Every week, patients walk into my clinic describing the same frustrating scenario. They eat what looks like a perfectly healthy high-protein breakfast, and within an hour, they’re running to the bathroom. Eventually, they ask the question on everyone’s mind: can eggs cause diarrhea?
Table of Contents
The honest answer is yes. Eggs can absolutely trigger digestive distress, and there are several medical reasons why this happens.
Eggs often get labeled as a nutritional powerhouse, and for many people, they truly are. But in the human gut, eggs also behave like a complex biological trigger. They rank among the top food allergens globally, they carry one of the most common bacterial pathogens in food, and they deliver dense proteins that can easily disturb an already sensitive digestive system.
In this guide, I’ll break down exactly how egg proteins interact with your intestinal lining. We’ll look at the difference between a serious immune reaction and a simple food intolerance, and you’ll learn how to identify what’s actually causing your symptoms. Based on what I see in clinical practice every day, understanding these mechanisms is the first real step toward fixing your gut health.
Quick Answer
Yes, eggs can cause diarrhea through several different biological pathways. The most common causes include an overactive gastrocolic reflex triggered by fat content, egg intolerance, an IgE-mediated allergy, bile acid malabsorption, or a bacterial infection like Salmonella enteritidis. The correct treatment depends entirely on identifying your specific trigger, which usually requires either a structured elimination diet or targeted medical testing.
Key Statistics and Clinical Data
- More than 2.5 million Americans live with some form of egg allergy or severe sensitivity (Food Allergy Research & Education, 2023).
- Salmonella enteritidis causes roughly 1.35 million infections and 26,500 hospitalizations in the United States every year (CDC, 2023).
- Adult-onset food intolerances have climbed nearly 20% over the past decade across all age groups.
- The gastrocolic reflex is hypersensitive in up to 60% of patients with Irritable Bowel Syndrome.
- Because of ovomucoid’s heat resistance, up to 70% of egg-allergic patients still react to baked egg products.
- Bile acid malabsorption accounts for almost 30% of chronic diarrhea cases linked to high-fat foods like egg yolks.
- Histamine intolerance affects roughly 1 to 3% of the population, making these individuals highly sensitive to egg whites.
How Your Body Actually Digests Eggs
To understand why a simple breakfast food can wreck your morning, we need to look at how your body processes complex proteins. Digestion isn’t a passive event. It’s a chemically demanding process that requires precise coordination between your stomach, pancreas, liver, and intestines. When any part of that system underperforms, the fallout shows up in your bathroom.

The process starts in the stomach, where hydrochloric acid and pepsin begin breaking down the tightly bound egg proteins. If your stomach acid is low, those proteins move into the small intestine largely intact. That single early failure sets off a chain reaction of digestive problems downstream.
Egg Proteins and Intestinal Permeability
Eggs contain dense protein structures that demand serious enzymatic activity to break down properly. When your digestive system doesn’t produce enough of those specific enzymes, undigested proteins pass straight into the lower intestine. We call this egg protein malabsorption, and it’s one of the main drivers of chronic morning bowel urgency.
Malabsorption pulls extra water into the colon through osmosis. As a result, patients end up with rapid, watery stools shortly after eating. The colon simply can’t handle the sudden flood of undigested matter and fluid.
If your intestinal lining is already compromised, often called leaky gut, those undigested proteins slip directly into the bloodstream. Your immune system then attacks them, creating inflammation that makes future meals even harder to digest.
Ovomucoid and the Heat Resistance Problem
Most patients assume that cooking eggs thoroughly neutralizes any digestive threat. This is one of the most common misconceptions I see in clinical practice, and it keeps a lot of people stuck in a cycle of symptoms.
Egg whites contain a specific protein called ovomucoid. What makes it so problematic for sensitive people is its unique ability to withstand heat. Even after hard-boiling, frying, or baking at high temperatures, ovomucoid’s molecular structure stays intact.
It doesn’t denature the way most proteins do. That means it keeps its full ability to trigger an immune response in your gut. This is why patients who switch from sunny-side-up eggs to hard-boiled eggs rarely see any real improvement. The protein survives the heat, reaches the digestive tract, and continues to cause cramping and loose stools.
Sulfur-Reducing Bacteria and Your Gut Microbiome
Eggs are loaded with sulfur-containing amino acids like methionine and cysteine. In a balanced gut, these get absorbed efficiently in the small intestine. But in patients with dysbiosis, the story plays out very differently.
When sulfur-containing proteins reach the colon undigested, opportunistic sulfur-reducing bacteria start fermenting them. This fermentation releases hydrogen sulfide gas, which is toxic to the intestinal lining in large amounts.
That toxic gas speeds up colonic transit by irritating the smooth muscle of the bowel. The end result is urgent, watery stools paired with severe, foul-smelling bloating. Managing this usually requires a temporary low-sulfur diet along with targeted antimicrobial support.
Expert Insight: If your diarrhea comes with distinctly sulfur-smelling gas, you’re likely dealing with an overgrowth of sulfur-reducing bacteria like Desulfovibrio. A hydrogen sulfide breath test can confirm this specific type of bacterial imbalance.
The Five Main Ways Eggs Cause Diarrhea
When a patient sits down in my clinic, I immediately start sorting their symptoms into clinical categories. You can’t treat an allergy with antibiotics, and you can’t treat an infection with an elimination diet. Getting the diagnosis right is everything.
