If you want to know how to stop coughing at night, the first step is identifying your specific respiratory trigger. Elevate your head with an 8-inch wedge pillow to counteract gravity and stop post-nasal drip. Run a cool-mist humidifier set to 45 percent humidity to keep your airway hydrated.
Table of Contents
For a dry cough, take a targeted antitussive. For a wet cough, use an expectorant with at least 16 ounces of water. And always address underlying issues like silent acid reflux or nocturnal asthma if you want lasting relief.

Key Statistics on Nighttime Coughing
- Over 30 million Americans deal with chronic nighttime respiratory disruptions every year.
- Upper Airway Cough Syndrome accounts for nearly 40 percent of all chronic cough diagnoses.
- Silent acid reflux causes up to 25 percent of unexplained nighttime throat irritation.
- Airway resistance naturally increases by up to 50 percent around 4:00 AM due to hormonal shifts.
- Keeping indoor humidity between 40 and 50 percent reduces airborne viral survival rates by about 30 percent.
Why Your Cough Gets Worse the Moment You Lie Down
As a board-certified pulmonologist and sleep specialist, I treat thousands of patients whose sleep is wrecked by nighttime coughing. If you’re desperately searching for how to stop coughing at night, there’s something you need to understand first: lying down changes your airway mechanics completely.

A persistent cough at night is rarely a standalone issue. It’s a physiological response to specific triggers that kick in when your body shifts into rest mode. Gravity changes when you lie flat. Your natural mucus clearance slows down. Circadian rhythms influence airway inflammation in ways most people never realize.
In this guide, I’ll walk you through the biomechanics behind your nighttime cough, cover evidence-based immediate remedies, outline the right medications, and share long-term strategies to fix the root cause. From what I see in clinical practice every day, treating the symptom without understanding the trigger leads to endless sleepless nights.
The Physiology Behind Nighttime Coughing
To truly understand how to stop coughing at night, you need to know what’s happening inside your respiratory system while you sleep. Your lungs and upper airways function very differently at night compared to the daytime. That sudden worsening at bedtime isn’t random. It’s a measurable result of positional changes and hormonal shifts.

Your body runs on a strict 24-hour internal clock called the circadian rhythm. During the night, your levels of cortisol and epinephrine naturally dip. These are the hormones that suppress inflammation and keep your bronchial tubes open during the day. When they drop, airway resistance increases, often leading to bronchospasm peaks in the early morning hours.
This is why so many patients report waking up gasping or wheezing right before dawn. It’s your circadian biology directly altering your airway mechanics while you sleep.
The Recumbent Position Effect
The recumbent position effect is the main reason your cough flares up the moment your head hits the pillow. When you’re upright during the day, gravity works as a natural drainage system, pulling nasal secretions and stomach acids safely downward.
Lying flat eliminates that gravitational help entirely. Your mucociliary clearance, the process where tiny hair-like structures called cilia sweep mucus out of your lungs and nasal passages, gets severely compromised. That mucus pools in the back of your throat and directly stimulates the vagus nerve.
The vagus nerve is a massive nerve network running from your brainstem into your abdomen. When pooled mucus irritates the nerve endings in your throat, it fires a rapid signal to your brain, which forces a violent exhalation to clear the perceived obstruction. You can’t fight this biology, but you can manipulate your sleeping position to outsmart it.
Upper Airway Cough Syndrome (Post-Nasal Drip)
Upper Airway Cough Syndrome is the modern clinical term for what most people call post-nasal drip. According to guidelines from the American College of Chest Physicians, this syndrome is responsible for the vast majority of chronic nighttime coughing. It’s incredibly common but frequently misunderstood.
Your nasal mucosa produces excess secretions due to allergies, sinus infections, or environmental irritants. The average person produces about 1.5 liters of mucus every day. During the day, you swallow it unconsciously. At night, the recumbent position causes that volume to accumulate right over your vocal cords, creating a maddening tickle in the back of your throat.
If you feel like you’re choking on thick mucus specifically when lying down, post-nasal drip is the likely culprit. Treating it means aggressively drying up the nasal passages before bed, which we’ll cover in the medication section below.
