You wiped, you glanced down, and something glossy and jelly-like was on the paper. Maybe it was on top of your stool. Maybe it was floating in the bowl. Either way, your brain went straight to one question: is something wrong with me?
Table of Contents
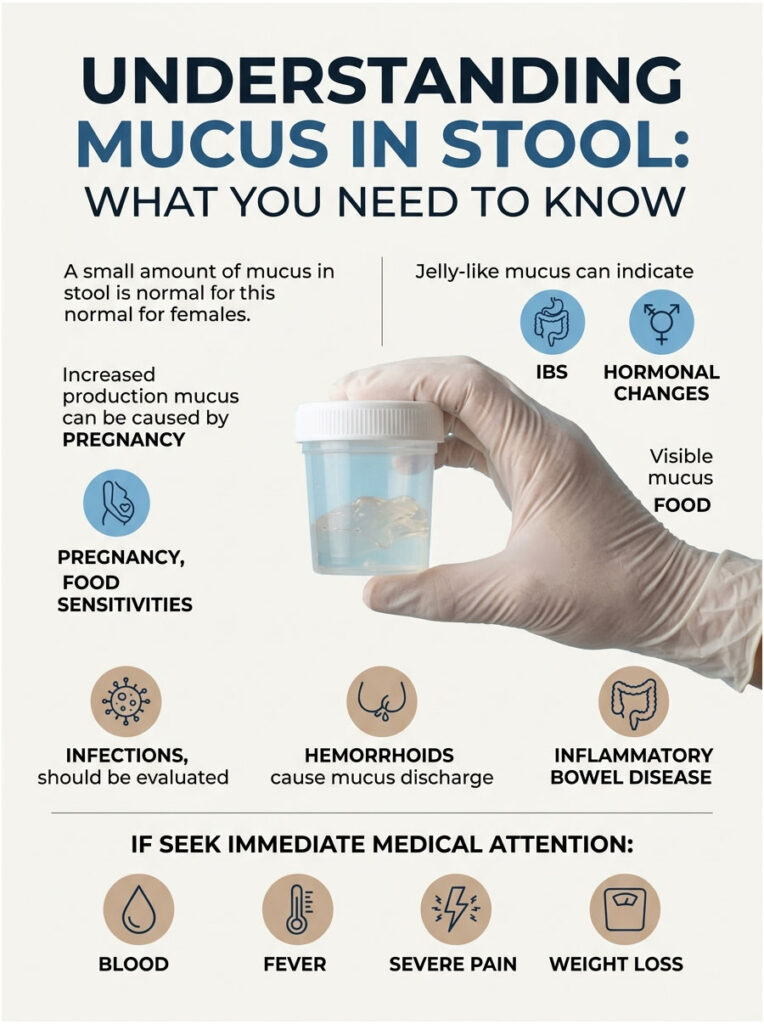
Quick Answer: A small amount of mucus in stool is normal in females. Visible, frequent, or jelly-like mucus is most often caused by IBS, hormonal shifts, pregnancy, food sensitivities, infections, hemorrhoids, or inflammatory bowel disease. Mucus paired with blood, fever, severe pain, or weight loss is a red flag and needs same-day medical attention.
At a Glance
- About 6.1% of US adults meet Rome IV criteria for IBS, and women carry roughly two-thirds of the burden (Cedars-Sinai, Gastroenterology 2023).
- Mucus color is a clue, not a diagnosis. Clear, white, yellow, green, brown, and bloody mucus each point to different causes.
- Estrogen and progesterone shifts across your cycle, pregnancy, and perimenopause can change how much mucus you see.
- Mucus plus blood, black stools, fever, or unintended weight loss is never normal and should be evaluated promptly.
- Diet adjustments, hydration, stress care, and targeted probiotics resolve most cases at home within 1 to 2 weeks.
- Symptoms lasting longer than 14 days deserve a stool panel or GI consult.
- HealthCareOnTime offers nationwide stool testing and digestive lab panels with home sample pickup in many US cities.
What Mucus in Stool Actually Is (and Why Women Notice It More)
Mucus is a slippery, jelly-like fluid produced by goblet cells lining your intestines. It coats the gut wall, traps bacteria, and helps stool slide through smoothly. A trace amount mixes invisibly with every bowel movement, which is why most people never see it.
