After 15 years of treating digestive disorders, I still get this question almost every week: can probiotics cause diarrhea? The short answer is yes, and it happens more often than most people expect.
Table of Contents
When you swallow a capsule packed with billions of live bacteria, you are dropping a small army into a complex ecosystem that was already in balance. Your existing gut bacteria have to make room for the newcomers, and that turf war creates real symptoms. Bloating, gas, and loose stools are all part of the adjustment.
The good news is that for most healthy adults, this phase is temporary and manageable. The key is knowing why it happens, how long it should last, and when symptoms cross the line from normal adjustment to something that needs medical attention. That is exactly what this guide covers.
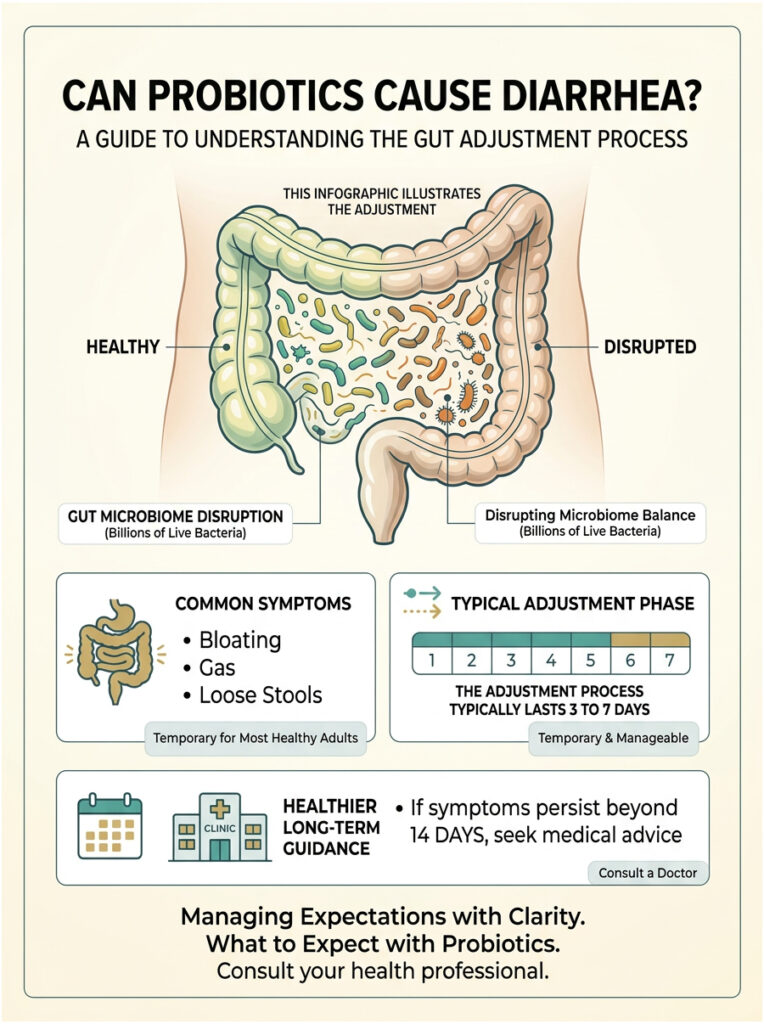
Quick Answer: Yes, probiotics can cause diarrhea. New bacterial strains temporarily disrupt your existing gut microbiome, triggering a recalibration phase. For most people, this resolves within 3 to 7 days. If symptoms persist beyond 14 days or become severe, consult a doctor.
Key Statistics on Gut Health and Probiotics
- Microbial Count: The average human gut contains over 39 trillion active microorganisms.
- Adjustment Window: Over 70% of patients report mild side effects that resolve within the first 7 days.
- Species Diversity: A healthy adult colon houses between 300 and 500 different bacterial species.
- High-Dose Risk: Adverse reactions are 60% more common when daily intake exceeds 50 billion CFUs.
- Water Absorption: The large intestine absorbs up to 1.5 liters of water daily, a process easily disrupted by microbial shifts.
- Resolution Rate: Only about 5% of patients experience digestive distress lasting longer than 14 days.
Why Probiotics Cause Diarrhea in Healthy Adults
Your digestive tract is not an empty tube. It is a dense, highly active ecosystem where trillions of bacteria live in a carefully maintained balance. These resident bacteria help you digest food, produce vitamins, and defend against harmful organisms.
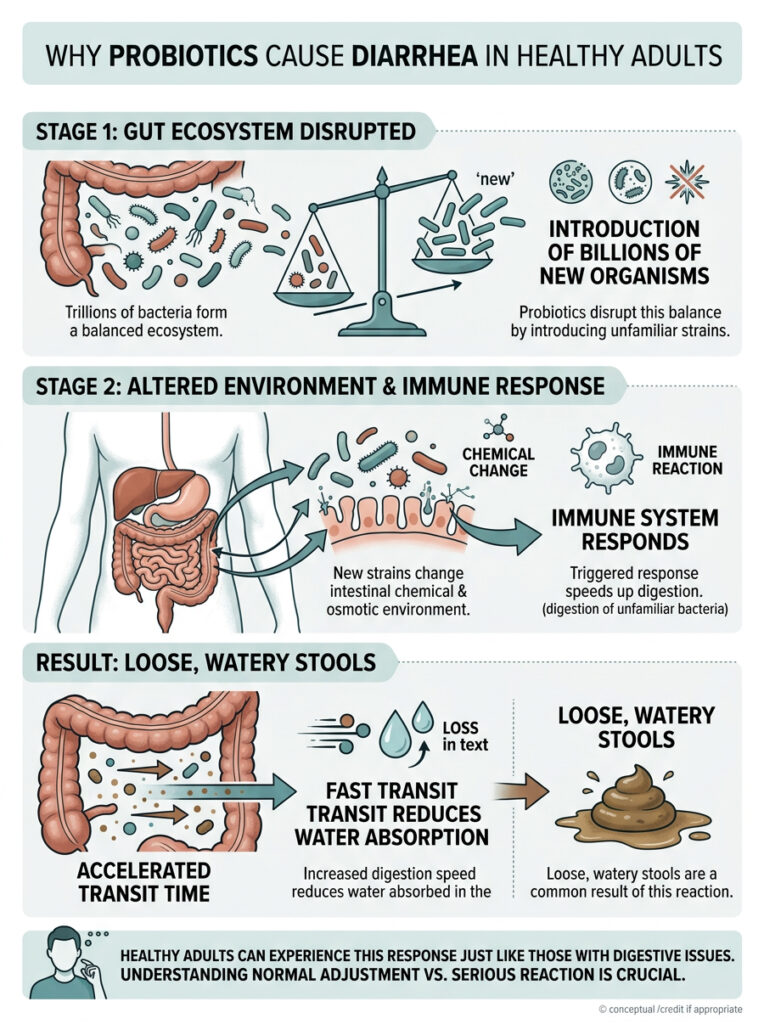
When you swallow a capsule containing 50 billion new organisms, you instantly shake up that balance. The new strains do not simply move in and settle quietly. They actively alter the chemical and osmotic environment of your intestinal tract.
