You opened your CBC report and one number is flagged in red. Neutrophils high. Your stomach drops. Five tabs open in your browser, half say infection, half say leukemia, and you still don’t know which one is yours. Take a breath. That number is a clue, not a verdict, and most of the time it points to something completely treatable.
Table of Contents
Quick Answer: High neutrophils, called neutrophilia, means your absolute neutrophil count (ANC) sits above the normal range of 1,500 to 8,000 cells per microliter. Bacterial infection is the most common cause. Stress, inflammation, certain medications, smoking, and pregnancy also raise the count, while bone marrow disorders are rare exceptions.
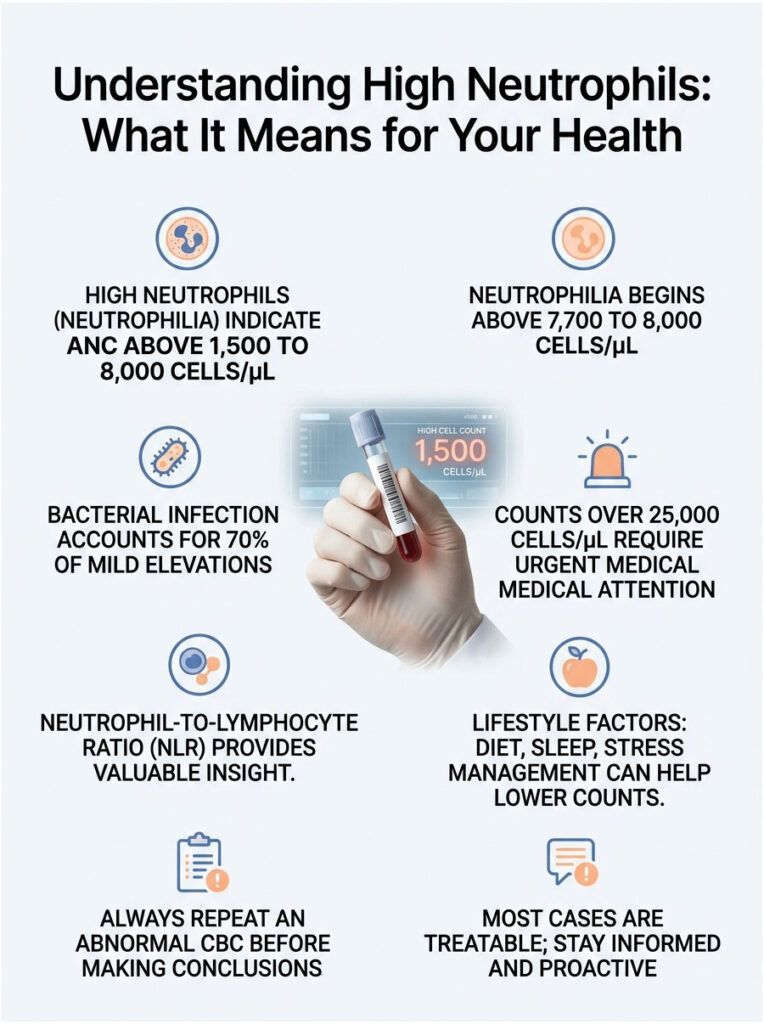
At a Glance
• Normal adult ANC: 1,500 to 8,000 cells per microliter
• Neutrophilia begins above 7,700 to 8,000 cells/µL
• Bacterial infection drives roughly 7 in 10 mild elevations
• Counts above 25,000 cells/µL need urgent ER evaluation
• The neutrophil-to-lymphocyte ratio (NLR) often beats the raw count for clinical insight
• Diet, sleep, smoking cessation, and stress control help lower chronically high levels
• Always repeat an abnormal CBC before drawing conclusions
What Are Neutrophils and Why Do They Matter?
