One of the most common questions patients ask during a visit to the gastroenterologist is simple: is diarrhea contagious in adults and children? The short answer is yes, when an infectious agent is behind it. Acute diarrhea is rarely just a passing inconvenience. In many cases, it is a highly transmissible condition driven by viruses, bacteria, or parasites that spread with surprising efficiency.
Table of Contents
When loose stools suddenly hit your household, your focus needs to shift quickly from personal discomfort to preventing the illness from spreading. These microscopic invaders move fast, especially through homes, schools, and workplaces. They thrive on gaps in everyday hygiene habits that most of us never think twice about.

This guide breaks down the exact mechanics of how infectious diarrhea spreads, the specific causes behind viral, bacterial, and parasitic infections, and evidence-based prevention strategies to protect your family, your coworkers, and your community.
Quick Answer: Yes, infectious diarrhea is highly contagious. It spreads mainly through the fecal-oral route when a healthy person accidentally swallows viral or bacterial particles. You remain contagious for at least 48 hours after your last symptom. Strict handwashing and isolation are essential to stop the spread.
Key Statistics on Gastrointestinal Infections
- Norovirus Impact: According to the CDC (2023), norovirus causes 19 to 21 million cases of acute gastroenteritis each year in the United States alone.
- Pediatric Risk: The World Health Organization reports that infectious diarrhea accounts for 9% of all deaths among children under age 5 globally.
- Surface Survival: Some non-enveloped viruses can survive on hard surfaces for up to 28 days without proper bleach disinfection.
- Hospital Spread: C. diff transmission in healthcare settings affects nearly 500,000 patients in U.S. facilities each year.
- Hydration Success: Early use of Oral Rehydration Therapy (ORT) reduces hospital admissions for severe dehydration by over 33%.
- Secondary Attack Rates: When one household member contracts norovirus, there is roughly a 30% chance another family member will catch it within 48 hours.
Understanding Whether Diarrhea Is Contagious
To prevent and treat diarrhea effectively, you first need to figure out what is causing the symptoms. Not every case of loose stools puts the people around you at risk. The key is separating infectious causes from chronic, non-transmissible conditions.
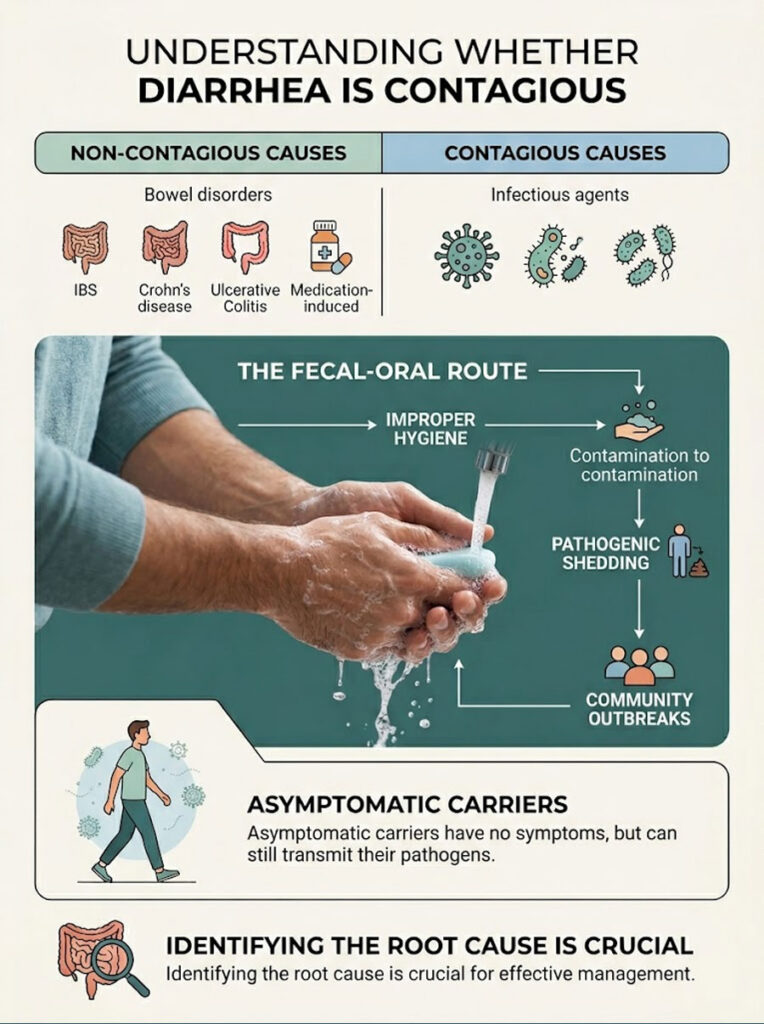
In clinical practice, many patients panic over symptoms that are not contagious at all. On the other hand, some families fail to isolate a highly infectious child, and the result is household-wide misery. Identifying the root cause is always the first step in managing any potential outbreak.
Non-Contagious Bowel Disorders You Should Know About
Many people mistake flare-ups of chronic conditions for contagious illness. Disorders like Irritable Bowel Syndrome (IBS), Crohn’s disease, and Ulcerative Colitis are immune or functional conditions. They do not involve any transmissible pathogens.
