People ask me this question in the clinic almost every week: can anxiety cause diarrhea? The short answer is absolutely yes. When you feel overwhelmed, your stomach reacts almost instantly. This physical response to mental distress is incredibly common, and it’s far more disruptive than most people realize.
Table of Contents
It isn’t just in your head. It’s a proven biological reality. Your brain and your digestive tract share a direct, high-speed communication line. When panic sets in, your body prioritizes immediate survival over routine digestion. We see this play out daily in gastroenterology practices.
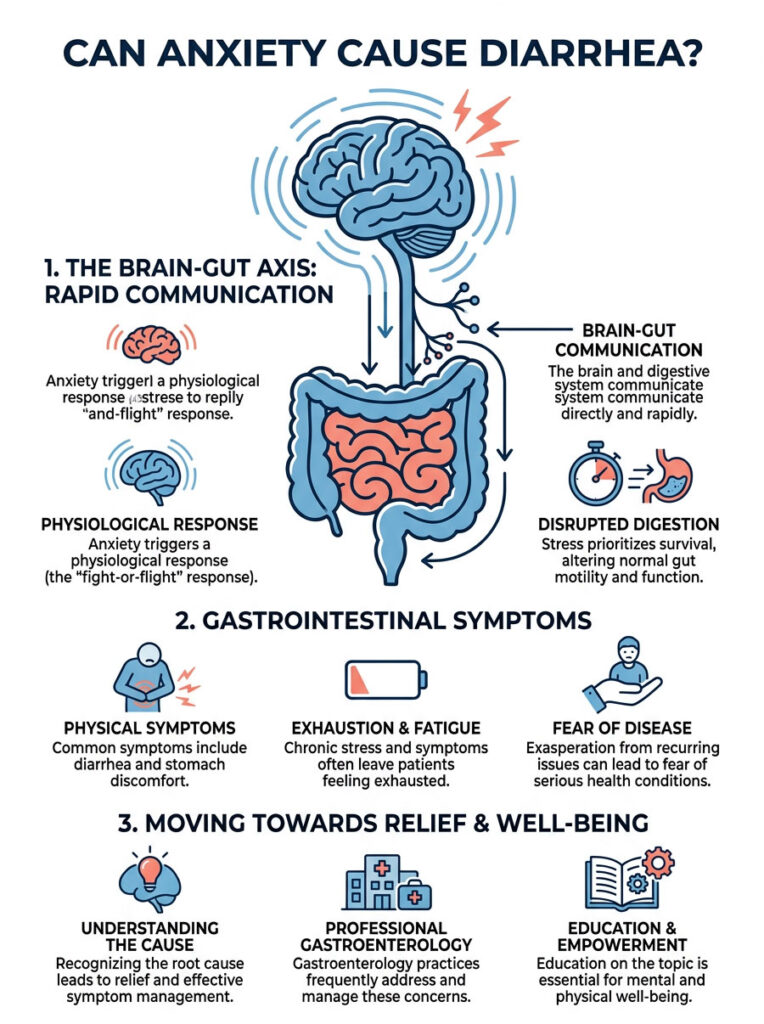
Patients arrive exhausted and terrified that something is seriously wrong. Once we walk them through the physiological mechanisms behind their symptoms, the relief is immediate. Understanding the “why” is often the first real step toward feeling better.
Quick Answer
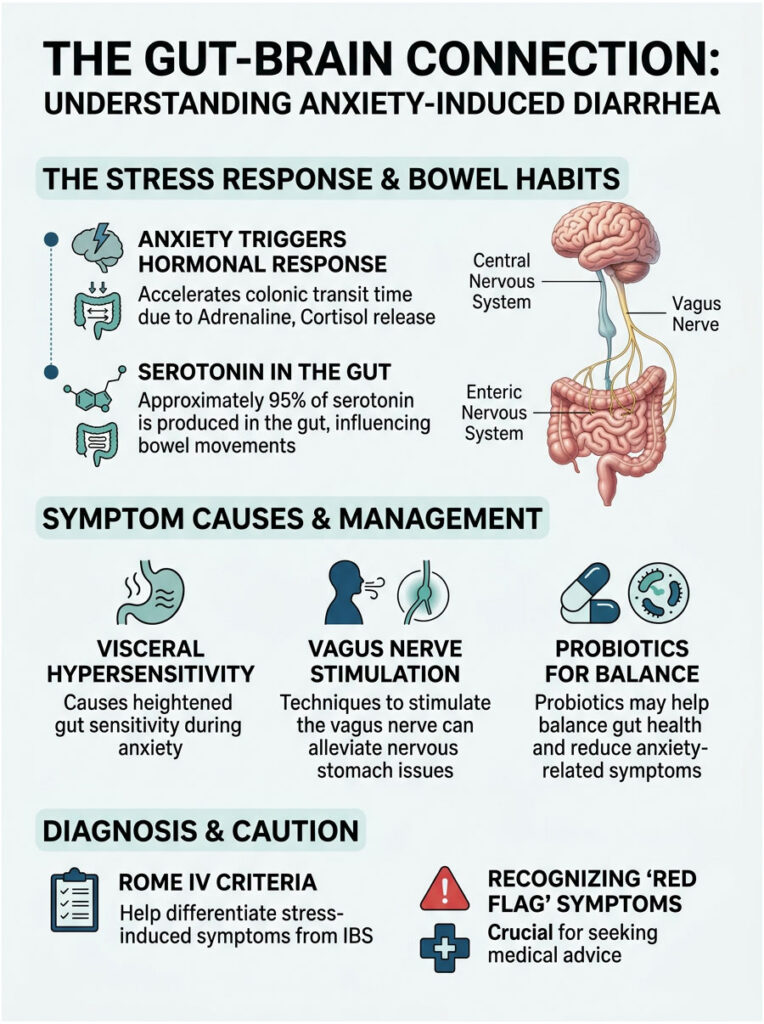
Yes, acute psychological stress activates the body’s fight-or-flight response, which alters digestive motility and leads to loose stools. This happens because the brain and the gut communicate directly through a complex network called the gut-brain axis. When you experience severe stress, your nervous system triggers rapid intestinal contractions, resulting in stress-induced diarrhea.
