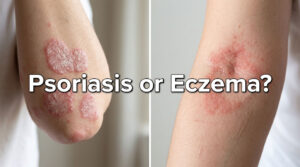
About one in three American adults walked into 2025 with a diagnosed allergic condition, according to fresh data released by the CDC in January 2026. That same year, the average US adult will also catch two or three colds. The kicker? On day one, both can feel nearly identical at 6 AM when you’re standing at the bathroom mirror trying to figure out what hit you.
Table of Contents
| Quick Answer: A cold usually starts gradually with a sore throat, develops into congestion, runny nose, and cough, and clears in 7 to 10 days. Allergies hit fast after exposure, often include itchy eyes and throat, and last as long as the trigger sticks around. Itchy eyes plus clear watery mucus for weeks signals allergies. Body aches, low fever, or discolored mucus signals a cold. |

| At a Glance • Colds are caused by viruses; allergies are an immune reaction to harmless triggers. • Itchy eyes and an itchy throat point to allergies, not a cold. • A fever rules allergies out entirely. • Colds resolve within about two weeks; allergies can drag on for months. • Treatment is completely different, so guessing wrong wastes money and time. • 25.2% of US adults have diagnosed seasonal allergies (CDC, 2024). • When in doubt, an IgE blood test or skin prick test can settle it within days. |
The Fast Way to Tell a Cold From Allergies
Cold or allergies looks like the same problem on the surface. Both hit your nose, throat, and eyes. The trick is reading the signals your body sends, not just the obvious overlap.

What a Cold Actually Is
A cold is a viral infection of your upper airway, set off by one of more than 200 respiratory viruses. Rhinoviruses cause most US cases, with adenoviruses, common human coronaviruses, parainfluenza viruses, and enteroviruses filling out the lineup.
Symptoms usually peak 2 to 3 days after exposure and fade within 7 to 10 days. Colds are contagious, often picked up from a co-worker, a kid at daycare, or a contaminated doorknob.
What Allergies Actually Are
Allergies are an immune response, not an infection. Your body has decided that pollen, dust mites, pet dander, or mold spores are dangerous invaders. So it releases histamines, which trigger the swelling, sneezing, and itching you feel.
Allergies are not contagious. They appear minutes after exposure and stop only when the trigger is removed or treated.
60-Second Self-Check
Three quick questions usually settle the cold vs allergies debate before you reach for any medicine.
- Are your eyes or throat itchy? Itch is the single most reliable allergy marker.
- Do you have a fever, even a low one? If yes, it’s a cold (or flu, or worse), not allergies.
- How long has this lasted? Past day 14, allergies become the prime suspect.
Our medical reviewers at HealthCareOnTime see this exact triage play out in patient questions almost every week during US allergy season. Two minutes of self-questioning often beats a $200 urgent-care visit.
| Symptom | Cold | Seasonal Allergies | Year-Round Allergies |
| Onset | Gradual over 1 to 3 days | Within minutes of exposure | Persistent, year-round |
| Duration | 7 to 10 days, up to 14 | Weeks during pollen season | Ongoing until trigger removed |
| Fever | Sometimes, low-grade | Never | Never |
| Itchy eyes, nose, throat | Rare | Very common | Common |
| Mucus | Clear early, may turn yellow or green | Clear and watery | Clear |
| Sore throat | Common, scratchy | Sometimes, mild | Sometimes |
| Body aches | Common, mild | Never | Never |
| Contagious | Yes | No | No |
Table 1: Cold vs allergies symptom comparison. Sources: Mayo Clinic Health System, CDC, NIH News in Health.
Why It Matters: US Numbers You Should Know
Misreading a cold as allergies (or the reverse) is more than a personal annoyance. It’s a national pattern that costs Americans billions every year and a lot of unnecessary time off work.

How Common Are Allergies and Colds in America?
