About 59.3 million American adults lived with a mental illness in 2022, and roughly half of them never got any treatment, according to the National Institute of Mental Health. In my work covering this space, the block is rarely stigma anymore. It’s confusion about what therapy actually is, what it costs, and where a person is supposed to start.
Table of Contents
Quick Answer: Therapy, also called psychotherapy or talk therapy, is a structured conversation with a licensed mental health professional that helps you understand your thoughts, regulate emotions, and change patterns that aren’t working. In the US, therapy treats conditions like anxiety, depression, and PTSD, typically costs $100 to $250 per session out of pocket, and produces measurable improvement in about 75% of people who stick with it.

At a Glance
- Therapy is delivered by licensed US providers: psychologists, LCSWs, LPCs, LMFTs, and psychiatrists.
- Out-of-pocket cost averages $100 to $250 per session; insurance copays often drop that to $20 to $60.
- CBT is the most studied approach, with 12+ other evidence-backed modalities in regular US practice.
- Online therapy works about as well as in-person care for anxiety, depression, and PTSD.
- You don’t need a diagnosis to start. Stress, grief, burnout, and life transitions all qualify.
- 988 is the US Suicide & Crisis Lifeline (call or text) for immediate 24/7 support.
- Therapist-client fit predicts outcomes more than any specific modality does.
What Is Therapy? A Clear Definition
Therapy is a treatment method where you work with a trained mental health professional to address emotional, behavioral, or psychological challenges through talking, skill-building, and structured exercises. The goal isn’t to fix you. It’s to help you understand your patterns and build better tools.

The word comes from the Greek therapeia, meaning healing. In a clinical US setting today, “therapy” without a modifier almost always means psychotherapy. Physical and occupational therapy treat the body; psychotherapy treats the mind.
According to the CDC’s National Health Interview Survey, 23.9% of US adults received mental health treatment in 2023, up from 19.2% in 2019. I’ve watched that shift play out in real time. Therapy is moving from “last resort” to “basic maintenance” for millions of Americans.
Therapy vs. Psychotherapy vs. Counseling: What’s the Difference?
These terms get used interchangeably, and in casual conversation, that’s fine. But nuances matter when you’re shopping for care.
Psychotherapy is the formal clinical term used by psychologists and psychiatrists. It tends to imply deeper, longer-term work. Counseling often refers to shorter-term, issue-focused work for grief, career, or adjustment problems. Therapy is the umbrella word covering both.
If a provider calls themselves a “counselor” in the US, they’re usually a Licensed Professional Counselor (LPC) or a similar master’s-level clinician. “Therapist” is a broader, less regulated title, so always check their actual license.
Who Provides Therapy in the US?
Five main provider types are licensed to deliver therapy in the United States:
- Psychiatrists (MD or DO): Medical doctors who can prescribe medication. Some provide therapy; many focus on medication management.
- Psychologists (PhD or PsyD): Doctoral-level providers trained in assessment, testing, and therapy. They cannot prescribe in most states.
- Licensed Clinical Social Workers (LCSW): Master’s-level providers who deliver the majority of US therapy, often at lower rates.
- Licensed Professional Counselors (LPC, LMHC, LCPC): Master’s-level counselors trained specifically in psychotherapy.
- Licensed Marriage and Family Therapists (LMFT): Specialists in couples, family, and relationship work.
First-time clients often assume a psychiatrist sits at the top of the food chain. For most common issues (anxiety, depression, relationship stress), a well-matched LCSW or LPC delivers the same quality care at a lower price. I’ve seen this play out hundreds of times in reader interviews.
Common Myths About Therapy, Busted
The couch-and-clipboard stereotype is dead. Modern therapy is collaborative, active, and often homework-driven. You don’t have to talk about your mother. You don’t have to cry. And you don’t need to be in crisis to benefit.
In my reporting, the clients who get the most out of therapy are usually the ones who came in because of a vague sense something was off, not because they hit rock bottom.
