Picture this. It’s mid-July in Houston, you’ve just finished a 90-minute spin class, and on the drive home you start to feel that familiar burn between your thighs. By Wednesday, there’s a red ring on your inner thigh that won’t quit. You’re not alone, and you’re not gross. You’ve got jock itch, and roughly 1 in 5 American adults will deal with it at some point in their lives.
Table of Contents
Quick Answer: Jock itch (tinea cruris) is a contagious fungal infection of the groin, inner thighs, and buttocks caused by dermatophyte fungi that thrive in warm, moist skin. Symptoms include a red or brown ring-shaped rash, itching, burning, and flaking. Most cases clear in 2 to 4 weeks with over-the-counter antifungal creams like terbinafine or butenafine, plus keeping the area dry and wearing loose, breathable clothing.
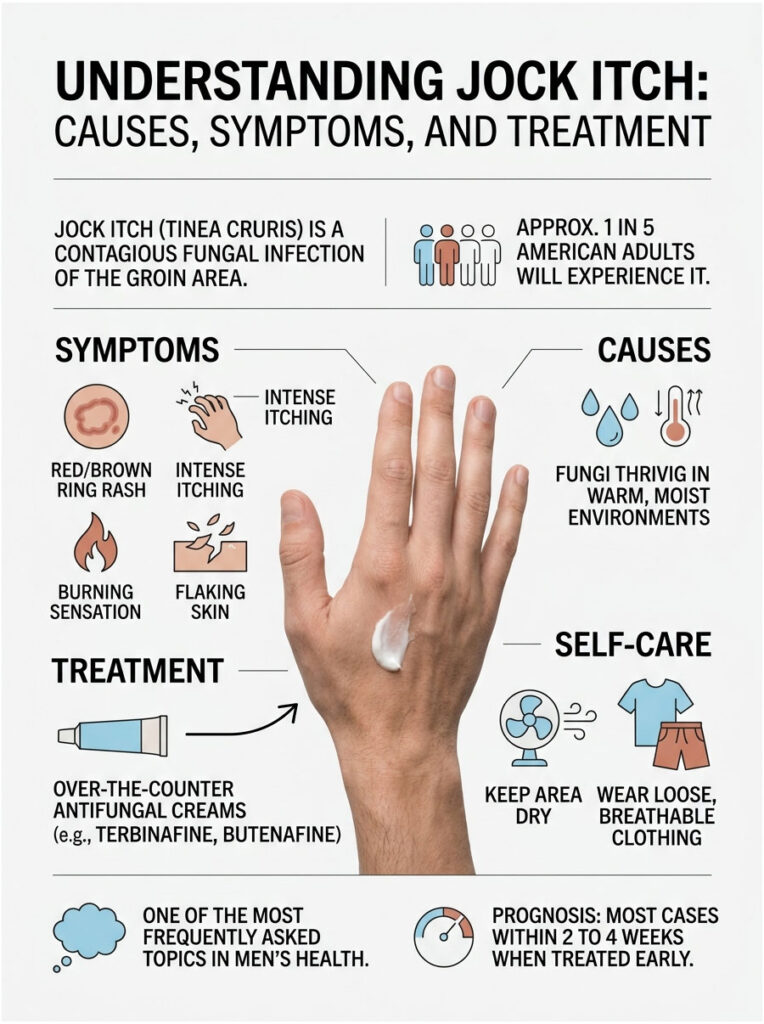
At a Glance
- Tinea cruris is the second most common dermatophyte infection in the world
- Trichophyton rubrum and Epidermophyton floccosum cause the vast majority of US cases
- Men are three times more likely than women to get jock itch
- Terbinafine creams clear most cases in 7 to 14 days
- Roughly half of cases recur within a year without lifestyle changes
- A drug-resistant strain (T. indotineae) is now spreading across US states
- See a doctor if symptoms haven’t improved after 2 weeks of OTC treatment
Patients calling HealthCareOnTime for skin and dermatology guidance ask about groin rashes more often than almost any other men’s health topic. The reassuring news: tinea cruris is common, treatable, and almost never serious when caught early. Read on for what’s actually causing your rash, what to put on it, and what to stop doing right now.