Diagnosing the Root Cause: Dry Cough vs. Productive Cough
You can’t treat a nighttime cough effectively without knowing what type you’re dealing with. The approach changes entirely depending on what’s irritating your airway.

A dry cough produces no mucus, feels scratchy, and often starts as a tickle in the upper throat. A productive cough brings up thick phlegm from deep in the chest. Mixing up these two diagnoses leads to wrong medication choices and prolonged misery.
Silent Reflux and Micro-Aspiration
Many patients are genuinely shocked to learn that their lungs are healthy but their stomach is causing the cough. This condition is called Laryngopharyngeal Reflux, or LPR. Unlike traditional heartburn, it often presents without any chest burning at all, which is why doctors call it silent reflux.
When you lie flat, microscopic droplets of acidic stomach fluid breach your upper esophageal sphincter and spill into the delicate larynx and trachea. Your vocal cords are incredibly sensitive to acid because they lack a protective mucosal barrier. Even a microscopic drop at a pH of 2.0 causes severe irritation and choking spasms.
If you wake up with a sour or metallic taste, morning hoarseness, or a sudden choking sensation, silent reflux is the probable cause. Managing it requires dietary changes and precise sleeping adjustments to keep stomach acid where it belongs.
Nocturnal Asthma and Cough-Variant Asthma
Asthma doesn’t always come with audible wheezing. Cough-variant asthma is a specific subtype where the only symptom is a chronic, dry, hacking cough that frequently peaks in the middle of the night.
Cooler bedroom temperatures and prolonged exposure to dust mites trigger a localized histamine response in your lungs. This causes the smooth muscles around your airways to constrict, a reaction known as a bronchospasm. If your chest feels tight and you have a dry cough that worsens in the early morning hours, nocturnal asthma is very likely. This needs evaluation by a pulmonologist for proper inhaled therapy. Over-the-counter syrups won’t relax smooth muscle tissue.
Post-Viral Airway Hyperresponsiveness
Recently recovered from a bad cold, the flu, or COVID-19? You might be dealing with post-viral airway hyperresponsiveness. A severe viral infection strips the protective top layer of cells from your airway, leaving sensitive nerve endings completely exposed.
This lingering irritation can last anywhere from three to eight weeks. Because the nerves are raw, even a slight change in air temperature or a deep breath can trigger a violent cough. If you have a persistent tickle that won’t go away after being sick, your airway just needs time to heal.
Expert Tip: Don’t panic if the irritation stretches into the second month. The respiratory epithelium regenerates slowly. Focus on keeping your throat lubricated to protect the exposed nerve endings while they rebuild.
Clinical Diagnostic Reference Table
| Symptom Profile | Nighttime Behavior | Likely Cause | First-Line Action |
| Dry, hacking tickle in throat | Worsens immediately when lying flat | Upper Airway Cough Syndrome | Elevate head, saline nasal rinse before bed |
| Dry spasm, bitter or acidic taste | Morning hoarseness, constant throat clearing | Silent Reflux (LPR) | Avoid late meals, sleep on left side |
| Wheezing, tight chest | Peaks between 3 AM and 5 AM | Nocturnal Asthma | Prescription bronchodilators, HEPA filter |
| Wet cough, yellow/green mucus | Deep chest congestion, nasal blockage | Bronchitis or active viral infection | Expectorant with aggressive hydration |
Immediate Strategies for Nighttime Cough Relief
When you’re wide awake and miserable at 2 AM, you need solutions that work right now. Figuring out how to stop coughing at night starts with fast, mechanical, positional, and topical interventions to calm the vagus nerve and get you back to sleep.
