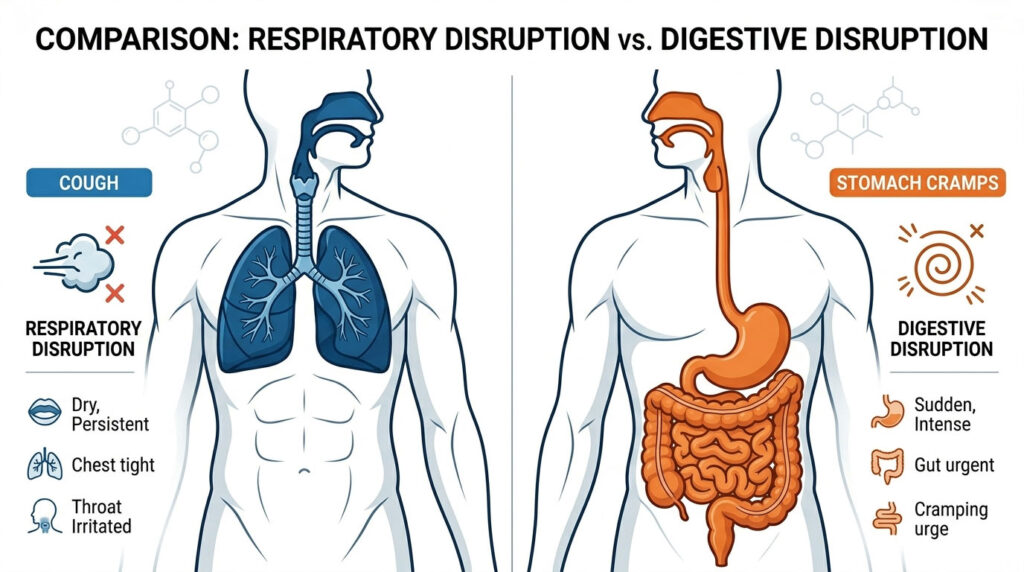
Sudden, explosive diarrhea is almost always caused by norovirus (viral gastroenteritis), not the flu. True influenza is a respiratory illness that rarely causes diarrhea in healthy adults. Confusing the two often leads to wrong treatments, delayed recovery, and dangerous dehydration.
Table of Contents
Every winter, my infectious disease clinic fills up with patients clutching their stomachs. They all want to know the same thing: is this diarrhea the flu or norovirus?
It is a fair question. The term “stomach flu” gets thrown around constantly, but it is medically misleading. The stomach flu is not actually the flu at all. Norovirus and influenza are two completely different illnesses that attack different parts of your body.
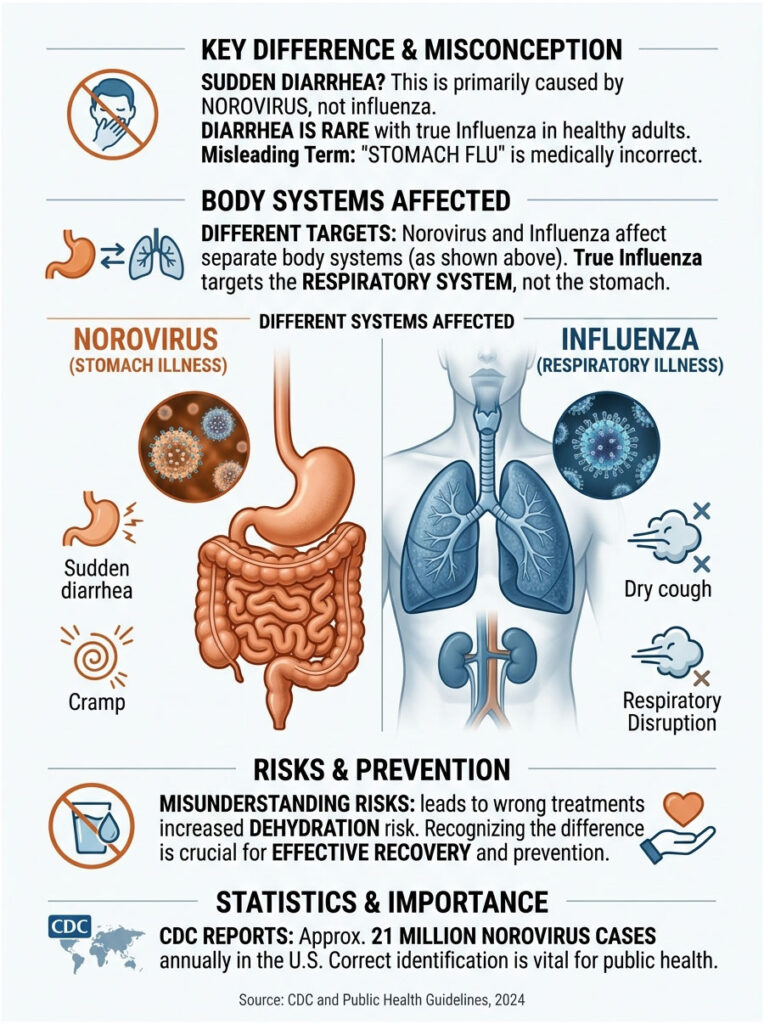
This confusion matters because it leads people to take the wrong medications, ignore dehydration, and spread illness to everyone around them. In this guide, I will walk you through the real medical differences between these two viruses so you can take the right steps to recover.
