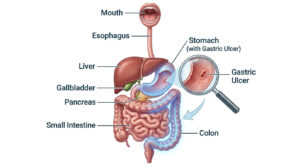
As a gastroenterologist with over 15 years of clinical experience, I see patients every week who are genuinely worried about what they find in the toilet. Noticing what looks like white mucus in stool can be startling, and most people immediately jump to worst-case scenarios.
Table of Contents
Before you spiral into anxiety, take a breath. Your gut is one of the most communicative organs in your body. The digestive tract naturally produces clear, microscopic fluids to keep waste moving smoothly. But when that fluid becomes thick, opaque, or clearly visible, it is your body sending a signal that something has changed.
Visible discharge means the internal mechanics of your digestion have shifted. In my practice, I always tell patients that understanding what is happening inside your gut is the first step toward feeling better. In this article, we will walk through the exact causes of this symptom, from harmless dietary changes to more serious inflammatory conditions.
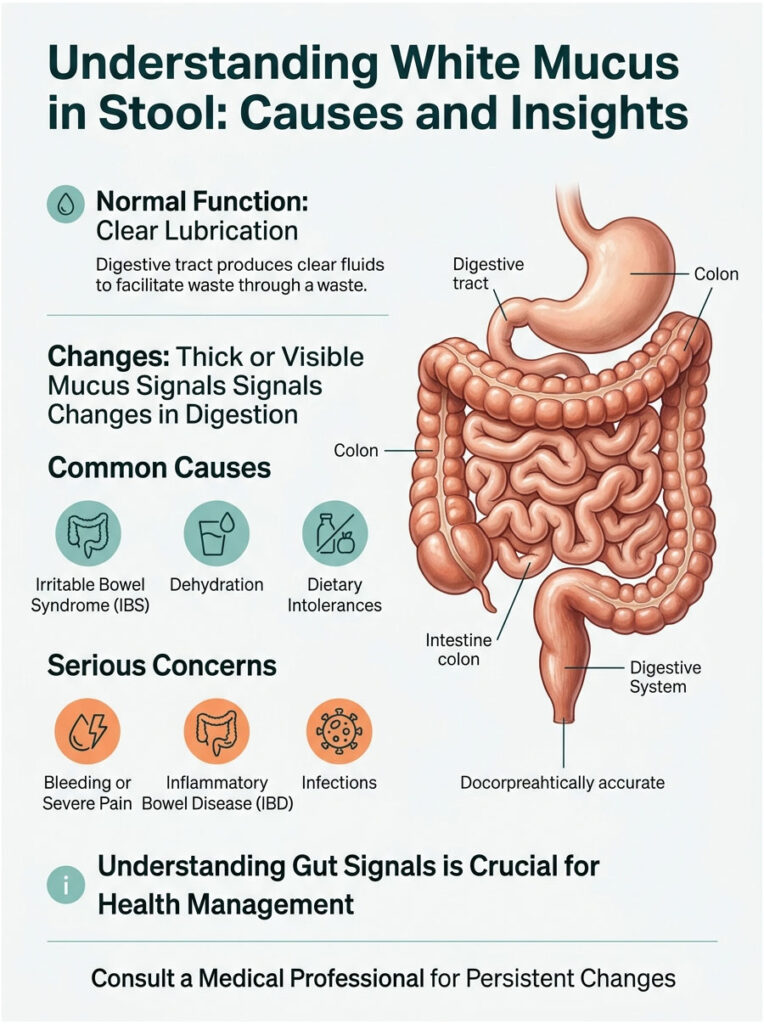
You will learn how to read these signals accurately and when it is time to call a doctor. Let us break down the science so you can stop worrying and start taking action.
Quick Answer: Visible white mucus in stool is most often caused by Irritable Bowel Syndrome (IBS), dehydration, or dietary intolerances. However, if mucus appears alongside bleeding, severe abdominal pain, or unexplained weight loss, it may point to Inflammatory Bowel Disease (IBD) or a gastrointestinal infection. Always consult a medical professional if you notice persistent changes in your bowel habits.
Key Statistics on Gut Health and Mucus Production
10% to 15%: The estimated percentage of American adults living with Irritable Bowel Syndrome, according to the American College of Gastroenterology.
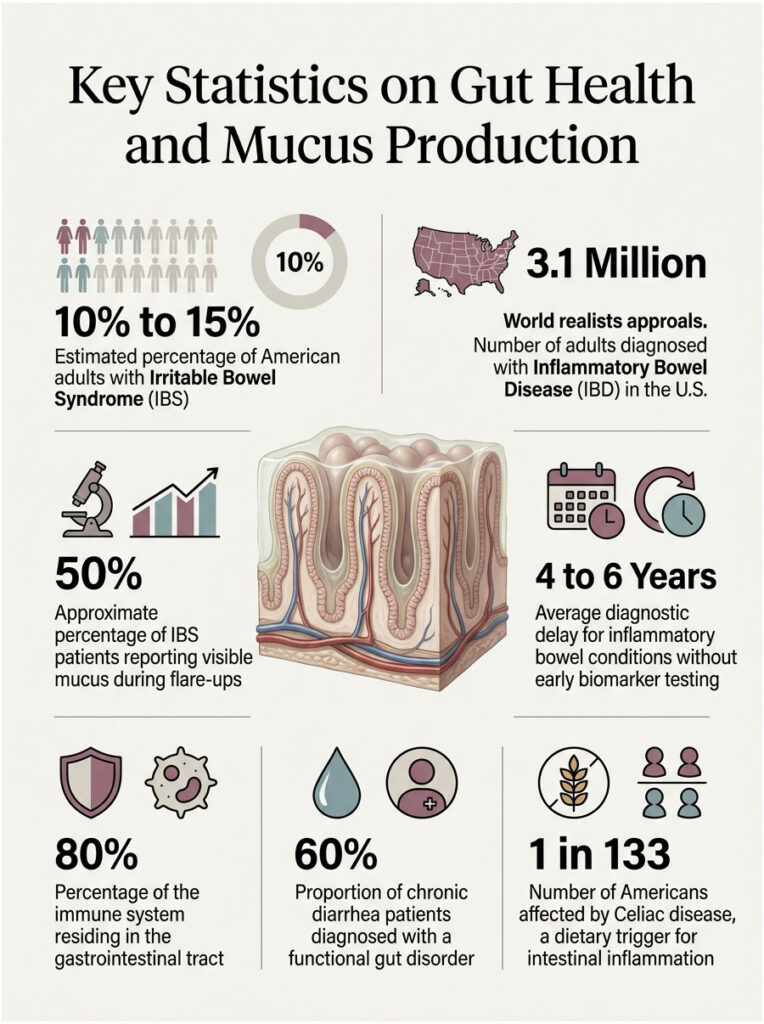
3.1 Million: The number of adults in the United States diagnosed with Inflammatory Bowel Disease (CDC, 2023).
50%: The approximate percentage of IBS patients who report visible mucus in bowel movements during acute flare-ups.