You absolutely cannot catch IBS from a family member or coworker. Similarly, food intolerances such as lactose intolerance or celiac disease trigger digestive symptoms after eating specific foods, but these are internal reactions based on your own genetics and enzyme levels.
Medication-induced diarrhea is another extremely common non-contagious cause. Antibiotics frequently disrupt natural gut flora and cause loose stools that cannot be passed to another person. If symptoms appear right after starting a new medication, the cause is almost certainly chemical, not infectious.
How the Fecal-Oral Route Works
Infectious diarrhea spreads almost entirely through what doctors call the fecal-oral route. It happens when microscopic particles of infected stool or vomit are accidentally swallowed by a healthy person. This transfer commonly occurs through contaminated hands, shared utensils, and compromised water supplies.
It takes only a tiny amount of an infectious agent to make someone seriously ill. When an infected person uses the bathroom without washing their hands properly, they leave particles on door handles, light switches, and kitchen surfaces. The next person touches that surface, then touches their mouth or food, and the cycle continues.
Pathogenic Shedding and Asymptomatic Carriers
A major driver of community outbreaks is pathogenic shedding. Infected individuals begin excreting viral or bacterial loads in their stool before symptoms even appear. More importantly, shedding continues long after physical symptoms have fully resolved.
This invisible phase is exactly why outbreaks spread so quickly in schools and offices. People feel better, return to normal activities too soon, and unknowingly leave infectious particles on shared surfaces. Shedding can last for days or even weeks depending on the organism.
Asymptomatic carriers add another layer of complexity. Some people harbor and shed enteric pathogens without ever feeling sick themselves. Their immune system suppresses the symptoms, but their stool remains highly infectious to vulnerable individuals nearby.
Viral Gastroenteritis: The Leading Cause of Contagious Outbreaks
Viruses are responsible for the vast majority of acute infectious diarrhea cases worldwide. When concerned parents call a clinic about contagion risks, they are usually dealing with a viral infection. These viruses are incredibly resilient and need only tiny doses to establish infection.
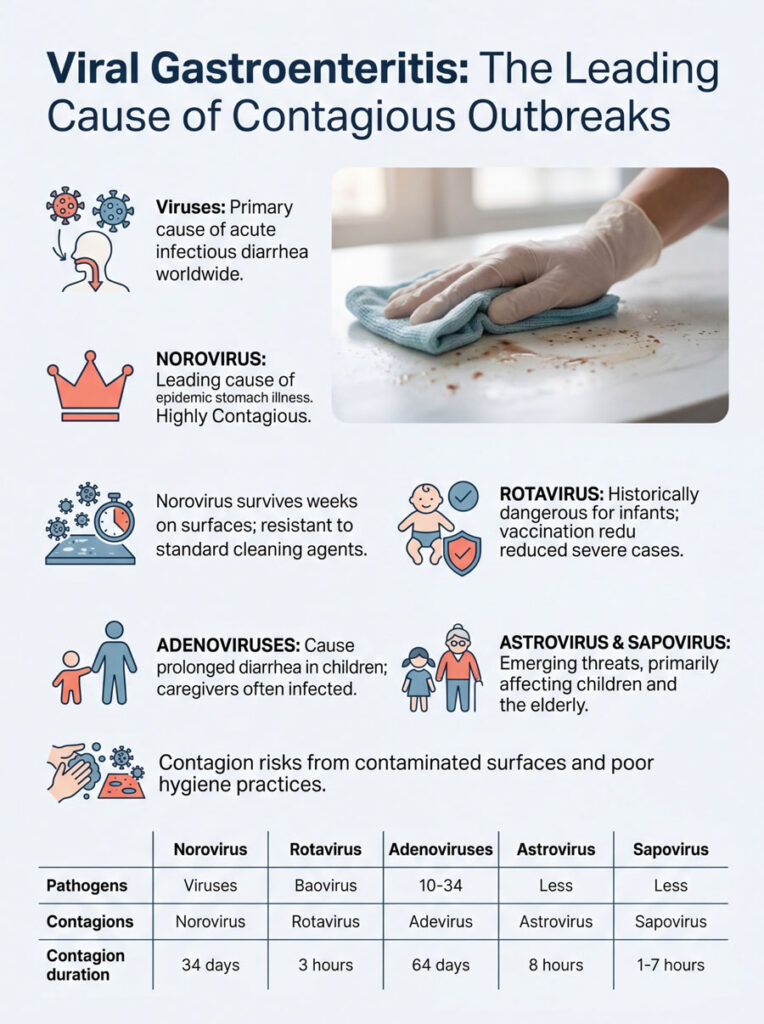
Unlike bacteria, viruses cannot multiply in food or water. They require a living human host to replicate. Once inside your digestive tract, they hijack your cellular machinery to create millions of copies of themselves, damaging the intestinal lining and preventing your body from absorbing water and nutrients. The result is the sudden, watery diarrhea that defines a classic stomach bug.