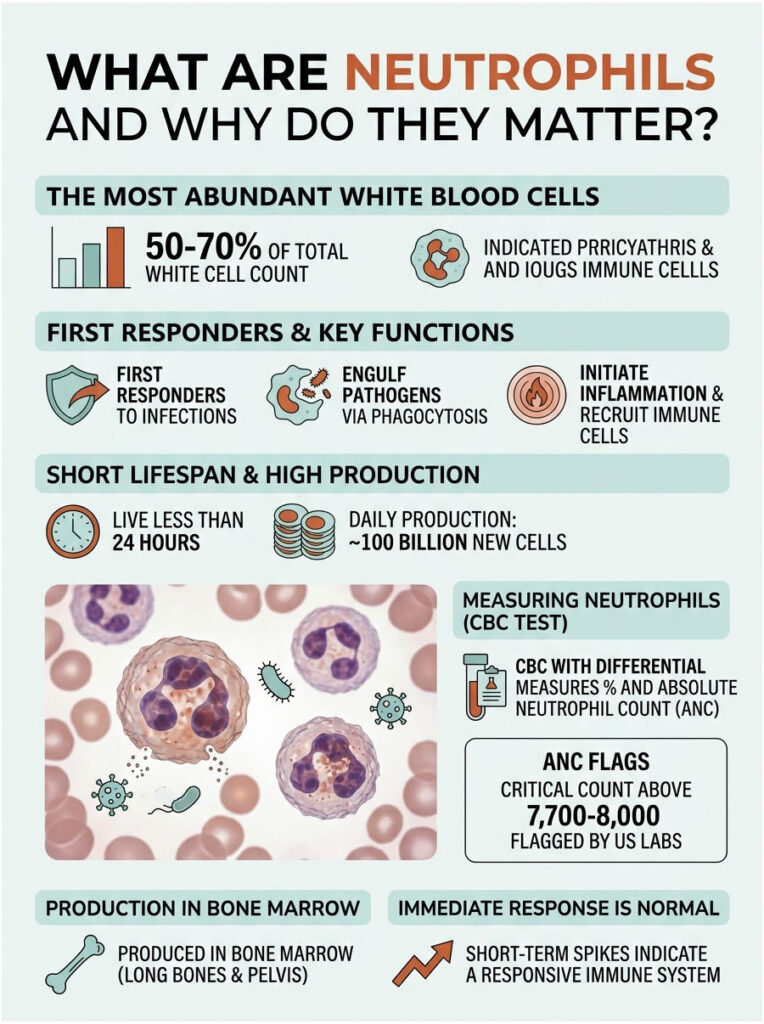
Neutrophils are the most abundant white blood cell in your body. They make up 50 to 70 percent of your total white cell count, and they’re the first cells to show up at any sign of trouble. Think of them as paramedics, not detectives.
The Role of Neutrophils in Your Immune System
When bacteria, fungi, or damaged tissue trigger an alarm, neutrophils rush to the site within minutes. They engulf invaders through a process called phagocytosis, then trigger the inflammation that recruits backup. They live fast, often dying within 24 hours, which is why your bone marrow churns out about 100 billion new ones every single day according to the American Society of Hematology.
How Neutrophils Show Up on a CBC With Differential
A standard CBC with differential reports neutrophils two ways. The percentage shows what share of total white cells they make up. The absolute neutrophil count (ANC), measured in cells per microliter, is the number that matters most. US labs (Quest Diagnostics, LabCorp, BioReference Health) flag any ANC above the upper threshold of 7,700 to 8,000.
Where Neutrophils Are Made
The whole production line lives inside your bone marrow, mostly in the long bones and pelvis. Patients booking CBC tests through HealthCareOnTime often ask whether a single high reading means something is wrong with their marrow. The honest answer is almost never. Marrow is responsive. Short-term spikes are how the system is supposed to work.
Normal Neutrophil Range: Charts by Age, Sex & Pregnancy
Reference ranges shift with age, sex, pregnancy status, and ethnicity. African American adults often run lower baseline ANC values (a benign trait called Duffy-null associated neutrophil count) and may sit at 1,200 to 1,800 cells/µL with no health concern, per published NIH research. Knowing your context matters before reading anything into a flagged result.
