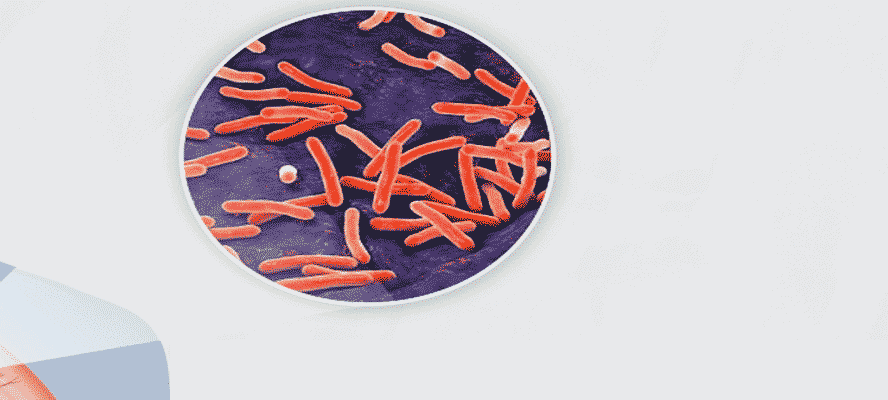
Why having Tuberculosis with Sugar is dangerous?
TB with Diabetes is an Unhealthy Partnership.
Tuberculosis and diabetes, one an age-old disease and the other steadily
gaining prominence. One caused by a bacteria, the other by poor lifestyle
habits and deviant immune activity. Where one is contagious, the other is
chronic. Two diseases that may appear to have no apparent similarities except
for their rise as worldwide epidemics. Yet, TB and diabetes have become unlikely
partners, one promoting the development of the other, or both even joining up
together to complicate situations that are already very serious.