You’ve stepped out of the shower, glanced down, and noticed your vulva looks a different color than you remember. Maybe darker. Maybe a patch of white. Maybe a spot that wasn’t there last month. The first thought that races in is usually the worst one. Take a breath. The vast majority of vulvar color changes are completely normal, and learning which ones aren’t is the difference between unnecessary worry and catching something important early.
Table of Contents
Quick Answer: Vulvar discoloration usually reflects normal variation in melanin, hormonal changes, friction, or post-inflammatory pigmentation, and is rarely dangerous. Common causes include puberty, pregnancy, aging, shaving, tight clothing, and infections. Less often, white, red, blue, or asymmetric changes can signal lichen sclerosus, eczema, or vulvar cancer. See a gynecologist if discoloration is new, growing, painful, itchy, bleeding, or shaped like an irregular mole.

At a Glance
- The vulva is naturally darker than surrounding skin in most women
- Hormones, friction, and aging cause most benign discoloration
- Lichen sclerosus produces white, thinning patches and raises long-term cancer risk
- About 6,500 US women are diagnosed with vulvar cancer each year (American Cancer Society)
- Vulvar melanoma is rare but aggressive; the ABCDE rule helps spot it
- Most cosmetic “vulva bleaching” products lack FDA oversight
- A new, changing, painful, or bleeding spot warrants a same-week clinic visit
Patients booking gynecology consultations through HealthCareOnTime regularly ask whether color changes “down there” are something to worry about. The honest answer is: usually no, sometimes yes, and the difference is something every woman deserves to understand. What follows is what actually causes vulvar discoloration, the warning signs your gynecologist wants you to know, and the treatment options that are evidence-based versus the ones to avoid.
What “Normal” Vulva Color Actually Looks Like
Before talking about discoloration, it helps to know what range counts as normal. Most online articles use the wrong word entirely.
Anatomy Refresher: Vulva vs Vagina
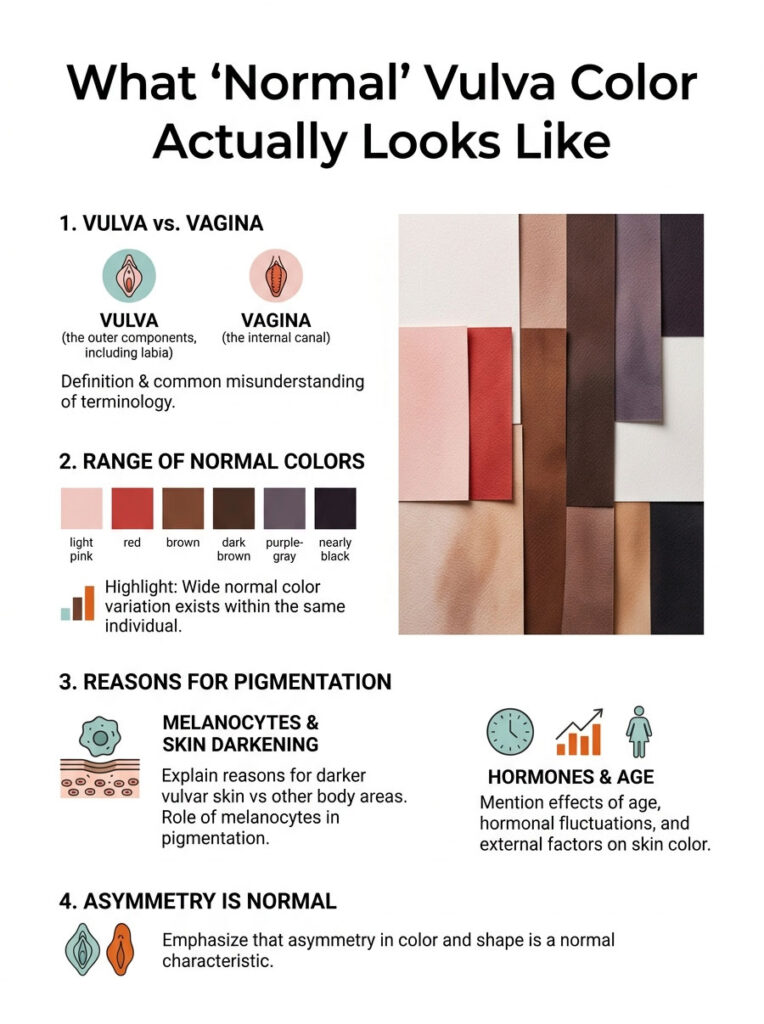
The vulva is the external part of the female genitals: the mons pubis, labia majora (outer lips), labia minora (inner lips), clitoris, and the area around the vaginal opening. The vagina is the internal canal. When people say “my vagina is dark,” they almost always mean the vulva. Getting this distinction right matters because skin conditions, pigmentation, and cancers behave differently inside versus outside.
