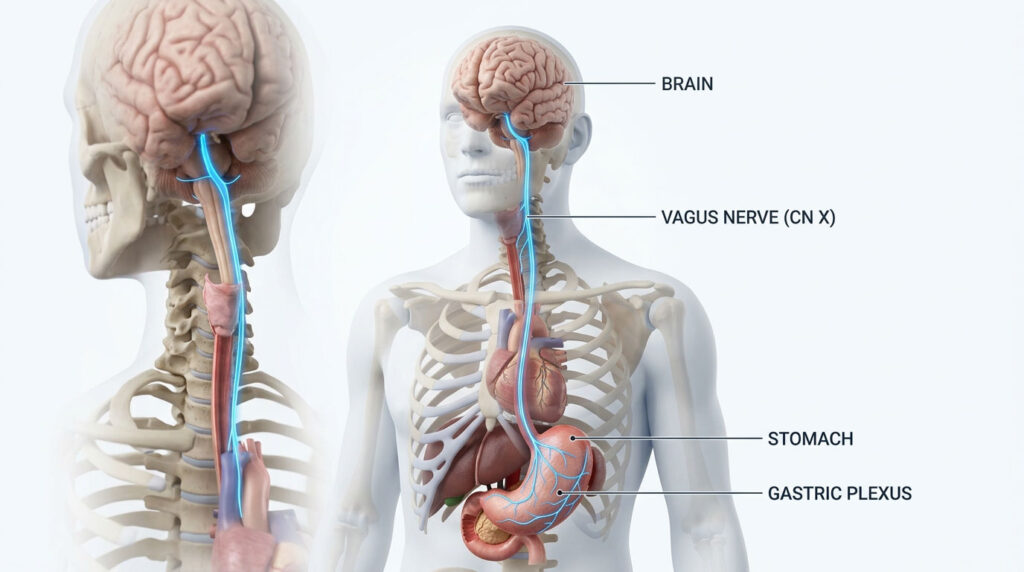
A patient walks into my gastroenterology clinic, completely convinced they are developing a serious panic disorder. Their heart races after every meal. They feel sudden waves of dread that come out of nowhere. When they finally ask, “can stomach acid cause anxiety?” the clinical answer is a clear and definitive yes.
Table of Contents
This is not a sign of psychological weakness. It is a biological reality driven by your nervous system. For decades, doctors treated mental health and digestive health as two entirely separate things. We now know that thinking was fundamentally wrong.
The relationship between your stomach and your brain is a two-way street, and it shapes how you feel on a daily basis. Both excess stomach acid (GERD) and low stomach acid (hypochlorhydria) can severely disrupt the production of neurotransmitters like serotonin and dopamine. If you have been dealing with unexplained panic attacks, racing thoughts, or chronic worry, the real culprit might be sitting in your digestive tract.
Quick Answer
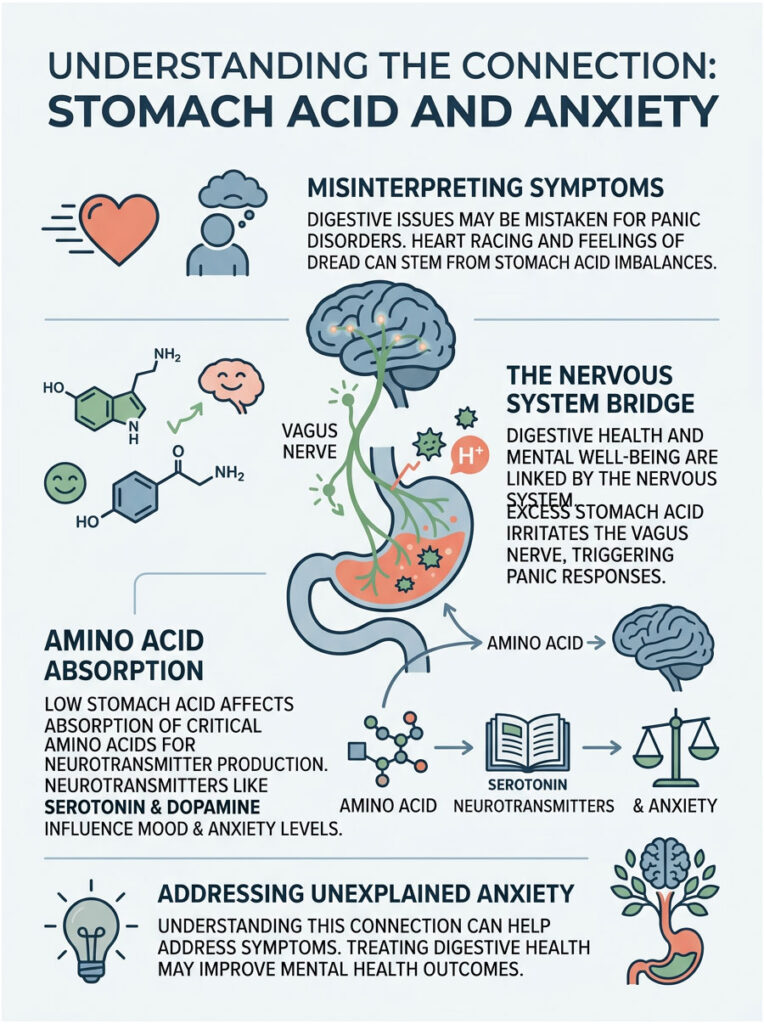
Can stomach acid cause anxiety? Yes. Excess stomach acid physically irritates the Vagus nerve, causing the brain to trigger a false fight-or-flight panic response. On the other hand, low stomach acid prevents absorption of the amino acids needed to produce serotonin and dopamine, leading to chronic anxiety and depression.
Key Statistics on the Gut-Brain Connection
95% of the body’s serotonin is manufactured directly in the gastrointestinal tract.
80-90% of Vagus nerve fibers send sensory data from the gut up to the brain, not the other way around.
