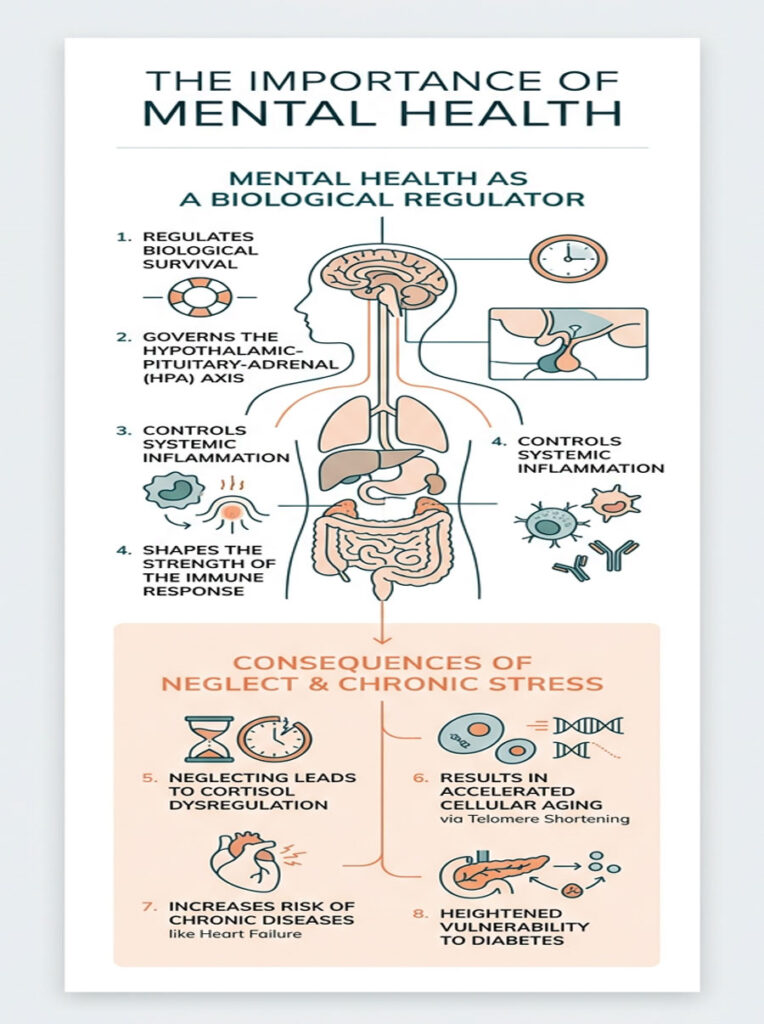
The importance of mental health goes far beyond how you feel on any given day. It is the primary regulator of your biological survival. Your mental state governs the Hypothalamic-Pituitary-Adrenal (HPA) axis, controls systemic inflammation, and directly shapes the strength of your immune response.
Table of Contents
When you neglect it, the consequences are measurable: cortisol dysregulation, accelerated cellular aging through telomere shortening, and a sharply higher risk of chronic diseases like heart failure and diabetes.