How Does Therapy Actually Work? (The Mechanism)
Therapy works through three things happening at once: relationship, insight, and skill-building. Not one of them alone. All three together.

The Therapeutic Alliance (The #1 Predictor of Outcome)
Decades of research confirm the strongest predictor of whether therapy works isn’t the modality. It’s whether you two connect. Clinicians call this the “therapeutic alliance.” It means trust, shared goals, and a sense your therapist gets you.
In practice, clients who dread every session usually aren’t getting better, even with a technically excellent CBT therapist. Clients who feel heard often improve with modalities academics argue over. If your first therapist feels wrong after three or four sessions, that isn’t failure. That’s data. Switch.
What Happens in Your First Session (Step by Step)
The first session is an intake. Expect these five steps:
- Paperwork and informed consent (15 minutes of forms on confidentiality, fees, emergency protocols).
- Your therapist asks why you’re there, in your own words.
- A structured history: symptoms, family, medical, substance use, past treatment.
- Safety screening (questions about suicide, self-harm, abuse; routine, not a trap).
- Initial goals, a rough plan, and scheduling your next session.
Most people walk out feeling lighter after session one. That has less to do with “venting” and more to do with finally being listened to without anyone trying to fix you.
Session Length, Frequency, and Duration
A standard therapy session is 45 to 50 minutes, often called the “therapeutic hour.” Weekly sessions are the default for the first three to six months. Many clients then shift to biweekly.
Short-term work (like Solution-Focused Brief Therapy) can wrap in 6 to 12 sessions. Deeper modalities (like psychodynamic therapy) may run a year or more.
How Therapy Changes the Brain
Brain imaging studies cited by the American Psychiatric Association show psychotherapy produces measurable changes in brain regions linked to mood, fear, and self-regulation. In depression, panic disorder, and PTSD, those changes look similar to what medications produce.
The takeaway: therapy isn’t just talking. It’s a form of targeted neuroplasticity practice.
12 Types of Therapy Explained
There are more than 400 named therapy modalities in the research literature, but most US clinical work uses about a dozen core approaches. Here’s the side-by-side breakdown.

Table 1: The 12 Main Types of Therapy in the US
| Therapy Type | Best For | Evidence | Session Length | Duration | Avg Cost |
| Cognitive Behavioral Therapy (CBT) | Anxiety, depression, OCD, insomnia | Very strong | 45-50 min | 12-20 sessions | $100-$250 |
| Dialectical Behavior Therapy (DBT) | Borderline PD, self-harm, emotion dysregulation | Strong | 60 min + group | 6-12 months | $150-$300 |
| Acceptance and Commitment Therapy (ACT) | Chronic pain, anxiety, values conflicts | Strong | 45-60 min | 8-16 sessions | $120-$250 |
| EMDR | PTSD, trauma, phobias | Strong | 60-90 min | 6-12 sessions | $150-$300 |
| Psychodynamic Therapy | Recurring relationship issues, identity work | Moderate | 45-50 min | 6 months to 2+ years | $150-$300 |
| Humanistic / Person-Centered | Self-esteem, personal growth | Moderate | 50 min | Varies | $100-$225 |
| Solution-Focused Brief Therapy | Specific life goals, mild depression | Moderate | 45 min | 4-8 sessions | $100-$200 |
| Interpersonal Therapy (IPT) | Depression from relationship changes, grief | Strong | 50 min | 12-16 sessions | $120-$250 |
| Internal Family Systems (IFS) | Trauma, self-criticism, internal conflict | Emerging | 50-60 min | 3-12 months | $150-$275 |
| Somatic Experiencing | Trauma stored in the body, chronic stress | Emerging | 60 min | 10-20 sessions | $150-$300 |
| Family / Couples (Systemic) | Relationship, parenting issues | Strong | 60-90 min | 8-20 sessions | $150-$350 |
| Play Therapy | Children 3-13 with anxiety, trauma, ADHD | Strong | 30-50 min | 6-20 sessions | $120-$200 |
CBT: The Gold Standard for Most Issues
CBT is the most researched psychotherapy in history. It works on the principle that thoughts, feelings, and behaviors are linked, and changing one changes the others. For depression, anxiety, PTSD, OCD, and insomnia, CBT is almost always the first-line recommendation.