4 to 6 Years: The average diagnostic delay for inflammatory bowel conditions when early biomarker testing is skipped.
80%: The percentage of your immune system that lives directly within your gastrointestinal tract.
60%: The proportion of patients with unexplained chronic diarrhea who are eventually diagnosed with a functional gut disorder.
1 in 133: The number of Americans affected by Celiac disease, a significant dietary trigger for intestinal inflammation.
How Intestinal Mucus Works: Why White Mucus in Stool Forms
To understand why white mucus in stool appears, you need to know how a healthy gut operates. The human digestive tract is lined with a specialized barrier called the epithelial lining. This cellular layer is incredibly thin, measuring only one cell thick in many places. It separates the active immune system in your bloodstream from the trillions of bacteria inside your colon.
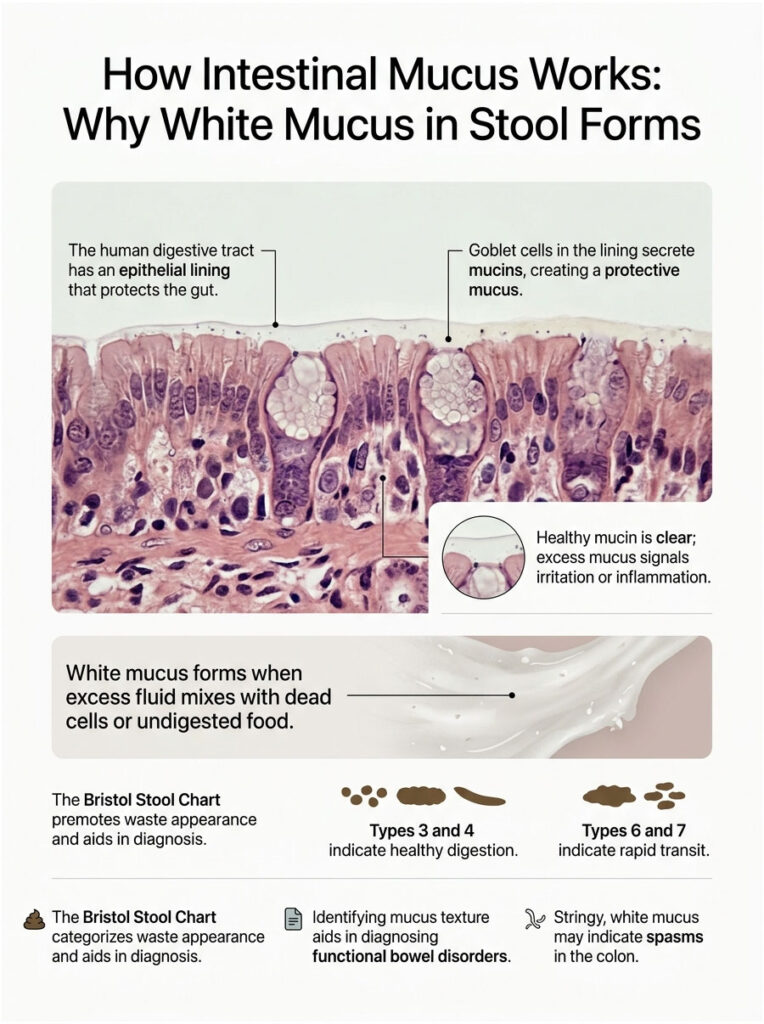
To protect this delicate barrier, the body relies on a built-in defense system. Without this protective layer, the friction and acids of digestion would seriously damage your internal tissues. Your body must constantly produce lubrication to keep everything running smoothly.
Expert Tip: Think of intestinal mucus like motor oil in your car engine. It creates a slick, protective coating that keeps the rough edges of digested food from scraping against your colon walls.
What Is Mucus and Why Does the Body Produce It?
Scattered throughout the epithelial lining are specialized structures called goblet cells. These tiny, cup-shaped cellular factories have one main job: they constantly secrete a gel-like substance made of water, lipids, and proteins called mucins.
In a healthy person, this mucin layer is completely clear and invisible to the naked eye. It coats the inside of the large intestine, letting solid waste pass smoothly without tearing the tissue. You actually pass a small amount of this clear fluid every time you use the restroom.
When the gut becomes irritated or inflamed, the baseline shifts. Goblet cells sense the danger and ramp up production dramatically. They pump out large amounts of extra fluid to flush the irritating substances out of your body.
Here is the key part. When this excess fluid mixes with dead white blood cells, undigested dietary proteins, or cellular debris, it turns cloudy and opaque. This is exactly how white mucus in stool forms.
The Bristol Stool Chart and Visual Identification
Gastroenterologists rely on a standard visual tool called the Bristol Stool Chart to evaluate digestion. This chart helps categorize the transit time of waste based on its physical appearance. Looking at Bristol Stool Chart mucus patterns is one way we diagnose functional bowel disorders.
The chart ranges from Type 1 (hard, separate lumps) to Type 7 (entirely liquid). Types 3 and 4 are considered ideal for healthy digestion. When waste moves too quickly, as in Types 6 and 7, the colon does not have enough time to reabsorb excess fluids.
Identifying the exact texture matters for a proper diagnosis. Is the substance a thin film coating the surface of the waste? Or is it thick, clumpy, and jelly-like?
Patients with fast transit times often notice Bristol Stool Chart mucus clinging to loose, watery bowel movements. Stringy, gelatinous, or opaque white strands usually point to a functional spasm happening in the colon.
Primary Functional Causes of White Mucus in Stool
When a patient walks into my clinic reporting white mucus in stool, my first clinical thought is usually a functional disorder. Functional disorders mean the physical structure of the gut is perfectly intact. The problem is in how the gut moves, contracts, and operates.