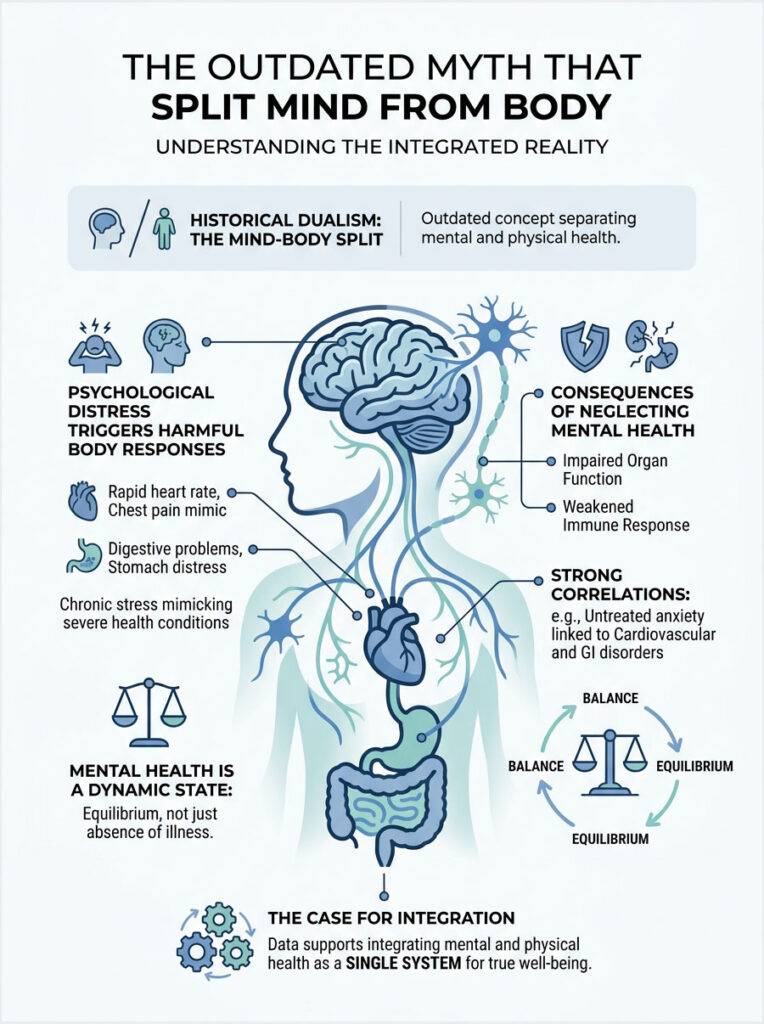
The Outdated Myth That Split Mind From Body
For decades, Western medicine operated under a flawed assumption. Doctors treated the head and the body as separate systems. That dualism is now medically obsolete. We understand today that the importance of mental health is not a slogan. It is a biological reality backed by hard science.
Understanding why your mental health matters more than you think has nothing to do with chasing happiness. It is about maintaining the biological machinery your body needs to survive. When we ignore psychological distress, we are not simply “feeling bad.” We are triggering a physiological cascade that degrades organ function, suppresses immune response, and physically rewires the brain.
As a clinical psychologist with nearly two decades of experience, I have seen the physical toll of psychological neglect firsthand. I have watched untreated anxiety transform into autoimmune disorders. I have seen chronic stress mimic the symptoms of cardiac arrest. Mental health is not the absence of illness. It is a dynamic state of internal equilibrium, the ability of your nervous system to regulate itself after a challenge.
This article breaks down the neuroscience of mental health, the mortality risks tied to psychological neglect, and the economic reality of burnout. We will look at data proving that the mind and body are not just connected. They are the same system.
Key Statistics You Should Know
- 32% Higher Mortality: High psychological distress is linked to a 32% increased risk of cancer mortality, according to the American Psychological Association.
- $1 Trillion Loss: Depression and anxiety cost the global economy $1 trillion annually in lost productivity (WHO).
- 60% Untreated: Nearly 60% of adults with a mental illness do not receive mental health services (NIMH).
- 95% Serotonin: About 95% of the body’s serotonin is produced in the gut, confirming the link between digestion and mood.
- 50% Chronic Disease: People with severe mental health conditions are 50% more likely to develop chronic physical conditions.
The Neurobiology of Wellness: It Is Not Just “In Your Head”
A common dismissal patients hear is that their symptoms are “all in their head.” That phrase betrays a fundamental misunderstanding of biology. Thoughts do originate in the brain, but the chemical messengers they trigger travel to every organ in your body. The neuroscience of mental health shows that every thought releases neurochemicals. These are either healing hormones like oxytocin or stress hormones like cortisol. The process is immediate and physical.

Your brain does not distinguish between a physical threat and an emotional one. If a lion is chasing you, your body prepares to run. If you are lying awake worrying about a mortgage payment, your body also prepares to run. The physiological cost is identical. The difference is that the lion eventually leaves. The mortgage worry stays. And that persistence is where the real damage begins.
