If you have ever searched for answers about vaginal dryness, painful intercourse, or discomfort during menopause, you are not alone. These issues affect millions of women worldwide, yet they rarely get the attention they deserve.
Table of Contents
In my urogynecology practice, patients ask me the same question almost every day: are laser treatments effective for female sexual health? And the honest, evidence-based answer is encouraging. Clinical studies consistently show that energy-based therapies deliver highly successful outcomes, especially for women dealing with estrogen loss and pelvic floor dysfunction.
I am Dr. Elena Rodriguez, MD, FACOG, and I specialize in regenerative medicine and female pelvic medicine. My clinical focus is helping women find evidence-based, non-hormonal menopause relief when traditional options fall short.

Modern gynecology has moved well beyond cosmetic procedures. In this article, we will explore the biological mechanisms behind vaginal laser therapy, compare these devices to traditional estrogen treatments, and carefully review FDA safety guidelines so you can make a fully informed decision.
Quick Answer
Yes. Clinical studies show that laser treatments are highly effective for female sexual health, particularly in treating Genitourinary Syndrome of Menopause (GSM) and vaginal atrophy. Devices like the Fractional CO2 laser and Erbium laser use controlled thermal energy to stimulate new collagen production, restore vaginal moisture, and significantly reduce painful intercourse, all without hormones.
Key Statistics on Female Pelvic Health
- Up to 50% of postmenopausal women develop symptoms of Genitourinary Syndrome of Menopause (Source: North American Menopause Society, 2022).
- Nearly 40% of breast cancer survivors experience severe vaginal atrophy caused by estrogen-blocking therapies.
- Clinical trials report an 85% improvement in vaginal dryness scores after three Fractional CO2 laser sessions.
- Over 75% of women report significant relief from painful intercourse after completing a full laser protocol.
- Fewer than 10% of women seek vaginal atrophy treatment, often due to embarrassment or lack of awareness about non-hormonal options.
- Histological biopsies show a 60% increase in epithelial thickness 90 days after treatment.
Understanding GSM: The Core Condition Behind Vaginal Atrophy
Before understanding how lasers can heal tissue, you need to understand the disease itself. Genitourinary Syndrome of Menopause, or GSM, is a medical term that describes the anatomical and physiological changes that happen when estrogen levels drop sharply.
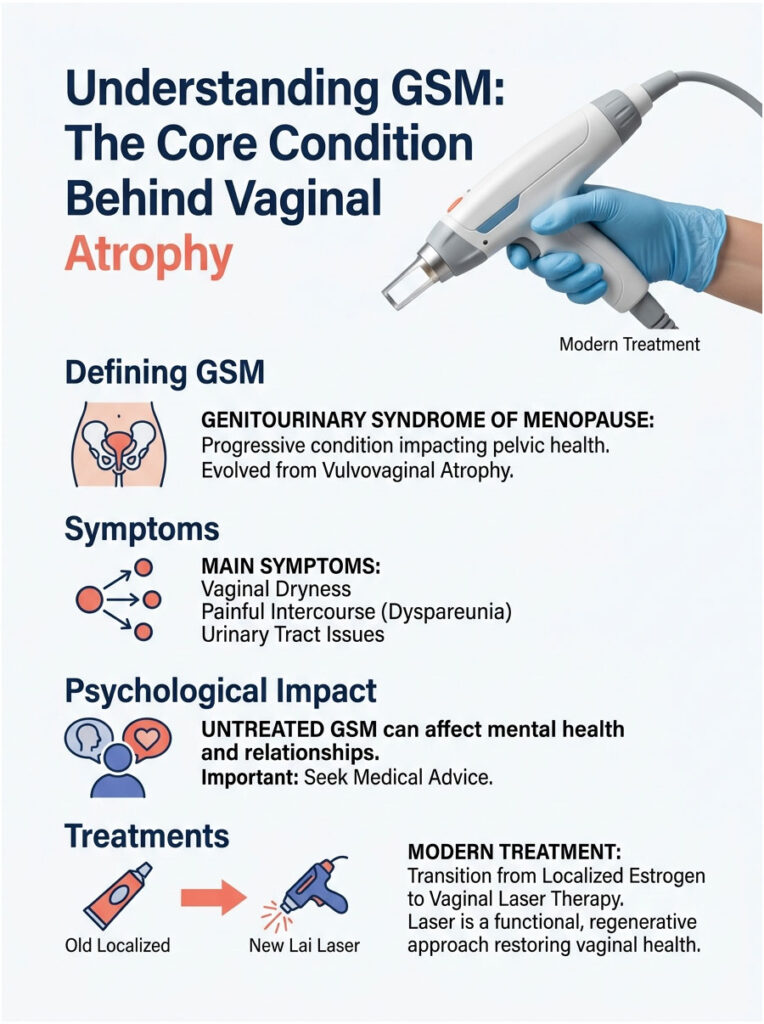
Doctors used to call this vulvovaginal atrophy. A few years ago, the North American Menopause Society updated the name to reflect the fact that symptoms affect the entire pelvic region, not just the vagina.
Unlike hot flashes, which tend to fade over time, GSM is progressive. Without intervention, the tissue continues to degrade year after year. Estrogen is the primary fuel that keeps pelvic tissue healthy. When the ovaries stop producing it during menopause, vaginal walls become thin, dry, and inflamed. This thinning process is the central target of any effective vaginal atrophy treatment.