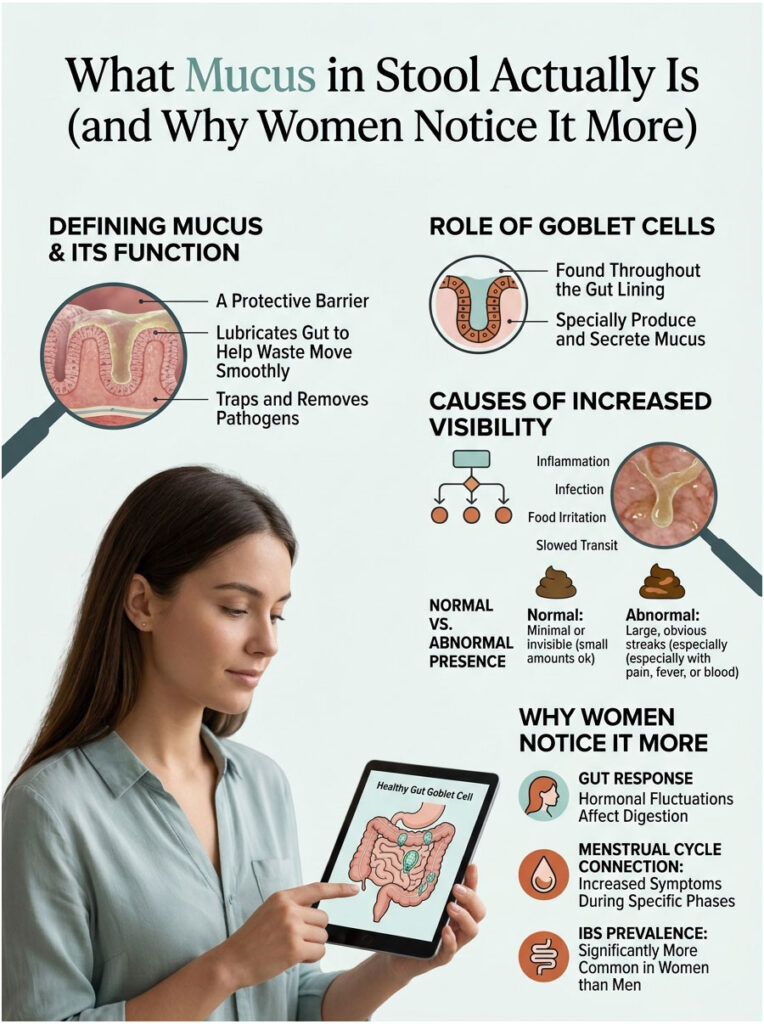
You start noticing mucus when something disrupts that balance. Inflammation, infection, food irritation, or slowed transit can all push the gut to make extra mucus as a defense response. The result is the visible, jelly-strand or coated-stool appearance that brought you here.
Patients booking digestive panels through HealthCareOnTime ask about visible mucus more than almost any other stool change, and the answer almost always begins with one of nine common causes covered below.
How the Gut Makes Mucus
Goblet cells sit between the absorptive cells of your intestinal lining and continuously secrete mucin proteins. These proteins absorb water and form the gel-like coating that protects the gut wall. When the lining is irritated, those cells ramp up production fast, sometimes within hours.
In healthy digestion, mucus is broken down and reabsorbed by the time stool reaches the rectum. When stool moves too quickly (diarrhea), too slowly (constipation), or passes over inflamed tissue, undigested mucus exits with the stool. That is when you see it.
Why Female Bodies Show Symptoms Differently
Women have a different hormonal landscape than men, and the gut responds. Estrogen and progesterone receptors sit directly on intestinal smooth muscle, slowing or speeding transit depending on the cycle phase.
NIH-funded epidemiology research shows women report IBS at 1.5 to 3 times the rate of men, with global IBS prevalence of about 14% in women versus 8.9% in men. Female-pattern symptoms also skew toward bloating, mucus, and constipation.
Our medical reviewers confirm this matches what we see in lab booking data: a high share of stool-test requests in our female panel come during the second half of the menstrual cycle.
Mucus in Stool Color Decoder for Women
Color alone does not diagnose the cause, but it narrows the suspect list fast. Patients booking stool tests with us often ask which color means what, so our diagnostic team built this quick reference based on US gastroenterology guidance.
