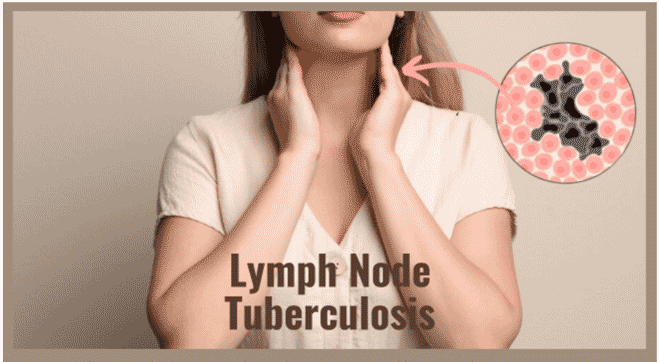
What Is Lymph Node Tuberculosis?
Lymph node tuberculosis, also known as tuberculous lymphadenitis or TB lymphadenitis, is a form of tuberculosis that primarily affects the lymph nodes. It affects the lymph nodes in the neck but can also occur in other areas, such as the armpits or groyne. It occurs when the bacteria responsible for tuberculosis infect the lymph nodes, resulting in their enlargement and the formation of small, painless lumps. Lymph node TB is infectious and can be transmitted to others through respiratory droplets when an infected individual coughs or sneezes. It is most commonly seen in individuals with weakened immune systems, such as those with HIV/AIDS.
Tuberculosis(TB), the word itself, brings a deep terror and does not need any further introduction. 10.6 million cases globally, as per the estimation of the World Health Organization (WHO), and India tops the list by carrying the greatest disease burden! Mycobacterium tuberculosis (MTB), the causative agent of this dreadful infection, has coevolved with its host and is enriched with various properties that make it a characteristically untamed pathogen. Its unique features and evading tactics allow it to spread and affect different organs other than its principal site, the Lungs. Of these other organs, the lymph node is one of the more commonly affected.
Types of Tuberculosis
Tuberculosis can be divided into following main types on the basis of its manifestation.
Pulmonary Tuberculosis: The one which infects the lungs and is confined to them.
Extrapulmonary Tuberculosis: The infectious bacteria can spread to other organs via the blood, Stream or lymphatic system and reside there, leading to tuberculosis infection in that particular organ; such TB is known as extrapulmonary tuberculosis or EPTB. EPTB affects different organs like lymph nodes, pleura, abdomen, genitourinary tract, skin, joints and bones, or meninges. The risk of EPTB infection increases with immunosuppression, constituting about 15-20% of all tuberculosis cases.
Common types of extrapulmonary TB include:
- Lymph Node Tuberculosis: Infection of the lymph nodes, often causing swelling in areas like the neck, armpits, or groin.
- Tuberculous Meningitis: Infection of the membranes surrounding the brain and spinal cord, leading to symptoms such as severe headache, fever, and neurological problems.
- Skeletal Tuberculosis: Affecting bones and joints, it can cause joint pain, bone destruction, and deformities.
- Abdominal Tuberculosis: Affecting the abdominal organs, it can lead to symptoms like abdominal pain, digestive issues, and weight loss.
- Genitourinary Tuberculosis: Affecting the kidneys, urinary tract, and reproductive organs, it can cause symptoms like painful urination and flank pain.
Drug-Resistant Tuberculosis: Some strains of Mycobacterium tuberculosis have developed resistance to the standard antibiotics used to treat TB. These strains are classified as drug-resistant TB and can be further categorised into multidrug-resistant TB (MDR-TB) and extensively drug-resistant TB (XDR-TB), based on the level of resistance to different types of antibiotics.
Latent Tuberculosis Infection: This is not a type of active TB disease, but rather a condition in which a person carries the TB bacteria but does not exhibit symptoms or spread the disease. It can later develop into active TB if the immune system becomes compromised.
Lymph Node Tuberculosis Stages
The key Tb lymph node stages include:
Stage 1: In the initial stage of lymph node tuberculosis, the affected node becomes enlarged, mobile, and discrete. It can be felt easily and moves freely under the skin.
Stage 2: As the disease progresses, the affected node becomes larger and firmer, getting fixed to the surrounding tissues. It loses its mobility and feels like a large rubbery mass.
Stage 3: The tuberculosis infection causes the node to soften and form an abscess. The abscess leads to developing a characteristic collar stud, where the node is elevated above the skin level.
Stage 4: In the final stage, the abscess may drain through a sinus tract. This is a slow healing process characterised by the formation of a channel that connects the spot to the skin surface, resulting in the discharge of pus.
Lymph Node Tuberculosis Symptoms
Some common Lymph Node TB symptoms include:
- Swelling of lymph nodes: The most common symptom of lymph node tuberculosis is the presence of swollen lymph nodes. These swollen nodes are usually painless and can be felt under the skin in various body parts.
