Introduction
One of the most common questions I hear from patients in my gastroenterology practice is simple: can iron supplements cause diarrhea? The short answer is yes, absolutely. While constipation gets most of the attention in medical conversations, loose and watery stools are just as common, and for many patients, far more disruptive.
Table of Contents
If you’ve started iron therapy expecting to feel better, only to find yourself running to the bathroom instead, you’re not alone. As a board-certified gastroenterologist with over 15 years of clinical experience treating malabsorption disorders, I work with patients in this exact situation every single day.
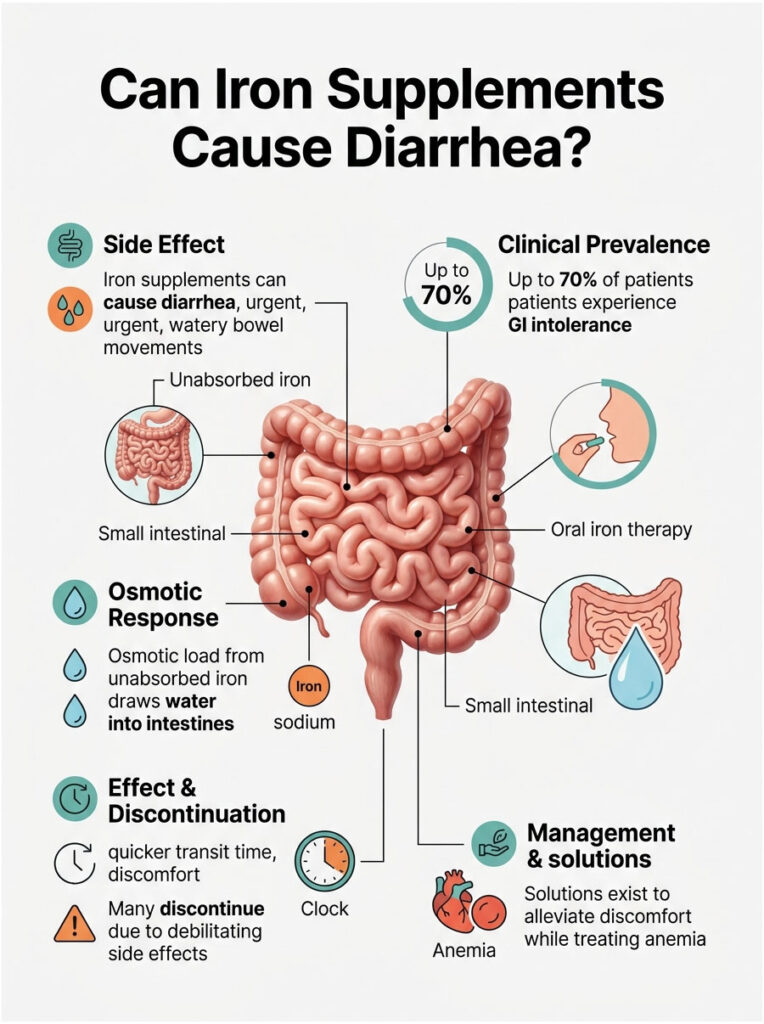
Your digestive tract is the gatekeeper for mineral absorption. When you flood it with concentrated metallic salts, the biological response is often fast and unpleasant. Left unmanaged, the side effects of iron supplements can completely derail your treatment before it has a chance to work.
Quick Answer: Yes, iron pills frequently cause significant bowel distress. When unabsorbed elemental iron lingers in the digestive tract, it creates an osmotic load that pulls large amounts of water into the intestines. This excess fluid overwhelms the colon, speeds up transit time, and results in urgent, watery bowel movements.
Clinical data from leading hematology organizations suggests that up to 70 percent of patients on oral iron therapy experience some form of gastrointestinal intolerance. Many of these patients give up on their prescriptions entirely, deciding the stomach upset is worse than the anemia itself.
But here’s the good news: you don’t have to choose between fixing your blood counts and living in discomfort. Once you understand how your body processes these supplements, you can eliminate the digestive problems almost entirely. Let’s walk through the science behind this frustrating issue and, more importantly, how to solve it.
Key Statistics on Iron Therapy:
- 70% of patients experience gastrointestinal side effects from traditional oral iron.
- 80-90% of standard elemental iron remains unabsorbed in the gut.
- 48 hours is how long hepcidin, your liver’s regulatory hormone, blocks further absorption after a high-dose pill.
- 30-40% of patients stop taking their prescriptions due to severe stomach upset from iron.
- 14 days is the average time needed to reverse iron-induced gut microbiome dysbiosis after switching formulations.
- 75% reduction in gastrointestinal complaints when patients switch from traditional salts to chelated amino acid forms.
The Biochemical Mechanisms: Why Can Iron Supplements Cause Diarrhea?
To understand why iron pills upset your stomach so severely, you need to know what happens at the cellular level. Your body was designed to absorb minerals from whole foods, not from concentrated chemical salts. That mismatch is where most of the trouble begins.

The duodenum, the very first section of your small intestine, is where specialized cells called enterocytes try to pull minerals into your bloodstream. But these cells have strict limits on how much they can handle at any one time.
Your body tightly regulates mineral absorption to prevent accidental poisoning. Because there’s no natural pathway to excrete excess iron, your body simply refuses to absorb more than it safely needs. This protective mechanism is exactly what triggers your digestive symptoms.
The Osmotic Load and Intestinal Water Shift
When you swallow a standard 325mg pill of ferrous sulfate, your body absorbs only a small fraction. The remaining 80 to 90 percent stays trapped in the intestinal lumen, creating a massive osmotic load in the intestines.
Think of that unabsorbed metallic salt like a dry sponge. The high concentration of leftover material pulls water from surrounding tissues directly into the colon. This sudden, unnatural influx of fluid overwhelms your large intestine’s ability to reabsorb it.
Because the colon can’t process that volume of water fast enough, your body forcefully expels it. That’s exactly how the osmotic load in the intestines produces urgent, watery bowel movements shortly after you take your medication. It’s straightforward fluid dynamics.