According to the CDC, norovirus causes roughly 21 million cases of viral gastroenteritis in the United States every year. Meanwhile, true influenza targets the lungs and respiratory tract, not the stomach.
Key Statistics on Viral Infections
- 21 million: Estimated annual U.S. cases of norovirus (CDC, 2023)
- 10% to 25%: Percentage of adult flu cases with any GI symptoms
- 12 to 48 hours: Typical incubation period for norovirus
- 109,000: Annual hospitalizations from viral gastroenteritis dehydration
- 900: Average annual U.S. deaths from norovirus, mostly among the elderly
- 2 weeks: Duration of viral shedding in stool after symptoms stop
How These Viruses Attack Your Body
To settle the norovirus vs flu debate once and for all, you need to understand what happens at the cellular level. These two viruses target entirely different systems in your body, and the symptoms they produce reflect that difference.

Viruses are essentially microscopic hijackers. They cannot reproduce on their own. Instead, they invade specific human cells to multiply. The type of cell a virus targets determines the symptoms you experience.
Viral Gastroenteritis: Norovirus, Rotavirus, and Adenovirus
When you catch viral gastroenteritis, you are dealing with enteric pathogens. These are viruses that have evolved to survive the harsh, acidic environment of your digestive tract. Most other viruses would be destroyed by your stomach acid on contact.
Once swallowed, these pathogens travel to your stomach and intestines and attach to the gastric mucosa, the delicate inner lining of your gut. From there, the virus enters your cells and replicates by the millions, triggering a powerful inflammatory response.
Your immune system recognizes the invader and tries to flush it out. This inflammation damages the tiny, finger-like structures in your intestines called microvilli. Normally, healthy microvilli absorb water and nutrients from digesting food.
When enteric pathogens destroy these microvilli, your intestines lose the ability to absorb water. All that unabsorbed fluid rushes straight through your system. This is the exact mechanism behind the sudden, watery diarrhea that defines a stomach bug.
Why Vomiting Happens with a Stomach Bug
The gastric mucosa is your gut’s first line of defense. When norovirus damages this lining, your body responds with sudden, forceful vomiting. It is literally trying to expel the invading pathogens.
This damage takes real time to heal. Even after the vomiting stops, your gut lining stays inflamed and sensitive. That is why you struggle to digest heavy meals for days afterward. You might also feel bloated because the damaged lining temporarily stops producing the digestive enzymes you need.
True Influenza: Type A and Type B
Influenza is strictly a respiratory pathogen. It targets the delicate tissues of your lungs, throat, and nasal passages, not your stomach.
When the flu virus enters your body through inhaled droplets, it binds to respiratory epithelial cells and hijacks them to replicate. Your immune system responds by releasing chemical messengers called cytokines. This massive chemical release, known as a cytokine storm, causes the classic flu misery: deep muscle aches (myalgia), high fevers, chills, and crushing fatigue.
Because the flu virus targets the respiratory tract, you will develop a severe cough and sore throat. You will not typically experience the forceful, projectile vomiting that comes with viral gastroenteritis.
Expert Insight: I regularly see patients who assume their stomach bug is the flu and ask for Tamiflu. Tamiflu only works against respiratory influenza. It does absolutely nothing for norovirus, and misusing it can actually irritate your stomach further.
Norovirus vs. Flu: A Side-by-Side Symptom Comparison
When comparing norovirus vs flu, the timeline of your symptoms tells the clearest story. The way these two illnesses begin looks completely different in a clinical setting. Knowing what to look for can save you an unnecessary trip to the emergency room.