Your immune system monitors the intestinal lining constantly. When billions of unfamiliar bacteria show up at once, the enteric nervous system responds defensively. It speeds up digestion, which reduces the time your colon has to absorb water. The result is loose, watery stools.
Surprisingly, healthy adults experience this reaction just as often as people with chronic digestive issues. A strong reaction can actually indicate a responsive immune system. The important thing is recognizing the difference between a healthy adjustment phase and a reaction that needs medical attention.
Osmotic Diarrhea vs. Secretory Diarrhea: What Is Happening Inside Your Gut
In gastroenterology, we classify diarrhea based on the underlying mechanism. Understanding this distinction matters because it helps determine whether your supplement is safe to continue.
Secretory Diarrhea
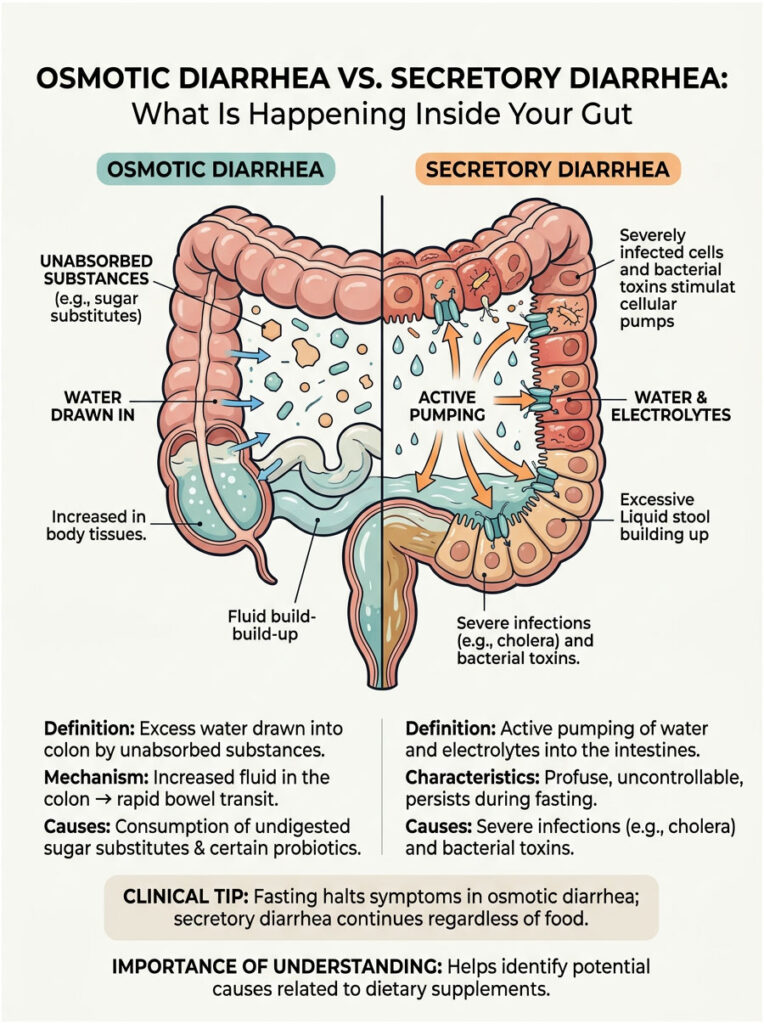
Secretory diarrhea occurs when your body actively pumps water and electrolytes into the intestines. This is typically caused by severe infections like cholera or specific bacterial toxins. It tends to be profuse, uncontrollable, and continues even during fasting. It requires immediate medical attention.
Osmotic Diarrhea
The loose stools caused by probiotics are almost always osmotic. Osmotic diarrhea happens when unabsorbed substances draw excess water from surrounding tissues into the colon. This extra fluid speeds up bowel transit, creating urgency.
Think of it this way. If you eat a large amount of sugar-free candy, the artificial sweeteners pass undigested into your colon. Through osmosis, they pull water from your intestinal walls. The same thing happens with many probiotic supplements. Manufacturers often pack capsules with prebiotic fibers meant to feed the bacteria. If your body cannot break these down quickly enough, they sit in the colon and draw water in.
The excess fluid stretches your intestinal walls, and your nervous system responds with rapid muscle contractions to empty the bowels. The result is a sudden, watery movement.
Clinical Tip: If fasting stops your symptoms entirely, you are likely dealing with osmotic diarrhea. Secretory diarrhea continues regardless of food intake. This simple distinction helps identify whether a specific supplement ingredient is the cause.
The Microscopic Mechanisms Behind Probiotic Side Effects
Your intestinal lining has a limited amount of physical space for bacteria to attach. When new strains like Lactobacillus and Bifidobacterium arrive, they compete aggressively with your existing bacteria for these attachment sites. Gastroenterologists call this process microbial antagonism.