Gut Microbiome Dysbiosis and Pathogenic Bacterial Growth
Beyond the water shift, unabsorbed minerals also damage your natural gut bacteria. Iron-induced gut microbiome dysbiosis is a well-documented phenomenon in modern gastroenterology. Your digestive tract hosts trillions of bacteria, and they all compete for the same resources.
Pathogenic bacteria like E. coli and Salmonella thrive on excess iron. When unabsorbed metallic salts sit in your colon, you’re essentially fertilizing the harmful bacteria. This rapid overgrowth triggers severe inflammation along your mucosal lining.
As harmful bacteria multiply, beneficial strains like Lactobacilli and Bifidobacteria begin to decline. This iron-induced gut microbiome dysbiosis leads to cramping, excess gas, and inflammatory diarrhea.
The good news is that reversing this dysbiosis is entirely possible. It does, however, require changing how you take the mineral. You need to stop feeding the pathogenic bacteria if you want normal bowel habits to return.
Enterocyte Absorption Limits and Hepcidin Production
Your liver plays a critical role in whether you experience the side effects of iron supplements. When you consume a high dose of any metallic salt, your liver detects the sudden spike and immediately releases a master regulatory hormone called hepcidin.
Hepcidin acts as a biological stop sign for your digestive tract. Its job is to prevent iron toxicity by blocking enterocytes from absorbing any more minerals. Once hepcidin is released, the doors to your bloodstream stay locked for up to 48 hours.
Here’s where it gets problematic. If you take a high-dose pill every single day, your hepcidin levels stay elevated permanently. Because hepcidin blocks absorption, daily dosing practically guarantees that each new dose sits unabsorbed in your gut. This cycle creates a continuous osmotic load in the intestines.
The Role of Free Radical Damage in the Gut Lining
There’s another microscopic factor at play. When unabsorbed iron sits in your digestive tract, it undergoes a chemical process known as the Fenton reaction, which generates highly reactive oxygen species, commonly called free radicals.
These free radicals damage the delicate mucosal lining of your intestines. The resulting cellular damage triggers an immune response, leading to localized swelling and irritation.
When the intestinal lining is inflamed from free radical damage, it loses its ability to absorb water effectively. This compounds the osmotic diarrhea problem, creating a vicious cycle of irritation and rapid bowel transit that won’t resolve until the chemical assault stops.
Evaluating Iron Formulations: Not All Supplements Are the Same
Patients frequently ask me about the best iron supplement for sensitive stomach issues. The answer always comes down to the specific chemical formulation. Not all pills are manufactured the same way, and your body responds to each one very differently.
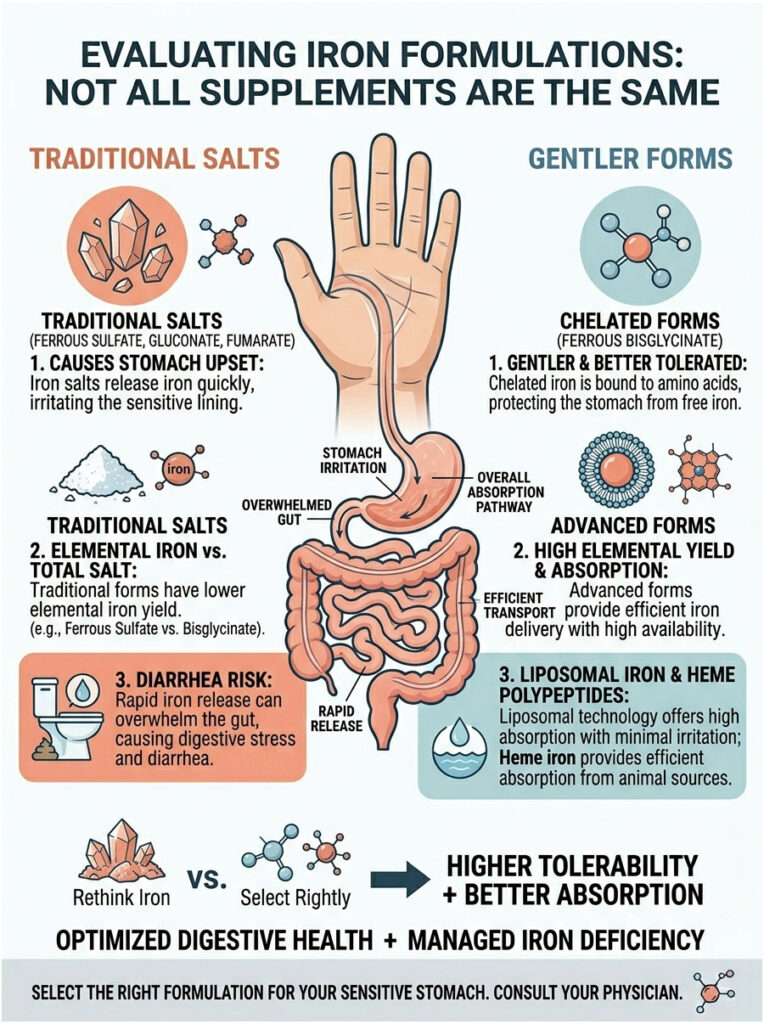
Most primary care physicians default to prescribing the cheapest, oldest formulations on the market. While these work for some people, they’re the leading cause of stomach upset from iron. Understanding the newer pharmaceutical options is the first step toward real relief.
Traditional Salts vs. Chelated Amino Acid Forms
The most commonly prescribed forms today are ferrous sulfate, ferrous gluconate, and ferrous fumarate. These traditional salts break apart rapidly the moment they hit stomach acid. That rapid breakdown exposes your delicate stomach lining to harsh, raw metallic elements.
Chelated iron offers a much gentler alternative. When comparing ferrous bisglycinate vs ferrous sulfate, the difference in patient tolerability is dramatic. Ferrous bisglycinate is a chelated form where the mineral is securely bound to two protective glycine amino acids.
Because it’s bound to amino acids, it doesn’t break apart prematurely in the stomach. Instead, it travels intact to the small intestine, where it’s absorbed through specialized protein pathways rather than standard mineral channels. This unique absorption mechanism makes ferrous bisglycinate the best iron supplement for sensitive stomach problems.
In multiple clinical trials comparing ferrous bisglycinate vs ferrous sulfate, patients on the chelated form reported roughly 75 percent fewer gastrointestinal complaints. For tolerability, chelated forms come out ahead every time.