The Wide Range of Normal Colors
There’s no single “correct” vulva color. Across women, the vulva can range from light pink to red, brown, dark brown, purple-gray, or nearly black. In most women, the genital areas will be darker than other skin. There is no “normal” colored vagina, vulva, or anus, the skin in that area is simply darker.
Color often varies even within the same woman. The labia majora may be one shade, the labia minora another, and the area near the vaginal opening yet another. Asymmetry is normal too. One labium may be darker, longer, or differently shaped than the other.
Why Your Vulva Is Darker Than Your Arm or Thigh
The vulvar skin contains a higher density of melanocytes, the pigment-producing cells responsible for skin color. This is caused by a higher amount of melanocytes that secrete melanin. Melanocytes naturally increase in the genital areas with age and during states of increased or fluctuating estrogen levels. Add in friction, hormones, and decades of subtle inflammation from clothing and grooming, and you get the natural pigmentation differences most women see across their lifetime.
The 5-Minute Vulvar Self-Exam Every Adult Should Know
Before getting into causes, learning what your own vulva looks like is the most useful thing you can do. A monthly self-check, ideally between periods, takes five minutes and catches almost every concerning change early.
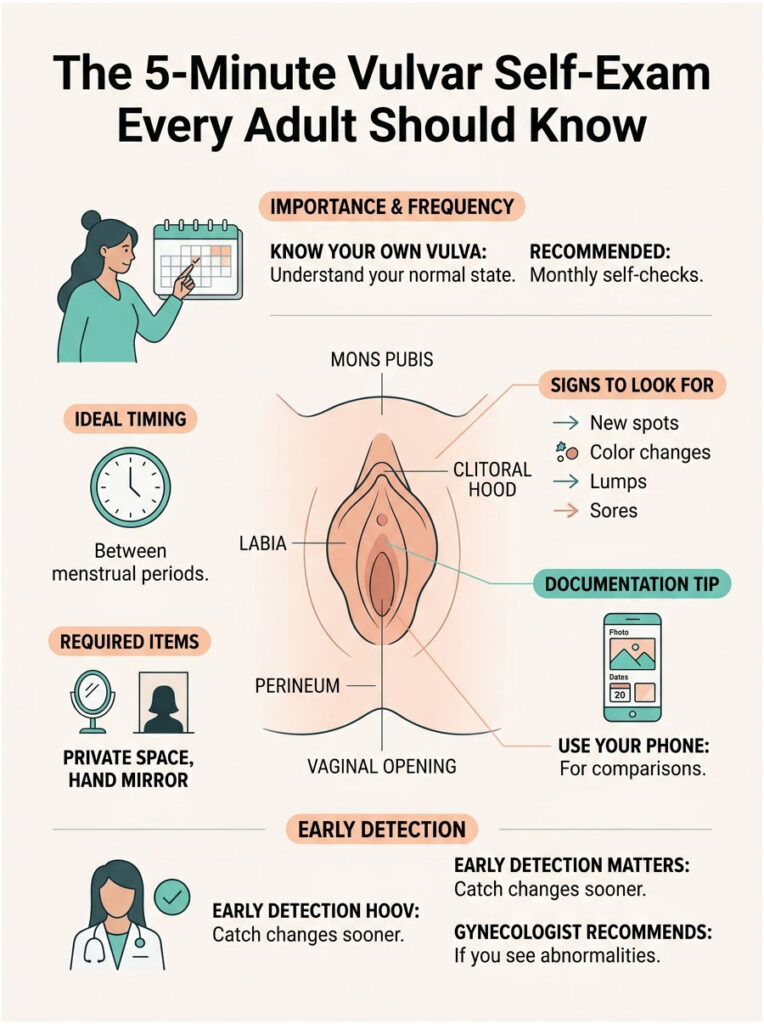
Find a private, well-lit space and a hand mirror. Sit, stand, or squat in whatever position lets you see clearly. Examine the mons pubis, both sets of labia, the clitoral hood, the perineum, and the area around the vaginal opening. Look for new spots, color changes, lumps, sores, or anything that wasn’t there last month.