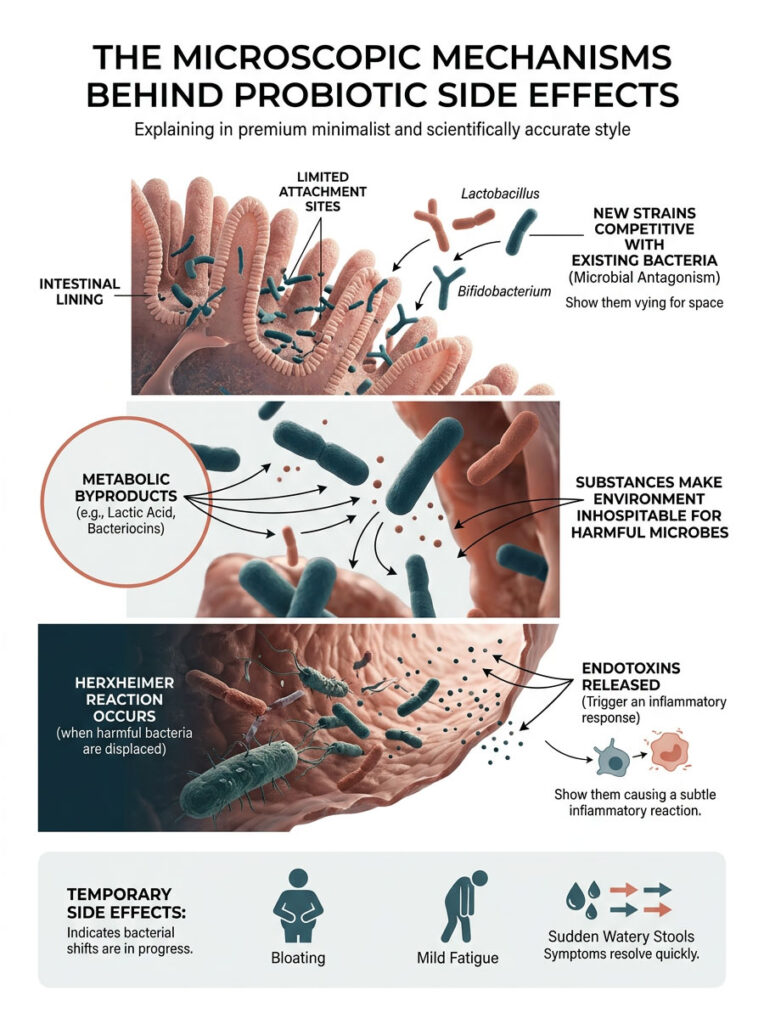
During this competition, the new strains produce metabolic byproducts like lactic acid and bacteriocins. These substances create an inhospitable environment for harmful microbes. While this is good for your long-term health, the chemical battle irritates the gut lining in the short term, stimulating rapid bowel contractions.
The Herxheimer Reaction (Die-Off Effect)
When effective probiotic strains displace harmful bacteria and yeast, those organisms die and their cell walls break open. This releases a flood of endotoxins into your digestive tract.
Your immune system detects these endotoxins and mounts an inflammatory response. The temporary inflammation causes bloating, mild fatigue, and sudden watery stools. While uncomfortable, this specific reaction actually indicates that pathogenic displacement is working. It was originally observed during early syphilis treatments and is now well documented in gut microbiome research.
The 50 Billion CFU Threshold: Why Higher Doses Cause More Problems
The wellness industry has pushed a narrative that more bacteria always means better results. Ten years ago, a standard probiotic contained about 5 billion CFUs (Colony Forming Units). Today, products routinely advertise 100 billion or even 200 billion CFUs per capsule.
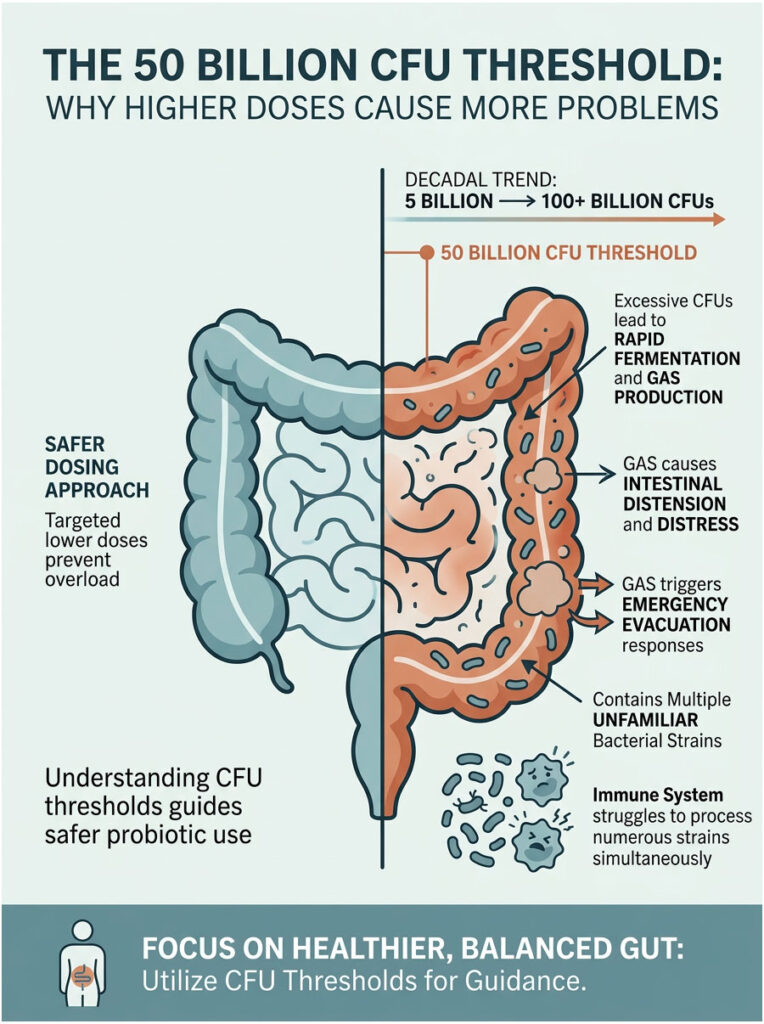
In clinical practice, the 50 billion CFU mark is generally where we see a sharp increase in adverse reactions. Exceeding this threshold floods your colon with too much fermentable activity at once. The bacteria immediately begin consuming starches and producing massive volumes of hydrogen and methane gas.