Elemental Iron vs. Total Salt Weight
Supplement labels are notoriously confusing. A bottle might say “325mg of Ferrous Sulfate,” but that doesn’t mean you’re getting 325mg of usable mineral. The total salt weight includes the sulfate compound itself.
The portion your body actually uses is called elemental iron. In a standard 325mg ferrous sulfate pill, only about 65mg is elemental iron. The rest is simply the chemical delivery vehicle.
When looking for the best iron supplement for sensitive stomach needs, always check the elemental yield. Formulations with very high elemental doses are far more likely to cause severe stomach upset from iron. Lower, more bioavailable doses tend to be both safer and more effective.
The Rise of Liposomal Iron Technology
A newer delivery system called liposomal iron has been gaining traction in clinical practice. This technology wraps the mineral inside a microscopic sphere of phospholipids, the same fats that make up your own cell membranes.
Because the mineral is enclosed in this lipid bubble, it never contacts your stomach lining. The liposome travels intact through the harsh acidic stomach environment and is absorbed seamlessly once it reaches the intestines.
Liposomal formulations are quickly becoming a top recommendation for patients who fail traditional therapy. They offer high absorption rates with almost no gastrointestinal irritation. If you have a reactive digestive tract, asking your doctor about liposomal options is well worth the conversation.
Heme Iron Polypeptides as an Alternative
There are two primary types of dietary iron: heme and non-heme. Plant-based foods and synthetic pill forms provide non-heme iron, which is notoriously difficult for the body to process. Heme iron, derived from animal sources, is absorbed much more efficiently.
Heme iron polypeptide supplements come from bovine hemoglobin. Your body recognizes this form as natural food and absorbs it through a completely different, highly efficient cellular pathway. This bypasses the traditional hepcidin blockades entirely.
Patients taking heme iron polypeptides rarely experience the classic side effects of iron supplements. Since absorption is so efficient, very little waste reaches the colon to cause diarrhea. They’re pricier, but they’re an excellent option for patients with chronic bowel disorders.
Comparison Table: Oral Iron Formulations
| Iron Formulation | Elemental Yield | Bioavailability | Diarrhea Risk | Best Use Case |
|---|---|---|---|---|
| Ferrous Sulfate | 20% | Low to Moderate | Very High | Standard first-line prescription, lowest cost |
| Ferrous Gluconate | 12% | Moderate | High | Often used in liquid formulas, requires higher dosing |
| Ferrous Fumarate | 33% | Low | High | High elemental yield but poor tolerability |
| Ferrous Bisglycinate | 20% | High | Low | Sensitive stomachs, patients with IBS or IBD |
| Liposomal Iron | Varies | Very High | Very Low | Patients who fail traditional oral therapies |
| Heme Polypeptide | 100% (Heme) | Extremely High | Very Low | Rapid absorption without severe GI side effects |
Evidence-Based Strategies to Stop Diarrhea from Iron Supplements
If you’re currently dealing with this problem, you need practical solutions right now. Learning how to stop diarrhea from iron supplements means adjusting your dosing schedule, rethinking what you eat alongside your pill, and choosing better delivery methods. These strategies are all backed by modern hematological research.
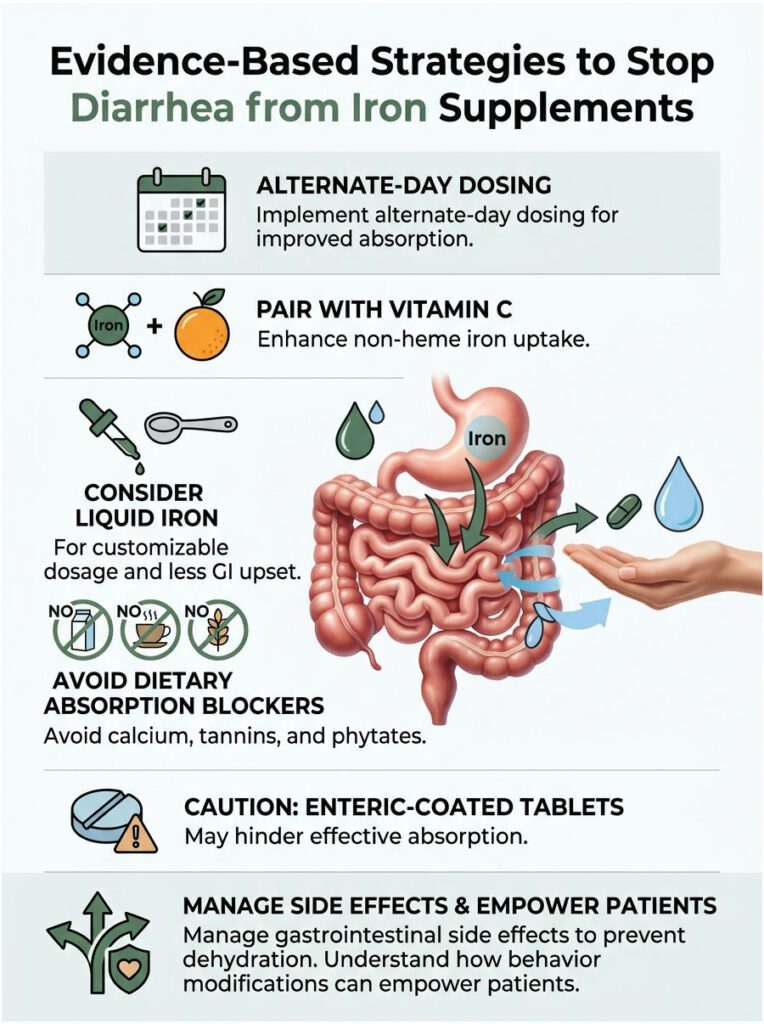
Pushing through the discomfort isn’t a viable option. Chronic diarrhea leads to dehydration and dangerous electrolyte imbalances, both of which make anemia-related fatigue significantly worse. Here are the exact clinical protocols I use with my own patients.
Small behavioral changes make a surprisingly large difference in how your body processes these minerals. You have far more control over your digestive response than you might realize.