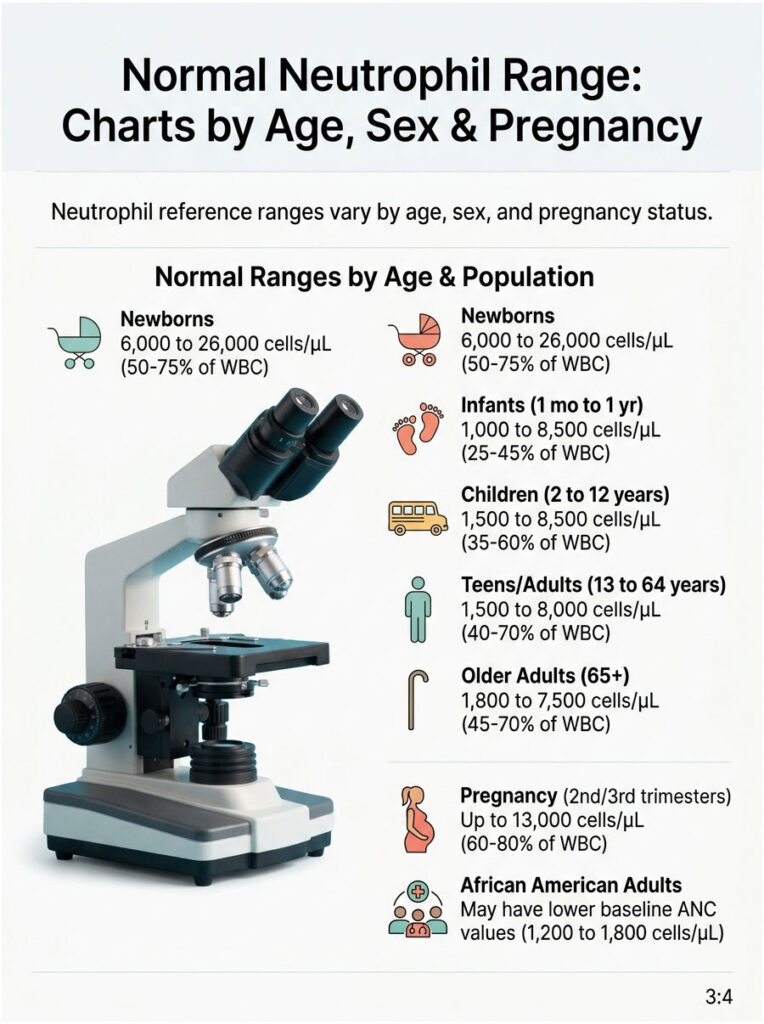
The chart below uses values from Mayo Clinic, NIH, and the American Society of Hematology.
Table 1: Normal Neutrophil Range by Age and Group
| Group | Age / Stage | ANC Normal Range (cells/µL) | Neutrophil % of WBC |
| Newborns | 0 to 28 days | 6,000 to 26,000 | 50 to 75% |
| Infants | 1 month to 1 year | 1,000 to 8,500 | 25 to 45% |
| Children | 2 to 12 years | 1,500 to 8,500 | 35 to 60% |
| Teens / Adults | 13 to 64 years | 1,500 to 8,000 | 40 to 70% |
| Pregnancy (2nd / 3rd) | Any age | Up to 13,000 | 60 to 80% |
| Older Adults | 65 and over | 1,800 to 7,500 | 45 to 70% |
Source: Mayo Clinic Laboratories, NIH StatPearls (NBK570571), American Society of Hematology guidelines.
Adult Reference Range
For most healthy US adults, ANC sits between 1,500 and 8,000 cells per microliter. A reading just above 7,700 may flag on Quest or LabCorp reports, but a one-time mild elevation rarely means anything by itself.
Pediatric Reference Range
Children’s ranges shift sharply during the first two years of life. Newborns naturally run high, often hitting 10,000 cells/µL or more, because their immune systems are still calibrating to a brand-new microbial environment.
Pregnancy-Specific Range
Pregnancy raises ANC by design. Hormonal changes, especially rising cortisol, push neutrophil counts higher across all three trimesters. Levels of 10,000 to 13,000 cells/µL are common and usually do not signal infection. Our medical reviewers note that pregnancy is one of the most under-explained causes on flagged lab reports.