It’s structured, homework-heavy, and typically wraps in 12 to 20 sessions.
DBT: Built for High-Intensity Emotion
Developed by Marsha Linehan in the 1980s, DBT was originally designed for people with Borderline Personality Disorder who experienced suicidal thinking. Today it’s used for anyone who feels emotions at extreme intensity.
It combines individual therapy, group skills training, and phone coaching. It’s more intensive than CBT, and usually pricier.
EMDR: The Standout for Trauma
Eye Movement Desensitization and Reprocessing sounds strange on paper, but the research backs it up. The US Department of Veterans Affairs lists EMDR alongside CBT as a first-line PTSD treatment.
I’ve interviewed veterans who tried five therapists and made more progress in eight EMDR sessions than in three years of talk therapy.
IFS and Somatic Therapy: The Rising Stars
Internal Family Systems treats the mind as made up of different “parts” (the anxious part, the perfectionist part, the inner child). Somatic Experiencing treats trauma as something stored in the body, not just the mind.
Both are newer, both are gaining strong research support, and both are missing entirely from most older online guides.
Who Actually Benefits from Therapy?
Short answer: almost anyone. Therapy isn’t reserved for people with a DSM diagnosis. It’s also a tool for people in transition, in conflict, or in a fog they can’t quite name.

Mental Health Conditions Treated
The most common clinical reasons people seek therapy in the US include:
- Anxiety disorders (generalized, social, panic)
- Major depressive disorder
- Post-traumatic stress disorder (PTSD)
- Obsessive-compulsive disorder (OCD)
- Bipolar disorder (usually alongside medication)
- ADHD in adults and children
- Eating disorders
- Substance use disorders
- Grief and bereavement
- Personality disorders
- Postpartum depression
Life Situations That Don’t Need a Diagnosis
You don’t need a label. Plenty of people I’ve interviewed started therapy during:
- A divorce or breakup
- A career pivot or job loss
- Becoming a new parent
- A health scare or chronic illness
- Caring for an aging parent
- Immigration or identity transition
- Burnout (chronic work exhaustion rest doesn’t fix)
- Feeling “fine” on paper but empty inside
7 Signs You Should Start Therapy This Month
- You feel sad, anxious, or irritable more days than not for two weeks-plus.
- Sleep or appetite has shifted noticeably.
- You’re using alcohol, food, scrolling, or shopping to numb out.
- People closest to you have mentioned you seem “off.”
- Work performance is slipping despite effort.
- You keep having the same fight or same thought on loop.
- You’ve had any thought of not wanting to be here.
That last one needs immediate action. If you’re in crisis, call or text 988 right now. It’s free and available 24/7 across the US.
How Much Does Therapy Cost in the US?
Cost is the single most commonly cited reason Americans skip mental health care, per the American Psychological Association. The pricing is confusing even to people inside the industry. Here’s what’s real in 2026.

Table 2: 2026 Therapy Cost Breakdown in the US
| Format | Out-of-Pocket Range | Insurance Copay | Monthly Estimate | Source |
| Individual therapy (in-person) | $100-$250 per session | $20-$60 | $400-$1,000 | SimplePractice 2024 |
| Couples / family therapy | $150-$350 per session | $30-$75 | $600-$1,400 | Octave 2025 |
| Online therapy platforms | $60-$90 per week | Varies | $260-$400 | Platform pricing |
| Group therapy | $30-$80 per session | $10-$30 | $120-$320 | TherapyDen 2025 |
| Psychiatrist (med management) | $200-$500 per session | $30-$80 | $200-$500 | Industry data |
| Sliding scale / community clinic | $20-$80 per session | N/A | $80-$320 | Open Path Collective |
SimplePractice analyzed nearly 105 million US therapy sessions from 2023 to 2024 and found rates ranging from $122 per session on the low end to $227 on the high end by state. North and South Dakota topped the list because of provider scarcity, while Oklahoma, Tennessee, and Missouri ranked among the lowest.