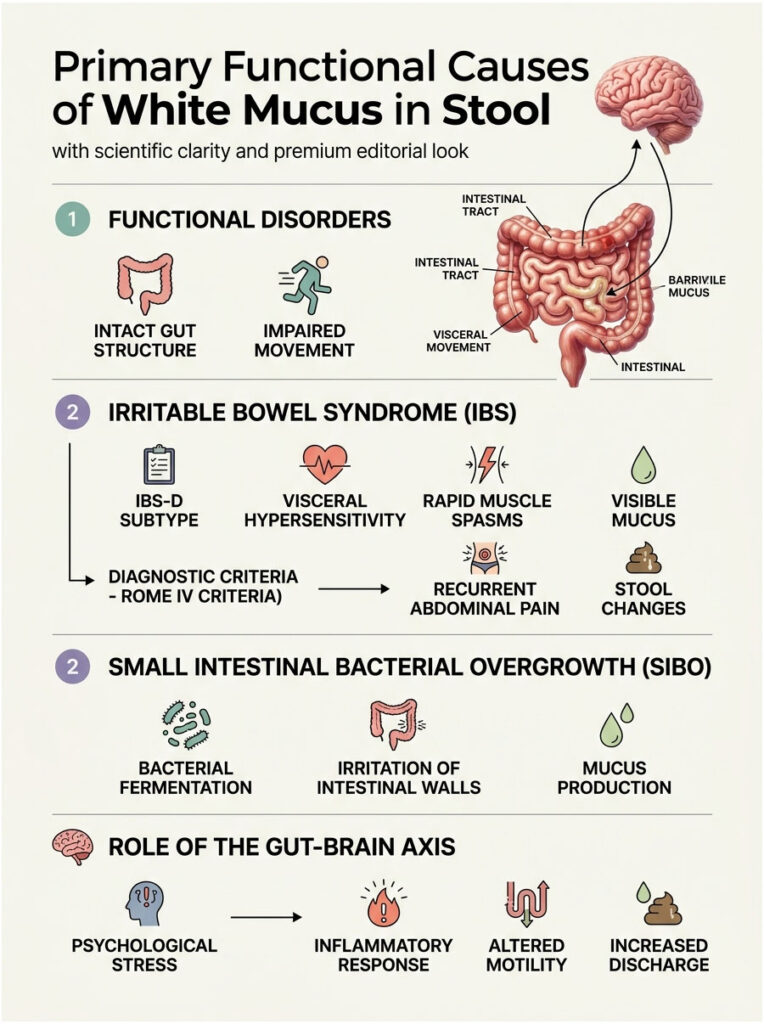
The vast majority of these cases are tied to Irritable Bowel Syndrome. This chronic condition changes how the nerves and muscles in the digestive tract communicate with your brain. It is essentially a software problem, not a hardware problem.
Irritable Bowel Syndrome (IBS)
Irritable Bowel Syndrome is the leading cause of visible discharge in otherwise healthy adults. It is a complex condition driven by visceral hypersensitivity in the gut’s nervous system. Your intestines become overly reactive to normal digestive processes.
IBS-D, the diarrhea-predominant subtype, is particularly relevant here. In IBS-D, the colon experiences rapid, chaotic, and often painful muscle spasms. These spasms push waste through the digestive system much too fast.
Because transit time is so short, the protective mucosal layer gets swept away before it can be reabsorbed. This produces highly visible mucus in bowel movements. The body then rushes to produce even more fluid to replace what was lost.
Gastroenterologists use the Rome IV criteria to make an official diagnosis. If you have recurrent abdominal pain at least one day per week, combined with noticeable changes in stool frequency or form, you likely meet the criteria. Seeing white mucus in stool is considered a classic supportive symptom of an IBS flare-up.
Small Intestinal Bacterial Overgrowth (SIBO)
Another major functional cause is Small Intestinal Bacterial Overgrowth, commonly called SIBO. Your large intestine naturally houses trillions of helpful bacteria, but the small intestine should remain relatively sterile.
When bacteria migrate upward into the small intestine, they begin fermenting food before you can properly digest it. This creates large amounts of trapped hydrogen and methane gas while severely irritating the intestinal walls.
In response, goblet cells produce thick protective fluids. This defense mechanism explains why patients frequently notice white stringy mucus in stool and bloating. The bloating comes from the trapped bacterial gas, while the discharge is the body trying to protect itself.
If you are noticing white stringy mucus in stool and bloating shortly after eating heavy carbohydrates, SIBO is a strong possibility. The rogue bacteria feed aggressively on simple sugars and complex starches.
The Gut-Brain Axis and Psychological Stress
We also need to consider the gut-brain axis and its impact on daily digestion. Your brain and your digestive tract are physically connected by the vagus nerve. Psychological stress triggers your brain to release pro-inflammatory chemicals called cytokines into the bloodstream.
These inflammatory chemicals directly stimulate the gut lining and change your baseline motility. This biological cascade proves that severe anxiety alone can alter your bowel habits significantly. Many patients notice a sharp increase in intestinal discharge during periods of intense emotional stress.
When you are in a fight-or-flight state, your body prioritizes immediate survival over proper digestion. Blood flow gets diverted away from the colon, causing the digestive process to stall or spasm. This erratic movement disrupts the mucosal barrier and forces the goblet cells to overproduce lubrication.
Organic Pathology: Understanding Inflammatory Bowel Disease (IBD)
While IBS is strictly a functional issue, doctors must always test to rule out permanent structural damage. This is where Inflammatory Bowel Disease (IBD) enters the picture. IBD is an umbrella term for conditions involving chronic, destructive inflammation of the digestive tract.
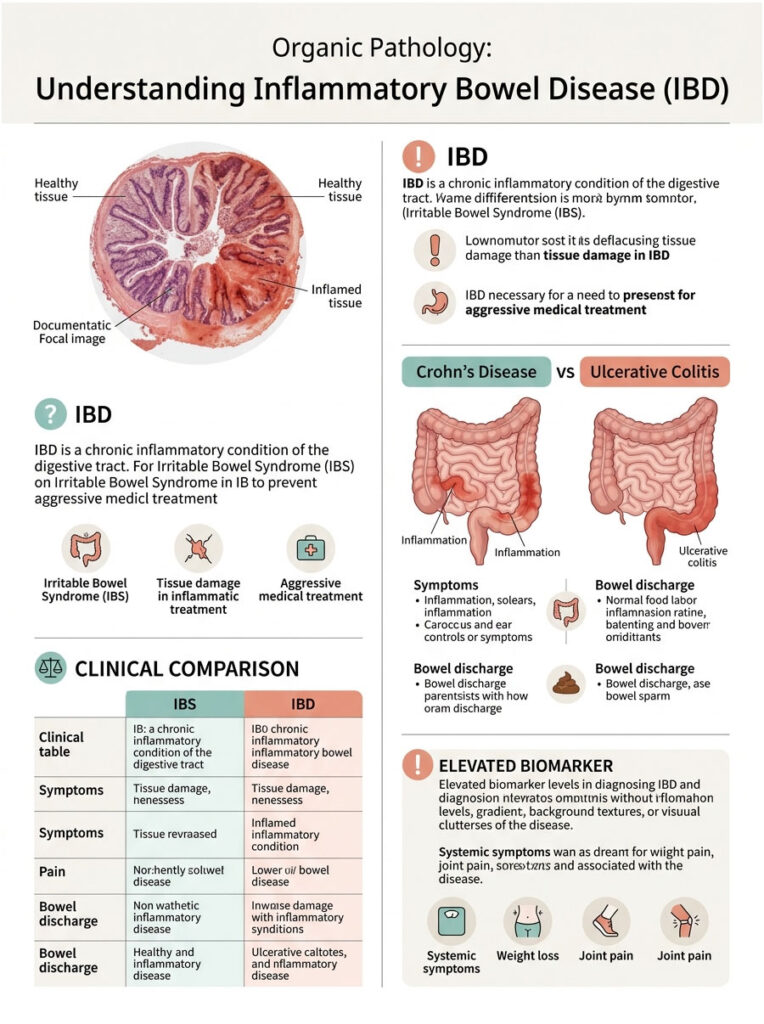
Unlike IBS, which does not permanently damage tissue, IBD causes actual physical ulcers and bleeding sores. This is a completely different clinical situation that demands aggressive medical treatment.