Norovirus: The Most Resilient Stomach Bug
Norovirus is the single leading cause of epidemic stomach illness across the globe. It is notorious for sweeping through cruise ships, schools, and military barracks. Because it lacks the fragile outer lipid membrane found in many other viruses, standard cleaning agents struggle to destroy it.
This biological armor makes norovirus exceptionally tough to kill in a home environment. It can survive on hard surfaces for weeks, withstand extreme temperatures (including freezing and heating up to 140 degrees Fahrenheit), and shrug off standard alcohol-based sanitizers. If one person brings norovirus home, the chances of the rest of the family catching it are remarkably high.
Rotavirus and Adenovirus in Children
Historically, rotavirus was the most dangerous gastrointestinal pathogen for young infants. It caused severe, rapid dehydration that frequently required emergency hospitalization. Thanks to widespread immunization programs, severe rotavirus cases have dropped significantly.
However, rotavirus remains highly contagious for unvaccinated children and immunocompromised adults. Enteric adenoviruses also cause prolonged loose stools in toddlers, often lasting more than a week. The viral load in a sick child’s diaper is extremely high, making safe diaper-changing practices essential. Caregivers are almost always the secondary targets in pediatric outbreaks.
Astrovirus and Sapovirus: Emerging Threats
While norovirus and rotavirus get the most attention, astrovirus and sapovirus are emerging as significant threats. These viruses primarily target young children and the elderly. Symptoms tend to be milder than norovirus, but the contagion risk remains very high.
Sapovirus outbreaks frequently occur in daycare centers during the colder months. Transmission dynamics mirror norovirus, relying heavily on contaminated surfaces and poor handwashing. Diagnostic testing for these viruses is rarely performed outside of serious hospital cases, so most doctors simply diagnose generic viral gastroenteritis. Regardless of the specific strain, the isolation and cleaning protocols stay the same.
Viral Pathogen Comparison
| Viral Pathogen | Primary Target | Incubation Period | Contagious Duration | Vaccine Available |
| Norovirus | All ages | 12 to 48 hours | Up to 2 weeks post-recovery | None currently approved |
| Rotavirus | Infants and toddlers | 48 hours | 10 to 21 days | Yes (highly effective) |
| Adenovirus | Children under 5 | 3 to 10 days | Up to 14 days | Military use only |
| Astrovirus | Elderly and young children | 3 to 4 days | Several days to weeks | None available |
Bacterial and Parasitic Infections: Beyond the Typical Stomach Bug
While viruses cause most community outbreaks, bacterial and parasitic infections present unique challenges. They often require targeted medical treatment rather than simple supportive care at home. These pathogens commonly enter the body through contaminated food or untreated water.

Stomach Flu vs. Food Poisoning: Key Differences
The difference between stomach flu and food poisoning matters greatly for treatment and household safety. Food poisoning typically occurs after eating pre-formed bacterial toxins in improperly stored food, and symptoms can hit within a single hour.
Here is the critical distinction: toxin-mediated food poisoning is generally not contagious from person to person. You cannot pass a Staphylococcus aureus toxin to your spouse by sharing a bathroom. However, true bacterial infections like Salmonella or Shigella actively multiply within the host and can spread through the fecal-oral route. Knowing the source of your illness determines which safety protocols your household needs.
Clostridioides difficile (C. diff): A Severe Hospital-Acquired Threat
C. diff is a severe bacterial infection that demands immediate medical attention. It most often develops in healthcare settings after a heavy course of broad-spectrum antibiotics. The antibiotics wipe out beneficial gut bacteria, allowing C. diff to multiply unchecked.
This aggressive bacterium produces highly resilient spores that cause life-threatening colon inflammation. C. diff spores can survive on hospital surfaces for months and require specialized bleach protocols to destroy. If a family member is discharged with C. diff, ask the doctor exactly how to clean your home safely.
Parasitic Infections from Recreational Water
Parasites like Giardia and Cryptosporidium are notorious for causing water-borne outbreaks during summer. They are often picked up during camping trips or from swallowing contaminated pool water. Their tough outer shells make standard chlorine treatments completely ineffective.
Parasitic infections cause prolonged, watery, foul-smelling loose stools lasting for weeks. Unlike viral gastroenteritis, they usually require specific prescription antiparasitic medications. You can easily pass these parasites to family members through poor bathroom hygiene. Strict handwashing is your primary defense.
Salmonella and E. Coli Transmission
Bacterial infections like Salmonella and E. coli are frequently linked to undercooked meat and unwashed produce. Once a person is infected, they become a transmission vector. These bacteria replicate rapidly in the intestines and are shed in massive numbers through feces.
E. coli O157:H7 is a particularly dangerous strain that can cause severe kidney failure, especially in young children. If a child in your home is diagnosed with E. coli, the entire household must adopt clinical-grade hygiene immediately. Sharing towels or sleeping in the same bed is not safe during the infectious phase.
