Children are the pioneers of our tomorrow, safeguard them to fortify their future.
How often does our mind trail to the thoughts that of an otherwise squealing baby now muffling uncomfortably might
possibly be a sign of imminent malady?
We usually have the tendency to neglect certain undoubted, incidences and then bewail later when adversity finally strikes. A very evident alteration in behavior and appearance is the first sign to raise our guards Reduced playfullness, apparent weight loss, persistent fever, and breathlessness are the prominent prodromes of thriving illness. Children are more prone to getting infections because they yet have not developed their protective immunities. Also, toddlers are exposed to the risk as they are always surrounded by people and are in contact with many other children, thus transmission of infection becomes easy. One such threat which is arising predominantly among the young is Tuberculosis – termed as ‘Pediatric TB‘.
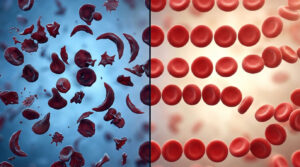
TB is an air-borne infection caused by the inhalation of droplet nuclei contaminated with an acid-fast bacillus, Mycobacterium tuberculosis, which are disease-causing pathogens. Although, TB is a preventable and curable disease, most of the cases go unrecognized and are left untreated due to nonspecific symptoms and difficulty in diagnosis. Owing to this, childhood TB has been termed as “hidden epidemic”. As per the World Health Organization (WHO) about 10 lakh children are being infected with TB each year.
Adults, Primary cause of Pediatric TB – The grim reality!
Young children are prone to infection because their immune system is not as strong and developed as the
adults. When such infants and children are exposed to adults with active-TB, they contract the TB bacilli.
Childhood tuberculosis is usually considered as primary infection because once they are exposed to the
bacilli they are at a higher risk of developing active TB than adults. They also have higher possibilities of
developing disseminated i.e miliary TB and TB meningitis; extrapulmonary manifestations. If a child is
diagnosed with active tuberculosis it is advised to investigate the family to analyze the source of infection.
Risk factors : Highs causing lows!
Children are at a higher risk of contracting the TB infection and developing active TB. Risk factors are
- Contact with infected adults, with active-TB
- Poor hygienic conditions
- Having latent stage TB infection
- HIV patients with a weakened immunity
- Infants below 3 years of age, and adolescents before or during puberty are more prone.
Pulmonary Tuberculosis
A condition where the child’s lungs are infected.
The manifestations are shown according to specificity
- Endobronchial tuberculosis
- Progressive primary pulmonary tuberculosis
It is infection of the functional parts of the pulmonary system and its signs and symptoms include, pneumonia, atelectasis and air-trapping
It is the infection of the tracheobronchial tree i.e branching tree of the airways from larynx to the lungs. Signs and symptoms include, bronchial obstruction, esophageal compression, vocal cord paralysis, hemidiaphragmatic paralysis.
Extrapulmonary Tuberculosis
It is an infection outside the lungs. Children appear to have a higher tendency of developing this form of TB
The manifestations are shown according to specificity
- Lymphadenopathy
- TB Meningitis
It involves the anterior or posterior cervical and supraclavicular lymph nodes. Infected Lymph nodes are firm and non-tender with no signs of inflammation.
It develops mostly in children younger than 2 years. Moderately acute signs and symptoms occurs after 3-6 months of initial infection which includes anorexia, weight Loss, fever, vomiting, seizures and alteration in sensory apparatus. Extreme conditions may cause major neurological defects including coma and abnormal movements (e.g. Paralysis).
Know it before you go through it! WHO estimated that out of 13 lakh pediatric TB cases only 13% turn out to be eligible for preventive measures. This statistics showcase the seriousness of early diagnosis because earlier the infection is detected, the better will be its treatment and prognosis.
Tests for detection of TB includes
This method is not specifically diagnostic but radiological findings are important for TB meningitis. Lymphadenopathy, hilar adenopathy and paratracheal adenopathy are the most common abnormalities identified by chest radiography.
Tuberculin Skin Test (Mantoux test) – Detects the presence of tuberculosis infection by studying the reaction of patients body to PPD upon injecting intradermally small amount of tuberculin protein (purified protein derivative; PPD).
It is the in vitro detection of immune response against M. tuberculosis antigens.
TB Culture and Drug Susceptibility Test
Culturing of the Mycobacterium proves to be more sensitive than smear microscopy, and it can also
allow subsequent characterization of the strain and drug susceptibility testing (DST).
- TB-PCR
- CBNAAT (GeneXpert MTB/RIF)
- MDR/XDR Line Probe Assay
It is a nucleic acid based test which detects specific DNA of MTB, and the technique has greater sensitivity than conventional diagnostic techniques. Along with sputum it can also be used for EPTB samples such as gastric aspirate, pleural fluid, endomerial tissue, Urine, and cerebrospinal fluid.
MTB/RIF is an automated, TB specific CBNAAT that uses real time PCR for the rapid detection of TB, as well as detection of rifampicin resistance, which counts as a surrogate marker for MDRTB. Sample preparation, amplification and detection are done by auto mation and the results are rapid (within 2 hours). It aids in diagnosing pulmonary TB and EPTB.
Line probe assay technology detects the genetic mutations associated with resistance to rifampicin, isoniazid (first line; MDR) fluoroquinolone, aminoglycosides, and cyclic peptides (second line; XDR). The relationship between the children and every other family member is based on pillars of care and love, and our support is the best we can give in such critical times of our lives. At our extent, awareness and knowledge is the crucial factor for precautionary measures. TB is a curable disease and its early diagnosis is the path to well-being!