Here’s the part most pregnancy forums get backwards: a common cold won’t hurt your baby, but the wrong remedy actually might. The cold itself is just a rhinovirus, one of more than 200 strains, and your immune system handles it the same way it always has. The risk lives in two places most people overlook: a fever that climbs above 100.4°F, and a few specific medications that look harmless on a CVS shelf. Patients booking prenatal panels through HealthCareOnTime ask us about these tradeoffs almost daily, so let’s walk through the safe recovery playbook.
Table of Contents
Quick Answer
Rest, drink 8 to 12 cups of fluids daily, run a humidifier, and use saline nasal spray. Acetaminophen (Tylenol) is the safest OTC option for fever or aches, capped at 3,000 mg per 24 hours. Avoid NSAIDs (ibuprofen, aspirin) after week 20, skip pseudoephedrine in the first trimester, and call your OB if your fever hits 100.4°F or higher.

At a Glance
- The common cold itself does not harm your baby; the fever sometimes can
- Pregnancy colds last 7 to 14 days, longer than the typical 7 to 10 days
- Acetaminophen is the only widely recommended OTC pain/fever option in pregnancy
- Saline spray, humidifier, honey, and warm fluids are safe across all three trimesters
- The FDA recommends avoiding NSAIDs (ibuprofen, naproxen, aspirin) after week 20
- Bath water should stay below 95°F to protect the fetus
- Patients booking prenatal labs through HealthCareOnTime often ask whether a fever signals trouble; the answer depends on temperature and timing
Will a Cold Hurt My Baby?
Take a breath. The plain answer is no, a common cold will not hurt your baby. The virus does not cross the placenta. Banner Health and ACOG both confirm that catching a cold during pregnancy is not dangerous to your developing baby on its own. The bigger questions live one layer up: is it actually a cold, and is your fever in safe territory?
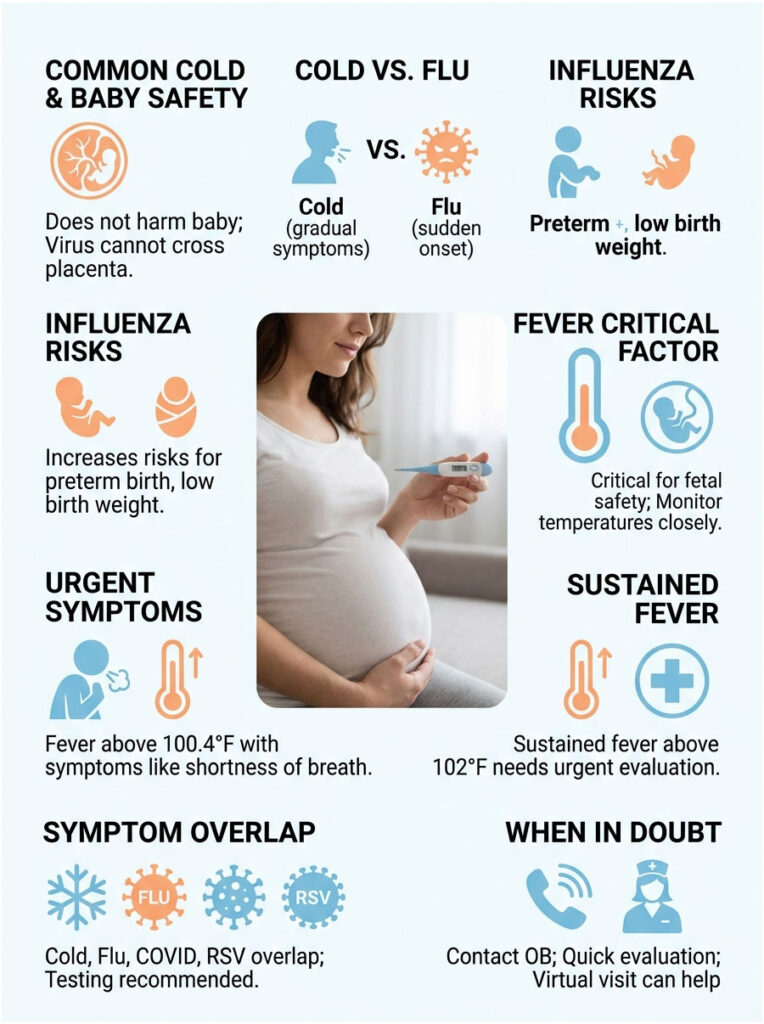
Common Cold vs the Flu (and Why the Difference Matters)
A cold builds slowly: scratchy throat one day, runny nose the next, mild congestion and cough by day three. The flu hits like a truck: sudden high fever, body aches, deep fatigue, dry cough. Banner Health reports that influenza during pregnancy raises the risk of preterm birth, low birth weight, and birth defects when high fever is involved.