The Three Main Symptoms of GSM
Severe vaginal dryness is usually the first complaint. Without estrogen, the tissue cannot produce adequate natural lubrication. This leads to chronic irritation, burning, and discomfort during everyday activities like walking or wearing fitted clothing.
Dyspareunia, or painful intercourse, is the second major symptom. As the vaginal lining thins, it loses its elasticity. Friction during intimacy causes tiny tears in the fragile tissue, making sexual activity painful. Many women begin avoiding intimacy entirely, which can deeply affect relationships. The anticipation of pain also triggers involuntary pelvic floor spasms, creating a frustrating cycle.
Urinary tract problems are the third symptom. Estrogen receptors line the urethra and bladder base. When estrogen drops, the urinary tract becomes vulnerable to pathogens. Women experience urgency, mild stress incontinence, and highly recurrent urinary tract infections as the thinning tissue loses its protective barrier.
The Psychological Impact of Untreated Atrophy
We cannot talk about pelvic health without addressing the emotional toll. Millions of women suffer in silence, believing that pain and dryness are just normal parts of aging. That silent suffering often leads to anxiety, depression, and a deep sense of disconnection from partners and their own bodies.
The good news: medical science offers real, tangible solutions. Restoring the structural integrity of the vaginal wall is entirely possible with the right technology. Chronic pain does not have to be your new normal.
Why Modern Urogynecology Is Shifting Toward Lasers
For decades, localized estrogen creams were the standard of care. But what about women who cannot safely take hormones? Or those who find daily creams impractical or messy?
This gap in care is precisely why vaginal laser therapy efficacy has become such a major focus. The field is moving away from the misleading marketing phrase “vaginal rejuvenation,” which implies a superficial cosmetic fix. Instead, modern urogynecology focuses on functional, regenerative cellular health, using precise light energy to rebuild tissue from the inside out.
How Vaginal Lasers Actually Work: The Science of Tissue Regeneration
Laser treatment for female sexual dysfunction works through a physiological principle called controlled thermal micro-trauma. The device delivers precise light energy to create microscopic injuries in the vaginal lining.
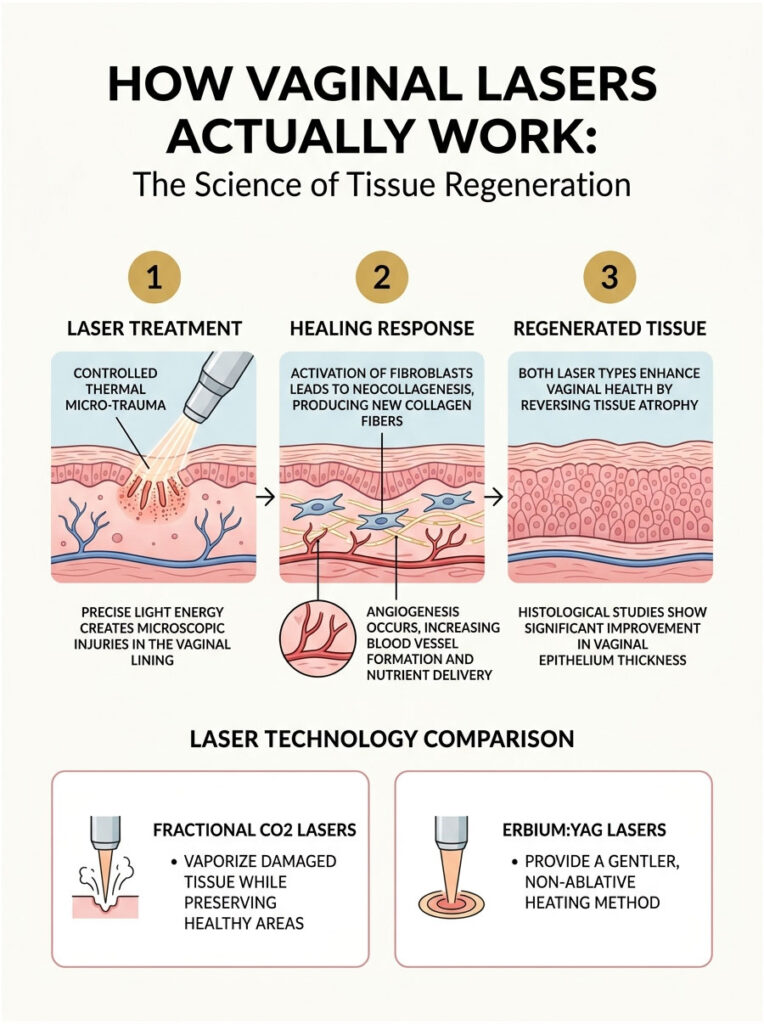
That might sound alarming, but the process is highly controlled and remarkably safe. Your body responds to these invisible micro-injuries by launching a massive healing response. It is the same science used in facial dermatology to reduce deep wrinkles and acne scars.
The targeted heat activates dormant cells called fibroblasts, the tiny factories in your body responsible for producing collagen and elastin. Once activated, they immediately get to work repairing the area.
Neocollagenesis and Angiogenesis
Fibroblast activation triggers a process called neocollagenesis, which literally means the creation of brand-new collagen fibers. These fibers act like scaffolding, providing crucial structural support to the vaginal wall.
At the same time, the thermal energy stimulates angiogenesis, the formation of new blood vessels within the tissue. More blood vessels deliver more oxygen and vital nutrients to the vaginal epithelium.
