Patients walk into my exam room every day worried about body changes they never expected. Morning sickness gets all the attention in movies and pregnancy books, but sudden shifts in bowel habits are just as common and often cause unnecessary panic.
Table of Contents
So let me answer the question directly: is diarrhea a symptom of pregnancy? As a Board-Certified OB-GYN with over 15 years of clinical experience, the short answer is absolutely yes. It affects a significant percentage of my expectant patients.
Pregnancy sets off a cascade of hormonal shifts that fundamentally change how your gastrointestinal tract works. Your body is adapting rapidly to support a growing baby, and your digestive system takes a real hit during the process. Many women experience everything from stubborn constipation to sudden, unpredictable loose stools.

Understanding what counts as clinical diarrhea versus a temporary bout of loose stools matters for your peace of mind. Clinical diarrhea means three or more watery bowel movements within a 24-hour period. A single episode of loose stool after a rich meal or a new prenatal vitamin is a different story entirely.
This guide is built on current clinical standards from the American College of Obstetricians and Gynecologists (ACOG) and the Centers for Disease Control and Prevention (CDC). We will walk through exactly why your gut is acting up, when you can safely manage it at home, and when you need to call your doctor right away.
Quick Answer
Is diarrhea a symptom of pregnancy? Yes. Hormonal surges, shifting gut bacteria, and prenatal vitamins frequently cause loose stools. First-trimester diarrhea is usually tied to rising hormones. Third-trimester diarrhea often signals your body preparing for labor. Always contact your doctor if symptoms last more than 48 hours or come with a fever over 100.4 F.
Key Statistics on Pregnancy and Digestion
34% of pregnant women report significant bowel changes in the first trimester (NIH, 2022).
10x higher risk of Listeria infection during pregnancy compared to the general population (CDC, 2023).
8-12 cups of water daily needed to maintain healthy amniotic fluid levels during pregnancy.
40%+ of women on high-dose iron supplements experience GI distress within the first week.
60% of women experience loose stools in the 48 hours before spontaneous labor begins.
25% reduction in pregnancy-related GI upset with daily probiotic use in clinical trials.
15% of pregnant women require short-term pharmacological intervention for severe loose stools.
The Physiological Domino Effect: Why Pregnancy Causes Diarrhea
When you conceive, the changes are not limited to your uterus. Every organ in your body adapts to support the new life growing inside you. Your digestive tract is extremely sensitive to these systemic shifts, which is exactly why early pregnancy diarrhea is so common.
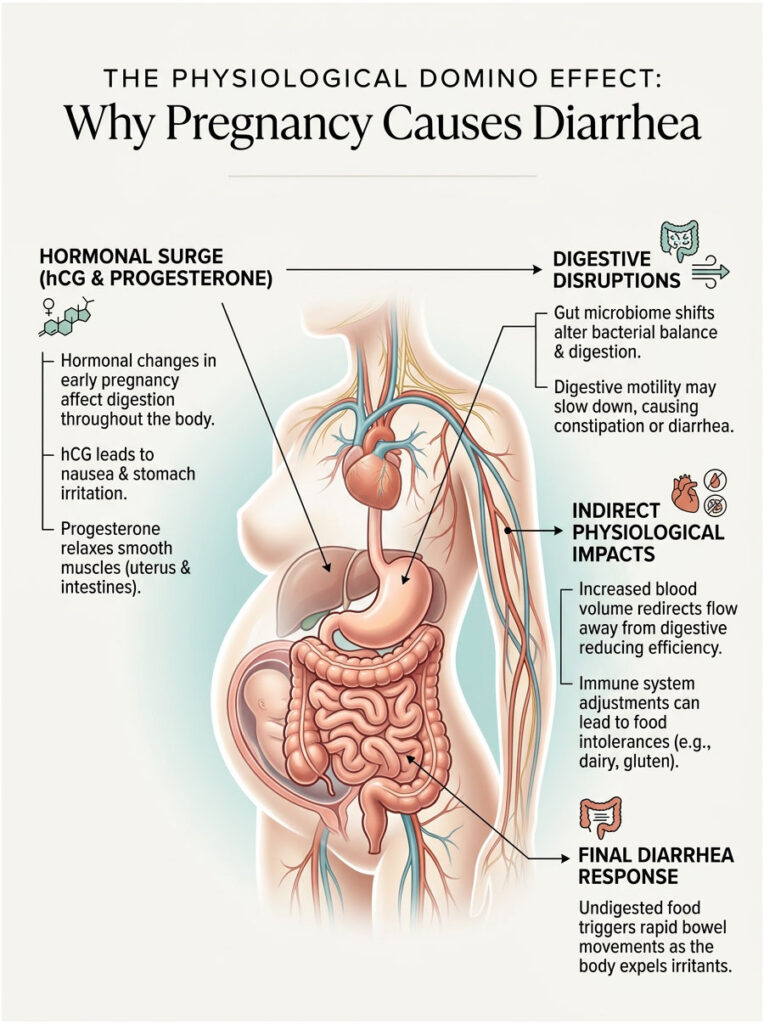
Your endocrine system starts producing massive amounts of hormones to keep the pregnancy safe. These powerful chemicals act as messengers, instructing your muscles and organs how to behave. The catch is that they are not very precise in their targeting. They affect your stomach and intestines just as much as your reproductive organs.