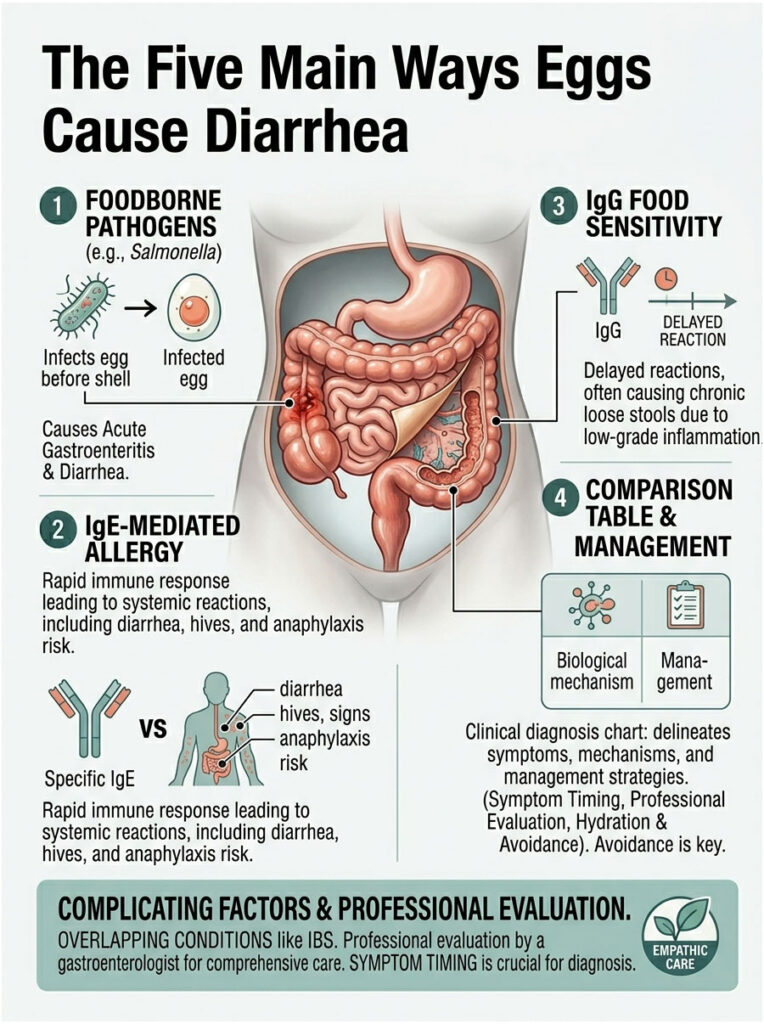
The timeline of your symptoms is the single most valuable clue. The number of minutes or hours between your breakfast and your bathroom visit tells me exactly which part of your system is malfunctioning. Here are the five pathways I investigate first.
1. Foodborne Pathogens and Bacterial Contamination
Even with modern sanitation and agricultural standards, eggs remain one of the most common sources of Salmonella enteritidis. Unlike surface contamination that can be washed off, this pathogen infects the ovaries of healthy hens. The egg is already contaminated internally before the shell ever forms.
Salmonella infection causes acute bacterial gastroenteritis. Symptoms include explosive watery diarrhea, fever, chills, and sharp abdominal cramping. These usually appear anywhere between 6 and 72 hours after eating.
If you suspect Salmonella, your first priority is oral hydration. Avoid over-the-counter anti-diarrheal medications because they trap the bacteria inside your intestinal tract and make things worse. If your fever lasts longer than 24 hours, seek medical care immediately.
2. IgE-Mediated Egg Allergy
A true egg allergy involves rapid deployment of Immunoglobulin E (IgE) antibodies. In this situation, the immune system misidentifies harmless egg proteins as dangerous invaders, which triggers a massive histamine release throughout the body.
Symptoms of an egg allergy include diarrhea, but the digestive issue is rarely isolated. You’ll usually see systemic reactions happening at the same time, including hives, facial swelling, vomiting, or wheezing.
Because these reactions can escalate to anaphylaxis within minutes, strict avoidance is non-negotiable. Patients with a confirmed IgE allergy need to carry an epinephrine auto-injector at all times.
3. IgG Food Sensitivity and Delayed Intolerance
IgG sensitivity is a delayed, non-allergic hypersensitivity. We usually refer to this as a classic egg intolerance. Symptoms can take up to 48 hours to appear, which makes it incredibly hard for patients to connect the dots.
The delay happens because IgG antibodies create low-grade inflammation in the mucosal lining of the gut over time. This chronic inflammation slowly impairs fluid absorption, leading to ongoing loose stools. Egg intolerance often shows up alongside brain fog, joint pain, and afternoon bloating.
Because the reaction is delayed, many patients blame their lunch or dinner for what was actually triggered by breakfast the day before. A properly structured elimination diet is really the only reliable way to uncover this sensitivity.
