A 72-year-old in Tampa books a digestive panel. She has not had a normal bowel movement in 9 days. Her grocery list looks healthy on paper: yogurt, white rice, bananas, deli turkey, cottage cheese. The lab work comes back clean. The problem sits in her cart, not her bloodstream. Her daily fiber intake totals 11 grams. She needs 22.
Table of Contents
This story repeats across the country. The Administration for Community Living reports that 95% of older Americans fall short on fiber, and chronic constipation now affects roughly one in three adults past 60. The fix is rarely a prescription. It usually waits in the produce aisle, the bulk bins, and the cereal box already in the kitchen.

Quick Answer: The best high-fiber foods for seniors include raspberries, pears with skin, prunes, lentils, black beans, oatmeal, brown rice, broccoli, sweet potatoes, chia seeds, and ground flax. Adults over 60 should target 22 grams of fiber daily for women and 28 grams for men, paired with 6 to 8 cups of water. Increase fiber gradually over 2 to 3 weeks to avoid bloating or gas.
At a Glance:
• USDA target for adults 51+: 22g (women), 28g (men) per day
• 95% of older Americans fall below the recommended fiber intake
• Top food per gram: cooked lentils at 15.6g per cup
• Fastest food fix: 5 prunes daily for stubborn constipation
• Hydration target: 6 to 8 cups of water per day
• Most overlooked sources: ground flax, chia seeds, edamame, dates
• Fiber works best when paired with movement, hydration, and a steady morning bathroom window
Why Seniors Are Hit Harder by Constipation
Aging shifts digestion in ways most people never feel coming. Muscle contractions in the colon slow down. The pelvic floor weakens. Signals between gut and brain quiet down. Stools sit longer, the colon reabsorbs water, and what eventually passes is dry and hard.

The American Gastroenterological Association reports that nearly 33% of adults over 60 deal with chronic constipation, with women affected at higher rates than men. The U.S. laxative market exceeds $1.7 billion in annual sales, a number that maps the size of the problem more than the strength of the solution.
The Aging Digestive System
Smooth-muscle contractions in the intestine, called peristalsis, weaken with each passing decade. Transit time stretches from a typical 24 to 36 hours in younger adults to 48 hours or more in many seniors. The longer stool sits, the drier it becomes, and the harder it is to pass.
Anal sphincter strength also declines. So does the rectal sensation that tells you it is time to go. A senior may feel no urge until the bowel is fully loaded, by which point the stool is already too dry for an easy pass.
Medications That Quietly Trigger Constipation
Many common senior prescriptions slow the bowel. The biggest offenders are opioid pain medications (codeine, oxycodone, hydrocodone), calcium channel blockers (amlodipine, diltiazem), anticholinergic drugs (oxybutynin, certain antihistamines), iron supplements, certain antidepressants, and antacids containing aluminum or calcium.
Patients booking GI panels through HealthCareOnTime often discover their constipation tracks back to a medication added in the past 6 months, not a sudden diet shift. A medication review with the prescribing doctor is a worthwhile first step before assuming food alone is the cause.
Hidden Contributors Most People Miss
Reduced thirst sensation, smaller meal sizes, dental issues that limit raw produce, and a sedentary day all stack the odds. Loss of teeth or ill-fitting dentures push seniors toward soft, processed foods that strip fiber out of the plate. Fluid intake often drops by half, sometimes because getting up to use the bathroom feels harder.
A low-fiber diet remains the single most modifiable factor in senior constipation, according to the HealthInAging.org caregiver guide. Fix the plate, and most of the rest improves on its own.
How Much Fiber Do Seniors Actually Need?
Daily fiber targets shift with age, sex, and calorie intake. The 2020 to 2025 USDA Dietary Guidelines for Americans set the rule at 14 grams of fiber per 1,000 calories consumed. For most seniors, that translates to 22 to 28 grams a day.