Together, these two processes completely reverse the thinning caused by estrogen loss. The tissue transforms from a pale, fragile state to a thick, healthy, robust condition. It is a genuine regenerative process driven entirely by your own biology.
Fractional CO2 Lasers: A Closer Look
The Fractional CO2 laser is the most widely studied device for this condition. The MonaLisa Touch system is one well-known example. It uses a wavelength of 10,600 nanometers that is highly absorbed by water inside tissue cells.
When fired, the laser vaporizes tiny columns of damaged tissue in an ablative process. It removes the old, degraded surface layer while delivering deep heat into the lamina propria, the connective tissue layer where real structural support lives.
Because the laser is fractional, it leaves bridges of healthy tissue between the vaporized columns, allowing for very rapid healing. This technology is especially effective for severe vaginal atrophy and autoimmune conditions like Lichen Sclerosus.
Erbium:YAG Lasers: A Gentler Approach
The Erbium (Er:YAG) laser, such as the Fotona Smooth system, works differently. It operates at a shorter wavelength of 2,940 nanometers. Because of its extremely high water absorption rate, it does not vaporize tissue. Instead, it delivers a non-ablative, photothermal heating effect.
This means it gently heats the vaginal lining without breaking the surface at all. The result is a much gentler recovery. The Erbium laser is an excellent choice for women with mild to moderate laxity or those who want moisture restoration with minimal downtime.
Expert Insight: Histological data from the American College of Obstetricians and Gynecologists shows that biopsies taken after three laser sessions reveal a significantly thicker vaginal epithelium, with tissue resembling a healthy, glycogen-rich pre-menopausal state.
CO2 vs. Erbium Laser: How They Compare
Both devices deliver excellent outcomes, but they serve slightly different patient profiles. The right choice depends on your specific symptoms, tissue health, and tolerance for downtime.

| Feature | Fractional CO2 (e.g., MonaLisa Touch) | Erbium:YAG (e.g., Fotona Smooth) |
| Mechanism | Ablative micro-trauma with deep thermal heating | Non-ablative photothermal heating |
| Tissue Penetration | Deep penetration into lamina propria | Shallower, controlled surface heating |
| Best For | Severe atrophy, GSM, Lichen Sclerosus | Mild to moderate laxity, moisture restoration |
| Recovery | 3 to 5 days of pelvic rest | 1 to 3 days of mild pelvic rest |
| Sensation | Mild prickling or internal vibration | Gentle warming sensation |
Some advanced clinics house both types of lasers, which allows providers to customize treatment plans. For example, a doctor might start with the Erbium laser for the first session and switch to the CO2 laser for the final treatment.
Proven Clinical Benefits of Laser Treatment for Vaginal Atrophy
When evaluating vaginal laser therapy efficacy, we look at measurable clinical outcomes, not just subjective impressions. Doctors use precise instruments to measure vaginal pH and tissue elasticity, along with validated medical scoring systems to track pain reduction over time.
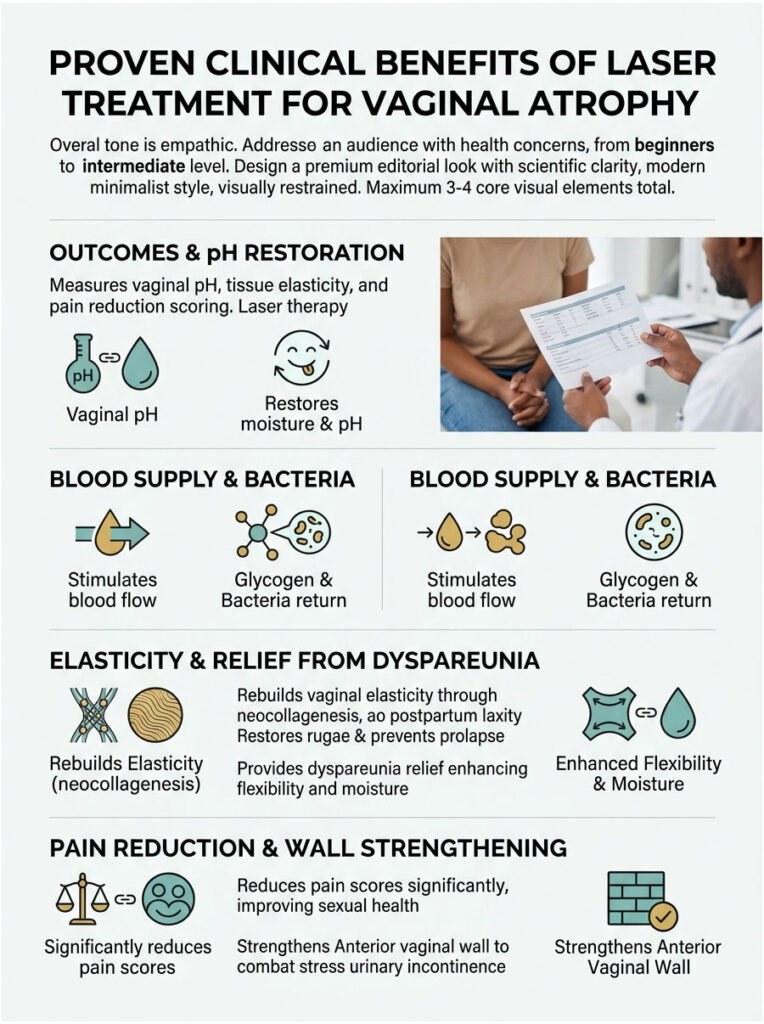
The benefits of a Fractional CO2 laser or Erbium laser extend far beyond basic comfort. These treatments genuinely restore the biomechanical function of the pelvic floor.