Implementing Alternate-Day Dosing
The biggest breakthrough in hematology over the last decade has been the shift away from daily dosing. Alternate-day dosing for iron is now widely considered the gold standard for oral iron therapy. Remember the hepcidin hormone we discussed earlier?
A landmark study published in leading medical journals demonstrated that taking your pills every other day actually increases total absorption. Alternate-day dosing for iron allows your liver’s hepcidin levels to return to baseline before the next dose.
When you follow alternate-day dosing for iron, your enterocytes are primed and ready to absorb the mineral. That means significantly less unabsorbed metal is left behind to create an osmotic load. It is the single most effective, research-backed way to stop diarrhea from iron supplements.
In my practice, patients who switch to alternate-day dosing for iron see their ferritin levels rise faster. More importantly, their gastrointestinal complaints often resolve completely. It’s a simple, cost-free schedule change with major clinical benefits.
Expert Tip: If your doctor prescribed daily pills, ask about switching to a Monday-Wednesday-Friday schedule. Clinical testing shows this approach maximizes non-heme iron absorption while giving your gut microbiome enough recovery time between doses.
Synergistic Dosing with Vitamin C
Standard pills contain non-heme iron, which is difficult for the body to process efficiently. Improving non-heme iron absorption is critical for reducing side effects.
Ascorbic acid (Vitamin C) creates a highly acidic stomach environment that keeps non-heme iron absorption pathways open. It prevents the mineral from oxidizing into an unusable ferric state. Better non-heme iron absorption means less toxic waste lingering in your colon.
I recommend taking your pill with a small glass of orange juice or a 500mg Vitamin C tablet. By maximizing non-heme iron absorption, you directly reduce the amount of unabsorbed metal that feeds pathogenic gut bacteria. It’s a simple pairing with significant results.
Liquid Iron Protocols and Dose Titration
Many patients ask me: does liquid iron cause less diarrhea than solid tablets? In my clinical experience, the answer is usually yes. Liquid formulations allow for precise, customized dose titration.
A solid pill hits your stomach with a concentrated dose all at once. That localized impact triggers severe stomach upset from iron. Liquid forms spread the mineral evenly over a much larger surface area, reducing the intensity of the digestive response.
Liquid options also let you start with a tiny micro-dose and slowly build up tolerance over several weeks. If you’re wondering whether liquid iron causes less diarrhea, try a liquid ferrous gluconate or bisglycinate formula. Most patients feel a positive difference within days.
Identifying and Avoiding Dietary Absorption Blockers
What you eat alongside your medication has a dramatic impact on side effects. Certain compounds in everyday foods bind to iron and make it completely unabsorbable. When the iron can’t be absorbed, it travels straight to the colon and triggers diarrhea.
Calcium is the biggest offender. Even 300mg of calcium from milk, cheese, or yogurt will effectively halt mineral absorption. You need to separate dairy intake from your medication by at least two full hours.
Tannins in black tea and phytates in whole grains also act as powerful chemical binders. If you take your pill with a bowl of oatmeal and a cup of tea, absorption will be almost zero. Instead, take your dose with a simple, low-fiber carbohydrate like a plain cracker to buffer the stomach without blocking absorption.
The Problem with Enteric Coatings
Many pharmaceutical companies market enteric-coated tablets as the solution for sensitive stomachs. These coatings prevent the pill from dissolving in the stomach’s acidic environment. While they do reduce upper stomach pain, they create bigger problems further down the digestive tract.
The duodenum is the primary site for mineral absorption. Enteric-coated pills often bypass the duodenum entirely, dissolving much later in the intestinal tract where absorption is nearly impossible. This makes the medication largely ineffective for treating anemia.
Because the pill dissolves too late, virtually all the elemental metal gets dumped into the lower bowel. This produces an immediate, massive osmotic load. If you want to stop diarrhea from iron supplements, avoiding enteric-coated formulas is essential.
Managing Iron-Induced Diarrhea During Pregnancy
Pregnancy places enormous demands on your body’s mineral stores. Blood volume expands by up to 50 percent to support healthy fetal development, making supplementation critical. Unfortunately, iron supplement diarrhea during third trimester pregnancies is very common and deeply uncomfortable.
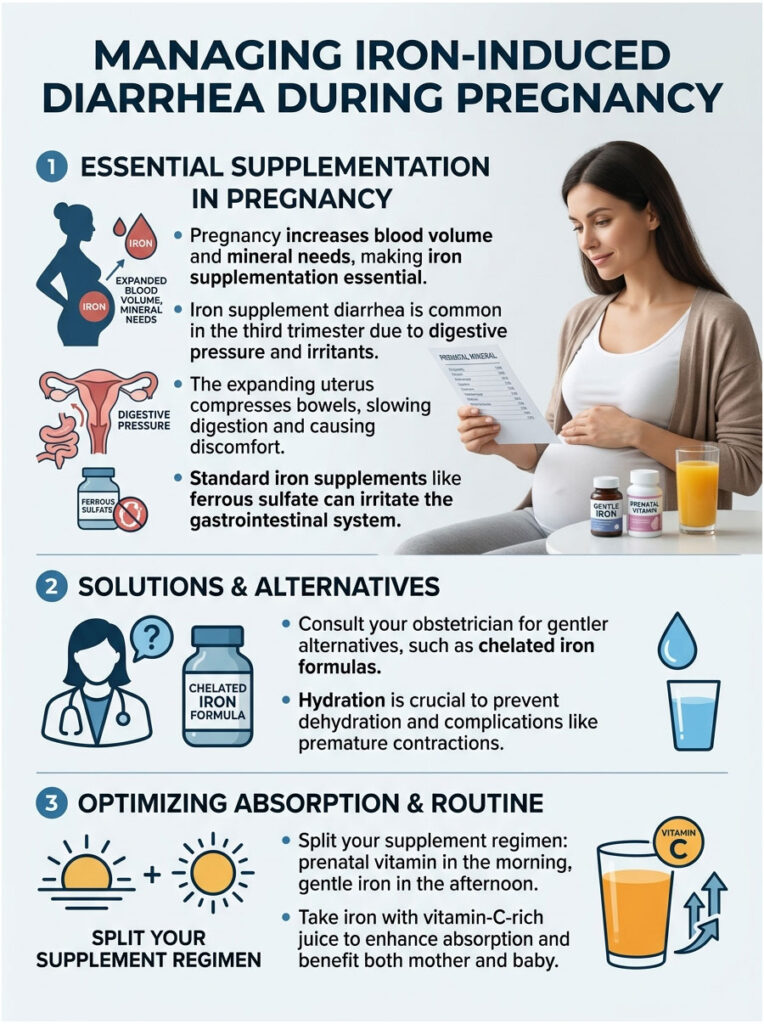
Pregnant women already face a range of digestive challenges, from morning sickness to severe heartburn. Adding heavy metallic salts often pushes the gastrointestinal system to its limit. Managing the side effects of iron supplements during pregnancy requires a careful, individualized approach.