In 2024, 31.7% of US adults had a diagnosed seasonal allergy, eczema, or food allergy, per the CDC National Center for Health Statistics. Roughly 1 in 4 adults specifically reported seasonal allergies.
Among American kids ages 0 to 17, 29.5% have at least one diagnosed allergy, and 20.6% deal with seasonal allergies. Children in non-metro counties get hit harder, at 25.6%. Patients booking tests with us often find their kids fall into this rural-county category without realizing higher exposure to grass and tree pollens drives the risk.
The common cold is even more universal. The CDC says US adults average two to three colds per year, while kids average six to eight. Together that adds up to an estimated one billion cold cases in the US each year.
How the Two Seasons Now Overlap
Cold season used to run November through March. Allergy season ran March through October. They barely shook hands.
That’s changed. Warmer winters across the Sun Belt and Southeast have pushed pollen counts up weeks earlier, and the cedar, tree, and grass allergens that follow now overlap heavily with respiratory virus season. Texas Health reported unusually early pollen surges in North Texas in early 2026, and similar patterns are showing up across Georgia, Arizona, and the Carolinas.
The practical effect: in February or October you can genuinely have a cold and an allergy flare running at the same time, which is why so many patients describe a “cold” that never ends.
| Condition | US Prevalence / Volume | Annual Impact | Source |
| Seasonal allergy (adults) | 25.2% of US adults (~66 million) | 4.1M physician visits/year | CDC NCHS, 2024 |
| Seasonal allergy (kids 0-17) | 20.6% of US children | Top reason for missed school days | CDC NCHS, 2024 |
| Eczema (adults) | 7.7% | Higher in women (9.5% vs 5.7%) | CDC NCHS, 2024 |
| Food allergy | 6.7% adults; 5.3% children | ~$25B/year family burden | FARE / CDC |
| Common cold (US adults) | 2 to 3 colds/year/adult | 75 to 100M MD visits; $7.7B cost | CDC |
| Cold-related work loss | 150M+ workdays missed | Over $20B economic impact | NIH / NLM |
Table 2: USA prevalence and economic impact of allergies vs colds.
Across the diagnostic network our lab partners support, allergy panel orders climb noticeably in March and again in September, right when patients are most likely to confuse the two conditions and self-medicate the wrong way.
Symptom Decoder: 9 Clues Your Body Is Giving You
Skip the guesswork. Run your symptoms through these nine signals and the cold or allergies question usually clears up fast.

Clue 1: How It Started (Sudden vs Gradual)
A cold creeps in. Day 1 you have a scratchy throat, day 2 sneezes start, day 3 you’re stuffed up and tired.
Allergies hit fast. You walk outside, mow a lawn, pet a friend’s cat, and within minutes your nose is running like a faucet. The timing alone often gives the answer away.
Clue 2: Itchy Eyes, Nose, or Throat
Itch is the single clearest tell. Watery, itchy eyes almost never happen with a cold. They’re a hallmark of allergic rhinitis.
If you find yourself rubbing your eyes, scratching the roof of your mouth, or feeling that crawling itch at the back of your throat, you’re looking at an allergy response. Patients commonly describe it as “the inside of my ear itches,” which is unique to allergies.
Clue 3: Fever or No Fever
Allergies never cause a fever, period. Not even a low-grade one.
Colds occasionally bring a low fever, especially in kids. A temperature above 100.4°F leans more toward flu, COVID-19, or RSV, and that’s worth checking with a rapid test from your local CVS or Walgreens.
Clue 4: Body Aches
Aching muscles, a heavy head, that “wrecked” feeling? Cold or flu territory. Allergies don’t produce systemic body aches.
A few patients describe a tired or drained feeling with severe allergies, but it’s not the same as the bone-deep ache of a viral infection. If you’re hurting all over, you’re not dealing with hay fever.
Clue 5: Mucus Color and Texture
Watery, clear, thin mucus that doesn’t change color over days suggests allergies.