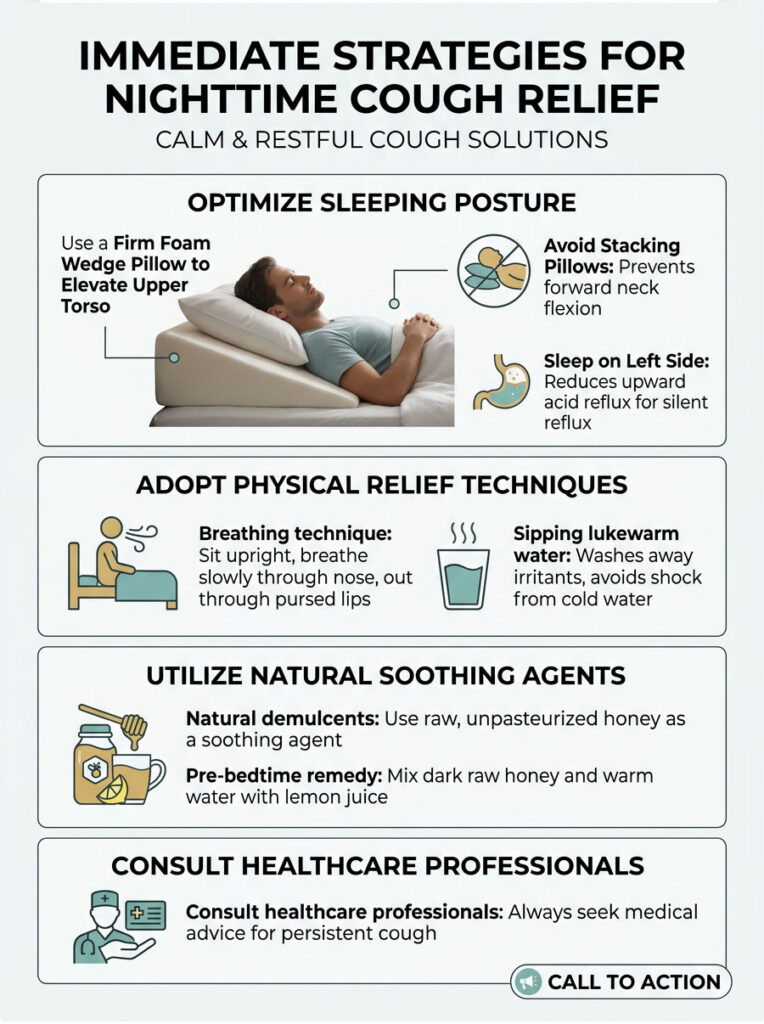
Fix Your Sleeping Position First
The single most effective immediate step is changing your resting position. I strongly recommend a firm 6 to 8-inch foam wedge pillow. Many patients try stacking standard pillows, but this is a common mistake. Stacking pillows causes forward neck flexion, which crimps your windpipe and can worsen conditions like sleep apnea.
A proper wedge pillow elevates your entire upper torso in a straight, anatomically correct line. This prevents post-nasal drip from pooling on your vocal cords and uses gravity to push acidic stomach fluids down, directly treating silent reflux flare-ups.
If you have documented silent reflux, also try sleeping on your left side. The anatomical shape of the human stomach makes upward acid reflux much harder from that position.
Breathing Techniques for Coughing Fits
If you wake up choking and need relief fast, sit bolt upright on the edge of the bed with both feet flat on the floor. Take slow, controlled breaths in through your nose and out through tightly pursed lips.
This pursed-lip breathing technique creates positive end-expiratory pressure inside your lungs, which physically props your collapsing airways open from the inside. Sipping lukewarm water will also wash away acidic irritants triggering the vagus nerve. Avoid ice-cold water during a spasm, as cold temperatures can shock the vagus nerve and cause throat muscles to constrict tighter.
Natural Demulcents: Honey, Lemon, and Warm Water
When patients ask me how to stop coughing at night without prescription medication, I always point them toward natural demulcents. A demulcent is a thick, viscous substance that creates a soothing physical film over raw mucous membranes, shielding exposed nerve receptors from airflow and acid irritation.
Peer-reviewed studies from the Cochrane Database confirm that raw, unpasteurized honey is a highly effective natural demulcent. Dark buckwheat honey, in particular, performs exceptionally well against over-the-counter syrups in clinical trials.
