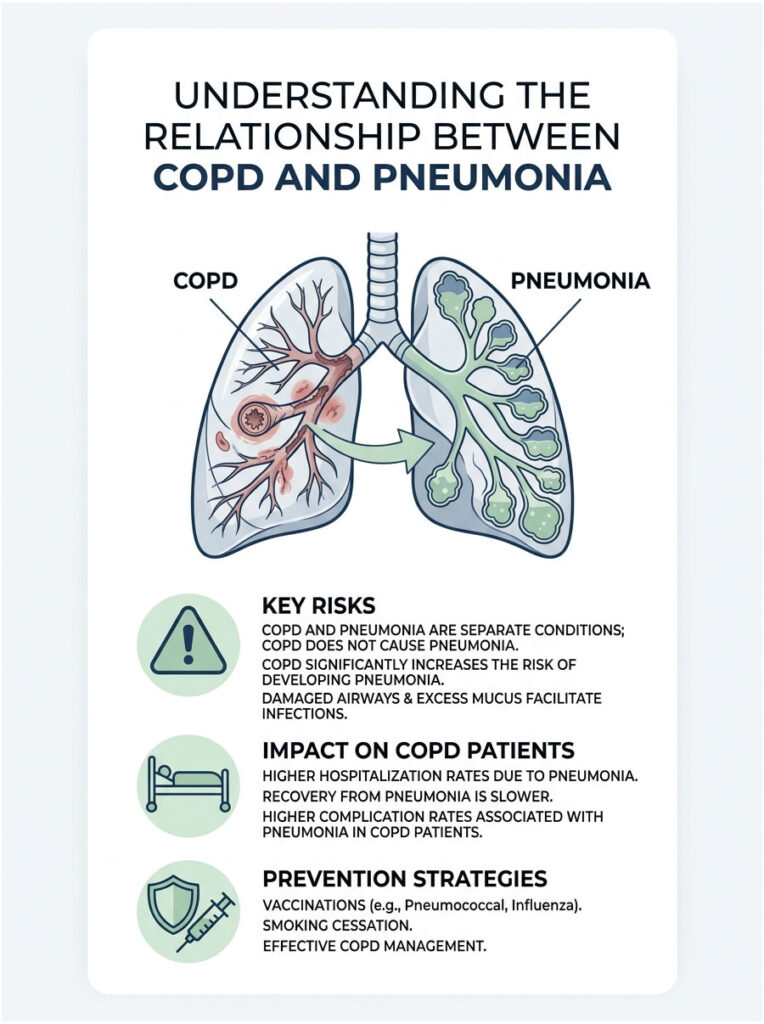
Here is something most people get backward: COPD does not turn into pneumonia, and it never will. They are two separate conditions. Yet if you live with COPD, a routine chest infection that a healthy neighbor would shake off in a week can put you in a hospital bed. The link is real, it is measurable, and the good news is that much of the added risk is something you can act on.
Table of Contents
Quick Answer: COPD does not cause pneumonia, but it sharply raises the risk of getting it and of getting a severe case. Damaged airways, excess mucus, and weakened lung defenses make it easier for infection to take hold. People with COPD who develop pneumonia often need hospitalization, recover more slowly, and face higher complication rates. Vaccines, quitting smoking, and good COPD control are the strongest ways to lower that risk.
At a Glance
- COPD and pneumonia are different conditions, but COPD makes pneumonia far more likely and more dangerous.
- Adults 65 and older with COPD face a much higher risk of pneumococcal pneumonia than healthy peers.
- A COPD flare-up and pneumonia share symptoms, which can delay treatment if the two are confused.
- Pneumonia in a COPD patient often means hospitalization, slower recovery, and a risk of respiratory failure.
- Pneumococcal, flu, COVID-19, and RSV vaccines are central to prevention.
- Sudden, severe breathlessness, high fever, or bluish lips are emergencies that need immediate care.
COPD and Pneumonia: How the Two Are Connected
To understand the link between COPD and pneumonia, it helps to be clear on what each one actually is. They affect the same organ, but they are not the same problem.