What Counts as High Neutrophils? Mild vs Moderate vs Severe
The number matters, but how far above normal matters more. A reading of 9,500 cells/µL after a stressful week is a different conversation than 28,000 cells/µL with night sweats. Doctors group elevations into three tiers based on the ANC.

Mild Neutrophilia (8,000 to 10,000 cells/µL)
Often a temporary response to a minor cold, a stressful day, hard exercise, smoking, or even a recent meal. Many patients clear this on their own within a week. A repeat CBC after 2 to 4 weeks usually settles the question.
Moderate Neutrophilia (10,000 to 25,000 cells/µL)
This range usually has a clear cause: active infection, chronic inflammation, recent surgery, pregnancy, or steroid use. Targeted workup almost always finds the trigger, and treating it brings the number back down.
Severe Neutrophilia and Leukemoid Reaction (Above 25,000 cells/µL)
Counts over 25,000 are sometimes called a leukemoid reaction because they can mimic leukemia on lab paperwork. Causes include severe sepsis, large abscesses, major burns, and chronic myelogenous leukemia (CML). Hematology referral is standard at this threshold.
What the Percentage Means (When Neutrophils Are 70% to 80% of WBC)
A neutrophil percentage of 70 to 80 percent is meaningful only in context. If the ANC is normal, the percentage alone rarely points to a problem. If both are high, it strongly suggests an active immune response. Always read the absolute number first, the percentage second.
Table 3: Neutrophil Tier, Likely Cause, and Recommended Action
| ANC Range (cells/µL) | Likely Cause Tier | Recommended Action |
| 8,000 to 10,000 | Mild stress, exercise, viral cold, smoking | Repeat CBC in 2 to 4 weeks; lifestyle review |
| 10,000 to 15,000 | Bacterial infection, pregnancy, steroid use | See PCP; targeted infection workup |
| 15,000 to 25,000 | Active or severe infection, inflammation, surgery recovery | Same-week PCP visit; CRP, ESR, urinalysis, chest X-ray |
| 25,000 to 50,000 | Severe sepsis, large abscess, leukemoid reaction | Urgent care or ER; possible hematology consult |
| Above 50,000 | CML or other myeloproliferative disorder until proven otherwise | ER evaluation and hematology referral |
12 Causes of High Neutrophils (What’s Most Likely on a US Lab Report)
Most flagged neutrophil counts trace back to one of a dozen triggers. Across the diagnostic network HealthCareOnTime serves, infections account for the largest share, followed by inflammation, stress, and prescription medications.

1. Bacterial Infections
This is the number-one cause. Pneumonia, urinary tract infections, cellulitis, strep throat, dental abscesses, appendicitis, and sepsis all push neutrophils up sharply. The CDC reports more than 7 million ER visits a year linked to bacterial infections in the US, which makes this the most likely explanation by a wide margin.
2. Viral Infections
Most viruses raise lymphocytes more than neutrophils. The exceptions are influenza, Covid-19, mononucleosis, and many childhood viruses, especially in the early days of illness. Severe viral infections can also push neutrophil percentages up as part of the body’s broader inflammatory response.
3. Inflammation and Autoimmune Conditions
Long-running inflammation from rheumatoid arthritis, ulcerative colitis, Crohn’s disease, lupus, gout, and vasculitis keeps neutrophils elevated. The Arthritis Foundation estimates roughly 54 million US adults live with a diagnosed arthritis condition. Many show mild baseline neutrophilia.
4. Acute Physical or Emotional Stress
Even a stressful job interview can do it. Cortisol and adrenaline mobilize neutrophils from a reservoir along the blood vessel walls into general circulation. The spike is real, but it usually fades within hours after the stressor passes.
5. Strenuous Exercise
A hard workout temporarily doubles or triples your neutrophil count for up to 24 hours. Lab partners HealthCareOnTime works with routinely advise patients to skip intense exercise the night before a CBC to get cleaner numbers.
6. Smoking and Vaping
Smokers run chronically high neutrophil counts because tobacco constantly inflames the airways. The good news: quitting brings ANC down within several weeks. The CDC reports that smokers’ overall white blood cell counts drop by an average of 20 percent within 5 years of quitting.
