Introduction
| Quick Answer: A healthy adult over 110 lbs can safely have up to 10 vials drawn in one visit, about 85 mL or under 3 fl oz. That’s less than 2% of total blood volume, and well below the FDA’s 550 mL / 8-week safety cap. Tube count varies: a CBC needs 1 vial, a CMP needs 1, and a full annual physical runs 3 to 5 vials total. |
| At a Glance One standard US vial holds 2 to 10 mL of blood, with 8.5 mL being the most common10 vials equals about 85 mL, well under 2% of your total blood volumeFDA research limit for healthy adults over 110 lbs is 550 mL in any 8 weeksA CBC takes 1 vial, a CMP takes 1, a lipid panel takes 1, a thyroid panel takes 1Anyone under 110 lbs follows the stricter 10.5 mL per kg rulePlasma returns to normal in 24 to 48 hours; red cells take 4 to 6 weeks |
Eight tubes on a tray. The phlebotomist lines them up like ammunition. You’re sitting in the chair and your brain does the math it always does: that can’t be normal, can it?
Table of Contents
It’s the single most common anxiety inside any US lab, and the answer almost nobody takes two minutes to explain. Your body holds 4.5 to 5.7 liters of blood. A scary-looking 10-tube draw takes out less than the volume of a shot glass. Your circulatory system doesn’t flinch.
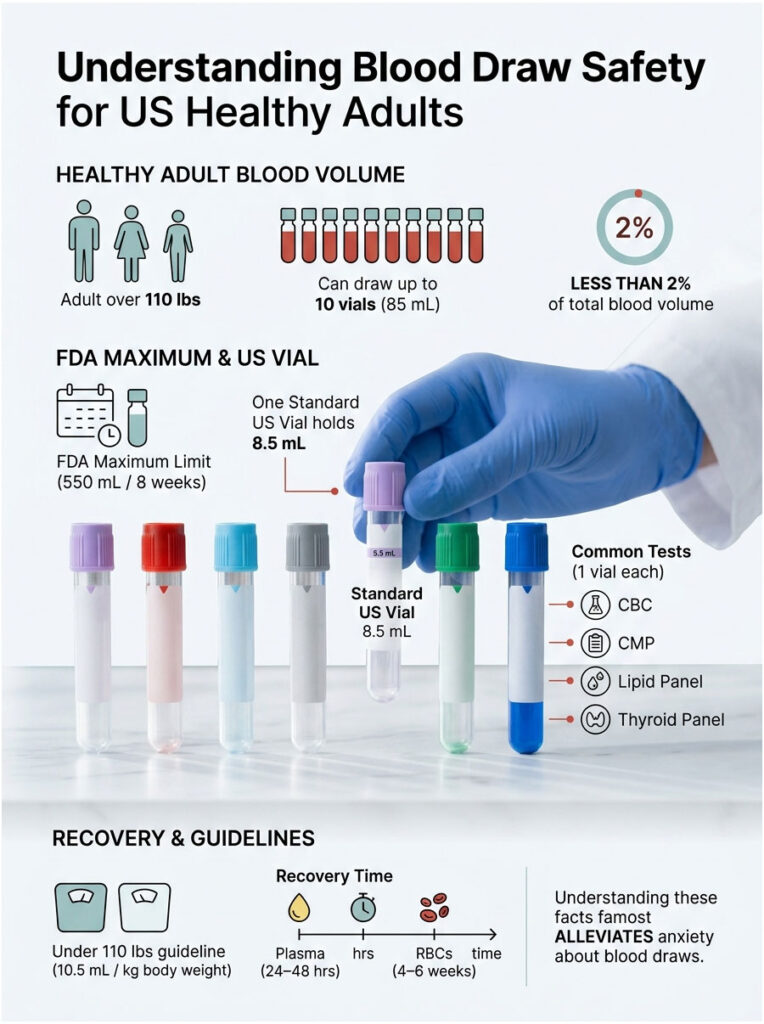
The problem is that most articles you’ll find either stop at that reassurance or bury it in clinical jargon. This one goes further. You’ll get real numbers, the exact vial count for every common US lab test, a weight-based safety chart in pounds, and the specific rules the FDA and major US hospitals actually enforce. By the end you’ll know exactly where your draw sits on the safety spectrum and what, if anything, is worth raising with your doctor.
Let’s get into it.
What Counts as Too Many Vials? The Real Answer
The first thing that trips people up is the idea that vials are the unit of risk. They aren’t. Total blood volume drawn, measured in milliliters, is what matters.
A phlebotomist could hand you a tray of 12 tubes and draw less blood than a single pediatric draw, depending on tube sizes. So when someone asks “is 10 vials too much,” the honest answer starts with “it depends on tube size and body weight.”
The Number That Actually Matters: Total mL Drawn
Every major US clinical guideline lands on the same rule. A safe single-session draw for a healthy adult is a percentage of total blood volume, not a fixed tube count. Standard practice stays below 10% of blood volume in any single session, and well below that for routine outpatient labs.
For an average 150-pound American, total blood volume is around 5,200 mL. Ten percent would be 520 mL. A typical annual physical draws about 30 mL. That’s 0.6% of your blood volume, an amount your body replaces while you finish your coffee.