What Is Jock Itch? Tinea Cruris, Defined
Jock itch is the everyday name for tinea cruris, a superficial fungal infection of the skin in the groin folds, upper thighs, and buttocks. The word “tinea” refers to the fungus family responsible, and “cruris” comes from the Latin word for leg. These fungi feed on dead skin cells, hair, and nails, and they rarely reach below the top layer of skin.

The condition picked up its sporting nickname because athletes who sweat heavily and stay in damp gear were among the first groups studied with it. Today, anyone with a warm, moist skin fold can develop it, regardless of athletic ability or hygiene habits.
How Common Is Jock Itch in the USA
Tinea cruris is the second most common clinical presentation of dermatophyte infection globally, and US risk factors stack up fast. Marathon runners show 22 to 31 percent prevalence of tinea pedis, miners 21 to 72.9 percent, and soldiers 16.4 to 58 percent, and athlete’s foot is the single biggest gateway to a groin infection.
About 73 million Americans hold a gym membership, and the CDC reports adult obesity at 41.9 percent. The American population is sitting on top of every major risk factor at once. Patients booking telehealth dermatology appointments through HealthCareOnTime often describe symptoms that started after a single weekend tournament, business trip, or hot summer commute.
What Causes Jock Itch: The Real Triggers
Tinea cruris isn’t punishment for poor hygiene. It happens when fungi already living quietly on your skin (or transferred from another person) find the warm, damp conditions they need to multiply.
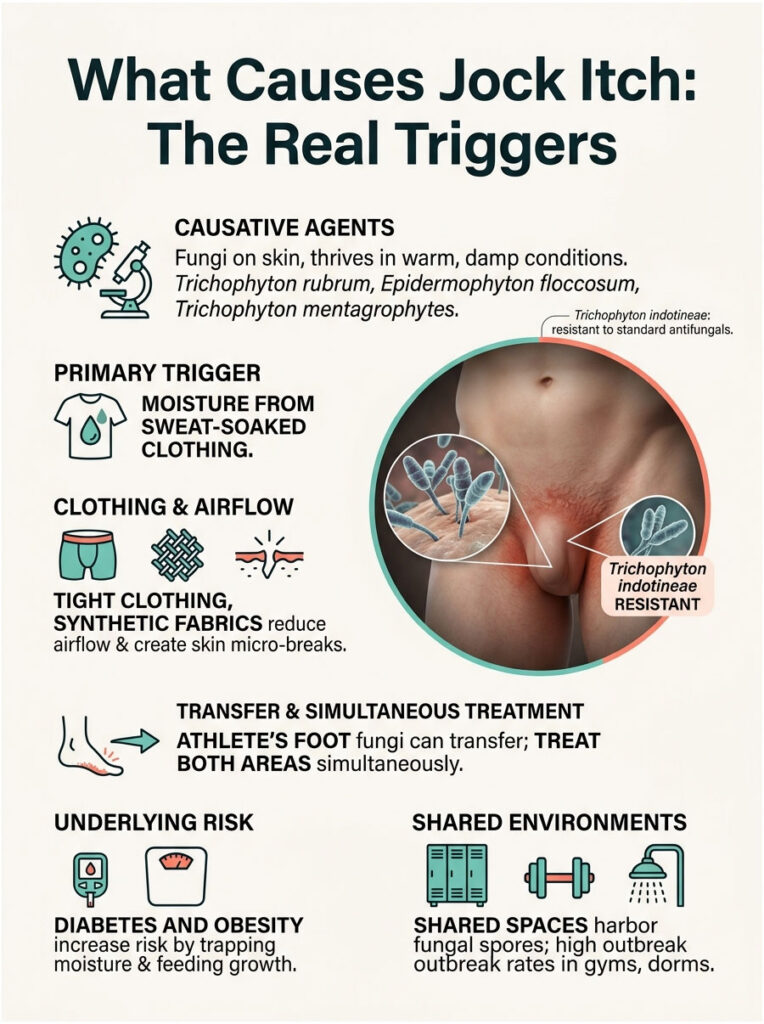
The Fungi Behind the Rash
Three organisms cause the bulk of US cases. Trichophyton rubrum leads the pack and is also the main culprit behind athlete’s foot. Epidermophyton floccosum is the classic groin-loving dermatophyte, often spread through shared towels and sports gear. Trichophyton mentagrophytes shows up less often but tends to produce more inflammation when it does.