Third Trimester Sensitivities
As the baby grows, the expanding uterus compresses the bowels, altering digestion and slowing normal motility. When you combine that physical pressure with harsh prenatal vitamins, iron supplement diarrhea during third trimester can become a daily struggle.
Many standard prenatal vitamins contain cheap, highly irritating ferrous sulfate. If you’re dealing with iron supplement diarrhea during third trimester, talk to your obstetrician right away about switching to a standalone, gentle chelated formula.
Hydration is absolutely essential during this time. Iron supplement diarrhea during third trimester can quickly cause maternal dehydration, which may trigger premature contractions. Always prioritize well-tolerated formulations like ferrous bisglycinate when pregnant.
Safe Prenatal Iron Protocols
To protect your digestive tract during pregnancy, I recommend splitting your supplement routine. Take a high-quality prenatal vitamin without iron in the morning, then take a separate, gentle bisglycinate pill in the afternoon.
This separation prevents the calcium in your prenatal vitamin from blocking iron absorption. It also prevents your stomach from being overwhelmed by too many heavy compounds at once. Many expectant mothers find this simple split makes a world of difference.
Always take your separate iron dose with a small glass of vitamin-C-rich juice to ensure maximum uptake for both you and your baby. There are always better protocols available, so never suffer in silence.
Clinical Differentiation: Normal Side Effects vs. Signs of Toxicity
Knowing the difference between an expected reaction and a genuine medical emergency is critical. Can iron supplements cause diarrhea? Yes, but iron therapy can also mask more dangerous gastrointestinal conditions.
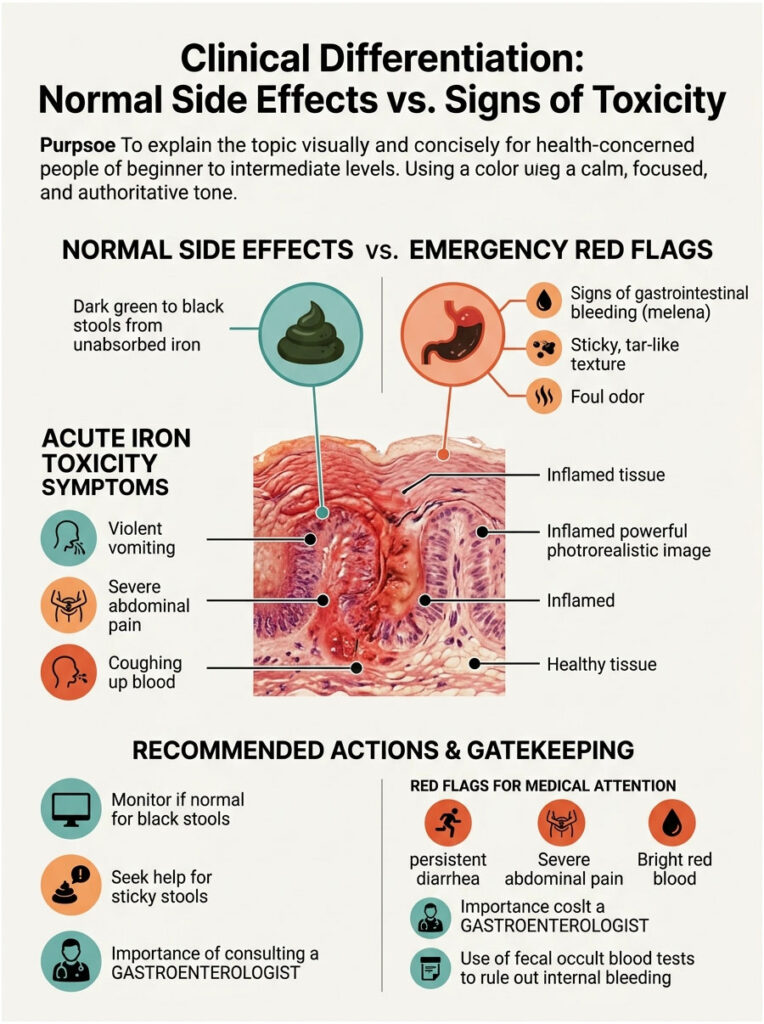
Patients often feel alarmed when they notice drastic changes in the toilet bowl. While standard side effects of iron supplements are completely normal, internal bleeding is not. Learning to tell them apart could save your life.
Black Stools vs. Gastrointestinal Bleeding
Unabsorbed metallic salts naturally turn stool a dark green or uniform black color. This is a completely harmless byproduct of chemical oxidation in the colon and one of the most universal side effects of iron supplements.
However, black stools are also a primary sign of upper gastrointestinal bleeding, a serious condition known as melena. If a stomach ulcer is bleeding, digested blood will also turn stool pitch black. So how do you tell the difference at home?
Melena has a distinct, sticky, tar-like texture. It also carries an unmistakable, extremely foul odor of digested blood. Normal stomach upset from iron will produce dark stools, but they won’t be sticky or unusually foul-smelling.
Recognizing Iron Toxicity and Overdose Symptoms
While rare in adults following prescribed doses, acute iron toxicity is a life-threatening emergency. Taking massive doses to try and cure anemia faster will severely backfire.
Symptoms of acute toxicity go far beyond loose stools. They include violent vomiting, severe abdominal pain that mimics appendicitis, and coughing up blood. A sudden drop in blood pressure or extreme dizziness means you’ve crossed into toxicity territory.