40% of patients with chronic acid reflux also have clinical anxiety (2021 gastroenterology data).
100 million nerve cells line the gastrointestinal tract, often called the “second brain.”
50% of the body’s dopamine is synthesized in the gut, regulating motivation and reward.
3x more likely for patients with chronic digestive issues to develop generalized anxiety disorder.
Understanding the Gut-Brain Axis and the Enteric Nervous System
To understand why stomach acid problems trigger panic, you need to look at how the human body is actually wired. The gut-brain connection is not just a trendy wellness phrase. It is a complex physical network of nerves, hormones, and chemical messengers that directly shapes how you experience the world.
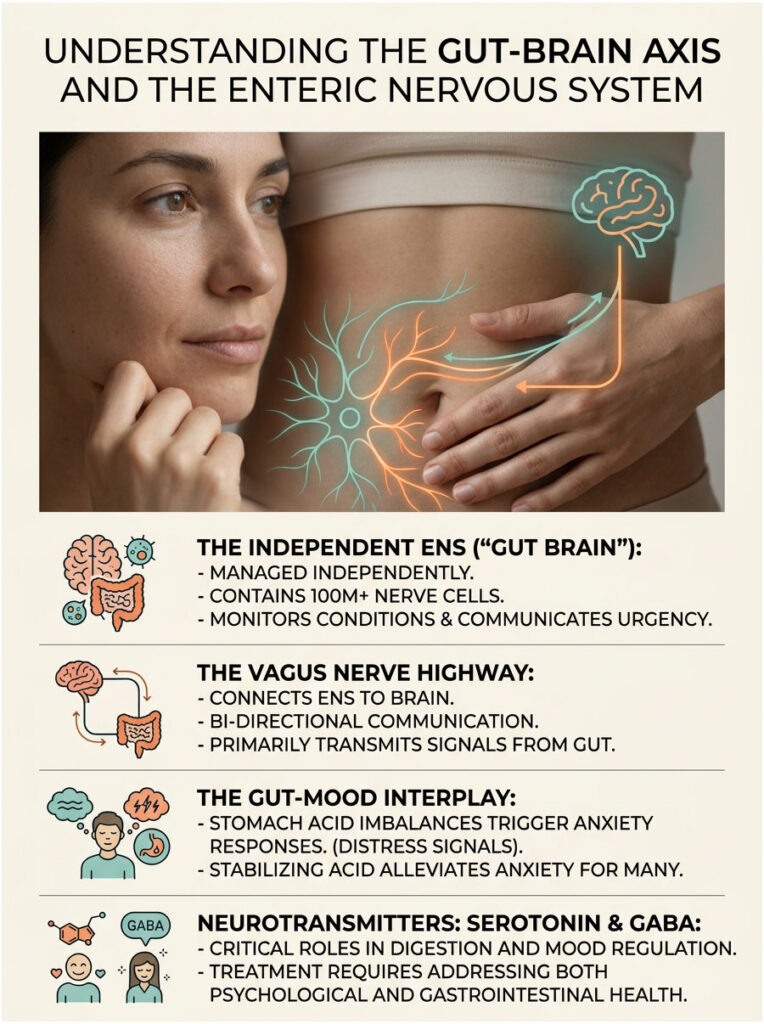
From what we see in functional gastroenterology, trying to treat anxiety without addressing this network is often a dead end. Communication between your digestive organs and your brain happens in milliseconds. When you eat a meal, your brain does not passively wait for nutrients to enter the bloodstream. It actively monitors every chemical reaction taking place in your stomach. If acid levels go haywire, the brain kicks off defensive responses almost instantly.
The Anatomy of the Second Brain
Deep inside the lining of your esophagus, stomach, and intestines lies the Enteric Nervous System (ENS). Clinicians often call it the “second brain” because of its staggering complexity. Over 100 million nerve cells line the gastrointestinal tract, which is actually more neurons than you have in your entire spinal cord.
This network operates with remarkable independence. It manages digestion, enzyme release, and muscle contractions without needing direct orders from your brain. But it constantly feeds updates to the central nervous system about conditions inside your stomach.
When acid levels are balanced, the ENS tells the brain everything is fine. You feel safe, fed, and calm. But when acid burns the esophageal lining or food sits undigested and fermenting, the signaling changes dramatically. It starts firing off urgent distress messages, and the brain reads those messages as anxiety.
The Vagus Nerve Highway
The main physical cable connecting your second brain to your primary brain is the Vagus nerve, the longest cranial nerve in the human body. It serves as the backbone of your parasympathetic nervous system, which controls your “rest and digest” functions.
Here is what makes this so important for mental health: 80 to 90 percent of vagal nerve fibers are sensory. They are dedicated entirely to sending information from the gut up to the brain, not the other direction. Your brain is essentially a receiver, constantly interpreting the chemical and physical data streaming up from the stomach lining.
If stomach acid splashes into the esophagus, the Vagus nerve picks up on the chemical burn immediately. It fires a high-priority distress signal to the brain stem. Because the brain struggles to tell the difference between a physical threat in the gut and an external life-or-death danger, it launches a full-blown anxiety response.
The Role of Neurotransmitters in Digestion
Beyond electrical signals, your gut depends heavily on chemical messengers called neurotransmitters. Most people think of serotonin and dopamine as brain chemicals tied to mood. In reality, these molecules evolved primarily to manage the complex process of digestion.
Serotonin in the gut controls how quickly food moves through the intestinal tract (peristalsis). When acid levels are off, the gut floods with serotonin to speed up digestion and flush out irritants. That sudden spike and crash in serotonin destabilizes your entire mood.
The gut also produces large amounts of GABA, your body’s primary calming neurotransmitter. Chronic inflammation from poor acid regulation suppresses GABA production, leaving your nervous system stuck in an agitated, hypervigilant state.
Expert Insight
Many patients spend years in cognitive behavioral therapy for panic attacks with limited improvement. Once we stabilize their stomach acid and calm the Vagus nerve, their “incurable” anxiety often disappears within weeks.