A newer concern is Trichophyton indotineae, a strain first identified in southern Asia in 2014 that is now spreading worldwide, including across multiple US states. This strain often resists standard topical antifungals, which is one reason untreated cases are getting harder to clear.
Top 7 Risk Factors USA Adults Face
The number-one trigger is moisture. Skin trapped under sweat-soaked clothing for hours creates exactly the temperature and humidity dermatophytes need. A 90-minute lifting session followed by a 45-minute drive home in damp shorts is more than enough.
Tight clothing and synthetic fabrics tighten the screws further. Compression shorts, slim jeans, and polyester underwear all reduce airflow, and friction creates micro-breaks in the skin that fungi exploit. Cotton, modal, and bamboo allow the skin to dry, and many dermatologists recommend switching from briefs to boxers during active treatment.
Athlete’s foot transfer is the most overlooked cause of all. The same fungus that lives between your toes happily relocates to your groin when you pull your underwear up over fungus-coated feet. Treating both areas at the same time is usually necessary to stop reinfection.
Diabetes and obesity raise the risk in two ways. High blood sugar feeds fungal growth, and skin folds in larger body types trap moisture for longer. Patients seeking diabetic skin care guidance through our care network see this pattern repeatedly, especially in adults over 50.
Shared spaces add another layer. Gym benches, sauna seats, dirty towels, and unwashed athletic supporters can carry live fungal spores for weeks. College dorms, military training bases, and CrossFit gyms report some of the highest cluster outbreaks in the country.
A weakened immune system (from HIV, chemotherapy, immunosuppressants, or chronic stress) blunts the body’s response to fungal overgrowth. Recurrent or unusually widespread cases sometimes flag an underlying immune issue worth investigating.
Finally, US climate matters. If you live in Florida, Louisiana, Texas, Georgia, or anywhere along the Gulf Coast, you’re battling the weather itself. Urgent-care visits for groin rashes spike between June and September across the South.
Jock Itch Symptoms: How to Know You Have It
The classic case is hard to miss once you know what to look for. The infection usually starts as a small red patch high on one inner thigh and grows outward.