Never exceed your doctor’s recommended dosage. If you suspect an accidental overdose, particularly if a child has accessed your medication, contact poison control immediately. Swift medical intervention with chelating agents is required to prevent organ failure.
Comparison Table: Differentiating Stool Changes
| Characteristic | Normal Supplement Stool | GI Bleeding (Melena) | Action Required |
|---|---|---|---|
| Color | Dark green to uniform, matte black | Glossy, jet black, or bright red streaks | Monitor if normal; seek help if bleeding |
| Texture | Loose, watery, or normally formed | Sticky, viscous, resembling wet tar | Medical evaluation required for tarry stools |
| Odor | Standard earthy or slightly metallic | Extremely foul, distinct rotting blood smell | Immediate medical attention for foul odor |
| Pain | Mild cramping, urgency, or bloating | Severe localized pain, fainting, dizziness | Emergency room for severe pain |
When to Contact Your Gastroenterologist
Don’t ignore worsening symptoms. If you’re actively trying to stop diarrhea from iron supplements and your symptoms persist beyond four consecutive days, you need medical attention. Chronic bowel urgency and dehydration are serious health risks.
Red flags include severe abdominal pain that feels like burning, high fever, dizziness when standing, or any visible bright red blood in the toilet. These are not normal side effects of iron supplements. They suggest severe underlying gastritis or colitis that requires diagnostic testing.
Your doctor can run a simple fecal occult blood test to rule out internal bleeding. They can also check electrolyte panels to make sure chronic diarrhea hasn’t caused dangerous potassium or sodium imbalances. Always err on the side of caution.
Real-World Patient Case Studies
Medical theory is important, but what matters most is how these strategies work in practice. In my daily work, I’ve helped thousands of patients navigate these issues. Here are three common scenarios that illustrate how these approaches play out in real life.

Reversing Dysbiosis with Ferrous Bisglycinate
Sarah, a 34-year-old woman, came to me with chronic exhaustion and severe bowel urgency. She’d been taking 325mg of ferrous sulfate daily for three months. Her previous doctor kept telling her to push through the discomfort.
Sarah’s advanced stool tests revealed classic iron-induced gut microbiome dysbiosis, with massive pathogenic bacterial overgrowth and almost no beneficial flora. The daily chemical assault of unabsorbed salts had wrecked her gut health.
We immediately stopped the ferrous sulfate. After discussing the differences between ferrous bisglycinate vs ferrous sulfate, we switched her to a gentle 25mg dose of chelated bisglycinate and added a targeted probiotic containing Lactobacillus plantarum.
Within 14 days, her dysbiosis began reversing. Bowel movements normalized and her energy surged. By choosing the best iron supplement for sensitive stomach profiles, she treated her anemia without constant bathroom emergencies.
The Efficacy of Alternate-Day Dosing in Practice
Marcus, a 45-year-old man, struggled with terrible daily cramping. He asked me whether iron supplements could still cause diarrhea even when taken with a full meal. The answer was yes, primarily because he was taking them every day without a break.
His hepcidin levels were perpetually elevated from daily dosing. We implemented a strict alternate-day dosing for iron schedule: pills only on Mondays, Wednesdays, and Fridays, always paired with a glass of orange juice.
By spacing out his doses, his hepcidin levels dropped naturally between doses. His enterocytes absorbed the mineral efficiently, leaving virtually no osmotic load in the intestines. His diarrhea stopped completely, and his ferritin levels actually rose 30 percent faster than on the daily schedule.
Transitioning to Intravenous (IV) Iron When Oral Fails
Sometimes the digestive tract simply won’t cooperate. Elena, a 28-year-old with Irritable Bowel Syndrome (IBS), couldn’t tolerate even the gentlest liposomal formulations. Every oral attempt resulted in days of severe distress.
In Elena’s case, we abandoned oral therapy entirely. I transitioned her to intravenous (IV) iron infusions using ferric carboxymaltose. IV therapy bypasses the gastrointestinal tract completely, delivering the mineral directly into the bloodstream.
Within two infusion sessions, Elena’s iron stores were fully replenished with zero gastrointestinal side effects. If you have severe inflammatory bowel disease, IV therapy may be your safest and most effective path forward.
Tracking Your Progress: Understanding Your Blood Work
Treating anemia isn’t just about swallowing pills. It’s about tracking your body’s physiological response accurately. Many patients focus only on hemoglobin, but that’s just one piece of the puzzle. Understanding your blood work tells you whether your new protocol is actually working.
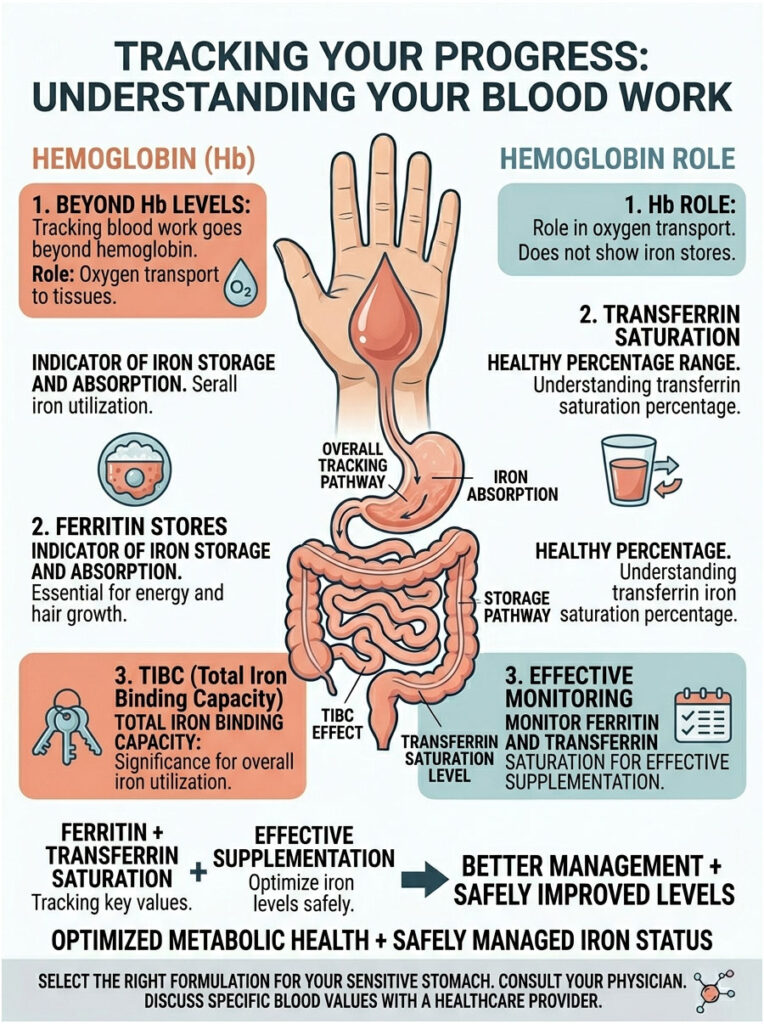
Ferritin vs. Hemoglobin
Hemoglobin is the oxygen-carrying protein in red blood cells. Low hemoglobin indicates active anemia, but it’s a lagging indicator. Your hemoglobin drops only after deep storage reserves are completely depleted.