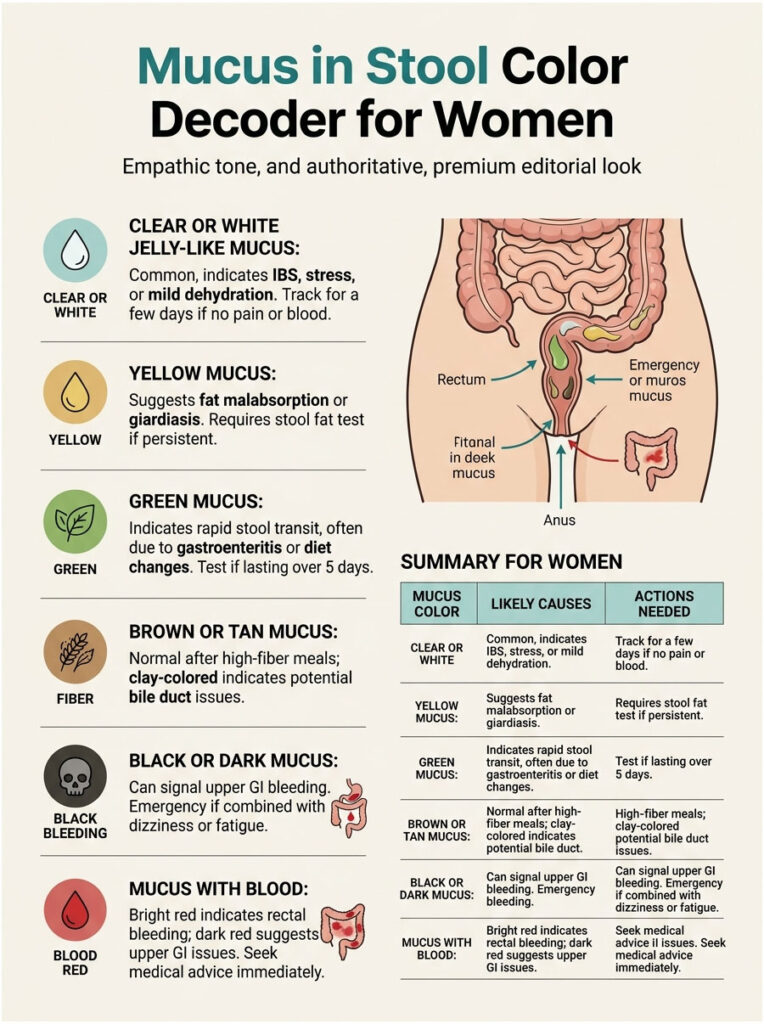
Clear or White Jelly-Like Mucus
This is the most common appearance and the least worrying on its own. Clear or whitish mucus typically points to IBS flare-ups, mild dehydration, slow transit, or stress-related gut irritation. If there is no pain, no blood, and no fever, watch it for a few days.
Yellow Mucus in Stool
Yellow can mean fat malabsorption, an early bacterial or parasitic infection, or in some cases giardiasis (common with well-water and travel exposure). It may come with greasy, floating stools or a foul smell. Yellow mucus lasting more than a week deserves a stool fat test and ova-and-parasite panel.
Green Mucus
Green often means stool moved through your colon too fast for bile to break down completely. This is typical of viral gastroenteritis, food poisoning, or a sudden high-leafy-green diet shift. Persistent green mucus with cramping is a reason to test for bacterial pathogens.
Brown or Tan Mucus
Light brown mucus can be normal residue mixed with stool, especially after a high-fiber meal. If it suddenly looks tan or clay-colored, that points toward bile duct or liver involvement and is not normal.
Black or Dark Mucus
Black, tar-like mucus or stool can indicate bleeding higher in the digestive tract (stomach or small intestine). Iron supplements and bismuth (Pepto-Bismol) also turn stool dark, so check your supplement list first. Black plus dizziness, weakness, or fatigue is an emergency-room visit, not a wait-and-see situation.
Mucus With Blood
Bright red blood streaks suggest rectal-end bleeding, often from hemorrhoids or fissures. Dark red or maroon mucus suggests higher-up GI bleeding. Either pattern combined with mucus warrants a same-day call to your primary care provider or a stool occult-blood test.
Table 1: Mucus Color, Likely Cause, and Action Needed (US Reference Guide)
| Mucus Color | Most Likely Causes | Female-Specific Note | Recommended Action |
| Clear or white jelly | IBS, mild dehydration, stress, slow transit | More common during luteal phase and PMS week | Hydrate, track 7 days, retest if persistent |
| Yellow | Fat malabsorption, giardiasis, mild infection | Pregnant women may see this with prenatal vitamins | Stool test for parasites and fat (book within 7 days) |
| Green | Viral gastroenteritis, food poisoning, fast transit | Cycle-related diarrhea can mimic this | Hydrate with electrolyte solution; test if over 5 days |
| Light brown / tan | Normal residue or bile duct issue | Watch for nausea or right-upper pain | If clay-colored, schedule liver function panel |
| Black or dark | Upper GI bleeding, iron supplements, bismuth | Heavy menstrual bleeders on iron commonly see this | Stop suspected supplement, ER if dizziness present |
| Bloody (red or maroon) | Hemorrhoids, fissures, IBD, infection, polyps | Postpartum hemorrhoids are very common | Same-day GP visit or stool occult blood test |
9 Real Causes of Mucus in Stool in Females
Across patients we serve, these nine causes cover roughly 95% of female mucus-in-stool cases. They are listed by US prevalence, not severity.