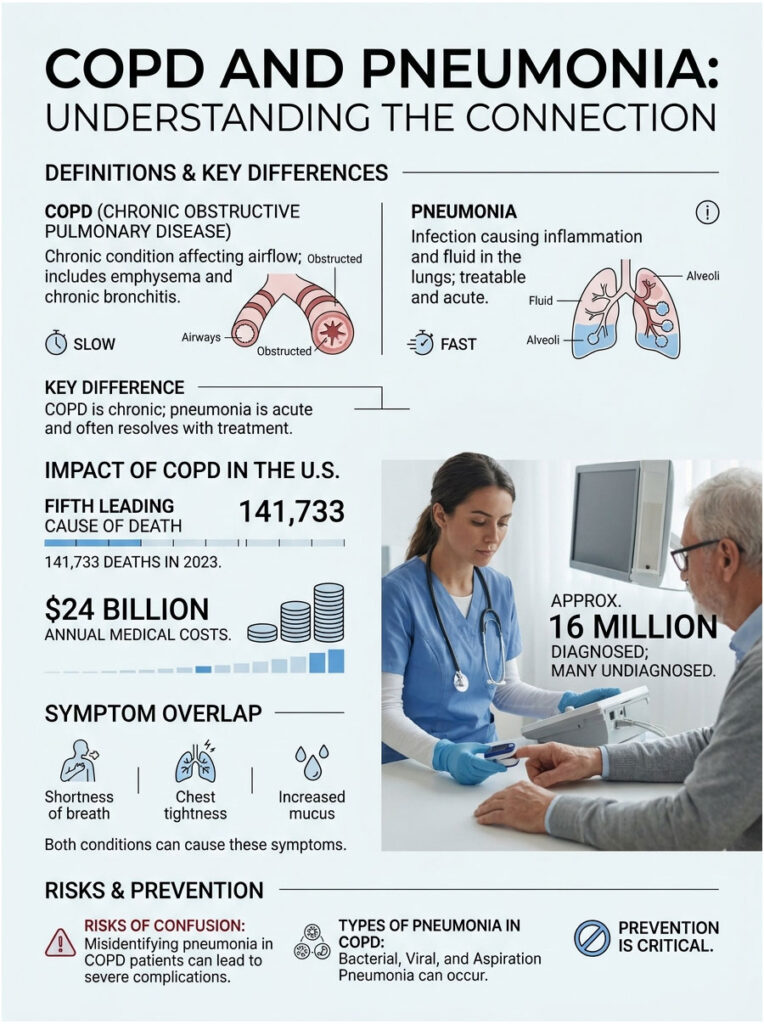
COPD, or chronic obstructive pulmonary disease, is a long-term condition that blocks airflow and makes breathing harder over time. It mainly includes emphysema, which damages the lung’s air sacs, and chronic bronchitis, which inflames the airways and produces extra mucus.
Pneumonia is different. It is an infection that inflames the air sacs in one or both lungs, often filling them with fluid or pus. Bacteria, viruses, and fungi can all cause it, and unlike COPD, most cases can be treated and resolved.
What COPD Is, and What Pneumonia Is
The simplest way to hold the difference in mind is this. COPD is chronic and lifelong, managed but not cured. Pneumonia is acute, an infection that arrives, peaks, and in most cases clears with treatment.
COPD is also widespread and serious. According to the CDC, COPD was the fifth leading cause of death in the United States in 2023, accounting for 141,733 deaths, and it carries about $24 billion in annual medical costs for adults aged 45 and older.
Roughly 16 million American adults have been diagnosed with COPD, and many more likely have it without knowing. Patients booking lung function tests with us often arrive surprised that mild, long-ignored breathlessness was an early sign all along.
Why the Two Are Easy to Confuse
Here is where things get tricky. COPD tends to flare up, settle, then flare again, and these flare-ups, called exacerbations, can look a great deal like pneumonia.
Both can bring shortness of breath, chest tightness, coughing, and more mucus than usual. When the symptoms overlap this much, it is easy for a patient to assume it is just another bad COPD day and wait too long to seek help.