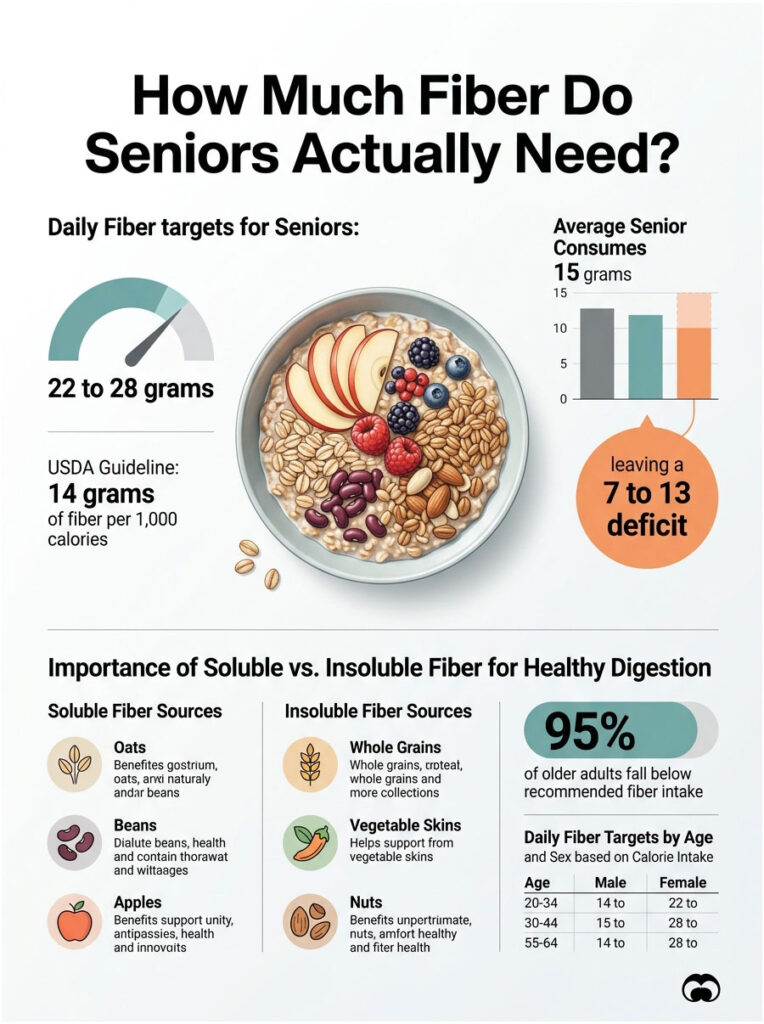
The National Institute of Diabetes and Digestive and Kidney Diseases recommends 22 to 34 grams daily for adults, with seniors landing in the lower half of that range due to typically smaller calorie needs. Yet USDA NHANES data show the average American senior consumes about 15 grams a day, leaving a 7 to 13 gram gap that constipation fills.
Soluble Versus Insoluble Fiber: Why You Need Both
Soluble fiber dissolves in water and forms a gel that softens stool. It lives in oats, beans, apples, citrus, psyllium, and chia seeds. Insoluble fiber adds bulk and pushes things along; you find it in wheat bran, whole grains, vegetable skins, nuts, and seeds.
Healthy bowels run on a mix of both. Soluble alone makes stool soft but slow; insoluble alone moves volume but can feel rough on a sensitive senior gut. Across patients we serve in nutrition consults at HealthCareOnTime, the seniors with the easiest bowel patterns are the ones eating from both categories at every meal.
The 14-Grams-Per-1,000-Calories Rule, in Practice
A senior woman eating 1,800 calories needs 25 grams of fiber by the rule (1.8 x 14). A senior man eating 2,200 calories needs 31 grams. Most major U.S. authorities round these numbers down to 22 and 28 grams to keep the targets achievable.
If your appetite has shrunk to 1,400 calories a day (common after 75), you can drop the fiber goal to about 20 grams. The rule scales with intake, which is why pushing past 50 grams a day on a small calorie budget can backfire.
Table 2: Daily Fiber Targets by Age, Sex, and Calorie Level
| Age Group | Sex | Daily Calories | Fiber Target | Source |
| 51 to 70 | Women | 1,600 to 1,800 | 22 grams | USDA Dietary Guidelines 2020-2025 |
| 51 to 70 | Men | 2,000 to 2,200 | 28 grams | USDA Dietary Guidelines 2020-2025 |
| 71 and older | Women | 1,600 | 22 grams | USDA Dietary Guidelines 2020-2025 |
| 71 and older | Men | 2,000 | 28 grams | USDA Dietary Guidelines 2020-2025 |
| Adults 51+ (alt) | Women | Variable | 21 grams | Nat. Resource Center on Nutrition & Aging |
| Adults 51+ (alt) | Men | Variable | 30 grams | Nat. Resource Center on Nutrition & Aging |
The variation between sources is small. Aim for 22 grams (women) and 28 grams (men) and you will satisfy every major U.S. authority. According to the Administration for Community Living, 95% of older adults fall below this number, which makes the gap one of the most fixable nutrition problems in U.S. healthcare.
30 Best High-Fiber Foods for Seniors (Ranked by Grams per Serving)
The chart below stacks 30 senior-friendly foods by fiber content per standard U.S. serving, with the soluble or insoluble dominance noted and a quick tip for older eaters. Values come from the USDA FoodData Central database.

