, white rice, unsweetened applesauce, and plain white toast. These foods act as binding agents, absorbing excess water in the colon to increase stool density. As symptoms stabilize, you can introduce lean, low-fat proteins like skinless baked chicken or scrambled eggs to provide the amino acids necessary for repairing the intestinal lining.
Why is soluble fiber recommended over insoluble fiber during a flare-up?
Soluble fiber dissolves in water to form a soothing, gel-like substance that slows gastric emptying and firms up stool consistency. In contrast, insoluble fiber—found in raw vegetables and whole grains—acts as a mechanical irritant. It stimulates rapid peristalsis (muscle contractions), which can worsen hyper-motility and abdominal cramping. During an acute episode, always choose peeled and cooked produce over raw, high-fiber alternatives.
Can I drink sports drinks to stay hydrated during gastrointestinal distress?
While popular, commercial sports drinks are often counterproductive. They typically contain excessive sugar and insufficient sodium, which can lead to high osmolarity in the gut. This imbalance pulls water from your bloodstream into your intestines, potentially worsening osmotic diarrhea. For clinical-grade hydration, it is better to use an Oral Rehydration Solution (ORS) that utilizes the sodium-glucose cotransport mechanism to maximize cellular water absorption.
Is the BRAT diet still the clinical gold standard for recovery?
The BRAT diet (Bananas, Rice, Applesauce, Toast) remains a useful short-term strategy for the first 24 to 48 hours because these foods are easy to digest. However, modern clinical guidelines suggest transitioning to a more nutrient-dense diet quickly. Prolonged use of the BRAT diet lacks the protein and healthy fats required for enterocyte regeneration and immune function. Once bowel movements slow, you should introduce lean proteins and fermented foods to support full recovery.
Why does dairy often make diarrhea worse even if I’m not lactose intolerant?
Acute gastrointestinal infections often cause a temporary condition called secondary lactose intolerance. The inflammation blunts the villi in your small intestine, where the enzyme lactase is produced. Without enough lactase, the milk sugar (lactose) remains unabsorbed, ferments in the colon, and draws in water via osmosis. It is best to avoid liquid milk and soft cheeses for at least one to two weeks until your intestinal brush border has fully healed.
Which probiotics are most effective for restoring gut health after an infection?
Clinical research highlights specific strains for diarrhea recovery, most notably the beneficial yeast Saccharomyces boulardii and the bacteria Lactobacillus rhamnosus GG. Unlike many standard probiotics, S. boulardii is resistant to antibiotics and highly effective at neutralizing bacterial toxins. These strains help shorten the duration of illness and prevent post-infectious gut dysbiosis by actively reseeding the microbiome.
How do I make a medical-grade Oral Rehydration Solution (ORS) at home?
To create a DIY ORS that meets World Health Organization standards, mix one liter of clean water with six level teaspoons of sugar and one-half level teaspoon of salt. This precise ratio of glucose to sodium activates the SGLT1 transport proteins in your small intestine, forcing water into your bloodstream even when the gut is inflamed. Sip the solution slowly—about 2 to 4 ounces every 15 minutes—to avoid triggering the vomit reflex.
What foods should I strictly avoid to prevent worsening my symptoms?
You must eliminate high-fat fried foods, caffeine, and artificial sweeteners like sorbitol or xylitol. Fats trigger the gastrocolic reflex, leading to urgent bowel contractions, while caffeine is a stimulant that accelerates intestinal transit time. Sugar alcohols act as powerful osmotic laxatives that the body cannot absorb, leading to explosive, watery stools and significant gas production.
Is bone broth better than plain water for rehydration?
Yes, bone broth is an exceptional recovery tool because it provides more than just fluid. It contains electrolytes like sodium and potassium, along with the amino acid glutamine, which is the primary fuel source for healing intestinal cells (enterocytes). The gelatin in properly prepared broth also acts as a soothing agent for the inflamed mucosal lining, making it superior to plain tap water during the first 24 hours of illness.
When should I stop home treatment and see a doctor for diarrhea?
Seek immediate medical attention if you observe ‘red flag’ symptoms: high fever (over 102°F), blood in the stool, or black, tarry stools. Additionally, if you show signs of severe clinical dehydration—such as extreme dizziness, an inability to urinate for 8 hours, or sunken eyes—you may require IV fluid resuscitation. Diarrhea lasting longer than three days without improvement also warrants a clinical evaluation and potential stool PCR testing.
Why do applesauce and bananas help firm up stool so effectively?
Both applesauce and bananas are rich in pectin, a type of soluble fiber. Pectin has unique binding properties; it absorbs excess liquid in the intestinal tract and transforms it into a thicker mass. This slows down the transit time of waste through the colon, allowing for better water reabsorption and resulting in firmer, more formed bowel movements.
Can chronic diarrhea be managed with the same foods as acute diarrhea?
Chronic diarrhea (lasting over four weeks) requires a different approach than acute episodes. While binding foods like rice can provide temporary relief, chronic issues often stem from underlying conditions like Bile Acid Malabsorption (BAM) or Small Intestinal Bacterial Overgrowth (SIBO). In these cases, a clinical Registered Dietitian might recommend a Low-FODMAP diet to identify specific fermentable carbohydrate triggers that are causing ongoing osmotic shifts and gas.
Disclaimer
This article is for informational purposes only and does not constitute medical advice. The dietary strategies discussed, including what to eat for diarrhea, are based on general clinical principles. Always consult a qualified healthcare professional or Registered Dietitian before making health decisions, especially if you experience high fever, bloody stools, or signs of severe dehydration.
References
- American College of Gastroenterology – https://gi.org/ – Clinical guidelines on the prevalence and management of acute gastrointestinal distress in adults.
- Mayo Clinic – https://www.mayoclinic.org/ – Data regarding the risks of clinical dehydration and symptoms requiring immediate medical intervention.
- Centers for Disease Control and Prevention (CDC) – https://www.cdc.gov/ – Statistics on norovirus impact and viral causes of acute gastroenteritis in the United States.
- World Health Organization (WHO) – https://www.who.int/ – Official formulations and guidelines for Oral Rehydration Salts (ORS) and global rehydration standards.
- Academy of Nutrition and Dietetics – https://www.eatright.org/ – Clinical perspectives on the evolution of the BRAT diet and low-residue nutritional protocols.
- National Institutes of Health (NIH) – https://www.nih.gov/ – Research regarding the efficacy of specific probiotic strains like Saccharomyces boulardii for gut recovery.
- Journal of Clinical Gastroenterology – https://journals.lww.com/jcge/ – Peer-reviewed studies on the role of soluble fiber and pectin in managing stool consistency.