You ran your tongue across your lower lip and found something that wasn’t there yesterday. A small, pale, stubborn bump. Before the mind sprints to worst-case scenarios, here’s the math: roughly 1 in 10 US adults gets these in any given year, and somewhere north of 95 percent of them are harmless. The faster you figure out which of five common conditions you’re looking at, the faster you can pick the right 14-day fix and the small set of warning signs that mean a dentist needs to take a look this week.
Table of Contents
Quick Answer: Most white bumps inside the lip are harmless mucoceles, canker sores, Fordyce spots, cold sores, or mild oral thrush that clear up in 7 to 14 days. Rinse with warm saltwater three times a day, switch to a soft-bristle toothbrush, skip spicy and acidic foods, and apply an OTC oral gel like Orajel or Kanka for pain. See a dentist if the bump lasts longer than two weeks, bleeds, hardens at the edges, or causes numbness.

At a Glance
- 5 conditions cause about 90 percent of white bumps inside the lip
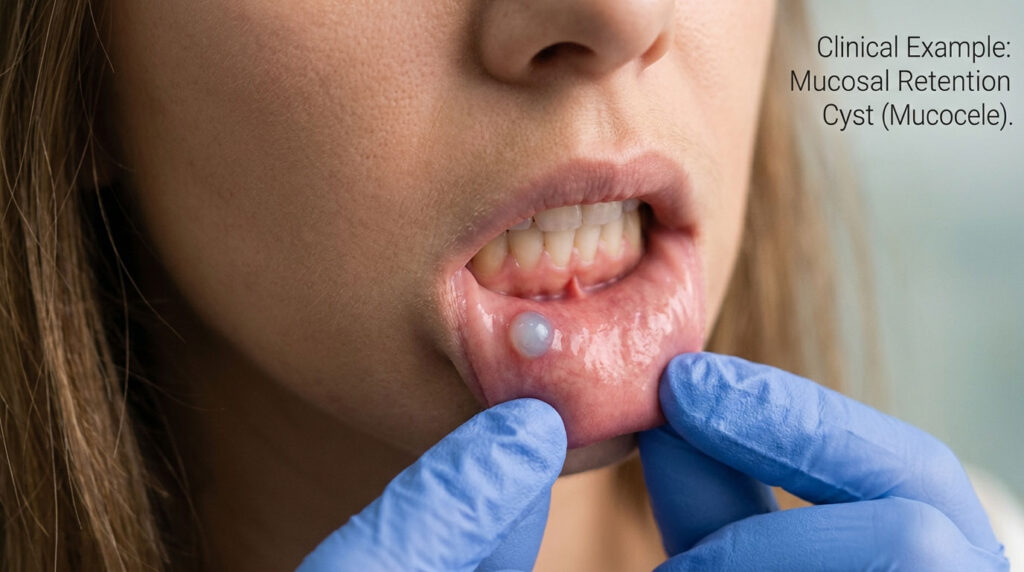
- Painless, dome-shaped, bluish-white bumps are usually mucoceles from a lip bite
- Painful, yellow-centered ulcers with a red ring are canker sores
- Warm saltwater rinses and benzocaine gels speed healing for most cases
- A bump lasting longer than 2 weeks needs a dentist visit, no exceptions
- Popping a mucocele almost always causes it to refill within days
- Most cases cost under $20 to treat at home; in-office removal runs $200 to $600
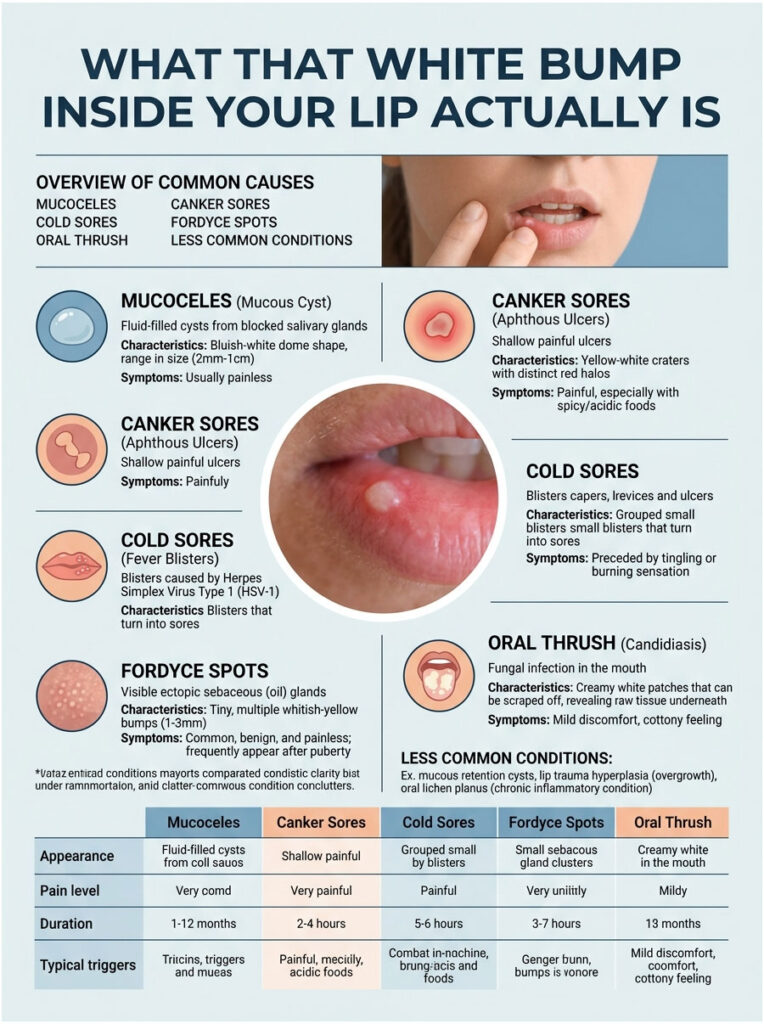
What That White Bump Inside Your Lip Actually Is
Lips are thin, vascular, and constantly moving. They take more daily abuse than almost any other patch of skin on the body. So when a bump appears, the cause is nearly always mechanical irritation, a low-grade infection, or a normal anatomical feature that finally caught your attention.