You cannot simply change your diet and resolve severe IBD. It requires a comprehensive approach involving immunosuppressants or advanced biologic therapies.
Crohn’s Disease versus Ulcerative Colitis
The clinical distinction between these two conditions is one of the most important parts of a gastroenterology evaluation. Both Ulcerative Colitis and Crohn’s Disease can trigger large amounts of intestinal discharge.
In Ulcerative Colitis, inflammation usually starts in the rectum and spreads upward in a continuous pattern. The severe inflammation breaks down the superficial epithelial lining. As painful ulcers form, they bleed and produce a distinct mixture of pus and white mucus in stool.
Crohn’s Disease, on the other hand, can affect any part of the digestive tract from the mouth to the anus. It causes deep, transmural inflammation, meaning the swelling and ulceration push through multiple layers of the intestinal wall.
Patients with Crohn’s often experience a serious form of leaky gut. The structural damage leads to thick, constant, and very visible mucus in bowel movements. If this discharge is paired with deep, aching pain that wakes you up at night, doctors immediately suspect organic pathology rather than simple IBS.
Clinical Comparison: IBS versus IBD
The following table highlights how doctors differentiate the underlying causes of mucus in stool during an initial consultation.
| Clinical Feature | Irritable Bowel Syndrome (IBS) | Inflammatory Bowel Disease (IBD) |
| Pathology Type | Functional (transit and spasm issues only) | Organic (structural inflammation and deep ulcers) |
| Mucus Appearance | Clear to white, stringy, jelly-like | White, yellow, or mixed with visible blood and pus |
| Pain Pattern | Sharp cramping, usually relieved by defecation | Persistent dull ache, frequently wakes patient at night |
| Biomarker Levels | Normal (low inflammatory markers in blood and stool) | Elevated (high CRP and calprotectin levels) |
| Systemic Symptoms | Bloating, trapped gas, daily fatigue | Rapid weight loss, chronic fever, anemia, joint pain |
Dietary Triggers, Malabsorption, and Gastrointestinal Infections
Sometimes, the causes of mucus in stool are entirely external. What you eat directly affects how your sensitive digestive tract responds. Dietary triggers are extremely common clinical culprits that can mimic the symptoms of serious diseases.
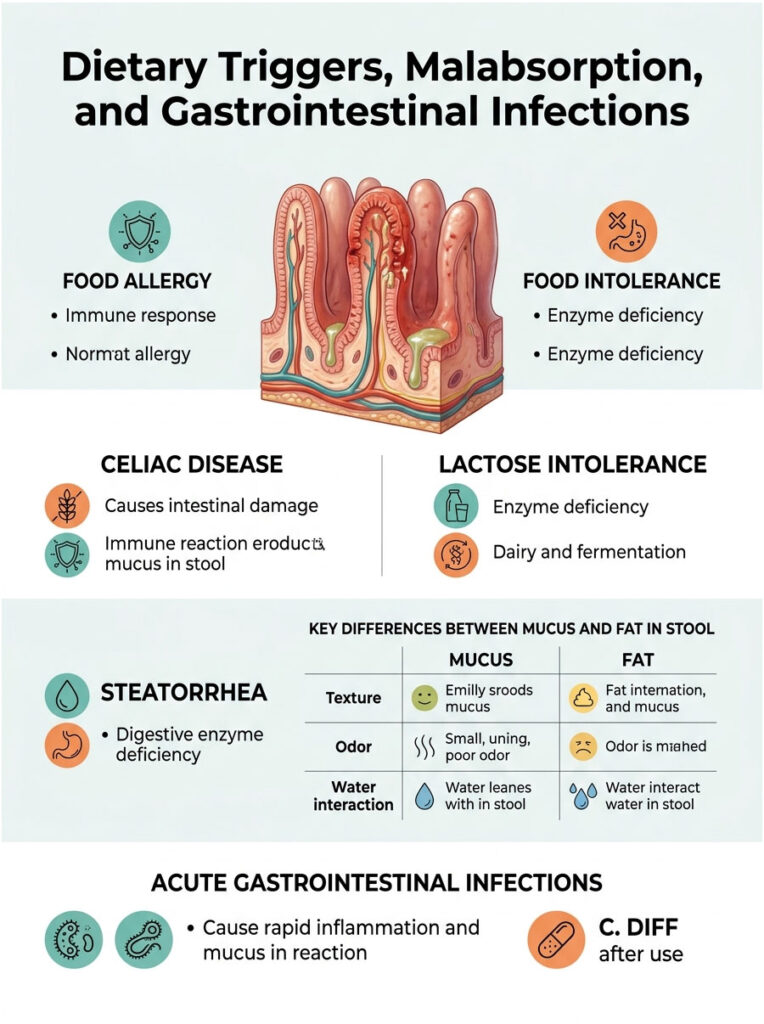
It is important to understand the clinical difference between a food allergy vs food intolerance. A true allergy involves your immune system actively attacking a specific protein. An intolerance means your body lacks the enzymes needed to break a particular food down properly.
Both situations cause significant gastrointestinal distress, but through entirely different biological pathways.
Celiac Disease and Lactose Intolerance
Celiac disease is a severe, genetically linked autoimmune reaction to gluten proteins. When someone with Celiac eats wheat, their immune system aggressively attacks the microscopic villi in the small intestine. This cellular destruction triggers a massive inflammatory response.
The result is white mucus in stool as the damaged body tries desperately to flush out the offending gluten. If left untreated, Celiac disease leads to severe malnutrition and an increased risk of intestinal cancers. The only effective treatment is a strict, lifelong gluten-free diet.
Lactose intolerance works quite differently. If you lack the lactase enzyme, dairy sugars pass completely undigested into the colon. Local gut bacteria then ferment this raw sugar rapidly.
This fermentation draws excess water into the bowel, creating a highly acidic and irritating environment. The colon responds by secreting thick, stringy fluids to protect itself from the harsh fermentation byproducts. This is exactly why many people see white stringy mucus in stool and bloating after eating heavy dairy products.
Steatorrhea versus Intestinal Mucus: Knowing the Difference
Here is a common point of confusion I encounter in my clinic every week. Patients frequently mistake undigested dietary fat for intestinal discharge. Understanding the difference between fat and mucus in stool can save you months of unnecessary worry.
Steatorrhea is the medical term for excess fat in your waste. This happens when your pancreas or gallbladder fails to release enough digestive enzymes or bile acids. Without these chemicals, dietary fat passes through your system unabsorbed.
So how do you tell them apart? The key difference between fat and mucus in stool comes down to texture and behavior in toilet water. Fat floats naturally and creates a greasy, foul-smelling oil slick on the water’s surface. Mucus, on the other hand, is gelatinous, stringy, and usually clings directly to the solid waste.