Key Statistics on Stress and Digestive Health

- According to the American Gastroenterological Association, nearly 42 percent of patients with generalized anxiety experience significant gastrointestinal symptoms.
- Up to 74 percent of patients seeking treatment for chronic digestive issues have co-occurring behavioral health conditions.
- The human gut contains over 100 million independent neurons, more neural tissue than the entire spinal cord.
- Approximately 95 percent of the body’s serotonin is produced directly in the digestive tract.
- Clinical studies show psychological interventions improve digestive symptoms in 50 to 72 percent of treatment-resistant patients.
- Acute stress can accelerate colonic transit time by up to 40 percent within minutes of the triggering event.
Why Anxiety Causes Diarrhea: The Nervous Stomach Explained
Understanding how stress affects digestion goes far beyond simple stomach aches. The human body doesn’t separate mental anguish from physical function. When a patient asks whether anxiety can cause diarrhea, I explain the concept of the gut-brain axis, a bidirectional communication network linking the central nervous system to the gastrointestinal tract.
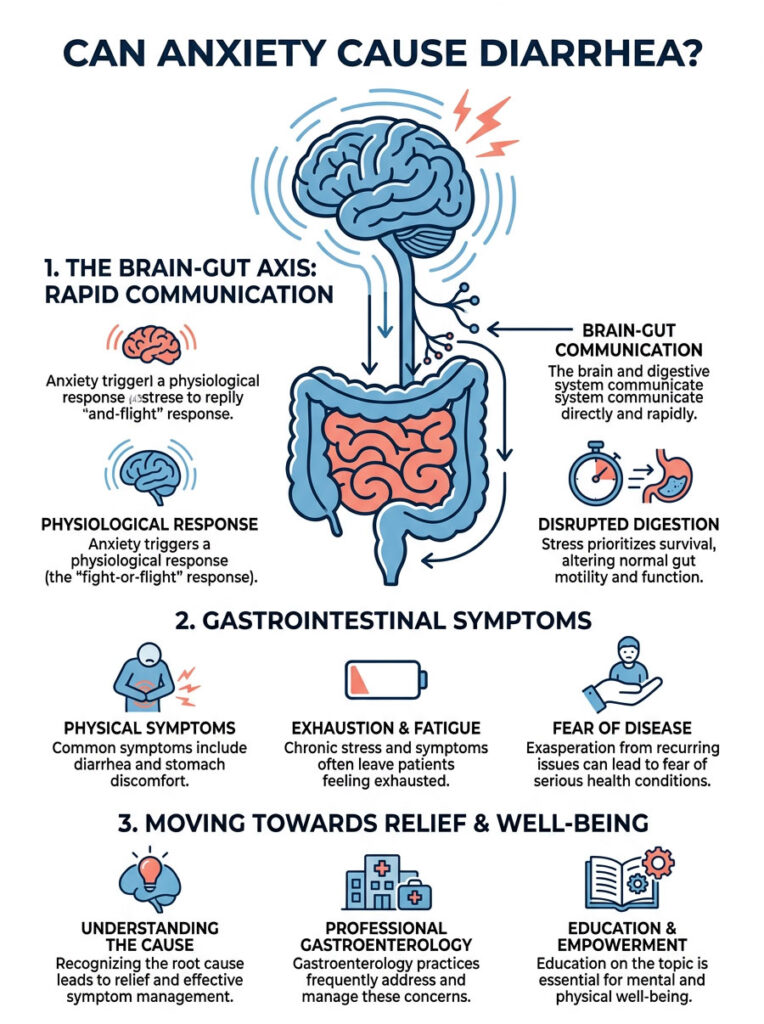
If your brain perceives a threat, it sends chemical signals straight to your abdomen. If your stomach is upset, it sends distress signals back up to your brain. This two-way street is exactly why you feel butterflies before a big presentation.
From an evolutionary perspective, your body reacts to a stressful email the same way it would react to a physical predator. The fight-or-flight response drastically alters digestive motility. Your body decides that digesting breakfast is a waste of energy if survival is at stake, so it attempts to empty your bowels to make you lighter and faster.
The problem is that modern stressors are constant and psychological rather than rare and physical. This leaves our digestive systems stuck in a chronic state of emergency. To fix the issue, we have to retrain the nervous system into feeling safe again.
The Physical Anatomy of the Gut-Brain Axis
To truly understand why anxiety triggers bowel urgency, we need to look at the biological structures that make this connection possible. Your digestive system isn’t just a hollow tube that processes food. It’s a highly sensitive, remarkably intelligent organ system that relies on a massive network of nerves, hormones, and chemical messengers.