Restoring Vaginal Moisture and pH Balance
Healthy vaginal tissue is naturally moist and slightly acidic, which protects your body from bacterial and fungal infections. When estrogen drops, the tissue loses its blood supply. Without adequate blood flow, epithelial cells stop producing glycogen, the primary food source for beneficial lactobacilli bacteria.
When these good bacteria die off, vaginal pH becomes dangerously alkaline, leading to constant dryness, odors, and chronic bacterial vaginosis.
Laser therapy stimulates angiogenesis, bringing fresh, oxygenated blood back to the tissue surface. This renewed blood supply allows epithelial cells to produce glycogen again. The lactobacilli return, pH drops to a healthy acidic level, and natural moisture is restored.
Rebuilding Elasticity and Treating Vaginal Laxity
Loss of structural support is a significant concern for many women, particularly those dealing with postpartum vaginal laxity after difficult deliveries. Childbirth stretches pelvic floor muscles and damages the connective tissue matrix. As we age, we also naturally lose elastin fibers throughout the body.
By triggering neocollagenesis, the laser forces the body to build new, tightly woven collagen bundles. This physically thickens the vaginal walls, restores the natural rugae (the textured folds inside a healthy vagina), and can help prevent pelvic organ prolapse over time.
Relief from Painful Intercourse (Dyspareunia)
One of the most meaningful benefits of laser treatment for female sexual dysfunction is relief from dyspareunia. Atrophic tissue is extremely fragile and tears easily. It lacks the flexibility needed for comfortable intimacy, and the resulting micro-tears can bleed and take days to heal.
The anticipation of this pain triggers involuntary pelvic floor muscle spasms, which make the problem worse, creating a painful cycle of fear and discomfort.
Once neocollagenesis rebuilds the tissue, the vaginal lining regains its stretch and flexibility. The restored moisture acts as a natural lubricant. Peer-reviewed studies show massive reductions in pain scores, allowing women to finally break free from this cycle.
Laser Therapy for Stress Urinary Incontinence
The front wall of the vagina directly supports the urethra and bladder neck. When this wall becomes thin and weak, the urethra loses its physical backboard. The result is stress urinary incontinence (SUI), the involuntary leaking of urine when you cough, laugh, sneeze, or exercise.
SUI is extremely common after childbirth and during later stages of menopause. By thickening the anterior vaginal wall with a Fractional CO2 or Erbium laser, we create a firmer support structure. When abdominal pressure increases, the urethra is compressed against this strengthened wall, effectively preventing unwanted leakage.
Laser Therapy vs. Estrogen Cream: Choosing the Right Path
In my practice, I spend a great deal of time discussing laser therapy versus estrogen cream. Both options are medically valid, but they suit very different lifestyles and medical histories.
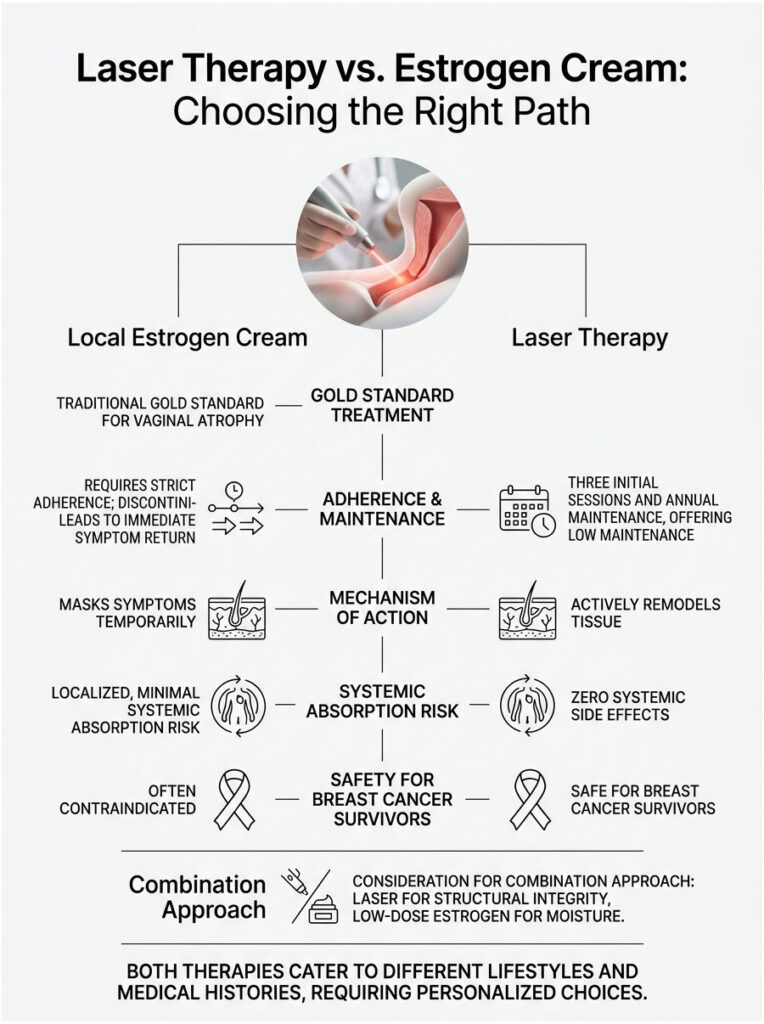
Local estrogen therapy is the traditional gold standard for vaginal atrophy treatment. It involves inserting a cream, tablet, or flexible ring directly into the vagina, where estrogen binds to cellular receptors and plumps the tissue.