Clinical Differential Diagnosis Table
To help you make sense of your symptoms, here’s a clinical diagnosis chart that breaks down the biological mechanisms and timelines for each type of egg-related distress.
| Condition Category | Primary Biological Mechanism | Onset of Symptoms | Accompanying Symptoms | Clinical Management Strategy |
|---|---|---|---|---|
| Bacterial Infection | Salmonella enteritidis invasion | 6 to 72 hours | Fever, chills, severe cramping, nausea | Oral rehydration, rest, medical evaluation if fever persists |
| IgE Egg Allergy | Rapid histamine release from immune system | Minutes to 2 hours | Hives, facial swelling, wheezing, vomiting | Strict avoidance, epinephrine, antihistamines |
| IgG Sensitivity | Delayed mucosal inflammation and malabsorption | 12 to 48 hours | Bloating, chronic loose stools, brain fog | 21-day elimination diet, gut microbiome support |
| IBS / Functional | Gastrocolic reflex hyperactivation | 15 to 60 minutes | Urgency, cramping relieved by defecation | Portion control, managing fat intake, stress reduction |
| Bile Acid Malabsorption | Excess bile dumping into colon from high fat | 1 to 3 hours | Bright yellow stools, burning, severe urgency | Bile acid sequestrants, low-fat diet, gallbladder check |
Overlapping conditions are common in clinical practice. A patient might have mild IBS and also carry a low-grade IgG sensitivity. That’s exactly why working with a skilled gastroenterologist matters so much for long-term recovery.
IBS and the Gastrocolic Reflex
For many frustrated patients, the real problem isn’t an allergy or intolerance at all. It’s the physical mechanics of digestion. If you have diarrhea-predominant Irritable Bowel Syndrome (IBS-D), your nervous system is probably hyper-reactive to dietary fat.
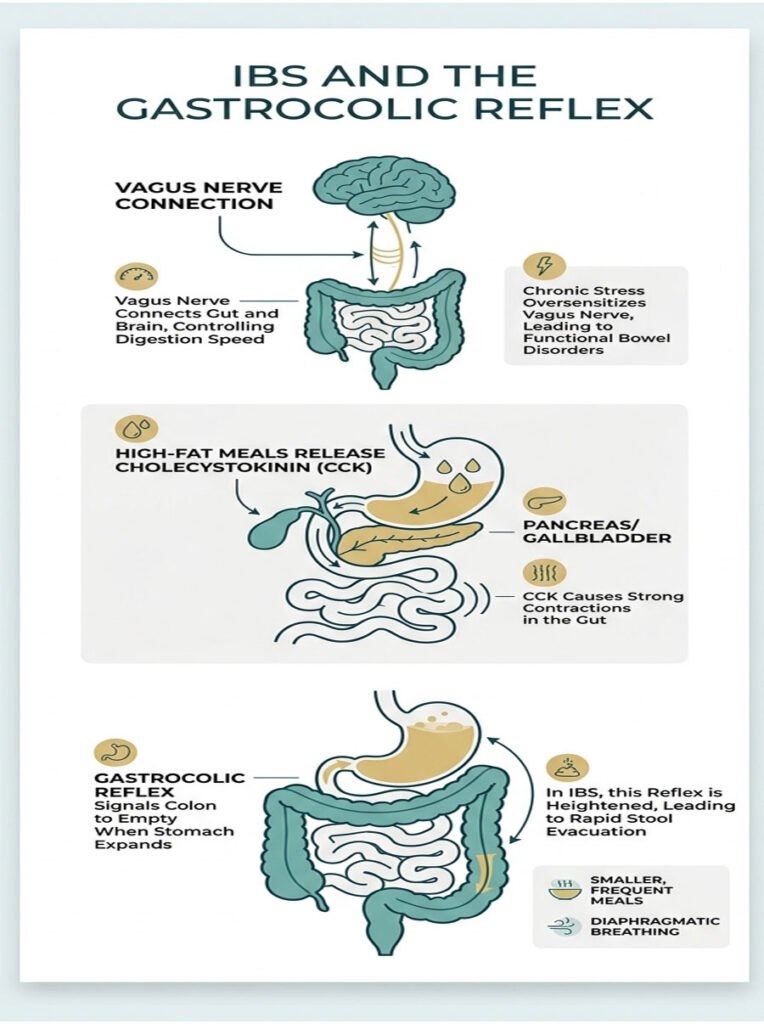
Your gut and brain communicate through the vagus nerve, which controls how fast your digestion moves. When this nerve becomes oversensitive from chronic stress or past infections, it reads normal food signals as emergencies. This miscommunication is what creates functional bowel disorders.
Why High-Fat Breakfasts Trigger IBS
Eggs are naturally high in fat and dense in protein. Eating a heavy, fat-rich meal first thing in the morning triggers the release of a hormone called cholecystokinin (CCK). This hormone tells your gallbladder and intestines to contract strongly to start digestion.
For someone with IBS, this is a textbook trigger. The sudden fat load overstimulates an already sensitive digestive tract. Your intestines start spasming, transit time speeds up, and urgency hits hard.
If you’re managing IBS, portion control matters. Three large eggs cooked in butter is a guaranteed disaster. Dropping to a single egg and cooking without added fats can sometimes ease the hormonal response enough to make breakfast tolerable again.
Understanding the Hypersensitive Gastrocolic Reflex
The gastrocolic reflex is a normal physiological response where stomach expansion signals your colon to empty. When food enters your stomach, your brain essentially tells your colon to make room for what’s coming.
In IBS patients, this reflex is cranked up way too high. Eating a dense protein like eggs triggers violent contractions in the lower gut. Stool gets pushed out rapidly before your colon has time to absorb water properly.
If you’re running to the bathroom within 20 minutes of eating, an overactive gastrocolic reflex is probably the cause. The food in the toilet isn’t the food you just ate. Your colon is actually evacuating yesterday’s meal under pressure from today’s breakfast.
To calm this reflex, I usually recommend smaller, more frequent meals. Diaphragmatic breathing before eating can also help downregulate your nervous system and settle the gut.