Document with your phone if you want a comparison point. Many gynecologists now encourage women over 40 to do this monthly. Patients booking annual exams through HealthCareOnTime often catch their own early warning signs this way.
Why Is Your Vulva Discolored? The 8 Most Common Causes
If you’ve noticed a real change rather than just a color you’ve always had, the cause usually falls into one of eight categories. Most are benign.
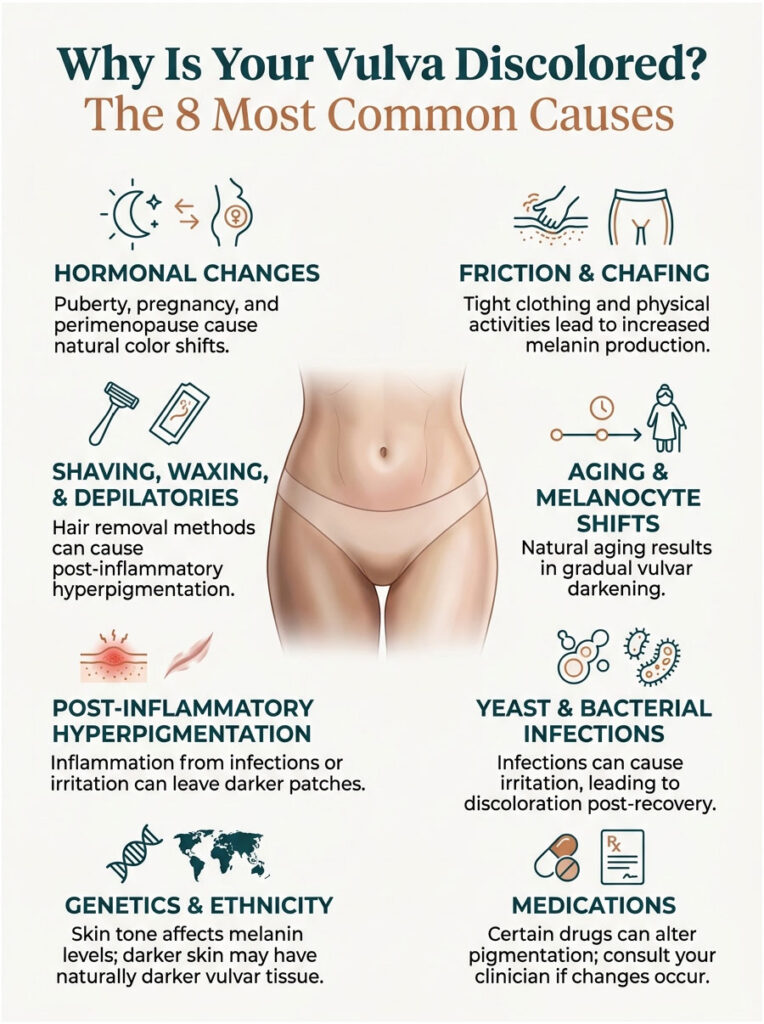
Hormonal Changes (Puberty, Pregnancy, Perimenopause)
Hormones like estrogen and progesterone play a key role in regulating melanin production. Puberty triggers the first major darkening, often surprising teenagers who don’t realize the change is normal. Pregnancy causes a noticeable second wave (along with the linea nigra on the abdomen and darker areolas), and perimenopause brings a third round of shifts.
Each phase of darkening is a normal response to changing hormone levels. None usually requires treatment.
Friction and Chafing
Tight leggings, skinny jeans, daily Peloton sessions, long runs, and even prolonged sitting at a desk can rub vulvar skin enough to trigger melanocyte activity. Repeated friction over months and years deposits more pigment, especially along the inner thigh creases and outer labia.
Across patients we see for skin and gynecology consults, friction-related darkening is one of the most common cosmetic concerns women raise once they feel comfortable asking.
Shaving, Waxing, and Depilatories
Hair removal is one of the biggest (and most overlooked) causes of vulvar darkening in American women. Razor irritation, waxing burns, and chemical depilatories all cause micro-inflammation. The skin responds by producing more melanin, leaving dark patches behind even after the redness fades.
This is called post-inflammatory hyperpigmentation, and it’s the same mechanism behind acne marks on your face.
Aging and Melanocyte Shifts
The vulva tends to darken gradually with age. The skin also becomes thinner and less elastic, which can change how light reflects off the surface and make existing pigmentation look more pronounced. Women in their 50s and 60s often describe vulvar color changes that have been quietly accumulating for decades.