Many women notice their digestion changes before they even miss a period. From a biological perspective, this makes perfect sense. The moment an embryo implants, chemical signals begin reshaping your baseline physiology.
How hCG and Progesterone Alter GI Motility
Human Chorionic Gonadotropin (hCG) is the hormone that turns a home pregnancy test positive. It spikes dramatically in the first few weeks and is directly linked to nausea, vomiting, and stomach upset. As your body adjusts to this hormone, your stomach lining can become highly irritated.
But progesterone is the real driver behind most digestive trouble during pregnancy. Progesterone causes smooth muscle relaxation throughout your pelvis, which is essential for keeping the uterus calm and preventing premature contractions. The problem is that your intestines are also made of smooth muscle tissue.
When progesterone relaxes the bowels, gastrointestinal motility changes significantly. For some women, digestion slows to a crawl, causing constipation. For others, the relaxed muscles fail to absorb water properly from waste, leaving excess water in the colon that rushes out as diarrhea.
According to data from the National Institutes of Health, progesterone’s effects on smooth muscle are profound. The hormone completely alters the rhythmic contractions of your intestines. When that rhythm is disrupted, bowel movements become entirely unpredictable. If you are wondering whether loose stool can be an early sign of pregnancy, the answer is yes. It can be one of the very first indicators that progesterone levels are climbing.
The Shift in the Gut Microbiome
Your gut contains trillions of bacteria that help you digest food every day. This complex ecosystem, the gut microbiome, is naturally altered during pregnancy. Your body intentionally reshapes these bacterial colonies to support fetal immune development.
Your immune system lowers its defenses slightly so it does not reject the growing fetus. Because the immune system is closely linked to your gut, the bacterial landscape shifts. When the balance of good and bad bacteria fluctuates, you experience unpredictable bowel movements.
In my practice, I regularly see women who suddenly cannot tolerate dairy or gluten. Their microbiome is actively adjusting. This adaptation phase is entirely normal, though understandably frustrating.
Increased Blood Volume and Digestion
Another major change is your total blood volume. During pregnancy, your body produces up to 50% more blood to supply the placenta. To support the uterus, blood flow is frequently diverted away from the digestive tract.
When your stomach and intestines receive less blood, their efficiency drops. Food is not broken down as thoroughly. Undigested particles traveling into the lower intestines can trigger a rapid bowel flush, as the body recognizes the undigested matter as an irritant and floods the colon with water to expel it quickly.
First Trimester Diarrhea: Tracking Early Pregnancy Symptoms
The first trimester is often a grueling period of survival. You are exhausted, nauseous, and dealing with unpredictable bathroom habits. Many patients ask about their stomach upset at their very first ultrasound appointment, wanting to know if it is a contagious bug or just the baby.
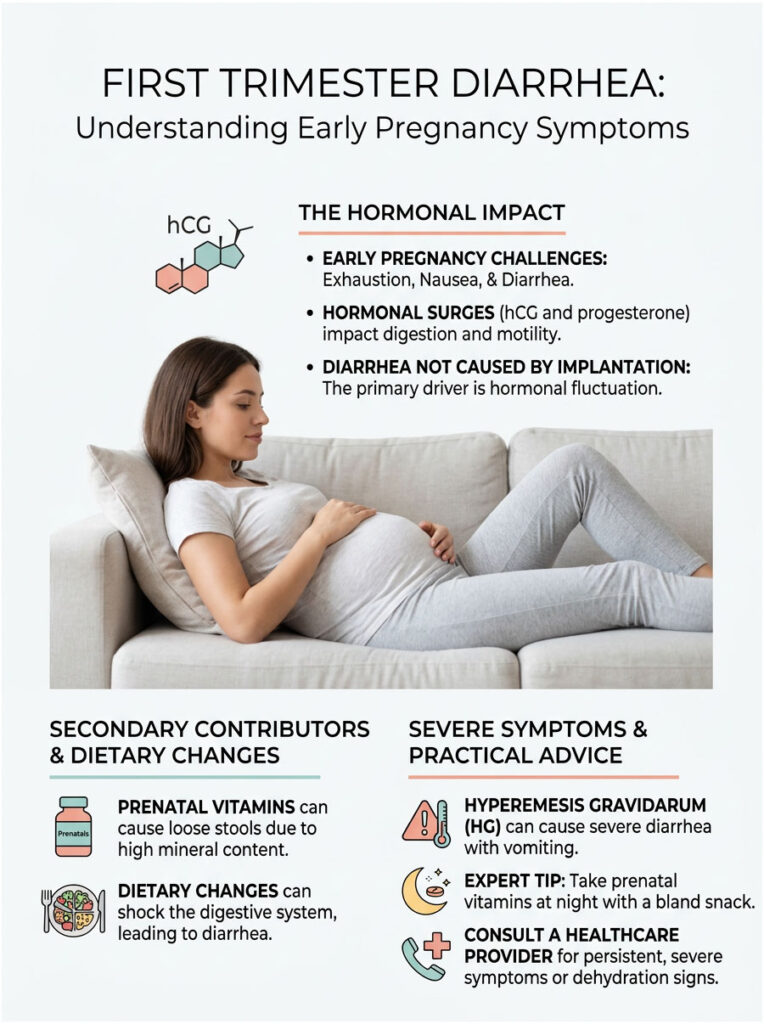
In many cases, it is strictly related to the pregnancy. The energy required to build a placenta and support rapid cell division takes a heavy toll on digestion. Diarrhea during the first trimester is a frequent and expected complaint.