Bile Acid Malabsorption: The Hidden Gallbladder Link
There’s another important pathway to discuss, and most patients have never heard of it. If you’ve ever experienced bright yellow, burning diarrhea after eating eggs, pay close attention to this section.

Bile is a digestive fluid made by your liver and stored in your gallbladder. Its job is to break down dietary fats, the way dish soap cuts through grease. Since egg yolks are rich in fat, they demand a significant amount of bile for proper digestion.
When you eat an egg, your gallbladder contracts and releases bile into the small intestine. In a healthy system, that bile does its job and gets reabsorbed at the end of the small intestine. But for some people, that recycling system breaks down.
The Laxative Effect of Excess Bile
When the small intestine fails to reabsorb bile, the fluid continues into the large intestine. The colon isn’t designed to handle raw bile acids. In fact, bile acts as a powerful, highly irritating laxative when it touches the colonic lining.
This condition is called Bile Acid Malabsorption (BAM). The colon responds by flushing water to get rid of the irritant, which creates explosive, urgent diarrhea one to three hours after a fatty meal.
Patients who’ve had their gallbladder removed (cholecystectomy) are at especially high risk. Without a gallbladder to store bile, the fluid drips continuously into the digestive tract. Adding a fatty egg meal on top of that easily overwhelms the system.
Why You’re Suddenly Reacting to Eggs as an Adult
One of the most emotional questions I hear goes something like this: “I’ve eaten eggs my entire life. Why am I suddenly sick?” It’s a fair question. The human body is dynamic, and your baseline immune tolerance can change dramatically over the years.
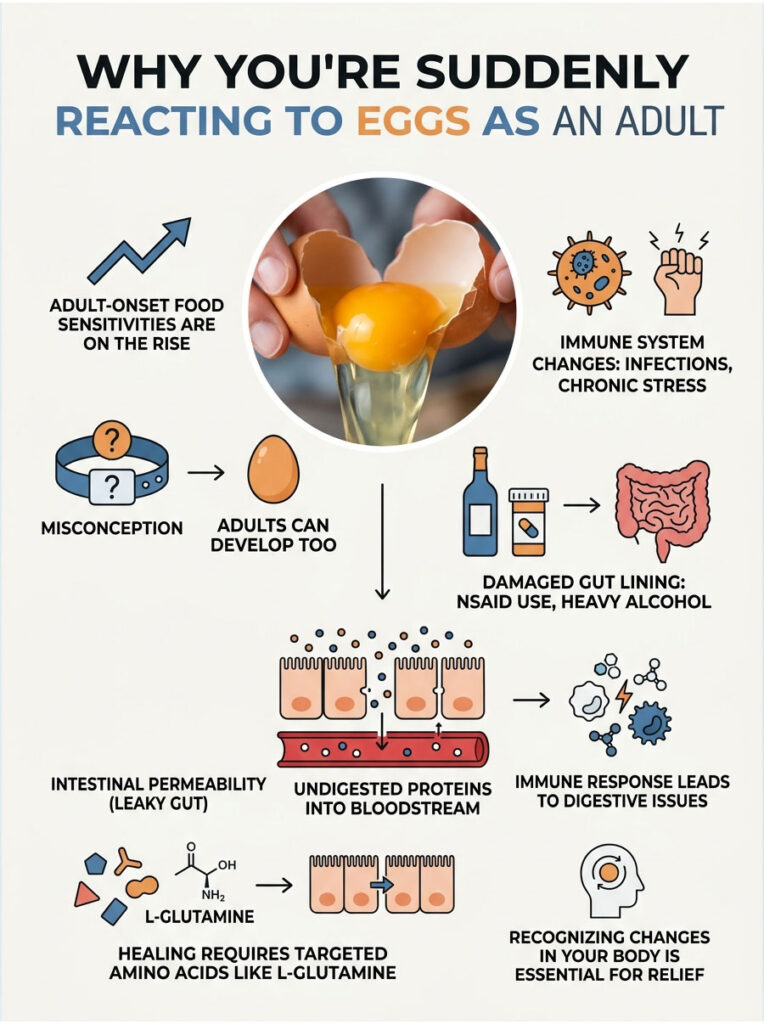
Adult-onset food sensitivities are rising quickly across the United States and Europe. If you’re suddenly dealing with serious digestive issues in your thirties, forties, or fifties, you’re definitely not alone.
The Myth That Egg Allergies Only Affect Kids
A persistent myth in mainstream nutrition is that egg allergies only matter for children. While plenty of kids outgrow their early allergies, gastroenterologists are seeing a sharp rise in adult-onset egg intolerance.
Your immune system constantly samples your environment. A serious viral infection, a bout of food poisoning, or chronic stress can permanently reprogram how your immune cells recognize familiar proteins. Suddenly a food you’ve eaten for decades gets flagged as a threat.
Patients who used to enjoy weekend omelets with no issues find themselves unable to handle a single bite. Accepting that your body has genuinely changed is the first step toward getting relief.
Intestinal Permeability and Leaky Gut Syndrome
Adult-onset sensitivities are often linked to a physical breakdown of the intestinal barrier. Your gut lining is only one cell thick, held together by structures called tight junctions. When those junctions get damaged, you develop intestinal permeability, commonly called leaky gut.
Several factors can damage these tight junctions, including long-term NSAID use (like ibuprofen or aspirin), heavy alcohol consumption, and chronic psychological stress. Once damaged, the barrier lets larger undigested egg proteins slip directly into the bloodstream.