Patients booking dental consultations through HealthCareOnTime usually walk in worried about the worst diagnosis, and walk out with one of five textbook conditions. Pinpointing which one you’ve got is half the battle.
The Five Most Common Causes
Mucoceles are fluid-filled cysts that show up when a tiny salivary gland in the lip gets pinched or bitten. The Cleveland Clinic puts the prevalence at about 2.4 per 1,000 people, with roughly 70 percent of cases occurring between ages 10 and 20. They look bluish-white, feel soft, and rarely hurt.
Canker sores (medically, aphthous ulcers) are small, painful, yellow-white craters with a red halo. The American Academy of Oral Medicine reports more than half the US population gets them at some point. They sting when you eat citrus, soda, or anything spicy.
Cold sores start as a tingle, blister within a day, and are caused by herpes simplex virus type 1. The National Institute of Dental and Craniofacial Research estimates nearly 90 percent of US adults carry HSV-1, even though only a fraction ever show symptoms. Cold sores prefer the lip border but can sneak just inside the lip.
Fordyce spots are tiny, pinhead-sized, pale yellow or white sebaceous glands. They’ve been on the lips since birth, just got more visible after puberty. A person can have one or a hundred. None of them need treatment.
Oral thrush shows up as creamy white patches that scrape off, revealing a red base. The cause is an overgrowth of Candida albicans yeast, and it tends to appear after antibiotic courses, in denture wearers, in people with diabetes, or in anyone with a weakened immune system.
Less Common but Worth Knowing
Mucous retention cysts are the deeper cousins of mucoceles. Lip trauma hyperplasia is a firm, scar-like bump from chronic cheek-chewing. Oral lichen planus shows up as lacy white streaks and usually needs a dentist’s eye to confirm. Together, these account for under 5 percent of inner-lip bumps in adults.