Cold mucus starts clear, then often turns yellow or green by day 3 or 4 as your immune system fights the virus. Color alone isn’t a perfect rule (green doesn’t always mean a bacterial infection), but it’s a useful piece of the puzzle when stacked with the other clues.
Clue 6: Duration (the 14-Day Rule)
Mayo Clinic’s most useful tip: most colds resolve in 7 to 14 days. Anything that drags on past two weeks is more likely allergies, a sinus infection, or both.
In tests booked through HealthCareOnTime, patients whose “cold” has lasted three or more weeks frequently turn out to have undiagnosed environmental allergies plus a secondary sinus issue. The fix often requires treating both at once, not just one.
Clue 7: Time of Day and Year
Spring and early fall, outdoors, near grass, trees, or ragweed: think pollen.
January through March, indoors, sharing space with kids or co-workers: think rhinovirus. Indoor allergies (dust mites, mold, pet dander) can hit year-round, especially when the heat or AC kicks on and stirs up particles. Morning-only symptoms often point to dust mites in the bedding.
Clue 8: Who Else in the House Has It
Colds spread. If your spouse, kids, or office have a matching set of symptoms within 3 to 5 days, you’re dealing with a virus.
Allergies don’t spread person to person. Two family members can flare at the same time if both are reacting to the same trigger (pollen, the new puppy, the carpet you just installed), but that’s exposure, not contagion.
Clue 9: Response to Antihistamines
This is the diagnostic shortcut your doctor uses too. A loratadine (Claritin), cetirizine (Zyrtec), or fexofenadine (Allegra) taken in the morning that wipes out your symptoms by lunch points strongly toward allergies.
If your symptoms barely budge after a second-generation antihistamine, you’re probably fighting a virus, and rest, fluids, and symptom relievers will serve you better than any allergy pill.
When You Should Get Tested (Not Guess)
For most people, the nine clues above will resolve the cold or allergies question in under five minutes. There’s a real category of patients, though, who genuinely benefit from testing instead of guessing.
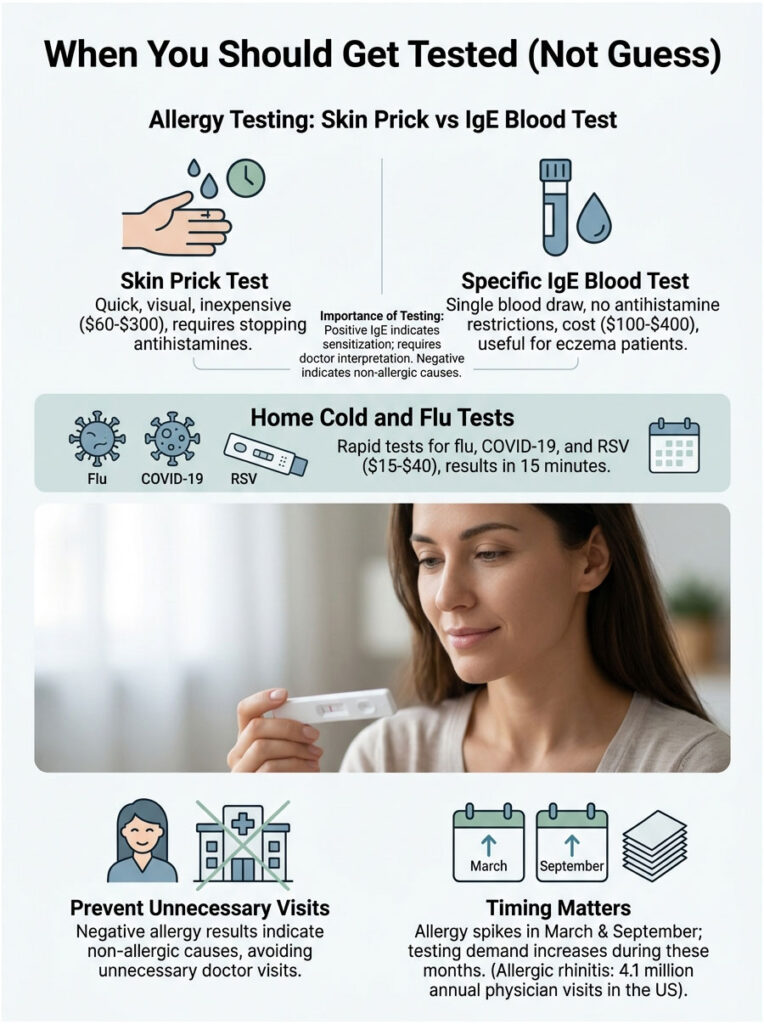
Allergy Testing: Skin Prick vs IgE Blood Test
Two main options dominate the US market.