High Stomach Acid, GERD, and Panic Attack Mimicry
When a patient asks whether stomach acid can cause anxiety, they are usually talking about the terrifying sensations that come with severe acid reflux. Gastroesophageal reflux disease (GERD) does not just cause mild heartburn. It can hijack your central nervous system and mimic a full psychiatric emergency.
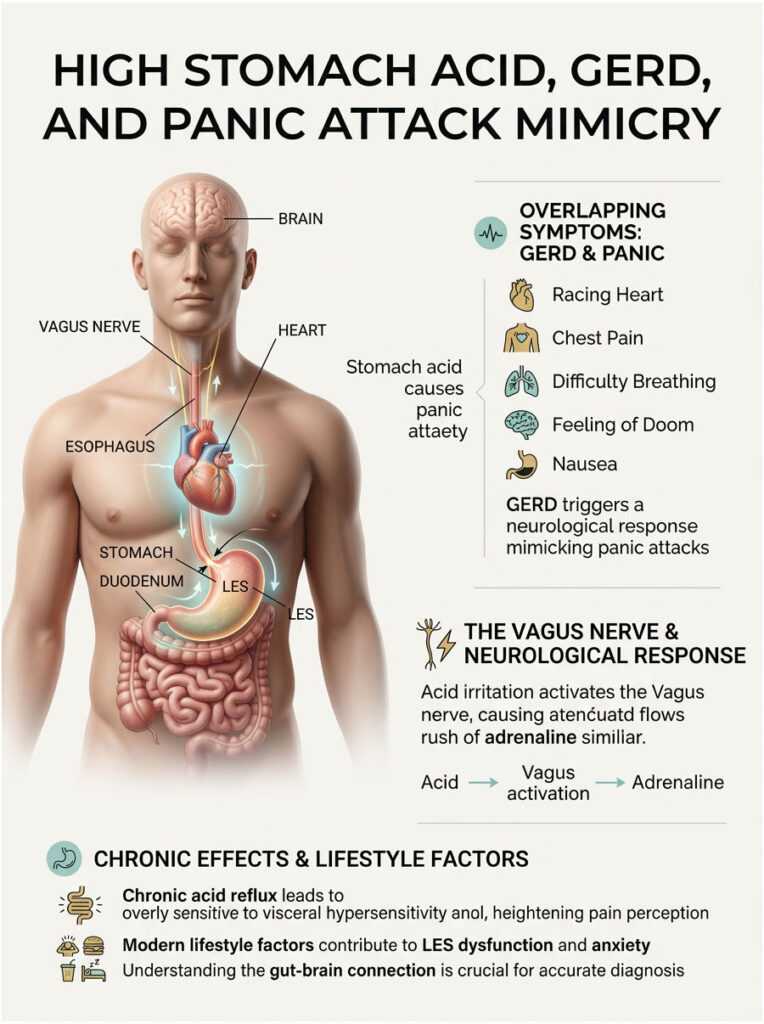
Excess acid creates a mechanical and neurological storm inside the chest. The physical irritation sets off a chain of chemical reactions that look and feel exactly like a clinical panic attack. Understanding this mechanism matters deeply for anyone who has ever rushed to the emergency room clutching their chest, because the overlap between a heart attack, a panic attack, and an acid reflux episode is remarkably high.
How Acid Reflux Triggers the Fight-or-Flight Response
Your stomach is lined with a thick, protective mucus layer built to withstand powerful hydrochloric acid. Your esophagus has no such protection. When the lower esophageal sphincter (LES) weakens, stomach acid breaches this barrier and flows upward into unprotected tissue.
This displaced acid burns the delicate esophageal lining almost instantly. Sitting right beneath that thin lining are thousands of highly sensitive vagal nerve endings. When acid scorches these nerves, the Vagus nerve goes into overdrive.
The brain’s amygdala, which is the central hub for fear processing, interprets this sudden nerve pain as a life-threatening emergency. It dumps adrenaline and cortisol into the bloodstream, causing your heart to race and your palms to sweat.
Visceral Hypersensitivity and the Brain’s Threat Detection
Over time, chronic acid reflux fundamentally rewires how your brain processes internal pain. This leads to a condition known as visceral hypersensitivity, where chronic esophageal inflammation permanently lowers your internal pain threshold.
Once this condition takes hold, even a normal, healthy amount of acid can trigger severe pain signals. The brain becomes hypervigilant, perceiving everyday digestive processes as intense pain or feelings of impending doom. Patients with visceral hypersensitivity often feel like they are having a heart attack after eating a perfectly ordinary meal.
Chest Pain vs. Panic Attacks: How Doctors Tell the Difference
One of the most common reasons people visit the emergency room is severe, unexplained chest pain. They believe they are having a cardiac event or a nervous breakdown. In many of these cases, the actual cause is severe acid reflux.
Both GERD and panic attacks cause tachycardia (a racing heartbeat you can feel in your throat), severe shortness of breath, and a crushing sensation behind the breastbone. This overlap is exactly why proper diagnosis requires understanding the gut-brain connection. Clinical data shows a 40 percent prevalence of anxiety in chronic reflux patients, confirming that GERD directly creates the psychological symptoms of panic.
The Lower Esophageal Sphincter and the Anxiety Loop
To stop this cycle, we have to look at the LES, the mechanical valve between the stomach and esophagus. In a healthy body, this valve stays tightly closed, opening only to let food pass downward.
Modern lifestyles frequently compromise this valve. Chronic stress, obesity, and diets heavy in ultra-processed foods cause the LES to become lax. When the valve weakens, acid escapes upward. High anxiety itself can cause the valve to spasm or weaken, allowing even more acid to escape. That acid then burns the esophagus, triggering more anxiety, which further weakens the valve, creating a devastating, self-perpetuating cycle.