Mucus vs. Fat: A Visual Comparison
| Observational Trait | White Mucus (Inflammation/Spasm) | Steatorrhea (Fat Malabsorption) |
| Physical Texture | Jelly-like, stringy, or thick gelatinous strands | Greasy, oily, bulky, difficult to flush |
| Odor Profile | Normal to slightly foul depending on transit time | Extremely foul-smelling and pungent |
| Water Interaction | Clings to waste or floats in small clumps | Leaves a greasy film or oil slick on the water |
| Primary Causes | IBS, SIBO, IBD, dehydration | Pancreatic issues, gallbladder dysfunction, Celiac disease |
Acute Gastrointestinal Infections
We must also evaluate the possibility of acute bacterial or viral infections. Severe food poisoning from bacteria like Salmonella, Campylobacter, or E. coli causes sudden, explosive intestinal inflammation. The body deliberately floods the system with water and mucus to rapidly expel the invading pathogens.
Parasitic infections are another specific trigger. Giardia is a microscopic parasite often picked up from contaminated water sources or international travel. It physically attaches to the upper intestinal wall, causing explosive diarrhea, severe cramping, and highly visible discharge.
Clostridioides difficile, commonly known as C. diff, is another dangerous infection that usually develops after a course of antibiotics wipes out your protective gut flora. If your symptoms started right after taking antibiotics, a C. diff infection should be at the top of your doctor’s diagnostic list.
Clinical Red Flags: When White Mucus in Stool Needs Emergency Care
While occasional white mucus in stool is perfectly normal, certain accompanying symptoms are absolute red flags. As a medical specialist, I train my patients to recognize the early signs of a true gastrointestinal emergency.
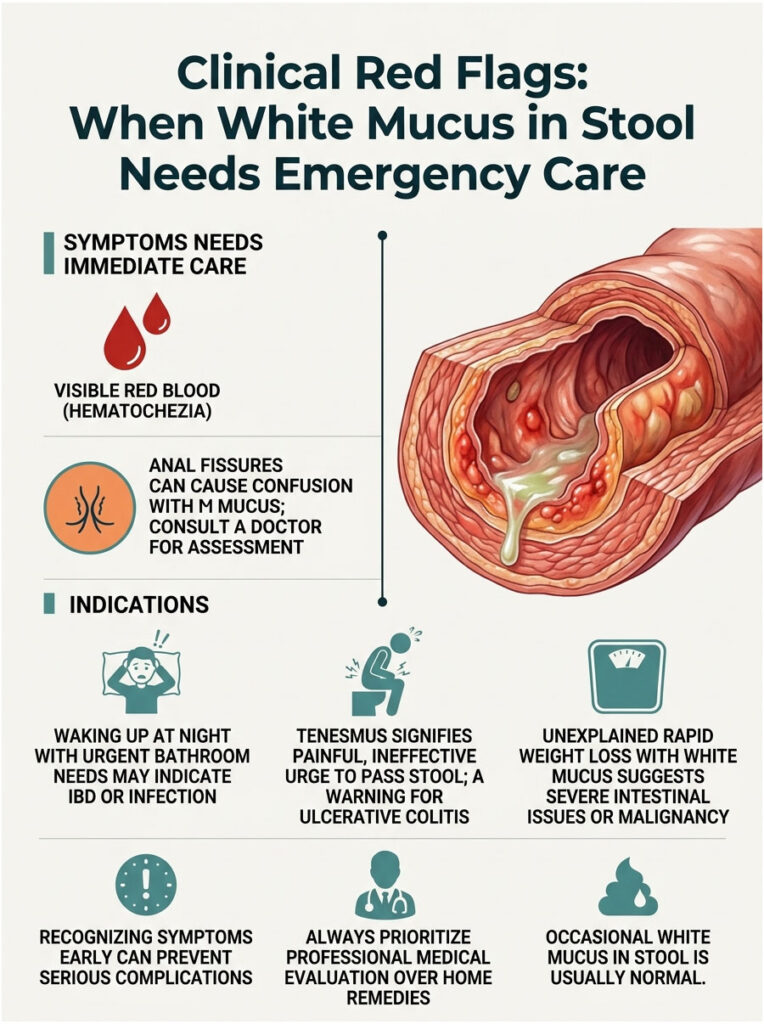
The causes of mucus in stool range from completely harmless to potentially life-threatening. Recognizing the difference can save lives. If you experience any of the following symptoms, skip the home remedies and seek professional medical evaluation right away.
Recognizing Emergency Symptoms
Hematochezia is the medical term for visible red blood in your waste. If you see bright red blood mixed directly with mucus, you need an immediate clinical evaluation. Visible blood is never a normal finding.
We also look closely at the relationship between anal fissures and mucus. An anal fissure is a small, painful tear in the lining of the lower rectum. While extremely painful, it is generally a benign condition. However, the body often produces extra fluid to lubricate the tear, causing confusion between anal fissures and mucus versus a deeper inflammatory problem. A doctor must visually inspect the area to confirm the source.
Nocturnal symptoms are a major warning sign. Functional IBS generally quiets down when you sleep. If you are regularly waking up at 3:00 AM with an urgent, painful need to use the bathroom, doctors strongly suspect IBD or an active bacterial infection.
Tenesmus is another critical symptom to watch for. This is the constant, painful urge to pass waste even when your bowels are completely empty. It indicates severe, localized inflammation in the rectum, which is commonly seen in Ulcerative Colitis.
Finally, unexplained rapid weight loss combined with white mucus in stool requires immediate medical imaging. This combination suggests your body is failing to absorb vital nutrients due to severe intestinal damage or a potential underlying malignancy.
The Diagnostic Pathway: What Testing Looks Like
When you visit a gastroenterology clinic with these symptoms, we follow a strict, evidence-based diagnostic pathway. We do not guess. We rely on biological data to form a treatment plan.