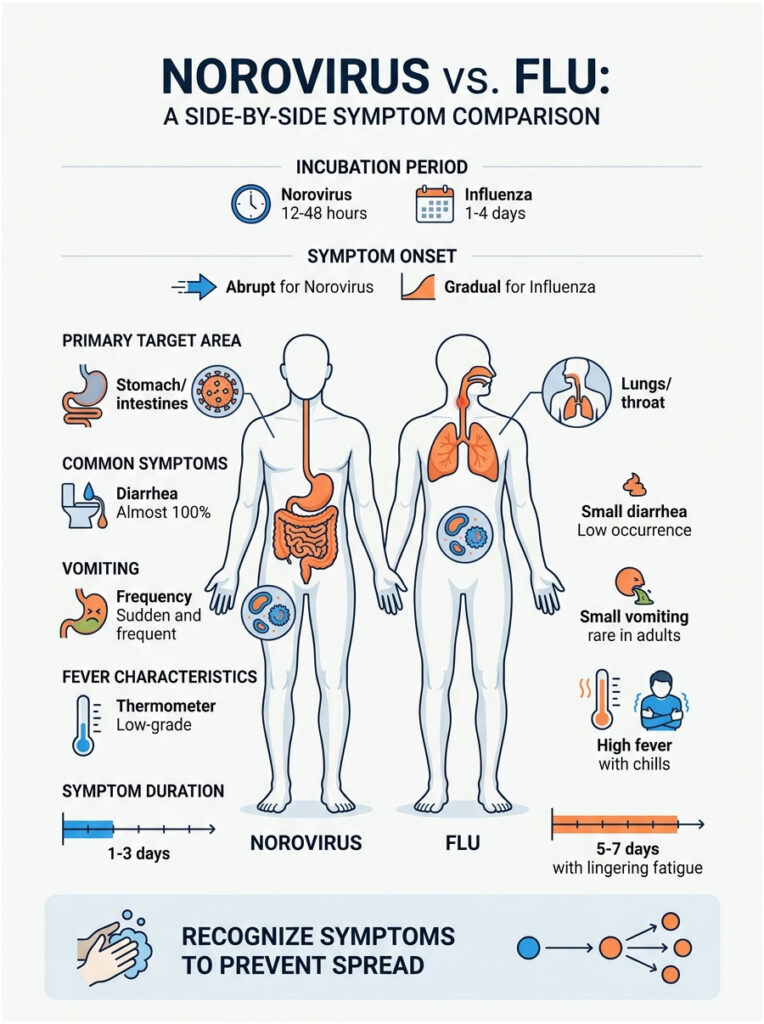
Incubation Periods and Onset
The incubation period is the time between exposure and the moment you feel sick. For norovirus, this window is extremely short, just 12 to 48 hours. The onset is abrupt. You might feel fine at breakfast and be violently ill by dinner.
Influenza has a longer incubation period of 1 to 4 days. Symptoms build more gradually, usually starting with a scratchy throat and a rising fever. It lacks that sudden, explosive quality of a stomach bug.
Tracking this timeline helps you figure out where you caught the illness, which is useful for warning others and preventing further spread.
Diagnostic Symptom Breakdown
| Clinical Feature | Norovirus (Viral Gastroenteritis) | Influenza (Respiratory Flu) |
| Primary Target | Stomach and intestines | Lungs, throat, and nasal passages |
| Diarrhea | Nearly 100% of symptomatic adults | Only 10-25% of adult cases |
| Vomiting | Sudden, forceful, and frequent | Rare in adults; occasional in children |
| Fever | Low-grade or absent | High fever with sudden onset and chills |
| Respiratory Signs | None | Severe cough, sore throat, congestion |
| Incubation Period | 12 to 48 hours | 1 to 4 days |
| Duration | 1 to 3 days of severe symptoms | 5 to 7 days, plus lingering fatigue |
The biggest giveaway is the primary target area. If your lungs are clear but your stomach is in agony, you are almost certainly dealing with viral gastroenteritis.
Can You Have Diarrhea with Influenza A?
While norovirus is by far the most common cause of sudden diarrhea, there are some edge cases worth discussing. Can you actually have diarrhea with Influenza A? The honest answer is yes, but it depends on your age and the specific strain circulating that year.

Adults vs. Children
Children’s immune systems are still developing and tend to react more aggressively to any infection. When a toddler contracts Influenza A, their strong systemic reaction can easily irritate the digestive tract. A sick child might have a high fever, a bad cough, and mild diarrhea all at once.
For parents trying to sort out norovirus vs flu in their children, focus on the primary complaint. Is the child coughing between trips to the bathroom? That points toward a respiratory flu with secondary stomach upset. If there are zero respiratory symptoms and the child is experiencing sudden projectile vomiting, it is almost certainly viral gastroenteritis.
Swallowed Mucus and Secondary Stomach Upset
There is another reason adults sometimes get mild stomach issues during a severe respiratory infection, and it has nothing to do with a stomach virus.
When you have a bad flu, your body produces excess mucus. As you sleep, this mucus drains down your throat into your stomach through post-nasal drip. The sensitive gastric mucosa becomes irritated, leading to nausea, loss of appetite, and mild loose stools.
This is a secondary reaction, not a direct gut infection. It is very different from the massive, uncontrollable volumes of watery stool that enteric pathogens produce. Hospital data from recent flu seasons confirms that fewer than 15% of admitted adults had any GI symptoms at all.
How These Viruses Spread: Transmission and Viral Shedding
Protecting your family starts with understanding how these viruses travel. The transmission routes for norovirus vs flu are completely different, which changes your prevention strategy.