The FDA’s 550 mL Rule (The One Every Lab Follows)
The anchor regulation here is FDA Title 21 CFR 46.110, which sets the expedited-review threshold for research blood draws. The rule is clear: healthy adults weighing 110 lbs or more can safely have up to 550 mL drawn over any 8-week period, with no more than two collections per week.
That 550 mL figure is the benchmark everyone follows. Clinical labs, hospitals, research studies, and employer wellness programs all operate well inside it. If your doctor ordered 10 vials, you’re looking at roughly 85 mL, or about 16% of the 8-week federal ceiling. You could have that same draw three more times within two months and still be under the safety threshold.
How Your Lab Draw Compares to a Blood Donation
Here’s the comparison that calms most patients down. When you donate a pint through the American Red Cross, the draw is 470 mL in about 10 minutes. That single donation is roughly 5.5 times the volume of a full 10-vial lab draw.
The Red Cross lets healthy adults donate every 56 days. Your body handles it. A lab draw is a fraction of that volume, collected for a fraction of the time. Pulling this comparison up is the single fastest way I’ve found to reset patient expectations.
How Much Blood Is Actually in One Vial?
The tube on the tray is called a vacutainer. It’s a small glass or plastic cylinder with a rubber stopper and a built-in vacuum that pulls blood in the moment the needle pierces the cap. Becton Dickinson, the primary US manufacturer, makes them in sizes from 2 mL up to 10 mL.
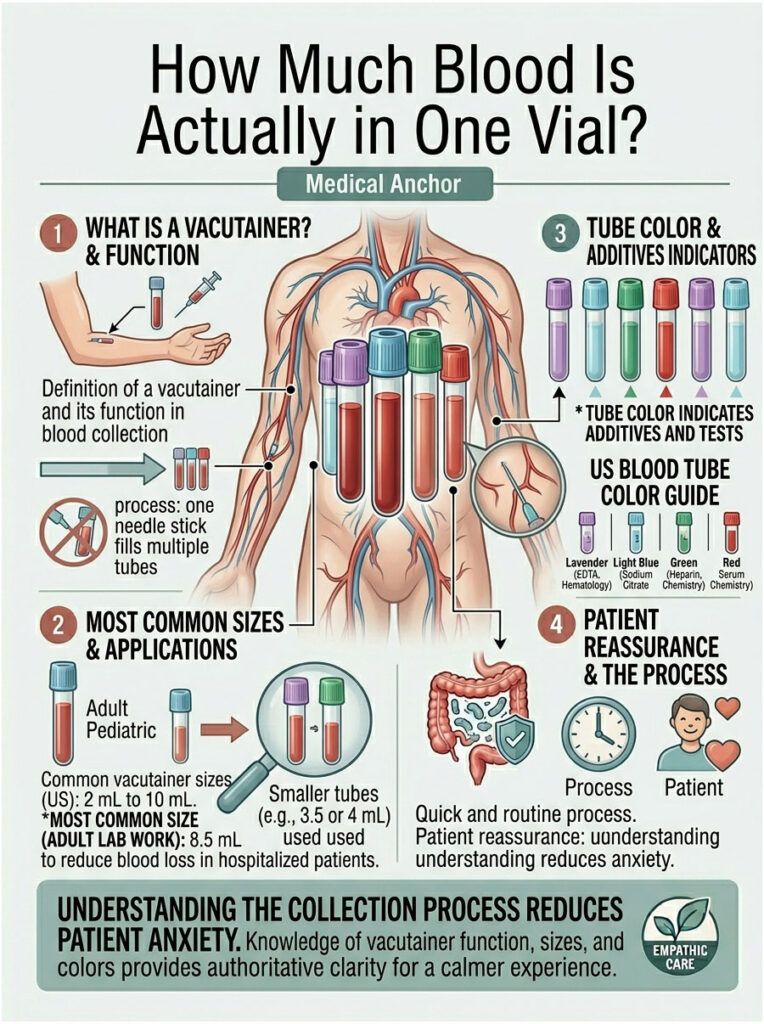
The most common size for adult lab work in the US is 8.5 mL. Labs increasingly use smaller 3.5 or 4 mL tubes for routine tests to reduce cumulative blood loss in hospitalized patients.
Standard US Tube Sizes (BD Vacutainer Range)
- 2 mL for coagulation studies in small-volume situations
- 3.5 to 4 mL for most routine chemistry and hematology tests
- 6 mL for trace element and hormone panels
- 8.5 mL for standard serum tests and most adult draws
- 10 mL for blood cultures and large-volume workups
- 0.25 to 0.5 mL pediatric microtainers for infants and young children
What Each Tube Color Means
The colored cap tells the lab two things: what additive is inside and which tests the tube is for. Mixing tests in the wrong tube ruins results, which is the real reason your doctor orders multiple tubes even when total blood volume is tiny.