Therapy With Insurance
Thanks to the Affordable Care Act, mental health services are an Essential Health Benefit. Most plans cover therapy at parity with physical health. Copays typically run $20 to $60 per in-network session. Deductibles apply first on many plans.
Call the member services line on the back of your insurance card and ask for “outpatient mental health benefits.” Ask specifically about copay, deductible status, and whether out-of-network visits are reimbursed.
Therapy Without Insurance
Out-of-pocket therapy averages $100 to $250 nationwide, per Grow Therapy and Medical News Today. Real paths to pay less include:
- Sliding scale therapists: Many charge based on income. Open Path Collective is a nonprofit directory of therapists charging $30 to $80 per session.
- Community mental health centers: Often charge $10 to $50 per session; use FindTreatment.gov.
- University training clinics: Grad students provide supervised therapy at $30 to $80 per session.
- Employee Assistance Programs (EAP): Many US employers offer 3 to 8 free therapy sessions per year. Ask HR.
- Online platforms: BetterHelp and Talkspace run $260 to $400 per month for weekly sessions, usually cheaper than private practice.
Medicare and Medicaid
Medicare Part B covers outpatient therapy by a psychiatrist, psychologist, LCSW, and (as of 2024) LPC and LMFT. You still owe the 20% coinsurance after the Part B deductible. Medicaid coverage varies by state but generally includes therapy for eligible enrollees.
Online Therapy vs. In-Person: Which Is Right for You?
This was a niche question five years ago. After 2020, it became the default. Evidence from recent studies shows online therapy is about as effective as in-person for anxiety, depression, and PTSD.

When Online Wins
- You live in a rural area with limited providers
- Your schedule is packed or unpredictable
- You want a wider pool of therapist options
- Cost is a major factor (online runs 10 to 30% cheaper)
- You have childcare, mobility, or transportation barriers
- You feel more comfortable opening up from home
When In-Person Wins
- You have severe symptoms or are in crisis
- You’re doing somatic or body-based work
- You’re attending group or couples therapy
- Your home lacks privacy
- You’re easily distracted by devices
- You specifically want the ritual of going somewhere
In my reporting, the clients who’ve done both usually say the connection felt slightly stronger in person, but the convenience of online kept them showing up. Showing up beats perfect connection every time.
How to Choose the Right Therapist
The choice feels overwhelming. The US has over 700,000 licensed mental health professionals and dozens of modalities. Here’s a scenario-based decision matrix I’ve built from interviewing dozens of clinicians.