GERD Symptoms vs. Panic Attacks: A Clinical Comparison
| Symptom | GERD / Acid Reflux | Clinical Panic Attack | Overlapping Features |
| Trigger | Post-meal, lying flat, trigger foods | Stress, psychological triggers, spontaneous | Sudden onset of extreme discomfort |
| Chest | Burning pain radiating upward | Tightness, crushing, sharp pain | Severe chest discomfort mimicking cardiac events |
| Breathing | Mild shortness from esophageal spasms | Hyperventilation, feeling unable to breathe | Labored breathing with chest restriction |
| Heart Rate | Palpitations from vagal irritation | Rapid tachycardia from adrenaline spikes | Racing heart and elevated pulse |
| Mental State | Secondary anxiety from physical pain | Primary feeling of doom or loss of control | Intense fear of a medical emergency |
The Silent Culprit: Hypochlorhydria (Low Stomach Acid) and Mood Disorders
While excess acid gets all the attention and pharmaceutical funding, there is a far more insidious problem affecting millions of people. Clinically low stomach acid, known as hypochlorhydria, is often much worse for mental health than having too much acid. When patients learn this, they are almost always shocked.
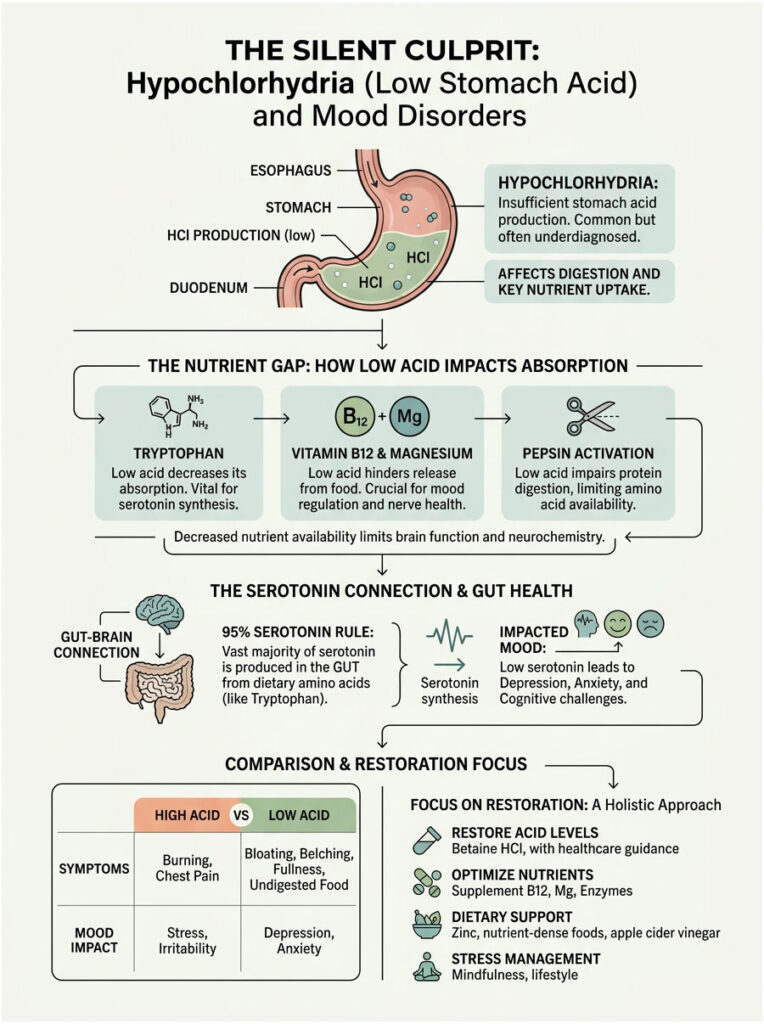
Hypochlorhydria and anxiety are deeply connected through the basic process of digestion and nutrient extraction. If your stomach cannot produce enough hydrochloric acid, your entire mental health foundation starts to crumble. Most people assume heartburn means they have too much acid, but in reality, low acid causes food to ferment in the stomach, creating gas that pushes acid upward. Millions of people are treating this with acid-blocking medications, unknowingly worsening their mental health.
The 95 Percent Serotonin Rule
Most people believe serotonin is produced entirely in the brain. That is a widespread misconception. In reality, 95 percent of the body’s serotonin is manufactured in the gut lining. But your gut cannot create serotonin from nothing. It needs amino acids extracted from dietary protein.
Stomach acid is the mandatory first step in breaking down dense proteins into usable amino acids. If you have low stomach acid, you cannot properly break down meat, eggs, or plant proteins. Without those raw materials, your gut cannot manufacture serotonin. The result is severe mood swings and persistent anxiety.
Protein Malabsorption and Neurotransmitter Deficiency
The specific amino acid required to build serotonin is tryptophan. When stomach acid drops too low, tryptophan passes through the digestive tract unabsorbed. This triggers a biological domino effect across the nervous system. Without tryptophan, serotonin production drops. When serotonin drops, melatonin production falls as well, leading to chronic insomnia.
It does not stop there. Low acid also prevents absorption of tyrosine, the direct precursor to dopamine. The result is lower dopamine levels, chronic depression, severe brain fog, and a nervous system that feels constantly on edge.
Micronutrient Depletion: Vitamin B12 and Magnesium
The connection between hypochlorhydria and anxiety extends well beyond amino acids. Strong stomach acid is critical for extracting vital micronutrients from your daily diet, especially Vitamin B12 and magnesium.
Low acid prevents the stomach from releasing intrinsic factor, a transport protein that B12 needs to survive the journey to the small intestine for absorption. Without B12, the myelin sheath protecting your nerves begins to degrade, directly contributing to anxiety and cognitive decline.
Magnesium serves as the body’s primary relaxation mineral. It calms the central nervous system and loosens tight muscles. Low acid causes severe magnesium malabsorption, which leads to chronic muscle tension, heart palpitations, and extreme irritability.