Table 1: US Blood Tube Color Guide (Core Comparison)
| Tube Cap Color | Additive Inside | Typical Volume | Tests It Is Used For |
| Lavender (Purple) | EDTA | 2 to 6 mL | CBC, HbA1c, ESR, blood typing |
| Red or Gold (SST) | Clot activator plus gel | 3.5 to 8.5 mL | CMP, lipid panel, LFT, thyroid, vitamin D, B12 |
| Light Blue | Sodium citrate | 2.7 to 4.5 mL | PT, INR, aPTT (coagulation) |
| Gray | Sodium fluoride | 2 to 4 mL | Fasting glucose, glucose tolerance test |
| Green | Lithium or sodium heparin | 4 to 6 mL | Ammonia, cortisol, chromosome studies |
| Royal Blue | Trace-element free | 6 mL | Zinc, copper, heavy metals, toxicology |
| Yellow (ACD) | Acid citrate dextrose | 8.5 mL | HLA typing, DNA, paternity testing |
| Black | Sodium citrate (ESR-specific) | 1.8 mL | Westergren ESR |
Why One Stick Fills Multiple Tubes
This catches most patients off guard. You get poked once, and the phlebotomist swaps in five or six tubes one after another. That single needle-stick is pulling blood into a shared collection system, splitting it into separate tubes with different additives.
I’ve watched patients visibly relax the second they understand this. One puncture. Several tubes. Not several pokes. The tray looks intimidating, but your vein only feels one needle.
How Many Vials for Each US Lab Test? The Complete Chart
This is the question every Reddit thread and Quora post circles back to, and somehow no ranking article answers it cleanly. Here’s the breakdown based on what CLIA-certified US labs actually draw.
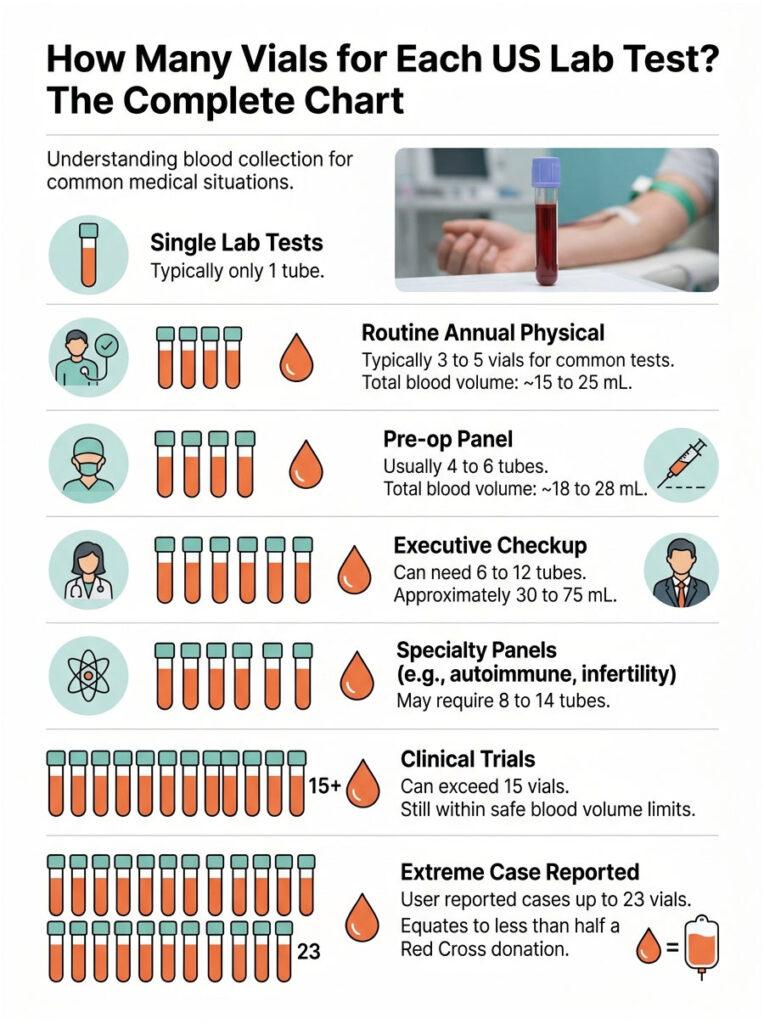
Individual Lab Tests
Most single tests need exactly one tube. That’s the part that surprises people.
- Complete Blood Count (CBC): 1 lavender tube, 3 to 4 mL
- Comprehensive Metabolic Panel (CMP): 1 red or gold SST tube, 3.5 to 5 mL
- Basic Metabolic Panel (BMP): 1 SST tube, 3 to 5 mL
- Lipid Panel (Cholesterol): 1 SST tube, 3 to 5 mL
- Liver Function Test (LFT): 1 SST tube, 3 to 5 mL
- Thyroid Profile (TSH, T3, T4): 1 SST tube, 3 to 5 mL
- HbA1c (Diabetes monitoring): 1 lavender tube, 2 to 3 mL
- Fasting Blood Sugar: 1 gray tube, 2 mL
- Vitamin D (25-OH): 1 SST tube, 3 mL
- Vitamin B12: 1 SST tube, 3 mL
- Iron Studies (Ferritin, TIBC): 1 SST tube, 3 to 5 mL
- PSA (Prostate screening): 1 SST tube, 3 mL
- Coagulation (PT / INR): 1 light-blue tube, 3 mL
- Blood Culture: 2 bottles (aerobic plus anaerobic), 8 to 10 mL each
The Annual Physical: 3 to 5 Vials, Here’s Why
If you’re heading in for a routine annual physical in the US, your doctor will usually order four tests: CBC, CMP, lipid panel, and TSH. That’s 3 to 4 tubes. Add HbA1c if you’re over 45 or have diabetes risk factors, and you’re at 4 to 5 tubes. Total blood volume: roughly 15 to 25 mL, about a tablespoon and a half.