If your symptoms come on within hours and you feel knocked flat, treat it as flu until proven otherwise and call your OB. ACOG and the CDC recommend antiviral medication (oseltamivir, Tamiflu) within 48 hours of flu symptoms in pregnancy.
When the Fever Becomes the Problem
Fever during pregnancy is the variable that actually matters for fetal safety. ACOG flags any fever of 100.4°F or higher coupled with shortness of breath, chest pain, or fainting as an immediate call to your provider. A sustained fever above 102°F at any point in pregnancy warrants urgent evaluation.
Nemours notes that elevated maternal temperature, especially in the first trimester, raises the risk of neural tube defects and other complications. That’s why bringing a fever down quickly with acetaminophen (under provider guidance) matters more than waiting it out.
Cold vs COVID vs RSV vs Flu in Pregnancy
Symptom overlap is real. ACOG recommends testing pregnant patients for both influenza and SARS-CoV-2 when respiratory symptoms appear, because treatment changes based on the cause. RSV is increasingly a concern; the CDC now recommends maternal RSV vaccine in late pregnancy (32 to 36 weeks) during RSV season.
If you have any uncertainty about which infection you’re dealing with, our medical reviewers recommend a same-day call to your OB rather than guessing. A 5-minute virtual visit usually clarifies it.
Why Colds Hit Harder During Pregnancy
Pregnancy changes your immune system in a deliberate way. The body partially suppresses certain immune responses to keep your developing baby from being treated as foreign tissue. The tradeoff is that minor infections, including the common cold, can feel rougher and last longer than they did before.
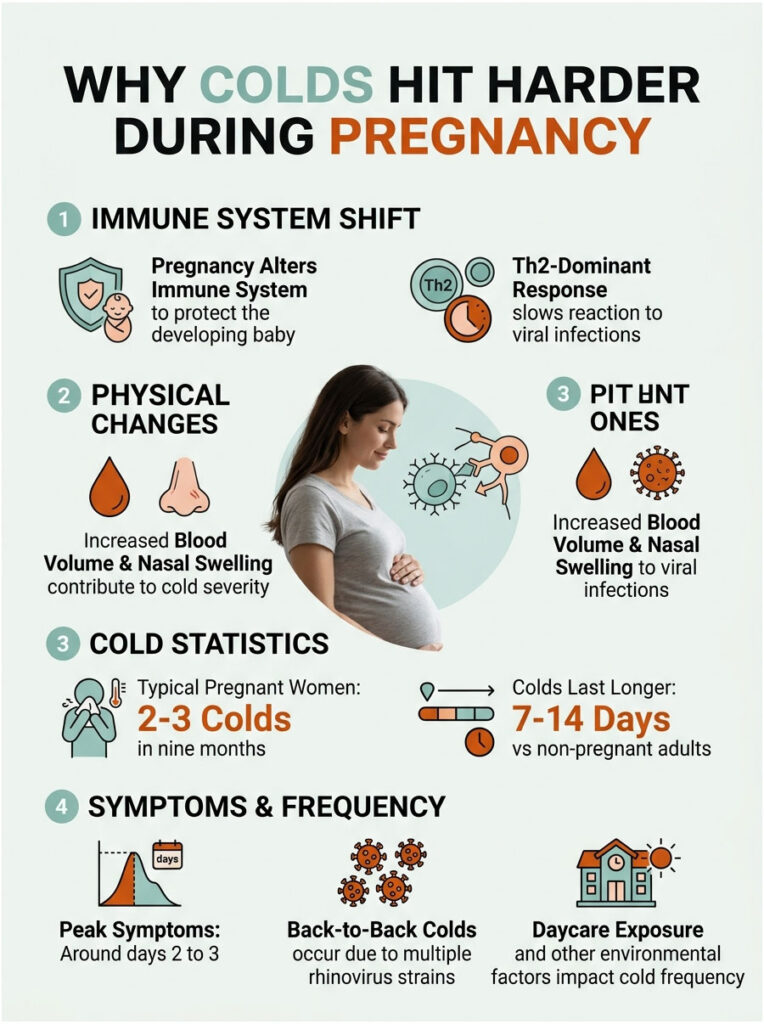
What Changes in Your Immune System
Your body shifts toward what immunologists call a Th2-dominant state during pregnancy. This protects the baby but slows your response to viral infections. Add the extra blood volume, hormonal swelling of the nasal passages (called pregnancy rhinitis), and the fatigue that already comes with growing a person, and a basic cold can feel like the flu.
The Bump notes that pregnant women typically experience two to three colds across nine months. Some people get more, some fewer. Children at home, daycare exposure, and seasonal timing drive most of the variation.
How Long a Cold Lasts in Pregnancy vs Normal