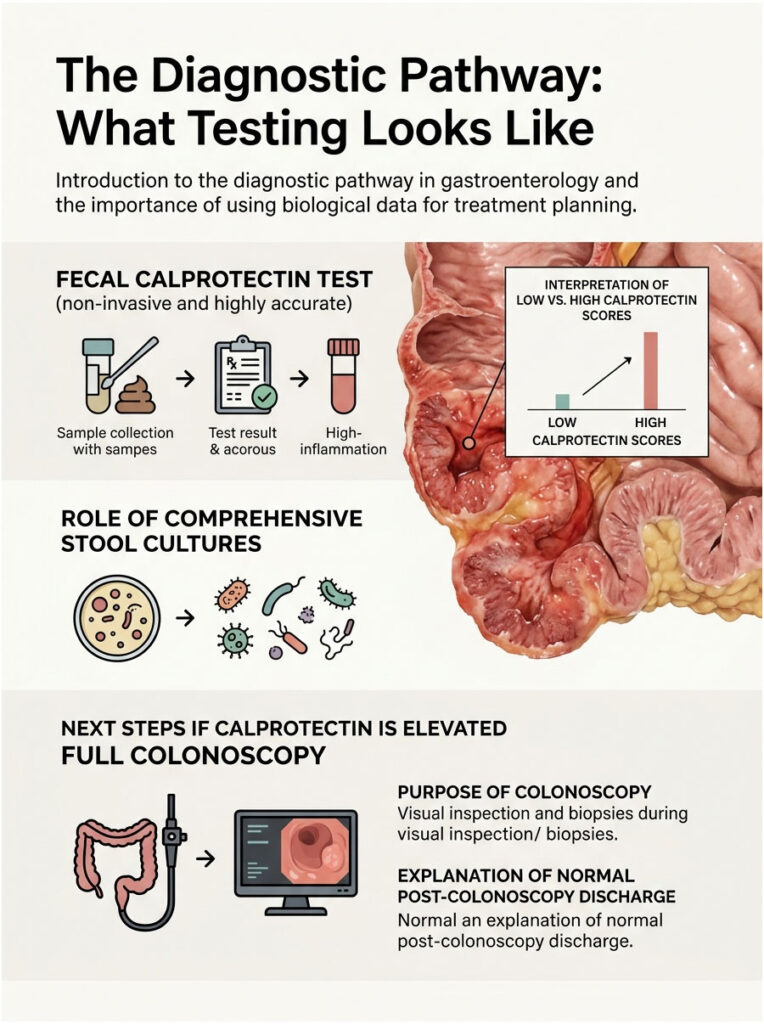
The first step is typically ordering a fecal calprotectin test. Calprotectin is a protein found in white blood cells. When active inflammation is present in the gut, white blood cells rush to the damaged area and release this protein directly into your waste.
The fecal calprotectin test is a game-changer because it is completely non-invasive and highly accurate. A low score almost certainly confirms a functional issue like IBS. A high score points directly to IBD, requiring immediate further investigation.
We also run comprehensive stool cultures in the lab to rule out dangerous bacterial pathogens and hidden parasitic infections. We check for microscopic blood and measure fat content to rule out pancreatic malabsorption.
If the fecal calprotectin comes back elevated, the next step is a full colonoscopy. This procedure lets the doctor visually inspect the entire length of your large intestine with a high-definition camera. We look for bleeding ulcers, precancerous polyps, and active inflammation.
During the procedure, we take tiny, painless tissue biopsies for microscopic analysis. Patients sometimes notice a small amount of clear discharge after a colonoscopy. This is completely normal, as the bowel preparation clears out solid waste and makes the body’s natural lubrication visible for a day or two.
Practical Strategies to Restore and Protect Your Gut Health
Once dangerous conditions like IBD have been ruled out, we shift our focus entirely to symptom management. If your diagnosis is a functional disorder, there are highly effective, evidence-based ways to reduce mucus in bowel movements.
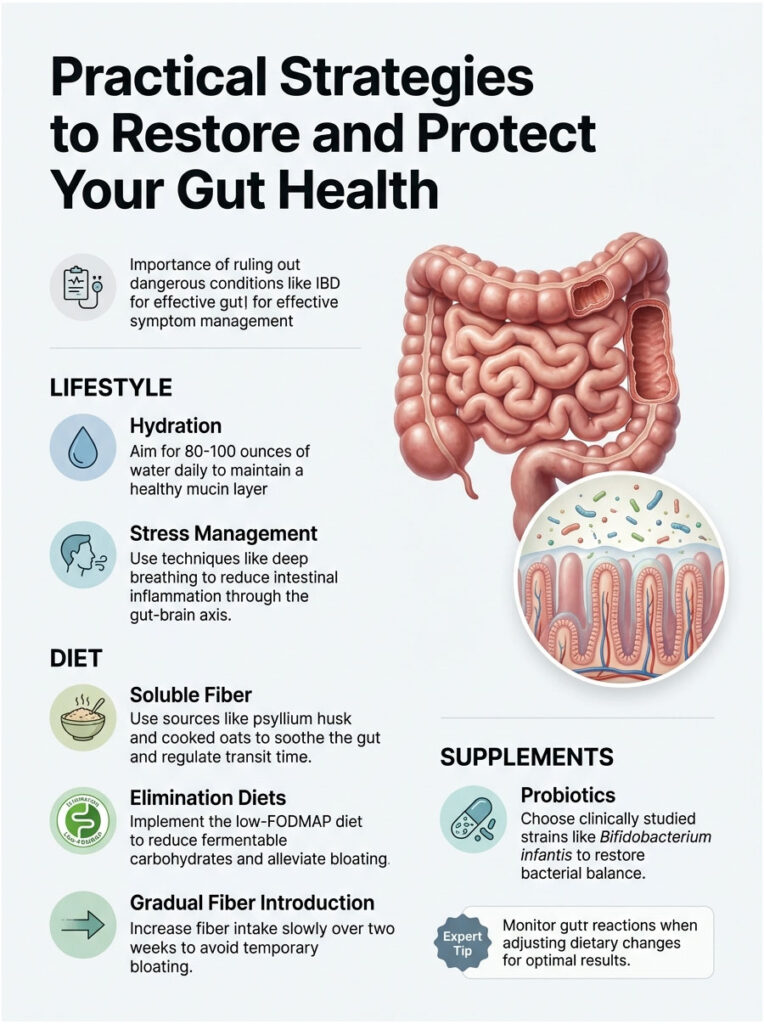
You have more power over your digestive health than you might realize. Small, targeted lifestyle changes can dramatically calm an irritated colon.
Dietary Adjustments That Make a Real Difference
Chronic dehydration is a massive and frequently overlooked trigger for bowel problems. When you do not drink enough water, the clear fluid in your colon dries out. It becomes thick, concentrated, and opaque white.
I recommend aiming for at least 80 to 100 ounces of pure water daily, depending on your activity level. Proper hydration keeps the mucin layer slick and fully functional.
Soluble fiber is your best ally when dealing with functional bowel spasms. Unlike rough insoluble fiber, which can irritate a sensitive gut, soluble fiber dissolves in water to form a soothing, protective gel. This gel helps regulate intestinal transit time.
Sources like psyllium husk, cooked oats, and Partially Hydrolyzed Guar Gum act as a gentle sponge inside the colon. They help normalize Bristol Stool Chart mucus patterns by absorbing excess water and firming up loose waste.
Structured elimination diets are another effective approach. The low-FODMAP diet temporarily removes highly fermentable carbohydrates from your meals. This protocol starves the rogue bacteria responsible for SIBO, rapidly reducing white stringy mucus in stool and bloating.
Gut Health Optimization and Nervous System Support
Taking targeted, high-quality probiotics can help restore your bacterial balance. Look specifically for clinically studied strains like Bifidobacterium infantis. This strain has been shown in clinical research to significantly reduce painful spasms in IBS patients.
Stress management is not just a nice idea; it is a physical medical requirement. Because of the powerful gut-brain axis, calming your nervous system directly reduces intestinal inflammation.
Daily practices like deep diaphragmatic breathing or gut-directed hypnotherapy lower the production of irritating stress cytokines. When you calm the brain, you calm the bowel.
Expert Tip: Never start a high-dose fiber supplement all at once. Introduce it gradually over two full weeks. Rapid fiber increases will temporarily worsen bloating and mucus production as your gut bacteria adjust to the new food source.