Bacterial and Parasitic Pathogen Comparison
| Pathogen Type | Primary Organisms | Common Source | Person-to-Person Risk | Treatment |
| Bacterial Infection | Salmonella, E. coli, Shigella | Undercooked food, raw dairy | High (fecal-oral route) | Antibiotics in severe cases |
| Bacterial Toxin | Staph aureus, Bacillus cereus | Improperly stored prepared foods | None (not contagious) | Supportive care only |
| Parasitic | Giardia, Cryptosporidium | Untreated water, pool water | Moderate (requires poor hygiene) | Prescription antiparasitics |
| Hospital Acquired | C. difficile | Post-antibiotic exposure | Very high (spore transmission) | Specialized antibiotics |
The Critical 48-Hour Rule and Secondary Attack Rates
Determining when it is safe to resume normal activities is the cornerstone of outbreak prevention. Returning to work, school, or social life too early guarantees the illness will spread to vulnerable people.

Many patients feel fine 24 hours after their last bout of vomiting. They assume their body has cleared the threat. This is a dangerous misconception that fuels community-wide epidemics every winter.
When to Return to Work and School
Medical guidelines strictly recommend the 48-hour rule. You must stay home until a full 48 hours have passed without any episode of vomiting, loose stools, or use of fever-reducing medications.
Returning prematurely fuels the secondary attack rate in your community. That rate measures the probability of infection among people who have close contact with a sick individual. Going to the office 24 hours after symptoms stop means your pathogenic shedding is still extremely high. You will inevitably contaminate shared surfaces, spiking infection risk for your colleagues.
How to Manage Household Spread
When one family member falls ill, the entire household is at serious risk. The secondary attack rate within a shared living space is naturally very high.
- Designate a single bathroom exclusively for the sick person if possible.
- If sharing a bathroom, disinfect it with bleach after every single use.
- Do not share towels, drinking glasses, utensils, or blankets.
- Caregivers should wear disposable gloves when handling soiled laundry or cleaning.
- After the patient reaches the 48-hour mark, do a thorough final cleaning of the isolation area.
The Psychology of Compliance
Human psychology plays a big role in why stomach bugs spread so rapidly. People feel a strong drive to return to productivity, ignoring their residual infectiousness. Parents face pressure from employers to return to work, which leads to sending recovering children back to daycare too soon.
We need to shift our cultural mindset. Staying home during illness is a protective community service, not a sign of weakness. And while everyone believes they wash their hands perfectly, clinical evidence says otherwise. Acknowledging our hygiene blind spots is the first step toward better infection control.
Expert Tip: Do not prepare food for anyone in your household while you are symptomatic. Wait at least 48 hours after full recovery before cooking again. An infected food handler is the leading cause of secondary household viral outbreaks.
Advanced Strategies to Break the Chain of Transmission
Standard household cleaning is not enough against aggressive enteric pathogens. Wiping a counter with a damp soapy cloth does nothing to stop norovirus. Proper eradication requires clinical-grade disinfection and a solid understanding of how these pathogens survive.

Why Hand Sanitizer Fails Against Stomach Bugs
A widespread misconception is that alcohol-based hand sanitizers kill all stomach bugs. This is medically incorrect. Because norovirus and rotavirus are non-enveloped viruses, alcohol simply cannot penetrate their tough protein capsids.
Using sanitizer on these viruses essentially moves live particles around on your skin. Vigorous handwashing with soap and warm water for at least 20 seconds is the only proven method. The soap lifts the oils trapping the virus, and running water washes the particles away. If you are caring for someone with viral gastroenteritis, wash your hands constantly, especially before eating and after touching any shared surface.
Bleach Disinfection Protocols
Household antibacterial wipes are generally ineffective against gastroenteritis viruses and bacterial spores. True disinfection requires a freshly mixed bleach solution.
The CDC recommends 5 to 25 tablespoons of standard household bleach per gallon of water. Apply this solution to high-touch surfaces like toilets, sinks, and doorknobs. Let it sit visibly wet for at least five full minutes before wiping clean with disposable paper towels. Discard the towels immediately in a sealed trash bag.
Safe Laundry Practices for Contaminated Linens
Never hug soiled laundry to your chest when carrying it to the washing machine. Shaking contaminated items can aerosolize viral particles, sending them into the air and onto clean surfaces.
Carry soiled items in a disposable plastic bag straight to the machine. Wash immediately using the longest cycle with hot water and bleach-based detergent if the fabric allows. Follow with high-heat drying. Always wash your hands after loading the machine, as the dials and surfaces can become contaminated during the transfer.
Kitchen Safety During an Outbreak
The kitchen is the most dangerous room in the house during a gastrointestinal outbreak. If an infected person touches food, that meal becomes a transmission vehicle instantly.
The sick individual must be completely banned from the kitchen. Even grabbing a glass of water from the fridge can contaminate the handle. Healthy caregivers must handle all meal preparation. Wash all produce under running water, and stick to hot, thoroughly cooked meals during the peak of the outbreak.
Managing Symptoms and Recognizing Danger Signs
While most healthy adults clear enteric pathogens within a few days, the resulting fluid loss is dangerous. Dehydration can cause severe, even fatal, complications if not managed properly from the start.