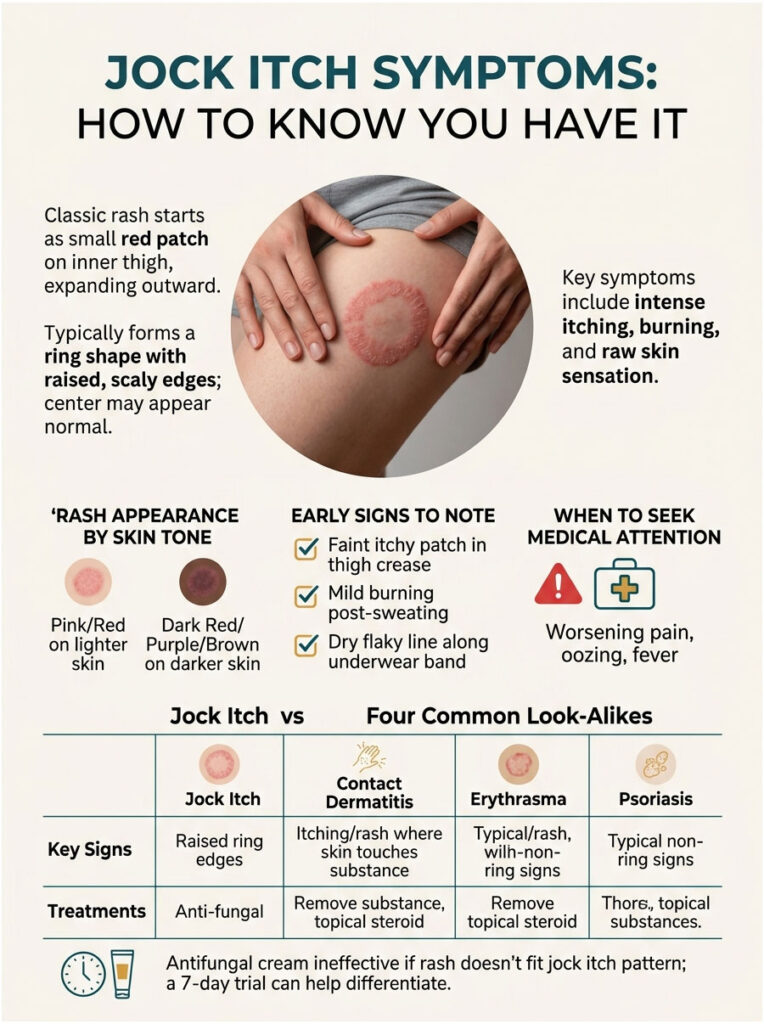
The Classic Rash Pattern
The rash typically forms a ring or half-moon shape with a clearly defined, slightly raised border. The center of the patch may look more normal than the edges, which can be scaly, bumpy, or peeling. Jock itch usually stays around the creases of the upper thigh and does not involve the scrotum or penis, which is one of the easier ways to tell it apart from other groin conditions. (Source: MedlinePlus)
Itching is the headline symptom. Burning, stinging, and a feeling of raw, rubbed skin show up alongside, especially after exercise or a hot shower.
How Symptoms Differ on Lighter vs Darker Skin Tones
On lighter skin tones, the rash usually appears pink or red. On darker skin tones, the rash can present as dark red, purple, brown, gray, or even tan. This difference matters because most medical reference photos still default to lighter skin examples, which delays self-recognition. In cases reviewed by our dermatology consultants, patients with darker complexions often arrive after weeks of being misdiagnosed with eczema or heat rash.
Early Signs You Shouldn’t Ignore
Catching tinea cruris early can shrink your treatment window from a month to a single week. Watch for a faint, slightly itchy patch in the crease where your thigh meets your hip, mild burning after sweating that doesn’t fully wash away, a dry flaky line along the underwear band area, or skin that feels warmer or thicker than the surrounding area.
If pure itching turns into real pain, oozing, blisters, fever, or rapid spreading, you may have a secondary bacterial infection on top of the fungus. That combination warrants a same-day call to a clinician.
Table 1: Jock Itch vs 4 Common Look-Alikes
| Condition | Cause | Typical Location | Key Sign | Standard Treatment |
| Jock itch (tinea cruris) | Dermatophyte fungus | Inner thighs, groin folds, buttocks; spares scrotum | Ring-shaped rash with raised, scaly edge | Topical antifungal (terbinafine, butenafine) for 1-2 weeks |
| Yeast infection (cutaneous candida) | Candida albicans | Skin folds, scrotum, vulva, under breasts | Bright red, satellite pustules at edges | Topical clotrimazole or nystatin |
| Inverse psoriasis | Autoimmune | Groin, armpits, under breasts | Smooth, shiny red plaques without scale | Topical steroids, calcineurin inhibitors |
| Eczema (intertrigo dermatitis) | Irritant or allergic | Any moist skin fold | Poorly defined edges, weeping, no ring shape | Barrier creams, low-potency steroids |
| Erythrasma | Bacterial (Corynebacterium minutissimum) | Groin, armpits | Coral-red glow under Wood’s lamp; no scale | Topical or oral erythromycin |
If your rash doesn’t fit the jock-itch pattern, antifungal cream alone won’t work. Patients commonly ask our care team how to tell these apart at home, and the safest answer is straightforward: if a 7-day antifungal trial doesn’t improve things, it’s probably not fungal.