Implantation and Hormonal Surges
Patients frequently ask if loose stools are directly caused by implantation. To be clear, loose stool is not a direct mechanical result of the embryo attaching to the uterine wall. Instead, the immediate hormonal surge after conception triggers the gastrointestinal distress.
Once implantation occurs, hCG and progesterone flood your bloodstream. This sudden chemical shift causes the gut to react defensively. The intestines may spasm or rapidly flush out their contents. This is why early pregnancy diarrhea often accompanies breast tenderness and profound fatigue. They are all side effects of the same hormonal flood.
If you experience severe cramping and diarrhea in early pregnancy, it may simply be this initial hormonal adjustment. However, severe pain is always monitored closely to rule out dangerous complications.
Why Do Prenatal Vitamins Cause Loose Stools?
This is one of the most common questions I hear. Prenatal vitamins are packed with high doses of iron, magnesium, and synthetic folates. Your body needs these nutrients, but your stomach lining does not always handle them well.
When you swallow a large prenatal vitamin, your body tries to absorb the heavy minerals. High-dose iron and magnesium are notoriously difficult to absorb completely. The unabsorbed minerals travel into the lower colon, where they draw water from your body through osmosis. This excess water floods the colon and results in sudden osmotic diarrhea.
Expert Tip
If prenatal vitamins are causing loose stools, try taking them at night before bed with a small, bland snack. If symptoms persist, ask your OB-GYN about switching to an iron-free, whole-food-based prenatal vitamin during the first trimester. You can supplement iron later when your stomach settles.
Hyperemesis Gravidarum and Paradoxical Bowel Movements
Standard morning sickness is manageable for most women, but Hyperemesis Gravidarum (HG) is a severe medical condition involving relentless vomiting that prevents you from keeping food or fluids down. This leads to extreme fluid shifts within the body.
You might expect constant vomiting to leave your bowels empty. Paradoxically, the resulting electrolyte imbalance can cause severe diarrhea alongside the vomiting. When potassium and sodium levels crash, intestinal muscles lose their ability to contract normally, leading to rapid, watery stools.
Diarrhea combined with HG in the first trimester is a dangerous combination that rapidly accelerates dehydration. If you are experiencing both, you need immediate clinical support, often involving intravenous fluids.
Dietary Cravings and Sudden Shifts
Your taste buds change drastically in the first twelve weeks. You might suddenly crave foods you never liked before. Eating large amounts of highly processed foods can shock your system.
For example, craving fast food introduces massive amounts of sodium and refined oils. Your stomach simply does not have the enzymes primed for this sudden change. The result is a rapid digestive flush. We see this often when patients switch from a whole-food diet to surviving on saltines and ginger ale. The lack of dietary fiber prevents stool from forming properly. Try to incorporate small amounts of soluble fiber even when you feel sick.
Second Trimester: The “Honeymoon Phase” and Digestive Surprises
By week 14, the placenta takes over hormone production and the jarring hCG spikes begin to level off. For most women, the second trimester brings welcome relief from nausea and early pregnancy diarrhea. Energy returns, the stomach settles, and the baby bump starts showing.
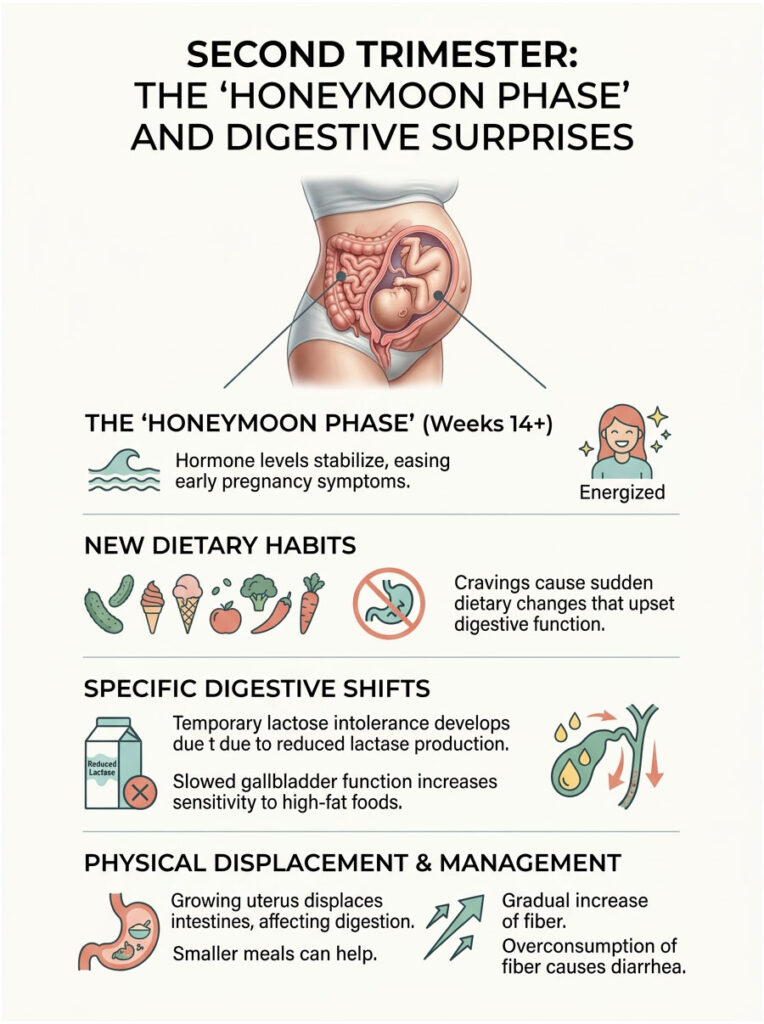
But this phase is not entirely free of digestive issues. While first-trimester diarrhea is mostly hormonal, second-trimester problems are usually dietary. Your appetite comes roaring back, and with it come unpredictable cravings.