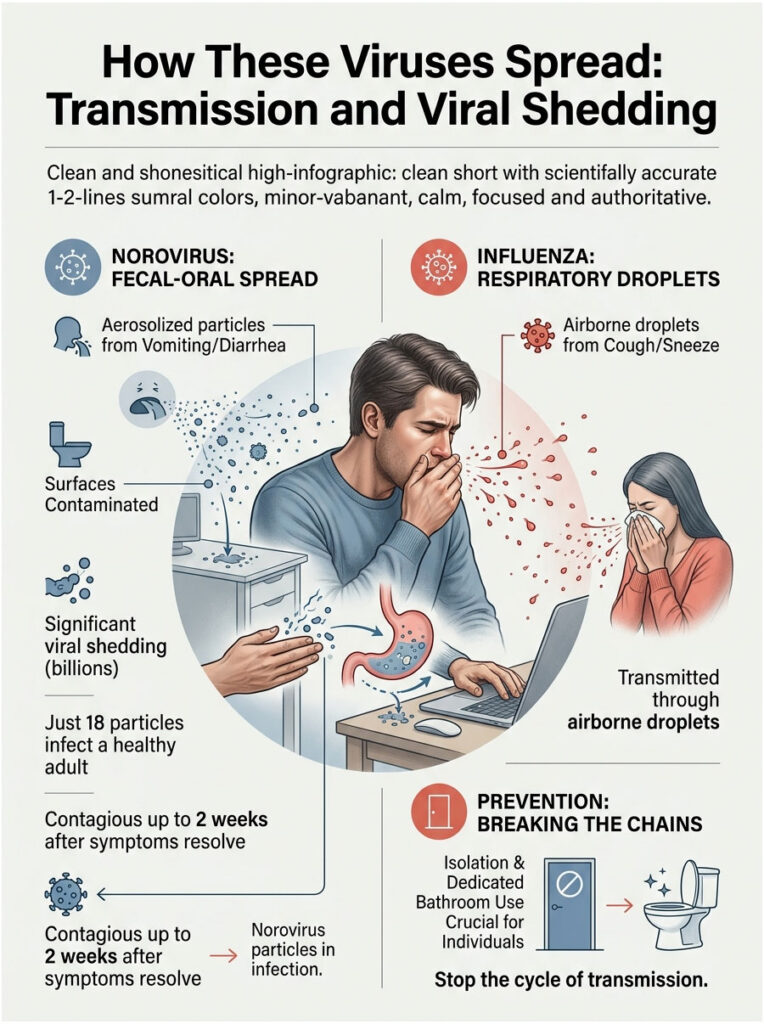
Fecal-Oral Route vs. Respiratory Droplets
Viral gastroenteritis spreads primarily through the fecal-oral route. Microscopic particles of feces or vomit from an infected person must physically enter your mouth for you to get sick.
When a person with norovirus vomits, the force creates an invisible cloud of aerosolized particles that settle on nearby surfaces, including countertops, doorknobs, light switches, and faucet handles. If you touch these surfaces and then touch your mouth or food, you ingest the virus. This is why norovirus tears through cruise ships and nursing homes so quickly.
Influenza, on the other hand, spreads through airborne respiratory droplets. When a sick person coughs or sneezes, the virus travels through the air in tiny moisture bubbles. You inhale them directly into your lungs, bypassing the stomach entirely.
The Hidden Danger of Viral Shedding
One of the most misunderstood aspects of viral gastroenteritis is viral shedding. During the acute phase, norovirus patients shed billions of infectious particles in their stool and vomit. It takes as few as 18 viral particles to infect a healthy adult.
Here is the part that catches people off guard: even after your diarrhea stops and you feel fine, you remain highly contagious. Norovirus patients keep shedding the virus in their stool for up to two full weeks after symptoms disappear. Without thorough handwashing, they continue to spread the illness.
With influenza, the shedding period is much shorter. Once your fever breaks and your cough subsides, the risk of transmission drops significantly.
Expert Insight: If someone in your household has a stomach bug, assign them a dedicated bathroom and keep them isolated for at least 48 hours after their last episode of vomiting or diarrhea. Strict bathroom isolation is often the only way to prevent a full household outbreak.
Prevention: Why Hand Sanitizer Fails Against Norovirus
Most people rely on alcohol-based hand sanitizers to stay clean, especially during cold and flu season. When it comes to a stomach bug, this is a major blind spot in public health.

The Science Behind the Failure
Norovirus lacks a viral envelope, the fragile fatty outer layer that protects some viruses. Alcohol-based sanitizers work by dissolving this lipid layer. Since influenza has a lipid envelope, hand sanitizer destroys it almost instantly.
Because norovirus has no such envelope, the alcohol simply bounces off its tough protein shell (called a viral capsid). Hand sanitizer is essentially useless against it.
The only reliable way to remove norovirus from your hands is good old-fashioned soap and water. Use warm water, plenty of soap, and vigorous scrubbing for at least 20 seconds. The soap physically lifts the virus off your skin, and the running water washes it away.