Jock Itch in Men vs Women: What’s Different
The “jock” name has done women a disservice. Women absolutely get tinea cruris, and the way it shows up matters.

Why Men Are 3x More Likely
Tinea cruris is three times more common in men than in women, driven by anatomy (more skin-on-skin contact at the scrotal-thigh fold), higher rates of athlete’s foot, and clothing patterns that trap heat. Men also tend to delay treatment longer, partly out of embarrassment, which lets a 7-day OTC fix turn into a 4-week prescription job.
Female-Specific Presentation and Triggers
In women, the rash often appears under the abdominal fold, in the bikini-line area, or where the inner thigh meets the labia. Common triggers include tight workout leggings worn for long stretches, swimsuits left on after pool sessions, and wet menstrual products.
Pregnancy raises the risk because of natural shifts in skin moisture and immune function. Patients booking dermatology consults through HealthCareOnTime during pregnancy are routinely advised to confirm any antifungal choice with their OB-GYN before starting.
Pediatric and Adolescent Cases
Children rarely develop jock itch before puberty. Once teen sweat glands kick in, especially among athletes, the case rate climbs sharply. High-school wrestling and football teams report repeated outbreaks every season. Treatment in teens is almost identical to adults, with extra attention to washing all gym gear in hot water.
Fast Relief: How to Treat Jock Itch That Actually Works
For most cases, you can clear tinea cruris at home in two weeks or less. The key is choosing the right active ingredient and using it long enough.

OTC Antifungal Options Compared
Four active ingredients dominate the US pharmacy aisle. Terbinafine (sold as Lamisil AT) kills fungi by blocking squalene epoxidase and is the fastest-acting option. Butenafine (sold as Lotrimin Ultra) works through a similar mechanism with longer-lasting skin penetration. Clotrimazole (sold as Lotrimin AF and Mycelex) blocks ergosterol synthesis and is reliable but slower. Miconazole (Micatin, Desenex) offers broad-spectrum coverage including some bacteria.
Terbinafine and butenafine generally outperform azoles in head-to-head trials. Both butenafine and terbinafine achieved higher cure rates than other antifungal creams for treating athlete’s foot, jock itch, and ringworm in randomized controlled studies. (Source: Miiskin Dermatology)
How Long Until You See Results
Itching usually drops within 3 to 5 days of consistent application. Visible rash improvement follows by day 7. Full clearance takes 1 to 4 weeks depending on the active ingredient. Keep applying for at least 1 week after symptoms vanish to prevent rebound, which is the single biggest reason cases come back.
Prescription Options for Stubborn Cases
If 2 weeks of OTC treatment hasn’t worked, a clinician may prescribe topical econazole (Ecoza), oxiconazole (Oxistat), ciclopirox, or luliconazole. Oral options include terbinafine, fluconazole (Diflucan), and itraconazole (Sporanox).
Oral antifungals require liver function awareness, especially for adults already taking statins, blood thinners, or chronic medications. In tests booked through HealthCareOnTime, our reviewers regularly add a basic liver panel before initiating oral antifungal therapy in patients over 50.