1. Irritable Bowel Syndrome (IBS)
IBS is the leading culprit. About half of people with IBS report visible mucus during flare-ups, and women are diagnosed nearly twice as often as men.
The Cedars-Sinai 2023 nationwide study of 88,000 US adults pegged Rome IV IBS prevalence at 6.1%, with women showing significantly higher odds. Stress, certain foods, sleep loss, and the second half of the menstrual cycle make it worse.
IBS comes in three patterns: IBS-C (constipation-dominant), IBS-D (diarrhea-dominant), and IBS-M (mixed). Mucus shows up across all three but is most visible in IBS-D. The reassuring news: IBS does not damage the bowel and does not raise cancer risk.
2. Hormonal Shifts Across the Menstrual Cycle
Estrogen and progesterone tug your gut in opposite directions through the month. Patients booking stool tests with us often report mucus appearing on a predictable cycle-day pattern, which is real, not imagined.
Follicular Phase (Day 1 to ~14)
Estrogen rises, motility speeds up, and bowel movements often feel lighter and more frequent. Mucus is rare here unless an underlying condition is active.
Ovulation (Around Day 14)
Some women feel mid-cycle cramping and looser stools as estrogen peaks and prostaglandins rise. Light, clear mucus is occasionally seen and usually resolves in 24 to 48 hours.
Luteal Phase (Day 15 to ~28)
Progesterone climbs, slows the gut, and constipation becomes more common. Slower transit means more mucus production and more chance of seeing it on stool.
Period (Day 1 to ~5)
Prostaglandins, the same compounds that drive uterine cramping, also stimulate bowel contractions. Diarrhea and visible mucus during your period are extremely common and usually settle within a few days of bleeding starting.
3. Pregnancy: Trimester-by-Trimester
Pregnancy reshapes digestion. Roughly 11 to 38% of pregnant women report constipation, and many notice mucus alongside slow transit.
Our medical team has reviewed common questions across trimesters and what each pattern usually means. A summary by stage:
First Trimester
Rising progesterone slows the gut, prenatal iron supplements harden stool, and morning sickness can dehydrate you. Clear or white mucus is common and rarely concerning unless paired with severe pain or bleeding.
Second Trimester
Many women feel digestive relief here, but food aversions and altered eating patterns can introduce new sensitivities. Sudden mucus with new foods often resolves once the trigger food is removed.
Third Trimester
The growing uterus presses on the rectum, hemorrhoids become common, and pelvic floor strain rises. Mucus from rectal irritation or hemorrhoidal discharge is frequent in late pregnancy.
Mucus combined with bleeding, severe abdominal pain, fever, or contractions should be reported to your OB the same day, regardless of trimester.
4. Endometriosis Affecting the Bowel
Around 5 to 12% of US women of reproductive age have endometriosis, and bowel involvement happens in roughly 5 to 12% of those cases (Remorgida et al., Gut).
When endometrial tissue implants on the rectum or sigmoid colon, it bleeds and inflames cyclically, producing mucus, pain, and altered stool form, often timed to the period.
If your bowel symptoms always cluster around your cycle and include pain with bowel movements, deep pelvic pain, or pain during sex, mention endometriosis to your gynecologist. It is one of the most under-diagnosed causes of mucus in stool in younger women.
5. Food Sensitivities (Lactose, Gluten, FODMAPs, Artificial Sweeteners)
The US gut reacts to a lot of modern food chemistry. Common female-pattern triggers our lab partners report seeing flagged on celiac and food-sensitivity panels include:
- Lactose (about 36% of US adults have some intolerance, per NIH)
- Gluten (celiac disease affects roughly 1 in 100 Americans)
- FODMAPs (fermentable carbs in onion, garlic, wheat, beans, certain fruits)
- Artificial sweeteners like sorbitol, mannitol, and sucralose
- Highly processed and high-fat fast food
Symptoms often peak 2 to 8 hours after the trigger food. Removing the food for 2 weeks and reintroducing it cleanly is the cheapest, fastest diagnostic.
6. Constipation and Pelvic Floor Dysfunction
Hard, dry stool scrapes the gut lining and triggers a defensive mucus response. Add the post-childbirth pelvic floor weakness many US women carry quietly, and you get incomplete emptying, straining, and a coating of mucus on every bowel movement.