Skin Prick Test
An allergist places small drops of suspected allergens on your forearm or back, then pricks the skin so the drop enters the top layer. A welt within 15 to 20 minutes confirms an allergy to that substance.
This test is fast, visual, and inexpensive in many US clinics, typically running $60 to $300 depending on the number of allergens tested. It does require stopping antihistamines for about a week beforehand, which is the main drawback.
Specific IgE Blood Test
A single blood draw is screened against panels of common allergens. The lab measures specific Immunoglobulin E antibodies against each one. No need to stop antihistamines first, no risk of a skin reaction, and excellent for patients with eczema or those who can’t tolerate skin testing.
Our lab partners report that specific IgE panel orders rise sharply in March and September across the US-facing diagnostic network we serve, matching the two big allergy spikes. Cost in the US typically ranges from $100 to $400 depending on panel breadth, often partially covered by insurance.
Cold and Flu Combo Tests at Home
Rapid at-home tests for flu, COVID-19, and RSV are now widely available across US pharmacies (CVS, Walgreens, Walmart). They run $15 to $40 per test and give results in 15 minutes.
A rapid test is the cleanest way to rule out flu and COVID-19 if you’re not sure whether you’ve got “just a cold.” That single result can change how you treat the next 48 hours.
What Lab Results Actually Tell You
A positive IgE test confirms sensitization to a specific allergen but doesn’t always mean clinical allergy. Your doctor interprets results alongside symptoms.
A negative result, especially across a broad panel, is highly reassuring and often points you toward viral or non-allergic rhinitis as the cause. Roughly 4.1 million US physician office visits per year list allergic rhinitis as the primary diagnosis (CDC NAMCS). Catching the correct cause early saves repeated doctor visits and wasted prescriptions.
Treatment That Actually Works
This is where guessing wrong costs the most. Cold meds and allergy meds aren’t interchangeable, even though they share a few ingredients.

Treating a Cold
There’s no cure for a cold. Treatment focuses on making the 7 to 10 days more livable.
What helps: rest, fluids (water, broth, herbal tea), saline nasal spray, throat lozenges, acetaminophen (Tylenol) or ibuprofen (Advil) for aches, and a humidifier in the bedroom. Honey in tea works for cough in adults and children over age 1.
What doesn’t: antibiotics. Colds are viral. Antibiotics do nothing and contribute to resistance. Skip them unless a doctor diagnoses a bacterial complication.
Treating Seasonal Allergies
The goal is to block or calm the immune response.
First-line: a second-generation oral antihistamine (loratadine, cetirizine, fexofenadine, levocetirizine). These don’t cause drowsiness for most people and run $10 to $25 for a 30-day supply in US drugstores.
Add-on: a nasal corticosteroid spray (Flonase, Nasacort, Rhinocort) for stuffy nose and post-nasal drip. Best results come from daily use during your allergy season, not “as needed.”
For itchy, watery eyes: antihistamine eye drops like ketotifen (Zaditor) or olopatadine (Pataday).