Every major US health system uses essentially the same panel. Your physical isn’t a scary draw. It’s one of the smallest you’ll ever have.
Pre-Op or Pre-Surgery Panel
Surgery prep workups typically add coagulation testing and a type-and-screen to the standard panel. That means 4 to 6 tubes total:
- CBC (1 lavender)
- CMP (1 SST)
- Coagulation PT/INR (1 blue)
- Type and screen (1 or 2 lavender)
- Occasionally a pregnancy test for women of childbearing age (1 SST)
Total blood volume: 18 to 28 mL. Still well under a single tablespoon of body volume.
Executive Checkup or Wellness Profile
This is where the vial count climbs. Comprehensive wellness panels marketed by Quest Diagnostics, LabCorp, and direct-to-consumer services like Quest Health or Function Health usually include 50 to 100 biomarkers. That translates to 6 to 10 tubes, roughly 30 to 60 mL of blood.
Premium executive packages that add hormones, advanced cardiac markers (like ApoB and Lp(a)), cancer screening markers (PSA, CA-125, CEA), and heavy metal testing can reach 10 to 12 tubes, around 50 to 75 mL. Still inside the FDA safety envelope for a healthy adult.
Specialty Panels
Certain diagnostic workups are genuinely tube-heavy. Autoimmune panels hit 8 to 12 tubes. Infertility workups often land at 10 to 14. Clinical trial enrollment draws can exceed 15 vials when baseline pharmacokinetic testing is required. One patient support forum user reported 23 vials in a single session, which sounds extreme but still equals only about 195 mL, less than half a Red Cross donation.
Safe Blood Draw Limits by Body Weight (US Pounds Chart)
The up-to-10-vials rule assumes you’re an average-weight adult. If you weigh 110 lbs, the math changes. If you weigh 250 lbs, it changes in the other direction. This is the part every competitor article skips.

The 10.5 mL per kg / 8-Week Rule in Plain English
US IRB guidelines for adult research draws set a clear ceiling: no more than 10.5 mL of blood per kilogram of body weight over any 8-week window, and no more than 550 mL total. A single session should stay under 1% of body weight in grams.
In pounds, converted for US readers:
Table 2: Safe Blood Draw Limits by Body Weight (US)
| Your Weight | Single-Session Safe Max | 8-Week Safe Max | Typical Vial Equivalent |
| 90 lbs (41 kg) | ~40 mL | ~430 mL | 5 standard vials |
| 110 lbs (50 kg) | ~50 mL | ~525 mL | 6 standard vials |
| 130 lbs (59 kg) | ~60 mL | 550 mL (FDA cap) | 7 standard vials |
| 150 lbs (68 kg) | ~70 mL | 550 mL (FDA cap) | 8 standard vials |
| 180 lbs (82 kg) | ~85 mL | 550 mL (FDA cap) | 10 standard vials |
| 210 lbs (95 kg) | ~95 mL | 550 mL (FDA cap) | 11 standard vials |
| 250+ lbs (113+ kg) | ~100 to 120 mL | 550 mL (FDA cap) | 12 to 14 standard vials |
Source: FDA 21 CFR 46.110 and NIH Clinical Center Phlebotomy Guidelines
The 8-week cap plateaus at 550 mL regardless of body weight. That’s the federal ceiling for healthy adults. Weight only changes what’s safe in a single session.
Children and Teens
Pediatric limits are far stricter because a child’s total blood volume is smaller. The standard used by the NIH Clinical Center and every US pediatric IRB:
- Maximum per draw: 2.4 mL per kg of body weight
- Maximum per month: 3% of total blood volume, or 50 mL, whichever is smaller
- Never more than two venipuncture attempts per draw
For a 40-pound (18 kg) child, that’s roughly 43 mL per draw and about 30 mL per month, enforced more conservatively in practice.
Adults Over 65
Age slows bone marrow regeneration. Older adults often have lower iron stores and slower red cell recovery. Most US physicians informally cap routine draws at 6 to 8 tubes for patients over 65 and recommend extra hydration before the appointment.
In my experience, the labs I’ve trained with always ask weight and age before an executive-panel draw for an older patient. If iron or hemoglobin came back low on a previous visit, they split the workup across two appointments.
Pregnant and Postpartum Women
Pregnancy increases blood volume by 30 to 50%, so the absolute safety margin actually goes up. But iron demand also skyrockets, and many pregnant women are already marginally iron-deficient. Most obstetricians prefer to space multi-tube draws across prenatal visits rather than stack everything in one session.
Postpartum, the picture flips. Blood loss at delivery, ongoing postpartum bleeding, and the demands of recovery mean OBs often limit draws to essential tests only for the first 6 to 8 weeks.