Dietary Changes and New Food Sensitivities
Sudden dietary shifts easily irritate the bowel. You might go from eating plain crackers to craving spicy food and ice cream at midnight. Your gut struggles to keep up with the influx of rich foods, overwhelming your available digestive enzymes.
New food sensitivities often develop mid-pregnancy. Temporary lactose intolerance is incredibly common. Even if you drank milk your entire life, pregnancy hormones can suppress lactase production, the enzyme needed to digest dairy. A large bowl of ice cream can suddenly trigger explosive loose stools.
Gallbladder Function and Fat Malabsorption
Sensitivity to high-fat foods also emerges during the second trimester. The gallbladder empties much more slowly during pregnancy due to systemic muscle relaxation. When you eat a greasy meal, your body struggles to break down the heavy fats. Undigested fat travels straight to the colon, causing a rapid, watery bowel movement.
We also see patients overcompensating with massive amounts of raw vegetables and fruits to make up for first-trimester malnutrition. Too much fiber introduced too quickly will cause temporary diarrhea. Increase your fiber intake gradually.
Fetal Growth and Intestinal Space
As the baby grows, the uterus expands upward and outward, displacing your intestines. This mechanical pressure changes how food moves through your body. Sometimes it creates pockets where waste moves too quickly, preventing proper water absorption. Eating smaller, more frequent meals helps mitigate this. Smaller portions require less space to digest and often resolve mid-pregnancy bowel issues entirely.
Third Trimester Diarrhea: Your Body Preparing for Labor
As you cross the 28-week mark, the baby grows rapidly and space in your abdominal cavity becomes scarce. Internal organs are pushed upward and compressed. Digestion naturally slows during this time.
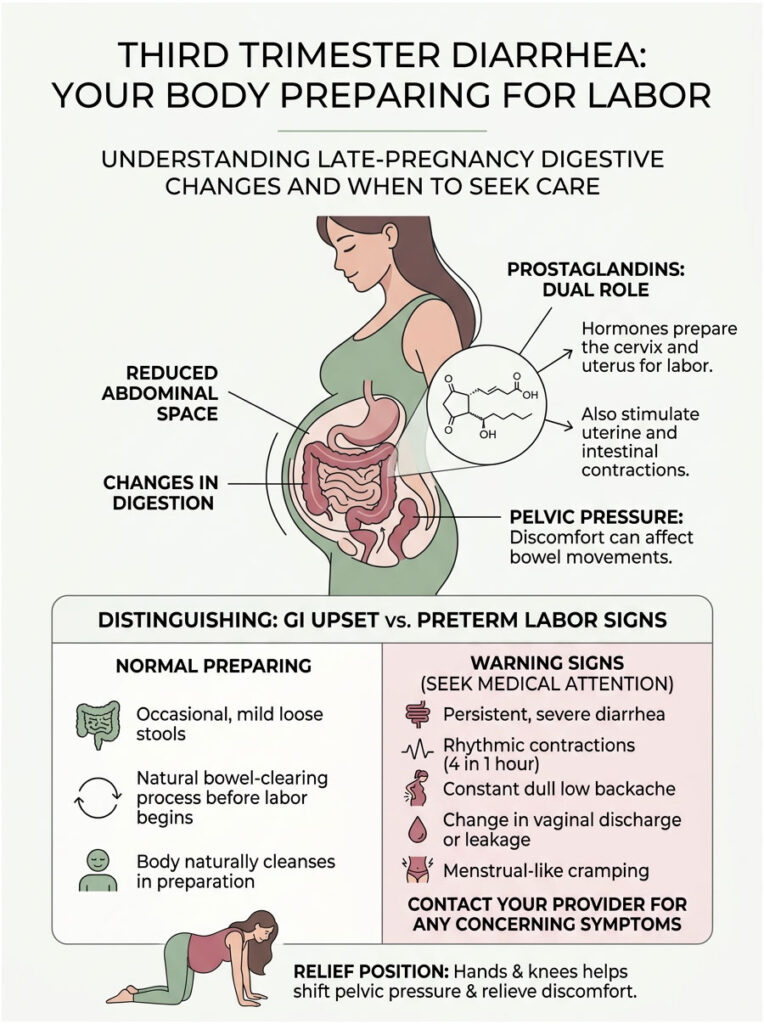
However, as you approach your due date, the picture changes. Diarrhea in the third trimester is a well-documented clinical phenomenon. When patients call my triage line at 38 weeks reporting sudden loose stools, I pay close attention. It is frequently the body’s natural way of clearing the bowels to make room for the baby’s descent into the birth canal.