However, local estrogen has practical limitations. It requires strict patient compliance. You must apply the cream twice a week, every week, for the rest of your life. If you stop, symptoms return almost immediately. You are tied to a pharmacy and a specific routine indefinitely.
The Convenience Factor
When comparing laser therapy versus estrogen cream, convenience matters. Laser therapy is a low-maintenance approach. You complete three initial sessions, then return once a year for a quick maintenance treatment.
Estrogen cream works passively: it only masks symptoms while the medication is present. It does not force the body to build new, permanent collagen. Laser treatments actively remodel the tissue architecture, relying on your own cellular regeneration rather than an external pharmaceutical product.
The Systemic Risk Debate
Many women worry about hormone replacement therapy. Even though localized estrogen is generally considered safe, some systemic absorption does occur. For most healthy women, this tiny amount poses no threat. But for women with a strong family history of blood clots or strokes, even minimal absorption causes anxiety.
Lasers solve this problem completely. Because they use light energy rather than chemicals, there is zero risk of systemic side effects. Your liver and cardiovascular system are entirely unaffected.
A Lifeline for Breast Cancer Survivors
This is where vaginal laser therapy efficacy truly stands out. Women who have survived hormone-receptor-positive breast cancer generally cannot use estrogen creams. Oncologists often prohibit even localized estrogen due to the small risk of systemic absorption.
These survivors are frequently placed on aromatase inhibitors that aggressively block all remaining estrogen production. As a result, they experience the most severe forms of GSM.
For these women, finding safe, non-hormonal menopause relief is a medical necessity. The Fractional CO2 and Erbium lasers offer a true lifeline, safely restoring vaginal health without introducing any hormones into the bloodstream.
| Consideration | Vaginal Laser Therapy | Local Estrogen Therapy |
| Hormonal Content | 100% non-hormonal and chemical-free | Contains localized estradiol or conjugated estrogens |
| Frequency | 3 initial sessions, then annual maintenance | Daily or bi-weekly application, ongoing |
| Systemic Risk | Zero risk of systemic absorption or clots | Minimal but documented absorption risk |
| Oncology Safety | Recommended for breast cancer survivors | Contraindicated for hormone-sensitive cancers |
| Tissue Remodeling | Actively stimulates neocollagenesis and repair | Passive plumping while medication is in use |
It is worth noting that some urogynecologists recommend a combination approach for severe cases, using the laser to rebuild structural integrity first, then prescribing a very low-dose estrogen cream for superficial moisture if the patient is a safe candidate.
Safety First: Understanding FDA Warnings and Potential Risks
As a medical professional, patient safety is my absolute priority. We need to have an honest conversation about the risks, because energy-based treatments are powerful surgical tools that demand respect.

You may have seen concerning headlines about FDA safety communications for vaginal lasers. Understanding the precise context behind those warnings is essential.
What the 2018 FDA Warning Actually Said
In 2018, the FDA issued strict warnings about the marketing of energy-based devices for vaginal health. Their focus was on the misleading term “vaginal rejuvenation” and the unsubstantiated cosmetic claims being made by medical spas.
These devices were originally cleared for well-documented gynecological uses, such as destroying precancerous cervical tissue or removing genital warts. But manufacturers began aggressively marketing them for unproven cosmetic tightening procedures.
The FDA stepped in to stop this deceptive marketing, warning that aggressive cosmetic use could lead to severe burns or scarring. They highlighted the danger of unqualified practitioners using powerful lasers for the wrong reasons.
Critically, the FDA did not invalidate the large body of peer-reviewed research supporting vaginal atrophy treatment. They demanded that providers stop promising cosmetic miracles without proper clinical evidence.
Known Side Effects and Contraindications
Like any legitimate medical procedure, laser treatment carries potential risks. The most significant is thermal injury to the vaginal wall. If energy settings are too high, or the provider moves the wand too slowly, severe burns can occur.
Other side effects include temporary spotting, mild pelvic cramping, and altered discharge for a few days. In extremely rare cases, severe thermal injury can cause permanent vaginal scarring. Proper technique is non-negotiable.
Strict contraindications also apply. You cannot undergo treatment if you have an active pelvic infection, undiagnosed vaginal bleeding, or a history of recent pelvic radiation therapy.
Red Flags to Watch for at Medical Spas
Your safety depends on choosing the right provider. Never receive an internal pelvic laser treatment at a standard cosmetic spa. Aestheticians and basic laser technicians are not trained to evaluate complex pelvic anatomy.
Seek out a board-certified urogynecologist or specialized gynecologist who understands the precise anatomy and knows exactly how to adjust energy settings for your tissue.
A qualified provider will always perform a thorough pelvic exam before treatment, ruling out hidden prolapse, silent infections, and precancerous lesions. If a clinic offers the procedure same-day without an exam, that is a serious red flag.