Post-Inflammatory Hyperpigmentation
Any inflammation, from infections to eczema to allergic reactions to heavily fragranced soaps, can leave behind extra pigment. Once the underlying cause clears, the discoloration usually fades over weeks to months. Stronger cases can last a year or more.
Yeast and Bacterial Infections
Vaginal infections, such as yeast infections or bacterial vaginosis, can trigger inflammation, itching, and discomfort. Constant scratching and irritation can leave darker skin once the infection clears. Treating recurrent infections promptly limits long-term pigment changes.
Genetics and Ethnicity
Naturally darker skin tones produce more melanin everywhere, including the vulva. Women of South Asian, African, Hispanic, and Mediterranean descent often have noticeably darker vulvar tissue from puberty onward. This is genetic baseline, not a problem to fix.
Medications
Certain medications can shift pigmentation in the vulvar area. Hormonal birth control, antibiotics like minocycline, and chemotherapy drugs are the most common culprits. If discoloration started shortly after a new prescription, mention it to your prescribing clinician.
Table 1: Common Vulva Discoloration Patterns Compared
| Discoloration Type | Likely Cause | Color Pattern | Symptoms | Concern Level |
| Symmetric darkening of labia majora | Hormones, age, genetics | Even brown to dark brown | None | Normal |
| Dark patches near groin folds | Friction, tight clothing | Brown, sharply defined | Mild itch or chafing | Low |
| Dark spots after shaving or wax | Post-inflammatory | Brown spots in ingrown hair pattern | None to mild itch | Low |
| White, thin, glistening patches | Lichen sclerosus | Ivory or porcelain white | Severe itch, soreness, painful sex | Moderate; requires diagnosis |
| Asymmetric, irregular dark mole | Possible vulvar melanoma | Multi-color (brown, black, red, blue) | Often none initially | High; urgent biopsy |
| Persistent red, scaly area | Paget disease, eczema, infection | Red, pink, or coral | Itching, soreness, sometimes pain | Moderate; needs eval |
If your discoloration matches the bottom two rows, schedule a clinic visit within the week. The top four rows usually aren’t urgent but are worth mentioning at your next gynecology appointment.
Vulva Discoloration Symptoms: What You Might Notice
Discoloration alone is rarely the only sign something needs attention. The accompanying symptoms tell you whether to monitor or act.

Color Shifts: Darker, Lighter, Red, White, Blue, Purple
Brown to dark brown is the most common shift and is usually benign. White patches deserve evaluation because they may indicate lichen sclerosus or vitiligo. Red can signal infection, dermatitis, or Paget disease. Blue or purple can indicate vulvar varicose veins, hematomas, or, rarely, severe infection.
Texture Changes
Healthy vulvar skin should feel like skin elsewhere on your body, slightly thicker and more cushioned in the labia majora area. Watch for skin that has become thinner, shinier, parchment-like, thickened, leathery, or scaly. Vulvar lichen sclerosus is a chronic inflammatory dermatosis characterized by ivory-white plaques or patches with glistening surface, with common symptoms of irritation, soreness, painful sex, and painful urination.
Itching, Burning, Pain, Bleeding
Persistent itching that doesn’t respond to over-the-counter products is one of the most common early signs of lichen sclerosus, eczema, or precancerous changes. Bleeding from a discolored area, especially without trauma, warrants a same-week appointment.
Differences Across Skin Tones
Most medical photos and reference images still default to lighter skin examples, which means women with darker complexions often don’t recognize warning signs as quickly. Hyperpigmentation looks different, and conditions like lichen sclerosus can present as paler-than-surrounding patches rather than the stark “white” described in textbooks. In cases reviewed by our medical team, women of color frequently arrive after months of misdiagnosis as eczema or chronic yeast infection.
When Discoloration Is Asymptomatic (and Still Worth Noting)
Vulvar melanoma can be completely painless and itch-free in early stages. Most vulvar melanomas are black or dark brown, but they can be white, pink, red, or other colors. They can be found throughout the vulva, but most are around the clitoris or on the labia majora or minora. Vulvar melanomas can sometimes start in a mole, so a change in a long-standing mole can also indicate melanoma. (Source: American Cancer Society) A new, irregular dark spot deserves attention even if it doesn’t hurt.
When Vulva Discoloration Signals Something Serious
These conditions are uncommon, but the consequences of missing them are real.