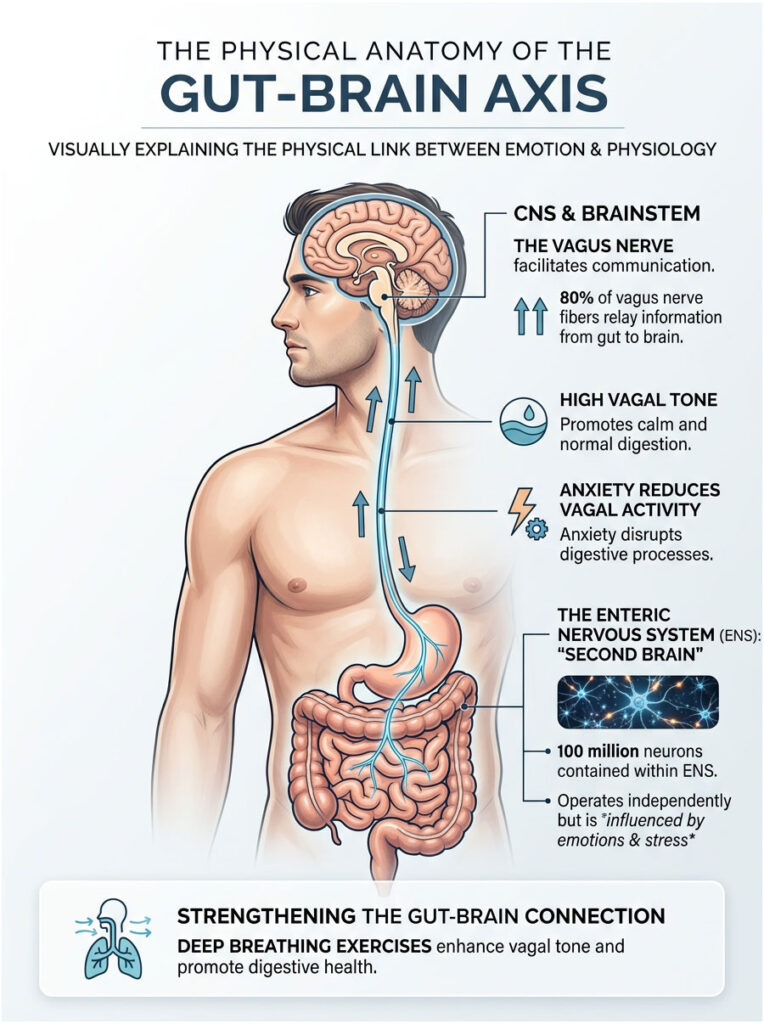
The Enteric Nervous System: Your Second Brain
The enteric nervous system is often called the body’s second brain. It’s an extensive mesh-like network of roughly 100 million neurons lining your gastrointestinal tract from esophagus to rectum. That’s roughly equivalent to the brain of a small dog.
This system can operate independently of the central nervous system. It controls swallowing, enzyme release, blood flow, and the rhythmic contractions that move food through your body. But while it can act alone, it’s heavily influenced by your emotional state.
When you feel panicked, the enteric nervous system receives alarm signals from the brain and responds by speeding everything up, leading directly to stress-induced diarrhea. These two nervous systems develop from the exact same embryonic tissue, which is why they speak the same chemical language using identical neurotransmitters.
The Vagus Nerve: Your Gut-Brain Superhighway
The vagus nerve is the primary cranial nerve connecting the brainstem to the abdomen. Think of it as a massive, high-speed cable running through your core. It’s the longest and most complex cranial nerve in the human body.
About 80 percent of its fibers carry information from the gut up to the brain. The remaining 20 percent travel from the brain down to the gut. The vagus nerve plays a critical role in the parasympathetic “rest and digest” state.
When your vagal tone is high, your body feels safe, digestion proceeds normally, and your heart rate stays steady. When anxiety strikes, vagus nerve activity drops sharply and the sympathetic nervous system takes over, disrupting normal digestion.
Expert Tip: Regular deep breathing exercises physically stimulate the vagus nerve in the chest cavity, sending a calming signal to your enteric nervous system to halt rapid bowel contractions.
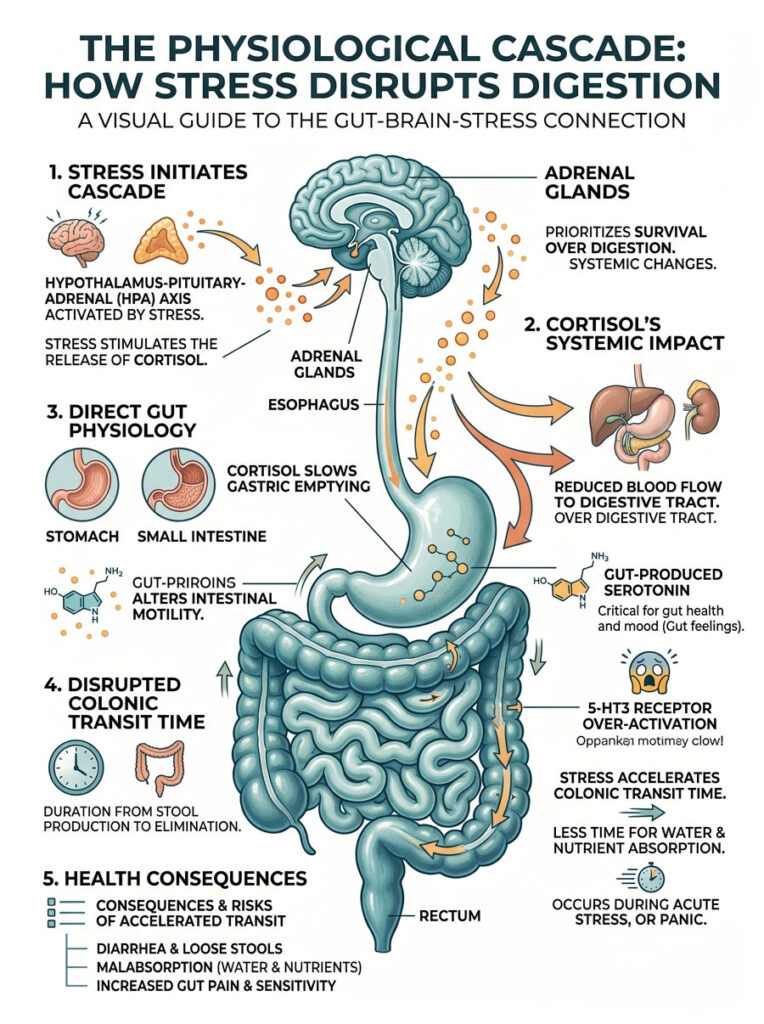
The Physiological Cascade: How Stress Disrupts Digestion
Now let’s look at what actually happens on a microscopic, chemical level when stress hits. Your body initiates a massive physiological cascade involving multiple organ systems and a sudden flood of hormones. Three specific mechanisms work together to prepare your body for immediate action, with gastrointestinal upset as the unavoidable side effect.