What to Expect: The Patient Journey from Consultation to Recovery
Many women feel anxious before their first treatment. Fear of the unknown is completely normal with intimate health issues. Understanding the step-by-step process helps ease that anxiety.
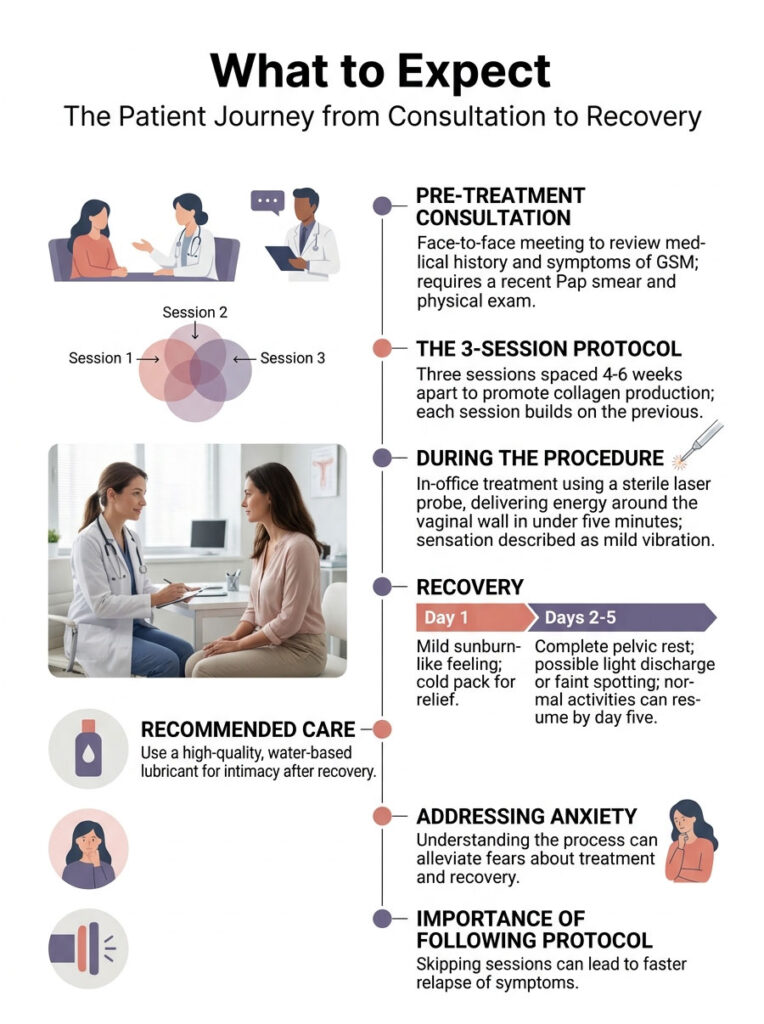
Pre-Treatment Consultation
Your journey starts with a face-to-face consultation where the doctor reviews your full medical history and discusses your specific symptoms of GSM. A recent, normal Pap smear is required before any laser therapy. A physical exam ensures there are no active infections.
There is very little preparation on your end. You do not need to fast or undergo general anesthesia. Simply arrive at the clinic well-hydrated and ready for a quick, in-office procedure.
The 3-Session Protocol
The standard clinical protocol involves three separate sessions. Why three? Because biological neocollagenesis takes time. The body simply cannot build all the necessary collagen in a single day.
The first session initiates the healing response. Sessions are spaced four to six weeks apart to align with the body’s natural cellular turnover cycle. The second session builds on the first. The third solidifies and tightens the structural changes. Skipping the final session often leads to a faster relapse of symptoms.
During the Procedure
You lie on an exam table as with a routine pelvic exam. The doctor inserts a specialized, sterile laser probe, usually smaller than a standard speculum, into the vaginal canal.
As the probe is slowly withdrawn, it delivers rapid pulses of energy 360 degrees around the vaginal wall. The entire internal process takes less than five minutes. Most patients describe the sensation as a mild vibration or light prickling feeling.
Recovery: Day 1 Through Day 5
Recovery is generally mild. You may feel a slight sunburn-like sensation internally for the first 24 hours. A cold pack applied to the vulva provides immediate relief.
The most important rule is complete pelvic rest for three to five days: no intercourse, no tampons, no hot tubs, no swimming, and no intense cycling. You may notice light, watery discharge or very faint pink spotting around day two. This is perfectly normal.
By day five, most women feel completely normal and can resume all regular activities. I advise using a high-quality, water-based lubricant the first time you resume intimacy to protect the newly healing tissue.
Clinical Evidence: What the Research Shows
As a medical specialist, I rely heavily on empirical data. Peer-reviewed science drives my clinical decisions. The body of evidence supporting vaginal laser therapy is extensive and growing every year.