This rapid gas production physically distends the intestines. Your nervous system responds by triggering an emergency evacuation, contracting the intestines forcefully and flushing out both the excess gas and unabsorbed water.
Many mega-dose products also contain dozens of different species packed together. Your immune system struggles to process 15 unfamiliar strains arriving simultaneously. Starting with a lower, targeted dose prevents this overload entirely.
Hidden Triggers: Prebiotics, FODMAPs, and Manufacturing Fillers
Sometimes the bacteria themselves are not the problem. The hidden ingredients inside the capsule are frequently the real culprits.

Prebiotic Fibers and FODMAPs
Many manufacturers include prebiotics like inulin, chicory root, and fructooligosaccharides. These are highly fermentable carbohydrates classified as FODMAPs. If you have a sensitive stomach, these fibers act like rocket fuel for your existing bacteria, generating large amounts of trapped gas within hours.
Patients with Small Intestinal Bacterial Overgrowth (SIBO) face especially serious risks. In SIBO, bacteria have migrated from the large intestine up into the small intestine. Feeding these misplaced bacteria with inulin causes severe bloating and immediate diarrhea.
Dairy, Soy, and Histamine-Producing Strains
Many commercial strains are cultured on dairy or soy mediums during manufacturing. If you have a dairy allergy, even trace amounts of milk protein can trigger intestinal inflammation.
Certain strains, including Lactobacillus casei and Lactobacillus bulgaricus, naturally produce high levels of histamine inside the gut. For people with histamine intolerance, these strains will almost certainly cause rapid bowel motility and discomfort.
Probiotic Strains and Diarrhea Risk: A Clinical Reference
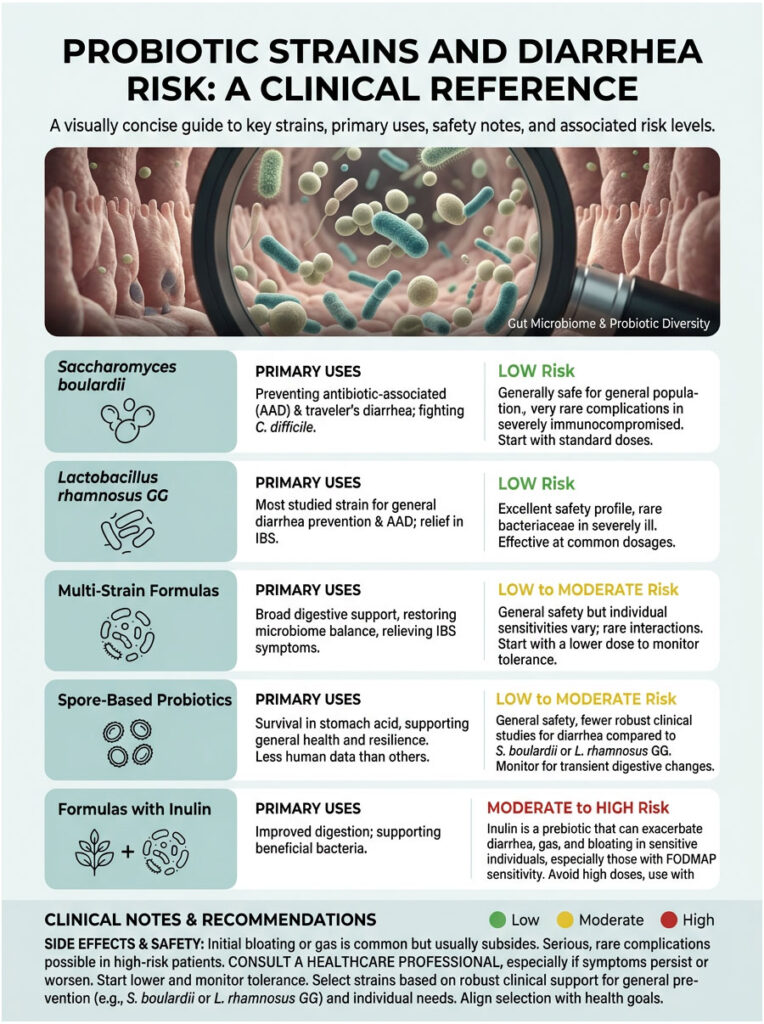
| Strain / Type | Primary Use | Diarrhea Risk | Clinical Notes |
| Saccharomyces boulardii | Acute or antibiotic-associated diarrhea | Very Low | A transient yeast that does not contribute to bacterial overgrowth. Secretes proteases that neutralize harmful toxins. |
| Lactobacillus rhamnosus GG | Gut diversity and immune support | Low to Moderate | Well-researched for safety. May cause mild initial osmotic shifts but stabilizes the mucosal barrier quickly. |
| Multi-Strain (100+ Billion CFU) | Severe dysbiosis, post-antibiotic recovery | High | Intense microbial competition causes rapid pathogenic displacement. High-dose reactions are very common without gradual introduction. |
| Spore-Based (Soil Organisms) | Intestinal permeability and immune modulation | Moderate | Survives stomach acid well. Can trigger strong Herxheimer reactions as it targets opportunistic yeast. |
| Formulas with Inulin (Prebiotics) | Feeding beneficial bacteria for long-term colonization | Very High | Rapid FODMAP fermentation pulls water into the colon. Causes severe gas and osmotic shifts. Avoid if SIBO is suspected. |
How Different Probiotic Strains Affect Bowel Motility
Not all probiotics are the same. Treating every supplement as interchangeable is a common mistake that leads to unnecessary digestive trouble.

The Lactobacillus family is the most common group in commercial products and fermented foods. These bacteria primarily live in the small intestine and produce lactic acid. While generally safe, aggressive strains like Lactobacillus acidophilus can cause mild cramping as they lower intestinal pH.