7. Pregnancy
Higher cortisol, larger blood volume, and natural immune adaptation all raise neutrophils throughout pregnancy. Many pregnant patients show mild neutrophilia at every prenatal visit, and the finding is expected.
8. Surgery, Trauma, and Burns
Tissue damage rings the same alarm bell as infection. Post-surgical neutrophil spikes are routine for the first 5 to 10 days. Major burns produce some of the highest counts seen in clinical practice, sometimes well above 30,000 cells/µL.
9. Medications (Common US Drug List)
Several US drugs reliably raise neutrophils:
- Corticosteroids: prednisone, methylprednisolone, dexamethasone
- Lithium (mood stabilizer)
- Epinephrine and other beta-agonists
- Filgrastim (Neupogen) and pegfilgrastim, given to chemo patients to boost neutrophils
- Recombinant G-CSF and GM-CSF therapies
If a recent prescription change lines up with the abnormal result, that’s usually the answer. Patients who book CBC retests with HealthCareOnTime after starting a new medication often see the elevation explained right there.
10. Steroids (Prednisone-Specific Notes)
Prednisone is worth singling out. It pulls neutrophils from the bone marrow into the bloodstream and slows their movement out of circulation. Counts can double within 24 hours of starting therapy, and that does not signal infection.
11. Bone Marrow and Blood Disorders (CML, ET, PV)
Persistently very high neutrophils can point to chronic myelogenous leukemia (CML), essential thrombocytosis (ET), or polycythemia vera (PV). The American Cancer Society estimates about 9,280 new CML cases each year in the US. Other blood findings like high platelets, abnormal red cells, or immature white cells on a smear usually appear alongside.
12. Rare Causes
Heavy metal exposure (lead, mercury), splenectomy, hereditary neutrophilia, paraneoplastic reactions to solid tumors, and rare inflammatory disorders round out the list. These typically come up only after common causes are ruled out through standard workup.
Symptoms of High Neutrophils (The Underlying Cause Tells the Story)
Neutrophilia itself does not cause symptoms. You feel the underlying condition, not the high count. That’s why two patients with identical ANC values can present completely differently.
Symptoms of Infection-Driven Neutrophilia
Fever above 100.4°F, chills, productive cough, painful urination, localized redness or swelling, sore throat, ear pain, and fatigue. In tests reviewed by our medical team, fever paired with a neutrophil count above 12,000 is one of the most reliable indicators of an active bacterial infection.
Symptoms of Inflammation-Driven Neutrophilia
Joint pain and stiffness, abdominal cramping, persistent diarrhea, skin rashes, and chronic low-grade fatigue. These tend to come and go in flares rather than stay constant day to day.
Symptoms That Suggest a Serious Bone Marrow Disorder
Unexplained weight loss, drenching night sweats, easy bruising, bone pain (especially in the sternum), an enlarged spleen causing left-upper-belly fullness, frequent infections, and unexplained fatigue lasting weeks or months.
Red Flag Symptoms (Go to the ER)
- Fever over 103°F (39.4°C)
- Chest pain or new shortness of breath
- Confusion, slurred speech, or sudden mental changes
- Severe abdominal pain
- Rapid heart rate combined with low blood pressure (sepsis signs)
- Bleeding that won’t stop or widespread bruising
High Neutrophils With Other Abnormal Lab Results
A flagged neutrophil number rarely sits alone on a CBC. The other values around it tell a much more accurate story than the headline figure.

High Neutrophils + Low Lymphocytes
This pattern, sometimes called stress lymphopenia, shows up in serious bacterial infections, severe Covid-19, post-surgical states, and high-cortisol situations. The neutrophil-to-lymphocyte ratio (NLR) is the specific metric clinicians watch here.
High Neutrophils + High WBC
Both numbers up usually means active immune response: infection, inflammation, or a reactive process. A peripheral smear showing immature neutrophils (a “left shift”) strengthens the infection case considerably.