Our medical reviewers note that this confusion is one of the biggest hidden dangers. A missed pneumonia in someone with COPD can escalate quickly, so knowing the warning signs matters more here than for almost anyone else.
Types of Pneumonia That Affect COPD Patients
Pneumonia is not a single illness. Several types can affect someone with COPD, and the cause shapes both treatment and prevention.
Bacterial pneumonia is the most common concern, and pneumococcal pneumonia, caused by Streptococcus pneumoniae, is a leading culprit. Viral pneumonia can follow influenza, COVID-19, or RSV, all of which circulate heavily in the colder months.
Aspiration pneumonia is another risk, especially in older adults, when food, liquid, or saliva is accidentally breathed into the lungs. Knowing that several routes lead to pneumonia explains why prevention has to work on more than one front at once.
Why COPD Raises Your Pneumonia Risk
COPD does not invite infection out of bad luck. It changes the lung in specific ways that make it a far friendlier place for germs to settle and multiply.
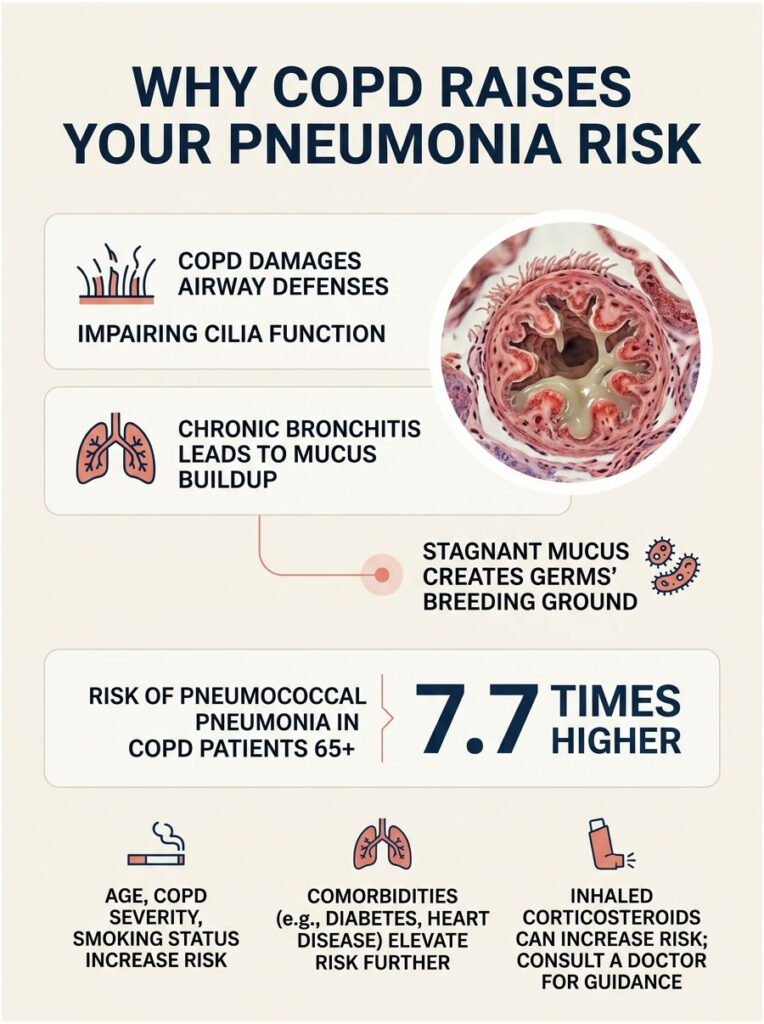
Weakened Airway Defenses and Excess Mucus
Healthy lungs have a built-in cleaning system. Tiny hair-like structures called cilia sweep mucus, dust, and germs up and out of the airways before they can cause harm.
COPD damages that system. The cilia work poorly, and chronic bronchitis floods the airways with thick mucus that the lungs struggle to clear. That stagnant mucus becomes an ideal place for bacteria and viruses to grow.
So a germ that a healthy lung would flush out within hours can linger in a COPD patient’s airway long enough to take hold. The lung’s first line of defense is simply not doing its job.