The HPA Axis and the Cortisol Cascade
To truly grasp the importance of mental health, you need to understand the HPA (Hypothalamic-Pituitary-Adrenal) axis. This is your body’s central command system for stress response. When you perceive a threat, whether it is a tiger or an angry email, the hypothalamus signals the pituitary gland. The pituitary then tells the adrenal glands to flood your bloodstream with cortisol and adrenaline.
In a healthy system, this switch flips off once the threat passes. But in modern life, the “threat” rarely passes. We live in a state of chronic, low-grade stress, and this leads to HPA axis dysfunction. The switch gets stuck in the “on” position.
The result is cortisol dysregulation. Excess cortisol is catabolic. It breaks down muscle tissue, increases visceral fat storage around the organs, and suppresses the immune system. Data from the National Institute of Mental Health (NIMH) shows that chronic activation of this system is a primary driver of hypertension and type 2 diabetes.
Neuroplasticity: How Your Thoughts Physically Wire Your Brain
The brain is not static. It is plastic. Neuroplasticity is the brain’s ability to reorganize itself by forming new neural connections throughout life. The fundamental rule of neuroscience is straightforward: neurons that fire together, wire together. Your mental habits are physically sculpting your brain structure every single day.
When you engage in repetitive negative rumination, you physically thicken the neural pathways associated with anxiety. You are literally training your brain to be anxious. On the other hand, practices like Cognitive Behavioral Therapy (CBT) or gratitude exercises reinforce pathways tied to resilience.
This is why mental health practices matter so much. You are building the infrastructure of your mind. In my practice, I often explain the tug-of-war between the Prefrontal Cortex (logic and regulation) and the Amygdala (fear and emotion). Chronic stress causes the Amygdala to enlarge and the Prefrontal Cortex to shrink. Over time, emotional regulation becomes increasingly difficult.
The Hippocampus Under Siege
The hippocampus is the brain region responsible for memory and learning. It is also highly sensitive to cortisol. When stress levels stay elevated for extended periods, cortisol becomes toxic to hippocampal neurons. It literally destroys brain cells.
This explains why people suffering from depression often report memory loss and brain fog. We used to believe this damage was permanent. Newer research, however, shows that treating the underlying mental health condition can reverse this shrinkage. That highlights the regenerative power of proper mental healthcare.
The 32% Factor: How Mental Health Affects Physical Health
The line between mental and physical health is an artificial one. The mental health and physical health connection is absolute. Data from oncology studies referenced by the American Psychological Association (APA) shows that high psychological distress can increase cancer mortality risk by up to 32%.

This is not because stress directly causes cancer. It is because stress degrades the body’s ability to fight it. When your body is stuck in fight-or-flight mode, it prioritizes immediate survival over long-term maintenance. It stops repairing DNA. It stops hunting for mutant cells. It directs all energy toward the muscles and heart. Over years, this lack of internal maintenance creates the perfect environment for disease to take hold.
Telomeres and the Science of Cellular Aging
One of the most compelling arguments for the importance of mental health comes from telomere research. Telomeres are protective caps on the ends of chromosomes. Think of them like the plastic tips on shoelaces. They prevent DNA from unraveling. As we age, telomeres naturally shorten.
Nobel Prize-winning research by Elizabeth Blackburn and colleagues demonstrated that chronic stress and untreated depression accelerate this shortening. In practical terms, poor mental health makes you age faster at a cellular level. A 40-year-old with chronic, untreated anxiety may have the cellular age of a 50-year-old. This biological aging sets the stage for early-onset cardiovascular disease and cognitive decline.
The encouraging finding? Stress reduction techniques have been shown to stabilize telomere length. Your mind genuinely has the power to slow your biological clock.