Bifidobacterium strains prefer the oxygen-free environment of the large intestine. They excel at breaking down complex carbohydrates and producing beneficial short-chain fatty acids. However, because they are heavy fermenters, introducing too many at once often causes excessive gas and loose stools.
Saccharomyces boulardii stands apart because it is not a bacterium at all. It is a non-pathogenic yeast that acts as a temporary visitor in your gut. Because it does not compete for the same attachment sites as bacteria, it rarely causes osmotic diarrhea. In fact, gastroenterologists specifically prescribe it to treat antibiotic-associated diarrhea.
Spore-based organisms like Bacillus coagulans have a tough protective shell that survives stomach acid. They are highly effective, but can trigger intense Herxheimer die-off reactions that produce temporary watery stools.
The Adjustment Period: What to Expect and When
Setting realistic expectations prevents unnecessary panic. Your body needs time to reach a new microbial balance.
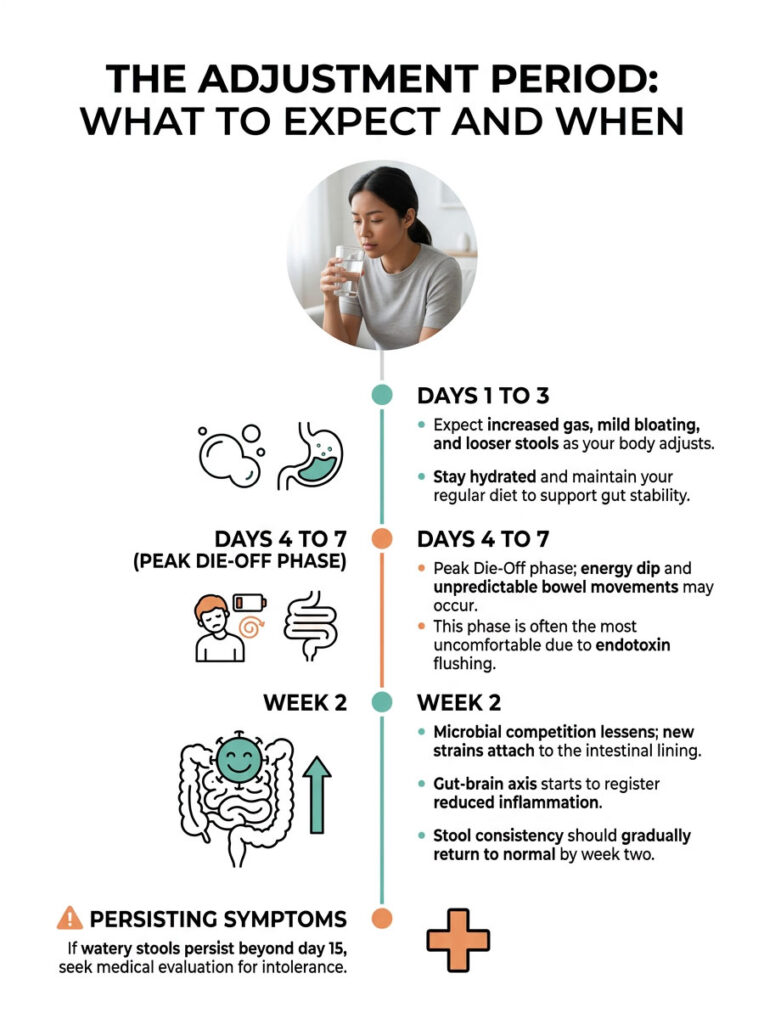
Days 1 to 3: The Acute Phase
As new strains enter your system, the adjustment begins almost immediately. Expect increased gas, mild abdominal bloating, and noticeably looser stools. This is a normal physiological response. Your resident bacteria are reacting to the newcomers. Stay hydrated and maintain your regular diet to give your gut a stable foundation.
Days 4 to 7: Peak Die-Off
This is typically when the Herxheimer reaction peaks. Your body is flushing out endotoxins released by dying pathogens. You may notice a slight dip in energy and unpredictable bowel movements. This is the most uncomfortable phase for most patients.
Week 2: Settling Down
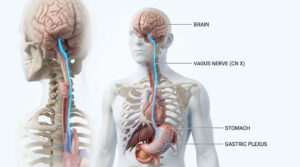
By the second week, the intense microbial competition should begin to ease. New strains are finding permanent attachment sites along your intestinal lining. Your gut-brain axis starts registering the reduced inflammation, and your enteric nervous system stops sending emergency signals. Stool consistency should gradually return to normal.
If you reach day 15 and still have watery stools with no improvement, this is no longer a normal adjustment. It indicates a medical intolerance that needs professional evaluation.
Medical Red Flags: When to Stop and See a Doctor
A mild upset stomach during probiotic adjustment is expected. But certain symptoms cross the line from harmless to dangerous. Learning to tell the difference could protect your health.

Dehydration Warning Signs
Frequent diarrhea causes rapid fluid and electrolyte loss. Watch for extreme thirst, dry mouth, dizziness when standing, and dark-colored urine. Severe fatigue and painful muscle cramps signal a dangerous electrolyte imbalance. If you cannot keep fluids down, seek immediate medical care.
Blood in Stool
Visible blood is never a normal probiotic side effect. Bright red blood (hematochezia) indicates active bleeding in the lower GI tract. Black, tarry stools (melena) suggest bleeding higher in the digestive system. Both require urgent evaluation.
Fever and Severe Pain
A mild die-off reaction may cause a slight temperature increase, but a high fever above 101 degrees Fahrenheit is a major warning sign. Sharp, debilitating abdominal pain that prevents you from standing upright is not a standard adjustment symptom. These signs may point to acute infection or severe colitis.
Immunocompromised Patients
People with weakened immune systems must be especially careful. Introducing live organisms to severely immunocompromised individuals carries a rare but real risk of systemic blood infection. Always consult your doctor before starting probiotics if you are undergoing chemotherapy or taking immunosuppressant medications.