Chronic Inflammation and Reduced Lung Reserve
COPD also keeps the lungs in a constant state of low-grade inflammation. Inflamed, narrowed airways move air poorly, and damaged air sacs cannot exchange oxygen the way healthy ones do.
This means a person with COPD already runs on a thinner margin. There is little spare lung capacity to fall back on. When pneumonia adds fluid and inflammation on top, that margin can vanish fast, which is why a COPD patient with pneumonia can deteriorate so quickly.
The numbers tell the story plainly. The American Lung Association reports that for adults 65 and older living with COPD, the risk of pneumococcal pneumonia is 7.7 times higher than for healthy peers of the same age.
Who Faces the Highest Risk
COPD raises pneumonia risk for everyone who has it, but some people carry an even heavier load. Age is a major factor, since the immune system weakens over time and most COPD patients are older adults.
The severity of COPD matters too. People with more advanced disease, frequent flare-ups, or low baseline oxygen levels tend to face greater danger from infection. So do those who continue to smoke, which keeps damaging the airways every day.
Other health conditions stack the odds further. Diabetes, heart disease, and a weakened immune system all make pneumonia more likely and harder to recover from. Ongoing exposure to dust, fumes, or secondhand smoke at home or work adds another layer of strain on already vulnerable lungs.
The Role of Inhaled Corticosteroids
There is one nuance worth knowing. Many people with moderate to severe COPD use inhaled corticosteroids to reduce flare-ups, and these inhalers genuinely help many patients.
But research has linked inhaled corticosteroids to a modestly higher pneumonia risk in some COPD patients. This is not a reason to stop your inhaler. It is a reason to talk with your doctor about whether your current regimen is the right fit, since the balance of benefit and risk varies from person to person.
| COPD and Pneumonia Statistic (USA) | Figure | Source |
| Pneumococcal pneumonia risk, COPD adults 65+ vs healthy peers | 7.7x higher | American Lung Association |
| US adults diagnosed with COPD | About 16 million | CDC |
| COPD deaths in the United States, 2023 | 141,733 | CDC NCHS Data Brief No. 529 |
| COPD rank among US causes of death, 2023 | 5th | CDC NCHS Data Brief No. 529 |
| Annual US medical cost of COPD, adults 45+ | About $24 billion | CDC NCHS Data Brief No. 529 |
COPD Flare-Up or Pneumonia? How to Tell the Difference
This is the question that worries COPD patients most, and for good reason. Telling a flare-up from pneumonia at home is genuinely hard, but a few patterns can guide you.

Overlapping Symptoms
A COPD exacerbation and pneumonia share a lot of ground. Both can cause more breathlessness than usual, more coughing, more mucus, chest tightness, and fatigue.
Because of this overlap, the difference is often in the details: how fast symptoms came on, whether a fever is present, and what the mucus looks like. None of these is a perfect test, but together they help.
Red-Flag Signs That Point to Pneumonia
A few features lean more toward pneumonia than a routine flare-up. A high fever with shaking chills is uncommon in a simple COPD exacerbation but typical of pneumonia.
Sharp chest pain that worsens with breathing or coughing is another clue. So is a change in mucus color. Normally clear or white sputum that turns green, yellow, or blood-tinged raises concern for infection.
In cases reviewed across our diagnostic network, the patients who do best are those who treat any sudden, sharp change as a reason to call their doctor rather than wait. The table below offers a side-by-side guide, but it does not replace medical assessment.
| Feature | Typical COPD Exacerbation | Typical Pneumonia | Why It Matters |
| Onset | Gradual, over hours to days | Often faster, can come on sharply | Sudden change leans toward infection |
| Fever | Mild or absent | High fever, shaking chills common | A clear fever points to pneumonia |
| Chest pain | Tightness, general discomfort | Sharp pain, worse on breathing or coughing | Sharp, localized pain is a red flag |
| Mucus color | Usual color, more in volume | Green, yellow, rust-colored, or blood-tinged | Color change suggests infection |
| Overall feeling | Unwell but familiar pattern | Markedly worse, confusion possible in older adults | Feeling much sicker warrants urgent care |
How Pneumonia Affects COPD: Complications and Outlook
Pneumonia is serious for anyone, but for a person with COPD the stakes are higher. Understanding why helps explain the strong push toward prevention.