Table 1: The 5 Most Common White Bumps Inside the Lip, Compared
| Condition | Appearance | Pain Level | Typical Duration | Common Trigger |
| Mucocele | Soft, bluish-white, dome-shaped, 2 to 10 mm | Painless to mild | 3 to 6 weeks | Lip biting, salivary duct trauma |
| Canker Sore | Yellow-white center, red ring, shallow ulcer | Moderate to high | 7 to 14 days | Stress, citrus, SLS toothpaste, minor injury |
| Cold Sore | Cluster of small fluid-filled blisters | Burning, tingling | 7 to 10 days | HSV-1 reactivation, sun, illness |
| Fordyce Spot | Pinhead-sized, pale yellow-white, often grouped | Painless | Permanent (harmless) | Normal anatomy, more visible after puberty |
| Oral Thrush | Creamy white patches that scrape off | Mild burning or none | 1 to 2 weeks with treatment | Antibiotics, dentures, weakened immunity |
How to Tell What Kind of Bump You Have
The good news: you can usually narrow it down at home with three quick questions. Our medical reviewers built this self-ID flow from the diagnostic checklist most US dentists run through in the first 30 seconds of an exam.
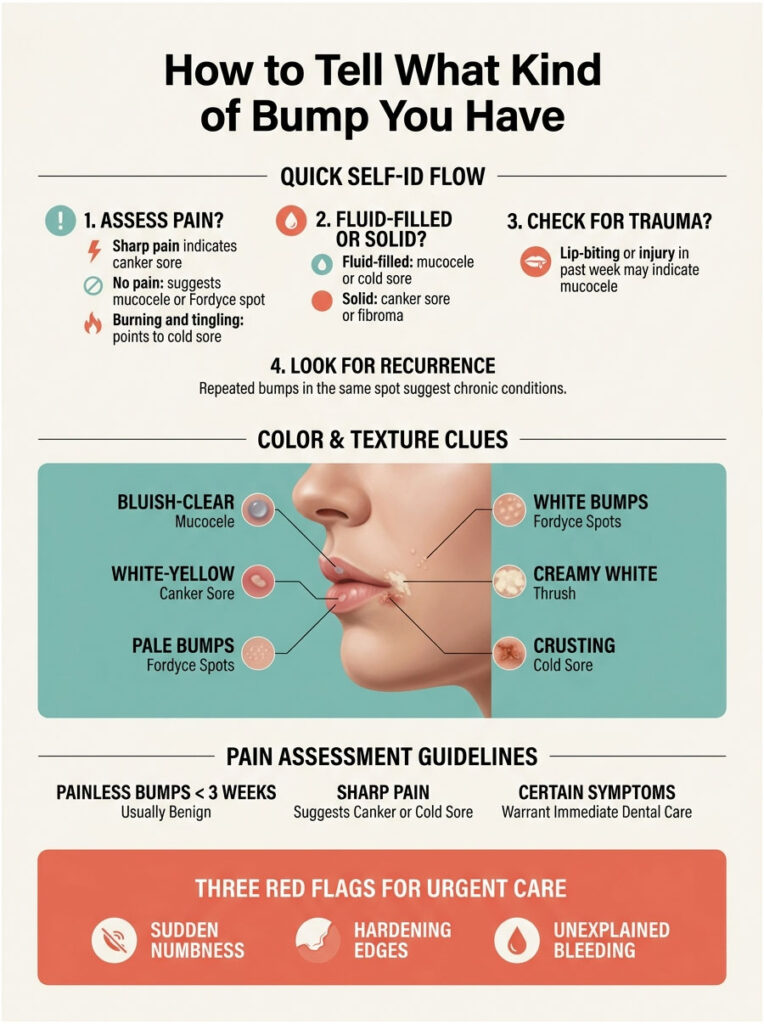
The Self-ID Decision Tree
Step 1, Does it hurt when you press it? A sharp “yes, ouch” points strongly to a canker sore. A “no, it’s just there” leans toward mucocele or Fordyce spot. A “yes, but it also burns and tingles” suggests a cold sore.
Step 2, Is it fluid-filled or solid? Press gently with a clean finger. If the bump feels like a tiny water balloon that shifts under pressure, it’s almost certainly a mucocele or cold sore. If it feels solid or like a raised crater, you’re looking at a canker sore or fibroma.