OTC Medications Compared (USD Pricing)
| Product | Active Ingredient | Use For | Approx US Cost | Best Time |
| Claritin | Loratadine | Allergies | $15 to $25 / 30 ct | Morning |
| Zyrtec | Cetirizine | Allergies | $15 to $25 / 30 ct | Morning or evening |
| Allegra | Fexofenadine | Allergies | $20 to $30 / 30 ct | Morning |
| Xyzal | Levocetirizine | Allergies (nighttime) | $20 to $30 / 35 ct | Evening |
| Benadryl | Diphenhydramine | Severe acute allergy (drowsy) | $8 to $15 / 100 ct | Short-term only |
| Sudafed | Pseudoephedrine | Cold or allergy congestion | $10 to $18 / 24 ct | Daytime, short-term |
| Flonase / Nasacort | Fluticasone / Triamcinolone | Allergies | $18 to $28 / 120 sprays | Daily |
| Mucinex | Guaifenesin | Cold mucus | $15 to $25 | With water |
| DayQuil / NyQuil | Combination cold relief | Cold | $10 to $18 | Day or night |
Reading the label matters. Combination cold products often stack acetaminophen with other ingredients, so adding a separate Tylenol can quietly push you over the safe daily dose. Our clinical reviewers see this accidental overdose pattern in patients far more often than people realize.
Prescription Options
If OTC products don’t deliver enough relief, several prescription pathways are worth discussing with an allergist or primary care doctor.
- Montelukast (Singulair): Oral leukotriene inhibitor for allergies plus mild asthma. The FDA placed a black-box warning on it in 2020 for neuropsychiatric side effects, so it’s not a first-line pick.
- Allergy immunotherapy (shots or sublingual tablets): Long-term retraining of the immune system. Effective for confirmed pollen, dust mite, or grass allergies, but takes 3 to 5 years.
- Biologics like Xolair (omalizumab): Approved by the FDA in 2024 for certain food allergies, with older approvals for chronic hives and severe allergic asthma.
Home Remedies That Hold Up to Science
A few traditional remedies actually do something measurable.
- Saline rinses with a Neti pot or NeilMed bottle reduce sinus congestion in both cold and allergy patients. Use distilled or previously boiled water; the FDA has issued warnings about tap water risks.
- Steam inhalation gives short-term relief from nasal stuffiness.
- Honey calms a nighttime cough as well as some OTC syrups in adults and older kids.
- Sleep, hydration, and a humidifier are quietly the highest-impact home remedies you have.
What Doesn’t Work
Mega-doses of vitamin C don’t shorten an active cold. Zinc lozenges may shave a day off duration in some studies but cause nausea and a metallic taste in many users.
Antihistamines won’t help a true viral cold once it’s underway, except for the sedating side effects of older drugs like Benadryl, which is why they show up in nighttime cold mixtures.
What to Do Tonight: A Practical Action Plan
The decision matrix below covers the cold vs allergies situations our team gets asked about most often.

| Your Situation | Most Likely Cause | What to Do First | When to Escalate |
| Itchy eyes, clear runny nose, no fever, comes on outdoors | Seasonal allergies | Daily Claritin/Zyrtec/Allegra + Flonase | If no relief in 7 days, see an allergist |
| Sore throat day 1, congestion day 2, body aches, low fever | Common cold | Rest, fluids, acetaminophen, saline spray | If symptoms persist past 14 days |
| Fever over 100.4°F, chills, severe body aches | Likely flu, RSV, or COVID-19 | Rapid home test, hydration, rest | High fever, breathlessness, chest pain |
| “Cold” that won’t quit after 3 weeks | Possible allergies, sinusitis, or both | Book an IgE blood test | If facial pain, thick yellow-green mucus |
| Itchy nose, clear mucus, sneezing fits in spring or fall | Almost certainly allergies | OTC antihistamine + check pollen count | If wheezing or chest tightness develops |
| Indoor-only symptoms, worse in morning | Dust mite or mold allergy | Allergy-proof bedding, dehumidifier | If symptoms disrupt sleep regularly |
| Symptoms spread to spouse and kids in 3 days | Almost certainly viral | Treat each person’s symptoms; isolate | Anyone with fever above 102°F or trouble breathing |
Table 3: Decision matrix for common cold or allergies situations.