Hospitalization, Respiratory Failure, and Recovery Time
When pneumonia strikes a COPD patient, the lungs are hit on two fronts at once. The result is often a sharp drop in oxygen levels and a real risk of respiratory failure, a condition where the body cannot get the oxygen it needs.
This is why people with COPD who develop pneumonia usually need hospital care, sometimes including supplemental oxygen or breathing support. Recovery also takes longer than it would for an otherwise healthy person.
Patients commonly ask us how long they will feel run down afterward. The honest answer is that it varies, but full recovery often stretches over several weeks, and some loss of stamina can linger longer.
Beyond the Lungs
The damage from pneumonia in a COPD patient is not always confined to the chest. When oxygen levels drop low enough, other organs feel the strain.
Low oxygen can stress the heart and has been linked to cardiovascular events, and severe infection can affect the kidneys and brain function. This whole-body ripple effect is part of why a pneumonia episode in someone with COPD is treated as a serious event, not a routine illness.
The Cycle of Infection and Decline
There is a pattern worth understanding. Each serious lung infection can leave the lungs a little weaker, and weaker lungs are more prone to the next infection.
This loop, sometimes described as a cycle of infection and decline, is part of why doctors treat pneumonia prevention so seriously in COPD. Breaking the cycle early, before infections stack up, protects lung function over the years ahead.
Patients commonly ask us whether one bad episode means a steep downhill slide. It does not have to. Many people stabilize well after pneumonia, especially when they tighten up vaccination and COPD management afterward.
What the Research Says About Long-Term Outcomes
The research is sobering but worth knowing. A 2018 analysis found that COPD patients who developed pneumonia faced higher 30-day and 90-day mortality than patients without COPD.
A separate study that followed COPD patients over six years found that those who developed pneumonia during follow-up had lower survival than those who did not. Pneumonia can also trigger or worsen COPD flare-ups, and a severe episode may leave lasting damage.
None of this is meant to frighten you. It is meant to make one point clearly: with COPD, preventing pneumonia is not a minor extra. It is a core part of protecting your health.
How to Lower Your Pneumonia Risk with COPD
Here is the encouraging part. A large share of pneumonia risk in COPD is modifiable. The steps are not complicated, and they work.

Vaccines That Matter
Vaccination is the single most effective tool. For people with COPD, several vaccines pull weight: the pneumococcal vaccine against the most common bacterial pneumonia, the annual flu shot, updated COVID-19 vaccines, and, for many older adults, the RSV vaccine.
These are not interchangeable. Each protects against a different cause of respiratory infection, and together they close gaps no single shot could cover on its own.
The Updated Pneumococcal Vaccine Guidance
The guidance here changed recently, so it is worth being current. In late 2024, the CDC’s Advisory Committee on Immunization Practices lowered the age for routine adult pneumococcal vaccination from 65 to 50.
Importantly, adults aged 19 to 49 with chronic lung disease, which includes COPD, are also recommended to receive a pneumococcal vaccine on a risk basis. If you have COPD and have not discussed pneumococcal vaccination with your provider, that conversation is worth having soon.
Quitting Smoking and Managing COPD Well
Smoking is the leading cause of COPD, and continuing to smoke keeps damaging the airway defenses you need most. Quitting at any age slows lung decline and lowers infection risk, and it is never too late to benefit.
Good COPD control matters just as much. Taking maintenance inhalers as prescribed, following your action plan, attending pulmonary rehabilitation if offered, and keeping regular checkups all reduce flare-ups, and fewer flare-ups means fewer openings for pneumonia.
Pulmonary Rehabilitation and Breathing Strength
Pulmonary rehabilitation deserves a special mention. These structured programs combine supervised exercise, breathing techniques, and education, and they rank among the most effective tools for living well with COPD.
Stronger breathing muscles and better exercise tolerance help the body handle stress, including the stress of fighting an infection. Many programs also teach airway clearance techniques that move mucus out, reducing the stagnant buildup where germs thrive.