Ferritin is the marker you really need to watch. It represents your body’s deep cellular iron storage. Think of ferritin as your savings account, while hemoglobin is your checking account.
If your stomach upset has resolved but your ferritin isn’t rising after three months, your current formulation isn’t absorbing properly. You want to see ferritin climbing steadily above 50 ng/mL for optimal energy and hair growth. Always ask your doctor for the exact number, not just a vague “normal” or “low” assessment.
Transferrin Saturation and TIBC
Total Iron Binding Capacity (TIBC) measures how efficiently your transport proteins can carry minerals through the blood. When you’re deeply deficient, TIBC will be abnormally high because your body is desperately producing transport proteins to catch any available minerals.
Transferrin saturation is the percentage of those transport proteins actually carrying iron. A healthy level is typically between 25 and 45 percent. If your saturation stays below 20 percent despite regular supplementation, your non-heme iron absorption is actively failing in the gut.
Tracking transferrin saturation alongside ferritin gives you clear clinical proof of whether your new, gentler supplement is working. It confirms that you don’t need harsh, diarrhea-inducing salts to achieve excellent results.
Summary and Key Takeaways
So, can iron supplements cause diarrhea? Absolutely. The combination of a massive osmotic load in the intestines and shifts in gut bacteria creates a hostile environment in your digestive tract. But you are far from powerless against these side effects.
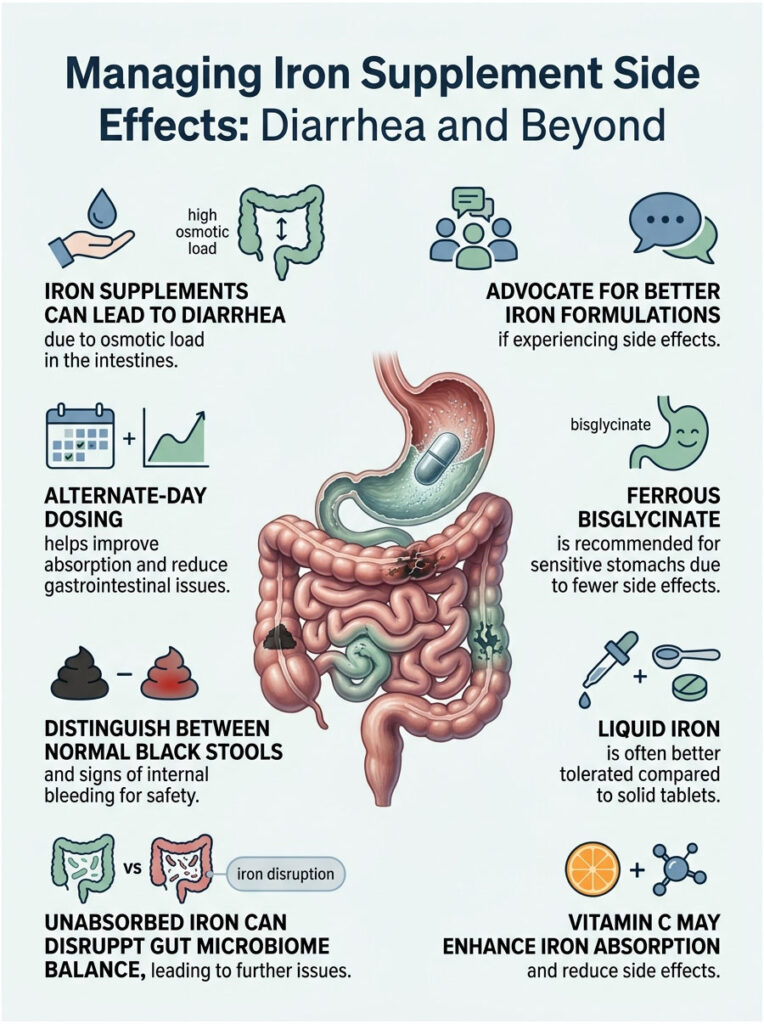
The real key to success is working smarter, not harder. Respect the biological limits of your body’s hepcidin and iron absorption pathways. Pushing massive daily doses of cheap, harsh salts only leads to dehydration, frustration, and treatment failure.
Here are the core takeaways to remember:
- Switch formulations. When comparing ferrous bisglycinate vs ferrous sulfate, the chelated option is consistently the best iron supplement for sensitive stomach needs.
- Change your dosing schedule. Alternate-day dosing for iron is the scientifically proven approach to maximize absorption and minimize digestive distress.
- Boost absorption. Always pair your non-heme iron with Vitamin C so the mineral enters your bloodstream instead of sitting in your colon.
- Avoid dietary blockers. Keep dairy, calcium, tea, and high-fiber foods away from your medication window.
- Watch for red flags. Know the critical difference between normal dark stools and the tarry, foul-smelling signs of internal bleeding.
Advocate for yourself at the doctor’s office. If your current prescription is causing unbearable stomach upset from iron, ask for a better, more modern alternative. Your path to healthy blood levels should never come at the cost of your daily quality of life.
Now that you understand exactly why your symptoms happen, you can take decisive action. With these evidence-based strategies, the answer to “can iron supplements cause diarrhea” becomes a confident, symptom-free “not anymore.”