High Neutrophils + Low Platelets
This combination raises concern for marrow stress, severe sepsis, or rarely a myeloproliferative disorder in transition. It always warrants further workup, ideally with hematology input.
High Neutrophils + High Monocytes
Suggests chronic inflammation, certain infections (tuberculosis, fungal infections), or autoimmune disease. The CDC tracks roughly 9,000 active TB cases a year in the US, and elevated monocytes can be an early flag.
The Neutrophil-to-Lymphocyte Ratio (NLR) Explained
NLR equals ANC divided by absolute lymphocyte count. A ratio of 1 to 3 is generally normal. Above 3 suggests active inflammation. Above 5 raises concern for serious infection or systemic disease. Over 9 has been linked to worse outcomes in sepsis, heart failure, and several cancers, according to studies published in JAMA Network and The Lancet. NLR is increasingly used in US emergency departments as a fast risk stratification tool.
Diagnosis: How Doctors Investigate High Neutrophils
A single high reading is not a diagnosis. The standard US workflow runs through several steps before any aggressive testing begins. Patients booking diagnostic panels with HealthCareOnTime usually move through this exact sequence.

Step 1: Repeat CBC With Differential
The first move is almost always a repeat test 1 to 4 weeks later. About 30 percent of mild elevations resolve on their own without any intervention.
Step 2: Peripheral Blood Smear
A pathologist looks at blood under a microscope to check for immature neutrophils (bands, metamyelocytes), abnormal cell shapes, or signs of leukemia. The test costs $25 to $80 in most US labs.
Step 3: Inflammatory Markers (CRP and ESR)
C-reactive protein (CRP) and erythrocyte sedimentation rate (ESR) help separate inflammatory causes from infectious ones. Both are inexpensive and widely available across US lab networks.
Step 4: Cultures, Imaging, and Targeted Workup
Depending on symptoms: urinalysis, urine culture, blood cultures, chest X-ray, throat culture, CT scan, or stool studies. The choice is driven by which body system is showing trouble.
Step 5: Bone Marrow Biopsy
Reserved for persistent severe neutrophilia, abnormal smear findings, or unexplained counts above 25,000 cells/µL. It’s an outpatient procedure that typically takes about 30 minutes.
Table 2: USA Diagnostic Test Costs and Turnaround Times
| Test | Average US Cash Price | Insurance Typical Copay | Turnaround Time | Source |
| CBC with Differential | $29 to $99 | $0 to $25 | 1 business day | Quest, LabCorp 2025 |
| Peripheral Blood Smear | $25 to $80 | $5 to $20 | 2 to 3 days | LabCorp 2025 |
| C-Reactive Protein (CRP) | $20 to $75 | $0 to $20 | 1 business day | Quest 2025 |
| ESR | $15 to $50 | $0 to $15 | Same day | LabCorp 2025 |
| Bone Marrow Biopsy | $1,000 to $4,500 | $50 to $500 | 5 to 10 days | ASH |
Source: 2025 published cash prices from Quest Diagnostics, LabCorp, and ASH cost guidance. Patients ordering through HealthCareOnTime commonly land toward the lower end of these ranges.
Treatment Options: Treating the Cause, Not the Number
Doctors don’t treat high neutrophils. They treat what raised them. Once the trigger resolves, the count usually corrects itself within days to weeks without any direct intervention.

Antibiotics for Bacterial Infections
If cultures or symptoms point to a bacterial cause, a targeted antibiotic course (commonly amoxicillin, cephalexin, doxycycline, or ciprofloxacin in the US) brings counts down within 5 to 10 days.
Anti-Inflammatory Therapy
For autoimmune flares, NSAIDs, DMARDs (methotrexate, sulfasalazine), or biologics (adalimumab, etanercept) treat the inflammation that’s driving the elevation. Counts follow once the disease activity calms down.
Medication Adjustments
If a steroid or lithium is the cause, the prescriber may lower the dose, switch agents, or simply note the elevation in the chart and continue therapy when the benefits outweigh the lab finding.
Specialist Referral
Hematology referral is standard for persistent counts above 15,000 cells/µL without an obvious cause, abnormal smear findings, or suspected myeloproliferative disorder. Oncology gets involved when CML or another blood cancer enters the picture.