Pelvic floor physical therapy is dramatically underused in the United States, despite Medicare and most commercial insurance covering it for postpartum patients. Patients commonly ask us whether they need a referral; in most US states, you do not.
7. Gut Infections (Bacterial, Viral, Parasitic)
Acute gastroenteritis ramps up mucus fast. Common US culprits include norovirus, Salmonella, Campylobacter, Shigella, Clostridioides difficile (especially after antibiotics), and Giardia (well water, daycare, travel). Mucus appears suddenly with diarrhea and often clears in 3 to 7 days.
A red flag specific to women: many infection symptoms (cramping, low pelvic ache, loose stools) overlap with menstrual or yeast-infection symptoms, leading to delayed care. If diarrhea with mucus lasts longer than 5 days or includes fever above 101°F, get a stool culture or PCR panel.
8. Inflammatory Bowel Disease (Crohn’s and Ulcerative Colitis)
IBD is less common than IBS but more serious. The CDC estimates 2.4 to 3.1 million US adults live with IBD, and roughly 1.9 million of them are women (CDC IBD Facts).
Crohn’s disease shows a slight female skew in adulthood; ulcerative colitis is roughly equal between sexes. The IBD red-flag pattern: persistent diarrhea (more than 4 weeks), blood with mucus, weight loss, night-time bowel movements that wake you, fatigue, and joint pain.
Unlike IBS, IBD damages the gut lining and needs prescription treatment. Early diagnosis matters because long-term complications, including colorectal cancer risk, rise with disease duration.
9. Hemorrhoids, Fissures and Anal Irritation
Hemorrhoids are extremely common in women, especially during and after pregnancy. They can leak a clear or slightly yellow mucus along with bright red blood on toilet paper. The mucus comes from the rectum, not the colon, so it usually coats the outside of stool rather than mixing in.
Anal fissures (small tears) cause sharp pain during bowel movements and small amounts of mucus and blood. Most resolve with stool softeners, fiber, sitz baths, and over-the-counter hydrocortisone within 2 to 4 weeks.
IBS vs IBD vs Infection vs Hemorrhoids: Tell Them Apart
The four most common female causes overlap in symptoms but differ sharply in seriousness and treatment. Use this table to gauge which lane you might be in before your appointment.

Table 2: Female-Pattern Comparison with US Prevalence Data
| Condition | US Prevalence in Women | Mucus Pattern | Other Key Symptoms | Source |
| IBS (all subtypes) | ~14 to 21% (Rome IV) | Clear or white, often with flare | Cramping, bloating, alternating constipation and diarrhea | IFFGD |
| IBD (Crohn’s + UC) | ~1.9 million US women | Often bloody mucus, persistent | Weight loss, fatigue, night-time stools, joint pain | CDC |
| Acute gut infection | ~48 million US foodborne illnesses yearly | Sudden onset, may be green or yellow | Fever, vomiting, recent travel or food exposure | CDC FoodNet |
| Hemorrhoids | ~50% of US adults by age 50 | Clear mucus on outside of stool | Bright red blood on paper, itching, pain on sitting | NIDDK |
| Endometriosis (bowel) | ~5 to 12% of women, of which 5 to 12% affect bowel | Cyclical mucus, pain with BM | Painful periods, pain with sex, deep pelvic pain | ACOG |
Red Flags: When Mucus in Stool Is an Emergency
Most of the time, mucus is a nuisance. Sometimes it is the body waving a flag. Knowing which is which is the difference between a wait-and-see week and a same-day visit.