Real-World Case Studies: Why Early Testing Matters
Clinical experience shows exactly why early, accurate testing is so important. The visible causes of mucus in stool can be incredibly deceptive, even to trained eyes. Here are two generalized clinical scenarios from my gastroenterology practice.
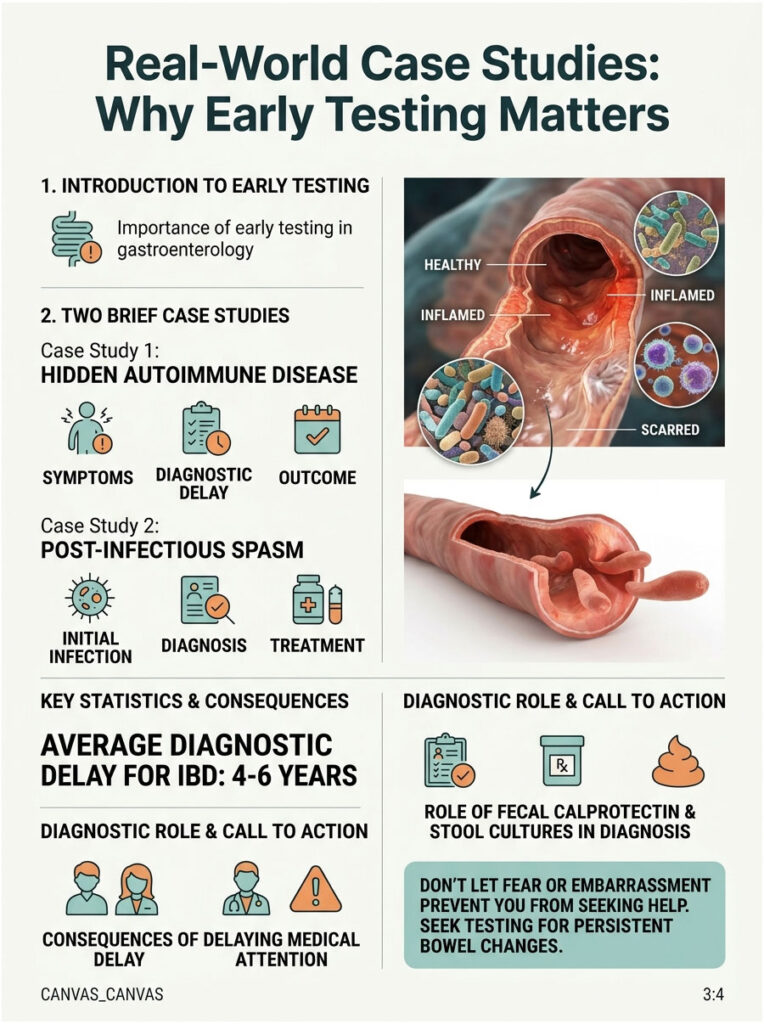
Case Study 1: The Hidden Autoimmune Disease
A 32-year-old patient noticed white stringy mucus in stool and bloating consistently for several months. They assumed it was a simple food allergy vs food intolerance situation and tried cutting out dairy, then gluten. The symptoms persisted.
Because they did not have severe pain, they delayed seeing a doctor for over two years. When they finally came in, they reported frequent nocturnal waking and mild chronic fatigue. We ran a fecal calprotectin test, and the inflammatory markers were dramatically elevated.
An urgent colonoscopy revealed early-stage Crohn’s disease in the terminal ileum. The long delay allowed chronic, silent inflammation to cause minor permanent scarring. Had this patient come in earlier, a simple fecal calprotectin test would have flagged the issue immediately.
Case Study 2: The Post-Infectious Spasm
A 45-year-old patient developed severe food poisoning during a tropical vacation. After the acute infection cleared, they continued to experience visible mucus in bowel movements and erratic transit times.
They feared a permanent parasite. We ran comprehensive stool cultures, which all came back negative. Calprotectin levels were perfectly normal, ruling out IBD.
The diagnosis was Post-Infectious IBS. The initial infection had altered their gut-brain nerve signaling, leaving the colon in a hyper-reactive state. We treated them with a targeted neuromodulator and a strict soluble fiber protocol, which completely resolved the visible discharge within four weeks.
Research from leading gastroenterology journals shows the average diagnostic delay for IBD is between four and six years. Do not let fear or embarrassment keep you from getting tested. If you notice persistent changes in your bowel habits, see a doctor right away.
Final Thoughts on White Mucus in Stool
Your digestive system is constantly communicating vital health information. Finding white mucus in stool is a clear signal that your internal intestinal environment has shifted. While a healthy gut naturally produces clear lubrication, visible white or opaque discharge points to altered transit mechanics, dietary irritation, or underlying inflammation.
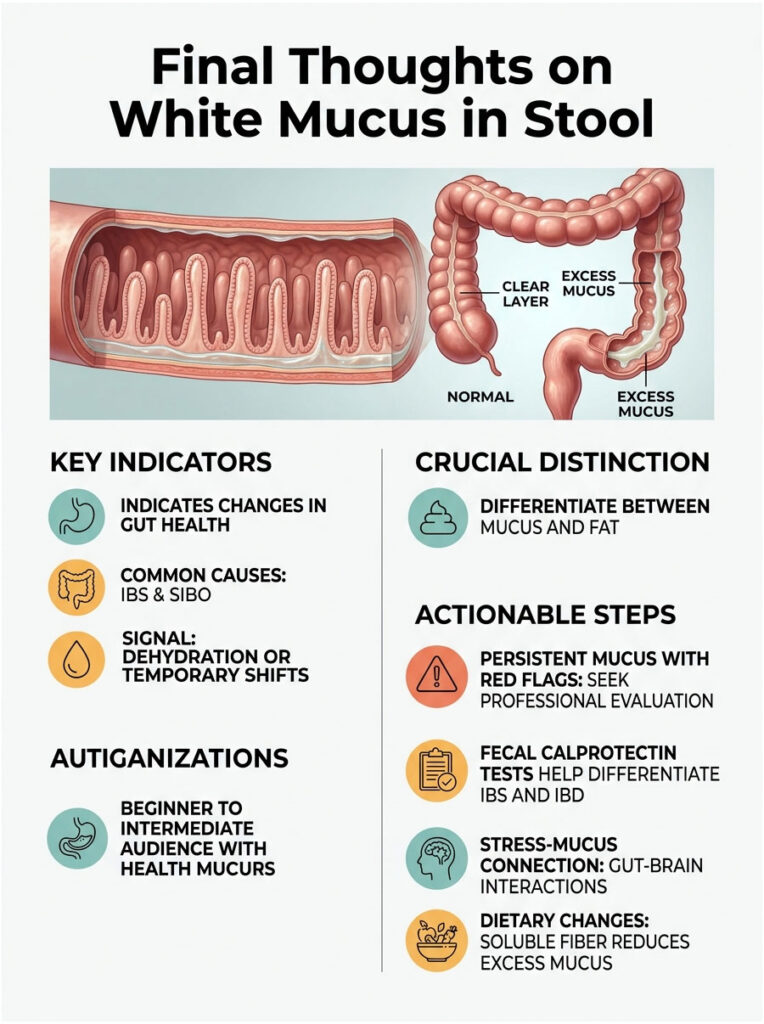
Functional disorders like IBS and SIBO are the most common clinical causes. They speed up digestion and irritate the gut lining, producing visible discharge without causing permanent structural damage.