Disinfection Method Comparison
| Method | vs. Norovirus | vs. Influenza | Recommendation |
| Handwashing (Soap & Water) | Highly effective | Highly effective | First-line defense for all illnesses |
| Alcohol Hand Sanitizer | Ineffective (no lipid envelope) | Highly effective | Only useful for respiratory viruses |
| Diluted Bleach Solution | Highly effective | Highly effective | Required for household surface cleaning |
| Standard Disinfectant Wipes | Moderate to poor | Highly effective | Check labels for enteric pathogen claims |
Cleaning Up After a Stomach Bug at Home
Norovirus is incredibly resilient. It can survive on hard surfaces for weeks and on soft fabrics for up to 12 days.
The CDC recommends mixing 5 to 25 tablespoons of standard household bleach per gallon of water for cleaning biological spills. Do not use splashless bleach, as it typically has lower sodium hypochlorite concentration. Apply the solution and leave the surface visibly wet for at least five minutes to break through the virus’s tough outer shell.
Wash all contaminated clothing, towels, and bedding on the longest cycle with the hottest water setting. Dry on high heat for an extended cycle to destroy any remaining virus.
Oral Rehydration: The Real Science of Staying Hydrated
With viral gastroenteritis, the virus itself is rarely fatal to a healthy adult. The real medical emergency comes from rapid, uncontrollable fluid loss. Getting hydration right can be the difference between recovering at home and ending up in the hospital.
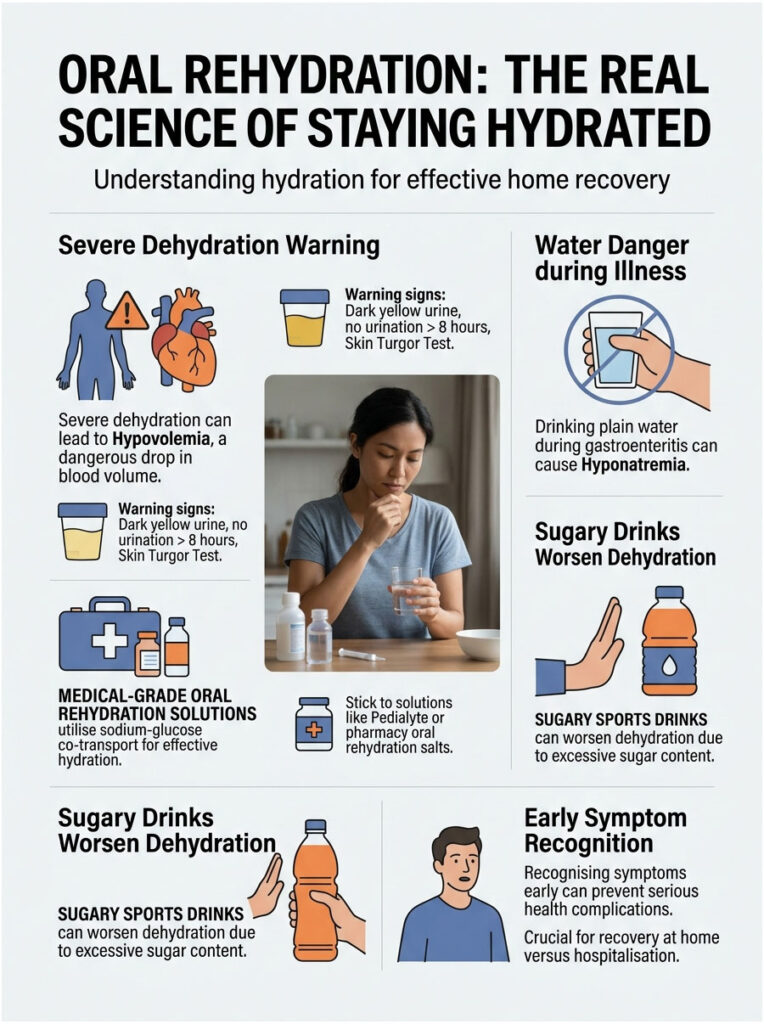
Recognizing Severe Dehydration
When you have explosive diarrhea and vomiting, you lose massive amounts of water and essential electrolytes. This can quickly lead to hypovolemia, a dangerous drop in blood volume that starves your organs of oxygenated blood.
Watch for these warning signs: dark yellow, strong-smelling urine, or no urination for over eight hours. Try the skin turgor test by pinching the skin on the back of your hand. If it stays tented up instead of snapping back, you are dangerously dehydrated. Other late signs include extreme dizziness upon standing and completely dry mouth with no saliva.
Why Plain Water Is Not Enough
Drinking plain water during severe gastroenteritis can actually be harmful. Plain water lacks electrolytes, and drinking large volumes dilutes the sodium remaining in your bloodstream. This can lead to hyponatremia, a dangerous condition that can trigger seizures.
Instead, use medical-grade oral rehydration solutions. These leverage a biological mechanism called the sodium-glucose co-transport system. When sodium and glucose are present in the right ratio, they bind together and get pulled across the damaged intestinal wall, dragging water molecules with them. This allows your gut to absorb water even when the microvilli are severely damaged.
Why Sports Drinks Make Things Worse
Many people reach for sugary sports drinks when they have a stomach bug. This is a mistake. Commercial sports drinks have far too much sugar and not enough sodium.