Here’s a pre-bedtime protocol that works: mix one tablespoon of dark raw honey into a small cup of warm water. Add a fresh squeeze of lemon juice, which acts as a mild astringent to cut through thick mucus. This combination is widely considered by pulmonologists to be one of the best natural remedies for chest congestion and throat irritation.
Choosing the Right Medication: A Pharmacological Guide
Sometimes, positional changes and honey aren’t enough. When you need to know how to stop coughing at night using pharmacy options, selecting the exact right medication class is critical. Choosing wrong can actually make symptoms worse.

The most important decision you’ll make in the pharmacy aisle is choosing between an antitussive and an expectorant. These two drug classes do completely opposite things. Millions of dollars are wasted annually on combination syrups that actively fight against each other. Target your specific symptom with a single-ingredient approach whenever possible.
Antitussives (Cough Suppressants)
Antitussives suppress coughing at the brain level. The most common active ingredient is Dextromethorphan, often labeled “DM” on the packaging. It crosses your blood-brain barrier, binds to sigma-1 receptors, and raises the cough threshold in your medulla oblongata. In simple terms, it tells your brain to ignore the distress signals from your irritated throat.
Use an antitussive only for a dry, non-productive cough that’s keeping you awake and producing no mucus. Never use a brain-level suppressant for a wet, productive cough. Suppressing a productive cough traps infected mucus deep in your lungs.
Expectorants and Mucolytics
If you’re dealing with a heavy, wet, rattling chest, you need an expectorant like Guaifenesin. It works by thinning out thick mucus, reducing its surface tension and viscosity so your natural clearance mechanisms can do their job.
Here’s the key detail most people miss: Guaifenesin requires a lot of water to work. If you take it while dehydrated, it does essentially nothing. Drink at least 16 ounces of water with the pill to activate the mucolytic process. And never mix an expectorant with an antitussive. Suppressing a productive cough traps dangerous bacterial infections in your lower airways, which can lead to pneumonia.
Antihistamines and Corticosteroids
If Upper Airway Cough Syndrome is your primary issue, you need to dry up the drip at its source. First-generation antihistamines like Diphenhydramine have strong anticholinergic properties that physically dry out dripping mucous membranes. Taking one 30 minutes before bed can stop post-nasal drip from forming in the first place.
For chronic, year-round sinus inflammation, intranasal corticosteroids like Fluticasone are the gold standard. These sprays reduce the cellular swelling inside your nasal passages, stopping the drip at its anatomical origin.
Many patients also ask about menthol chest rubs. These don’t actually dilate your airways, but the strong scent stimulates cold receptors in your nasal passages, tricking your brain into feeling like breathing is easier. A menthol rub is a solid supplemental comfort measure during a viral infection.
Medication Reference Table
| Drug Class | Active Ingredient | How It Works | Best For | Warning |
| Antitussive | Dextromethorphan (DM) | Raises cough threshold in the brain’s medulla | Dry, sleep-disrupting cough | Never use for asthma or wet chest congestion |
| Expectorant | Guaifenesin | Thins mucus viscosity to improve airway clearance | Thick, deep chest congestion | Requires 16oz of water to activate properly |
| Antihistamine | Diphenhydramine | Blocks histamine receptors, dries secretions | Allergy-driven post-nasal drip | Can cause severe next-day grogginess |
| Topical Analgesic | Menthol (Vapor Rub) | Creates cooling sensation in nasal receptors | Mild viral upper airway irritation | Does not physically open constricted airways |
Always consult your physician or a licensed pharmacist before combining over-the-counter medications, especially if you take prescription blood pressure drugs.
Optimizing Your Bedroom Environment for Respiratory Health
Treating your bedroom as a recovery space is one of the most effective strategies for how to stop coughing at night. The air you breathe for eight hours every night needs to be optimized for healing. Dust, dry air, and pet dander act like sandpaper on an inflamed respiratory tract.

Humidity Control
Dry air strips moisture from your respiratory mucosa with every breath, triggering bronchospasms and making a dry cough worse. You need to add clean, filtered moisture back into your bedroom air.