Step 3, Did you bite your lip, eat something sharp-textured, or take a knock to the mouth in the last week? Trauma within the past 7 days is the giveaway clue for a mucocele. The Cleveland Clinic lists accidental lip-biting during chewing as the single most common trigger.
Step 4, Is this a repeat performer? Recurring bumps in the same exact spot usually mean a chronic mucocele (the salivary duct keeps refilling), nutritional-deficiency-driven canker sores, or cold sores triggered by sun, illness, or stress.
Color and Texture Clues
Bluish-clear and translucent equals mucocele. White-yellow center with a red halo equals canker sore. A row of tiny, near-identical pale bumps equals Fordyce spots. Creamy white patches that wipe off equal thrush. Crusting, blistering, scabbing equals cold sore.
Pain vs. No Pain: What Each Signals
A painless bump under three weeks old is almost always benign. Sharp pain on day one usually means canker sore or cold sore. Sudden numbness around a bump, hardening at the edges, or unexplained bleeding are the three red flags that move a case from “watch and wait” to “see a dentist this week.” In cases reviewed by our oral-health team, those three signs together account for the vast majority of urgent specialist referrals.
At-Home Treatment: The 14-Day Recovery Protocol
Most white bumps inside the lip don’t need a prescription. They need 14 days, basic oral hygiene, and a few smart product picks. Here’s the day-by-day playbook our patient-care team recommends for self-resolving cases.

Day 1 to Day 3: Calm and Protect
The first 72 hours are about reducing inflammation and stopping further irritation. Rinse with warm saltwater (half a teaspoon of salt in 8 ounces of warm tap water) three to four times daily, especially after meals. The Mayo Clinic confirms saltwater rinses calm mouth-ulcer inflammation safely and cheaply.
Swap your toothbrush for a soft-bristle model and drop any toothpaste with sodium lauryl sulfate (SLS). Sensodyne Pronamel and Biotene are two widely available SLS-free options in US drugstores. Skip citrus, vinegar, tomato, soda, hot peppers, and salt-and-vinegar chips for the first three days, and drink through a straw if the bump sits near the lip border.
Day 4 to Day 7: Reduce and Heal
By the middle of the week, pain should be fading and the bump’s color should be lightening. Apply a benzocaine-based oral gel like Orajel or Anbesol two to three times a day for canker-sore pain. Kanka or Zilactin-B forms a thin protective film that keeps food and acid off the bump for several hours.
If you suspect a cold sore, start docosanol cream (Abreva) at the first tingle. The earlier it goes on, the more it can shorten the outbreak. For thrush, an OTC antifungal lozenge or a dentist-prescribed nystatin rinse is the standard route.
Day 8 to Day 14: Monitor and Prevent
By day 8, most mucoceles have either ruptured naturally or noticeably shrunk. Canker sores should be visibly healing, with the yellow center fading and the red ring receding. Keep the saltwater rinses going and the soft-bristle toothbrush in rotation. Start a quick mental log of what foods or habits preceded the bump so you can dodge them next time.
OTC Products That Work in US Drugstores
The pharmacy aisle gets crowded fast, so here are the workhorses our patients reach for repeatedly. Orajel and Anbesol (benzocaine 10 to 20 percent) numb pain on contact. Kanka and Zilactin-B form protective films. Colgate Peroxyl (1.5 percent hydrogen peroxide rinse) cleans and speeds healing. Abreva (docosanol 10 percent) is the only FDA-approved OTC cold-sore antiviral. For thrush, clotrimazole troches sit on shelves at most CVS and Walgreens locations.
What Not to Do
Do not pop a mucocele with a needle or pin. The Cleveland Clinic warns that DIY drainage almost always causes the cyst to refill within days and raises infection risk.
Skip straight alcohol mouthwash on an open canker sore (it stings ferociously and slows healing). Don’t scrape thrush patches (the raw skin underneath becomes a fresh infection site). And don’t share lip balm, drinking glasses, or utensils during an active cold-sore outbreak.