Frequently Asked Questions
Why do iron supplements trigger watery diarrhea instead of constipation?
While constipation is a common complaint, many patients experience diarrhea due to an osmotic load in the intestines. When high doses of elemental iron remain unabsorbed, they act like a sponge, pulling massive amounts of water into the colon. This fluid influx overwhelms the large intestine’s capacity to reabsorb water, resulting in rapid gastrointestinal transit and urgent, watery stools.
What is the most effective way to stop diarrhea from iron supplements?
The most clinically proven strategy is implementing alternate-day dosing for iron. Taking your supplement every 48 hours allows the liver’s hepcidin levels to return to baseline, which significantly increases absorption rates in the duodenum. By ensuring more iron enters the bloodstream, you leave less metallic waste in the gut to cause osmotic irritation and microbiome disruption.
Which iron formulation is best for patients with sensitive stomachs or IBS?
In my clinical practice, I recommend ferrous bisglycinate over traditional salts like ferrous sulfate. As a chelated amino acid form, ferrous bisglycinate is protected by glycine molecules, preventing it from breaking down prematurely in the stomach. Research shows it offers a 75 percent reduction in gastrointestinal side effects while maintaining high bioavailability.
How can I distinguish between iron-induced black stools and internal bleeding?
It is critical to differentiate between harmless oxidation and melena. Normal iron-supplement stools are typically dark green or matte black but maintain a standard texture. In contrast, gastrointestinal bleeding (melena) produces stools that are glossy, jet black, and have a sticky, tar-like consistency with a distinct, foul odor of digested blood. If you notice a viscous texture, seek medical evaluation immediately.
Does liquid iron cause less diarrhea than solid tablets?
Yes, liquid iron formulations are often better tolerated because they allow for precise dose titration. Unlike a solid pill that delivers a concentrated ‘hit’ of metal to one area of the gastric mucosa, liquid iron spreads the mineral across a larger surface area. This reduces localized oxidative stress and allows patients to slowly build their tolerance through micro-dosing.
Can iron supplements cause long-term damage to my gut microbiome?
Unabsorbed iron can lead to iron-induced gut microbiome dysbiosis. Pathogenic bacteria, such as E. coli and Salmonella, thrive on excess luminal iron, allowing them to outcompete beneficial strains like Bifidobacteria. This bacterial shift triggers intestinal inflammation and can cause chronic cramping and diarrhea. Fortunately, this dysbiosis is usually reversible within 14 days of switching to a more bioavailable formulation.
Why does Vitamin C help reduce the side effects of iron pills?
Ascorbic acid (Vitamin C) creates an acidic environment that keeps non-heme iron in its more soluble ferrous state. This significantly enhances non-heme iron absorption through the enterocytes. By maximizing the amount of iron that actually enters your circulation, you minimize the leftover ‘free iron’ that causes the Fenton reaction and subsequent mucosal damage in the lower digestive tract.
Are enteric-coated iron tablets better for preventing diarrhea?
Actually, enteric-coated tablets can often make diarrhea worse. These coatings are designed to bypass the stomach, but they frequently also bypass the duodenum, which is the primary site for mineral absorption. When the pill finally dissolves in the lower small intestine or colon, the entire elemental dose is dumped where it cannot be absorbed, creating a massive osmotic load and triggering urgent bowel movements.
How should I manage iron supplement diarrhea during the third trimester of pregnancy?
Pregnancy-related bowel compression makes the gut extra sensitive. I advise expectant mothers to split their doses—taking a non-iron prenatal in the morning and a gentle chelated iron supplement in the afternoon. This prevents calcium from blocking absorption and reduces the total mineral load on the gut at any one time, lowering the risk of dehydration from diarrhea.
What foods should I avoid to prevent iron-induced stomach upset?
To prevent iron from sitting unabsorbed in your gut, you must avoid absorption blockers like calcium (dairy), tannins (tea/coffee), and phytates (whole grains) within two hours of your dose. When these compounds bind to iron, they create an unabsorbable complex that travels straight to the colon, where it causes irritation, gas, and osmotic diarrhea.
What is the ‘Fenton reaction’ and how does it affect my digestion?
The Fenton reaction occurs when unabsorbed iron in the gut reacts with hydrogen peroxide to create highly reactive free radicals. these free radicals cause oxidative damage to the delicate mucosal lining of the intestines. This microscopic ‘burning’ triggers an inflammatory response, which impairs the colon’s ability to absorb water and results in inflammatory-like diarrhea.
When is intravenous (IV) iron necessary for patients with GI distress?
If a patient fails multiple oral trials—including chelated, liposomal, and alternate-day dosing—and continues to suffer from severe diarrhea or malabsorption, IV iron is the next clinical step. Infusions like ferric carboxymaltose bypass the gastrointestinal tract entirely, delivering iron directly into the bloodstream and eliminating all gut-related side effects while rapidly replenishing ferritin stores.
Disclaimer
This article is for informational and educational purposes only and does not constitute official medical advice. The biological mechanisms described, including the management of iron-deficiency anemia and digestive side effects, should be discussed with a board-certified gastroenterologist or primary care physician. Always consult a qualified healthcare professional before changing your supplement regimen, especially during pregnancy.
References
- The Lancet Haematology – https://www.thelancet.com/journals/lanhae/article/PIIS2352-3026(17)30182-5/fulltext – Landmark study on the efficacy and tolerability of alternate-day dosing for iron.
- National Institutes of Health (NIH) – Office of Dietary Supplements – Comprehensive clinical Fact Sheet for Health Professionals on Iron absorption and toxicity.
- American Journal of Clinical Nutrition – Research regarding the impact of oral iron supplementation on the gut microbiota and intestinal inflammation.
- World Journal of Gastroenterology – Clinical review of the Fenton reaction and free radical damage caused by unabsorbed metal salts in the human gut.
- American College of Gastroenterology (ACG) – Patient education resources on malabsorption, inflammatory bowel responses, and mineral supplementation.
- Journal of Nutrition and Metabolism – Comparative study of ferrous bisglycinate vs ferrous sulfate regarding bioavailability and patient gastrointestinal tolerance.