The HPA Axis and Cortisol Release
The Hypothalamic-Pituitary-Adrenal (HPA) axis is the central stress response system. When you perceive danger, the hypothalamus releases CRH, which tells the pituitary gland to release ACTH, which prompts the adrenal glands to release cortisol and adrenaline.
Cortisol diverts blood flow away from the stomach and intestines, sending it to skeletal muscles instead. Digestion practically shuts down in the upper stomach (you may feel nauseous or lose your appetite), while the lower intestines are triggered to empty rapidly. Your body is literally dumping cargo to prepare for a fight.
HPA Axis Activation Timeline:
- Seconds 1 to 5: The brain perceives a threat. The amygdala signals the hypothalamus.
- Seconds 5 to 15: Adrenaline enters the bloodstream. Heart rate and blood pressure spike.
- Minutes 1 to 3: The HPA axis fully activates, releasing a surge of cortisol.
- Minutes 3 to 10: Blood diverts from the gut. The enteric nervous system triggers urgent bowel evacuation.
Serotonin and the 5-HT3 Receptors
Most people think of serotonin as a brain chemical tied to mood and happiness. In reality, 95 percent of the body’s serotonin is produced in the gut by specialized enterochromaffin cells. It’s heavily responsible for regulating the speed at which food moves through your system.
During intense fear, the enteric nervous system releases a massive surge of serotonin. This overstimulates 5-HT3 receptors, causing rapid, violent muscle contractions in the bowel walls. This chemical flood is a primary reason for sudden urgency during panic attacks. It’s also why certain antidepressants cause stomach upset when you first start taking them.
Accelerated Colonic Transit Time
Colonic transit time is the speed at which waste moves through your large intestine. Under normal conditions, this process is slow and controlled, giving your body time to absorb water and form solid stools.
The fight-or-flight response accelerates this process dramatically. Because waste moves through so quickly, the body has no time to absorb water, resulting in watery, urgent, painful stress-induced diarrhea. If the stress doesn’t go away, your colonic transit time stays permanently accelerated, leading to chronic malabsorption, dehydration, and fatigue.
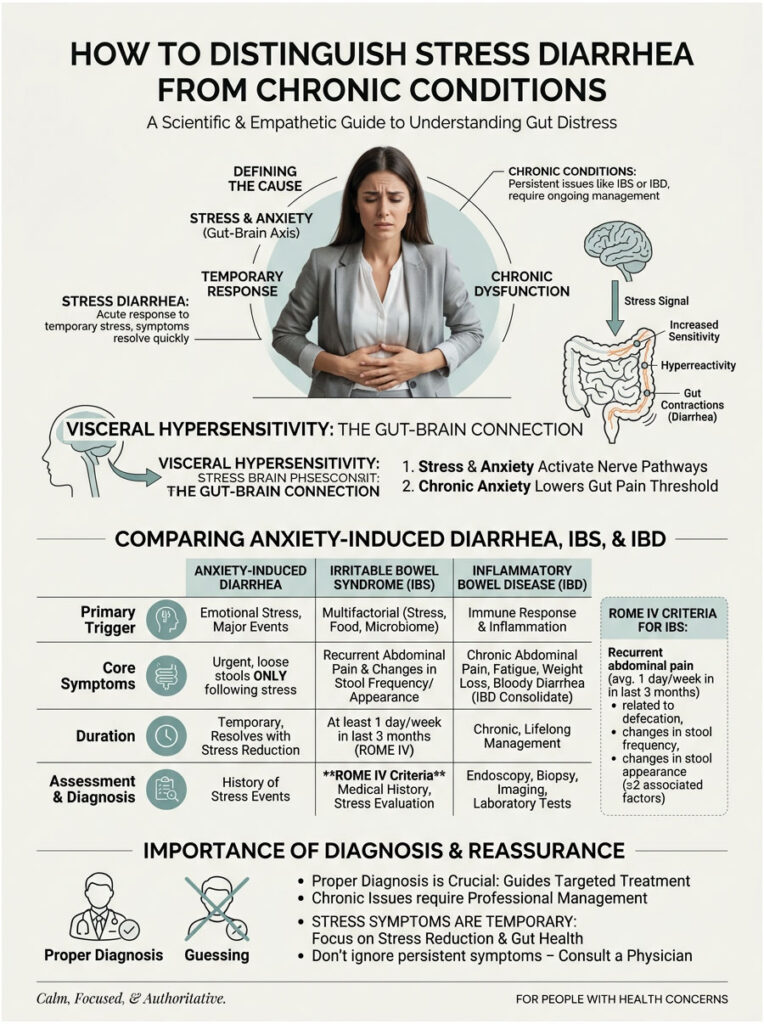
How to Tell Stress Diarrhea Apart from Chronic Conditions
It’s perfectly normal to have an upset stomach before a major event. But it’s vital to understand the difference between a temporary nervous stomach and a diagnosable clinical disorder. While the symptoms feel remarkably similar, the underlying pathology is very different, and proper diagnosis dictates proper treatment.
The Rome IV Criteria for IBS
Gastroenterologists worldwide use the Rome IV criteria to diagnose Irritable Bowel Syndrome. A patient must experience recurrent abdominal pain at least one day a week for the last three months, distinctly associated with two or more factors: pain related to defecation, a change in stool frequency, or a change in stool form.
If you only get loose stools before public speaking, you don’t meet the Rome IV criteria for IBS. This distinction matters for your peace of mind. IBS is a diagnosis of exclusion, meaning we only assign it after ruling out structural problems. We don’t guess based on anxiety levels alone.