Table 2: USA OTC Treatment Comparison (Average Drugstore Prices, Q1 2026)
| Product | Best For | Average US Price | Key Active Ingredient |
| Orajel Mouth Sore Gel | Canker sores, lip ulcers | $7 to $10 (CVS, Walgreens) | Benzocaine 20% |
| Kanka Mouth Pain Liquid | Canker sores, irritation | $8 to $12 (Walgreens, Amazon) | Benzocaine 20% |
| Zilactin-B Oral Gel | Canker sores (long-lasting) | $9 to $13 (Walmart, Target) | Benzocaine 10% |
| Abreva Cream | Cold sores (HSV-1) | $18 to $22 (CVS, Target) | Docosanol 10% |
| Colgate Peroxyl Rinse | Healing, mild thrush | $7 to $9 (Walgreens, Amazon) | Hydrogen peroxide 1.5% |
| Generic Clotrimazole | Oral thrush | $10 to $15 (Walmart, CVS) | Clotrimazole 10 mg |
Sources: CVS.com, Walgreens.com, Walmart.com.
Why It Probably Isn’t Cancer (but Here’s When to Worry)
The single biggest fear patients booking tests with us name is oral cancer. The numbers offer real reassurance. The American Cancer Society estimates about 59,660 new oral cavity and oropharyngeal cancer cases each year in the US, in a country of 330 million. That works out to under 0.02 percent of Americans receiving the diagnosis annually.
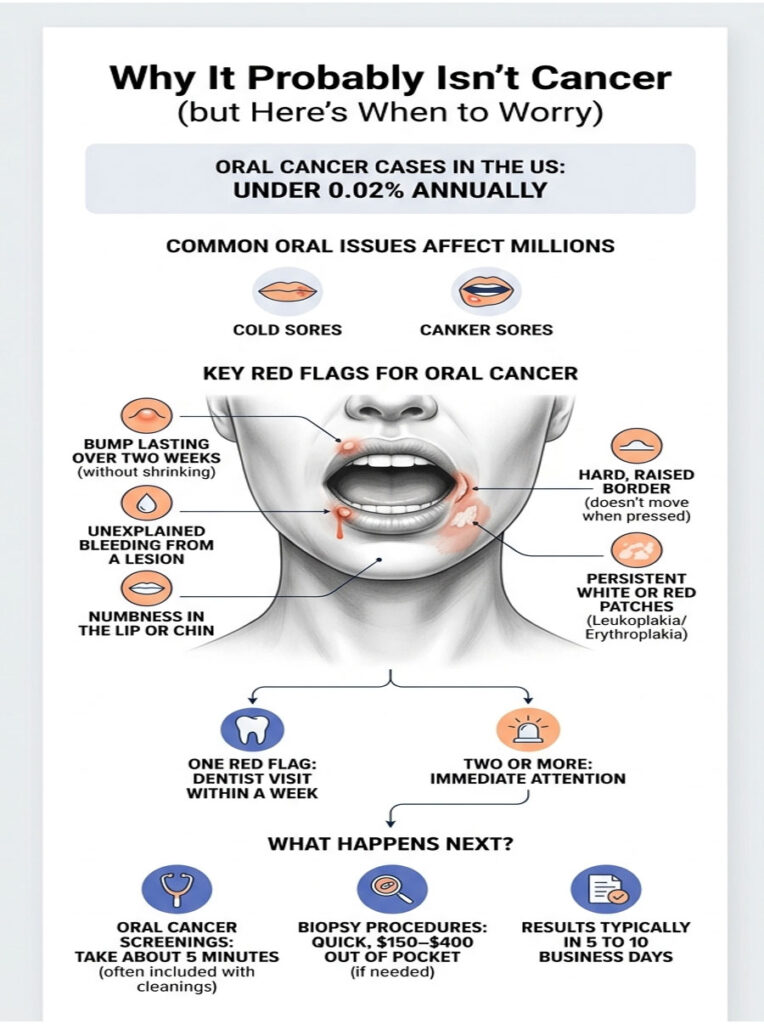
Cold sores, canker sores, and mucoceles, by contrast, affect tens of millions of US adults every year. Statistically, the deck is stacked overwhelmingly toward “benign.”
Oral Cancer Red Flags
That said, the American Dental Association lists clear warning signs worth memorizing. A bump that lasts longer than two weeks without shrinking. Unexplained bleeding from the lesion. Numbness in the lip or chin near the bump. A hard, raised border that doesn’t move when you press it. A white or red patch (called leukoplakia or erythroplakia) that wipes nothing off.