A typical adult cold runs 7 to 10 days. During pregnancy, expect 7 to 14 days, with peak symptoms around days 2 to 3, and a slow improvement curve after that. Texas Health reports that pregnancy colds run a little longer than the normal 7 to 10 days.
In cases reviewed by our medical team, the most common reason a cold seems to “stick around” is actually back-to-back exposure: with 200-plus rhinovirus strains in circulation, you can catch a brand-new cold the day your last one resolves. That’s not a worsening illness, just bad luck.
Safe Home Remedies That Actually Work
Most colds during pregnancy resolve with rest, fluids, and a handful of low-tech tools you already have at home. None of these carry medication risk, and most are recommended by US OB-GYN groups.

Hydration: Water, Decaf Tea, Broth
Aim for 8 to 12 cups of fluid daily when you’re sick. Plain water, decaf tea with lemon, warm broth, and electrolyte drinks all count. Texas Health recommends water, juice, and broth specifically to help flush out the virus. Hot fluids also thin mucus and soothe a sore throat naturally.
Watch caffeine: ACOG limits pregnancy intake to 200 mg per day (about one 12-oz coffee). Decaf herbal teas without caffeine fit the safe column.
Rest and Sleep Position
Sleep 8 to 10 hours, take naps without guilt, and elevate your head with two pillows or a wedge to ease overnight congestion. Side-lying (preferably left side) is the recommended pregnancy sleep position from the second trimester onward.
Banner Health specifically recommends elevating the head while sleeping to ease congestion. Across patients we serve, sleep is the single most underused recovery tool, especially for people juggling jobs and other kids.
Steam: Showers, Humidifiers, Warm Bowl Method
Steam thins mucus and reopens swollen nasal passages without any medication. A 10-minute hot shower with the door closed works well. A cool-mist or warm-mist humidifier in your bedroom adds overnight relief. The bowl-and-towel method (a bowl of warm water, towel over your head, breathe in steam) is fine, just keep your face a safe distance from the water.
One critical limit: bath water and hot tubs must stay below 95°F. Medical News Today notes that core body temperature increases above this point can harm a fetus, so skip the long soak in scalding water no matter how good it sounds.
Saline Spray and Nasal Rinse
Saline nasal sprays are universally safe in pregnancy and recommended by ACOG, Banner Health, Nebraska Medicine, and Catholic Health. They flush mucus, hydrate dry nasal passages, and don’t carry any decongestant ingredients.