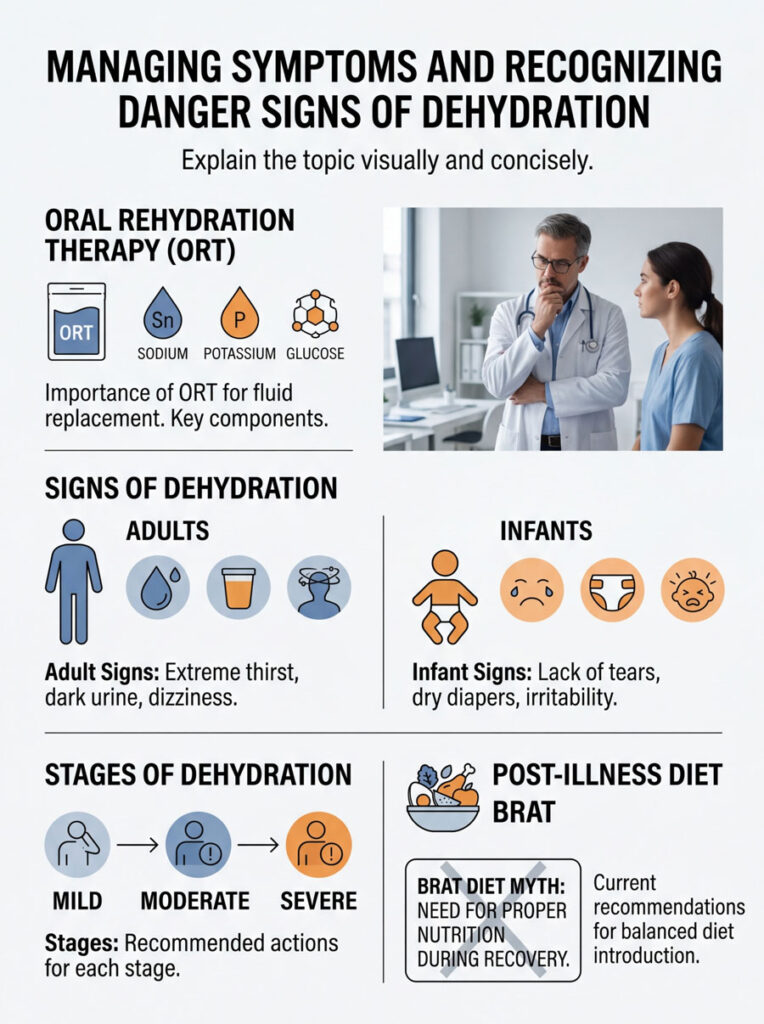
Oral Rehydration Therapy (ORT) and Preventing Severe Fluid Loss
The primary clinical goal during a bout of infectious diarrhea is preventing hypovolemia, a dangerous drop in blood volume caused by massive fluid loss. When blood volume drops significantly, organs do not get enough oxygen, which can lead to shock.
Oral Rehydration Therapy (ORT) is the gold standard for fluid replacement. Plain water alone is not enough because it lacks the vital electrolytes your body is losing. Sugary sports drinks are also inadequate because excess sugar can pull more water into the gut, worsening diarrhea.
ORT solutions contain precise ratios of sodium, potassium, and glucose. This specific ratio triggers the sodium-glucose cotransporter in the intestinal wall, facilitating rapid water absorption far more effectively than plain water.
Tracking Dehydration in Adults vs. Infants
Caregivers must actively monitor for signs of dehydration around the clock. Infants, toddlers, and the elderly can deteriorate in a matter of hours.
Adults typically show clear warning signs: extreme thirst, dark urine, and dizziness when standing. Infants, however, cannot communicate these symptoms. Parents should watch for a lack of tears when crying, dry diapers for over three hours, and unusual irritability.
If you observe signs of severe dehydration, do not wait. Hypovolemia at an advanced stage requires intravenous fluids in a hospital setting. This is especially critical for infants and toddlers who can deteriorate rapidly.
Dehydration Stages and Recommended Actions
| Stage | Signs in Adults | Signs in Infants/Toddlers | Recommended Action |
| Mild | Increased thirst, dry mouth, slight headache | Slightly dry lips, normal urine | Begin ORT at home immediately |
| Moderate | Dark urine, dizziness, severe fatigue | Fewer wet diapers, no tears, irritability | Increase ORT. Consult a doctor. |
| Severe | Confusion, rapid heart rate, fainting, no urine | Sunken fontanelle, sunken eyes, lethargy | Medical Emergency. Seek ER care for IV fluids. |
The BRAT Diet Myth and Modern Recovery Nutrition
For decades, doctors recommended the BRAT diet (Bananas, Rice, Applesauce, Toast) during recovery. The idea was that bland foods would bind the stool and rest the gut. However, modern gastroenterology has largely moved away from this approach.
The BRAT diet is low in protein, fat, and nutrients needed for cellular repair. While these foods are fine for the first 24 hours, sticking with them too long actually delays healing. Your gut needs proper nutrition to rebuild its damaged lining. Current guidance recommends returning to a balanced diet as soon as your stomach can handle it. Avoid greasy or heavily spiced foods initially, but introduce lean proteins and complex carbohydrates early.