Our medical reviewers note that any single red flag warrants a dentist visit within a week. Two or more together warrant a visit the same week.
What an Oral Cancer Screening Looks Like
A standard screening at a US dental office takes about 5 minutes. The dentist or hygienist visually inspects all surfaces of the mouth, palpates the neck and jaw for lumps, and may use a blue-light scanner (VELscope) or run a brush biopsy if anything looks off. The exam is usually included free with a regular cleaning under most US dental insurance plans.
If a biopsy is needed, it’s an in-office procedure, takes about 10 minutes, and runs roughly $150 to $400 out of pocket. Results come back in 5 to 10 business days.
When to See a Doctor or Dentist (and What It Costs)
In tests and consultations booked through HealthCareOnTime, the majority of “white bump” cases resolve without a clinic visit. The remainder fall into clear red-flag buckets that benefit from a professional eye.

Red Flags Within 24 Hours
Spreading swelling that affects breathing or swallowing. Severe pain that OTC gels can’t dent. Pus drainage with a fever above 100.4°F. Sudden numbness in the lip or chin. Any of these mean call your dentist or visit urgent care today, not tomorrow.
Red Flags Within 2 Weeks
A bump that hasn’t shrunk after 14 days of consistent home care. A recurring mucocele in the same spot more than twice. A canker sore larger than half an inch across. Unexplained weight loss or persistent fatigue alongside the bump. A bump that bleeds when you brush near it.
What the Visit Will Include
A general-dentist visit for a lip bump typically takes 20 to 30 minutes. Expect a visual exam, a gentle palpation of the area and surrounding lymph nodes, and a brief medical-history review. The dentist will usually take an intraoral photo for the chart and may recommend one of four treatments based on what they see.
Treatment Options at the Clinic
Surgical excision is the gold standard for stubborn mucoceles. The cyst and the affected gland come out under local anesthesia, and recovery takes about a week.
Laser ablation uses a focused light beam to vaporize the cyst with minimal bleeding. The Journal of Oral and Maxillofacial Pathology reports laser treatment has lower recurrence rates than scalpel excision in many published studies.
Cryotherapy freezes the cyst with liquid nitrogen. It’s quick, with no cutting, though multiple sessions are sometimes needed.
Intralesional corticosteroid injection shrinks the cyst over 1 to 3 weeks without any cutting at all. It’s a great option for kids and anyone needle-shy about scalpel work.
Cost Range in the USA, With and Without Dental Insurance
A general dentist consult averages $75 to $200 in major US cities. Mucocele excision runs $200 to $600 out of pocket. Laser removal sits at $300 to $800. A biopsy adds $150 to $400. Most US PPO dental insurance plans cover 50 to 80 percent of medically necessary procedures, which can knock the patient share down significantly. HSA and FSA funds usually apply.
Table 3: Decision and Action: What to Do Based on What You See
| Symptom Pattern | Severity | Recommended Action |
| Painless bluish-white bump, under 5 mm, less than 7 days old | Low | Saltwater rinses + soft toothbrush; reassess at day 14 |
| Painful yellow ulcer with red ring, eating uncomfortable | Mild | OTC benzocaine gel (Orajel or Kanka) + SLS-free toothpaste + bland diet |
| Cluster of tingling, blistering bumps near lip border | Mild to moderate | Start Abreva at first tingle; avoid lip contact with others; replace lip balm |
| Bump persists beyond 14 days or recurs in same spot | Moderate | Book a dentist visit within 2 weeks for evaluation |
| Bleeding, numbness, hardening, or rapid growth | High | Dentist or urgent care within 7 days, biopsy may be needed |
| Pus, fever above 100.4°F, swelling affecting swallowing | Urgent | Urgent care or ER same day |
Special Cases: Kids, Pregnancy, Braces, and Recurring Bumps
The general playbook works for most adults, but four groups need slightly different handling.

Bumps in Kids and Toddlers
Children are mucocele magnets. The Cleveland Clinic data shows 70 percent of cases happen between ages 3 and 20, peaking in adolescence. Kids bite their lips, fall on their faces, chew pencils, and play sports. Most cases clear up on their own.