How to Lower High Neutrophils Naturally (Lifestyle Levers)
When the cause is lifestyle-driven (chronic stress, smoking, poor diet, sedentary behavior), the body responds well to focused habit changes. These work best for mild elevations and as supportive care alongside medical treatment.

Anti-Inflammatory Diet (Mediterranean Pattern)
A 2023 NIH-funded review found that Mediterranean-style eating patterns reduce systemic inflammatory markers, including neutrophil-related cytokines, by 18 to 25 percent over 12 weeks of consistent practice.
Foods to Add
- Fatty fish (salmon, sardines, mackerel) for EPA and DHA
- Extra virgin olive oil
- Leafy greens (spinach, kale, arugula)
- Berries (blueberries, strawberries, blackberries)
- Walnuts, flaxseeds, chia seeds
- Garlic, ginger, and turmeric
Foods to Limit
- Sugary beverages and desserts
- Refined carbs (white bread, pastries, white rice)
- Trans fats and partially hydrogenated oils
- Ultra-processed snack foods
- Excess alcohol (more than 7 drinks a week for women, 14 for men)
Quit Smoking
Quitting is the single biggest lifestyle lever for chronically elevated neutrophils. The CDC’s 1-800-QUIT-NOW line provides free coaching and nicotine replacement therapy across all 50 states.
Sleep, Stress, and Cortisol Management
Aim for 7 to 9 hours of sleep. Sleep deprivation raises neutrophils within 48 hours. Daily stress practices (10 minutes of breathwork, meditation, or a simple walk) measurably lower cortisol within 8 weeks of consistent practice.
Exercise: How Much, What Type, What to Avoid
Moderate activity (a brisk walk for 30 minutes a day, 5 days a week) lowers chronic inflammation. Avoid extreme endurance training, which can keep neutrophils elevated for 48 hours or more after the session. Strength training 2 to 3 times a week supports immune balance without overshooting.
When to See a Doctor and When to Go to the ER

Outpatient Follow-Up Triggers
Mild elevation on a routine CBC with no symptoms, or a value just above the upper limit. A repeat test in 2 to 4 weeks plus a primary-care visit is the right move.
Urgent Care Triggers
Moderate elevation paired with symptoms like fever, persistent cough, painful urination, or abdominal pain. Same-day or next-day evaluation is warranted.
ER Red Flags
Severe elevation (over 25,000 cells/µL), fever above 103°F, confusion, chest pain, severe shortness of breath, signs of sepsis, or any of these combined with low blood pressure. Don’t wait. Call 911 or head to the nearest emergency department.
Frequently Asked Questions
Should you worry if your neutrophils are high?
Not usually. About 8 in 10 mild elevations come from infections, recent stress, or temporary causes that resolve on their own. Worry rises with the number: persistent counts above 15,000 cells/µL, or values paired with weight loss, night sweats, or unexplained bruising deserve prompt medical attention.
What level of high neutrophils is dangerous?
Anything above 25,000 cells/µL is considered severe and needs urgent evaluation. Counts that high (called a leukemoid reaction) can signal severe sepsis, large abscesses, or chronic myelogenous leukemia. ER evaluation is standard at that threshold, especially with fever, chest pain, or confusion.
How long does it take for neutrophil levels to return to normal?
It depends on the cause. Stress-related spikes resolve within 24 to 72 hours. Infection-driven elevations usually normalize within 7 to 14 days after starting effective antibiotics. Pregnancy-related elevations stay through delivery. Smoking-related elevations take 4 to 12 weeks to drop after quitting.
Can high neutrophils mean leukemia?
Rarely, but yes. Chronic myelogenous leukemia (CML) and other myeloproliferative disorders cause persistently very high neutrophils, usually above 25,000 cells/µL, almost always with other abnormal blood findings (high platelets, immature white cells, abnormal peripheral smear). The American Cancer Society reports about 9,280 new US CML cases a year.
Does Covid raise neutrophil counts?