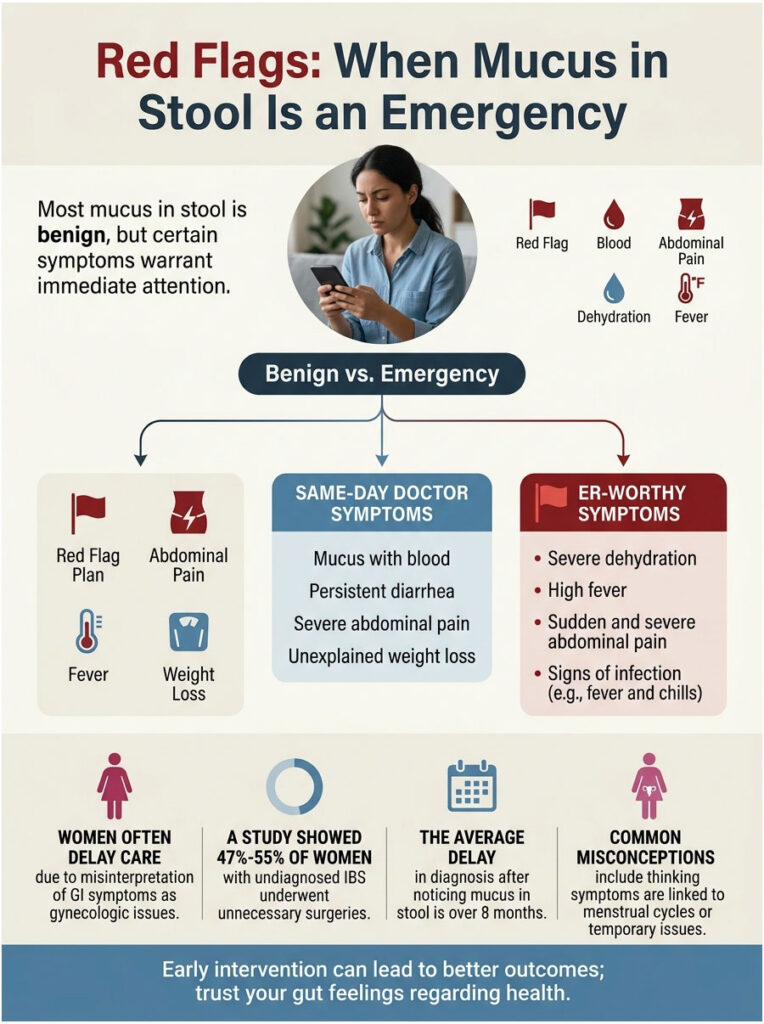
Same-Day Doctor Symptoms
Call your primary care provider or book a same-day visit if you see any of these:
- Mucus with blood (bright red or dark)
- Persistent diarrhea longer than 5 days
- Mucus with unexplained weight loss
- Mucus with fever over 101°F
- New nighttime bowel movements that wake you from sleep
- Severe or worsening abdominal pain
ER-Worthy Symptoms
Go to the emergency department for:
- Black, tarry stools with weakness or dizziness
- Heavy rectal bleeding (more than streaks on paper)
- Severe pain with vomiting and inability to keep fluids down
- Signs of dehydration (no urine for 8+ hours, confusion, racing heart)
- Severe abdominal pain in pregnancy
Why Women Often Delay Care (and Shouldn’t)
A long-standing IFFGD analysis found that women with undiagnosed IBS had hysterectomy or ovarian-surgery rates between 47% and 55%, far higher than female peers without IBS, often because GI symptoms got mistaken for gynecologic problems for years before the right diagnosis was made.
That delay pattern is real, and it costs both time and trust. In cases reviewed by our medical team across our diagnostic network, the average gap between first noticing mucus in stool and ordering the right stool panel is over 8 months.
Most of those delays come from “I thought it was just my period” or “It went away last time, so I waited.” If your gut is talking to you, listen sooner rather than later.
How to Get Rid of Mucus in Stool: A Real Action Plan
For most women, the cause is benign and fixable from home in 2 to 4 weeks. The plan below is what our nutrition and GI consultants recommend most often before ordering tests.

Diet: Foods to Add and Foods to Cut
Add for one month:
- 25 to 30 grams of soluble fiber daily (oats, psyllium husk, chia, ground flax, peeled apples)
- Cooked vegetables before raw ones (easier on flared guts)
- Bone broth or low-FODMAP soups (gentle gut healing)
- Fermented foods if tolerated (plain Greek yogurt, kefir, sauerkraut)
- Lean protein at every meal (eggs, chicken, white fish, tofu)
Cut for two weeks, then reintroduce one at a time:
- Dairy (especially cow’s milk, ice cream)
- Gluten-heavy foods (bread, pasta, baked goods)
- Onion, garlic, beans (high FODMAP)
- Artificial sweeteners (sucralose, sorbitol, mannitol, found in sugar-free gum and many “diet” snacks)
- Alcohol and caffeine over 200 mg per day
Hydration Protocol (US Measurements)
Aim for half your body weight in ounces of water per day as a baseline. A 150-pound woman targets roughly 75 fluid ounces, more if you are pregnant, breastfeeding, exercising, or in a hot climate. Underdrinking is one of the silent drivers of constipation and mucus we see flagged often.
Probiotics That Actually Help Women
US clinical evidence is strongest for strains like Lactobacillus plantarum 299v, Bifidobacterium infantis 35624, and multi-strain blends like VSL#3 (now Visbiome) for IBS-related symptoms. Give any probiotic 4 to 6 weeks before judging if it works. Skip if you are immunocompromised without doctor approval.