Special Situations
A few groups need a different playbook for the cold or allergies question.
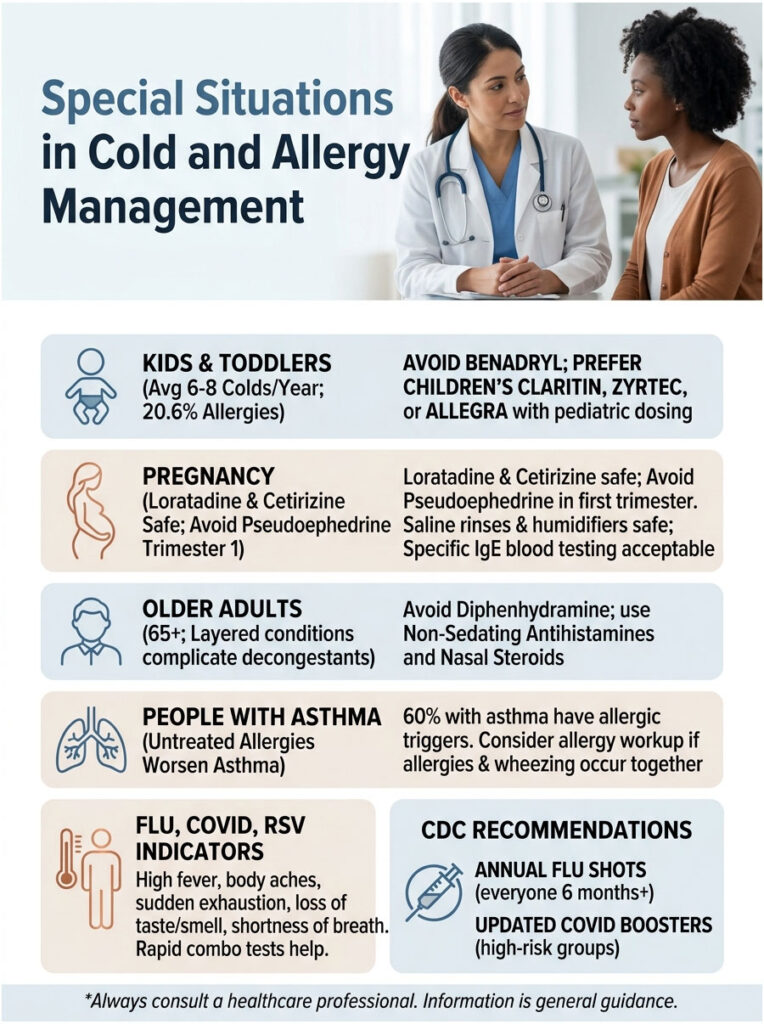
Kids and Toddlers
Children get 6 to 8 colds a year on average, and 20.6% of US kids have diagnosed seasonal allergies. Benadryl can cause hyperactivity in kids under 6 and should be avoided as a first-line allergy med.
Children’s Claritin, Zyrtec, or Allegra in pediatric dosing is generally preferred. Always check with a pediatrician before giving any cold or allergy product to a child under 4.
Pregnancy
Many pregnant patients are wary of taking anything. Most US OB-GYNs clear loratadine (Claritin) and cetirizine (Zyrtec) as safer choices during pregnancy, while pseudoephedrine is usually avoided in the first trimester.
Saline rinses, humidifiers, and rest are universally safe. Patients commonly ask us whether allergy testing is safe during pregnancy. Specific IgE blood testing is, since it’s a routine blood draw with no allergen exposure.