Prostaglandins and Bowel Stimulation
As your body prepares for delivery, it releases hormone-like lipids called prostaglandins. Their primary role is cervical ripening, softening the cervix so it can thin out and open. But prostaglandins do not stay localized in the cervix. They circulate through your bloodstream and heavily impact the digestive tract.
Because the bowels are sensitive to prostaglandins, they react by contracting and emptying. Usually 24 to 48 hours before contractions begin, prostaglandin levels peak, causing the intestines to flush themselves. This ensures the lower abdomen is as empty as possible, giving the uterus maximum space to work effectively.
So, is diarrhea a symptom of pregnancy nearing its end? Yes. Diarrhea in the third trimester, especially after 37 weeks, is often your body’s early warning system that labor is approaching.
Distinguishing Preterm Labor from Normal GI Upset
While loose stools at 39 weeks are expected, diarrhea at 30 weeks requires careful evaluation. We must differentiate between standard GI upset and the onset of preterm labor, which also involves premature prostaglandin release.
Normal GI upset typically resolves shortly after using the restroom. The cramping is diffuse, mild, and located higher in the abdomen. Preterm labor, in contrast, comes with specific warning signs: rhythmic cramping that wraps from your belly to your lower back, intense pelvic pressure as if the baby is pushing down, loss of the mucus plug, or unexpected vaginal bleeding.
If you experience diarrhea in the third trimester with more than four contractions per hour, head directly to labor and delivery triage. We can often stop preterm labor if caught early, but we cannot help if you stay home assuming it is just a stomach bug.
Pelvic Pressure and Rectal Nerves
As the baby’s head drops into the pelvis, it presses against the lower colon and rectum. This stimulates the rectal nerves constantly, and your brain interprets this as an urgent need to empty the bowels. The result is frequent, small, loose movements. This is not true clinical diarrhea, but it certainly feels like it. The medical term is tenesmus.
You can relieve this pressure temporarily by spending time on your hands and knees. This position lets the baby shift slightly off the rectal nerves and provides brief relief from constant bathroom trips.
When to Worry: Hormonal Changes vs. Clinical Infections
Not all stomach issues during pregnancy are harmless. While diarrhea is generally a normal symptom of pregnancy, there are critical exceptions. Your immune system is significantly altered right now, making you highly susceptible to dangerous foodborne pathogens.
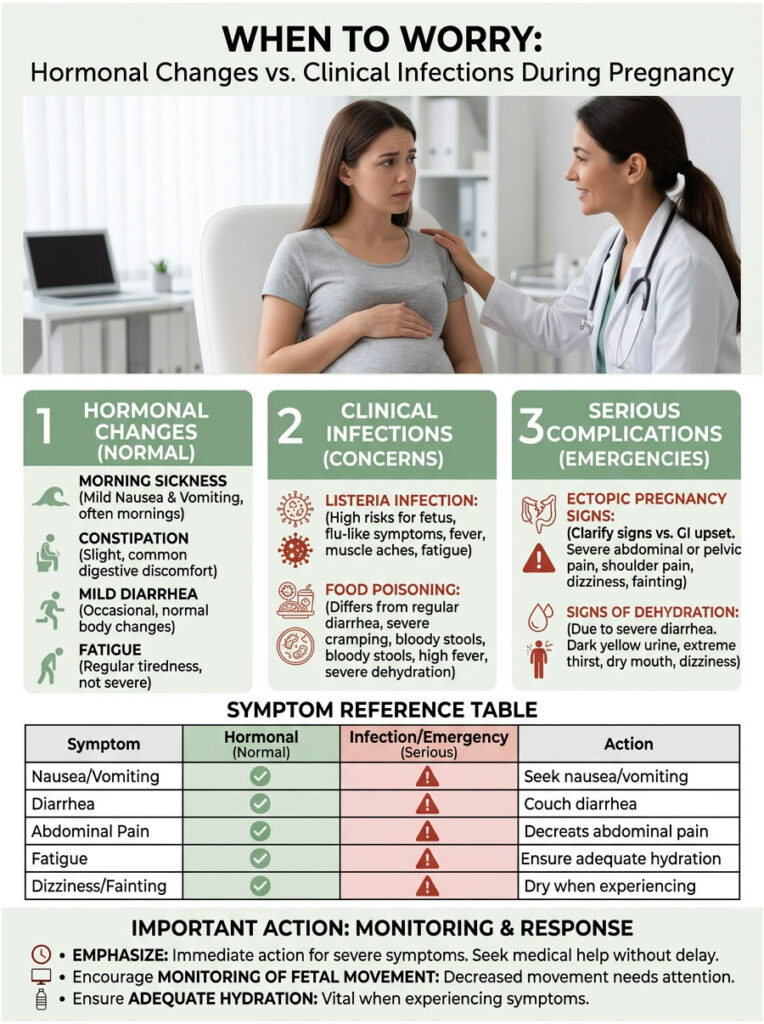
You must know the difference between a hormonal digestive flush and a clinical infection. Ignoring a dangerous pathogen can lead to severe fetal complications, including miscarriage or stillbirth.