If You’re Already Anemic or Have Low Iron
If your most recent hemoglobin was under 11 g/dL (women) or 13 g/dL (men), most US physicians scale back the draw. Typical approach:
- Cap the session at 3 to 5 tubes
- Split remaining tests to a follow-up visit
- Prescribe or recommend iron supplementation before the next draw
- Use smaller-volume (3.5 mL) tubes instead of 8.5 mL
It’s completely reasonable to ask your phlebotomist if they can use pediatric tubes for your draw. Most can, and they often will if you explain why.
What 10 Vials Really Looks Like (And Why You Won’t Notice)
Numbers on a page feel abstract. Here’s what 85 mL actually is in terms you’ve handled with your own hands.

- In fluid ounces: 2.87 fl oz, barely more than a shot and a half
- Compared to a 12 oz soda can: Less than one quarter of the can
- Compared to a Starbucks tall coffee (12 oz): About one quarter
- Compared to a standard Red Cross donation (470 mL): About 18% of a single pint
- Compared to an average menstrual period (30 to 80 mL over 5 days): Roughly one period’s worth
- Compared to total blood volume (5,200 mL average): 1.6%
Your body replaces the fluid portion of that 85 mL in 24 to 48 hours, purely through drinking water and normal hydration. You will not feel it unless you were already dehydrated, fasting for 14 hours, or running on no sleep.
Side Effects After Multiple Vials (What’s Normal, What Isn’t)
Most people walk out of a blood draw feeling completely fine. A minority feel something mild. A very small group experience something worth reporting. Knowing which category you’re in is half the battle.
Normal (No Action Needed)
- A small bruise or tender spot at the needle site for 1 to 3 days
- Mild lightheadedness, especially if you were fasting
- Tiredness for a few hours
- Nervousness or a shaky feeling immediately after the draw
I’ve seen post-draw dizziness resolve within two minutes of a patient lying down with their feet elevated. It’s almost always vasovagal response, not blood loss.
Pay Attention
- A large or expanding bruise (hematoma) at the puncture site
- Actually fainting during or after the draw
- Tingling or numbness in the arm that doesn’t resolve within a day
- Bleeding that continues after 10 minutes of direct pressure
Any of these is worth mentioning to the phlebotomist before you leave the lab. None are emergencies by themselves.
Call Your Doctor
- Severe or sharp arm pain radiating from the puncture site
- Redness, warmth, pus, or swelling at the needle site after 24 hours (possible infection)
- Dizziness, heart palpitations, or extreme fatigue lasting more than 48 hours
- Shortness of breath
- Signs of severe anemia after a large draw (pale skin, rapid heartbeat, weakness)
When It Signals Iatrogenic Anemia
Here’s a nuance rarely covered in patient guides. In hospital settings (not outpatient labs) repeated daily blood draws can add up to clinically significant blood loss. This is called iatrogenic anemia or hospital-acquired anemia.
A 2023 JAMA study by Siegal et al. found that switching ICU patients to small-volume blood collection tubes reduced red blood cell transfusion needs by roughly 10 transfusions per 100 critical care patients. The average hospital patient loses around 22 mL of blood per day just from lab testing. Over a two-week ICU stay, that’s 300+ mL, roughly a donation-sized loss.