Once there, your immune system attacks them, creating a new localized immune response. This leads to egg protein malabsorption and chronic digestive distress. Healing the gut lining with targeted amino acids like L-glutamine is usually required to reverse this.
Egg Whites vs. Egg Yolks: Finding Your Specific Trigger
Not all parts of an egg are equal when it comes to digestion. The white and yolk have completely different nutritional profiles, fat contents, and allergenic potential. Knowing the difference can help you pinpoint exactly what’s causing your symptoms.

Many patients find they can tolerate one part but react strongly to the other. By separating them, you can figure out whether your issue is fat digestion or pure protein allergy.
| Egg Component | Primary Proteins & Lipids | Allergenic Potential | Digestibility Profile | Common Clinical Presentation |
|---|---|---|---|---|
| Egg Whites | Ovalbumin, Ovomucoid, Lysozyme | Extremely High | Difficult if protease enzymes are impaired | Severe cramping, rapid transit, histamine reactions |
| Egg Yolks | Livetin, Phosvitin, Arachidonic Acid | Low to Moderate | Easier to digest, but high fat triggers reflex | Fatty stools, gallbladder pain, IBS urgency |
As you can see, egg whites contain the most reactive proteins. If you have true egg allergy symptoms, the whites are almost always the culprit. On the other hand, if your issue is IBS or bile acid malabsorption, the yolks will cause more distress because of their dense fat content.
Histamine Intolerance: The Hidden Egg White Reaction
There’s a lesser-known mechanism that often confuses both patients and doctors. Some people test completely negative for egg allergies and standard intolerances but still get violent diarrhea from egg whites. Histamine is usually the answer.

Histamine is a chemical your immune system produces naturally, and it’s also found in certain foods. Eggs themselves aren’t high in histamine, but egg whites are classified as histamine liberators. They trigger your body’s mast cells to release stored histamine into the bloodstream.
In a healthy person, an enzyme called Diamine Oxidase (DAO) breaks down excess histamine quickly. But if you have a DAO deficiency, that histamine floods your digestive tract. It binds to receptors in the gut, triggering fluid secretion and rapid muscle contractions.
The result is sudden, explosive diarrhea. If you also react poorly to aged cheeses, fermented foods, or red wine, histamine intolerance is a strong possibility. A DAO enzyme supplement taken before meals can sometimes prevent this reaction.
Hidden Egg Ingredients and Cross-Contamination Risks
Patients trying to avoid eggs often fail because they only remove whole eggs from their breakfast. The food industry makes complete avoidance incredibly difficult because egg derivatives show up in thousands of processed foods.
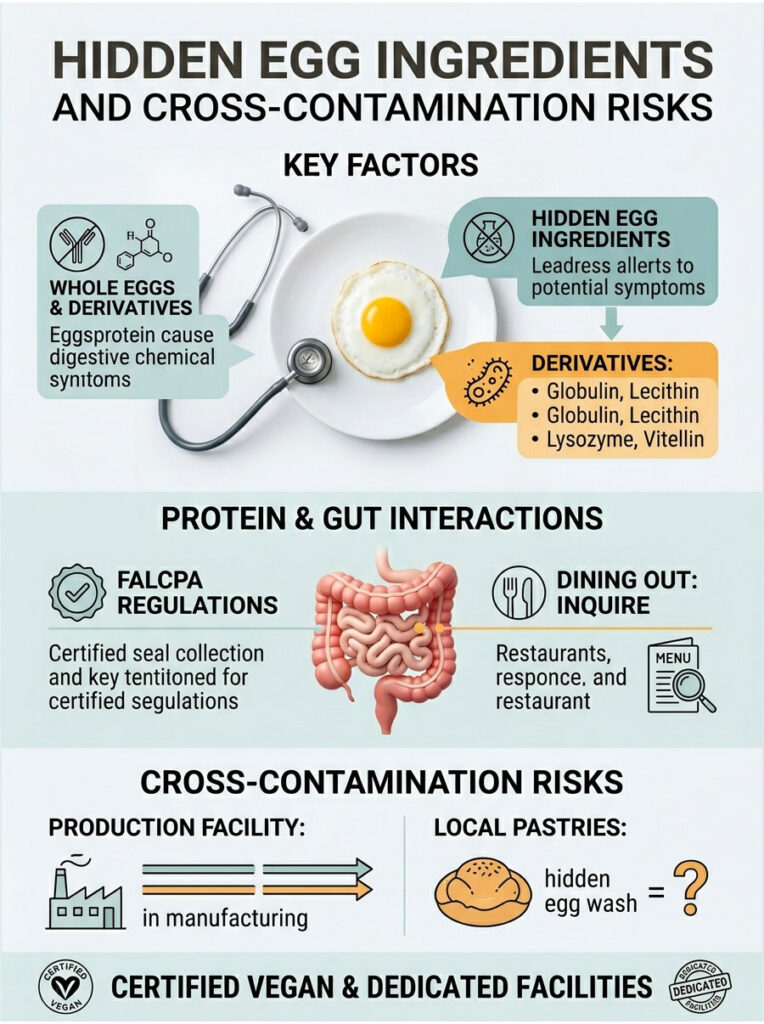
If you’re still having diarrhea after dropping whole eggs, you’re probably still eating hidden derivatives. Becoming a skilled label reader is essential for healing your gut.