Table 1: 30 High-Fiber Foods for Seniors, Ranked by Grams per Serving
| # | Food | Serving | Fiber (g) | Type | Senior Tip |
| 1 | Split peas, cooked | 1 cup | 16.3 | Mostly soluble | Pureed pea soup is dental-friendly |
| 2 | Lentils, cooked | 1 cup | 15.6 | Both | Easy to mash; freezes well |
| 3 | Black beans, cooked | 1 cup | 15.0 | Both | Rinse canned beans to cut sodium |
| 4 | Chickpeas, cooked | 1 cup | 12.5 | Both | Hummus is a no-chew option |
| 5 | Kidney beans, cooked | 1 cup | 11.3 | Both | Soft texture suits dentures |
| 6 | Chia seeds | 2 tbsp | 10.0 | Mostly soluble | Soak first; never eat dry |
| 7 | Avocado | 1 medium | 9.2 | Both | Spreadable, no chewing strain |
| 8 | All-Bran cereal | 1/2 cup | 9.0 | Insoluble | Soften with milk before eating |
| 9 | Green peas, cooked | 1 cup | 8.8 | Both | Mashable; great for soft diets |
| 10 | Edamame, shelled | 1 cup | 8.0 | Both | Bonus protein for senior muscle |
| 11 | Raspberries | 1 cup | 8.0 | Both | Frozen works fine; cheaper |
| 12 | Medjool dates | 5 dates | 8.0 | Both | Nature’s stool softener |
| 13 | Artichoke, cooked | 1 medium | 6.9 | Mostly soluble | Soft hearts are easy to chew |
| 14 | Barley, cooked | 1 cup | 6.0 | Mostly soluble | Slow-cook for tender texture |
| 15 | Pear, with skin | 1 medium | 5.5 | Both | Eat skin on for full fiber |
| 16 | Quinoa, cooked | 1 cup | 5.2 | Insoluble | Soft grain, mild flavor |
| 17 | Broccoli, cooked | 1 cup | 5.1 | Both | Steam until fork-tender |
| 18 | Spinach, cooked | 1 cup | 4.3 | Insoluble | Wilts down; easy to swallow |
| 19 | Apple, with skin | 1 medium | 4.4 | Both | Stewed apple suits sensitive teeth |
| 20 | Oatmeal, cooked | 1 cup | 4.0 | Mostly soluble | Adds water to your day too |
| 21 | Brussels sprouts | 1 cup | 4.0 | Both | Roast until soft |
| 22 | Whole wheat bread | 2 slices | 4.0 | Insoluble | Look for 100% whole wheat |
| 23 | Ground flaxseed | 2 tbsp | 4.0 | Both | Stir into yogurt or oatmeal |
| 24 | Sweet potato w/ skin | 1 medium | 3.8 | Both | Bake whole for soft flesh |
| 25 | Blueberries | 1 cup | 3.6 | Both | Frozen retains all the fiber |
| 26 | Carrots, raw | 1 cup | 3.6 | Both | Grate for easier chewing |
| 27 | Popcorn, air-popped | 3 cups | 3.6 | Insoluble | Skip if dental work is fragile |
| 28 | Almonds | 1 ounce | 3.5 | Insoluble | Almond butter is the easy form |
| 29 | Brown rice, cooked | 1 cup | 3.5 | Insoluble | Rinse and cook longer for tenderness |
| 30 | Prunes (dried plums) | 5 pieces | 3.5 | Both | The senior gold standard |
Top 5 Fruits for Senior Bowel Health
Fruits hit a sweet spot: water, fiber, natural sugars, and (in some cases) sorbitol that pulls water into the colon. The five highest-impact picks for seniors are raspberries, pears with skin, prunes, apples with skin, and oranges.
Prunes earn the most clinical attention. A randomized trial published in Alimentary Pharmacology & Therapeutics found that 50 grams of prunes (about 5 to 6 pieces) outperformed psyllium for chronic constipation in older adults. Sorbitol is the secret: a non-absorbed sugar alcohol that draws water into the bowel.
Top 5 Vegetables for Daily Plates
Cooked vegetables almost always beat raw for senior digestion. Heat softens cellulose, makes chewing easier, and reduces gas-forming compounds. The five most senior-practical picks are broccoli, Brussels sprouts, sweet potatoes (with skin), green peas, and spinach.
Steaming and roasting both work well. Boiling can leach water-soluble nutrients into the cooking water, so keep that broth for soups when possible. Patients commonly ask us about carrots: grated or lightly cooked, they deliver 3.6 grams per cup with very low chewing effort.
Top 5 Whole Grains for Older Eaters
Whole grains keep the bran and germ that white rice or refined flour throws out. Oatmeal leads the pack for senior practicality: cheap, soft, hot, and naturally adds water to the day.
Other strong picks include barley, quinoa, brown rice, and 100% whole-wheat bread. Read the front label carefully. “Multigrain,” “wheat,” and “stone-ground” can still mean refined flour. Only “100% whole grain” or “100% whole wheat” guarantees the bran is still in the package.
Top 5 Legumes (Beans, Lentils, Peas)
Legumes are the highest-fiber category in the supermarket. One cup of cooked lentils delivers 15.6 grams, more than 70% of the daily female senior target in a single bowl.
Lentils, black beans, chickpeas, kidney beans, and split peas all sit above 11 grams per cup. Start small, half a cup at a time, to avoid the gas that scares seniors away. Rinsing canned beans cuts sodium by 40% and washes off some of the gas-causing oligosaccharides too.
Top 5 Nuts and Seeds
Nuts and seeds bring fiber, healthy fats, and minerals seniors often miss. Chia seeds top the list at 10 grams per 2 tablespoons. Soak them in water, milk, or yogurt first; never swallow dry chia, as it can absorb fluid in the throat and cause choking.