None of this applies to your routine outpatient draw. But it’s worth knowing if you or a family member ends up admitted. It’s reasonable to ask the attending physician whether small-volume tubes are being used.
How Fast Your Body Replaces Blood After a Draw
Recovery happens in stages. Different blood components rebuild at different speeds.
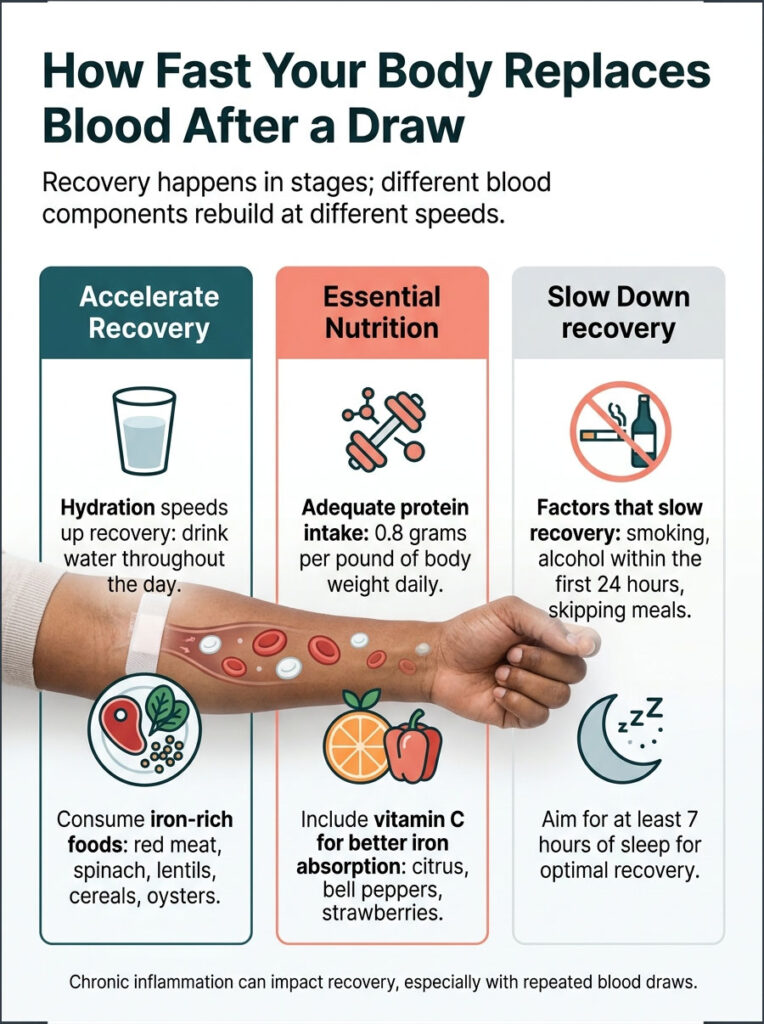
- Plasma (the fluid portion): 24 to 48 hours, just from normal hydration
- Platelets: About 72 hours
- White blood cells: A few days
- Red blood cells: 4 to 6 weeks
- Iron stores: 6 to 8 weeks, faster if your diet supports it
What speeds it up: drinking water throughout the day, iron-rich foods (red meat, spinach, lentils, fortified cereals, oysters), adequate protein (0.8 grams per pound of body weight daily), vitamin C to help iron absorption (citrus, bell peppers, strawberries), and at least 7 hours of sleep.
What slows it down: smoking, alcohol within the first 24 hours, skipping meals, and chronic inflammation. None of these are dealbreakers for a routine draw, but they matter if you’re having repeated blood work over weeks.
Scenario-Based Decisions: Your Situation, Your Next Steps
Most blood draw anxiety comes from not knowing whether your specific situation is normal. Here’s a quick-reference matrix.

Table 3: Your Scenario to Recommended Action
| Your Scenario | What’s Usually Happening | What to Do |
| Six tubes for your annual physical | Standard CBC, CMP, lipid, TSH, HbA1c plus a spare | Nothing. Eat a snack after, drink water |
| 10+ vials for a workup | Autoimmune, hormone, or specialty diagnostic panel | Normal. Ask for small-volume tubes if concerned |
| Under 110 lbs and they want 8 tubes | Order not adjusted for body weight | Ask for 3.5 mL tubes instead of 8.5 mL |
| Anemic and they ordered a full panel | Labs may not cross-reference your last hemoglobin | Mention your anemia. Ask to split across two visits |
| Fainted last time and they want 10 tubes | Vasovagal history not flagged | Request to lie flat. Eat protein 30 minutes before |
| 12 tubes drawn, tired the next day | Normal fluid loss plus stress | Drink 2 to 3 liters of water. Resolves in 24 to 48 hours |
| Pregnant and they want 8 tubes | Prenatal workup, usually split by trimester | Confirm with OB whether tests can be staggered |
| Your kid is having 4 tubes drawn | Pediatric workup; should use microtainers | Ask what tube size is being used. Microtainers hold 0.5 mL |
Pro Tips from Working in Phlebotomy
A few things I only learned after years around labs, worth their weight in gold.
Hydrate 2 hours before, not 20 minutes before. Drinking water on your way to the appointment doesn’t fill your veins in time. Your kidneys need time to circulate it. A full glass two hours before, then another 30 minutes before, makes the stick easier and reduces lightheadedness.
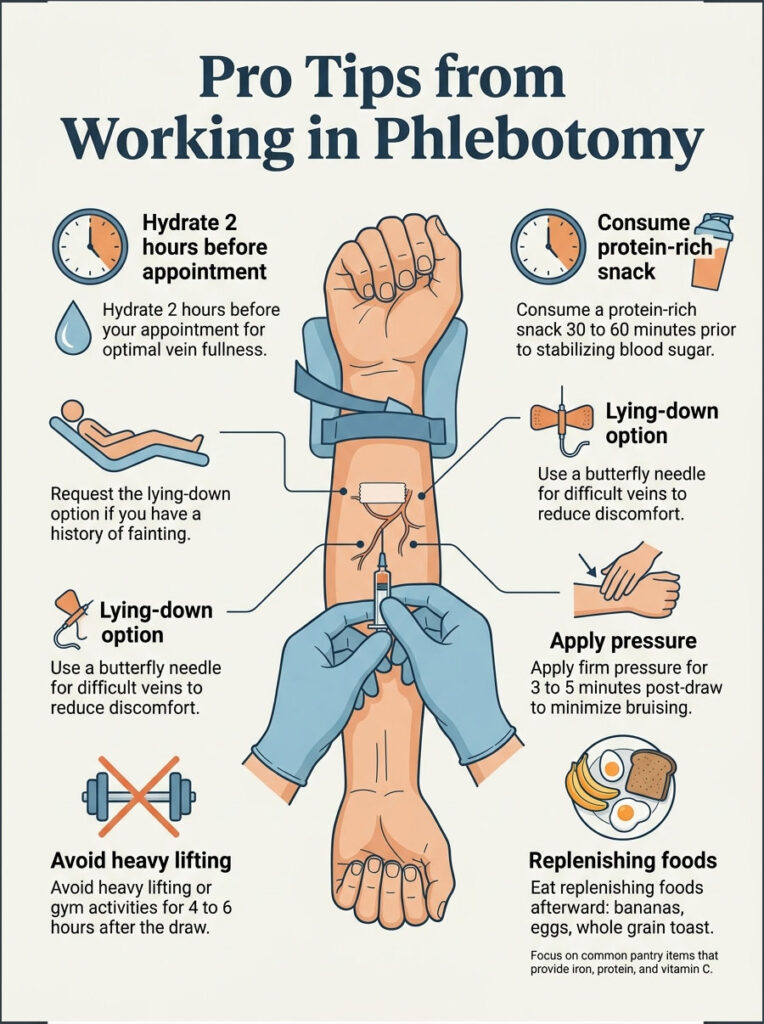
Eat something with protein 30 to 60 minutes before, unless you’re fasting for the test. Eggs, Greek yogurt, peanut butter on toast, a handful of almonds. Protein stabilizes blood sugar and prevents the vasovagal drop that causes most post-draw fainting.