Neti pots and nasal irrigation devices work the same way. Use only distilled, sterile, or previously boiled (and cooled) water. Tap water carries rare but serious infection risk.
Honey and Lemon for Sore Throat
A spoonful of honey in warm water with lemon coats and soothes a raw throat. Honey is safe for pregnant adults (the warning about honey applies only to babies under 12 months). One tablespoon two to three times a day is reasonable.
Salt-Water Gargle
Mix 1/2 teaspoon of salt in 8 oz of warm water, gargle, spit, repeat two or three times a day. Reduces throat inflammation, no medication risk. Recommended by Nebraska Medicine for sore throat relief during pregnancy.
Ginger Tea, Soup, Bone Broth
Fresh ginger steeped in hot water with a touch of honey eases nausea, sore throat, and mild cough. Bone broth and chicken soup deliver hydration plus electrolytes plus a small protein boost. Trogolo Obstetrics highlights ginger as one of the most-used pregnancy-safe remedies for cough and congestion.
Foods That Quietly Help
Citrus (oranges, grapefruit), bell peppers, kiwi, and strawberries deliver vitamin C. Leafy greens, garlic, and yogurt with live cultures support immune response. None of these is a cure, but they hold the foundation while your body does the work.
OTC Medications: Safe, Caution, Avoid
This is where US pregnancy forums spread the most misinformation. The safety profile of any OTC cold medicine depends on the active ingredient, the trimester, your medical history, and the dose. Here’s the practical guidance our medical reviewers walk patients through, consolidated from ACOG, FDA, Banner Health, Catholic Health, and Genesis OBGYN.

For pain and fever, acetaminophen (Tylenol) is the only widely OB-recommended OTC. Cap it at 3,000 mg per 24 hours and use the lowest effective dose for the shortest time. Recent FDA discussions prompted ACOG to reaffirm that acetaminophen, used in moderation, remains the safest choice; alarming claims linking it to autism or ADHD have not been proven by science, per Nemours and ACOG.
For cough relief, dextromethorphan (Robitussin DM, Delsym) is generally considered safe across all trimesters at the lowest strength for the shortest time, per Banner Health and Genesis OBGYN. Always run it past your provider first.
For chest congestion, guaifenesin (Mucinex) is considered safe in the second and third trimesters but typically avoided in the first 12 weeks. Stick with the plain single-ingredient version, not Mucinex DM or any combo formula.
For nasal decongestion, pseudoephedrine (Sudafed) is considered safe in the second and third trimesters but should be skipped in the first trimester due to a small association with rare birth defects. Phenylephrine carries a less-clear safety profile. Pregnant patients with high blood pressure should avoid both. Saline spray is the always-safe alternative.
For runny nose and post-nasal drip, chlorpheniramine (Chlor-Trimeton), diphenhydramine (Benadryl), and loratadine (Claritin) are generally considered safe across pregnancy. Diphenhydramine causes significant drowsiness, which can be useful at bedtime but rough during the day.
For chest rubs, Vicks VapoRub on the chest or under the nose is widely used in pregnancy and considered safe per The Bump’s expert sources. Avoid applying to broken skin, inside the nostrils, or in large amounts.
What to skip entirely: NSAIDs (ibuprofen, naproxen, aspirin) after week 20, given the FDA’s warning about low amniotic fluid and ductus arteriosus complications. Avoid aspirin throughout pregnancy unless prescribed for a specific medical reason. Skip combination cold medicines that mix multiple active ingredients; you may unknowingly double-dose a single ingredient. Avoid alcohol-based liquid cold formulas (some NyQuil, Theraflu original) and herbal supplements like echinacea unless your OB approves.