Recent Research and Expert Insights
The field of gastroenterology continues to evolve as researchers uncover the long-term effects of acute infections. A severe stomach bug can affect the body well beyond the initial episode. The damage left behind requires careful, ongoing management.

Gut Flora Depletion and Post-Infectious IBS
Clinical studies increasingly highlight the phenomenon of post-infectious IBS. After a severe bout of contagious diarrhea, the natural microbiome takes a serious hit. Aggressive pathogens, combined with the rapid flushing of the bowels, strip away beneficial bacteria in massive numbers.
This disruption can lead to lingering bowel irregularities lasting for months: bloating, cramping, and unpredictable bowel habits long after the virus is gone. Expert consensus increasingly supports the use of targeted probiotic strains to support recovery. These symptoms should not be ignored.
mRNA Vaccine Development for Norovirus
While the rotavirus vaccine has been a major public health achievement, there is currently no approved vaccine for norovirus, the largest remaining gap in our defense. Norovirus mutates rapidly, which has caused traditional vaccine development to fail repeatedly.
Clinical trials are now underway for mRNA vaccines targeting norovirus specifically. These aim to provide multi-strain immunity for vulnerable populations. The mRNA platform allows scientists to update the vaccine quickly as new strains emerge. Until these vaccines become available, strict hygiene and isolation remain our best tools.
The Role of Targeted Probiotics in Mucosal Healing
Not all probiotics are equal when it comes to recovery from an enteric infection. A random grocery-store yogurt will not rebuild a severely damaged gut lining. You need specific, clinically studied strains proven to survive stomach acid.
Strains like Saccharomyces boulardii and Lactobacillus rhamnosus GG have shown strong results in clinical trials. They help with mucosal healing, reduce inflammation, and accelerate microbiome restoration. Always consult a gastroenterologist before starting high-dose probiotics after a severe illness.
How Long Is Diarrhea Contagious? A Detailed Timeline
One of the most urgent questions during recovery is how long is diarrhea contagious. The answer is not tied to how you feel physically. It depends entirely on the microscopic shedding of the pathogen, which follows a predictable biological curve.
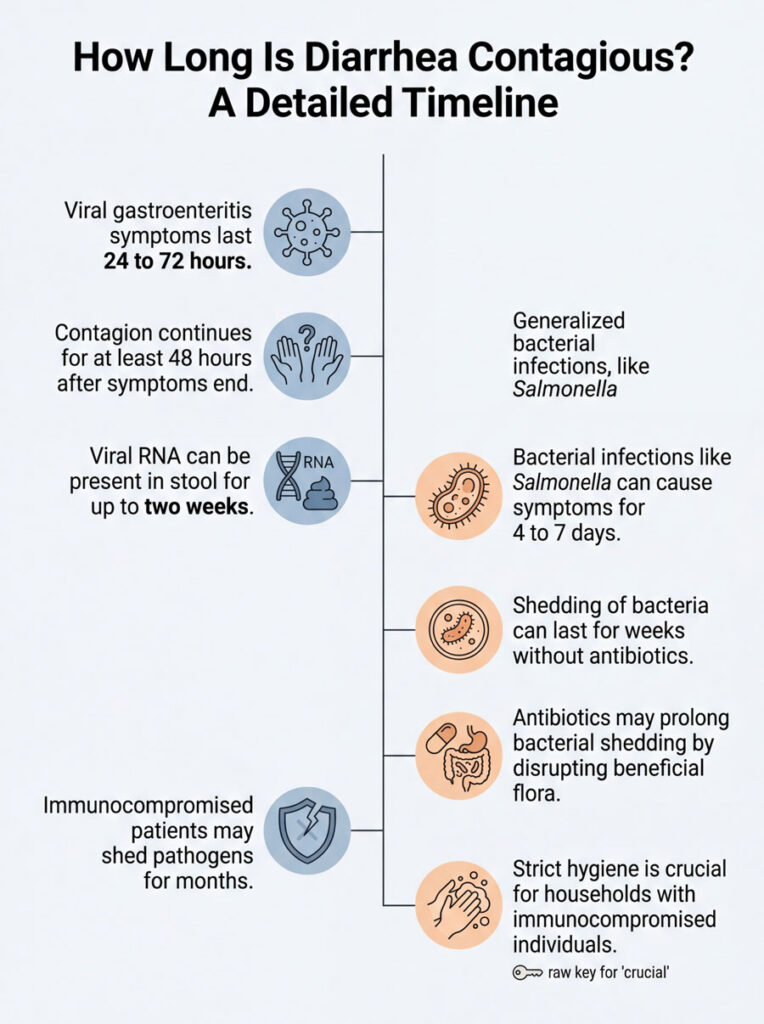
Viral Shedding Timelines
For viral gastroenteritis, the contagion timeline is longer than most people realize. Acute symptoms usually last 24 to 72 hours, but that is only the symptomatic phase.
Pathogenic shedding continues at high levels for at least 48 hours after the very last symptom. This is the minimum isolation period. Beyond that window, viral RNA can continue to appear in stool for up to two full weeks. You are most contagious while actively sick and for the 48 hours immediately after. But you remain a mild risk for weeks, which is why perfect bathroom hygiene matters long after you feel better.