Normal Adjustment vs. Medical Red Flags: Quick Reference
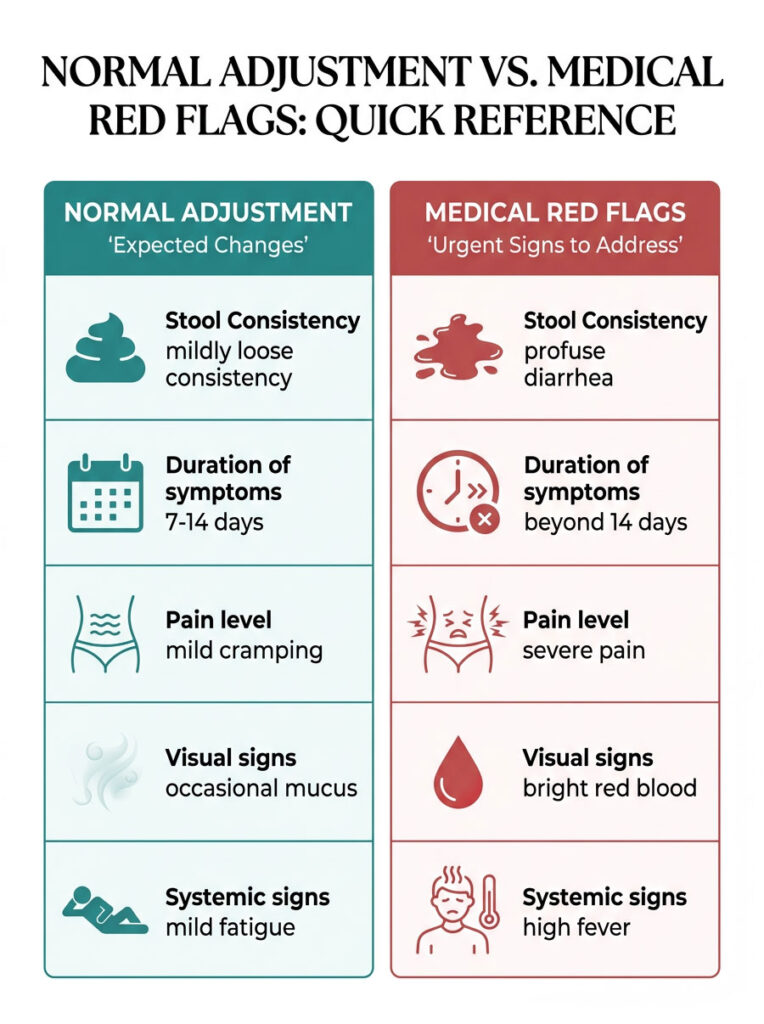
| Symptom | Normal Adjustment (Die-Off Phase) | Medical Red Flag (Seek Care Immediately) |
| Stool Consistency | Mildly loose or mushy, 2-3 times daily. | Profuse liquid diarrhea, 6+ times daily with rapid dehydration. |
| Duration | Resolves within 7 to 14 days. | Persists beyond 14 days with no improvement. |
| Pain Level | Mild cramping, fullness, or general bloating. | Severe, sharp pain preventing normal daily activity. |
| Visual Signs | Occasional mucus; minor color changes (green/yellow). | Bright red blood or black, tarry stools. |
| Systemic Signs | Mild fatigue, slight headache, low-grade temperature. | High fever over 101 F, dizziness, confusion, or fainting. |
What Recent Research Says About Probiotic Dosing
Microbiome research has advanced rapidly over the past decade. Major clinical trials have shifted how gastroenterologists approach bacterial supplementation. The trend is clearly moving away from blind mega-dosing and toward targeted, strain-specific therapy.

Recent studies from major academic centers confirm that higher CFU counts do not automatically produce better outcomes. Aggressive dosing consistently increases adverse GI events without adding therapeutic benefit. Modern protocols strongly favor a start-low, go-slow approach to ensure sustainable colonization.
Postbiotics: The Next Frontier
We are seeing growing clinical interest in postbiotics, which are the beneficial metabolic byproducts (like butyrate and acetate) produced by live bacteria. Supplementing directly with postbiotics delivers anti-inflammatory benefits without the risk of osmotic diarrhea.
Precision Microbiome Mapping
Advanced DNA stool testing now allows doctors to identify exactly which bacterial strains your colon lacks. This targeted approach prevents patients from taking incompatible strains that trigger unnecessary side effects. Lactobacillus rhamnosus GG, for example, consistently demonstrates the ability to stabilize intestinal permeability with a remarkably low risk of severe motility issues.
A Gastroenterologist’s Protocol for Sensitive Stomachs
If you want the benefits of probiotics without the misery, you need a strategic approach. Here is the clinical protocol I recommend to my patients.

Step 1: Start with Micro-Dosing (Titration Method)
Do not start with a 50 billion CFU capsule on day one. Find a quality supplement offering 5 to 10 billion CFUs. If you can only find high-dose capsules, pull the capsule apart and use a quarter of the powder mixed into cold water or applesauce. Take this micro-dose for three days. If you tolerate it well, increase to half a capsule for the next three days.
Step 2: Time Your Dose With Meals
Taking probiotics on an empty stomach is a common mistake. Your stomach acid is designed to kill incoming microbes. Instead, take your supplement in the middle of a meal containing healthy fats. The food buffers stomach acid and slows gastric transit, giving bacteria a safer journey to the lower intestines.
Step 3: Choose Enteric-Coated Capsules
Enteric coatings resist stomach acid and only dissolve in the alkaline environment of the small intestine. This significantly reduces upper digestive irritation and improves bacterial survival rates.
What to Eat During the Probiotic Adjustment Period
Your diet plays a huge role in how smoothly the adjustment goes. Here is what works.