Table 1: OTC Cold Medication Safety in Pregnancy
| Medication | Active Ingredient | First Trimester | 2nd/3rd Trimester | Notes |
| Tylenol | Acetaminophen | Generally safe | Generally safe | Max 3,000 mg/24 hr |
| Sudafed | Pseudoephedrine | Avoid | Generally safe | Avoid if hypertension |
| Mucinex | Guaifenesin | Avoid | Generally safe | Consult provider |
| Robitussin DM | Dextromethorphan | Generally safe | Generally safe | Lowest dose, shortest time |
| Benadryl | Diphenhydramine | Generally safe | Generally safe | Causes drowsiness |
| Chlor-Trimeton | Chlorpheniramine | Generally safe | Generally safe | Not while breastfeeding |
| Claritin | Loratadine | Generally safe | Generally safe | Non-drowsy option |
| Vicks VapoRub | Camphor/Menthol | Generally safe | Generally safe | Topical only |
| Saline Spray | Sodium chloride | Always safe | Always safe | Use as needed |
| Advil/Motrin | Ibuprofen (NSAID) | Caution | Avoid after 20 wk | FDA warning |
| Aspirin | Acetylsalicylic acid | Avoid | Avoid | Unless prescribed |
| NyQuil/Theraflu | Multi-ingredient | Generally avoid | Consult provider | Often contains alcohol |
Trimester-by-Trimester Recovery Guide
Your body’s needs and the medication safety picture shift as pregnancy progresses. The same cold can call for different responses depending on your trimester.

First Trimester (Weeks 1-12, Most Cautious Window)
Your baby’s vital organs form during these weeks, so US OB-GYNs recommend the most conservative approach: rest, fluids, saline spray, humidifier, honey-and-lemon. For fever or aches, acetaminophen with provider approval. Skip pseudoephedrine, guaifenesin, NSAIDs, aspirin, and combination cold medicines unless your OB specifically clears them.
In tests booked through HealthCareOnTime, first-trimester patients ask the most “is it OK to take…” questions. The answer is usually: when in doubt, default to non-medication remedies first.
Second Trimester (Weeks 13-27, More Options)
Most additional OTC options open up here: Sudafed, Mucinex, dextromethorphan-based cough syrups all become commonly OB-approved with provider input. Acetaminophen remains the go-to for pain and fever.
This is also the safest time for the inactivated flu shot if you haven’t had one yet, per CDC and ACOG guidance, and the COVID-19 booster if eligible.
Third Trimester (Weeks 28-40, Comfort + Late-Pregnancy Cautions)
Comfort matters most here. Sleep gets harder, congestion can feel worse with elevated estrogen, and the FDA’s NSAID warning becomes absolute after week 20. Stick with acetaminophen, saline, humidifier, and rest.
If you’re past 36 weeks, our medical reviewers recommend calling your OB for any cold-like symptoms, since labor onset and infection symptoms sometimes overlap.
When to Call Your Doctor (and When to Go to the ER)
Most pregnancy colds don’t need a doctor visit. A few do. Here’s the line.

Same-Day Call Triggers
Call your OB the same day if you have a fever of 100.4°F or higher, symptoms that came on suddenly (think flu), a cough that produces colored mucus or blood, vomiting that prevents fluid intake, or symptoms in the third trimester past 36 weeks.
Within 24 to 48 Hours
Call within a day or two if symptoms haven’t started improving by day 5, if you can’t sleep due to congestion, if you’re worried about how a remedy might interact with prenatal vitamins, or if a sore throat is severe enough to make swallowing painful.
Emergency Room Red Flags
Go to the ER (or call 911) for shortness of breath at rest, chest pain, fainting, severe weakness, signs of dehydration (no urine output for 8+ hours, dizziness on standing), confusion, or any decrease in fetal movement after 28 weeks. ACOG flags fever above 100.0°F coupled with shortness of breath or chest pain as an immediate evaluation trigger.
Why Flu Symptoms Are an Urgent Call
Antiviral medications work best within 48 hours of symptom onset. The CDC and ACOG recommend that pregnant women suspected of flu start oseltamivir presumptively, without waiting for test results. Time matters more than confirmation.