Bacterial Clearance and the Impact of Antibiotics
Bacterial infections follow a different timeline. A severe Salmonella infection may produce acute symptoms for four to seven days. Without antibiotics, the body naturally sheds live bacteria in stool for several weeks.
Antibiotics can actually complicate things. While they kill the primary infection, they also destroy beneficial bacteria that compete with the pathogen. This can sometimes prolong shedding. For hospital-acquired C. diff, the risk remains extremely high until the patient finishes specialized treatment and produces consistently solid stools.
Long-Term Monitoring for Immunocompromised Patients
Different rules apply to patients with weakened immune systems. Elderly individuals, cancer patients, and those on immunosuppressant medications cannot clear pathogens quickly. An immunocompromised person might shed infectious norovirus for months after symptoms resolve.
If you live with an immunocompromised individual, your household hygiene must be meticulous. The standard 48-hour rule does not apply. Maintain strict disinfection routines until a doctor confirms they are no longer contagious.
Summary and Key Takeaways
Managing a gastrointestinal outbreak at home requires vigilance, proper hygiene, and a solid understanding of how these pathogens work. Here are the most important points to remember:
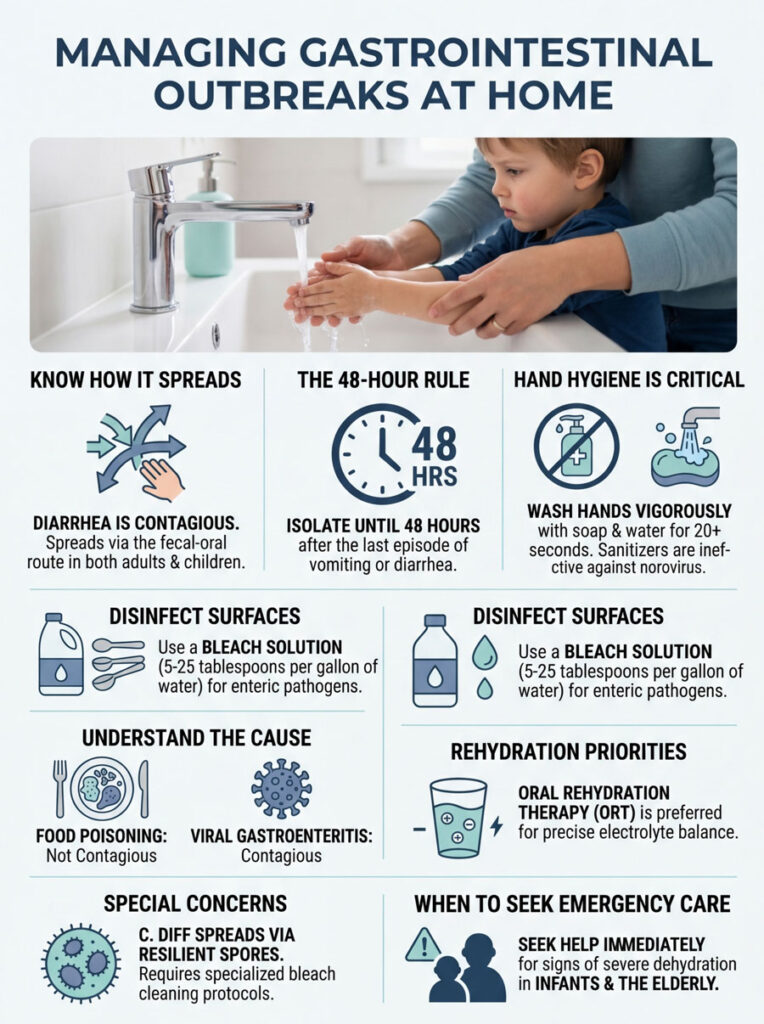
- Viruses lead the way. Norovirus and rotavirus are the top causes of acute viral gastroenteritis worldwide. They need very small viral loads to cause widespread illness.
- Soap beats sanitizer every time. Alcohol-based hand sanitizers cannot neutralize non-enveloped viruses. Vigorous handwashing with soap and warm water is mandatory.
- Respect the 48-hour rule. Pathogenic shedding continues long after symptoms fade. Stay isolated until 48 hours after your last symptom to lower the secondary attack rate.
- Hydration is the top priority. Use Oral Rehydration Therapy to prevent dangerous fluid loss. Seek emergency care for severe dehydration signs like confusion, rapid heart rate, or sunken eyes.
- Disinfect the right way. Standard wipes fail against enteric pathogens. Use a bleach-to-water solution and allow five minutes of contact time on surfaces.
The health of your household depends on treating these illnesses with the seriousness they deserve. By understanding the fecal-oral route and following strict clinical guidelines, you can prevent a minor illness from becoming a major outbreak. The next time someone asks you, is diarrhea contagious in adults and children, you will know exactly how to answer, and exactly how to keep your family safe.
Frequently Asked Questions
Is diarrhea contagious in both adults and children?
Yes, infectious diarrhea is highly contagious across all age groups. It primarily spreads via the fecal-oral route, where microscopic viral, bacterial, or parasitic particles are accidentally ingested. However, diarrhea caused by chronic conditions like IBS, IBD, or food intolerances is not transmissible.