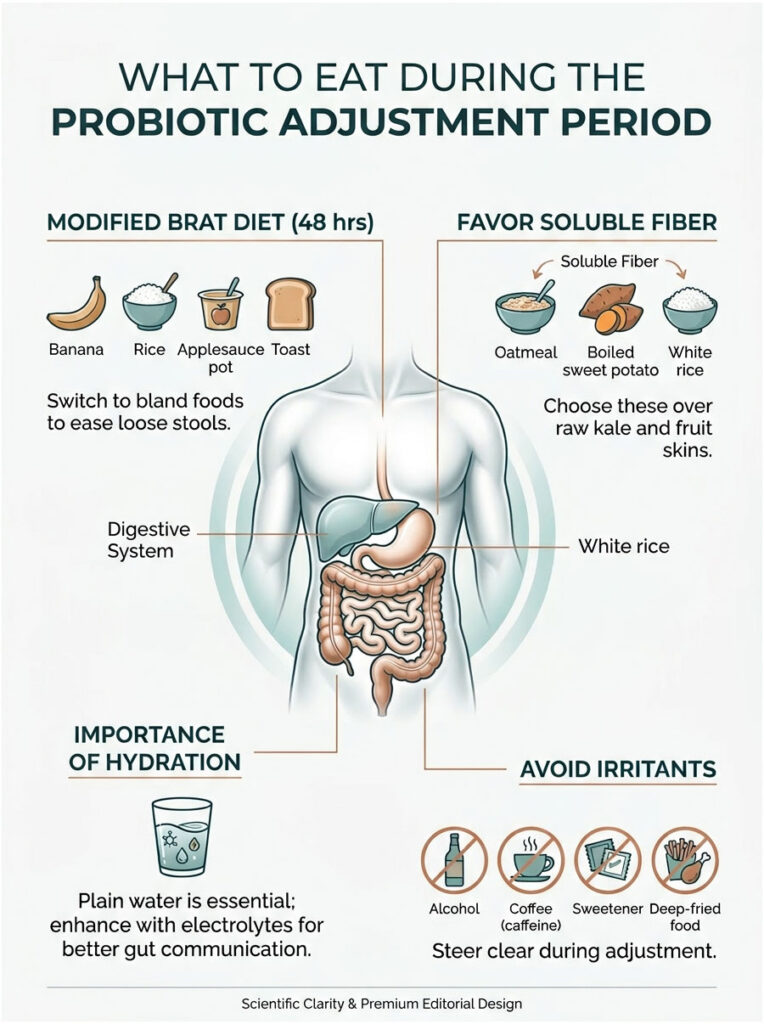
Modified BRAT Diet for Loose Stools
If you experience diarrhea, switch to a modified BRAT diet (Bananas, Rice, Applesauce, Toast) for 48 hours. These bland, binding foods add bulk to your stool and slow down rapid bowel transit.
Soluble Fiber Over Insoluble Fiber
Insoluble fiber from raw kale and fruit skins speeds up digestion, which is the last thing you want during an adjustment phase. Focus instead on soluble fiber sources like plain oatmeal, boiled sweet potatoes, and white rice. Soluble fiber absorbs excess water in the colon, forming a gel that firms up loose stools.
Hydration and Electrolytes
Staying hydrated is critical. Plain water helps, but adding electrolytes is significantly better. Balanced sodium and potassium intake supports gut-brain communication and helps regulate the smooth muscle contractions causing your symptoms.
Foods to Avoid
While your microbiome adjusts, strictly avoid alcohol, excessive caffeine, artificial sweeteners, and deep-fried foods. These irritants will make symptoms noticeably worse. Give your gut clean, bland fuel while it establishes a healthy new bacterial balance.
Final Thoughts
Can probiotics cause diarrhea? Absolutely, and now you understand exactly why. Introducing large numbers of live bacteria naturally disrupts your gut ecosystem. The resulting microbial competition, pathogenic displacement, and die-off reactions produce temporary digestive discomfort.
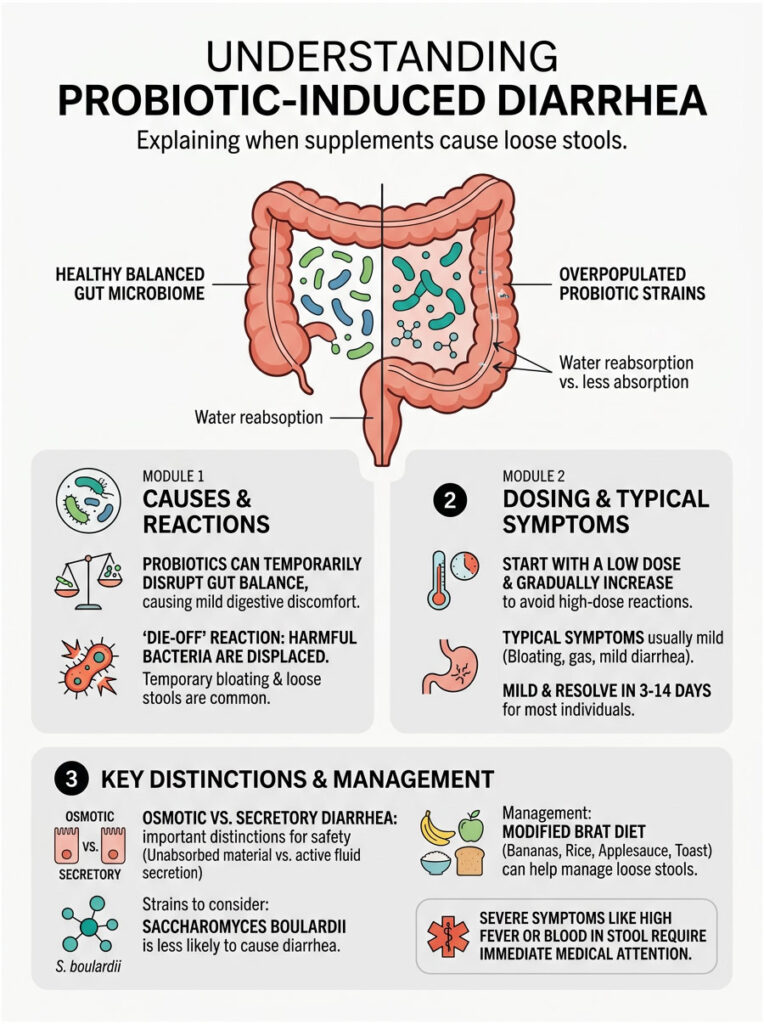
For most people, mild bloating, gas, and loose stools resolve within 7 to 14 days. High-dose reactions are easily prevented by starting with a low dose and increasing gradually. Choose your strains carefully, take them with food, and stay hydrated.