Ground flaxseed at 4 grams per 2 tablespoons is the safest seed for older adults. Whole flax passes through undigested, so always buy ground or grind at home. Almonds, pistachios, and pumpkin seeds round out the top five.
5 Unsung Heroes Worth Adding
Avocado (9 grams per fruit), edamame (8 grams per cup), Medjool dates (8 grams in 5 pieces), artichoke hearts (6.9 grams each), and air-popped popcorn (3.6 grams per 3 cups) get less attention than they deserve. Across the senior nutrition consults logged through HealthCareOnTime, these five are the swaps that move people from “stuck at 15 grams” to “hitting 25 grams without trying.”
Soft and Easy-to-Chew High-Fiber Foods for Seniors
Dental problems, swallowing issues (dysphagia), and reduced appetite can all push seniors toward low-fiber processed foods. The good news: plenty of high-fiber options need almost no chewing.

Best Picks for Dentures and Sensitive Teeth
Mashed sweet potato, oatmeal, soft-cooked lentils, ripe pears, stewed apples, ripe banana, avocado, hummus, smooth peanut or almond butter, and silken tofu all deliver fiber without strain. Pureed bean soups, like a smooth black bean or split pea soup, can pack 8 to 12 grams in a single bowl.
Smoothies, Soups, and Stewed Fruits
A single fiber-loaded smoothie can hit 15 grams. A reliable senior-friendly recipe: 1 cup unsweetened almond milk, 1 cup raspberries, 1 medium banana, 2 tablespoons ground flax, 1 tablespoon chia. Caregivers calling our patient support team often start here, then adjust to taste once the bowel pattern stabilizes.
Stewed prunes, baked apples, and slow-cooked pears with cinnamon turn high-fiber fruit into spoon-soft food. Add a tablespoon of ground flax on top for an extra 2 grams per serving.
Strategies for Limited Mobility or Bedridden Seniors
For seniors with limited movement, fiber matters more, not less. Slow transit gets slower without walking. Focus on liquid sources (smoothies, broths, prune juice) and meals that pack fiber into small portions: hummus on whole-wheat crackers, oatmeal with chia, lentil soup with avocado.
Chewing aids and adaptive utensils help. Our medical reviewers note that homecare patients who keep a 16-ounce water bottle within arm’s reach (refilled four times daily) report fewer constipation episodes, regardless of fiber load.
7-Day High-Fiber Senior Meal Plan
The plan below hits 22 grams (women) or 28 grams (men) every day. Add a fiber bonus snack from the list to push toward 28 grams as needed. All servings are U.S. measurements.
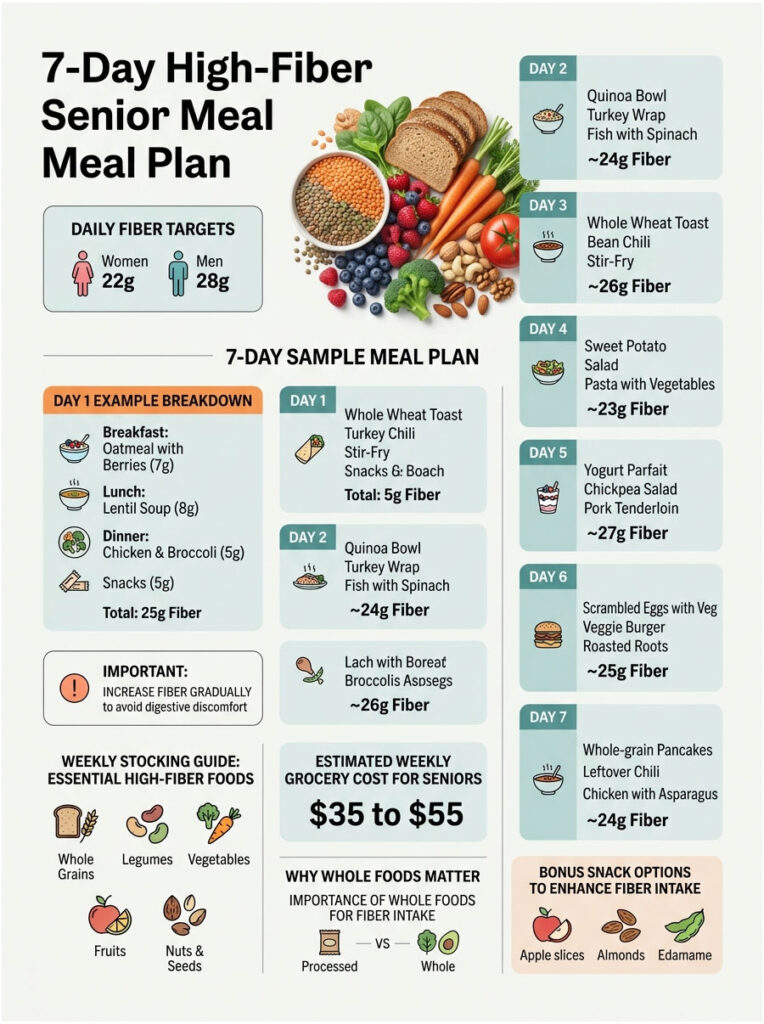
Day 1 (Sample Day, Showing the Math)
Breakfast: 1 cup oatmeal (4g) with 2 tablespoons ground flax (4g) and 1 cup raspberries (8g). Subtotal: 16g.