Table 2: USA OTC Antifungal Comparison
| Active Ingredient | Common US Brand | Typical Cure Time | Average US Retail Price | Reported Cure Rate |
| Terbinafine 1% | Lamisil AT | 1 to 2 weeks | $12 to $18 (12g tube) | ~85 to 90% |
| Butenafine 1% | Lotrimin Ultra | 1 to 2 weeks | $14 to $20 (12g tube) | ~85 to 90% |
| Clotrimazole 1% | Lotrimin AF, Mycelex | 2 to 4 weeks | $6 to $12 (1 oz tube) | ~70 to 80% |
| Miconazole 2% | Micatin, Desenex | 2 to 4 weeks | $7 to $13 (cream/spray) | ~70 to 80% |
| Tolnaftate 1% | Tinactin | 2 to 4 weeks | $8 to $14 | ~65 to 75% |
Source: US News Health 2025 OTC rankings, Cleveland Clinic, Healthline, retail pricing across major US pharmacy chains.
Home Remedies: What Helps and What’s a Myth
The internet is loaded with home cures for jock itch. A few have modest evidence behind them. Most don’t deserve the attention they get.

Tea tree oil at 5 to 10 percent dilution shows mild antifungal action and works best alongside, not instead of, an antifungal cream. Apple cider vinegar diluted in water may reduce surface fungal load, though it burns broken skin and isn’t worth the discomfort for most people. Garlic extract topicals have limited but real lab evidence behind them and rarely justify the smell.
Some popular ideas are worse than useless. Petroleum jelly (Vaseline) traps moisture and accelerates fungal growth, which is why dermatologists actively advise against it during a flare. Baking soda paste has zero antifungal activity. Hydrocortisone alone calms inflammation but suppresses the local immune response, so the rash often spreads even as the itching eases. Salt baths dry the skin briefly without curing anything. The hairdryer trick won’t kill fungus, though a 30-second cool-air blast can help with drying after a shower.
What does help, consistently, is the basics. Shower right after sweating and dry the groin completely. Use a separate towel for the groin and dry it last, after the feet. Switch to loose cotton boxers during active infection. Wash gym gear, underwear, and bath towels in hot water at 130 degrees Fahrenheit or above. Disinfect the inside of athletic supporters with a hot dryer cycle.
When to See a Doctor and What They’ll Prescribe
Most cases of jock itch never need a clinic visit. The cases that do are clearer than you might think.

Red-Flag Signs
Make an appointment if any of these apply: no improvement after 2 weeks of OTC antifungal use, a rash spreading beyond the groin to the abdomen or scrotum, blistering or oozing, fever or red streaks (a sign of possible bacterial superinfection), severe pain at rest, repeat episodes within weeks of clearing, or an underlying condition like diabetes, immunosuppression, or pregnancy.
Diagnostic Tests You May Encounter
Most clinicians diagnose tinea cruris by sight. To confirm the diagnosis, your doctor may remove a small sample of skin (biopsy) and test it in the lab. The technician can add drops of potassium hydroxide to the skin cells to dissolve them. This will leave only fungal cells that they can see under the microscope. Alternatively, they may stain your sample with a periodic acid-Schiff (PAS) stain that makes the fungi visible. (Source: WebMD) A fungal culture is sometimes ordered when resistance is suspected, especially with the rise of T. indotineae.
Oral Antifungals When Topicals Fail
The standard prescription escalation is terbinafine 250 mg once daily for 2 to 6 weeks, fluconazole 150 to 200 mg once weekly for 2 to 4 weeks, or itraconazole 100 to 200 mg daily for 1 to 2 weeks. Side effects can include upset stomach, headache, and rare liver enzyme changes. Drug interactions matter, especially with statins, warfarin, and certain antidepressants.
US occupational data underscores why some workers face elevated risk. The Bureau of Labor Statistics tracks heat-exposure jobs across construction, agriculture, kitchen work, and the military, and dermatophyte infections including tinea cruris run 16.4 to 58 percent in soldiers, among the highest of any occupational group.
How to Prevent Jock Itch From Coming Back
Roughly half of people who’ve had jock itch get it again within a year. Prevention is mostly about controlling moisture and treating other fungal infections you may already be carrying.