Ask for the lying-down option if you’ve ever felt faint. Every accredited US lab has a recliner or draw bed. Using it isn’t weakness. It’s the single most effective tool for preventing vasovagal syncope.
Watch for the butterfly needle if your veins are difficult. A butterfly needle is smaller (23-gauge vs 21) and gentler on fragile or rolling veins. If the phlebotomist struggles to find your vein, ask if a butterfly is available.
Apply pressure for 3 to 5 minutes after, not 30 seconds. Most bruising happens because people lift the bandage too early. Hold firm pressure, then leave the bandage on for at least an hour.
Skip heavy lifting or the gym for 4 to 6 hours. Using the arm right away can cause the puncture site to reopen or bruise. Your body recovers quickly, but the tiny vein puncture takes an hour or two to seal.
What to eat afterward, using a US pantry. A banana and a glass of orange juice rebuild fluid and potassium. Scrambled eggs and fortified toast hit iron and protein. Peanut butter on whole wheat, a bowl of Cheerios, a turkey sandwich. Nothing exotic. Just real food with iron, protein, and vitamin C.
Summary: Your Blood Draw Action Plan
Here’s the whole thing compressed into five steps.
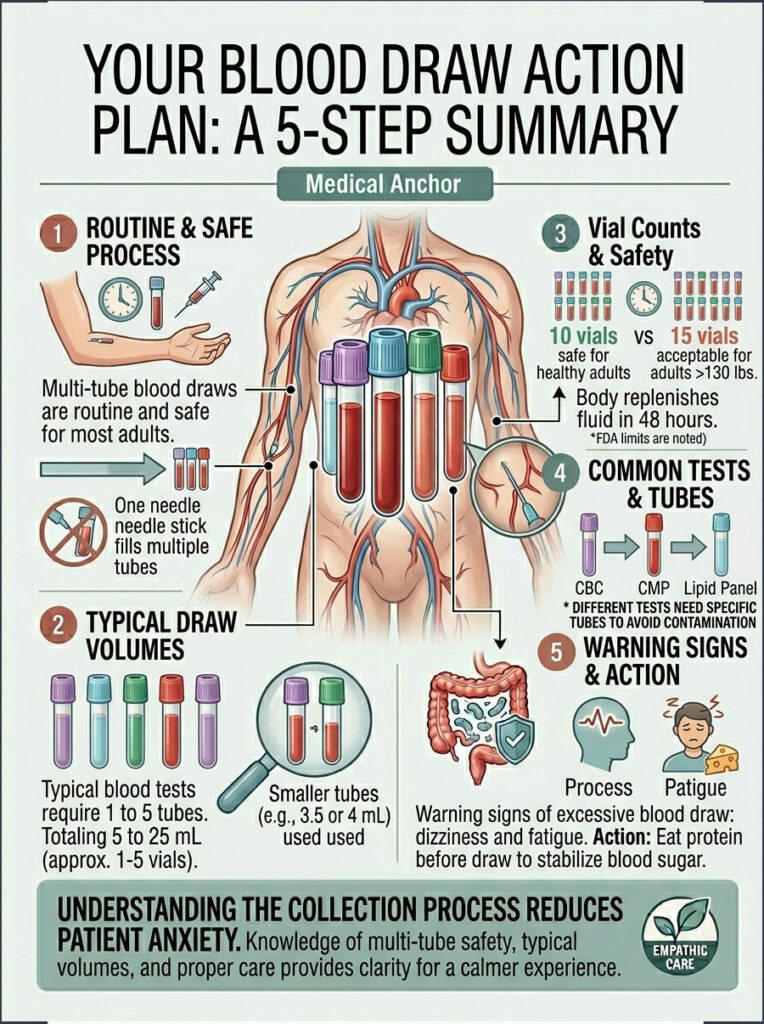
- Check the order. Ask which tests your doctor ordered and how many tubes they translate to. You have every right to know.