Visceral Hypersensitivity
A central feature of chronic functional gut disorders is visceral hypersensitivity, a heightened experience of pain in the internal organs. In a healthy person, digestion and gas pass unnoticed. For someone with visceral hypersensitivity, these normal processes register as painful and alarming.
Chronic anxiety physically lowers the pain threshold in the gut. The continuous firing of the enteric nervous system keeps nerve endings inflamed and reactive, creating a self-perpetuating cycle of discomfort and worry. If your nerves are already frayed from chronic stress, even a small amount of gas will feel like a severe cramp. This requires targeted neuromodulator therapies rather than standard painkillers.
Clinical Comparison: Anxiety Diarrhea vs. IBS vs. IBD
| Feature | Anxiety-Induced Diarrhea | IBS | IBD |
| Primary Trigger | Acute psychological stressors | Food, chronic stress, hormones | Autoimmune response, inflammation |
| Duration | Resolves when stressor ends | Chronic (1+ day/week for 3 months) | Chronic with unpredictable flares |
| Pain | Mild cramping, sudden urgency | Significant, relieved by defecation | Severe, often with joint/systemic pain |
| Stool | Loose, watery, never bloody | Variable (diarrhea/constipation/mixed) | Often bloody, may contain mucus |
| Classification | Psychosomatic response | Functional GI disorder | Structural autoimmune disease |
Real-World Triggers and the Somatization Cycle
In practice, patients don’t complain about their HPA axis. They complain about not being able to leave the house without mapping out every public restroom. Somatization is the clinical process where mental distress manifests as actual physical symptoms, and it’s a powerful physiological event.
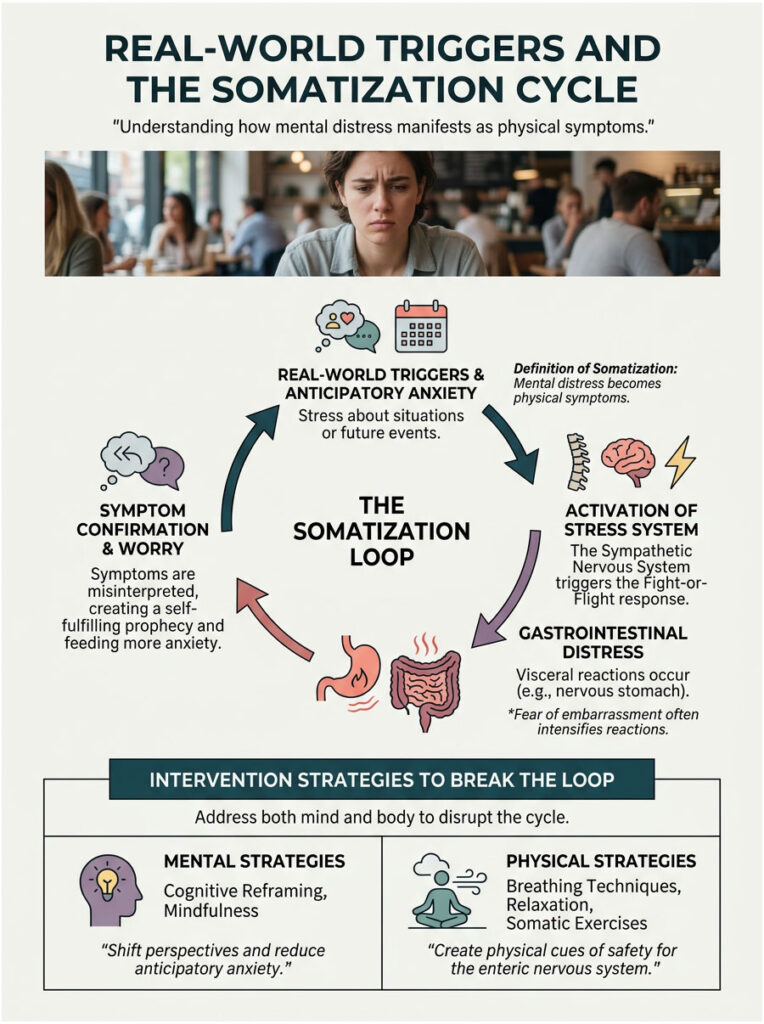
Anticipatory Anxiety and Social Triggers
Anticipatory anxiety, the fear of what might happen in the future, is a massive driver of gastrointestinal distress. When you worry about an upcoming event, your brain keeps the sympathetic nervous system engaged for days, dripping small amounts of adrenaline into your bloodstream and chronically irritating the enteric nervous system.
By the time the event arrives, your colonic transit time has already been altered. Social triggers are especially potent. The fear of embarrassment is processed by the primitive brain as a literal survival threat. Your body prepares you to flee the boardroom the same way it would flee a predator.
Breaking the Somatization Loop
One of the most frustrating aspects of a nervous stomach is the self-fulfilling prophecy it creates. You worry about getting sick, which triggers stress hormones, which directly cause the symptom you’re trying to avoid. Then, because it happened, your fear is validated. Next time your anticipatory anxiety is even higher, and visceral hypersensitivity gets worse.
Breaking this loop requires both mental and physical interventions simultaneously. You have to convince the enteric nervous system that you’re safe. It doesn’t respond to logic. It only responds to physiological cues of safety, which we must purposefully create.
Evidence-Based Clinical Interventions
For patients with severe gut-brain axis dysfunction, simple advice to “relax” is useless. Modern psychogastroenterology offers life-changing tools, and we now treat the brain and the gut simultaneously. These are rigorously tested protocols used in major hospitals.

Cognitive Behavioral Therapy (CBT) for GI Disorders
CBT helps rewire the brain’s response to stress, directly reducing physical gastrointestinal symptoms. During specialized CBT, patients learn to identify catastrophic thinking patterns. Instead of “I will definitely get sick at this dinner,” the thought becomes “I might feel uncomfortable, but I can handle it.”