Psychoneuroimmunology: Your Immune System Is Listening
Psychoneuroimmunology studies the interaction between psychological processes and the nervous and immune systems. Your nervous system communicates with your immune system constantly. When the brain interprets the environment as unsafe (through anxiety or depression), it signals the immune system to prepare for injury. This increases systemic inflammation.
At the same time, it suppresses specific immune functions. It reduces production of T-cells and Natural Killer (NK) cells, the ones responsible for hunting down viruses and mutant cells. Studies show that people with high stress levels have weaker antibody responses to vaccines and slower wound healing.
If you find yourself getting sick frequently, it is often a sign that your mental health and physical health connection is out of balance. Your immune system is too exhausted from fighting your stress to fight the actual virus.
Acute Stress vs. Chronic Toxic Stress
It is important to distinguish between adaptive stress, which helps us grow, and toxic stress, which breaks us down. The effects of stress on the body vary significantly based on duration.
| Feature | Acute Stress (Adaptive) | Chronic Toxic Stress |
| Duration | Short-term (minutes to hours) | Long-term (weeks, months, years) |
| Hormones | Temporary spike in adrenaline/cortisol | Sustained cortisol elevation |
| Physical Effect | Heightened alertness, immune boost | Systemic inflammation, immune suppression |
| Brain Impact | Improved memory formation | Hippocampal shrinkage, memory loss |
| Recovery | Body returns to homeostasis quickly | Body loses ability to self-regulate |
| Long-term Risk | Minimal (builds resilience) | High risk of heart disease, diabetes, stroke |
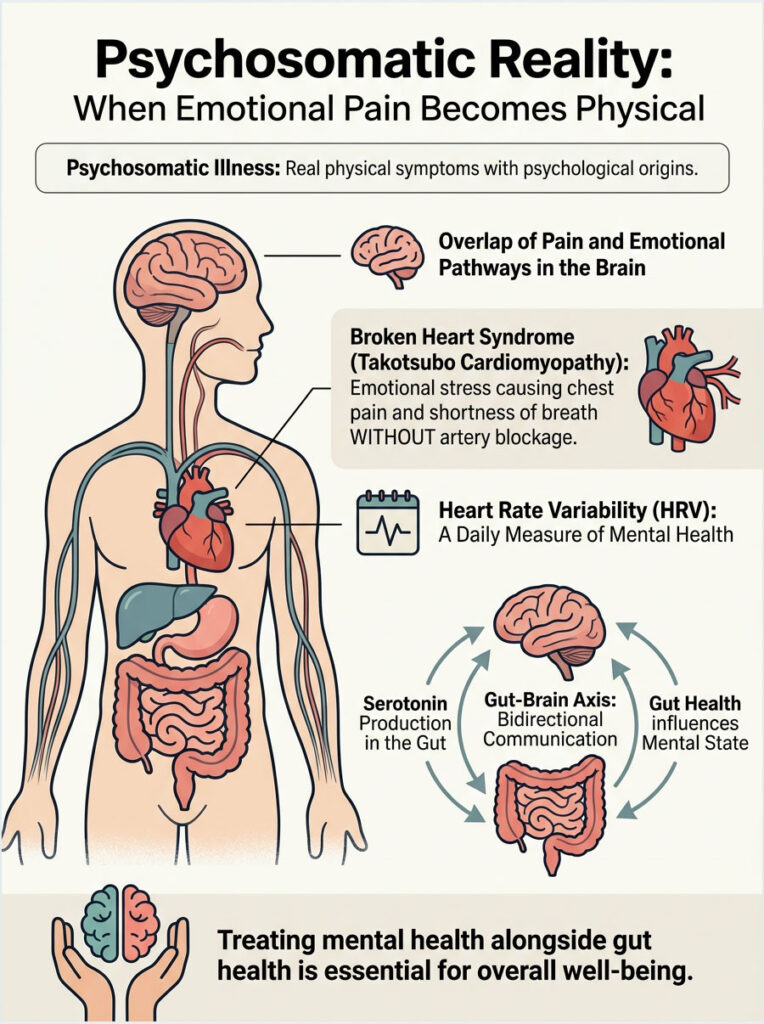
Psychosomatic Reality: When Emotional Pain Becomes Physical
The term “psychosomatic” is often misused to mean “fake.” In clinical reality, psychosomatic illness refers to real physical symptoms with a psychological origin. The effects of stress on the body are tangible and measurable. Pain pathways in the brain frequently overlap with emotional pathways, which is why antidepressants are sometimes prescribed for chronic pain conditions.