Manufacturers love eggs because they’re cheap, effective binders. Eggs hold gluten-free bread together, give ice cream its smooth texture, and clarify certain wines. You have to look beyond the obvious sources.
Reading Complex Food Labels
The food industry uses eggs as binders, emulsifiers, and clarifying agents. Learning to spot hidden egg ingredients on labels is a survival skill for sensitive patients. Ingredients like globulin, lecithin, lysozyme, and vitellin are all egg-derived.
Even tiny traces of these ingredients can trigger diarrhea in highly sensitive people. Mayonnaise, commercial salad dressings, frozen meatballs, and boxed baked goods commonly contain these hidden binders.
The FDA requires major allergens to be clearly listed under FALCPA regulations. But restaurant menus rarely list every ingredient, so always ask the chef about hidden binders and emulsifiers when eating out.
Cross-Contamination in Processing
Beyond hidden ingredients, the manufacturing process itself matters. Even trace amounts of leftover protein can trigger a major reaction in sensitized patients.
Shared manufacturing equipment for baked goods, pastas, and breaded items is a daily risk. Cross-contamination happens when a facility produces an egg-containing product and then runs an egg-free product on the same equipment without a deep clean.
For patients with severe egg allergy symptoms, this trace exposure is plenty to cause a full reaction. Look for certified vegan labels or statements that say “manufactured in a dedicated egg-free facility” if your sensitivity is serious.
Expert Insight: Local coffee shop pastries are a common source of hidden exposure. Even when eggs aren’t in the batter, bakers often brush a raw egg wash on top of breads and pastries for that shiny glaze. Always ask the barista before ordering.
A Practical Four-Step Treatment Plan
If you’re dealing with consistent digestive issues, it’s time to stop guessing and start taking action. Masking symptoms with over-the-counter medication will never address the root cause.
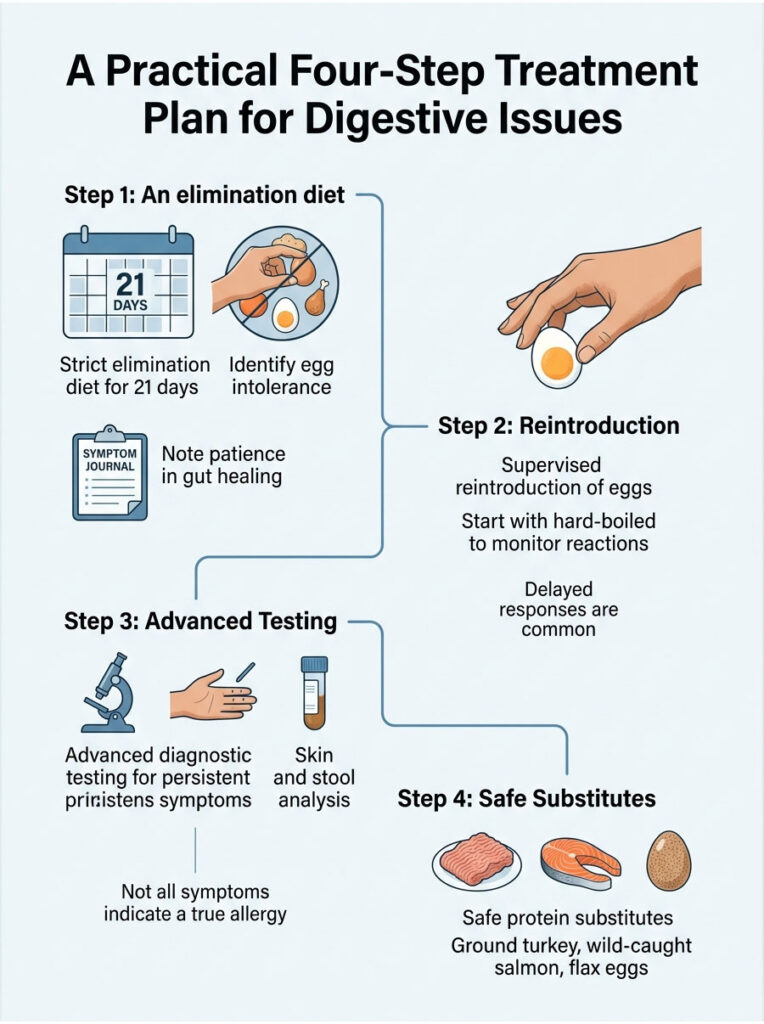
Based on years of testing this approach in my clinic, I’ve built a four-step protocol that helps patients identify their trigger, heal their gut lining, and find safe alternatives. Don’t rush this process. Your gut needs time to regenerate, and your immune system needs time to settle down.
Step 1: The Strict 21-Day Elimination Diet
The clinical gold standard for identifying egg intolerance is a strict elimination diet. Blood tests are often unreliable, but your body’s physical response never lies. Remove all visible and hidden sources of eggs for at least 21 days.
This gives your damaged intestinal lining time to heal and lets systemic inflammation subside. During this period, be hyper-vigilant about checking labels for hidden egg ingredients.
Keep a detailed daily symptom journal. Track bowel movements, gas, bloating, and energy levels. Most patients see a dramatic reduction in morning urgency within the first seven days of total elimination.
Step 2: Supervised and Strategic Reintroduction
After the 21-day phase, it’s time to test your tolerance. Reintroduce hard-boiled eggs first before moving to scrambled or fried versions. Because of ovomucoid’s heat resistance, some proteins survive cooking, but others partially denature with intense heat, making hard-boiled a slightly safer starting point.