Listeria Symptoms in Pregnancy
Pregnant women are uniquely vulnerable to Listeria monocytogenes. According to the CDC, you are 10 times more likely to contract Listeria while pregnant. Symptoms often mimic a severe stomach bug: deep muscle aches, profound fatigue, and explosive diarrhea.
Listeria is especially dangerous because the bacteria can cross the placental barrier, infecting the baby directly even if the mother feels only mildly ill. Salmonella and E. coli from undercooked meats or unwashed produce present similar dangers.
A normal pregnancy bowel upset will never cause a high fever. A fever over 100.4 F paired with diarrhea requires immediate emergency triage. If stool contains visible blood, heavy mucus, or is black and tarry, contact your OB-GYN immediately.
Ectopic Pregnancy vs. GI Upset
In very early pregnancy, ectopic pregnancy must be ruled out. An ectopic pregnancy occurs when the fertilized egg implants outside the uterine cavity, usually in a fallopian tube. This is a life-threatening emergency.
Telling the difference between ectopic pregnancy and GI upset can be tricky. Both cause abdominal pain. However, severe cramping and diarrhea in early pregnancy that is localized to one side of the pelvis is a major red flag. As the fallopian tube stretches, it leaks blood into the abdomen, irritating the bowels and causing sudden diarrhea.
GI upset causes generalized, dull cramps that improve after a bowel movement. Ectopic pain is sharp, stabbing, and one-sided. It often radiates to the shoulder tip because internal bleeding irritates the diaphragm. If you experience severe early-pregnancy cramping with shoulder pain or dizziness, go to the emergency room immediately.
Food Poisoning vs. Normal Pregnancy Diarrhea
Food poisoning strikes rapidly and violently, usually within two to six hours of eating contaminated food. Normal hormonal diarrhea is more gradual and less intense. Food poisoning is almost always accompanied by severe nausea, forceful vomiting, cold sweats, and cramps that do not stop.
If you suspect food poisoning, monitor your fluid intake carefully. The combination of vomiting and diarrhea will dehydrate you in hours. Never hesitate to seek urgent care if you cannot keep water down.
Signs of Dehydration During Pregnancy
Regardless of the cause, fluid loss is the primary danger of loose stools. Dehydration during pregnancy can escalate rapidly. When you lose water, blood volume drops, reducing the oxygenated blood flowing through the placenta to your baby.
Early warning signs include dark yellow urine, extreme thirst, dry mouth, and chapped lips. More severe signs include maternal tachycardia (a rapid, pounding heart rate) and dizziness when standing. Most importantly, watch for decreased fetal movement. If the baby is not kicking as much after a bout of stomach upset, your amniotic fluid levels may be dropping. Do not wait to see if it improves. Seek clinical evaluation right away.
Symptom Reference: When to Act
| Category | Normal Pregnancy Diarrhea | Potential Infection or Complication | Action Required |
| Stool | Loose, watery, normal color | Blood, heavy mucus, or black/tarry | Contact OB-GYN immediately |
| Pain | Mild cramps relieved by bowel movement | Severe, sharp, localized, does not subside | Seek ER evaluation |
| Temperature | Normal baseline | Fever over 100.4 F | Go to urgent care or triage |
| Duration | Resolves within 24-48 hours | Persistent beyond 48 hours | Schedule clinical consultation |
| Other Signs | Mild nausea, fatigue, food aversions | Dizziness, dark urine, decreased fetal movement | Immediate medical intervention |
Evidence-Based Treatment for Pregnancy Diarrhea
Once infections and preterm labor have been ruled out, the focus shifts to symptom management. You do not have to just suffer through it. There are safe, evidence-based steps to get your gut back on track. The goal is to slow intestinal transit, bulk up the stool, and replace lost fluids. We always start with dietary adjustments before considering medication.

The BRAT Diet and Nutritional Adjustments
The BRAT diet (Bananas, Rice, Applesauce, and Toast) is well-documented in medical literature and highly effective for managing diarrhea during pregnancy. These foods are bland, low in fat, and easy to digest. They are high in soluble fiber, which absorbs excess water in the colon and helps bulk up loose stools without irritating the intestinal lining.
Bananas are especially helpful because they are rich in potassium, a critical electrolyte lost during watery bowel movements. Applesauce contains pectin, a natural thickening agent that slows digestion. While on the BRAT diet, avoid fried foods, spicy meals, high-sugar snacks, and dairy. Stick to it for 24 to 48 hours until stools begin forming normally.
Safe Hydration Strategies
Replacing lost fluids is your single most important task. Plain water alone is not always enough. When you have loose stools, you lose sodium, potassium, and chloride. Medical-grade oral rehydration solutions (ORS) like Pedialyte contain the precise ratio of salt and sugar needed to pull water across the intestinal wall and into the bloodstream.