Broken Heart Syndrome (Takotsubo Cardiomyopathy)
Perhaps the most dramatic example of the importance of mental health is Takotsubo Cardiomyopathy, commonly known as Broken Heart Syndrome. Extreme emotional stress causes the heart’s left ventricle to balloon and malfunction. Common triggers include the death of a loved one or a catastrophic financial loss.
The symptoms mimic a massive heart attack. Patients experience chest pain and shortness of breath. Yet there is no blockage in the arteries. The damage comes from a sudden surge of stress hormones that stun the heart muscle. This condition, recognized by the American Heart Association, proves that an emotional event can cause organ failure. It is a stark reminder that emotional health is cardiovascular health.
Heart Rate Variability: A Daily Metric of Mental Health
While Takotsubo is extreme, Heart Rate Variability (HRV) offers a daily window into mental health. HRV measures the variation in time between heartbeats. A high HRV indicates a flexible, resilient nervous system. A low HRV suggests a system stuck in fight-or-flight mode.
Chronic anxiety and depression consistently lower HRV. This reduced variability is a strong predictor of future cardiac events. By improving mental health, you can improve HRV, literally strengthening your heart’s ability to adapt to stress.
The Gut-Brain Axis and Serotonin
The gut is often called the “second brain,” and this is not a metaphor. The enteric nervous system in your gut contains millions of neurons. More importantly, roughly 95% of the body’s serotonin, the key neurotransmitter for mood regulation, is produced in the gut. The bacteria in your digestive tract play a crucial role in manufacturing this chemical.
Communication between the gut and brain is bidirectional, running through the Vagus Nerve. Anxiety causes gastrointestinal distress (IBS, ulcers, nausea) because the brain signals the gut to slow digestion and divert energy to survival. Conversely, poor gut health caused by inflammation or a bad diet sends distress signals back to the brain, manifesting as anxiety or depression.
This mental health and physical health connection means you cannot treat the mind without considering the body’s microbiome. Probiotics and a healthy diet are, in a real sense, psychiatric interventions.
The Economic and Professional Cost of Neglecting Mental Health
Beyond biology, the importance of mental health carries massive economic weight. The World Health Organization estimates that depression and anxiety cost the global economy $1 trillion per year in lost productivity. For the individual professional, neglecting mental health is a career-limiting move and an expensive oversight.

We often wear stress as a badge of honor in corporate culture. We believe sacrificing sleep and sanity demonstrates commitment. The data says otherwise. The brain requires downtime to perform at a high level. Without it, the quality of work suffers, leading to errors that cost companies millions.
Burnout as an Occupational Phenomenon
Burnout is not just a buzzword. The WHO now classifies it as an occupational phenomenon. It is characterized by three dimensions: feelings of energy depletion or exhaustion, increased mental distance from your job (cynicism), and reduced professional efficacy. It is a state of vital exhaustion.
Burnout destroys executive function by impairing the prefrontal cortex, the area responsible for decision-making, planning, and emotional control. When a professional is burnt out, they are not just “tired.” Their cognitive capacity is biologically diminished. They make poorer decisions, struggle with impulse control, and lose their creative edge. Treating burnout takes more than a vacation. It requires a systemic restructuring of how you approach work and rest.
Presenteeism: The Hidden Cost Employers Miss
Absenteeism is when employees miss work. Presenteeism is when employees show up but are too mentally unwell to function effectively. Research suggests presenteeism costs employers up to ten times more than absenteeism.