Skip the benzocaine gels for children under 2 (the FDA has flagged a rare but serious risk called methemoglobinemia) and use plain saltwater rinses instead. For older kids, a pediatric dentist’s chair-side reassurance often does more than any product.
Pregnancy-Related Oral Changes
Hormonal shifts during pregnancy can trigger or worsen canker sores and small lip cysts. Most OTC oral gels are safe during pregnancy, but always run new products by the OB-GYN first. Gentle saltwater rinses, hydration, and folate-rich foods (spinach, lentils, fortified cereals) usually handle the issue without medication.
Bumps Caused by Braces, Retainers, or Dentures
A wire, bracket, or ill-fitting denture rubbing the inside of the lip creates tiny but constant trauma that often produces a recurring mucocele or canker sore. Orthodontic wax over the offending wire (free from any orthodontist) usually fixes the trigger within a day or two. For dentures, a quick reline appointment is the durable fix.
Recurring Mucoceles and What They Mean
A mucocele that comes back in the same exact spot three or more times usually has a damaged salivary duct that won’t heal on its own. Patients booking dental consultations with us often resolve recurring mucoceles with a single laser session, and the duct heals shut for good. Surgical removal of the associated gland is the most permanent fix.
How to Prevent White Bumps from Coming Back
A bump that healed is a bump that can return. The five highest-yield prevention habits are stunningly simple, and most cost nothing.

Habit Fixes
Stop chewing pens, fingernails, ice, and the inside of your cheek. If you grind or clench at night, ask a dentist about a $20 OTC night guard from any pharmacy or a custom one through the clinic. Sugar-free gum can occupy a busy mouth and break lip-biting habits, though limit it if you have TMJ pain.
Diet and Nutrition
Recurring canker sores often track with low B12, low iron, or low folate. The National Institutes of Health lists clams, beef liver, fortified breakfast cereals, eggs, and dairy as top US-accessible B12 sources. A standard CBC plus B12, folate, and ferritin panel booked through HealthCareOnTime confirms or rules out deficiency in a single blood draw.
Oral Hygiene Routine
Brush twice a day with a soft-bristle toothbrush and SLS-free toothpaste. Floss once. Rinse with a non-alcoholic mouthwash (Biotene or ACT) at night. Replace the toothbrush every 90 days. After any cold-sore outbreak, swap the toothbrush immediately to avoid reinfecting yourself.
Stress and Sleep Triggers
The American Dental Association flags chronic stress as a top canker-sore trigger. Aim for 7 to 9 hours of sleep, basic daily movement, and one stress-release habit you’ll actually do (walking, journaling, prayer, breath work, whatever sticks).
Frequently Asked Questions
Will a white bump on my inner lip go away on its own?
Yes, the vast majority do. Mucoceles typically resolve in 3 to 6 weeks. Canker sores heal in 7 to 14 days. Cold sores clear in 7 to 10 days. Fordyce spots are permanent but harmless. Only oral thrush and bacterial infections need active treatment to clear. If a bump lasts longer than two weeks without shrinking, see a dentist.
Can I pop a mucocele at home?
No. Popping a mucocele with a pin, needle, or tweezers almost always backfires. The Cleveland Clinic confirms the cyst typically refills within days, the rupture introduces bacteria, and you risk scarring or infection. Wait for natural resolution or have a dentist remove it cleanly with laser or excision.
How long does it take for a canker sore to heal?
Minor canker sores (under 1 cm) heal in 7 to 14 days. Major canker sores (over 1 cm) can take 2 to 6 weeks and may leave a small scar. Herpetiform canker sores, the rare clustered type, heal in about 7 to 10 days. OTC benzocaine gels speed pain relief but don’t shorten the underlying healing timeline significantly.
Is a painless white bump inside my lip ever dangerous?
Painless bumps are usually safer than painful ones, but not always. Early-stage oral cancer is often painless in its first weeks. If a painless bump has lasted longer than two weeks, has hardened edges, bleeds when touched, or causes numbness in the surrounding tissue, book a dentist evaluation. Most cases turn out benign, but the screening takes five minutes.
What’s the fastest home remedy for a white bump inside the lip?