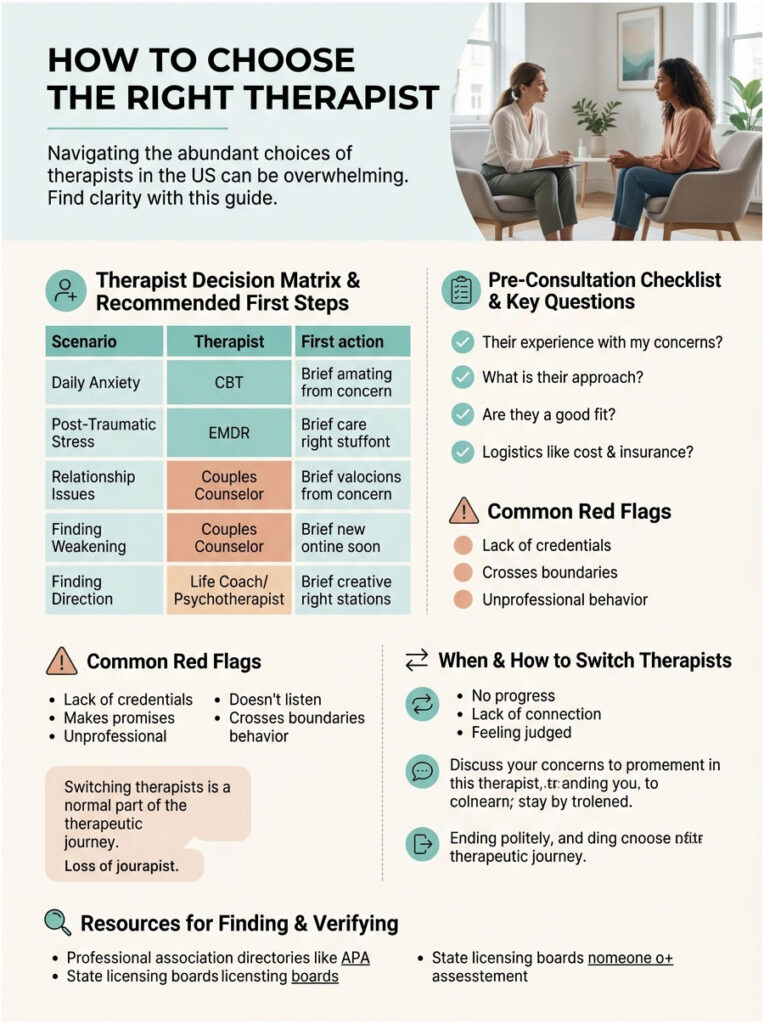
Table 3: Therapist Decision Matrix (Scenario to Action)
| Your Situation | Recommended Therapist Type | First Step |
| Panic attacks, racing thoughts, trouble sleeping | LPC or Psychologist trained in CBT | Search “CBT therapist near me” on Psychology Today |
| Processing childhood trauma or abuse | Trauma specialist trained in EMDR or IFS | Filter by trauma specialty on FindAPsychologist.org |
| Grief after loss of a loved one | LCSW trained in grief counseling or IPT | Ask hospice social worker for referrals |
| Marriage or relationship problems | Licensed Marriage and Family Therapist (LMFT) | Search AAMFT.org TherapistLocator |
| Teen struggling in school or at home | Adolescent therapist using Play Therapy or CBT | Ask pediatrician or school counselor |
| Burnout, career anxiety, chronic stress | LCSW or LPC trained in ACT or Solution-Focused | Check if employer offers EAP sessions |
| Possible ADHD, bipolar, or need for medication | Psychiatrist (MD or DO) | Ask primary care physician for a referral |
The 7-Question Pre-Consultation Checklist
Most therapists offer a free 15-minute phone consultation. Use it. Ask:
- Are you licensed in my state?
- What’s your specialty and primary modality?
- Have you treated my specific issue before?
- Do you take my insurance, or offer sliding scale?
- What’s your cancellation policy?
- How do you measure progress?
- What happens if I’m not feeling better after 8 sessions?
Red Flags of a Bad Therapist
In my work covering this space, I’ve heard the same warning signs from clients over and over:
- Their license can’t be verified on the state board website
- They push a specific modality without explaining why
- They answer every question with “how does that make you feel?”
- They dominate the conversation or give constant advice
- They bring up their own personal life more than yours
- They try to become friends, business partners, or anything outside the therapist role
- They shame, guilt, or argue with you about your feelings
- Sessions feel worse, not just harder, for weeks on end
Every state has a licensing board website where you can verify a therapist’s credentials and disciplinary history. Use it before your first session.
When and How to Switch Therapists
Switching isn’t a failure. It’s often the smart move. A clear sign to switch: you’ve gone 6 to 8 sessions and feel no better, or you dread every appointment.
Tell your current therapist you’d like to end or take a break. A good one will help you transition, maybe even offer referrals.