If your doctor has not mentioned pulmonary rehab, it is worth asking about. Programs are widely available across the US, and many are covered by insurance for people with COPD.
Everyday Infection-Prevention Habits
Small daily habits add up. Wash your hands often and well, especially before eating and after being in public spaces. During respiratory virus season, avoid close contact with people who are sick.
Stay on top of general health too. Good nutrition, adequate sleep, managing other conditions like diabetes, and staying active within your limits all help your immune system do its job. Our lab partners report that COPD patients who keep up with both vaccines and routine monitoring tend to face fewer infection crises.
Reducing Harmful Exposures at Home
Your environment counts as well. Air pollution, dust, strong fumes, and secondhand smoke all irritate already sensitive airways and can make infection easier to catch.
Where you can, limit time outdoors on high-pollution days, keep your home free of tobacco smoke, and use proper ventilation around cleaning products or strong chemicals. These adjustments are simple, and for vulnerable lungs they remove one more avenue for trouble.
Diagnosis and Treatment: What to Expect
If your doctor suspects pneumonia, knowing what comes next can ease some of the worry. The process is usually quick and focused.
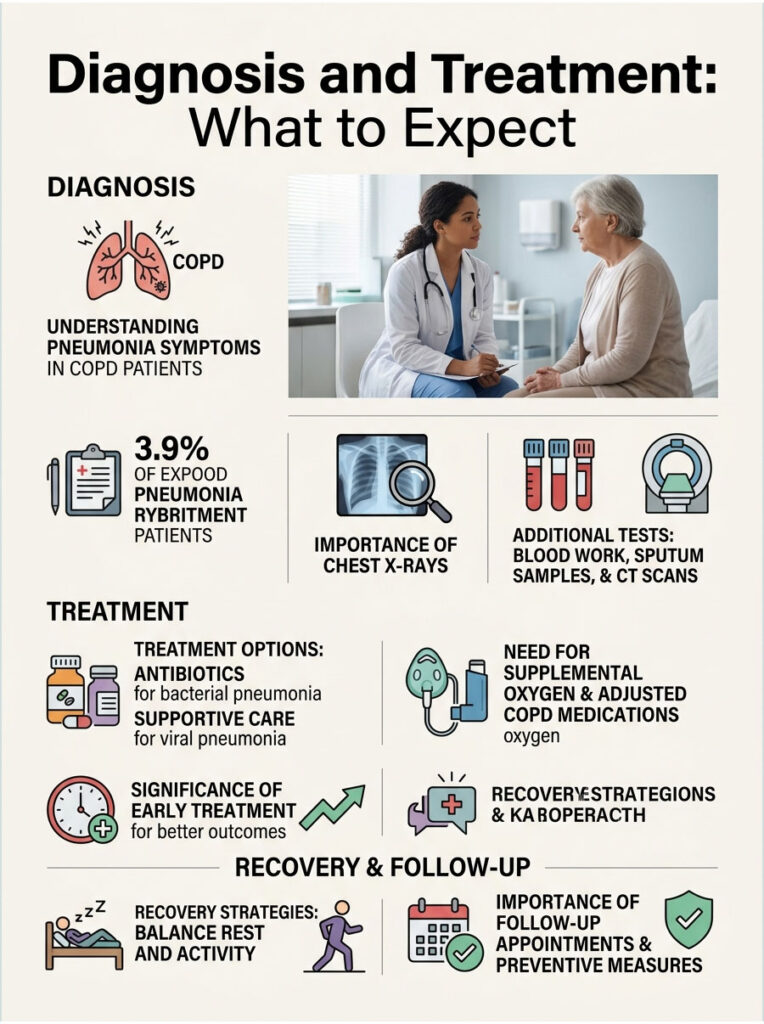
How Doctors Confirm Pneumonia in a COPD Patient
Because pneumonia and a COPD flare-up look so similar, doctors rely on tests rather than symptoms alone. A chest X-ray is the most common step, since pneumonia often shows up as a distinct area of infection on the image.