- Weight loss: Unexplained weight loss can occur as a symptom of lymph node tuberculosis. This can be due to a loss of appetite and the body’s efforts to fight the infection.
- Fever: A low-grade fever may be present in individuals with lymph node tuberculosis. This fever is usually persistent and does not respond to typical fever-reducing medications.
- Fatigue: Feeling tired and lacking energy can be a symptom of lymph node tuberculosis. This can be due to the body’s immune response to the infection.
- Night sweats: Excessive sweating during sleep, especially at night, is a common symptom of neck Tb. This can lead to disrupted sleep patterns and further fatigue.
- Cough: In some cases, a persistent cough may be present in individuals with lymph node tuberculosis. This cough may be accompanied by phlegm or blood in severe cases.
- Chest pain: Chest pain can occur if the lymph nodes in the chest are affected by tuberculosis. This pain may worsen with deep breathing or coughing.
- General weakness: Individuals with lymph node tuberculosis often report a general feeling of weakness and malaise. This can affect daily activities and overall quality of life.
- Loss of appetite: Decreased appetite and unintentional weight loss are common symptoms of lymph node tuberculosis. It can lead to nutritional deficiencies and further weakening of the immune system.
- Respiratory symptoms: In some cases, lymph node tuberculosis can cause respiratory symptoms such as shortness of breath or difficulty breathing. It can occur if the infection spreads to the lungs.
Causes Of Tuberculous Lymphadenitis In Neck
A bacterial infection is considered one of the common causes of lymph node Tb. The bacteria responsible for this condition is Mycobacterium tuberculosis, transmitted through droplets when an infected person coughs or sneezes. Factors that can increase the risk of developing tuberculosis of the lymph nodes include:
- A weakened immune system
- Close contact with an infected individual
- Living in crowded or unsanitary conditions
- Malnutrition
The infection typically begins in the lungs and spreads to the lymph nodes through the lymphatic system.
Lymph Node Tuberculosis Complications
In advanced stages, softening and enlargement of nodes may disturb the surrounding structures and impede their normal functioning. Intrathoracic nodes may compress the bronchus, predisposing to lung infections. In some cases, the cervical nodes can result in extrathoracic upper tract obstruction.
Here are some potential complications of lymph node tuberculosis:
- Abscess Formation: In some cases, the infected lymph nodes can develop into abscesses, which are pockets of pus that form due to the body’s immune response. Abscesses can lead to pain, swelling, and the need for drainage procedures.
- Fistula Formation: If an abscess is not properly treated or if the infection spreads, it can create abnormal connections between different structures in the body, such as a fistula connecting the affected lymph node area to the skin. Fistulas can lead to persistent drainage, pain, and increased risk of infection.
- Chronic Lymphedema: In some cases, chronic inflammation and scarring can cause a condition called lymphedema. This involves swelling due to the impaired drainage of lymph fluid from the affected area. Lymphedema can cause discomfort, skin changes, and an increased risk of infections.
- Secondary Bacterial Infections: Due to the weakened immune response caused by TB infection, there’s a risk of secondary bacterial infections occurring in the affected lymph nodes. These secondary infections can exacerbate the symptoms and complicate the treatment process.
Lymph Node Tuberculosis Diagnosis
Diagnosis of EPTB is challenging due to vague lymph node TB symptoms and insidious onset. In the case of cervical Tb lymphadenitis, it is crucial to differentiate tuberculous from non-tuberculous Mycobacterial infection because they have different treatment protocols. Co-infection with HIV demands all cervical tuberculous lymphadenitis patients undergo HIV testing. As MTB is a slow-growing bacteria, culturing and traditional diagnosis prove to be time-consuming, and hence newer and more advanced approaches are undertaken. Following are some of the commonly used diagnostic techniques for TLD
- Physical Examination Any palpable lymph node should be evaluated for its location (generalised or localised), size, consistency and mobility (mobile nodes are usually associated with lymphoma).
- Tuberculin test It is an intradermal test which detects the delayed hypersensitive reaction against mycobacterial antigen, using PPD i.e. purified protein derivative as a reagent.
- IGRA Interferon gamma releasing assay is an in vitro blood test that measures the interferon gamma released by the T cells following exposure to MTB complex antigens. Two main types of IGRA are: QuantiFERON-TB Gold In-Tube (QFT) assay and TSPOTTB assay.
- Fine Needle Aspiration Cytology and Staining It is a simple, quick and inexpensive diagnostic procedure. It is used as an initial diagnostic test used for the sampling of superficial masses. The procedure includes the collection of samples from the lesion by means of a narrow gauge needle, which can be followed by microscopic examination. Aspirated samples are subjected to staining.