The Role of Pepsin in Mental Health
Hydrochloric acid does not digest food on its own. Its primary job is to lower the stomach’s pH enough to activate pepsin, a powerful protein-digesting enzyme. Your stomach secretes an inactive substance called pepsinogen. When it contacts strong acid, it transforms into active pepsin. If your acid is weak, this transformation never happens, and protein digestion stalls completely.
Without active pepsin, the critical mood-boosting amino acids stay locked inside the food you eat. You could be eating the healthiest diet imaginable, but without pepsin, you remain functionally malnourished. This hidden cellular starvation is a leading yet rarely diagnosed cause of chronic anxiety disorders.
High Acid vs. Low Acid: Mental Health Impact Comparison
| Clinical Marker | High Acid (Hyperchlorhydria) | Low Acid (Hypochlorhydria) |
| GI Symptoms | Heartburn, acid regurgitation, frequent burping | Bloating after meals, undigested food in stool |
| Neurological Impact | Vagus nerve irritation, immediate fight-or-flight | Neurotransmitter starvation, poor nerve conduction |
| Anxiety Type | Acute panic attacks, racing heart, health anxiety | Chronic low-grade anxiety, brain fog, depression |
| Nutrient Absorption | Generally intact unless altered by medication | Severe malabsorption of B12, iron, zinc, magnesium |
| Treatment Focus | Soothing esophageal lining, regulating vagal tone | Restoring HCl levels, supplementing digestive enzymes |
How Acid-Suppressing Medications Affect Your Mental Health
When patients experience heartburn, the standard medical response is to prescribe acid-blocking medications. While these drugs provide fast physical relief, they often create serious long-term psychiatric consequences. By artificially shutting down stomach acid production, we are essentially turning off the body’s primary digestive engine, with profound implications for the microbiome gut-brain axis.
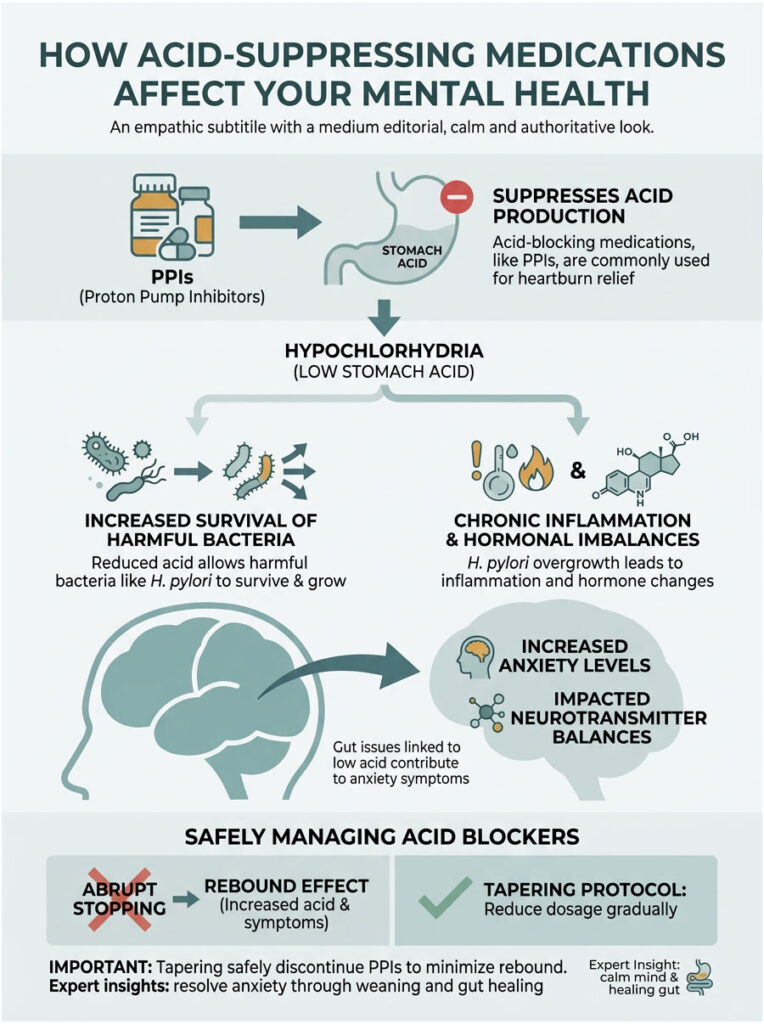
Many patients in my clinic report that their anxiety started right around the time they began taking antacids. This is not a coincidence. It is a direct biological reaction to artificially induced digestive shutdown.
Proton Pump Inhibitors (PPIs) and the Microbiome
Proton Pump Inhibitors are among the most widely prescribed daily medications in the world. They work by permanently disabling the acid-producing pumps in your stomach lining. While highly effective for healing acute ulcers, long-term use artificially creates a state of hypochlorhydria, and as we covered, hypochlorhydria and anxiety go hand in hand.
There is another critical issue. Strong stomach acid is your body’s first line of immune defense. It sterilizes food by killing harmful bacteria entering through your mouth. Without this acidic barrier, pathogenic bacteria survive and travel into your intestines, destroying the delicate balance of the microbiome gut-brain axis.
H. pylori Overgrowth and Chronic Inflammation
When the stomach lacks sufficient acid, a resilient bacteria called Helicobacter pylori can easily colonize the upper GI tract. H. pylori burrows deep into the stomach lining, creating chronic, low-grade inflammation you might not even feel.
This hidden infection throws off the balance of gastrin and stress hormones. H. pylori manipulates the system, causing spikes in systemic inflammation and forcing the body to keep cortisol levels elevated. Chronically high cortisol disrupts enteric nervous system signaling and damages brain tissue over time. Recent clinical trials show a strong correlation between extended PPI use, H. pylori overgrowth, and increased rates of clinical depression.
The Rebound Effect of Stopping Acid Blockers
If you have been taking acid blockers for years, you cannot simply stop cold turkey. Specialized cells in the stomach lining monitor acid levels constantly. When they sense acid has been suppressed, they multiply to try to override the medication.