Older Adults (65+)
Seniors often have layered conditions (high blood pressure, prostate issues, glaucoma) that complicate decongestant use. Older antihistamines like diphenhydramine sit on the American Geriatrics Society Beers List as drugs to avoid in this group because of fall risk and confusion.
Non-sedating second-generation antihistamines and nasal steroids are the safer route for adults over 65.
People With Asthma
Untreated allergies can worsen asthma control. Around 60% of US adults with asthma have at least one allergic trigger, per the Asthma and Allergy Foundation of America.
If allergies and wheezing show up together, an allergy workup is worth doing rather than treating the asthma alone.
When It’s Probably Flu, COVID, or RSV Instead
High fever above 101°F, intense body aches, sudden exhaustion, loss of taste or smell, or shortness of breath all point away from a routine cold and away from allergies. A rapid combo test at home is the fastest way to sort it out.
CDC guidance still recommends an annual flu shot for everyone 6 months and older, and updated COVID-19 boosters for high-risk groups.
When to See a Doctor

Red flags that mean it’s time to get evaluated:
- Fever above 102°F or lasting more than 3 days
- Trouble breathing, wheezing, or chest pain
- Sinus pain, facial swelling, or pus-like discharge for more than 10 days
- Severe sore throat, especially with white patches (possible strep)
- Symptoms lasting more than 14 days with no improvement
- An allergic reaction with swelling of the lips or tongue or trouble swallowing (this is anaphylaxis; call 911)
For anything in the gray zone, a primary care visit or a telehealth appointment is enough. Cases reviewed by our clinical team show that early evaluation cuts both treatment costs and recovery time, especially when the cold or allergies confusion has dragged on for weeks.
Frequently Asked Questions
Can allergies cause a fever?
No, allergies don’t cause a fever. The immune reaction in allergies releases histamines, but it doesn’t trigger the fever response your body uses to fight viruses. If you have a fever along with sneezing or congestion, you’re looking at a cold, flu, COVID-19, RSV, or a sinus infection. A temperature above 100.4°F is a strong signal to test for flu and COVID-19 at home.
How long does a cold last vs allergies?
A typical cold runs 7 to 10 days, with some lingering up to two weeks. Allergies last as long as you’re exposed to the trigger. Seasonal allergies can drag on for 6 weeks or more during peak pollen season, while year-round indoor allergies may not let up until the trigger is removed or treated. Mayo Clinic uses the 14-day rule: anything beyond two weeks is more likely allergies, sinusitis, or both.
Why do my allergies feel like a sinus infection?
Allergies cause inflammation in the same nasal and sinus tissues that bacterial sinus infections inflame. Both produce congestion, facial pressure, and post-nasal drip. The difference is that allergy mucus is usually clear and watery, while sinus infection mucus turns thick, yellow, or green and is often accompanied by facial pain and fever. Untreated allergies can actually lead to recurrent sinus infections, so chronic “sinus issues” often deserve an allergy workup.
What color is allergy mucus?
Allergy mucus is typically clear, thin, and watery. Cold mucus starts clear and often turns yellow or green after a few days as your immune system breaks down the virus. Color alone isn’t a perfect diagnostic clue (green doesn’t always mean bacteria), but combined with itchy eyes and a fast onset, clear watery mucus strongly suggests allergies. Thick, discolored mucus with facial pain is worth a doctor visit.
Can you have a cold and allergies at the same time?
Yes, and it happens more often than people realize. Your immune system is busy fighting a virus while still reacting to environmental triggers. The two conditions amplify each other, with allergy-driven inflammation making cold symptoms feel worse and slower to clear. If a “cold” hits during peak pollen season and lingers unusually long, mixed cold-plus-allergies is a likely explanation. Treating both at once is usually the fastest way to feel better.
Do antihistamines work on cold symptoms?