If you experience severe abdominal pain, high fever, or visible blood in your stool, stop the supplement immediately and see your doctor. A temporary upset is often just the first step toward genuine, lasting digestive improvement.
Frequently Asked Questions
Why do probiotics cause diarrhea in healthy adults?
As a gastroenterologist, I often explain this as a ‘microbial turf war.’ When you introduce billions of new bacterial agents into your gut, they must compete with existing commensal bacteria for physical real estate on the intestinal lining. This competition, known as microbial antagonism, causes temporary irritation and osmotic shifts that draw excess water into the colon, leading to rapid bowel motility and loose stools.
How long should I expect probiotic-induced diarrhea to last?
For most patients, the digestive adjustment period is temporary. You will typically see symptoms resolve within 3 to 7 days as your microbiome reaches a new state of equilibrium. However, if your symptoms persist beyond the 14-day window without any improvement in stool consistency, it is no longer a standard adjustment and requires a clinical consultation.
What is the ‘die-off’ or Herxheimer reaction in gut health?
The Herxheimer reaction occurs when potent bacterial strains successfully displace opportunistic pathogens or yeast. As these harmful organisms perish, their cell walls rupture and release endotoxins into your digestive tract. Your immune system responds to these toxins with localized inflammation, which can manifest as temporary bloating, fatigue, and watery diarrhea.
Is a higher CFU count always better for digestive health?
Not necessarily. In clinical practice, we see a sharp increase in adverse gastrointestinal events once a supplement exceeds the 50 billion CFU (Colony Forming Units) threshold. Hyper-dosed products can overwhelm the colon with fermentable activity, producing massive amounts of gas and triggering an emergency evacuation response from the enteric nervous system.
How can I tell the difference between osmotic and secretory diarrhea?
The distinction is vital for patient safety. Osmotic diarrhea, usually caused by supplements or malabsorption, occurs when unabsorbed substances pull water into the bowel; it typically stops if you fast. Secretory diarrhea is more dangerous, often caused by infections or toxins that force the body to pump water into the intestines, and it continues regardless of food intake.
Can hidden ingredients like inulin cause a reaction?
Absolutely. Many manufacturers include prebiotics like inulin or chicory root to ‘feed’ the bacteria. These are highly fermentable carbohydrates (FODMAPs) that can cause severe gas and osmotic diarrhea in sensitive individuals, particularly those with Small Intestinal Bacterial Overgrowth (SIBO), where bacteria inappropriately ferment these fibers in the small intestine.
What is the best way to introduce a new probiotic to avoid side effects?
I recommend the titration method: start ‘low and slow.’ Begin with a micro-dose of 5 to 10 billion CFUs, or even a fraction of a higher-dose capsule, for the first few days. Gradually increase the dosage over two weeks to allow your enteric nervous system and existing microbiome to adapt without triggering a defensive flushing response.
Should I take my probiotic on an empty stomach or with food?
To minimize gastric distress, I advise taking your supplement in the middle of a substantial meal that contains healthy fats. Food acts as a natural buffer against corrosive stomach acid, raising the pH level and protecting the live organisms. This also slows down gastric transit time, ensuring a gentler delivery to the lower intestines.
Are there specific strains that are less likely to cause diarrhea?
Saccharomyces boulardii is an excellent choice for sensitive patients. Unlike most supplements, it is a non-pathogenic yeast rather than a bacterium. It does not engage in the same aggressive microbial antagonism as bacterial strains and is frequently used clinically to actually halt diarrhea caused by antibiotics or pathogens.
What are the medical red flags that indicate I should stop supplementation?
You should seek immediate medical attention if you experience hematochezia (visible blood in stool), melena (black, tarry stools), a high fever over 101°F, or signs of severe dehydration such as dizziness and dark urine. Sharp, debilitating abdominal pain that prevents daily activity is also a sign of a serious adverse event rather than a normal adjustment.
Can probiotics cause issues for immunocompromised patients?
Yes, patients with compromised immune systems must exercise extreme caution. Because probiotics contain live biological agents, there is a rare but documented risk of these bacteria entering the bloodstream and causing a systemic infection. Always consult your specialist if you are undergoing chemotherapy or taking immunosuppressants before starting a regimen.
What should I eat if I am experiencing loose stools from a supplement?
Switch to a modified BRAT diet (Bananas, Rice, Applesauce, Toast) for 48 hours to provide binding bulk to your stool. Focus on soluble fiber sources like plain oatmeal or boiled potatoes, which absorb excess water in the colon. Avoid insoluble fiber (like raw kale), caffeine, and artificial sweeteners, as these will further irritate the gut lining during the recalibration phase.
Disclaimer
This article is for informational purposes only and does not constitute medical advice. The biological reactions described, including diarrhea and the Herxheimer reaction, can vary significantly between individuals. Always consult a qualified healthcare professional or board-certified gastroenterologist before starting a new supplement regimen, especially if you are immunocompromised, pregnant, or have underlying gastrointestinal conditions.
References
- National Institutes of Health (NIH) – Office of Dietary Supplements – Comprehensive fact sheet on probiotic strains, dosage (CFU), and documented side effects.
- World Gastroenterology Organisation (WGO) – Global Guidelines on Probiotics and Prebiotics – Clinical evidence regarding the use of L. rhamnosus GG and S. boulardii for diarrhea management.
- Journal of Clinical Gastroenterology – Research paper on “Microbial Antagonism and the Gut Microbiota” detailing the competition between commensal and introduced bacterial strains.
- Harvard Health Publishing – “Health benefits of taking probiotics” – Expert insight into the osmotic shifts and digestive adjustment periods in healthy adults.
- American Journal of Health-System Pharmacy – Study on the “Herxheimer Reaction in Microbiome Shifting” – Clinical data regarding endotoxin release during pathogenic die-off.
- International Scientific Association for Probiotics and Prebiotics (ISAPP) – Statistical data on the 50 billion CFU threshold and the prevalence of mild gastrointestinal side effects.