Lunch: Lentil soup, 1.5 cups (8g) with 1 medium pear (5.5g). Subtotal: 13.5g.
Dinner: Baked sweet potato with skin (3.8g) topped with 1/2 cup black beans (7.5g) and 1 cup steamed broccoli (5.1g). Subtotal: 16.4g.
Snack: 5 prunes (3.5g) or 1 ounce almonds (3.5g).
Daily fiber total: roughly 49g, which exceeds even the male senior target. Drop one item or shrink portions if you are starting at 15g a day; jumping straight to 49g will cause bloating. The point of Day 1 is to show how easy it is to overshoot once whole-food fiber becomes the default.
Day 2 (Target 28g)
Breakfast: Whole-grain toast with 1/2 mashed avocado and 1 tablespoon chia (10g).
Lunch: Chickpea salad with mixed greens, cherry tomatoes, and olive oil (12g).
Dinner: 1 cup brown rice with stir-fried Brussels sprouts and chicken (8g).
Day 3 (Target 22g)
Breakfast: 1/2 cup bran cereal with 1 ripe banana and milk (12g).
Lunch: Turkey sandwich on 100% whole-wheat bread with 1 medium pear on the side (10g).
Dinner: Baked salmon with 1/2 cup quinoa and 1 cup spinach (7g).
Day 4 (Target 28g)
Breakfast: Greek yogurt with 1 cup raspberries and 2 tablespoons ground flax (12g).
Lunch: 1.5 cups split pea soup with whole-grain crackers (16g).
Dinner: Grilled chicken with mashed sweet potato and 1 cup green peas (12g).
Day 5 (Target 22g)
Breakfast: 1 cup oatmeal with 1 cup blueberries and 1 ounce slivered almonds (10g).
Lunch: Hummus with whole-grain pita and grated carrots (10g).
Dinner: Barley risotto with mushrooms and a small mixed-green salad (6g).
Day 6 (Target 28g)
Breakfast: Avocado toast on whole-grain bread with one medium orange on the side (10g).
Lunch: Kidney bean chili, 1.5 cups, topped with diced avocado (14g).
Dinner: Roasted vegetables (broccoli, sweet potato, carrots) with 1/2 cup quinoa (8g).
Day 7 (Target 22g)
Breakfast: Smoothie with raspberries, banana, chia, and ground flax in almond milk (15g).
Lunch: Lentil wrap on a 100% whole-wheat tortilla with mixed greens (10g).
Dinner: Baked apple with cinnamon, walnuts, and a side of cottage cheese (5g).
Senior Grocery List Summary
Stock the following weekly: oatmeal, 100% whole-wheat bread, brown rice, quinoa, lentils, black beans, chickpeas, raspberries (frozen is fine), pears, apples, prunes, broccoli, sweet potatoes, spinach, avocados, chia seeds, ground flaxseed, almonds. Total weekly cost in most U.S. supermarkets runs $35 to $55 for one senior.
When Will It Work? A Realistic Results Timeline
Patients commonly ask how fast a high-fiber diet ends constipation. The honest answer: most seniors notice changes inside a week, with the fullest effect by day 14.

Day 1 to 3: Initial Adjustment
Stools start to bulk up as fiber draws water in. Some seniors feel mild gas or fullness during the first 72 hours; this is the gut microbiome adapting, not a problem with the diet. Keep portions modest and water steady.
Day 4 to 7: Regularity Returns
By the end of the first week, most seniors report softer stools, less straining, and a more predictable bathroom pattern. A 2018 review in Therapeutic Clinics in Risk Management confirmed that dietary fiber meaningfully improves stool frequency and consistency within 1 to 2 weeks for most older adults.
Day 8 to 14: Stable Pattern
The bowel settles into a near-daily rhythm. Energy often improves alongside it, partly because feeling backed up dampens appetite and mood. If you reach day 14 with no improvement, the cause is probably not fiber alone, and a doctor visit is warranted.
Foods Seniors Should Limit or Avoid
A diet high in fiber works best when paired with smaller amounts of foods that slow the bowel. The biggest offenders are high-fat, low-fiber processed items.