I recommend a cool-mist humidifier over a warm-mist vaporizer. Warm mist can cause inflamed nasal passages to swell further, and the heating element poses a burn risk. The sweet spot for bedroom humidity is between 40 and 50 percent, high enough to soothe raw mucosa but low enough to prevent dust mites and mold from thriving.
A quick note on nebulizers vs. humidifiers: a nebulizer is a medical device that turns liquid prescription medication into a breathable mist for deep lung delivery. A humidifier simply adds water vapor to room air. If you have diagnosed asthma, you may need a nebulizer during severe flare-ups. For everyday airway comfort, a humidifier is the right tool.
Managing Indoor Allergens
Irritated airways are incredibly sensitive to microscopic airborne particles. Pet dander, pollen, and dust mite debris are notorious triggers for Upper Airway Cough Syndrome.
Invest in a True HEPA air purifier for your nightstand. These filters capture particles as small as 0.3 microns with 99.97 percent efficiency. Run it on high for two hours before bed, then switch to a low setting while you sleep. Also wash all bedding in hot water (at least 130 degrees Fahrenheit) every week to kill embedded dust mites.
Safe Remedies for Children: Pediatric Considerations
Children are not just small adults. Their respiratory systems are anatomically smaller, their tracheas are floppier, and their drug metabolism is highly variable. A child’s airway is roughly the diameter of a drinking straw, so even minor mucosal swelling can cause serious respiratory distress.

FDA Guidelines and Age-Appropriate Care
The FDA has issued strict warnings against using over-the-counter cold medicines in young children. Children under four should never receive pharmacological suppressants like Dextromethorphan. The risk of accidental overdose and respiratory depression is too high.
So what can you do at 3 AM with a coughing toddler? Focus on safe, non-pharmacological approaches: gentle saline nasal drops followed by careful bulb suctioning, and continuous cool-mist humidification throughout the night.
For children over one year, natural honey formulations are recommended by pediatricians worldwide. Clinical studies show honey is just as effective as commercial syrups for suppressing nighttime coughing in toddlers. However, never give honey to an infant under 12 months. Their digestive systems can’t handle botulism spores occasionally found in honey. Stick to saline and cool mist for babies under one.
When to See a Doctor: Clinical Red Flags
Most nighttime coughs are ultimately harmless, but some symptoms demand immediate medical attention. Knowing how to spot the red flags is a critical skill.

- Hemoptysis (coughing up bright red blood or blood-streaked mucus) is never normal and requires an immediate chest X-ray or CT scan.
- Symptoms persisting longer than eight consecutive weeks officially classify as a chronic cough and require a full diagnostic workup, including spirometry.
- Rapid unintentional weight loss, severe shortness of breath at rest, or drenching night sweats are major warning signs.
- Pink, frothy sputum is an emergency. Go to the ER immediately.
These symptoms could point to undiagnosed COPD, congestive heart failure, or severe pulmonary infections. Do not rely on home remedies if any of these apply to you.
Final Takeaways: How to Stop Coughing at Night for Good
Learning how to stop coughing at night is entirely possible when you apply clinical science to your specific symptoms. It comes down to identifying your trigger and matching it with the correct therapy.