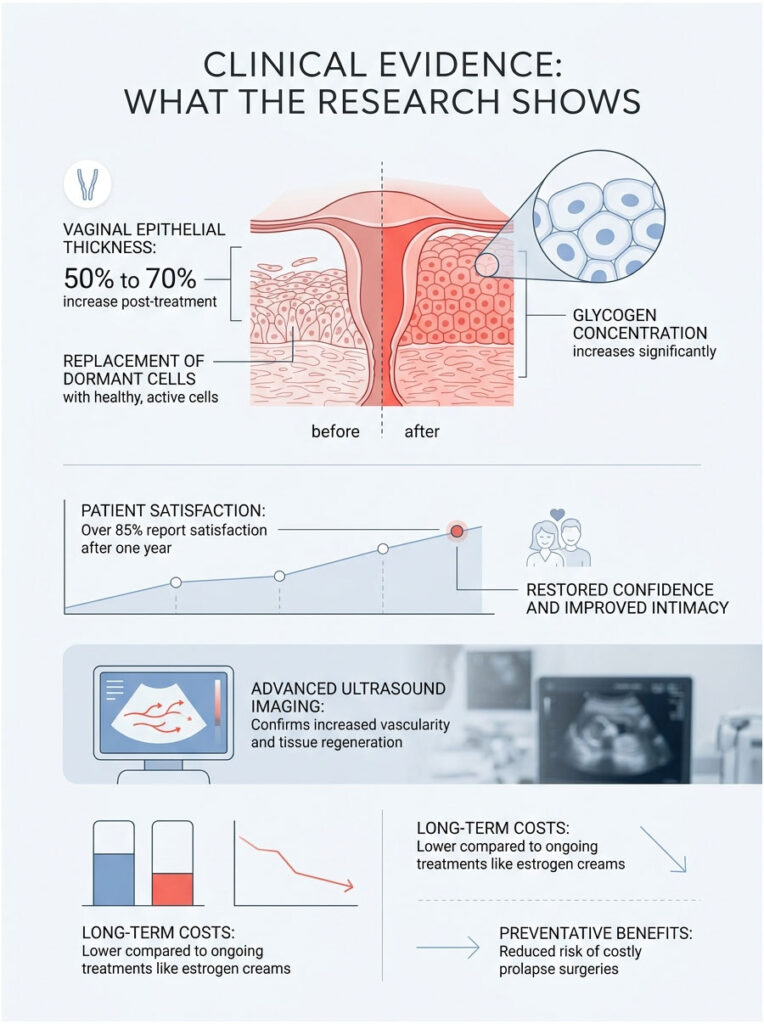
Histological Evidence from Tissue Biopsies
Researchers have taken tiny biopsies of the vaginal wall before treatment and again three months after the final session. The findings under a high-powered microscope are compelling.
Studies consistently show a 50% to 70% increase in overall vaginal epithelial thickness. Dormant, flat cells are completely replaced by plump, active, healthy cells. Glycogen concentration increases dramatically. Advanced ultrasound imaging also confirms increased vascularity in the pelvic region, proving genuine tissue regeneration rather than temporary swelling from heat.
Patient Satisfaction Data
Multi-center studies evaluating devices like MonaLisa Touch and Fotona Smooth show remarkably similar results. Over 85% of treated patients report being satisfied or very satisfied with their functional outcomes at the one-year mark.
Women frequently describe a renewed sense of confidence and the joyful return of spontaneous intimacy without excessive lubricants. For breast cancer survivors seeking non-hormonal menopause relief, these treatments are routinely described as life-changing.
Long-Term Cost-Benefit Analysis
The upfront cost of laser therapy can seem significant. But consider the long-term picture. Purchasing premium estrogen creams, specialized lubricants, and antibiotics for recurrent UTIs adds up substantially over five years.
Laser therapy requires a larger initial investment, but maintenance costs are very low. When you factor in eliminated copays for recurrent UTI visits, the financial gap narrows considerably. More importantly, restoring structural integrity now can help prevent costly and invasive prolapse surgeries later. Preventative regenerative medicine is the smarter financial and medical choice.
Final Verdict: Are Laser Treatments Effective for Female Sexual Health?
The answer, backed by extensive clinical data and real-world histological outcomes, is a clear yes. Whether you and your doctor choose a Fractional CO2 laser or an Erbium laser, the biological process of neocollagenesis works to restore your tissue.

These devices successfully reverse the progressive damage caused by Genitourinary Syndrome of Menopause. They offer lasting relief from painful intercourse, restore natural moisture and acidity, and provide a critical avenue for non-hormonal menopause relief, especially for breast cancer survivors who cannot use estrogen.
However, you must respect the power of these medical devices. Understand the FDA safety communications for vaginal lasers and why they were issued. Protect yourself by seeking treatment exclusively from board-certified urogynecologists or highly specialized gynecologists.
When performed correctly by an expert, vaginal atrophy treatment with a laser can safely and effectively restore your quality of life. Do not let embarrassment keep you from seeking the care you deserve. The evidence is clear: laser treatments are a transformative tool in modern gynecology.
Frequently Asked Questions
Are laser treatments truly effective for improving female sexual health?
Yes, clinical evidence and histological data confirm that laser treatments are highly effective for female sexual health. By utilizing controlled thermal energy, these devices stimulate neocollagenesis and angiogenesis, which restores the structural integrity of the vaginal wall. This process effectively reverses symptoms of Genitourinary Syndrome of Menopause (GSM), such as dryness and loss of elasticity, leading to improved comfort and sexual function.
How do Fractional CO2 lasers and Erbium lasers actually regenerate vaginal tissue?
Both technologies rely on the principle of controlled thermal micro-trauma. The laser energy targets the lamina propria, activating fibroblasts—the ‘factories’ responsible for producing collagen and elastin. This triggers a healing cascade that thickens the vaginal epithelium and increases blood flow (angiogenesis), transforming thin, fragile tissue into a robust, glycogen-rich environment similar to pre-menopausal states.