Table 3: When-to-Worry Decision Guide for Cold During Pregnancy
| Symptom | Duration / Detail | Recommended Action | Timeline |
| Fever 100.4°F+ | Any | Call OB | Same day |
| Fever 102°F+ | Not breaking with Tylenol | Go to ER | Within hours |
| Shortness of breath / chest pain | Any | Call 911 / ER | Now |
| Sudden severe symptoms (flu-like) | Any | Call OB for antivirals | Within 48 hours |
| Decreased fetal movement (28+ wk) | Any | ER | Now |
| Symptoms worsening past day 7 | Persistent | Call OB | Within 24 hours |
| Mild cold (no fever) | Under 7 days | Home care | Watch and rest |
Cold Recovery Habits That Speed Things Up
Beyond the remedies, a few daily habits shorten recovery and prevent setbacks.
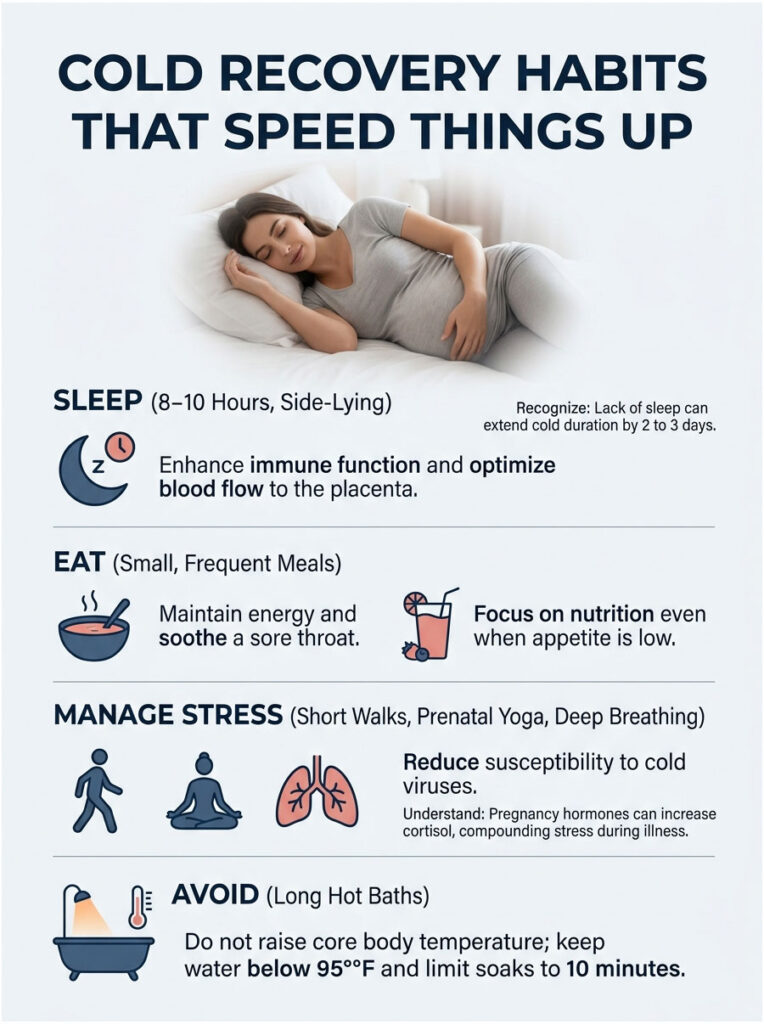
Sleep 8 to 10 Hours, Side-Lying
Sleep is when your immune system actually works. Pregnant patients we serve often try to push through a cold for work or family obligations; the cold typically lengthens by 2 to 3 days when sleep falls short. Side-lying (left preferred) keeps blood flow to the placenta optimal.
Eat Often, Even If You’re Not Hungry
Small, frequent meals beat skipping food. Soups, smoothies, yogurt, eggs, and toast are easy on a sore throat and weak appetite. Texas Health specifically recommends small portions throughout the day when you can’t stomach larger meals.
Manage Stress and Hormones
Pregnancy hormones already raise cortisol; a cold piles on. Short walks, prenatal yoga, deep breathing, or simply lying down with your eyes closed help. Cushelle research notes that stress increases susceptibility to cold viruses.