Doctors may also order blood work to check for signs of infection, a sputum sample to identify the responsible germ, and a measure of blood oxygen levels. A CT scan is sometimes used when the picture is unclear.
Treatment Approaches and Why Early Action Matters
Treatment depends on the cause. Bacterial pneumonia is treated with antibiotics, sometimes given through an IV in the hospital, while viral pneumonia is managed with supportive care and, in some cases, antiviral medication.
A COPD patient may also need extra support: supplemental oxygen, adjusted COPD medications, or treatment for an accompanying flare-up. The single biggest factor in a good outcome is timing. Early treatment limits lung damage and lowers the risk of complications, which is exactly why recognizing the warning signs early is so valuable.
Recovering Well After Pneumonia
Recovery does not end when the antibiotics finish. The weeks afterward are a chance to rebuild, and how you spend them matters.
Rest when your body asks for it, but reintroduce gentle activity as your doctor allows, since staying completely still too long can slow recovery. Keep your follow-up appointments so your team can confirm the infection has fully cleared and check whether your COPD treatment needs adjusting.
Use the recovery period to close any gaps too. If a vaccine is overdue or your inhaler technique has drifted, this is the moment to fix it and lower the odds of a repeat infection.
When to Call Your Doctor or Go to the ER
With COPD, knowing when to act is a skill worth practicing. Waiting too long is the most common and most dangerous mistake.

Symptoms to Monitor at Home
Pay attention to change. More breathlessness than your usual baseline, a new or worsening cough, a shift in mucus color or amount, a fever, or unusual fatigue all deserve a call to your doctor, ideally the same day.
Keeping a simple daily sense of your normal helps you catch these shifts early. Many COPD patients use a written action plan from their care team for exactly this purpose.
Emergency Warning Signs
Some symptoms cannot wait. Severe or sudden shortness of breath, chest pain, a high fever that will not come down, bluish lips or fingertips, and confusion or extreme drowsiness are medical emergencies.
If any of these appear, call 911 or get to an emergency room right away. With COPD, the margin for delay is thin, and quick action genuinely saves lives.
| If You Notice This | What It May Mean | What to Do |
| More mucus than usual, mild fatigue, no fever | Possible early flare-up or mild infection | Call your doctor today; follow your COPD action plan |
| Mucus turns green, yellow, or blood-tinged | Possible respiratory infection or pneumonia | Contact your doctor promptly for assessment |
| Fever with shaking chills plus worse breathing | Pneumonia is a real possibility | Seek same-day medical care; do not wait it out |
| Sharp chest pain that worsens when you breathe | Possible pneumonia or other lung complication | Get urgent medical evaluation |
| Severe breathlessness, bluish lips, or confusion | Possible respiratory failure or low oxygen | Call 911 or go to the ER immediately |
Living with COPD: Reducing Long-Term Risk
Pneumonia prevention is not a one-time task. It works best as a steady routine woven into how you manage COPD overall.

An Action Plan and Follow-Up Testing
Ask your care team for a written COPD action plan if you do not have one. It spells out your usual baseline, what worsening looks like, and exactly what to do at each stage, which removes guesswork on a hard day.
Regular follow-up matters too. Lung function testing, monitoring of oxygen levels, and reviews of your inhaler technique and vaccine status all help your team catch trouble early and keep your treatment matched to your needs.
Building a Support and Monitoring Routine
You do not have to manage COPD alone. Pulmonary rehabilitation programs, support groups, and a reliable circle of family or friends all improve both confidence and outcomes.
Across patients we serve, the ones who stay steadiest are those who treat COPD as something they actively manage day to day, not something they simply endure. Vaccines, smoking cessation, prompt care, and consistent follow-up are the foundation, and together they meaningfully lower your pneumonia risk.
The Role of Caregivers and Family
Family members and caregivers play a real part in prevention. Staying current on their own flu and COVID-19 vaccines lowers the chance of bringing an infection into the home.
Caregivers can also help by watching for early warning signs, supporting medication and inhaler routines, and knowing the emergency plan in advance. With COPD, a second set of eyes often catches a worsening change sooner than the patient does.