When you suddenly stop, those multiplied cells release a massive surge of hydrochloric acid. This is known as acid rebound hypersecretion. The flood of acid severely burns the esophagus, triggering an extreme vagal nerve response and intense panic attacks. This terrifying rebound effect convinces patients they need the medication to survive, trapping them in a lifelong cycle. Safely exiting requires a carefully planned tapering protocol with natural soothing agents to protect the esophageal lining.
Expert Insight
We consistently see patients whose anxiety peaked shortly after starting long-term PPI therapy. Weaning them off safely while healing the gut lining with targeted nutrients often resolves their psychiatric symptoms entirely.
Clinical Case Studies: Real-World Evidence
To truly grasp how stomach acid can cause anxiety, it helps to look at real clinical scenarios. These cases demonstrate how the gut-brain connection plays out in practice, exactly as the biochemistry predicts.
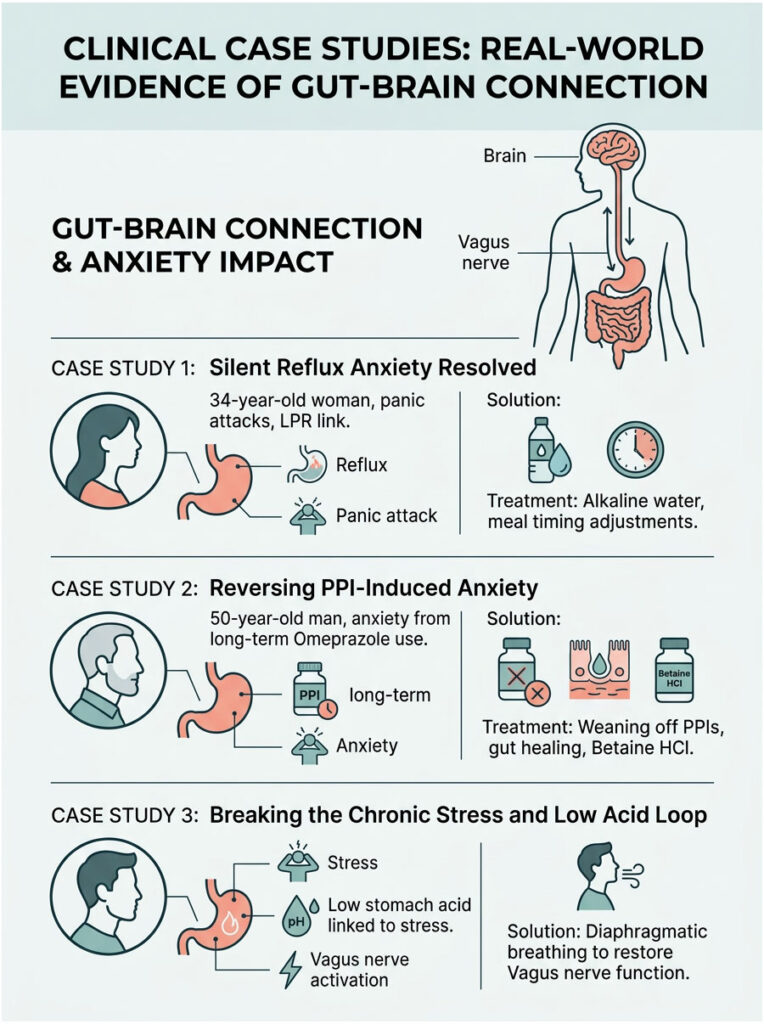
Case Study 1: Silent Reflux Anxiety Resolved
A 34-year-old woman came in with a formal diagnosis of generalized anxiety disorder. She had sudden panic attacks, a constant urge to clear her throat, and a sensation of a tight lump in her throat. She never once experienced classic heartburn.
Endoscopic testing revealed Laryngopharyngeal Reflux (LPR), or silent reflux. Microscopic droplets of aerosolized stomach acid were bypassing her esophagus entirely and landing on her vocal cords and upper vagal nerve endings. Because she felt no burning in her chest, previous doctors completely missed the digestive connection.
The invisible acid was irritating the Vagus nerve in her throat, triggering visceral hypersensitivity. We treated her by neutralizing pepsin in her throat with alkaline water protocols and adjusting her meal timing. Her panic attacks disappeared completely within three weeks.
Case Study 2: Reversing PPI-Induced Anxiety
A 50-year-old man had been taking daily Omeprazole for over ten years. Over the last three, he developed crippling anxiety that prevented him from working. He suffered from brain fog, chronic fatigue, and daily panic attacks despite being medicated.
Comprehensive blood panels revealed dangerously low B12 and zero detectable stomach acid, confirming severe medically induced hypochlorhydria. His gut could not absorb tryptophan, meaning his prescribed SSRI had no serotonin to work with.
We slowly weaned him off PPIs over two months while healing his gut lining with L-glutamine. Betaine HCl supplements restored his digestive power, stabilized his neurotransmitter levels, and completely cured his daily panic attacks.
Case Study 3: Breaking the Chronic Stress and Low Acid Loop
A 28-year-old software engineer dealt with severe bloating after meals, a racing heart, and intense social anxiety. He assumed his high-stress job was simply wearing him down psychologically.
We discovered that chronic stress had suppressed his Vagus nerve function. Because the Vagus nerve controls acid secretion, his stress caused acid production to plummet. Low acid made his meals ferment, creating gas that pressed against his diaphragm and heart, triggering vagal palpitations that fueled his anxiety further.
We broke the cycle with deep diaphragmatic breathing exercises before meals to manually engage the Vagus nerve. By forcing his body into a parasympathetic state before eating, his natural acid production returned and his post-meal anxiety vanished.
Practical Strategies for Gut-Brain Healing
Now that we have established that stomach acid issues cause anxiety, what can you actually do about it? You do not have to live at the mercy of a dysfunctional gut-brain connection. There are concrete, clinically proven steps you can take starting today.