An employee struggling with untreated depression may stare at a screen for eight hours but accomplish only two hours of actual work. This efficiency gap is a direct result of the cognitive slowing that comes with mental health disorders. Prioritizing mental wellness is not just a health initiative. It is a profitability strategy.
Emotional Intelligence (EQ) as a Performance Metric
In high-stakes professional environments, Emotional Intelligence (EQ) is often a better predictor of success than IQ. EQ requires a high degree of mental clarity and self-regulation. Leaders who prioritize the importance of mental health manage conflict better, empathize with their teams, and stay calm under pressure.
Conversely, untreated stress leads to reactive, toxic leadership styles. A leader who cannot regulate their own nervous system cannot effectively lead a team.
The Social Brain: Why Loneliness Is a Health Crisis
Humans are an obligate social species. We are not designed to survive in isolation. Our nervous systems are wired to co-regulate with others, meaning our biology stabilizes when we feel safe and connected. The absence of that connection, loneliness, is physically devastating.

The U.S. Surgeon General has equated the mortality risk of loneliness to smoking 15 cigarettes a day. Loneliness increases vascular resistance (raising blood pressure) and elevates cortisol. It puts the brain in a hyper-vigilant state, constantly scanning for threats because there is no “tribe” to provide safety.
Maintaining strong social connections is a pillar of mental health. It triggers oxytocin release, which counteracts cortisol. Investing in relationships is, therefore, an investment in physical longevity.
Preventative Mental Healthcare: Actionable Strategies
We need to shift from “treating illness” to “building resilience.” Preventative mental healthcare is about strengthening the mind before a crisis hits. Think of it in terms of managing Allostatic Load, the cumulative wear and tear on your body from chronic stress. You would not drive a car 100,000 miles without an oil change. You should not run your brain without maintenance either.

The 5-Minute Micro-Habit That Changes Everything
You do not need an hour of meditation to see real results. Start with 5 minutes of box breathing: inhale for 4 seconds, hold for 4 seconds, exhale for 4 seconds, hold for 4 seconds. This simple act stimulates the Vagus Nerve. It forces the body out of fight-or-flight and into rest-and-digest mode. It is one of the fastest ways to reset your nervous system.
Cognitive Behavioral Therapy (CBT) Techniques for Daily Life
CBT is the gold standard in psychotherapy, but its principles are practical enough for everyday use. I teach my clients the “Catch, Check, Change” method.
- Catch the negative thought (“I am going to fail this presentation”).
- Check the evidence. Is this fact or fear? Have you actually failed before?
- Change the narrative (“I am prepared, and I can handle challenges”).
This interrupts the neural firing that leads to a cortisol spike. By stopping the thought, you stop the chemical reaction in your body.
Mindfulness-Based Stress Reduction (MBSR)
Meditation is often misunderstood as purely spiritual. In reality, it is mental weightlifting. Mindfulness-Based Stress Reduction (MBSR) has been shown in clinical imaging to increase gray matter density in the prefrontal cortex and hippocampus. By practicing mindfulness, you are physically upgrading your brain’s hardware so it can better handle the software of everyday life. This is a cornerstone of preventative mental healthcare.
Sleep Hygiene and the Glymphatic System
Sleep is non-negotiable. It is the foundation of mental stability. During deep sleep, the brain’s Glymphatic System activates. It works like a waste clearance crew, flushing out neurotoxins including beta-amyloid plaques associated with Alzheimer’s disease.
If you do not sleep, you do not clean your brain. The result is brain fog, irritability, and heightened emotional reactivity. Strict sleep hygiene, a cool room, no blue light before bed, and a consistent schedule, is the most effective preventative mental healthcare strategy available. It is when your brain repairs the damage of the day.
Exercise as a Neural Fertilizer
Physical exercise is one of the most potent antidepressants available. When you exercise, your body releases Brain-Derived Neurotrophic Factor (BDNF). Scientists often call BDNF “Miracle-Gro for the brain.” It encourages the growth of new neurons and shields existing ones from stress damage.