Peer-reviewed data from the American Psychological Association confirms that a 12-week CBT program can significantly decrease the frequency of stress-induced diarrhea. By lowering mental panic, you lower physical cortisol output, allowing the enteric nervous system to return to its baseline rest-and-digest state.
Gut-Directed Hypnotherapy
This is a legitimate clinical tool developed in the 1980s by Dr. Peter Whorwell in the UK. It induces deep physical relaxation to calm the enteric nervous system using visualization techniques focused on the digestive tract. Research shows it provides long-term relief for up to 72 percent of patients who don’t respond to traditional medications.
Do not confuse clinical gut-directed hypnotherapy with stage hypnosis. This is a rigorous medical protocol conducted in major hospital systems by licensed practitioners specializing in functional gastrointestinal disorders.
Immediate Strategies for Acute Symptom Relief
While therapy provides long-term healing, you need tools you can use right now. When you feel the sudden urge before an event, you need to manually override the stress signals being sent to your enteric nervous system.

Vagus Nerve Stimulation Techniques
Stimulating the vagus nerve is your best defense against a nervous, overactive stomach. The most accessible method is the 4-7-8 breathing technique: breathe in through your nose for 4 seconds, hold for 7 seconds, and exhale slowly through pursed lips for 8 seconds. This physically massages the vagus nerve and forces your heart rate to slow.
Splashing ice-cold water on your face triggers the mammalian dive reflex, instantly calming the gut. Humming or singing loudly also works because the vagus nerve runs through your vocal cords, and the vibration sends a calming signal to your intestines.
Dietary Adjustments for High-Stress Periods
What you eat during stressful times matters enormously. I recommend a temporary low-residue protocol before known stressful events: easily digestible foods like white rice, ripe bananas, and lean poultry. Focus on soluble fiber like oatmeal, which absorbs excess water and adds bulk to loose stools.
Avoid caffeine, artificial sweeteners, and greasy foods when anxious. Caffeine directly stimulates colonic transit time, making everything worse. Alcohol temporarily calms the mind but severely irritates the intestinal lining and disrupts your microbiome, leading to worse anxiety the next day.
The Microbiome Connection: Gut Bacteria and Mental Health
You can’t discuss the gut-brain connection without addressing the trillions of bacteria living inside you. Your microbiome doesn’t just digest food. These organisms actively produce neurotransmitters, including serotonin and dopamine, which directly influence your daily mood.
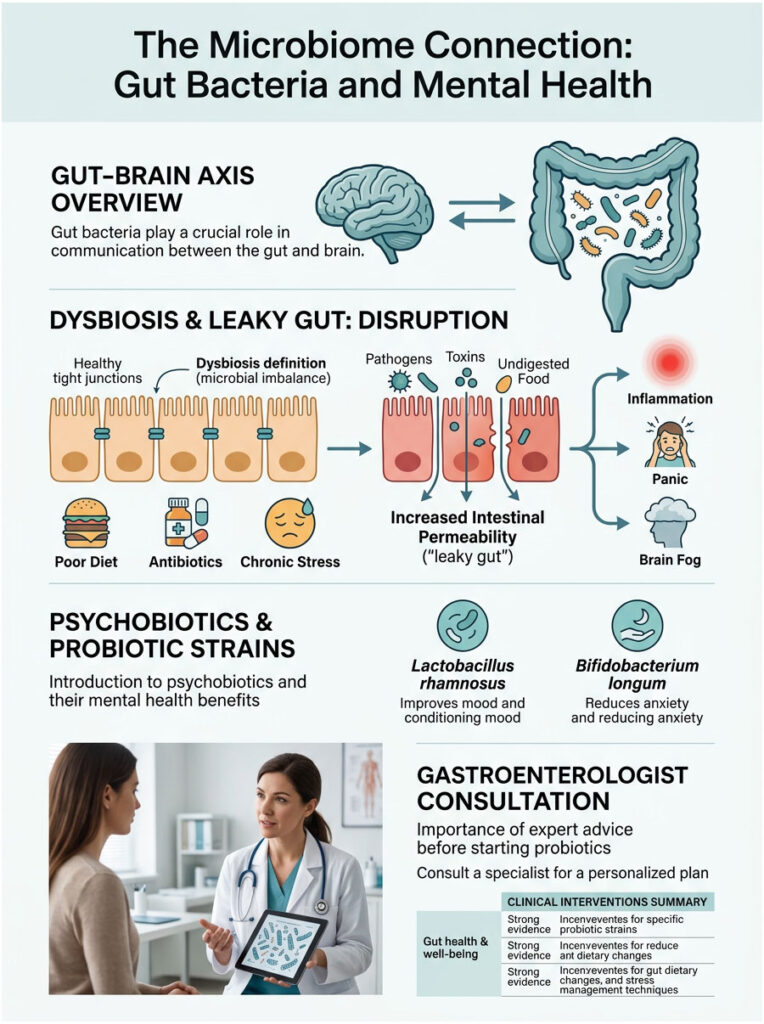
Dysbiosis and Its Impact
Dysbiosis is a state of severe microbial imbalance where harmful bacteria outnumber beneficial ones. It’s commonly caused by poor diet, frequent antibiotics, or chronic stress. When dysbiosis takes hold, the intestinal lining becomes inflamed, sending distress signals up the vagus nerve and physically worsening feelings of panic and brain fog.
An imbalanced microbiome can also increase intestinal permeability (“leaky gut”), allowing microscopic toxins to enter the bloodstream and trigger a systemic immune response that further stresses the central nervous system. Fixing dysbiosis is critical for long-term healing. Feed the good bacteria with prebiotics: garlic, onions, asparagus, and underripe bananas.
Psychobiotics: Targeted Probiotic Strains
Psychobiotics are specific bacterial strains that yield measurable mental health benefits when ingested. Clinical trials show that strains like Lactobacillus rhamnosus and Bifidobacterium longum can actively reduce systemic cortisol levels and blunt HPA axis activation during stressful events.