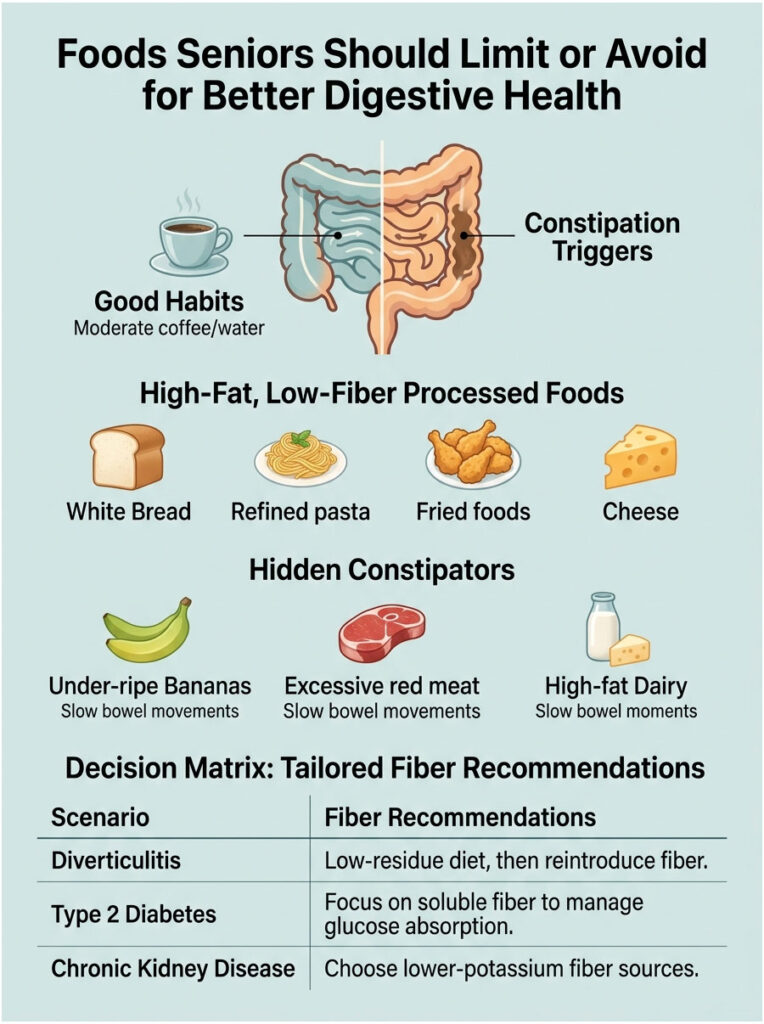
Common Constipation Culprits
White bread, white rice, refined pasta, fried foods, cheese, processed meats (hot dogs, deli salami, bacon), commercial baked goods, and ice cream all reduce stool transit time. Cheese gets singled out by Johns Hopkins Medicine for its particular constipation effect; the combination of high fat and zero fiber is hard on a senior gut.
Hidden Constipators
Bananas (especially under-ripe ones), excessive red meat, full-fat dairy, and high-protein low-carb diets like keto can all back things up. Coffee in moderation actually helps motility, so a single morning cup is fine for most seniors.
Table 3: Constipation Scenario / Recommended Action
The decision matrix below pairs common senior scenarios with the right fiber move.
| If You Have… | Then Prioritize | Limit or Avoid | Notes |
| Diverticulitis (active flare) | Low-residue diet temporarily, then return to fiber | Nuts, seeds, popcorn during flare only | Reintroduce fiber after flare resolves; long-term high fiber prevents recurrence |
| Type 2 Diabetes | Soluble fiber (oats, beans, lentils, chia) | Refined carbs, fruit juice | Soluble fiber slows glucose absorption |
| Chronic Kidney Disease | Lower-potassium fiber (apples, berries, white beans) | High-potassium beans, sweet potato, spinach (late-stage CKD) | Coordinate potassium load with the nephrologist |
| Dentures or chewing trouble | Smoothies, oatmeal, hummus, mashed beans, stewed fruit | Raw nuts, popcorn, raw vegetables | Pureed soups deliver 8 to 12g per bowl |
| On opioid pain medication | Prunes, ground flax, psyllium supplement | Cheese, refined grains | Opioids slow gut transit; aggressive fiber and fluid required |
| IBS with constipation | Soluble fiber (oats, psyllium), low-FODMAP options | Onions, garlic, beans (FODMAP triggers) | Insoluble fiber can worsen IBS-C; go gradual |
| Bloating on new high-fiber diet | Smaller portions across more meals; extra water | Adding multiple new high-fiber foods at once | Increase fiber by 5g per week, not 15g overnight |
Fiber Supplements for Seniors: When and Which
Whole foods come first. They bring fiber plus vitamins, minerals, and polyphenols that capsules cannot match. That said, some seniors cannot eat enough volume to hit 22 grams a day. A supplement bridges the gap.

Metamucil (Psyllium) Versus Citrucel (Methylcellulose)
Psyllium is a soluble fiber that forms a gel and softens stool. It works well for constipation but can cause gas in the first week. Methylcellulose is a non-fermentable soluble fiber, gentler on gas but slightly less effective for stubborn constipation, per Mayo Clinic Q&A guidance.
Benefiber (Wheat Dextrin) Versus FiberCon (Calcium Polycarbophil)
Benefiber dissolves clear in water, which makes it easy for seniors with appetite issues to add to coffee or tea. FiberCon (calcium polycarbophil) both firms loose stools and softens hard ones, useful for seniors who alternate between constipation and looseness.
Drug Interactions Seniors Must Know
Fiber supplements bind to certain medications. Take psyllium, methylcellulose, or wheat dextrin at least 2 hours apart from thyroid medication (levothyroxine), warfarin, digoxin, lithium, tricyclic antidepressants, and diabetes drugs. Senior supplement choice often depends on the full medication profile, which is why a quick check with the prescribing doctor is the safest first step.