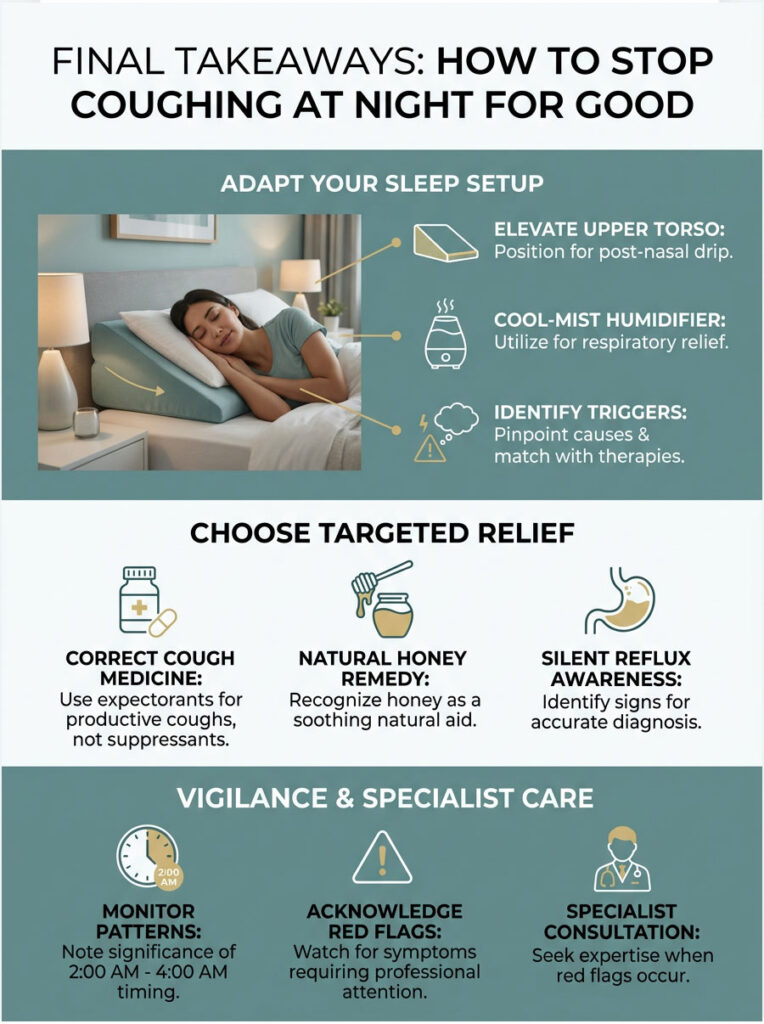
- Identify your trigger: Is it Upper Airway Cough Syndrome, silent reflux, or nocturnal asthma? Dry vs. wet cough dictates your entire treatment plan.
- Fix your sleeping posture: Use a firm 8-inch wedge pillow. The right position counteracts the recumbent position effect and prevents acid micro-aspiration.
- Hydrate your raw mucosa: A warm cup of water with dark buckwheat honey is one of the best natural remedies for throat irritation before bed.
- Choose medication wisely: Antitussives for dry coughs, expectorants for wet coughs. Never suppress a productive, infected chest.
- Optimize your bedroom air: Keep humidity between 40 and 50 percent with a cool-mist humidifier. Use a HEPA filter to remove allergens.
Apply these strategies consistently, and you can reclaim your sleep and let your respiratory system heal. If symptoms persist beyond eight weeks or include any red flags, see a pulmonologist. With the right approach, you’ll finally know how to stop coughing at night and wake up actually feeling rested.
Frequently Asked Questions
Why does my cough intensify specifically between 2:00 AM and 4:00 AM?
This nocturnal spike is driven by your body’s circadian rhythm. During these early morning hours, your levels of endogenous cortisol and epinephrine—hormones that naturally suppress inflammation and dilate bronchial tubes—reach their lowest point. This hormonal dip increases airway resistance and heightens your sensitivity to triggers, often resulting in severe bronchospasms.
What is the most effective sleeping position to stop post-nasal drip from triggering a cough?
To combat the ‘recumbent position effect,’ you should use a firm 6 to 8-inch foam wedge pillow to elevate your entire upper torso. Unlike stacking standard pillows, which can cause neck flexion and restrict the airway, a wedge pillow keeps your trachea aligned and uses gravity to prevent mucus from pooling on your vocal cords or stomach acid from reaching the larynx.
How can I tell if my nighttime cough is caused by ‘silent reflux’ (LPR)?
Laryngopharyngeal Reflux (LPR) often lacks traditional heartburn symptoms. Clinical indicators include a sour or metallic taste upon waking, chronic morning hoarseness, and a frequent need to clear your throat. This occurs due to micro-aspiration, where acidic gastric fluid irritates the delicate laryngeal tissue, which lacks a protective mucosal barrier.
Can I use a cough suppressant for a chesty, productive cough?
As a pulmonologist, I strongly advise against using central antitussives (suppressants) like Dextromethorphan for a wet, productive cough. Suppressing the urge to expel mucus traps infected secretions deep within the lower respiratory tract, significantly increasing your risk of developing secondary bacterial pneumonia. Instead, use an expectorant like Guaifenesin with 16 ounces of water to thin the mucus.