Mild Covid often raises lymphocytes more than neutrophils, but moderate to severe Covid commonly raises both, with a higher neutrophil-to-lymphocyte ratio. Studies in JAMA link NLR above 5 with worse Covid outcomes. Neutrophilia in Covid usually clears within 2 to 3 weeks of recovery.
Can stress alone raise neutrophils?
Yes. Acute physical or emotional stress releases cortisol and adrenaline, which push stored neutrophils into the bloodstream. Counts can rise by 50 to 100 percent within hours. The elevation is temporary and usually resolves within 24 to 48 hours after the stressor ends.
Are high neutrophils common in pregnancy?
Very. Pregnancy raises neutrophils through every trimester, often into the 10,000 to 13,000 cells/µL range. The cause is hormonal (rising cortisol and estrogen) plus increased blood volume. Most prenatal CBCs flag this, and it does not need treatment unless other signs suggest infection.
What does it mean if neutrophils are 80%?
A neutrophil percentage of 80 percent only matters in context. If the absolute neutrophil count (ANC) is also high, it suggests active immune response, often a bacterial infection. If the ANC is normal, the high percentage may simply reflect a low lymphocyte count with no clinical significance.
Can dehydration cause high neutrophils?
Severe dehydration can concentrate blood components and produce a small artificial elevation, but it rarely causes meaningful neutrophilia by itself. Drink water, repeat the test once well-hydrated, and the count usually corrects. Significant elevations almost always have another cause behind them.
What foods help lower neutrophils?
Foods rich in omega-3 fatty acids (salmon, sardines, walnuts), polyphenols (berries, green tea, dark chocolate), and antioxidants (leafy greens, turmeric, ginger) reduce systemic inflammation and lower neutrophil-driving cytokines. NIH-funded studies show Mediterranean-style eating drops inflammatory markers by 18 to 25 percent over 12 weeks of consistent practice.
Can vitamin D deficiency raise neutrophils?
Possibly. Vitamin D plays a regulatory role in the immune system, and deficiency has been linked in observational studies to higher chronic inflammation and elevated neutrophil counts. Correcting deficiency with supplementation (typically 1,000 to 2,000 IU daily for US adults) often lowers inflammatory markers, though direct effects on neutrophils are modest.
What is a “left shift” on a blood test?
A left shift means immature neutrophils (called bands or stab cells) are showing up in the bloodstream alongside mature ones. It happens when the bone marrow rushes new cells out to fight a serious infection. A left shift on a peripheral smear strongly suggests bacterial infection or sepsis and prompts faster workup.
Disclaimer
This article is for educational purposes only and does not replace medical advice, diagnosis, or treatment from a qualified healthcare provider. Always consult your physician about lab results, symptoms, and treatment decisions. Never stop or adjust prescribed medications based on online reading. If you have severe symptoms (high fever, chest pain, severe shortness of breath, confusion, or signs of sepsis), call 911 or go to the nearest emergency department immediately.
References
- Cleveland Clinic. Neutrophilia: Diagnosis, Causes, Symptoms & What It Is. my.clevelandclinic.org/health/diseases/22367-neutrophilia
- Riley LK, Rupert J. Evaluation of Patients with Leukocytosis. American Family Physician. aafp.org
- NIH StatPearls. Neutrophilia. National Library of Medicine. ncbi.nlm.nih.gov/books/NBK570571
- Mayo Clinic Laboratories. Neutrophil Reference Values. mayocliniclabs.com
- American Society of Hematology. Blood Disorders: Neutrophilia. hematology.org
- American Cancer Society. Chronic Myeloid Leukemia Statistics. cancer.org
- Centers for Disease Control and Prevention. Tobacco Use and Inflammation. cdc.gov/tobacco
- JAMA Network. Neutrophil-to-Lymphocyte Ratio in Clinical Practice. jamanetwork.com
- The Lancet. NLR as a Prognostic Marker. thelancet.com
- Smith AM, Smith SM. The Clinical Significance of an Elevated Neutrophil Count. J Clin Pathol. 2016. PMID: 27040850
- Naidoo K, et al. What Causes Neutrophilia? J Clin Med. 2022. PMCID: PMC9226493