Frequently Asked Questions
Can COPD turn into pneumonia?
No. COPD and pneumonia are separate conditions, and one does not become the other. COPD is a chronic airway disease, while pneumonia is an infection. However, COPD damages the lungs in ways that make catching pneumonia significantly more likely and more severe.
How can you tell a COPD flare-up from pneumonia?
It can be hard, since both cause breathlessness, coughing, and more mucus. Pneumonia is more likely when symptoms come on fast, a high fever with chills appears, chest pain sharpens with breathing, or mucus turns green, yellow, or blood-tinged. Any sudden change warrants a prompt medical check.
Why are people with COPD more likely to get pneumonia?
COPD damages the airway’s natural cleaning system and produces excess mucus where germs thrive. It also leaves the lungs inflamed with little spare capacity. Together, these changes make it easier for infection to take hold and harder for the body to fight it off.
Is pneumonia more dangerous if you have COPD?
Yes. People with COPD who develop pneumonia are more likely to need hospitalization, to recover slowly, and to face complications like respiratory failure. Research also links COPD with higher pneumonia-related mortality, which is why prevention and early treatment matter so much.
Which pneumonia vaccine should COPD patients get?
That depends on your age and vaccination history. The CDC now recommends routine pneumococcal vaccination for all adults 50 and older, and on a risk basis for adults 19 to 49 with chronic lung disease, including COPD. Your doctor or pharmacist can confirm the right vaccine for you.
How long does it take to recover from pneumonia with COPD?
Recovery is usually slower than for people without COPD. Many patients feel weak or short of breath for several weeks, and full stamina can take longer to return. Following your treatment plan and attending follow-up appointments supports the steadiest recovery.
Can pneumonia cause permanent lung damage in COPD?
It can. A severe pneumonia episode may leave lasting scarring or further reduce lung function, especially in already damaged lungs. This is one reason early treatment is so important, since prompt care helps limit the extent of damage from the infection.
Does pneumonia make COPD worse over time?
It can. Pneumonia can trigger COPD flare-ups and may accelerate decline in lung function, particularly with repeated or severe infections. Each serious infection can chip away at lung reserve, which is why preventing pneumonia is a core part of long-term COPD management.
What is the life expectancy with COPD and pneumonia?
There is no single answer, since outcomes depend on COPD severity, age, overall health, and how quickly pneumonia is treated. Studies show higher mortality when the two occur together, but early treatment, vaccines, and good COPD control all improve the outlook considerably.
Can you prevent pneumonia if you have COPD?
You cannot eliminate the risk, but you can lower it substantially. Staying current on pneumococcal, flu, COVID-19, and RSV vaccines, quitting smoking, managing COPD well, and practicing good hand hygiene are all proven, practical steps that meaningfully reduce your chances.
Should COPD patients get the flu shot too?
Yes. Influenza is a common trigger for both COPD flare-ups and pneumonia. An annual flu vaccine is recommended for people with COPD and works alongside the pneumococcal vaccine to cover different infection causes. The two protect against separate threats and are not interchangeable.
What color is the mucus when a COPD patient has pneumonia?
Mucus that is normally clear or white may turn green, yellow, rust-colored, or blood-tinged when an infection like pneumonia is present. A noticeable color change, especially alongside fever or worse breathing, is a signal to contact your doctor promptly.
Disclaimer: This article is for general educational purposes and is not medical advice. It does not diagnose, treat, or replace care from a licensed healthcare professional. COPD and pneumonia are serious conditions, and symptoms can escalate quickly. If you have COPD and notice worsening breathing, fever, or other concerning changes, contact your healthcare provider promptly or seek emergency care.
References
- CDC, National Center for Health Statistics, Data Brief No. 529: Chronic Obstructive Pulmonary Disease in Adults
- CDC: Chronic Disease Indicators, COPD
- CDC: Pneumococcal Vaccine Recommendations
- American Lung Association: The Connection Between Pneumonia and Lung Disease
- National Library of Medicine: Influence of Pneumonia on the Survival of Patients with COPD
- National Library of Medicine: Effects of Pneumonia and COPD on Patient Mortality