Healing requires a comprehensive approach that addresses both the physical and biochemical sides. You need to calm the nerve irritation, restore natural acid production, and fix the underlying bacterial balance. Consistency is the key, because you are working to rewire a nervous system that has been stuck on high alert for years.
Vagus Nerve Exercises for GERD and Anxiety
If you are experiencing a panic attack driven by acid reflux, you need to manually override your nervous system by stimulating the Vagus nerve to enforce a calm, parasympathetic state.
Deep diaphragmatic breathing (4-7-8 method): Place your hand on your belly and breathe in slowly through your nose for four seconds, ensuring your belly expands. Hold for seven seconds, then exhale through pursed lips for eight seconds. Expanding the lower lungs mechanically stimulates the Vagus nerve.
Cold water exposure: Splash ice-cold water on your face, targeting the area around your eyes and upper cheeks. This triggers the mammalian dive reflex, which slows your heart rate and resets enteric nervous system signaling.
Nutritional Interventions for Healthy HCl Production
If low stomach acid is driving your anxiety, rebuilding your digestive capacity is essential. Diet plays a major role in this process.
Zinc-rich foods: Incorporate roasted pumpkin seeds, fresh oysters, and grass-fed beef into your diet. Zinc is a mandatory co-factor for the cellular production of stomach acid.
Bitter herbs before meals: Consume dandelion root tea, gentian, or fresh arugula about 15 minutes before eating. The bitter taste activates receptors that signal the brain to release gastric juices, improving protein breakdown and stopping tryptophan malabsorption.
Addressing Hidden Bacterial Overgrowth
You cannot fully heal the microbiome gut-brain axis while harboring a hidden bacterial infection. Overgrowths like SIBO or H. pylori constantly manipulate gastrin levels and stress hormones to ensure their own survival.
Ask your functional doctor for comprehensive stool testing, such as a GI-MAP. If H. pylori is present, targeted antimicrobial protocols are necessary. Once pathogens are cleared, rebuild the microbiome with specific probiotic strains like Lactobacillus rhamnosus and Bifidobacterium longum, which have been clinically shown to lower cortisol and support GABA production.
Strategic Supplementation for Nervous System Support
While food comes first, supplementation can accelerate healing. In cases of severe acid deficiency, Betaine HCl with Pepsin supplements, taken midway through a protein-heavy meal, supply the acid your body is failing to produce. This stops tryptophan malabsorption and allows serotonin synthesis to resume. Work closely with a qualified practitioner to find the right dosage.
Additionally, high-quality magnesium glycinate taken before bed calms the nervous system and relaxes esophageal spasms. Sublingual Vitamin B12 drops bypass the broken digestive tract entirely, absorbing directly into the bloodstream to help repair damaged vagal nerves.
Summary and Key Takeaways
We started with a critical question: can stomach acid cause anxiety? The scientific research, biochemical pathways, and clinical evidence all point to a resounding yes. Your digestive tract and your brain are wired together as a single, highly reactive system.
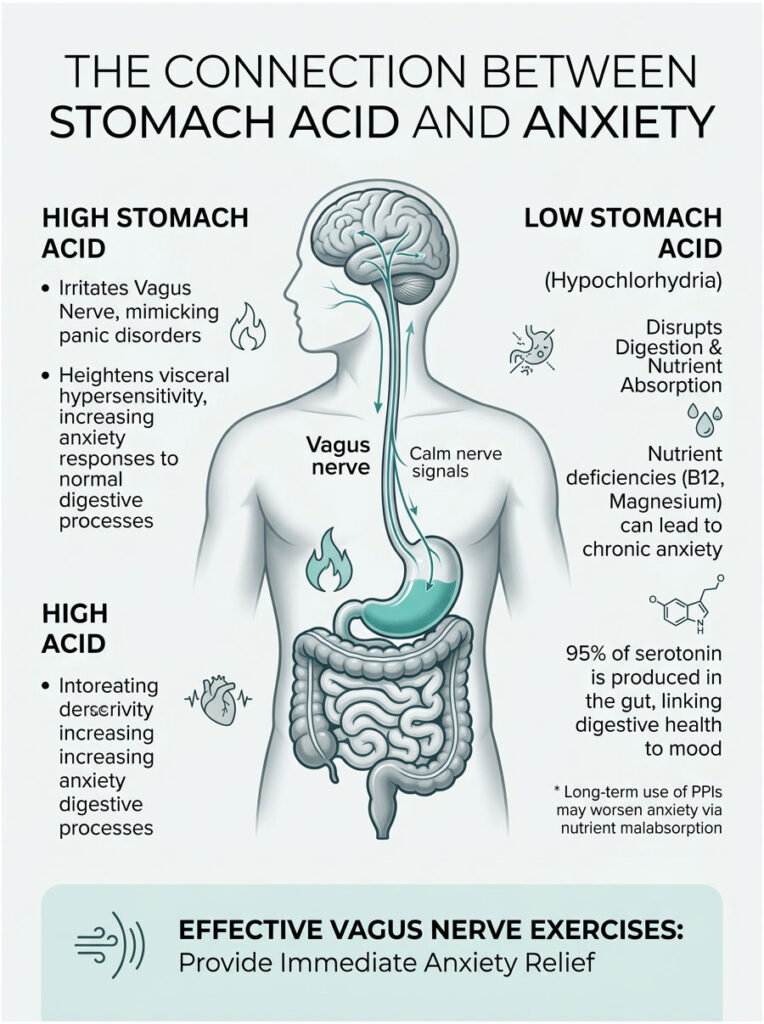
Excess acid causes physical nerve irritation that triggers visceral hypersensitivity. This sends false alarms up the Vagus nerve, resulting in acute panic mimicry that often presents as silent reflux anxiety. On the other side, low stomach acid causes a systemic failure in digestion. This leads to hypochlorhydria and anxiety through chronic nutrient starvation, where tryptophan malabsorption prevents serotonin production and B12 and magnesium deficiencies systematically destroy nerve health.