By balancing gut flora with targeted strains, you can potentially lower the frequency of stress-induced diarrhea. Always consult a gastroenterologist before starting high-dose probiotics. The wrong strain can cause temporary bloating, and you need a targeted approach based on your specific symptoms.
Clinical Interventions Reference Table
| Category | Modality | Mechanism | Evidence Level |
| Psychological | Gut-Directed Hypnotherapy | Modulates central pain processing, slows gut motility | High (Rome Foundation) |
| Psychological | CBT | Reduces somatization, catastrophic thinking | High (strong empirical backing) |
| Physiological | Diaphragmatic Breathing | Stimulates vagus nerve, activates parasympathetic state | Moderate-High (acute relief) |
| Dietary | Low-FODMAP Diet | Reduces osmotic load, rapid gas production | High (best for co-occurring IBS) |
| Microbiome | Targeted Psychobiotics | Balances gut flora, may lower systemic inflammation | Moderate (strain-dependent) |
Medical Treatments and Pharmacological Support
Sometimes breathing exercises and probiotics aren’t enough. When symptoms severely impact your ability to work or socialize, medication becomes a legitimate option. There’s no shame in using medical tools to regain quality of life.

Antispasmodic Medications
Antispasmodics like dicyclomine or hyoscyamine work directly on the smooth muscle of the intestinal wall, preventing the violent spasms behind stress-induced diarrhea. They can be taken situationally before a stressful event. Over-the-counter loperamide (Imodium) is also effective for slowing colonic transit time as an emergency brake.
Neuromodulators and SSRIs
For chronic, debilitating symptoms, gastroenterologists often prescribe low-dose antidepressants for their gut effects, not for treating clinical depression. Tricyclic antidepressants slow colonic transit time and reduce visceral hypersensitivity. SSRIs stabilize the erratic serotonin signaling that occurs during panic attacks. Finding the right medication and dosage takes patience and consistent communication with your doctor.
Natural Supplements
Enteric-coated peppermint oil is one of the most studied natural antispasmodics. The menthol acts as a calcium channel blocker, gently relaxing intestinal smooth muscle. L-glutamine fuels the cells lining your intestinal wall and may help repair increased permeability. Magnesium glycinate helps lower cortisol and promotes restorative sleep, which directly translates to calmer digestion the next day.
Lifestyle Modifications to Build Gut-Brain Resilience
Medical treatments need to be supported by a solid foundation. Your daily habits set the baseline stress level of your nervous system. You can’t out-medicate a lifestyle that constantly keeps your body in fight-or-flight mode.

Sleep and Digestive Health
During deep sleep, your body performs critical maintenance on the digestive tract, repairing tissue and flushing inflammatory markers. Poor sleep spikes your cortisol awakening response, which immediately triggers the enteric nervous system and leads to morning urgency.
Prioritize strict sleep hygiene: keep the bedroom cold and dark, avoid screens for an hour before bed. Melatonin isn’t just a sleep hormone. It also regulates gut motility, signaling the bowels to slow down at night. Protecting melatonin production is essential for stopping early morning symptoms.
Exercise: Finding the Right Balance
Gentle, steady-state cardio like walking or swimming promotes healthy blood flow to the intestines and naturally lowers cortisol. Yoga is particularly effective because it combines movement with diaphragmatic breathing.
However, high-intensity interval training or heavy weightlifting can activate the same fight-or-flight response that causes stress-induced diarrhea. During periods of high anxiety, scale back to restorative movements that signal safety to your nervous system.
When to See a Gastroenterologist: Red Flag Symptoms
While the mind heavily influences the body, you should never assume every digestive issue is just nerves. If your symptoms are changing rapidly or you don’t meet the Rome IV criteria for IBS, get a professional evaluation immediately.

- Unexplained weight loss: A major sign of severe malabsorption or systemic disease.
- Nocturnal diarrhea: Stress diarrhea rarely wakes you from deep sleep. Nighttime episodes require urgent investigation.
- Blood in the stool: Whether bright red or dark black, blood is never a normal response to anxiety.
- Family history of colon cancer, celiac disease, or inflammatory bowel disease warrants early screening.
- Persistent fever or anemia indicates systemic inflammation or hidden bleeding, not just an overactive gut.
A doctor can run comprehensive stool tests, check inflammatory markers like fecal calprotectin, or perform a colonoscopy to rule out organic disease. Once you have a clean bill of health, you can confidently focus on the psychological aspects of your symptoms.
Final Takeaways
The relationship between your brain and your digestive system is profound, intricate, and deeply physical. You’re not imagining your symptoms, and you’re not broken. Your body is simply overreacting to modern stressors using ancient survival mechanisms.
- The physical response to mental distress is real, driven by the evolutionary fight-or-flight response.
- The gut-brain connection operates via the vagus nerve and enteric nervous system, communicating in milliseconds.
- Stress hormones like cortisol and serotonin accelerate colonic transit time, preventing water absorption and causing loose stools.
- You can differentiate a nervous stomach from clinical IBS using symptom duration and the Rome IV criteria.
- Vagus nerve stimulation techniques like diaphragmatic breathing offer immediate acute relief.
- Long-term management often requires CBT or gut-directed hypnotherapy to reduce visceral hypersensitivity.
- Never ignore red flag symptoms like bleeding or unexplained weight loss. Always consult a medical professional.
By understanding the biology, you can confidently answer the question: can anxiety cause diarrhea? More importantly, you now have the knowledge and strategies to protect both your mental and digestive health going forward.
Frequently Asked Questions
How exactly does anxiety trigger immediate diarrhea?
When you experience acute anxiety, your brain activates the fight-or-flight response, which releases a surge of adrenaline and cortisol. This hormonal cascade diverts blood flow away from the digestive tract and signals the enteric nervous system to rapidly accelerate colonic transit time. Your body attempts to ‘dump cargo’ to prepare for a perceived physical threat, resulting in loose, watery stools and sudden urgency.