How long am I contagious after a stomach bug?
Clinical guidelines dictate the 48-hour rule: you remain highly contagious until a full 48 hours have passed since your last episode of vomiting or diarrhea. It is critical to note that pathogenic shedding in the stool can continue for days or even weeks after your physical symptoms have completely resolved.
Does hand sanitizer kill norovirus and other stomach bugs?
No. Norovirus and rotavirus are non-enveloped viruses, meaning they lack a lipid membrane that alcohol can disrupt. They have a tough protein capsid that renders most hand sanitizers ineffective. Vigorous handwashing with soap and warm water for at least 20 seconds is the only proven method to mechanically remove these particles.
What is the best way to disinfect surfaces to prevent the spread of diarrhea?
Standard household wipes are often insufficient against aggressive enteric pathogens. The CDC recommends a freshly mixed solution of 5 to 25 tablespoons of household bleach per gallon of water. This solution must remain visibly wet on high-touch surfaces for at least five minutes to ensure total microbial eradication.
What is the difference between food poisoning and a contagious stomach flu?
Food poisoning often results from ingesting pre-formed bacterial toxins and typically manifests within hours; it is generally not contagious. Viral gastroenteritis (stomach flu) is an infection that replicates within the host and is highly transmissible via the fecal-oral route. If multiple household members get sick sequentially, it is likely a contagious infection.
Why is Oral Rehydration Therapy (ORT) recommended over plain water?
ORT is the gold standard for preventing hypovolemia because it uses a precise clinical ratio of sodium, potassium, and glucose. This specific balance triggers the sodium-glucose cotransporter in the intestinal wall, facilitating much more rapid water absorption into the bloodstream than plain water or sugary sports drinks.
How does C. diff spread and who is at risk?
Clostridioides difficile (C. diff) is a severe bacterial infection that often follows a course of broad-spectrum antibiotics, which deplete healthy gut flora. It spreads via highly resilient spores that can survive on surfaces for months. It is a major cause of nosocomial (hospital-acquired) transmission and requires specialized bleach protocols for disinfection.
Can you catch diarrhea from someone who has no symptoms?
Yes. Asymptomatic carriers can harbor and shed enteric pathogens without ever feeling ill themselves. Additionally, infected individuals often begin pathogenic shedding before their clinical symptoms appear, making early isolation difficult in settings like schools and offices.
When is diarrhea considered a medical emergency in infants and the elderly?
You must seek immediate emergency care if you observe markers of severe dehydration or hypovolemia. These include extreme lethargy, sunken eyes, a sunken fontanelle in infants, rapid heart rate, confusion, or anuria (no urine output for several hours). These patients often require intravenous fluids for stabilization.
Should I follow the BRAT diet while recovering from a stomach bug?
Modern gastroenterology has largely moved away from the restrictive BRAT diet (Bananas, Rice, Applesauce, Toast). While these foods are gentle, they lack the protein and fats necessary for mucosal healing. Clinical consensus now suggests returning to a balanced, age-appropriate diet as soon as tolerated to accelerate the repair of the intestinal lining.
Is it safe to go swimming after having an infectious diarrheal illness?
No. Individuals should wait at least two weeks after symptoms resolve before entering recreational water. Parasites like Cryptosporidium have tough outer shells that are resistant to standard pool chlorine, and a single accident can lead to a massive water-borne community outbreak.
Can a contagious stomach bug cause long-term digestive issues?
Yes, some patients develop post-infectious Irritable Bowel Syndrome (PI-IBS). The acute infection can cause significant disruption to the gastrointestinal mucosal lining and the microbiome. Targeted use of clinically studied probiotic strains, such as Saccharomyces boulardii, may help restore microbial balance and reduce lingering symptoms like bloating and cramping.
Disclaimer
This article is for informational and educational purposes only and does not constitute medical advice. The information provided regarding symptom management, hypovolemia prevention, and Oral Rehydration Therapy (ORT) is not intended to substitute for professional medical diagnosis or treatment. Always consult with a qualified healthcare provider or board-certified gastroenterologist regarding any severe gastrointestinal symptoms, especially in infants, the elderly, or immunocompromised individuals.
References
- Centers for Disease Control and Prevention (CDC) – https://www.cdc.gov/norovirus/ – Comprehensive data on norovirus burden, trends, and transmission prevention in the United States.
- World Health Organization (WHO) – https://www.who.int/news-room/fact-sheets/detail/diarrhoeal-disease – Global statistics on diarrheal disease impact and pediatric mortality rates.
- National Institutes of Health (NIH) – https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3913031/ – Research on the mechanics of the sodium-glucose cotransporter in Oral Rehydration Therapy.
- American Journal of Infection Control – https://www.ajicjournal.org/ – Peer-reviewed studies on the efficacy of bleach disinfection against non-enveloped viruses.
- Mayo Clinic – https://www.mayoclinic.org/diseases-conditions/viral-gastroenteritis/ – Clinical overview of viral gastroenteritis symptoms, causes, and patient care.