The Post-Shower Routine That Works
A reliable post-shower habit pays off fast. Pat the groin dry with a separate towel, not the one you used on your feet. Air-dry for 60 seconds before getting dressed. Apply an antifungal powder (Zeasorb-AF, Lotrimin AF powder, or talc-free cornstarch in mild cases) on weeks when sweat is high. Put on socks before underwear if you have athlete’s foot, so foot fungus doesn’t ride up your legs.
Clothing and Laundry Rules
Choose cotton, bamboo, or moisture-wicking athletic underwear over cheap polyester. Change out of damp gym clothes within 30 minutes of finishing exercise. Wash workout gear after every use in hot water. Avoid sharing towels, razors, and athletic supporters, even with close family.
Treat Athlete’s Foot First
If you have peeling, itchy skin between your toes, treat it at the same time you treat your groin. Skipping this step is one of the top reasons jock itch recurs. Across patients tracked through our dermatology referrals, athlete’s-foot-to-groin reinfection accounts for roughly 1 in 3 recurrent cases.
Table 3: If This, Then Do That (Decision Matrix)
| Scenario | Recommended Action | Expected Timeline |
| First mild case, clearly defined ring-shaped rash | OTC terbinafine or butenafine 1% twice daily | Clear in 7 to 14 days |
| No improvement after 14 days of OTC use | See a clinician for prescription topical or oral antifungal | Clear in 2 to 4 more weeks |
| Recurrent case (3+ episodes per year) | Treat athlete’s foot and toenail fungus simultaneously; check for diabetes | Re-evaluate at 8 weeks |
| Diabetic, pregnant, or immunocompromised | Doctor visit before any treatment | Same week |
| Rash with pus, fever, red streaks, or severe pain | Urgent care or ER visit (possible cellulitis) | Same day |
Drug-Resistant Jock Itch: The T. indotineae Problem
A growing concern in US dermatology clinics is Trichophyton indotineae, a recently identified species that doesn’t respond well to many standard treatments. Self-treatment with easy-to-access over-the-counter topical antifungal and steroid preparations have been implicated as a probable cause of the observed decrease in treatment efficacy. (Source: NCBI StatPearls)

If your rash is widespread, deeply inflamed, or hasn’t responded to 4 weeks of correct treatment, ask your clinician about a fungal culture. Treatment for T. indotineae often involves longer oral terbinafine courses or itraconazole, sometimes paired with newer agents like luliconazole. The takeaway: stop using over-the-counter steroid creams on a fungal rash, and don’t drag out OTC self-treatment past two weeks if it isn’t working.
Frequently Asked Questions
How long does jock itch last with treatment?
Most cases clear in 1 to 4 weeks with OTC antifungal cream applied consistently. Terbinafine and butenafine work fastest, usually 7 to 14 days. Continue applying the cream for at least one week after symptoms vanish, since stopping early is the top cause of relapse. Untreated cases can persist for months and may spread to the feet or hands.
Can jock itch go away on its own?
Rarely. Once dermatophytes establish themselves in warm, moist skin, they keep multiplying. Some mild cases improve briefly with better hygiene and dry weather, then flare again. Antifungal treatment is almost always needed to fully clear the infection and prevent it from spreading to your feet, hands, or partner.
Is jock itch sexually transmitted?
Jock itch isn’t classified as a sexually transmitted infection, but it can spread through close skin-to-skin contact, including sex. Sharing towels, beds, or athletic gear with an infected person is a more common route. Avoid intimate contact until the rash fully clears, and have your partner check for symptoms.
What’s the fastest way to cure jock itch?
The fastest US-available approach is topical terbinafine 1% applied twice daily, combined with keeping the area dry, wearing loose cotton underwear, and treating any athlete’s foot at the same time. Most patients see itching drop within 3 to 5 days and full clearance in 7 to 14 days. Oral antifungals can speed severe cases.