Regular aerobic exercise increases the size of the hippocampus, directly countering the effects of cortisol. The mental health and physical health connection works both ways. Moving the body heals the mind.
Reactive vs. Proactive Mental Healthcare
| Aspect | Reactive (Standard) | Proactive (Optimized) |
| Trigger | Seeking help only after a crisis | Incorporating daily wellness habits |
| Intervention | Medication or emergency therapy | Meditation, sleep hygiene, routine therapy |
| Mindset | “I just need to fix this symptom” | “I am building cognitive reserve” |
| Cost | High (medical bills, lost work) | Low (time investment, preventative care) |
| Outcome | Symptom management | Enhanced performance and longevity |
Breaking the Stigma and Seeking Professional Help
Despite the data, stigma remains a major barrier. Internalized stigma often stops high-functioning individuals from admitting they are struggling. As noted earlier, nearly 60% of people with a mental illness do not seek treatment.

Recognizing the importance of mental health means accepting that the brain, like the heart or lungs, requires professional care. It is an organ, and it can malfunction. We need to reframe help-seeking behavior. Going to therapy is not a sign of weakness. It is a sign of strategic intelligence, the utilization of resources to optimize performance. Just as an athlete uses a coach to improve physical form, a professional uses a psychologist to improve mental form.
Trauma-Informed Care
Modern psychology is increasingly moving toward trauma-informed care. This approach shifts the question from “What is wrong with you?” to “What happened to you?” The Adverse Childhood Experiences (ACEs) study demonstrated that unresolved childhood trauma correlates strongly with adult chronic illness.
Addressing these root causes is essential for long-term physical health. If trauma remains unprocessed, the body stays in a state of defense, perpetuating the cycle of inflammation and disease.
When to See a Clinical Psychologist
You do not need to be in crisis to see a psychologist. However, there are red flags that indicate professional help is necessary:
- Sleep disruption lasting more than two weeks
- Loss of interest in activities you once enjoyed (anhedonia)
- Significant changes in appetite
- Reliance on substances to cope
Resources like the APA locator or Psychology Today can help you find accredited providers. Early intervention leads to faster recovery and less biological damage.
Summary and Key Takeaways
The importance of mental health is irrefutable. It is the foundation on which physical health, longevity, and professional success are built. We have explored the neuroscience of mental health, confirming that thoughts drive chemistry. We have seen the mental health and physical health connection through the lens of telomeres and the immune system. And we have identified the effects of stress on the body, from the HPA axis to the heart itself.

Neglecting your mind is biologically expensive. It costs you years of life, immune resilience, and cognitive capacity. The most effective strategy is preventative mental healthcare: prioritizing sleep, practicing cognitive reframing, and managing stress before it becomes toxic.
Your mind is the architect of your body. Treat it with the respect it commands. I encourage you to implement one strategy from this article today. Whether it is a five-minute breathing exercise or booking a therapy session, the investment will yield dividends for the rest of your life. Do not wait for the system to break before you decide to maintain it.
Frequently Asked Questions
How does mental health directly influence physical longevity?
Mental health regulates the HPA axis and systemic inflammation, which are key determinants of biological survival. Neglecting psychological well-being can lead to accelerated telomere shortening and a 32% higher risk of cancer mortality, effectively aging your body at a cellular level.
What is the role of the HPA axis in chronic stress management?
The Hypothalamic-Pituitary-Adrenal (HPA) axis is the body’s central command for the stress response, releasing cortisol and adrenaline during perceived threats. In cases of chronic stress, this system becomes dysregulated, leading to sustained cortisol elevation that breaks down muscle tissue and increases visceral fat storage.
Can untreated anxiety cause permanent damage to the brain’s structure?
While chronic stress can cause the amygdala to enlarge and the hippocampus to shrink, the brain’s inherent neuroplasticity allows for significant repair. Utilizing evidence-based interventions like Cognitive Behavioral Therapy (CBT) can help rewire neural pathways and has been shown to reverse hippocampal volume loss over time.