ZN (Ziehl-Neelsen) staining is used to detect the classical Mycobacteria, which are acid fast bacilli (AFB). They are called acid fast because they retain the colour of the stain following acid treatment. This acid fast property is attributed to the presence of membrane mycolic acids bound to the peptidoglycan. Fluorescent staining techniques can prove advantageous in detection in case of lesser bacterial load.
- Culture MGIT (Mycobacteria Growth Indicator Tube)- Liquid culture system facilitates rapid bacterial growth than the conventional solid culture technique using Lwenstein-Jensen (LJ) medium. It also facilitates drug susceptibility testing (DST), used to test the resistance of TB bacteria to certain drugs. All these advantages facilitate early detection and can lead to timely, effective treatment.
- PCR Polymerase Chain Reaction is a rapid, sensitive method used in the detection of MTB. It provides an edge over other techniques, as it does not require culturing, which takes a very long time, and other tests are not very specific. It has now become a routine diagnostic technique. The commonly used PCR profile is 156110 for people susceptible to Mycobacterial cervical lymphadenitis.
- NAAT (Nucleic acid amplification tests) – It is characterised as a rapid, sensitive and specific mode of diagnosis. It helps in the simultaneous detection of MTB and drug (rifampicin) resistance.
Lymph Node Tuberculosis Treatment
Tuberculous lymphadenitis treatment involves several stages:
- The first stage is diagnosis, where a thorough medical examination and tests are conducted to confirm the presence of tuberculosis in the lymph nodes.
- After diagnosis, the next stage is the initiation of anti-tuberculosis medication. This typically involves a combination of drugs that must be taken for a specific duration.
- The treatment stage also includes regular monitoring of the patient’s progress through clinical examinations and laboratory tests.
- Surgical intervention may be considered in cases where the lymph node swelling does not respond to medication.
- The final stage is the completion of the treatment course, which typically lasts for several months, to ensure complete eradication of the infection.
Lymph Node Tuberculosis Treatment Side Effects
Common lymph node Tb treatment side effects in the initial stage include
- Fatigue
- Loss of appetite
- Mild fever
- Nausea and vomiting
- Joint pain
- Dizziness
- Skin rash
- Liver problems
- Gastrointestinal issues
Some individuals may experience rare side effects like vision changes, hearing problems, numbness or tingling in the extremities throughout the treatment, severe allergic reactions, kidney damage, and mental health changes.
Lymph Node Tuberculosis Prevention
Early detection is crucial for the prevention of lymph node tuberculosis. Here are a few prevention methods to follow:
- Regular Health Screening and diagnostic tests can help identify the disease early.
- Maintaining good hygiene practices, such as regular handwashing and covering the mouth when coughing or sneezing, can help prevent the spread of the bacteria causing lymph node tuberculosis.
- Vaccination against tuberculosis, particularly the Bacillus Calmette-Guérin (BCG) vaccine, can protect against lymph node tuberculosis.
- Avoid close contact with individuals with active tuberculosis, which can increase the risk of contracting lymph node tuberculosis.
- Timely and appropriate treatment for tuberculosis can prevent the progression of the disease to the lymph nodes. This includes completing the full course of medication as prescribed by a healthcare professional.
- Education and awareness programs promoting knowledge about tuberculosis prevention, symptoms, and treatment can help prevent lymph node tuberculosis.
Lymph Node Tuberculosis Diet
A proper lymph node tuberculosis diet can help support the immune system and aid recovery. Consuming a balanced diet with plenty of fruits, vegetables, whole grains, and lean proteins is essential. Also, foods rich in vitamin C, such as citrus fruits, and foods high in iron, such as leafy greens and lean meats, can be beneficial. Avoid eating processed foods, sugary snacks, and excessive alcohol consumption is also recommended. It’s best to consult a healthcare professional or a registered dietitian for personalised dietary advice.
Note From HeathcareOnTime
Lymph node tuberculosis (TB) is a form of extrapulmonary TB that primarily affects the lymph nodes. It primarily affects the lymph nodes in the neck, also known as Tb in the neck, but can also occur in other parts of the body. Diagnosing Lymph node Tb can be challenging due to its non-specific symptoms and resemblance to other diseases. It can lead to the enlargement and inflammation of lymph nodes, causing pain and discomfort. Early detection and intervention can help prevent further complications and spread of the disease. Timely diagnosis, comprehensive treatment, and follow-up are crucial in managing lymph node TB effectively.
Sources
Ref Links:
- https://www.cdc.gov/tb/education/corecurr/pdf/chapter2.pdf
- https://www.nhs.uk/conditions/tuberculosis-tb/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4450036/
- https://www.drugs.com/health-guide/tuberculosis.html
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7425845/