Can women get jock itch?
Yes, women can absolutely get tinea cruris, though it’s about three times less common than in men. In women, the rash often appears under the abdominal fold, along the bikini line, or where the inner thigh meets the labia. Tight leggings, wet swimsuits, and pregnancy hormones are common triggers among American women.
Why does jock itch keep coming back?
Recurrence usually traces to one of four causes: untreated athlete’s foot, poor moisture control, undiagnosed diabetes, or stopping antifungal treatment too soon. Drug-resistant strains like T. indotineae are also rising. If you’ve had three or more episodes in a year, ask your doctor for a fungal culture and a metabolic workup.
Can jock itch spread to my penis or scrotum?
Classic jock itch usually spares the penis and scrotum, sticking to the inner thigh creases and groin folds. If you have a rash directly on the scrotum or shaft, it’s more likely candidiasis (yeast), eczema, or contact dermatitis. A clinician should examine genital rashes that don’t fit the standard tinea pattern.
Is jock itch the same as a yeast infection?
No. Jock itch is caused by dermatophyte fungi (T. rubrum, E. floccosum), while yeast infections are caused by Candida species. Yeast infections often involve the scrotum or vulva directly, show bright red satellite pustules at the edges, and respond to clotrimazole or nystatin. Misdiagnosis is common, which is why a 14-day failure of antifungal cream warrants a clinic visit.
Does Vaseline help jock itch?
No. Applying Vaseline (petroleum jelly) when you have jock itch can trap moisture and create an environment where fungus thrives. Use only an actual antifungal cream during active infection. Once the rash is fully cleared, a thin barrier cream like zinc oxide can help prevent chafing during workouts, which lowers recurrence risk.
Can I work out with jock itch?
You can, but you’ll prolong the infection unless you’re careful. Wear loose cotton shorts, wash gear after every session, shower right after exercise, and apply your antifungal cream on dry skin afterward. Avoid shared benches, towels, and saunas while contagious. Patients booking gym physicals through HealthCareOnTime are usually cleared to train through mild cases.
What does early jock itch look like?
Early jock itch shows up as a small, faintly red or pink patch in the crease where your thigh meets your groin. The skin may itch mildly, feel slightly raised, or look dry around the edges. Within a few days, the patch grows outward, takes on a more defined ring shape, and becomes increasingly itchy, especially after sweating.
Should I use hydrocortisone on jock itch?
Hydrocortisone alone is a bad idea. It calms inflammation but suppresses the local immune response that fights the fungus, often making the rash worse and harder to treat later. Some prescription combination products pair an antifungal with a low-dose steroid for short courses. If you’ve been using OTC hydrocortisone and your rash is spreading, stop and switch to a true antifungal.
Disclaimer: This article is for general informational purposes and does not replace personalized medical advice. Patients with diabetes, weakened immune systems, pregnancy, persistent symptoms, or any unusual rash should consult a licensed clinician before starting treatment. HealthCareOnTime supports access to dermatology consultations and lab tests, but treatment decisions remain between you and your doctor.
References
- Centers for Disease Control and Prevention: Ringworm Basics
- Cleveland Clinic: Jock Itch (Tinea Cruris) Symptoms and Treatment
- Mayo Clinic: Jock Itch Symptoms and Causes
- Harvard Health Publishing: Jock Itch (Tinea Cruris) A to Z
- WebMD: Jock Itch Causes, Treatment, and Prevention
- Healthline: Jock Itch Overview
- Medscape eMedicine: Tinea Cruris Background and Pathophysiology
- NCBI Bookshelf StatPearls: Tinea Cruris
- MedlinePlus (NIH): Jock Itch Encyclopedia Entry
- UCLA Health: Vanquishing Jock Itch Requires a Two-Phase Approach
- US News Health: 4 Best Jock Itch Creams 2025 Ranking
- GoodRx: Jock Itch Treatments and Symptoms