If you suffer from chronic anxiety, it is time to look beyond the confines of the brain. Seek a functional gastroenterology approach to your mental health. By restoring natural acid levels, calming the Vagus nerve, and balancing your microbiome, you can reclaim your mental health from the ground up.
Frequently Asked Questions
Can stomach acid levels actually trigger a clinical panic attack?
Yes, absolutely. High stomach acid can physically irritate the Vagus nerve, which is the primary sensory highway between your gut and brain. When this nerve is scorched by acid reflux, it sends high-priority distress signals to the amygdala, triggering a systemic fight-or-flight response that perfectly mimics a primary panic disorder.
What is the relationship between hypochlorhydria and chronic anxiety?
Hypochlorhydria, or low stomach acid, prevents the proper breakdown of dietary proteins into amino acids. Without sufficient acid to activate the enzyme pepsin, your body cannot extract tryptophan, the essential precursor for serotonin. This leads to a chemical deficiency in the gut-brain axis, manifesting as chronic anxiety and mood instability.
How does the Vagus nerve influence the gut-brain connection?
The Vagus nerve contains roughly 80 to 90 percent sensory fibers that send data from the gut upward to the brain. It acts as a receiver for the chemical environment of your stomach. If the enteric nervous system detects inflammation or improper acid levels, the Vagus nerve transmits this as a ‘biological threat,’ causing the brain to initiate psychological anxiety protocols.
Why is 95 percent of serotonin produced in the gut significant for mental health?
Since the vast majority of your ‘happy chemical’ is manufactured in the gastrointestinal tract, any digestive dysfunction directly impacts your emotional state. If stomach acid is too low to facilitate nutrient absorption, your gut-based serotonin production plummets, leaving you vulnerable to depression and generalized anxiety disorder.
Can long-term use of PPIs or acid blockers cause anxiety?
Clinical evidence suggests that long-term Proton Pump Inhibitor (PPI) use can indeed worsen anxiety. By artificially suppressing stomach acid, these medications induce a state of medical hypochlorhydria, which leads to the malabsorption of Vitamin B12 and magnesium—two micronutrients that are critical for nervous system stability and stress regulation.
What is ‘silent reflux anxiety’ or LPR?
Laryngopharyngeal Reflux (LPR), or silent reflux, occurs when microscopic droplets of acid reach the throat without causing traditional heartburn. This irritates the upper Vagus nerve endings, often causing a ‘lump in the throat’ sensation (globus pharyngeus) and triggering unexplained panic attacks that doctors often misdiagnose as purely psychological.
How do I distinguish between a heart attack, a panic attack, and GERD?
The symptoms—tachycardia, chest tightness, and shortness of breath—overlap significantly. However, GERD-related panic often follows heavy meals, occurs when lying flat, or is accompanied by a burning sensation behind the breastbone. Because they are so similar, we use functional testing to see if calming the Vagus nerve resolves the chest discomfort.
What is visceral hypersensitivity and how does it affect mood?
Visceral hypersensitivity is a neurological condition where chronic inflammation in the esophagus lowers your internal pain threshold. Your brain becomes hyper-vigilant, overreacting to normal digestive processes or minor acid fluctuations as if they were life-threatening emergencies, keeping your nervous system in a state of constant agitation.
Can a H. pylori infection contribute to anxiety disorders?
Yes. H. pylori bacteria can colonize the stomach lining, disrupting gastrin levels and causing chronic low-grade inflammation. This infection forces the body to maintain elevated cortisol levels and disrupts the microbiome gut-brain axis, which is strongly correlated with increased rates of clinical depression and panic.
How does low stomach acid lead to magnesium and B12 deficiency?
Strong hydrochloric acid is required to release Vitamin B12 from food proteins and to initiate the absorption of minerals like magnesium. Without adequate acid, these nutrients pass through the system unabsorbed. A deficiency in B12 degrades the nerve’s myelin sheath, while low magnesium prevents the nervous system from entering a relaxed, parasympathetic state.
What are the best Vagus nerve exercises for immediate anxiety relief?
To manually override a gut-induced panic response, I recommend the 4-7-8 diaphragmatic breathing technique, which mechanically stimulates vagal receptors. Additionally, splashing ice-cold water on your face can trigger the mammalian dive reflex, instantly slowing a racing heart and resetting the enteric nervous system signaling.
Should I take Betaine HCl if I have anxiety and digestive issues?
If your anxiety is rooted in hypochlorhydria (low acid), supplementing with Betaine HCl and Pepsin can help restore proper protein digestion and neurotransmitter synthesis. However, this must be done under professional guidance, as adding acid to an already inflamed or ulcerated stomach lining can cause severe irritation and worsen Vagus nerve distress.
Disclaimer
This article is for informational purposes only and does not constitute medical advice. The connection between digestive health and mental state is a complex biological process that requires professional diagnosis. Always consult a qualified healthcare professional or gastroenterologist before making changes to your medication or starting new supplementation protocols.
References
- Cleveland Clinic – https://my.clevelandclinic.org/health/body/the-gut-brain-connection – Comprehensive overview of how the enteric nervous system communicates with the brain.
- Harvard Health Publishing – https://www.health.harvard.edu/diseases-and-conditions/the-gut-brain-connection – Detailed insights into how gastrointestinal distress can be the cause or product of anxiety.
- Journal of Clinical Medicine – “The Relationship Between GERD and Anxiety Disorders” (2021) – Clinical study identifying the 40% prevalence rate of anxiety in chronic reflux patients.
- Nature Communications – “Gut-derived Serotonin and its Role in Global Health” – Research paper confirming that 95% of the body’s serotonin is manufactured in the GI tract.
- National Center for Biotechnology Information (NCBI) – https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5859128/ – Study on Vagus nerve stimulation and its effects on emotional regulation and the parasympathetic nervous system.
- American Psychological Association (APA) – https://www.apa.org/monitor/2012/09/gut-feeling – Expert insight into the “second brain” and the role of gut bacteria in mood regulation.