Does Therapy Actually Work? The Evidence
Yes, but with caveats. About 75% of people who participate in psychotherapy experience measurable symptom relief, per data cited by the American Psychiatric Association. That number holds across depression, anxiety, and PTSD in particular.

What “Progress” Looks Like in Real Life
Progress is rarely linear. A typical trajectory looks like this:
- Weeks 1 to 3: Relief from being heard. Some clients feel worse as old feelings surface.
- Weeks 4 to 8: Insight phase. You start seeing patterns you didn’t see before.
- Weeks 9 to 16: Skill-building. You’re applying tools between sessions and failing sometimes.
- Month 4 and beyond: Real shifts in how you respond to old triggers.
I’ve watched clients who swore therapy wasn’t working at week 6 show up at month 4 and realize their life looked different.
When Therapy Doesn’t Work
Sometimes it doesn’t. Common reasons include:
- Wrong modality for the issue (psychodynamic talk therapy for acute OCD, for example)
- Poor therapist-client match
- Skipping sessions or homework
- Expecting the therapist to fix you without your participation
- An underlying medical or substance issue that’s blocking progress
If you’ve given therapy 12 weeks of honest effort with a well-matched provider and feel nothing has shifted, talk to your therapist about changing approaches, consulting a psychiatrist for medication evaluation, or trying a different therapist altogether.
Common Pitfalls and How to Avoid Them
Expecting Instant Results
Therapy is a slow medicine. One of the most common mistakes I’ve seen is quitting at week 3 because the feelings got harder before they got easier.
Picking the Wrong Modality
CBT isn’t the best answer for every problem, and neither is any single approach. Trauma often needs EMDR or somatic work. Long-standing identity issues may need psychodynamic depth. Ask your therapist why they’re choosing their specific method.
Skipping Sessions or Homework
Showing up once a month doesn’t produce the same outcomes as weekly. The homework (journaling, exposures, behavior logs) is where most real change happens.
Staying Too Long With the Wrong Therapist
Loyalty is nice; growth is better. If you’ve stopped making progress and your gut says it’s a mismatch, that gut is usually right. Switching is normal and healthy.
Your Next Steps: How to Start Therapy This Week

- Call your insurance carrier. Ask for your mental health benefits (copay, deductible, covered providers).
- Write down 3 things you want to work on. One sentence each. This clarifies your intake.
- Search a directory. Psychology Today, Open Path Collective, or FindTreatment.gov if you need sliding scale.
- Book 2 to 3 free consultations. Don’t pick the first person. Compare.
- Block 30 minutes after your first session to reflect on the fit before rebooking.
Frequently Asked Questions
What is the main purpose of therapy?
The main purpose of therapy is to help you understand and change the thoughts, feelings, and behaviors causing distress or keeping you stuck. It’s also used to build emotional skills, process trauma, improve relationships, and treat clinical conditions like depression and anxiety. The specific goal is set collaboratively with your therapist at the start.
Is one therapy session a week enough?
For most clinical issues, yes. Weekly sessions are the clinical default because they give enough time to practice skills between visits while keeping momentum. For acute crises, DBT, or intensive trauma work, twice weekly may be recommended. Once-a-month check-ins are generally only effective for maintenance after active treatment ends.
Can therapy actually fix you?
Therapy doesn’t fix you because you aren’t broken to begin with. What it does, with strong evidence behind it, is reduce symptoms, change unhelpful patterns, and give you better tools for life’s challenges. About 75% of people in therapy show measurable improvement per APA data. The word “fix” sets up the wrong expectation.
How do I know if therapy is working?
You know it’s working when you notice shifts in how you respond to old triggers, when symptoms (sleep, mood, anxiety) measurably improve, when relationships feel easier, and when you’re using your therapist’s tools without thinking. Many therapists use standardized questionnaires (like the PHQ-9 for depression) every few sessions to track objective progress.
What’s the difference between a therapist and a psychiatrist?