Hydration, Movement, and Daily Habits That Multiply Fiber’s Effect
Fiber without water can make constipation worse, not better. The colon pulls water out of stool to send back into the body; if there is not enough water in the system, the stool dries and gets harder to pass.
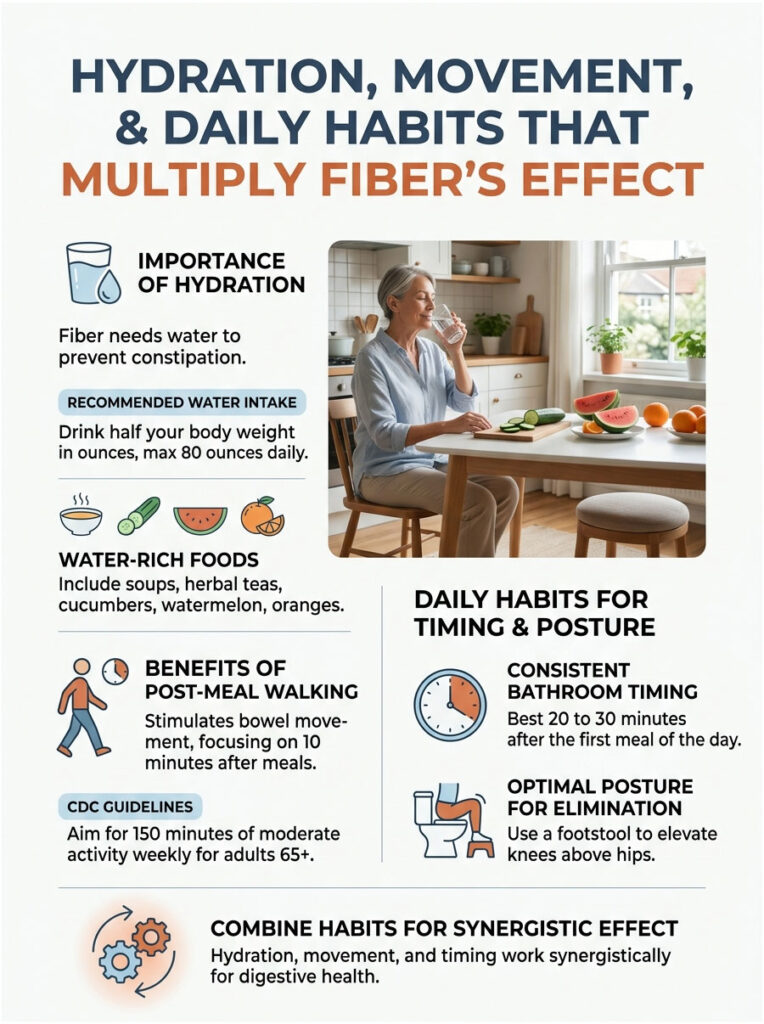
The Water-Fiber Formula
A practical rule for seniors: drink half your body weight in ounces of water per day, up to a ceiling of 80 ounces. A 160-pound senior should aim for about 80 ounces (10 cups). Soups, herbal teas, and water-rich foods (cucumber, watermelon, oranges) all count toward the total.
The 10-Minute Walking Ritual
Walking after meals stimulates the gastrocolic reflex, which triggers bowel movement. Even 10 minutes after breakfast can make a difference. The CDC recommends 150 minutes of moderate activity per week for adults 65 and over, broken into manageable daily walks.
Bathroom Posture and Timing
Seniors do better with a consistent morning bathroom window, ideally 20 to 30 minutes after the first meal of the day. A small footstool that raises the knees above hip level (the “Squatty Potty” position) makes elimination easier on aging pelvic floors.
Red Flags That Mean See a Doctor
Diet handles most senior constipation. It does not handle every cause. The HealthCareOnTime diagnostic team frequently runs a colonoscopy and full stool test panel when any of the following appear.
Watch for blood in the stool (red or black/tarry), unexplained weight loss of 10+ pounds, severe abdominal pain that does not resolve, persistent vomiting, sudden change in stool caliber (pencil-thin stools), constipation that arrives suddenly after years of regular bowels, or constipation that lasts more than 3 weeks despite diet and fluid changes.
These signs can point to colorectal cancer, bowel obstruction, thyroid disease, or other conditions that need imaging or lab work. Fiber is medicine for the routine cases. The exceptions need a physician.
Frequently Asked Questions
What is the best fiber food for seniors with constipation?
Prunes top the list for seniors. Five prunes deliver 3.5 grams of fiber plus sorbitol, a sugar alcohol that pulls water into the colon. Clinical trials show prunes outperform psyllium for chronic constipation in older adults. Lentils run a close second at 15.6 grams per cooked cup, with both soluble and insoluble fiber working together.
How much fiber should an 80-year-old eat per day?