Eat one plain egg and monitor your bowel movements, gas, and stool consistency for 48 hours. Don’t eat any other potential trigger foods (like dairy or gluten) during this window. We want an isolated response.
If symptoms appear within an hour, your gastrocolic reflex or gallbladder is likely the problem. If symptoms show up the next day, you’re dealing with delayed intolerance. If you pass 48 hours with no issues, eggs are probably safe in moderation.
Step 3: Advanced Diagnostic Testing
If symptoms continue despite strict elimination, advanced testing is necessary. An allergist can perform a skin prick test or specific IgE blood test to rule out true allergy. This is especially important if you’ve ever had hives or facial swelling.
For non-allergic intolerances, gastroenterologists often recommend a comprehensive stool analysis. This checks markers like Fecal Elastase-1, pancreatic enzyme levels, and inflammatory markers like Fecal Calprotectin. It confirms whether egg protein malabsorption is actually driving your symptoms.
We can also test for bacterial overgrowth using hydrogen and methane breath tests. This layered diagnostic approach makes sure we’re not missing anything underlying.
Step 4: Safe Protein Substitutes
Keeping your protein intake up during elimination matters. Removing eggs from your morning routine can leave you hungry and tired if you don’t replace those calories properly.
Low-allergen alternatives include lean ground turkey, wild-caught salmon, and hydrolyzed collagen peptides. High-quality collagen powder stirred into warm oatmeal provides a solid protein boost without triggering the gastrocolic reflex.
For baking, a mixture of ground flaxseed and warm water mimics the binding properties of eggs well. This “flax egg” also adds omega-3 fatty acids without any of the gastrointestinal risks.
Key Takeaways
The relationship between eggs and your digestive system is more complex than most people realize. Can eggs cause diarrhea? Absolutely, and through several distinct mechanisms that each need their own targeted approach.
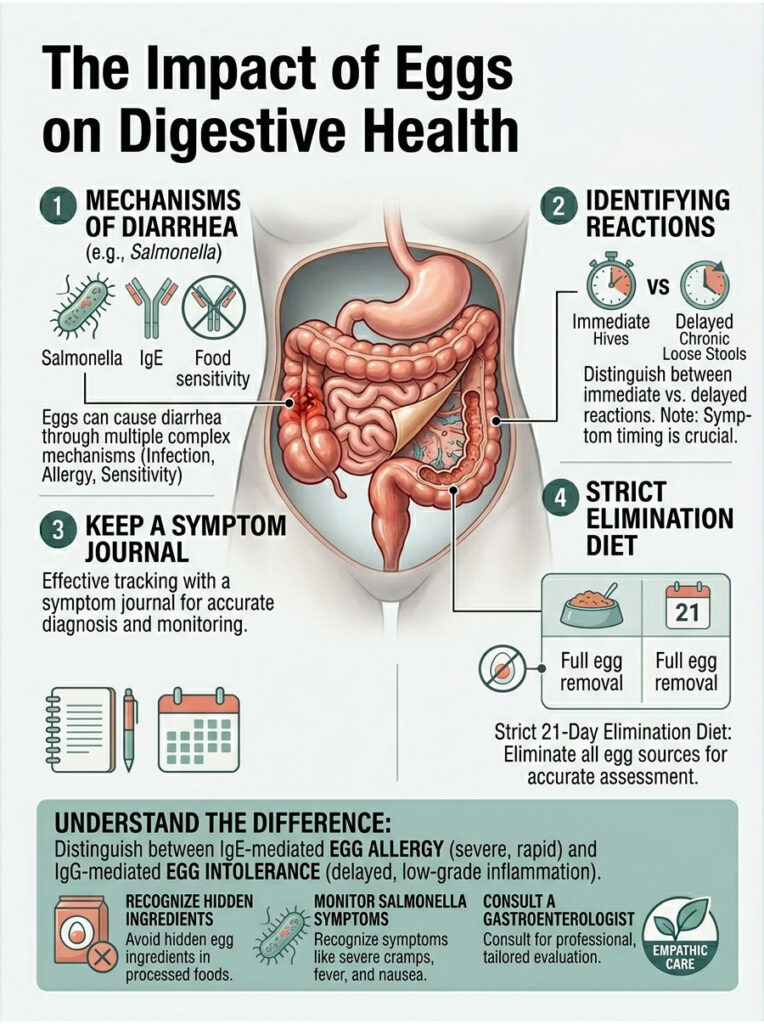
Whether your symptoms come from Salmonella, a hyperactive gastrocolic reflex from IBS, a true IgE allergy, or a delayed IgG intolerance to heat-resistant proteins, identifying the exact cause matters. Covering up the problem with temporary medication isn’t a real solution.
By keeping a detailed symptom journal, committing to a strict 21-day elimination diet, and working with a qualified gastroenterologist, you can figure out exactly what’s triggering your symptoms. You have the power to heal your gut and fix your morning digestive distress for good.
If you’re still asking yourself whether eggs can cause diarrhea, remember this: your symptoms are real, they’re scientifically explainable, and they’re absolutely treatable.
Frequently Asked Questions
Why do I experience immediate diarrhea within minutes of eating eggs?
If your symptoms occur within 15 to 60 minutes, you are likely experiencing a hyperactive gastrocolic reflex. This is common in patients with IBS-D, where the presence of a dense protein and fat-rich meal triggers the hormone cholecystokinin (CCK), causing the colon to contract prematurely and evacuate stool before water can be properly reabsorbed.