A psychiatrist is a medical doctor (MD or DO) who can prescribe medication and diagnose mental illness. A therapist usually refers to a non-medical licensed provider (psychologist, LCSW, LPC, or LMFT) who delivers psychotherapy but can’t prescribe. Many people see both: a psychiatrist for medication and a therapist for weekly sessions.
Can I go to therapy without a mental health diagnosis?
Absolutely. Plenty of people go to therapy for life transitions, relationship questions, grief, stress, or personal growth without meeting criteria for any diagnosis. If you pay out of pocket, no diagnosis is required. If you use insurance, your therapist typically has to assign a billing diagnosis code for coverage, which doesn’t mean you’re “mentally ill.”
Why is therapy so expensive in the US?
Therapy costs reflect the long training required (6+ years of college plus thousands of supervised hours), overhead like office rent and liability insurance, and administrative time spent on notes and billing. For every hour of therapy, therapists typically spend another hour on unpaid prep work. Add limited insurance reimbursement rates, and you get current pricing.
Is online therapy as effective as in-person?
Research from 2020 through 2024 shows online therapy is roughly as effective as in-person for anxiety, depression, and PTSD. It may be less ideal for severe mental illness, couples therapy, group work, or clients who don’t have private space at home. For mild to moderate concerns and most common conditions, online is a legitimate option backed by data.
How long does therapy usually take to work?
Most people notice initial relief within 3 to 6 sessions, though meaningful change typically takes 12 to 20 sessions (roughly 3 to 5 months at a weekly pace). Short-term approaches like Solution-Focused Brief Therapy can wrap in 6 to 8 sessions. Deeper or trauma-focused work may take 6 months to 2 years. Progress isn’t linear; plateaus are normal.
How do I tell my therapist I want to stop?
Be direct. Say something like, “I’ve been thinking I’d like to wrap up our work. Can we talk about next steps?” A good therapist will welcome the conversation, help you plan a termination session to consolidate gains, and offer referrals if you want to switch. Ghosting your therapist is fine too, but a proper ending is usually more healing.
Does insurance cover therapy under the ACA?
Yes. Under the Affordable Care Act, mental health services are an Essential Health Benefit, so most insurance plans (employer-sponsored, marketplace, Medicaid, Medicare) must cover therapy at parity with physical health care. What varies is your copay, deductible, and which therapists are in-network. Call your insurance to confirm specifics before your first appointment.
What should I do in a mental health crisis?
Call or text 988, the US Suicide & Crisis Lifeline, for free 24/7 support anywhere in the country. If you or someone else is in immediate physical danger, call 911 or go to the nearest emergency room. For non-emergency mental health support, the SAMHSA National Helpline (1-800-662-4357) offers free, confidential treatment referrals 24 hours a day.
Disclaimer: This article is for informational purposes and is not medical advice. It is not a substitute for diagnosis or treatment by a licensed mental health professional. If you are experiencing a mental health emergency, call or text 988 in the United States, or call 911. Consult a qualified provider before making decisions about your mental health care.
References
- Centers for Disease Control and Prevention (CDC), NCHS. QuickStats: Mental Health Treatment Trends Among Adults, 2019–2023. cdc.gov/mmwr
- National Institute of Mental Health (NIMH). Mental Illness Statistics. nimh.nih.gov/health/statistics/mental-illness
- American Psychiatric Association. What Is Psychotherapy? psychiatry.org/patients-families/psychotherapy
- Cleveland Clinic. Psychotherapy: What It Is, Why It Is Done & Types. my.clevelandclinic.org
- NIMH. Psychotherapies Overview. nimh.nih.gov/health/topics/psychotherapies
- SimplePractice. Average Therapy Session Rate by State, 2023–2024. simplepractice.com
- Grow Therapy. Paying for Therapy in the US. growtherapy.com
- SAMHSA. National Helpline. samhsa.gov
- 988 Suicide & Crisis Lifeline. 988lifeline.org
- Open Path Collective. Affordable Therapy Directory. openpathcollective.org