Avoid the Bath-Trap
A long, hot soak feels heavenly when you’re sick but can push core body temperature into fetal-risk territory. Keep bath water under 95°F (warm, not hot), keep soaks under 10 minutes, and skip hot tubs and saunas entirely.
How to Lower Your Risk of the Next Cold
US adults catch about 1 billion colds per year, per Genesis OBGYN. Pregnancy-period prevention matters because each cold means more discomfort, more days off, and more medication decisions.
Flu, Covid, RSV, and Tdap Vaccines in Pregnancy
The CDC and ACOG recommend the inactivated flu shot during any trimester, the COVID-19 vaccine and boosters as appropriate, the RSV vaccine in late pregnancy (32-36 weeks during RSV season), and the Tdap vaccine in the third trimester to protect the newborn from whooping cough.
These don’t prevent the common cold (no vaccine does), but they significantly reduce your risk of the more dangerous viral illnesses that get confused with a cold.
Hand Hygiene
Wash your hands with soap and warm water for at least 20 seconds, especially after touching shared surfaces, before eating, and after being near sick people. Banner Health notes regular handwashing protects against 1 in 5 respiratory infections.
Limiting Exposure
If you have a school-age child or work in a high-contact environment, you’ll catch more colds. Practical steps: ask sick coworkers to mask up or work from home when possible, avoid sharing utensils and cups, disinfect doorknobs and phones, and don’t touch your face with unwashed hands.
Diet, Sleep, and Prenatal Vitamins as Defense
A balanced diet with adequate vitamin C, vitamin D, and zinc supports immune function. Prenatal vitamins with folate, iron, and DHA cover the basics most pregnant women need. Aim for 7 to 9 hours of sleep nightly, 30 minutes of moderate movement most days, and stress-reduction time built into your week.
Table 2: US Cold and Flu Pregnancy Statistics
| Statistic | Figure | Source |
| US colds per year (adults) | ~1 billion | Genesis OBGYN |
| Average colds per pregnancy | 2 to 3 | The Bump |
| Cold duration in pregnancy | 7 to 14 days | Texas Health / The Bump |
| Pregnant women hospitalized with flu | Higher in 2nd/3rd trimester | ACOG |
| Fever threshold for OB call | 100.4°F | ACOG |
| Acetaminophen daily max | 3,000 mg/24 hr | Banner Health |
| FDA NSAID restriction | After week 20 | FDA |
| Antiviral window for flu | Within 48 hours | CDC |
Frequently Asked Questions
Can a cold hurt my baby during pregnancy?
A common cold itself does not cross the placenta and does not harm your baby. The risk lies in a high fever (above 100.4°F) and the wrong choice of medication. Most US OB-GYN groups, including ACOG and Banner Health, confirm that the virus is not a direct threat; manage the fever, hydrate, rest, and the cold runs its course safely.
What cold medicine can I take in the first trimester?
The most cautious choice is no medication, just home remedies: rest, fluids, saline spray, humidifier, honey, and warm broth. If a fever or significant ache develops, acetaminophen (Tylenol) with OB approval is the standard. Skip pseudoephedrine, NSAIDs, aspirin, and combination cold medicines in the first trimester unless your provider specifically recommends them.
Is Tylenol safe for a cold during pregnancy?
Yes, in standard doses. ACOG and most US OB-GYN groups consider acetaminophen the safest OTC pain and fever option in pregnancy when used at the lowest effective dose for the shortest time, with a maximum of 3,000 mg per 24 hours. Avoid the multi-symptom Tylenol Cold formulas without checking each ingredient.
Is Sudafed safe during pregnancy?
Sudafed (pseudoephedrine) is generally considered safe in the second and third trimesters with provider approval, per Banner Health and Catholic Health. Avoid it in the first trimester due to a small association with rare birth defects. Skip it entirely if you have high blood pressure. Saline spray is the universally safe alternative for nasal congestion.