What is the gut-brain axis and why does it affect my digestion?
The gut-brain axis is a complex, bidirectional communication network linking your central nervous system to your enteric nervous system. They are physically connected by the vagus nerve and share the same neurotransmitters, such as serotonin. Because of this high-speed connection, psychological distress in the brain is instantly translated into physiological changes in the gut, and vice versa.
Why is serotonin mentioned in relation to anxiety-induced diarrhea?
While often thought of as a brain chemical, approximately 95 percent of your body’s serotonin is produced in the gut. During periods of high stress, the enteric nervous system can release a sudden surge of serotonin. This excess chemical overstimulates 5-HT3 receptors in the intestinal lining, causing violent muscle contractions and rapid bowel evacuation, which is a hallmark of stress-induced gastrointestinal distress.
What are the Rome IV criteria for differentiating stress from IBS?
The Rome IV criteria are clinical guidelines used to diagnose Irritable Bowel Syndrome (IBS). To meet these criteria, a patient must have recurrent abdominal pain at least one day per week for the last three months, associated with two or more of the following: pain related to defecation, a change in stool frequency, or a change in stool form. If your diarrhea only occurs during isolated stressful events, it is likely a psychosomatic response rather than chronic IBS.
How can I stimulate my vagus nerve to stop a nervous stomach?
You can manually override an overactive enteric nervous system by stimulating the vagus nerve. The most effective method is deep diaphragmatic breathing, specifically the 4-7-8 technique (inhale for 4 seconds, hold for 7, exhale for 8). This sends a mechanical signal to the brain to activate the ‘rest and digest’ parasympathetic state, which slows down intestinal contractions and reduces urgency.
What is visceral hypersensitivity and how does anxiety worsen it?
Visceral hypersensitivity is a condition where the nerves in your gut become abnormally sensitive to normal biological processes like gas or digestion. Chronic anxiety keeps your nervous system in a state of high alert, which physically lowers your pain threshold. This creates a cycle where even minor intestinal activity is perceived by the brain as severe cramping or a medical emergency.
Can certain probiotics actually help with anxiety-related gut issues?
Yes, a specialized field called psychobiotics focuses on using specific bacterial strains to improve mental and digestive health. Strains like Lactobacillus rhamnosus and Bifidobacterium longum have been shown in clinical trials to lower systemic cortisol levels and blunt the body’s stress response. By balancing the microbiome, you can reduce the frequency of stress-induced diarrhea from the inside out.
What is gut-directed hypnotherapy and does it really work?
Gut-directed hypnotherapy is an evidence-based clinical protocol that uses deep relaxation and visualization to calm the enteric nervous system. Unlike stage hypnosis, this is a medical treatment that helps patients retrain their gut-brain communication. Clinical research indicates it provides long-term relief for up to 72 percent of patients with functional gut disorders by reducing visceral hypersensitivity.
Which foods should I avoid when I am feeling highly anxious?
During high-stress periods, you should avoid ‘gastric irritants’ that accelerate motility. This includes caffeine, which directly stimulates colonic contractions, as well as alcohol, artificial sweeteners, and greasy foods. Instead, opt for a low-residue diet consisting of easily digestible foods like white rice, bananas, and lean proteins to minimize the workload on your sensitive digestive tract.
How do neuromodulators and SSRIs help treat chronic diarrhea?
In clinical practice, low-dose neuromodulators (like tricyclic antidepressants) are used to slow down colonic transit time and raise the pain threshold in the gut. Selective Serotonin Reuptake Inhibitors (SSRIs) can also help stabilize the erratic serotonin signaling between the brain and the enteric nervous system. These medications treat the underlying communication breakdown in the gut-brain axis rather than just the physical symptoms.
What is the ‘somatization loop’ in gastrointestinal health?
The somatization loop is a self-perpetuating cycle where the fear of having diarrhea in public triggers the very stress hormones that cause it. You worry about a bathroom emergency, your brain releases adrenaline, your bowels react, and the resulting symptom validates your original fear. Breaking this loop requires a combination of cognitive behavioral therapy (CBT) and physiological interventions to convince the body it is safe.
When should I stop blaming anxiety and see a doctor for diarrhea?
You should consult a gastroenterologist immediately if you experience ‘red flag’ symptoms that suggest organic disease rather than functional stress. These include nocturnal diarrhea (waking up from sleep to use the bathroom), blood in the stool, unexplained weight loss, persistent fever, or a family history of inflammatory bowel disease (IBD) or celiac disease. These signs require clinical investigation to rule out structural issues.
Disclaimer
This article is for informational purposes only and does not constitute medical advice. The biological connection between anxiety and gastrointestinal symptoms is complex; therefore, you should always consult a board-certified gastroenterologist or a qualified healthcare professional before starting new treatments or if you experience “red flag” symptoms like bleeding or unexplained weight loss.
References
- American Gastroenterological Association – https://gastro.org – Provided statistics on the prevalence of GI symptoms in patients with generalized anxiety.
- The Rome Foundation – Rome IV Diagnostic Criteria – Detailed the clinical standards for diagnosing Irritable Bowel Syndrome and functional gut disorders.
- American Psychological Association – https://www.apa.org – Provided data on the efficacy of Cognitive Behavioral Therapy (CBT) for managing physical health conditions.
- Journal of Clinical Investigation – Dr. Peter Whorwell’s Research – Supported the findings and success rates of gut-directed hypnotherapy in clinical settings.
- Harvard Health Publishing – The Gut-Brain Connection – Expert insights into the enteric nervous system and the role of the vagus nerve in digestive motility.
- Nature Reviews Gastroenterology & Hepatology – Microbiome and Mental Health – Supporting data for the role of psychobiotics and gut flora in stress regulation.