What is the primary difference between the MonaLisa Touch and Fotona Smooth systems?
The MonaLisa Touch uses a Fractional CO2 laser (10,600 nm) which is ablative, meaning it vaporizes tiny columns of tissue to trigger deep remodeling. The Fotona Smooth uses an Erbium:YAG laser (2,940 nm) which is non-ablative, providing gentle photothermal heating without breaking the surface. CO2 lasers are often preferred for severe atrophy and Lichen Sclerosus, while Erbium lasers are excellent for mild laxity and moisture restoration with minimal downtime.
Can laser therapy provide relief from dyspareunia (painful intercourse)?
Absolutely. Dyspareunia in postmenopausal women is primarily caused by the thinning of the vaginal mucosa and a lack of lubrication. Laser therapy restores the tissue’s natural rugae (folds) and elasticity while stimulating the production of moisture. By thickening the vaginal walls, the treatment prevents the micro-tears and friction that cause pain, allowing women to resume intimacy comfortably.
Is vaginal laser therapy a safe alternative for women who cannot use estrogen creams?
Laser therapy is an ideal non-hormonal alternative for women who are contraindicated for estrogen, such as those with a history of blood clots or hormone-sensitive cancers. Unlike localized estrogen, which carries a small risk of systemic absorption, energy-based therapies are 100% chemical-free and rely entirely on the body’s natural regenerative processes to heal the tissue.
Why is laser treatment considered a ‘lifeline’ for breast cancer survivors?
Breast cancer survivors often suffer from severe vaginal atrophy due to aromatase inhibitors, which aggressively block estrogen. Since oncologists typically prohibit the use of hormonal creams for these patients, laser therapy offers the only evidence-based medical solution to restore pelvic health and alleviate the agonizing symptoms of GSM without introducing hormones into the bloodstream.
What did the 2018 FDA safety communication regarding vaginal lasers actually mean?
The FDA issued a warning against the deceptive marketing of ‘vaginal rejuvenation’ for purely cosmetic purposes by unqualified practitioners. However, the FDA did not invalidate the clinical efficacy of these lasers for treating medical conditions like vaginal atrophy or GSM. The communication was a call for transparency and a warning against using these powerful surgical tools without proper medical oversight.
Can these laser treatments help with stress urinary incontinence (SUI)?
Yes. By targeting the anterior vaginal wall, the laser stimulates collagen production that provides firmer support for the urethra and bladder neck. This increased structural integrity acts as a mechanical ‘backboard,’ allowing the urethra to compress more effectively during physical strain (like coughing or sneezing), which significantly reduces or eliminates involuntary urine leakage.
How many sessions are typically required to see results for vaginal atrophy?
The standard clinical protocol requires three initial sessions spaced approximately four to six weeks apart. This timeline is essential because biological neocollagenesis is a gradual process. While some patients notice improvement after the first session, the full three-session cycle is necessary to solidify the structural changes and ensure long-lasting relief from symptoms.
What is the expected recovery and ‘pelvic rest’ period after a procedure?
Recovery is generally mild, but we mandate a period of ‘pelvic rest’ for three to five days post-treatment. During this time, patients must avoid intercourse, tampons, hot tubs, and intense exercise. This allows the micro-injuries in the vaginal epithelium to heal without irritation. Most women return to their full normal activities within a week.
Are there any specific medical contraindications for vaginal laser therapy?
Yes, laser therapy should not be performed on patients with active pelvic or vaginal infections, undiagnosed vaginal bleeding, or a history of recent pelvic radiation. A thorough pre-treatment screening, including a normal Pap smear and a physical exam by a urogynecologist, is mandatory to ensure the procedure is safe for the patient’s specific anatomy.
Why should I choose a board-certified urogynecologist over a medical spa for this treatment?
Internal pelvic lasers are powerful medical devices that require an intimate understanding of pelvic floor anatomy. A urogynecologist can perform a comprehensive diagnostic exam to rule out underlying pathologies, adjust energy settings based on tissue thickness, and manage complex cases. Medical spas often lack the clinical expertise to differentiate between simple atrophy and more serious conditions like prolapse or precancerous lesions.
Disclaimer
This article is for informational purposes only and does not constitute official medical advice, diagnosis, or treatment. The use of energy-based devices for vaginal health should only be performed by board-certified medical professionals. Always consult with your doctor or a qualified urogynecologist to discuss your specific medical history and determine if laser therapy is a safe and appropriate option for your unique health needs.
References
- North American Menopause Society (NAMS) – menopause.org – 2022 Position Statement on the management of Genitourinary Syndrome of Menopause (GSM).
- American College of Obstetricians and Gynecologists (ACOG) – acog.org – Clinical guidelines regarding the use of fractional CO2 laser for vulvovaginal atrophy.
- U.S. Food and Drug Administration (FDA) – fda.gov – 2018 Safety Communication regarding the marketing of energy-based devices for “vaginal rejuvenation.”
- Journal of Minimally Invasive Gynecology – jmig.org – Peer-reviewed study on the long-term efficacy of Fractional CO2 lasers in postmenopausal women.
- International Urogynecological Association (IUUA) – iuga.org – Patient education resources on non-hormonal treatments for pelvic floor dysfunction and atrophy.
- PubMed Central (National Institutes of Health) – ncbi.nlm.nih.gov – Histological analysis of vaginal tissue remodeling following Erbium:YAG laser treatment.