Warm saltwater rinses three times daily, plus a benzocaine gel like Orajel or Kanka for pain, give the fastest visible improvement within 48 hours. Cold compresses outside the lip reduce swelling. Skip acidic foods (citrus, tomato, vinegar) and SLS toothpastes. Most bumps shrink noticeably by day 3 with consistent care.
Why do I keep getting white bumps in the same spot?
Recurring bumps usually mean an unresolved trigger. Common culprits: a sharp tooth edge, ill-fitting filling, orthodontic bracket, denture rub, persistent lip-biting habit, or chronic nutritional deficiency. A dental exam can identify mechanical triggers in minutes. Blood work checks B12, iron, and folate. Fixing the root cause prevents the cycle.
Can stress cause a white bump inside the lip?
Yes, particularly canker sores. The American Dental Association lists psychological stress as one of the top documented triggers, alongside lack of sleep, hormonal changes, and food sensitivities. Stress also reactivates dormant herpes simplex virus, triggering cold sores. Managing sleep, hydration, and daily stress reduces frequency for most chronic sufferers.
Are white bumps inside the lip contagious?
Only cold sores. Mucoceles, canker sores, Fordyce spots, and most thrush cases are not contagious. Cold sores spread through saliva contact (kissing, sharing utensils, shared lip balm) and shed virus even without visible blisters. During an active outbreak, avoid close contact with infants, immunocompromised people, and anyone with active eczema.
What’s the difference between a canker sore and a mucocele?
Canker sores are painful, shallow, yellow-white ulcers with a red border, usually under 1 cm, that sting when you eat. Mucoceles are painless, soft, bluish-white domes filled with saliva, usually on the lower lip after a bite. Canker sores heal in 1 to 2 weeks; mucoceles take 3 to 6 weeks. Different causes, different treatments.
Can vitamin deficiency cause white bumps in the mouth?
Yes. B12, iron, folate, and zinc deficiencies are well-documented triggers for recurrent canker sores. The NIH Office of Dietary Supplements notes vegetarians, vegans, older adults, and people on metformin or proton-pump inhibitors carry higher B12 deficiency risk. A simple blood panel through HealthCareOnTime confirms the gap, and most cases respond to oral supplementation within 8 to 12 weeks.
Should I use mouthwash on a white bump?
Yes, but choose carefully. Alcohol-based mouthwashes (most original Listerine variants) sting and slow healing on open canker sores. Better choices include Colgate Peroxyl (a 1.5 percent hydrogen peroxide rinse formulated for mouth sores), Biotene, or plain saltwater. Use after meals and at bedtime for the first week.
What does early oral cancer actually look like?
Early oral cancer often appears as a flat white patch (leukoplakia), a red patch (erythroplakia), or a small painless lump with hard edges that doesn’t heal within two weeks. It may bleed easily, feel firm to the touch, or cause numbness in the surrounding tissue. The American Cancer Society recommends an annual oral cancer screening at every dental cleaning, especially for tobacco or heavy alcohol users.
Medical Disclaimer: This article is for educational purposes only and is not a substitute for professional medical or dental advice, diagnosis, or treatment. Always consult a qualified healthcare provider regarding any oral health concerns. HealthCareOnTime does not provide diagnostic services through this content. If you experience severe pain, bleeding, swelling that affects breathing or swallowing, or symptoms lasting longer than two weeks, contact a dentist or physician promptly.
References
- Cleveland Clinic: Oral Mucocele
- National Institute of Dental and Craniofacial Research: Fever Blisters & Canker Sores
- Mayo Clinic: Canker Sore
- American Cancer Society: Key Statistics for Oral Cavity and Oropharyngeal Cancers
- American Dental Association: Oral and Maxillofacial Cancer
- Healthline: White Bumps on Lips: Causes, Treatments, and More
- Colgate: Mucoceles and How To Treat Them
- Ohio State Health: What is this white bump on my lip?
- American Academy of Oral Medicine: Canker Sores
- PubMed Central: Nonsurgical Management of Oral Mucocele
- NIH Office of Dietary Supplements: Vitamin B12 Fact Sheet
- HealthPartners: How to know if it’s a cold sore or something else