Stress and the Gut-Brain Axis
The vagus nerve connects gut and brain in both directions. Chronic stress raises cortisol, slows gut transit, increases inflammation, and amplifies mucus production. Twenty minutes a day of any stress practice (walking, breath work, yoga, prayer, journaling) measurably moves the needle within 4 weeks for most women.
Cycle Tracking Tip for IBS Sufferers
Use a free app or paper chart to log bowel movements, mucus, pain, and food alongside your cycle for 60 days. Patterns that took months to spot become obvious in two cycles. This single habit is the most useful thing patients tell us they did before their GI visit.
Table 3: Symptom Pattern, Recommended Action, and Expected Timeline
| Your Symptom Pattern | Recommended First Step | Expected Timeline to Improvement |
| Clear mucus once or twice, no other symptoms | Hydrate, track 7 days, no action needed | 1 to 7 days |
| Mucus during or before period only | Cycle tracking + magnesium glycinate 200mg/day at night (with doctor OK) | 1 to 2 cycles |
| Mucus + bloating + alternating stools | 2-week low-FODMAP trial + soluble fiber | 2 to 4 weeks |
| Yellow or green mucus with diarrhea > 5 days | Stool culture, ova and parasites, calprotectin panel | Test results in 2 to 5 days |
| Mucus + blood + weight loss + fatigue | Same-day GP visit; likely IBD workup | Diagnostic clarity within 2 to 4 weeks |
| Postpartum mucus with rectal pain or red blood | Stool softeners, sitz bath, OTC hemorrhoid cream, GP visit if no relief in 2 weeks | 2 to 4 weeks |
Tests Doctors Use to Diagnose the Cause
In tests booked through HealthCareOnTime, female patients with mucus complaints most often run one of four panels first. Knowing what to ask for shortens the diagnostic loop.

Stool Studies
The standard first line includes a fecal calprotectin (inflammation marker that helps separate IBS from IBD), fecal occult blood (looks for hidden bleeding), stool culture (bacterial pathogens), and ova and parasites (parasitic exam). A C. difficile toxin test is added if you took antibiotics in the past 60 days.
Blood Tests
A complete blood count, C-reactive protein, ESR, and a celiac panel (tissue transglutaminase IgA + total IgA) cover most of what your provider needs. Iron studies are added if you are bleeding or have heavy periods.
Imaging and Endoscopy
A colonoscopy is the gold standard if IBD or polyps are suspected, and US screening guidelines now start at age 45. A flexible sigmoidoscopy is shorter and looks at just the lower colon. Pelvic MRI is added when endometriosis is on the differential.
What to Expect at the Visit
Bring a 14-day symptom log, a current medication list, and a record of recent travel or antibiotic use. Patients who arrive prepared shave an average of one follow-up visit off the diagnostic process, our intake team has noticed.
When to Book a Test, See a Doctor, or Wait It Out
If symptoms are mild, intermittent, and not paired with red flags, two weeks of the diet and hydration plan above is reasonable. If mucus is still showing up after 14 days, book a stool panel rather than waiting longer.

HealthCareOnTime offers home sample collection for stool tests and full digestive panels in many US cities, which patients tell us removes the biggest barrier to actually getting tested. If a red flag appears at any point, skip the wait-and-see and call your provider the same day.
Mucus by itself is rarely an emergency. Mucus with blood, fever, weight loss, or severe pain is a different signal entirely.
Frequently Asked Questions
Is mucus in stool a sign of cancer in women?
Mucus alone is rarely a cancer sign. Colorectal cancer can cause mucus mixed with blood, weight loss, and a change in bowel habits lasting more than 4 weeks. If you are over 45 (the new US screening age) or have a family history, schedule a colonoscopy regardless of mucus status. For women under 45 with no family history and no red flags, the cancer probability from isolated mucus is very low.
Why do I see jelly-like mucus in my stool?
Jelly-like mucus usually means your gut is producing extra protective coating, often from IBS, mild irritation, slow transit, or a recent food trigger. Clear or white jelly without blood or pain is the most common pattern and typically resolves in a few days. If it persists more than 2 weeks, get a stool calprotectin test to rule out inflammation.
Can my period cause mucus in stool?
Yes. Prostaglandins released from the uterine lining at the start of menstruation stimulate bowel contractions and shift transit speed, often causing diarrhea, mucus, or both during the first 1 to 3 days of your period. This is a normal cycle pattern. If symptoms last beyond your period or worsen each cycle, mention it to your gynecologist; bowel-involved endometriosis can mimic this pattern.