Can I use Vicks VapoRub while pregnant?
Yes, Vicks VapoRub is widely considered safe during pregnancy when applied topically to the chest or under the nose, per The Bump. The active ingredients (camphor, menthol, eucalyptus) are absorbed minimally. Avoid applying to broken skin, inside the nostrils, or in large amounts. It’s a popular pregnancy-safe choice for nighttime congestion relief.
How long does a cold last during pregnancy?
Pregnancy colds typically last 7 to 14 days, with peak symptoms around days 2 to 3. That’s a few days longer than a typical adult cold. Symptoms usually improve gradually after day 4 or 5. If symptoms worsen instead of improve after day 5, or last beyond 10 days, call your OB to rule out a secondary infection like sinusitis or bronchitis.
When should I call my doctor about a cold while pregnant?
Call your OB the same day for any fever of 100.4°F or higher, sudden flu-like symptoms, colored or bloody mucus, inability to keep fluids down, or symptoms in the third trimester past 36 weeks. Go to the ER for shortness of breath, chest pain, fainting, severe dehydration, or decreased fetal movement after 28 weeks. ACOG flags fever plus respiratory symptoms as an immediate evaluation trigger.
Can I take Mucinex while pregnant?
Mucinex (guaifenesin) is generally considered safe in the second and third trimesters when used as directed and with OB approval, per Banner Health. It’s typically avoided in the first trimester. The plain Mucinex (single-ingredient) is preferred over Mucinex DM or multi-symptom versions. Hydration plus a humidifier often achieves similar results without medication.
Is it safe to take a hot bath when sick during pregnancy?
A warm bath is fine, but the water must stay below 95°F. Medical News Today and ACOG warn that core body temperature increases above this threshold can harm a fetus, especially in the first trimester. Keep soaks under 10 minutes, skip hot tubs and saunas entirely, and use a thermometer if you’re unsure about water temperature.
Can I drink Theraflu while pregnant?
Use caution. Theraflu products contain multiple active ingredients, often including pseudoephedrine, dextromethorphan, and sometimes alcohol or NSAIDs depending on the formula. Some formulations are not recommended in pregnancy, especially for women with high blood pressure or in the first trimester. Read the label carefully and call your OB before taking any multi-ingredient cold formula.
Does pregnancy make colds worse?
For many people, yes. Pregnancy shifts your immune system to protect the baby, which slows your viral defense response. Add pregnancy rhinitis (hormone-driven nasal swelling), increased blood volume, and existing fatigue, and a basic cold can feel rougher than usual. Symptoms also tend to last a few days longer than a non-pregnancy cold.
Can my cold pass to my baby?
The cold virus itself does not cross the placenta, so your baby in utero will not catch your cold. However, in the third trimester, a serious respiratory illness in the mother can affect oxygen supply or trigger early labor. After delivery, you can pass the virus to your newborn through close contact, which is why hand hygiene and avoiding face-to-face exposure when sick are important in the postpartum period.
Disclaimer
This article is for general health education and does not replace personal medical advice. Pregnancy medication safety depends on individual history, trimester, and dosage. Always consult your OB-GYN, midwife, or licensed pharmacist before starting any new medication or supplement during pregnancy. Call 911 or your nearest emergency department for severe symptoms or any concern about fetal movement.
References
- ACOG, Influenza in Pregnancy: Prevention and Treatment
- CDC, Recommendations for Obstetric Health Care Providers Related to Use of Antiviral Medications
- FDA, NSAIDs After 20 Weeks of Pregnancy
- MedlinePlus, Pregnancy and the Flu
- Banner Health, How to Treat the Flu or Cold During Pregnancy
- Catholic Health, How to Treat a Cold or Flu When Pregnant
- Nebraska Medicine, Safe Cold and Flu Medications While Pregnant
- American Pregnancy Association, Cough and Cold During Pregnancy
- The Bump, How to Treat a Cold During Pregnancy
- Nemours, Navigating Cold and Flu Season While Pregnant