Excess sugar in the gut draws more water out of your bloodstream and into your intestines through osmosis, making your diarrhea worse. Stick to medical-grade solutions like Pedialyte or generic oral rehydration salts from your pharmacy.
Managing Symptoms and Rebuilding Your Gut
Surviving the first 48 hours is only half the battle. Once the acute vomiting stops, you need to rehabilitate your digestive system carefully. Rushing your recovery often makes things worse.
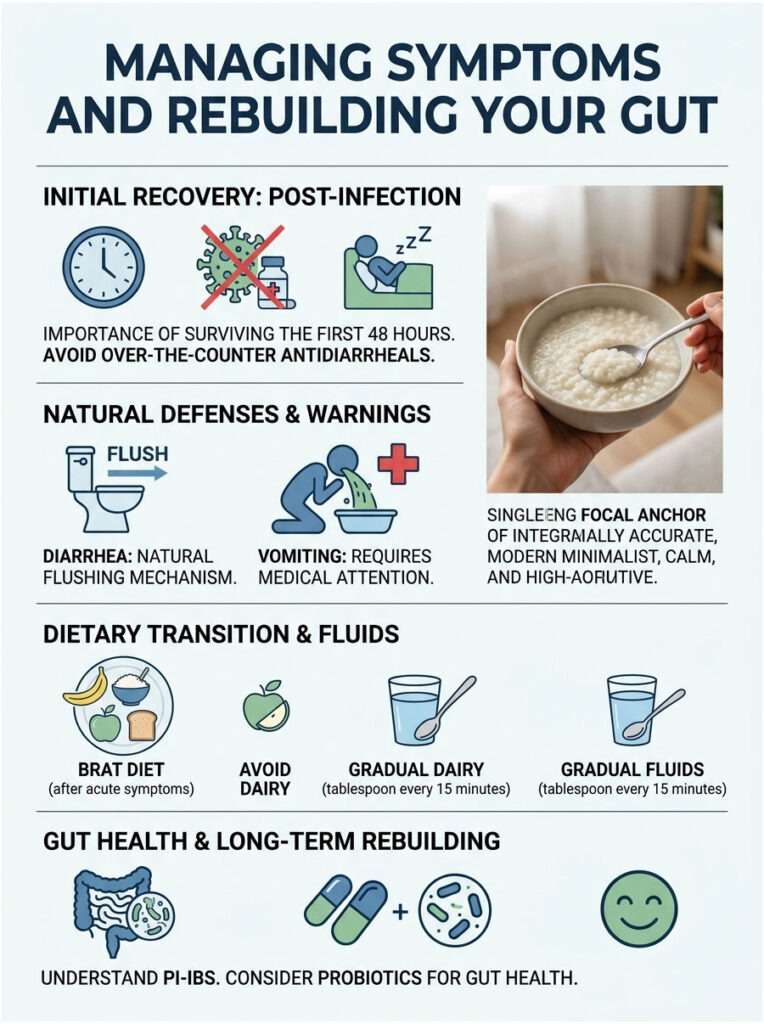
Should You Take Antidiarrheal Medication?
Patients constantly ask me for something to stop the diarrhea. I almost always advise against over-the-counter antidiarrheal medications during the first 48 hours.
Here is why: the diarrhea is your body’s natural mechanism for flushing out the virus. If you take a medication that slows your gut, you trap the living pathogen inside. This prolongs the illness and extends the contagious period.
Vomiting is a different story. If a patient cannot keep any fluids down, they are at serious risk for dehydration. In those cases, doctors will prescribe antiemetics like Zofran to stop the nausea and allow the patient to tolerate oral rehydration therapy.
The BRAT Diet and Dietary Transition
Once the worst symptoms pass, your gastric mucosa is still inflamed. Do not jump straight back to heavy meals. Transition slowly with the BRAT diet: Bananas, Rice, Applesauce, and Toast. These foods are bland, easy to digest, and contain soluble fiber that helps firm up loose stools.
Avoid dairy products entirely at first. Viral gastroenteritis temporarily strips your gut of lactase, the enzyme needed to digest milk. Drinking milk too soon will cause painful bloating and recurrent diarrhea.
When reintroducing fluids, take one tablespoon of an oral rehydration solution every fifteen minutes. Do not gulp a full glass, as this will trigger the stretch receptors in your stomach and cause immediate vomiting.
Post-Infectious Irritable Bowel Syndrome (PI-IBS)
Some patients report that their stomach never quite feels right after a severe norovirus infection. Lingering cramps, unpredictable bowel movements, and excessive gas can persist for months. This is a recognized condition called Post-Infectious Irritable Bowel Syndrome.
PI-IBS happens because the viral infection fundamentally disrupted your gut microbiome. The massive flush of diarrhea washed away billions of healthy bacteria. To help repopulate your gut flora, consider starting a high-quality probiotic containing Lactobacillus and Bifidobacterium strains about a week after your acute symptoms resolve.