Can eggs cause delayed diarrhea up to 48 hours later?
Yes, this is characteristic of an IgG-mediated food sensitivity or clinical egg intolerance. Unlike a rapid allergic reaction, an IgG response involves delayed mucosal inflammation in the gut lining. This low-grade inflammation impairs fluid absorption over time, often resulting in loose stools, bloating, and brain fog one to two days after ingestion.
Why are my stools bright yellow and burning after consuming egg yolks?
This specific presentation often indicates Bile Acid Malabsorption (BAM). Because egg yolks are high in fat, they require a significant release of bile for digestion. If your small intestine fails to reabsorb this bile, it enters the colon where it acts as a potent chemical laxative, causing urgent, yellow, and often irritating diarrhea.
Does thoroughly cooking or hard-boiling eggs prevent digestive distress?
Not necessarily. While heat denatures many proteins, the egg protein known as ovomucoid is remarkably heat-resistant. It maintains its molecular structure even after extensive boiling or baking. For patients with a specific sensitivity to ovomucoid, fully cooked eggs will still trigger an inflammatory immune response and subsequent diarrhea.
How can I tell the difference between an egg allergy and an egg intolerance?
A formal IgE-mediated egg allergy usually causes rapid-onset symptoms within minutes, including hives, swelling, or vomiting alongside diarrhea. An egg intolerance (IgG-mediated) is localized to the digestive tract, lacks systemic symptoms like wheezing, and typically manifests as delayed abdominal cramping and loose stools hours or even days later.
Why do I suddenly have an egg intolerance as an adult after years of eating them?
Adult-onset food sensitivities often stem from increased intestinal permeability, or ‘leaky gut.’ Factors like chronic stress, NSAID use, or past infections can damage the tight junctions of your intestinal lining. This allows undigested egg proteins to enter the bloodstream, leading the immune system to suddenly flag them as foreign invaders and trigger a new inflammatory response.
Can I be sensitive to egg whites but still eat egg yolks?
Often, yes. Egg whites contain the most highly allergenic proteins like ovalbumin and lysozyme. If your issue is a protein-based sensitivity, you may find relief by consuming only the yolks. However, if your diarrhea is triggered by fat-induced motility issues (IBS), the yolk may actually be the primary culprit due to its high lipid content.
What are the symptoms of a Salmonella infection from eggs compared to a sensitivity?
Salmonella enteritidis causes acute bacterial gastroenteritis, which is much more severe than a sensitivity. Symptoms include explosive watery diarrhea, high fever, chills, and intense nausea. These typically manifest 6 to 72 hours after eating contaminated eggs and require careful monitoring for dehydration.
Why does eating eggs cause foul, sulfur-smelling gas and diarrhea?
Eggs are rich in sulfur-containing amino acids like methionine. If these proteins reach the colon undigested due to malabsorption, opportunistic sulfur-reducing bacteria (such as Desulfovibrio) ferment them. This process produces hydrogen sulfide gas, which irritates the bowel lining and accelerates transit time, leading to urgent, foul-smelling stools.
Can egg whites trigger a histamine reaction in the gut?
Yes, egg whites are known as histamine liberators. They can trigger mast cells in the digestive tract to release stored histamine. If you have a deficiency in the Diamine Oxidase (DAO) enzyme, this histamine buildup can cause rapid smooth muscle contractions in the gut, resulting in sudden, explosive diarrhea.
What are common hidden egg ingredients I should look for on food labels?
To fully avoid egg-related diarrhea, you must look for derivatives such as globulin, lecithin, lysozyme, vitellin, and albumin. These are frequently used as binders or emulsifiers in processed foods, salad dressings, and even some medications, and can be enough to trigger symptoms in highly sensitized individuals.
What is the most effective way to diagnose an egg-related digestive issue?
The clinical gold standard is a strict 21-day elimination diet followed by a controlled reintroduction. While blood tests for IgE can rule out allergies, they are less reliable for intolerances. Tracking your symptoms in a journal during the elimination phase allows you to see if your intestinal lining heals and if symptoms return upon reintroducing specific egg components.
Disclaimer
This article is for informational purposes only and does not constitute medical advice, diagnosis, or treatment. The information provided by a board-certified gastroenterologist is intended to supplement, not replace, the relationship between a patient and their physician. Always consult with a qualified healthcare professional before starting an elimination diet or making significant changes to your healthcare regimen, especially if you suspect a life-threatening allergy.
References
- Food Allergy Research & Education (FARE) – https://www.foodallergy.org – 2023 Statistics on egg allergy prevalence and severe sensitivities in the United States.
- Centers for Disease Control and Prevention (CDC) – https://www.cdc.gov – Clinical data regarding Salmonella enteritidis infection rates and hospitalization statistics.
- Journal of Clinical Gastroenterology – Research paper on the prevalence of the hypersensitive gastrocolic reflex in patients diagnosed with IBS-D.
- American College of Gastroenterology – https://gi.org – Guidelines on the diagnosis and management of Bile Acid Malabsorption (BAM) and chronic diarrhea.
- World Journal of Gastroenterology – Study on the heat resistance of ovomucoid proteins and their impact on pediatric and adult-onset food allergies.
- The Mast Cell Disease Society – Information on histamine liberators and the role of egg whites in triggering localized histamine reactions in the gut.