Partially. Older first-generation antihistamines like diphenhydramine (Benadryl) can dry up a runny nose and help you sleep, which is why they show up in NyQuil and similar nighttime cold mixes. Second-generation antihistamines (Claritin, Zyrtec, Allegra) target histamine-driven allergy symptoms and won’t do much for a true viral cold. If a non-drowsy antihistamine wipes out your symptoms quickly, you were almost certainly fighting allergies.
When should I get an allergy test in the US?
Consider an allergy test if your symptoms last longer than 6 weeks, repeat at the same time each year, don’t respond to OTC antihistamines, or interfere with sleep, work, or school. A specific IgE blood test or skin prick test pinpoints the exact triggers so you can target treatment instead of guessing. Patients booking allergy panels with us often discover unexpected indoor triggers (dust mites, mold) that explain years of “winter colds.”
Is my sore throat from allergies or a virus?
A cold sore throat is usually sharper, scratchier, and worse when you swallow, often the first symptom of the cold. An allergy sore throat is milder, often described as a tickle or a feeling of post-nasal drip running down the back of the throat. Allergy sore throats tend to be worse in the morning or after time spent in dusty or pollen-heavy environments. A severe sore throat with white patches and fever could be strep and needs a test.
Why are my allergies worse this year?
Several US-specific factors are pushing allergy seasons longer and more intense. Warmer winters mean earlier and heavier pollen production across the South and Southeast. Higher overall CO2 levels boost pollen output from grasses and ragweed. Climate-shifted growing seasons in cities like Atlanta, Phoenix, and Dallas now produce pollen weeks earlier than a decade ago. If a typically mild year now hits hard, the environment is doing more of the work than your body.
Can allergies cause body aches?
True body aches are a cold or flu signal, not an allergy one. Some people with severe allergies report fatigue, brain fog, or general malaise that can feel similar, but the deep muscle and joint ache of a viral infection is not part of the allergy picture. If you have body aches along with sniffling, a cold, flu, COVID-19, or RSV is far more likely than allergies, and a rapid home test will sort it out.
Do allergies go away with age?
Sometimes, yes. Many children outgrow milk, egg, or wheat allergies by adolescence. Adult allergies tend to be more persistent, but symptom severity can shift as immune system reactivity changes with age. New allergies can also appear after age 30, often linked to a move to a new region or a new pet. Annual or biannual IgE retesting helps track changes if symptoms shift noticeably.
When should I worry about a cold lasting too long?
Past the 10-day mark, a cold that isn’t slowly improving deserves a closer look. Symptoms that worsen after day 7, fever returning after a few good days, severe facial pain, or thick discolored mucus all suggest a bacterial sinus infection that may need antibiotics. Symptoms lingering past 14 days with no improvement increase the chances of allergies, sinusitis, or an underlying issue worth diagnosing.
| Disclaimer: This article is for general health education and is not medical advice. Symptoms vary widely, and what looks like a routine cold or allergy can occasionally be a more serious condition. Talk to a licensed US healthcare provider for diagnosis and treatment specific to your situation. If you have a high fever, trouble breathing, severe facial swelling, or any signs of anaphylaxis, call 911 or go to your nearest emergency room. |
References
- Centers for Disease Control and Prevention. About Common Cold.
- CDC NCHS Data Brief 545. Diagnosed Allergic Conditions in Adults: United States, 2024.
- CDC NCHS Data Brief 546. Diagnosed Allergic Conditions in Children Ages 0-17: United States, 2024.
- CDC FastStats: Allergies and Hay Fever.
- NIH News in Health. Cold, Flu, or Allergy?
- Mayo Clinic Health System. Is it an allergy or a common cold?
- Mayo Clinic. COVID-19, cold, allergies and the flu: What are the differences?
- Texas Health Resources. Spring Allergies vs. Cold: How to Tell the Difference.
- FoodAllergy.org (FARE). Facts and Statistics.
- GoodRx. Allergies or Cold? How to Tell the Difference.
- Asthma and Allergy Foundation of America. Allergy Symptoms.