When to Go to the Emergency Room
Most cases of viral gastroenteritis resolve on their own with proper home care. But there are critical situations where dehydration becomes too severe to manage without IV fluids. Ignoring these warning signs can lead to permanent kidney damage or worse.
Red Flag Symptoms
- Blood in vomit (hematemesis): Bright red streaks or dark, coffee-ground-like material
- Bloody stools: Norovirus causes watery diarrhea, not bloody. Blood may indicate a bacterial infection like Salmonella or E. coli
- High fever unresponsive to Tylenol
- Extreme lethargy or sudden confusion: Confusion is a dangerous sign that your brain is not receiving enough blood flow
- Symptoms that improve then suddenly worsen: This may signal a secondary bacterial infection
Special Risks for Children and the Elderly
Infants have very little internal fluid reserve due to their small body mass. They can become dangerously dehydrated within hours. If an infant has no wet diapers for six hours or cries without producing tears, seek emergency care immediately. Also check the fontanelle (the soft spot on top of the head). A sunken fontanelle is a classic sign of severe pediatric dehydration.
Elderly adults are equally vulnerable. Many have a diminished sense of thirst and may already take diuretics for blood pressure. The vast majority of norovirus-related deaths occur in adults over 65. If an elderly relative becomes confused or cannot stand without fainting, call an ambulance immediately.
Current Research and the Future of a Norovirus Vaccine
Patients often wonder why we have a flu shot but nothing for the stomach bug. It is a valid question, and the scientific hurdles are significant.
Why the Flu Shot Does Not Protect Against Norovirus
The annual flu vaccine targets specific respiratory influenza strains only. Because norovirus and influenza belong to entirely different viral families, cross-protection is biologically impossible. Getting your flu shot is still highly recommended for protecting your lungs, but it will not shield your stomach from norovirus.
People sometimes claim they got a stomach bug right after their flu shot. This is coincidence, not cause and effect. They simply caught a circulating enteric pathogen around the same time they visited the clinic.
mRNA Vaccine Trials and the Road Ahead
Researchers are currently running advanced clinical trials for an mRNA-based norovirus vaccine. The biggest challenge is the virus’s rapid mutation rate. Norovirus constantly changes the shape of its protein capsid, and natural human immunity after infection lasts only a few months.
This means you can catch viral gastroenteritis multiple times in the same year if new strains circulate. Developing a durable, multi-strain vaccine remains a top priority for infectious disease researchers worldwide.
Until a vaccine reaches the market, our best defenses remain strict hygiene: thorough handwashing with soap and water, proper bleach disinfection of surfaces, and responsible isolation of sick family members.
Key Takeaways: Is Diarrhea Flu or Norovirus?

- The core difference: Norovirus attacks the stomach and intestines, causing explosive diarrhea and vomiting. Influenza targets the lungs, causing coughs, high fevers, and body aches.
- Adults vs. children: True flu rarely causes diarrhea in adults (only 10-25% of cases). Children are more likely to have mild GI symptoms alongside respiratory illness.
- Contagious window: You shed norovirus in your stool for up to two weeks after symptoms stop. The contagious period for a stomach virus is much longer than most people realize.
- Hygiene matters: Alcohol hand sanitizer does not kill norovirus. You must use soap and water with vigorous scrubbing.
- Hydration is critical: Use medical-grade oral rehydration solutions, not sports drinks or plain water. Both can make diarrhea worse.
- Medication caution: Avoid antidiarrheal medications early on. They trap the virus in your body. Antiemetics can help if vomiting prevents hydration.
Understanding these differences puts you in a much better position to protect your family, prevent household outbreaks, and get the right treatment. Keep oral rehydration solutions stocked at home, practice thorough handwashing, and respect how contagious these winter viruses really are.
Frequently Asked Questions
Is diarrhea a common symptom of the seasonal respiratory flu in adults?
As an infectious disease specialist, I frequently clarify that true respiratory influenza rarely presents with diarrhea in healthy adults. Clinical data shows that only 10% to 25% of adult flu cases involve gastrointestinal symptoms. If your primary symptom is explosive diarrhea without a significant cough or sore throat, you are likely suffering from viral gastroenteritis, commonly caused by norovirus, rather than the flu.
How can I clinically differentiate between norovirus and the respiratory flu?
The most reliable diagnostic tool is the primary target area of the symptoms. Norovirus targets the gastric mucosa, leading to sudden projectile vomiting and watery diarrhea within a 12 to 48-hour incubation period. Influenza is a respiratory pathogen that targets the lungs and throat, characterized by high fevers, severe myalgia (muscle aches), and a hacking cough, typically appearing 1 to 4 days after exposure.
Why doesn’t alcohol-based hand sanitizer kill the ‘stomach flu’ or norovirus?
Norovirus is a non-enveloped virus, meaning it lacks the fatty lipid envelope that alcohol-based sanitizers are designed to dissolve. It is protected by a hardy protein shell called a capsid. To effectively remove these enteric pathogens, you must use mechanical friction by washing your hands with soap and warm water for at least 20 seconds to physically lift the virus from the skin.