Is mucus in stool normal during pregnancy?
Small amounts are common, especially in the first and third trimester. Slowed digestion from progesterone, prenatal iron supplements, and pressure from the growing uterus all contribute. Mucus combined with bleeding, severe pain, fever, or contractions is never to be ignored and warrants a same-day call to your OB.
How long does mucus in stool usually last?
For most benign causes (food sensitivity, mild stress, cycle-related shifts), mucus clears within 3 to 7 days once the trigger is removed. Infection-related mucus typically resolves in 5 to 10 days. Mucus persisting beyond 14 days, or returning often, deserves a stool panel and provider visit.
Can stress alone cause mucus in stool?
Yes. The gut-brain axis means high cortisol levels, anxiety, and sleep deprivation can directly raise mucus production and shift bowel habits. This is most common in women already prone to IBS. A 30-day stress practice combined with normal sleep often resolves stress-only mucus without medication.
What does yellow mucus in stool mean for a woman?
Yellow mucus can signal fat malabsorption, an early gut infection (giardiasis, bacterial), or in some cases liver or gallbladder issues. It is more likely to need testing if it lasts more than 7 days, comes with greasy or floating stools, or is paired with right-upper abdominal pain. Pregnant women on iron-rich prenatal vitamins sometimes see a yellow tint that is harmless.
Can perimenopause cause mucus in poop?
Yes. Estrogen fluctuations during perimenopause shift gut motility and sensitivity, and many women develop new IBS-pattern symptoms, including mucus, in their 40s and 50s. If you also have new constipation, weight changes, or sleep disruption, talk to your provider; perimenopause-pattern GI changes respond well to fiber, hydration, and sometimes hormone therapy when appropriate.
Does endometriosis cause mucus in stool?
Bowel endometriosis can. About 5 to 12% of women with endometriosis have bowel involvement, and they often see cyclical mucus, pain with bowel movements, deep pelvic pain, and sometimes blood, all timed around the period. If your bowel symptoms cluster on your cycle, ask a gynecologist about endometriosis evaluation.
Is mucus in stool with no pain or blood serious?
Usually not. Painless, blood-free mucus is the most common pattern and typically traces back to IBS, food sensitivity, hydration, or stress. Track it for 14 days; if it does not clear with diet and hydration adjustments, book a stool panel for peace of mind.
Can probiotics get rid of mucus in stool?
Sometimes. Targeted strains (Bifidobacterium infantis 35624, Lactobacillus plantarum 299v, multi-strain blends like Visbiome) have the strongest US evidence for reducing IBS-related mucus and bloating. Allow 4 to 6 weeks before deciding it is not working. Probiotics are not a fix for IBD or active infection.
When should a woman see a doctor about mucus in stool?
See a doctor if mucus lasts more than 14 days, comes with blood, fever above 101°F, severe pain, unintended weight loss, or nighttime bowel movements that wake you. Pregnant women should call their OB the same day for any mucus paired with bleeding, severe pain, or fever.
Disclaimer: This article is for educational purposes only and is not a substitute for professional medical evaluation, diagnosis, or treatment. Always consult a licensed healthcare provider regarding any digestive symptoms, especially during pregnancy or if you have a chronic condition. The information here reflects general US clinical guidance and should not be used to delay or replace personalized care. HealthCareOnTime offers diagnostic lab testing across the United States; bookings are facilitated through our partner network and do not constitute a doctor-patient relationship.
References
- Centers for Disease Control and Prevention. IBD Facts and Stats. 2024.
- Almario CV, et al. Prevalence and Burden of Illness of Rome IV IBS in the United States. Gastroenterology, 2023.
- International Foundation for Gastrointestinal Disorders. IBS Facts and Statistics.
- Crohn’s & Colitis Foundation. INPUT Study on US IBD Prevalence. 2023.
- Canavan C, et al. The epidemiology of irritable bowel syndrome. Clin Epidemiol, NIH/PMC.
- Cleveland Clinic. Mucus in Stool: Causes & When to Be Concerned.
- Mayo Clinic. Mucus in stool: A concern?
- Johansson ME, Hansson GC. Mucus production and function in the gastrointestinal tract. Nat Rev Gastroenterol Hepatol, 2011.
- Ohman L, Simrén M. Mucus production in irritable bowel syndrome. J Gastroenterol, 2007.
- Remorgida V, et al. Gastrointestinal tract endometriosis: a systematic review. Gut, 2008.
- National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). Hemorrhoids.
- American College of Obstetricians and Gynecologists (ACOG). Endometriosis.