What is the ‘pursed-lip breathing’ technique for stopping a coughing fit?
If you wake up with a spasmodic fit, sit upright and inhale slowly through your nose, then exhale through tightly pursed lips as if blowing out a candle. This creates positive end-expiratory pressure (PEEP) within the lungs, which physically props open collapsing airways and helps stabilize the vagus nerve trigger.
Why is a cool-mist humidifier preferred over a warm-mist vaporizer for respiratory relief?
Cool-mist humidifiers are clinically superior because warm mist can cause further swelling of already inflamed nasal passages. Additionally, cool-mist units are safer in pediatric settings and help maintain the ideal humidity range of 40 to 50 percent, which is the ‘sweet spot’ for soothing raw mucosa without encouraging the growth of dust mites or mold.
How long is a ‘normal’ post-viral cough expected to last?
Following a viral infection like COVID-19 or the flu, you may experience ‘post-viral airway hyperresponsiveness.’ Because the respiratory epithelium—the protective top layer of airway cells—regenerates slowly, it is clinically normal for a lingering tickle or dry cough to persist for three to eight weeks as the nerve endings remain hypersensitive to airflow.
Is honey actually an effective clinical remedy for nocturnal coughing?
Yes. Peer-reviewed studies confirm that raw honey, particularly dark buckwheat honey, acts as a potent natural demulcent. It forms a viscous protective film over the pharyngeal mucosa, physically shielding exposed nerve receptors from irritation. For adults and children over age one, it has been shown to be as effective as many over-the-counter chemical suppressants.
What are the clinical ‘red flags’ that indicate I need to see a pulmonologist?
You should seek specialist care if you experience hemoptysis (coughing up blood), drenching night sweats, rapid unexplained weight loss, or severe dyspnea (shortness of breath). Additionally, any cough that persists beyond eight weeks is classified as chronic and requires a diagnostic workup, including spirometry or chest imaging.
How does Upper Airway Cough Syndrome (UACS) differ from a standard cold?
UACS is the clinical term for chronic post-nasal drip. While a cold is an acute infection, UACS is often a prolonged response to allergies or environmental irritants. It causes a constant drip that accumulates over the vocal cords when you lie flat, triggering a persistent, maddening tickle rather than the systemic aches and fevers associated with a virus.
Can I give my infant honey to help with their nighttime congestion?
Absolutely not. You must never give honey to an infant under 12 months of age due to the risk of infant botulism, a rare but potentially fatal condition caused by Clostridium botulinum spores. For infants, stick to non-pharmacological supportive care such as saline nasal drops, bulb suctioning, and cool-mist humidification.
Does a menthol chest rub actually help open the airways?
Menthol does not act as a physical bronchodilator; it does not widen the bronchial tubes. Instead, it aggressively stimulates cold receptors in the nasal passages, which tricks the brain into perceiving that breathing is easier and deeper. While it provides significant sensory comfort and can aid sleep, it should be used as a supplemental therapy rather than a primary treatment for constriction.
Disclaimer
This article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. Always seek the advice of a board-certified physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read in this article.
References
- American College of Chest Physicians (CHEST) – journal.chestnet.org – Clinical guidelines for the diagnosis and management of chronic and nocturnal cough.
- Cochrane Database of Systematic Reviews – cochranelibrary.com – Meta-analysis on the efficacy of honey as a demulcent for acute pediatric and adult respiratory spasms.
- U.S. Food and Drug Administration (FDA) – fda.gov – Official safety communications regarding the use of OTC cold and cough products in children under 4.
- Mayo Clinic – mayoclinic.org – Expert insights on Laryngopharyngeal Reflux (LPR) and its impact on the respiratory system.
- National Sleep Foundation – thensf.org – Research on the impact of bedroom environment and humidity on sleep architecture and breathing.
- Environmental Protection Agency (EPA) – epa.gov – Standards for HEPA filtration and indoor air quality management for respiratory patients.