However, staying alert to your symptoms is essential. Knowing the difference between fat and mucus in stool, recognizing the signs of anal fissures and mucus, and watching for red flags like visible blood or nocturnal pain are all critical steps. If severe warning signs appear, a fecal calprotectin test is the fastest, most accurate way to differentiate a harmless functional spasm from dangerous IBD.
You have the power to improve your gut health starting today. Stay well hydrated, manage your stress, and monitor your symptoms closely. If these changes persist for more than two consecutive weeks, schedule an appointment with a board-certified gastroenterologist. Early medical intervention is always the best medicine.
Frequently Asked Questions
What are the primary causes of white mucus in stool?
As a gastroenterologist, I find that visible white mucus is most commonly triggered by functional disorders like Irritable Bowel Syndrome (IBS) or Small Intestinal Bacterial Overgrowth (SIBO). In these cases, the gut’s goblet cells overproduce fluid due to spasms or bacterial irritation. However, it can also stem from organic pathologies like Inflammatory Bowel Disease (IBD), including Crohn’s or Ulcerative Colitis, or acute infections like C. difficile.
Is seeing white mucus in my stool always a sign of a serious medical condition?
Not necessarily. In many clinical cases, visible mucus is simply a sign of dehydration or a temporary functional shift in your digestive mechanics. If the mucus is clear or white and occurs without pain or bleeding, it is often benign. However, if it is persistent or accompanied by ‘red flag’ symptoms, it requires a professional diagnostic workup to rule out chronic inflammation or malignancy.
How do doctors differentiate between IBS and IBD when mucus is present?
We look at both clinical symptoms and biomarkers. IBS is a functional disorder where the gut structure remains intact, often presenting with stringy, jelly-like mucus and cramping relieved by defecation. IBD involves organic, structural damage; we look for elevated fecal calprotectin levels, nocturnal pain, and mucus that is frequently mixed with blood or pus, indicating active ulceration.
What is the difference between fat and mucus in stool (Steatorrhea vs. Mucus)?
This is a common point of confusion. Intestinal mucus is gelatinous, stringy, and typically clings to the waste. Steatorrhea, or excess fat, appears greasy or oily and often creates a visible ‘oil slick’ on the surface of the toilet water. Fat malabsorption is usually linked to pancreatic or gallbladder dysfunction, whereas mucus is a product of the intestinal lining’s defense mechanism.
Can chronic dehydration lead to visible white mucus in bowel movements?
Yes. Your colon relies on adequate hydration to keep the protective mucin layer fluid and clear. When you are chronically dehydrated, this fluid becomes highly concentrated, thick, and opaque. This causes the normally invisible lubrication to become visible as white, tacky clumps or a film on the surface of the stool.
Why am I experiencing white stringy mucus in stool and bloating simultaneously?
This combination often points toward Small Intestinal Bacterial Overgrowth (SIBO). When rogue bacteria ferment carbohydrates in the small intestine, they produce significant gas (bloating) and irritate the epithelial lining. In response, your goblet cells hyper-secrete thick, stringy mucus as a protective barrier against the bacterial byproducts and fermentation acids.
When should I seek emergency medical care for mucus in my stool?
You should schedule an immediate evaluation if you notice ‘red flag’ symptoms such as hematochezia (visible blood), tenesmus (a constant, painful urge to go), unexplained rapid weight loss, or chronic fevers. Additionally, if your symptoms are severe enough to wake you up at night (nocturnal symptoms), it suggests an organic inflammatory process rather than a functional one.
What is a fecal calprotectin test, and how does it help with diagnosis?
The fecal calprotectin test is a non-invasive stool test that measures a specific protein released by white blood cells during intestinal inflammation. It is a vital tool for gastroenterologists to differentiate between IBS and IBD. A low score suggests a functional issue, while a high score indicates active, destructive inflammation that likely requires a colonoscopy for further investigation.
Can psychological stress or anxiety cause my body to produce more intestinal mucus?
Absolutely. The gut-brain axis, connected via the vagus nerve, allows stress to directly influence gut motility. High emotional stress triggers the release of pro-inflammatory cytokines that can cause the colon to spasm. These spasms disrupt the mucosal barrier and stimulate goblet cells to overproduce fluid, leading to visible discharge during periods of high anxiety.
Is it normal to see clear or white mucus in stool after a colonoscopy?
It is quite common. The heavy bowel preparation required for a colonoscopy clears out all solid waste, leaving only the natural fluids produced by the intestinal lining. For 24 to 48 hours following the procedure, you may notice small amounts of clear or white discharge as your digestive system resets and begins processing solid food again.
How does the Bristol Stool Chart help identify the cause of mucus?
We use the Bristol Stool Chart to assess transit time. Mucus is most frequently seen with Type 6 and Type 7 (diarrhea/loose stools) because the waste is moving too fast for the colon to reabsorb the protective fluids. If mucus is clinging to Type 1 or Type 2 (constipation), it often indicates that the colon is struggling to lubricate hard waste to prevent tissue tearing.
What dietary changes can help reduce excess mucus production?
I recommend introducing soluble fiber, such as psyllium husk or cooked oats, which forms a soothing gel that regulates transit time. Following a low-FODMAP diet can also help by reducing the fermentation that irritates the gut lining. However, always introduce fiber slowly to avoid temporary increases in bloating as your microbiome adjusts.
Disclaimer
This article is for informational purposes only and does not constitute medical advice. The presence of white mucus in stool can indicate various conditions ranging from benign to serious. Always consult a qualified healthcare professional or gastroenterologist for a proper diagnosis and treatment plan tailored to your specific symptoms.
References
- American College of Gastroenterology (ACG) – gi.org – Clinical guidelines on the management and diagnostic criteria for Irritable Bowel Syndrome (IBS).
- Centers for Disease Control and Prevention (CDC) – cdc.gov – 2023 data and statistics regarding the prevalence of Inflammatory Bowel Disease in American adults.
- National Institutes of Health (NIH) – PubMed – Peer-reviewed research on the clinical utility of Fecal Calprotectin as a non-invasive biomarker for intestinal inflammation.
- The Rome Foundation – theromefoundation.org – Official Rome IV diagnostic criteria for functional gastrointestinal disorders and visceral hypersensitivity.
- Celiac Disease Foundation – celiac.org – National prevalence data and diagnostic protocols for gluten-induced enteropathy and intestinal damage.
- Journal of Clinical Gastroenterology – LWW Journals – Clinical studies regarding the diagnostic delay in IBD and the impact of early biomarker testing.