Avoid high-sugar sports drinks, as the heavy sugar content can worsen osmotic diarrhea by drawing more water into the colon. Also steer clear of caffeinated beverages. Caffeine acts as a diuretic and bowel stimulant, increasing urgency and worsening dehydration.
Medication Safety: Loperamide and What to Avoid
Sometimes diet and hydration are not enough. Current FDA and ACOG guidelines allow careful use of Loperamide (Imodium) after the first trimester. It works by slowing down rapid intestinal contractions. However, always consult your provider first, and use is typically limited to short 24-hour courses to prevent rebound constipation.
Medications containing Bismuth Subsalicylate (Pepto-Bismol) are strictly unsafe during pregnancy. Salicylates are chemically similar to aspirin and can increase maternal bleeding risks. They can also harm fetal circulation by prematurely closing the ductus arteriosus, a vital blood vessel in the baby’s heart that must remain open until birth.
Probiotics and Gut Health Restoration
Once acute symptoms resolve, rebuilding gut flora is a crucial step. Clinical trials show daily probiotic use reduces pregnancy-related GI upset by 25%. Look for third-party tested, pasteurized supplements with Lactobacillus and Bifidobacterium strains.
You can also get these from fermented foods like pasteurized yogurt, kefir, and mild sauerkraut. Just make sure any fermented food is fully pasteurized to avoid Listeria exposure.
Treatment Safety Reference
| Intervention | Safety Status | Clinical Notes |
| Oral Rehydration Salts | Highly Safe | Essential for replacing sodium, potassium, and fluids |
| BRAT Diet | Highly Safe | Binds loose stools naturally without harmful chemicals |
| Loperamide (Imodium) | Use with Caution | Generally safe after 1st trimester; requires doctor approval |
| Pepto-Bismol | UNSAFE | Contains salicylates; increases bleeding risk and harms fetal circulation |
| Probiotics | Generally Safe | Restores gut flora; choose pasteurized, third-party tested brands |
Summary and Key Takeaways
Pregnancy is a massive physical stress test for your entire body, and the gastrointestinal tract bears much of the burden. So, to answer the question definitively: is diarrhea a symptom of pregnancy? Yes. It is a common, biologically expected response to the incredible work your body is doing.
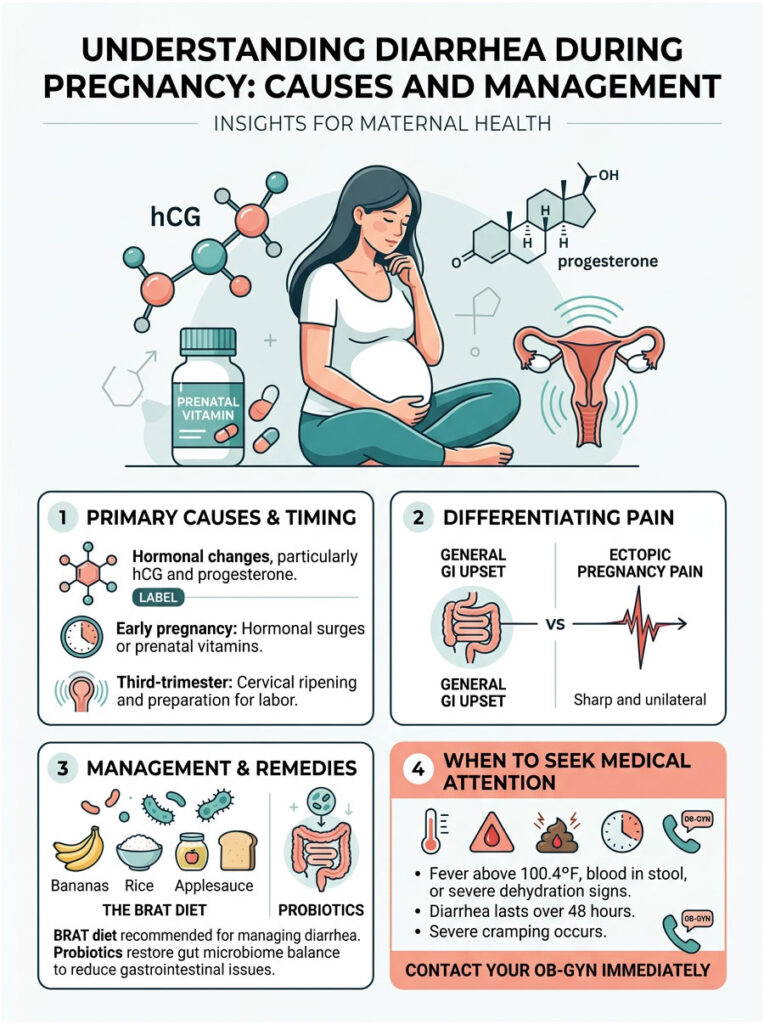
Early pregnancy diarrhea is usually a normal hormonal response to rising hCG and progesterone, or a reaction to a new prenatal vitamin. Third-trimester diarrhea is frequently a positive sign of cervical ripening, driven by prostaglandins preparing your body for labor.