Why is the gut-brain axis significant for mood regulation and serotonin?
Approximately 95% of the body’s serotonin is produced in the gut, making the microbiome a primary driver of emotional stability. The bidirectional communication via the Vagus Nerve means that gastrointestinal inflammation can directly trigger symptoms of anxiety and depression in the brain.
What are the physical symptoms of Broken Heart Syndrome?
Known clinically as Takotsubo Cardiomyopathy, this condition involves a sudden weakening of the left ventricle triggered by severe emotional distress. It mimics a massive heart attack with chest pain and shortness of breath, proving that an acute psychological event can cause immediate organ failure.
How does psychological distress impact the efficacy of the immune system?
Through the field of psychoneuroimmunology, we know that chronic stress suppresses the production of T-cells and Natural Killer cells. This leaves the body vulnerable to viruses and mutant cells while simultaneously increasing harmful systemic inflammation that can lead to autoimmune disorders.
What is the difference between adaptive stress and chronic toxic stress?
Adaptive stress is short-term and helps build resilience, whereas toxic stress is chronic and leads to a high allostatic load. Toxic stress prevents the body from returning to homeostasis, eventually resulting in hypertension, type 2 diabetes, and an increased risk of stroke.
How does presenteeism impact professional productivity and the economy?
Presenteeism occurs when employees are physically at work but cognitively impaired by untreated mental health conditions, costing the global economy $1 trillion annually. It significantly diminishes executive function in the prefrontal cortex, leading to poor decision-making and reduced professional efficacy.
What are the clinical benefits of practicing mindfulness-based stress reduction?
Mindfulness-Based Stress Reduction (MBSR) acts as mental weightlifting by physically increasing gray matter density in the prefrontal cortex and hippocampus. Regular practice strengthens the brain’s ability to regulate the amygdala, fostering long-term emotional resilience and superior cognitive reserve.
Why is sleep hygiene considered a form of preventative mental healthcare?
During deep sleep, the brain’s Glymphatic System activates to flush out neurotoxins like beta-amyloid plaques associated with Alzheimer’s. Neglecting sleep hygiene prevents this essential cleaning process, resulting in chronic brain fog, heightened emotional reactivity, and long-term cognitive decline.
How does physical exercise act as a neural fertilizer for the brain?
Physical activity triggers the release of Brain-Derived Neurotrophic Factor (BDNF), which promotes the growth and protection of neurons. This process directly counters the catabolic effects of cortisol, effectively acting as a natural antidepressant by increasing the size of the hippocampus.
When is it necessary to seek professional help from a clinical psychologist?
You should consult a professional if you experience persistent sleep disruption, anhedonia, or rely on substances to cope for more than two weeks. Early intervention is a strategic intelligence move to prevent biological damage and optimize your nervous system’s ability to self-regulate.
Disclaimer
This article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. The biological and psychological connections discussed are based on current clinical research but individual results may vary. Always consult a qualified healthcare professional or clinical psychologist before making significant changes to your health regimen or if you are experiencing a mental health crisis.
References
- American Psychological Association (APA) – apa.org – Research linking high psychological distress to a 32% increase in cancer mortality risk.
- World Health Organization (WHO) – who.int – Global statistics on the $1 trillion economic impact of depression and anxiety on productivity.
- National Institute of Mental Health (NIMH) – nimh.nih.gov – Data regarding HPA axis activation and its role in hypertension and type 2 diabetes.
- Nobel Prize Outreach – nobelprize.org – Summary of Elizabeth Blackburn’s research on telomeres and the impact of chronic stress on cellular aging.
- American Heart Association (AHA) – heart.org – Clinical overview of Takotsubo Cardiomyopathy (Broken Heart Syndrome) and its emotional triggers.
- Journal of Psychoneuroimmunology – Elsevier Publication – Studies regarding the interaction between the nervous system and immune response under stress.
- Harvard Health Publishing – health.harvard.edu – Insights into the gut-brain axis and the production of serotonin in the enteric nervous system.