How long is the contagious period for a stomach virus infection?
The contagious window for norovirus is surprisingly long. While the acute symptoms of vomiting and diarrhea usually subside within 1 to 3 days, patients continue a process called viral shedding. You can remain highly infectious and shed billions of viral particles in your stool for up to two full weeks after you feel completely recovered, making strict bathroom hygiene essential.
Can children experience diarrhea during a bout of Influenza A or B?
Yes, pediatric presentations differ significantly from adult cases. Children’s immune systems often trigger a more aggressive systemic inflammatory response to respiratory viruses, which can irritate the digestive tract. Additionally, young children often swallow infected mucus (post-nasal drip), which can cause secondary gastric irritation and mild diarrhea, though it is rarely as explosive as a primary norovirus infection.
What is the most effective way to disinfect a home after a norovirus outbreak?
Standard grocery store disinfectant wipes are often insufficient against the resilient protein capsid of norovirus. We recommend a diluted bleach solution (5 to 25 tablespoons of household bleach per gallon of water). This solution must remain wet on hard surfaces for a ‘dwell time’ of at least five minutes to successfully denature the virus. Always use hot water cycles for contaminated linens and clothing.
Why are sports drinks considered suboptimal for treating severe dehydration from diarrhea?
Commercial sports drinks often contain high concentrations of sugar and insufficient sodium. High sugar levels in the intestines can trigger osmosis, which actually draws more water out of the bloodstream and into the gut, potentially worsening the diarrhea. For medical-grade recovery from hypovolemia, use an isotonic Oral Rehydration Solution (ORS) that utilizes the sodium-glucose co-transport system for optimal cellular absorption.
When should I seek emergency medical care for viral gastroenteritis symptoms?
Seek immediate intervention if you observe ‘red flag’ symptoms such as hematemesis (blood in vomit), bloody stools, or signs of profound hypovolemia. These signs include a complete lack of urination for over eight hours, extreme dizziness upon standing, sunken eyes, or sudden mental confusion. These symptoms indicate that home rehydration has failed and intravenous (IV) fluids are likely required.
Does the annual flu shot provide any protection against norovirus?
No. The annual influenza vaccine is specifically engineered to target respiratory strains of the Influenza A and B viruses. Because norovirus belongs to an entirely different family of enteric pathogens, there is no cross-protection. While researchers are currently exploring mRNA-based vaccines for norovirus, none are currently available to the general public.
Should I take over-the-counter antidiarrheal medication for a stomach bug?
In most clinical settings, we advise against using antidiarrheals during the first 48 hours of a viral infection. Diarrhea is the body’s natural defense mechanism to flush enteric pathogens out of the system. Artificially stopping this process can trap the active virus inside the gut, potentially prolonging the infection and the contagious period. However, prescription antiemetics like Zofran may be used to help patients tolerate fluids.
What is the recommended dietary transition after the vomiting stops?
Once you have successfully tolerated small sips of an isotonic solution for several hours, we recommend the BRAT diet (Bananas, Rice, Applesauce, and Toast). These foods are low in fiber and easy on the inflamed gastric mucosa. It is critical to avoid dairy products for several days, as viral infections temporarily strip the gut of the lactase enzyme, leading to secondary lactose intolerance and recurrent bloating.
Why do I have lingering stomach issues weeks after a norovirus infection?
You may be experiencing Post-Infectious Irritable Bowel Syndrome (PI-IBS). Severe viral gastroenteritis can cause a massive disruption of the gut microbiome, flushing out beneficial bacteria and leaving the intestinal lining hypersensitive. To restore balance, I often recommend a high-quality probiotic containing Lactobacillus and Bifidobacterium strains to help repopulate the gut flora.
Disclaimer
This article is for informational purposes only and does not constitute formal medical advice. The distinction between diarrhea flu or norovirus can be complex, and symptoms may vary by individual. Always consult a qualified healthcare professional or seek emergency services if you experience signs of severe dehydration, high fever, or bloody stools.
References
- Centers for Disease Control and Prevention (CDC) – Norovirus Overview – Comprehensive data on annual US cases, transmission dynamics, and prevention protocols.
- World Health Organization (WHO) – The Treatment of Diarrhea – Clinical guidelines on Oral Rehydration Therapy (ORT) and the sodium-glucose co-transport system.
- Journal of Clinical Virology – “Pathophysiology of Viral Gastroenteritis” – Peer-reviewed research on how enteric pathogens damage the gastric mucosa and microvilli.
- Mayo Clinic – Influenza (Flu) Diagnosis – Expert insights into respiratory vs. gastrointestinal manifestations of Type A and B influenza.
- National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) – Viral Gastroenteritis (Stomach Flu) – Official data on viral shedding periods and dietary management (BRAT diet).
- Infectious Diseases Society of America (IDSA) – Clinical Practice Guidelines – Professional standards for differentiating respiratory pathogens from enteric viruses in clinical settings.