You need immediate medical attention only under specific circumstances: a fever over 100.4 F, visible blood in the stool, or severe signs of dehydration. Your body is adapting and changing every single day. Stay hydrated, eat bland foods when your stomach is upset, and never hesitate to call your OB-GYN. We are always here to keep both you and your baby safe.
Frequently Asked Questions
Is diarrhea a symptom of pregnancy?
Yes, diarrhea is a common pregnancy symptom. As an OB-GYN, I frequently see patients experiencing loose stools due to the rapid hormonal surges of hCG and progesterone, which fundamentally alter gastrointestinal motility and the gut microbiome during gestation.
What causes diarrhea during pregnancy first trimester?
The primary triggers are the sudden spike in Human Chorionic Gonadotropin (hCG) and the muscle-relaxing effects of progesterone. These hormones can irritate the stomach lining and slow down or disrupt the rhythmic contractions of the intestines, leading to unpredictable bowel movements.
Is diarrhea in the third trimester a sign of labor?
It often is. As your body prepares for delivery, it releases prostaglandins to ripen the cervix. These hormone-like lipids also stimulate the smooth muscles of the bowels, causing them to empty—a natural process that clears space for the baby’s descent into the birth canal.
Why do prenatal vitamins cause loose stools?
Many prenatal vitamins contain high concentrations of iron and magnesium. These minerals can cause an osmotic shift, drawing excess water into the colon. If your body doesn’t absorb the minerals quickly enough, the resulting water influx leads to sudden osmotic diarrhea.
How can I tell the difference between ectopic pregnancy vs GI upset?
Gastrointestinal upset typically involves diffuse, dull cramping that improves after a bowel movement. In contrast, an ectopic pregnancy often causes sharp, stabbing, unilateral pelvic pain, sometimes radiating to the shoulder, and requires immediate emergency evaluation.
Can I safely take Imodium (Loperamide) while pregnant?
Loperamide is generally considered safe for short-term use after the first trimester, but you must consult your provider first. However, you should strictly avoid Bismuth Subsalicylate (Pepto-Bismol), as it can increase bleeding risks and potentially harm fetal circulation.
What are the specific Listeria symptoms in pregnancy?
Listeriosis often mimics a severe stomach bug or the flu, presenting with high fever, deep muscle aches, and explosive diarrhea. Because Listeria can cross the placental barrier, any fever over 100.4°F accompanied by GI distress needs immediate medical attention.
What are the most dangerous signs of dehydration risks during pregnancy?
You should watch for dark yellow urine, extreme thirst, maternal tachycardia (a pounding heart rate), and dizziness. Most importantly, if you notice decreased fetal movement following a bout of diarrhea, it may indicate a drop in amniotic fluid levels due to dehydration.
How do prostaglandins and bowel stimulation affect late pregnancy?
Prostaglandins are released to soften the cervix for labor, but they also act as powerful bowel stimulants. This often results in a ‘pre-labor flush’ 24 to 48 hours before active labor begins, helping the body clear the lower abdomen for the contracting uterus.
What is the recommended diet for managing pregnancy-related diarrhea?
I recommend the BRAT diet—Bananas, Rice, Applesauce, and Toast. These foods are high in soluble fiber and pectin, which help absorb excess water in the colon and provide essential electrolytes like potassium lost during loose stools.
Are probiotics safe for treating pregnancy-related gut issues?
Daily probiotic use is generally safe and can reduce gastrointestinal upset by up to 25% in expectant mothers. Strains like Lactobacillus help restore the gut microbiome, which naturally shifts during pregnancy to support fetal immune development.
When should I call my doctor about severe cramping and diarrhea in early pregnancy?
You should contact your OB-GYN immediately if the diarrhea lasts more than 48 hours, is accompanied by a fever over 100.4°F, contains blood or mucus, or if the cramping is localized to one side of the pelvis, which could indicate an ectopic pregnancy.
Disclaimer
This article is for informational purposes only and does not constitute medical advice. Pregnancy symptoms can vary significantly between individuals, and gastrointestinal distress can sometimes indicate serious complications. Always consult with your Board-Certified OB-GYN or a qualified healthcare professional before starting new supplements, taking medications like Loperamide, or making significant dietary changes during pregnancy.
References
- American College of Obstetricians and Gynecologists (ACOG) – https://www.acog.org – Clinical guidelines on managing gastrointestinal issues and OTC medication safety during pregnancy.
- Centers for Disease Control and Prevention (CDC) – https://www.cdc.gov/listeria – Official data regarding Listeria infection risks and food safety protocols for pregnant individuals.
- National Institutes of Health (NIH) – PubMed Central – 2022 study on the prevalence of bowel habit changes and the impact of progesterone on GI motility in the first trimester.
- Mayo Clinic – https://www.mayoclinic.org – Medical overview of dehydration risks, electrolyte imbalance, and the efficacy of the BRAT diet.
- Journal of Clinical Gastroenterology – Research paper on the shift of the gut microbiome during pregnancy and its effects on maternal digestion.
- Cleveland Clinic – Medical insights into the role of prostaglandins in cervical ripening and their secondary effect on bowel stimulation.