An 80-year-old woman should target 22 grams of fiber daily; an 80-year-old man should target 28 grams. These figures come from the USDA Dietary Guidelines for Americans (2020 to 2025) and apply to all adults aged 51 and older. Seniors with smaller calorie needs can drop slightly to 21 and 26 grams respectively.
Are bananas good or bad for senior constipation?
Ripe bananas (yellow with brown spots) help; unripe bananas (green-tipped) can constipate. A medium ripe banana provides 3.1 grams of fiber plus pectin, which softens stool. Unripe bananas contain resistant starch that slows transit. For senior constipation, choose only fully ripe bananas, and pair with prunes or oatmeal for stronger effect.
What is the fastest fiber food to relieve constipation?
Prunes and prune juice work fastest, often within 6 to 24 hours. The combination of fiber and sorbitol triggers a bowel response sooner than most other foods. Kiwi fruit (2 per day) is a research-backed runner-up; the enzyme actinidin adds to its laxative effect, per Johns Hopkins guidance.
Can seniors eat too much fiber?
Yes. Going past 50 grams a day can cause bloating, gas, cramping, and ironically, constipation if water intake does not keep pace. The Mayo Clinic warns against more than 50 grams of supplemental fiber per day, since high doses can also reduce absorption of certain minerals and prescription medications.
What soft high-fiber foods work for seniors with dentures?
Mashed sweet potato, oatmeal, soft-cooked lentils, hummus, ripe pear, banana, avocado, stewed apples, smooth nut butter, and pureed bean soups all deliver substantial fiber without chewing strain. A bowl of split pea soup alone can hit 16 grams. Smoothies with chia and ground flax push past 15 grams in a single glass.
Is Metamucil safe for daily use in seniors?
Metamucil (psyllium) is generally safe for daily senior use when taken with adequate water (8 ounces per dose). It can interfere with absorption of thyroid medication, warfarin, lithium, and diabetes drugs, so take it at least 2 hours apart from prescriptions. Always confirm with the prescribing doctor before starting any daily supplement.
What drinks help senior constipation?
Water leads the list. Prune juice (4 to 8 ounces) works fast for stubborn cases. Warm water with lemon in the morning stimulates bowel motion. Black coffee in moderation triggers the gastrocolic reflex within 30 minutes. Avoid alcohol and excessive caffeine, both of which can dehydrate and worsen constipation in older adults.
Are oats high enough in fiber for seniors?
A cup of cooked oatmeal delivers 4 grams of fiber, mostly soluble (beta-glucan). On its own, oats cover 18% of the female senior daily target. Pair oatmeal with raspberries (8g), ground flax (2g), and a banana (3g), and a single breakfast bowl can hit 17 grams.
How long until fiber relieves constipation?
Most seniors feel improvement within 3 to 7 days of hitting their daily fiber target with adequate water. Stool consistency softens first, then frequency normalizes. Full bowel pattern stability typically takes 14 days. If 2 weeks pass with no change, contact a doctor to rule out non-dietary causes like thyroid issues or medication side effects.
Should diabetic seniors avoid high-fiber fruits?
Diabetic seniors should embrace high-fiber fruits, not avoid them. Fiber slows sugar absorption and improves glycemic control. The best diabetic-friendly fiber fruits are raspberries, blackberries, pears, apples, and oranges. Limit higher-glycemic fruits like watermelon and pineapple, and pair fruit with protein or fat (yogurt, nuts) to flatten the blood-sugar curve.
Can fiber interact with senior medications?
Yes. Fiber and fiber supplements can bind to thyroid medication, warfarin, lithium, digoxin, tricyclic antidepressants, certain diabetes drugs, and some heart medications. Take fiber supplements at least 2 hours away from prescription doses. Whole-food fiber is much less likely to cause interactions, but timing still matters for very high-fiber meals (40+ grams in one sitting).
Disclaimer: This article is for general educational purposes and does not replace personalized medical advice. Seniors with chronic constipation, diabetes, kidney disease, diverticular disease, or who take prescription medications should consult their physician or a registered dietitian before making major dietary changes. Speak with a doctor if constipation is accompanied by blood in the stool, unexplained weight loss, severe pain, or sudden bowel changes.
References
- USDA Dietary Guidelines for Americans, 2020 to 2025
- NIDDK: Eating, Diet, & Nutrition for Constipation
- Administration for Community Living: Nutrition Needs for Older Adults — Fiber
- Mayo Clinic: Chart of High-Fiber Foods
- Johns Hopkins Medicine: Foods for Constipation
- Healthline: Best Fiber Sources for Older Adults
- HealthInAging.org: Caregiver Guide — Constipation Problems
- USDA FoodData Central
- Yang J, et al. Dietary Fiber in the Management of Constipation: A Clinical Review. Therapeutic Clinics in Risk Management. 2018
- Camilleri M. Management of Chronic Constipation in Older Adults. Drugs & Aging. 2017
- Horiuchi R, et al. Foods and Dietary Patterns Associated with Constipation in Older Adults. Nutrients. 2020
- Mayo Clinic Q&A: Increasing Fiber Intake for Constipation Relief