- Hydrate and eat unless you’re fasting for the test. Water 2 hours before, small protein snack 30 minutes before.
- Speak up about your history. Fainting, anemia, low body weight, pregnancy, or repeat draws all justify adjustments. A good phlebotomist welcomes the heads-up.
- Lie down if it helps. It’s the simplest defense against vasovagal response, and it’s your right to request.
- Refuel after. Water, protein, iron-rich food, and an hour of light activity before you hit the gym.
For the vast majority of Americans, multi-tube draws are routine, safe, and completely within FDA and NIH safety limits. The number of tubes on the tray is a logistics detail, not a risk signal. Your body handles it.
Frequently Asked Questions
How many vials of blood do they take for a regular blood test?
Most routine US lab visits involve 1 to 5 tubes, totaling 5 to 25 mL of blood. A simple fasting glucose check takes 1 vial. An annual physical with CBC, CMP, lipid panel, and thyroid usually takes 3 to 5 vials. Anything more typically means a comprehensive wellness profile or a specialty diagnostic workup.
Is 10 vials of blood too much?
No. For a healthy adult over 110 pounds, 10 vials equals roughly 85 mL, about 1.6% of your total blood volume and well below the FDA’s 550 mL / 8-week safety ceiling. Your body replaces the fluid within 48 hours. Unless you’re underweight, anemic, or pediatric, 10 vials is medically routine.
How many vials of blood are taken for a CBC?
One lavender-capped EDTA tube holding 3 to 4 mL. That’s it. The CBC is one of the simplest draws in US laboratory medicine. Every result on your report (red cells, white cells, platelets, hemoglobin, hematocrit) comes from that single tube.
How many vials of blood are taken for a CMP?
One red or gold SST tube holding 3.5 to 5 mL. The Comprehensive Metabolic Panel runs 14 tests (glucose, kidney function, liver enzymes, electrolytes, proteins) all from one tube. Your insurance codes this as CPT 80053, a single-tube billing code.
How many vials for a lipid panel?
One red or gold SST tube, 3 to 5 mL. The standard lipid panel (total cholesterol, LDL, HDL, triglycerides) fits in one serum-separator tube. Most labs combine it with your CMP draw if both are ordered, using the same tube.
How many vials of blood for an annual physical?
Typically 3 to 5 vials for most US adults. A standard physical includes CBC (1 tube), CMP (1 tube), lipid panel (1 tube), and thyroid (1 tube). Adults over 45 or those with diabetes risk factors usually get an HbA1c as a fifth tube. Total volume: 15 to 25 mL.
Is 15 vials of blood too much to draw at once?
For a healthy adult over 130 pounds, no. Fifteen vials equals about 130 mL, still less than 3% of total blood volume and well under the FDA’s 8-week cap. Patients with lupus, autoimmune conditions, or infertility workups routinely receive 15 or more vials in one session safely.
Why do they need so many vials for one blood test?
Different tests require different chemical additives in the tube. Mixing anticoagulant tubes with serum-separator tubes would ruin results. Each colored cap represents a specific preservative. Labs also keep a small reserve in case a test needs to be repeated for quality control.
Can taking too much blood during testing make me anemic?
A single outpatient draw (even 15 vials) won’t cause anemia in a healthy adult. Repeated daily hospital draws can add up to clinically significant loss, a condition called iatrogenic anemia. A 2023 JAMA study found low-volume tubes prevent about 10 transfusions per 100 ICU patients. Routine outpatient labs don’t pose this risk.
How long does it take your body to replace blood after a draw?
Plasma (the fluid portion) returns to normal within 24 to 48 hours. Platelets rebuild in about 72 hours. White blood cells bounce back in a few days. Red blood cells take 4 to 6 weeks. Iron stores take 6 to 8 weeks, faster with an iron-rich diet and vitamin C.
How do I know if too much blood was taken?
Warning signs include severe or prolonged dizziness, heart palpitations, extreme fatigue lasting more than 48 hours, shortness of breath, or pale skin with rapid heartbeat. These are rare after outpatient draws. If any of them hit, contact your doctor. Mild tiredness or brief lightheadedness is normal and not a concern.
Should I eat before a blood draw with multiple vials?
Yes, unless your specific test requires fasting (glucose, lipid panel, some liver tests). Eating protein 30 to 60 minutes before stabilizes blood sugar and reduces the risk of post-draw lightheadedness. If fasting is required, hydrate with water and schedule the draw for early morning so you can eat right after.
Disclaimer
| This article is for educational purposes only and is not a substitute for professional medical advice. Always consult your healthcare provider for personalized diagnosis and treatment. If you have concerns about a specific blood draw, speak with your physician or phlebotomist directly. |
References
- FDA Title 21 CFR 46.110: Expedited Review Categories
- American Red Cross: Blood Donation Process
- NIH Clinical Center: Biospecimen and Blood Draw Guidelines
- JAMA 2023 Siegal et al.: Small-Volume Tubes and ICU Transfusion
- CDC NHANES Phlebotomy Procedures Manual
- Mayo Clinic: Blood Tests Overview
- Cleveland Clinic: Phlebotomy and Blood Draw
- College of American Pathologists (CAP) Laboratory Accreditation