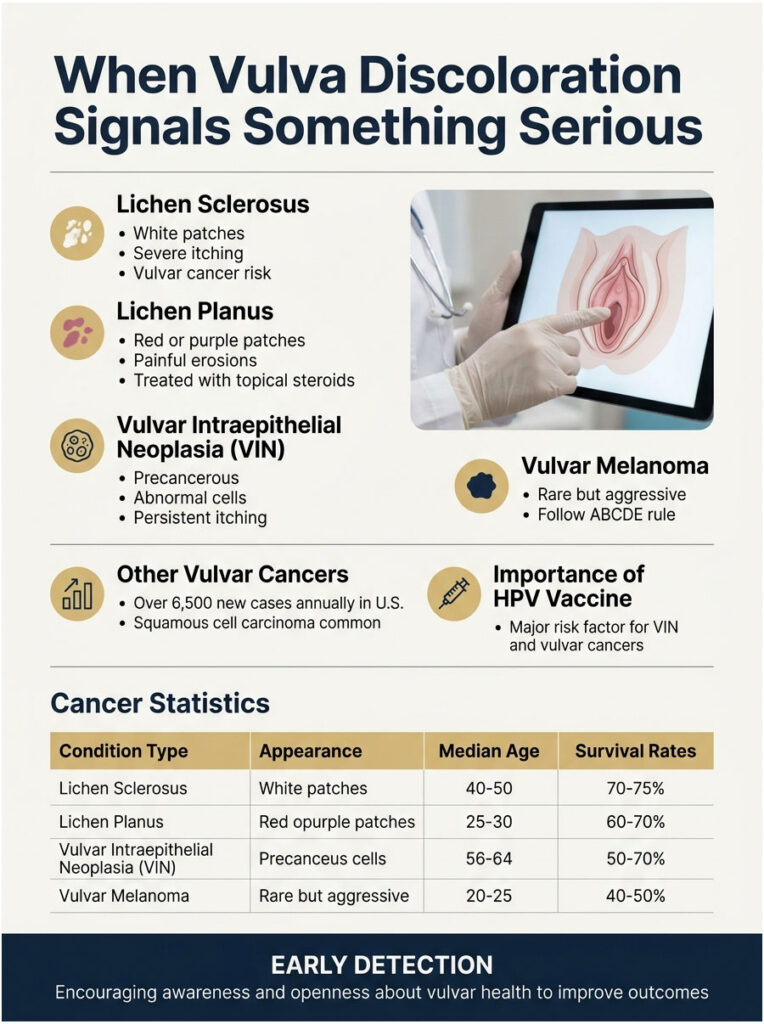
Lichen Sclerosus: The White-Patch Warning
Lichen sclerosus (LS) is a chronic inflammatory skin condition that affects roughly 1 in 30 older women, with another peak in girls before puberty. LS results in inflammation, marked hypopigmentation, tissue thinning, areas of thickening, and scarring.
The classic look is ivory or porcelain-white patches that may form a figure-eight pattern around the vulva and anus. Severe itching, painful sex, and tearing of the skin are common. LS is treatable with high-potency topical steroids, but it requires monitoring because untreated LS slightly raises the long-term risk of vulvar squamous cell carcinoma.
Lichen Planus and Chronic Vulvar Purpura
Lichen planus often produces red, purple, or violet patches and may cause painful erosions. Chronic vulvar purpura is a clinical term for different chronic inflammatory dermatoses presenting as red, bluish, or violaceous discoloration on the vulva, often associated with cayenne pepper-like speckling. The most common diseases include Zoon’s vulvitis, lichen aureus, pigmented purpuric dermatosis, and vulvar lichen planus. Treatment usually involves potent topical steroids and sometimes systemic medications.
Vulvar Intraepithelial Neoplasia (VIN)
VIN is a precancerous condition where abnormal cells form in the top layer of vulvar skin. VIN may look thicker and lighter than the surrounding skin, but it can also appear red, pink, or darker than normal. The most common symptom is persistent itching that won’t go away. HPV is the major risk factor, which is one reason the HPV vaccine matters.
Vulvar Melanoma and the ABCDE Rule
Vulvar melanoma is rare, accounting for about 5 percent of vulvar cancers, but it’s aggressive. The ABCDE rule, originally developed for skin melanoma, applies here too:
- Asymmetry: one half doesn’t match the other
- Border: ragged, notched, or blurred edges
- Color: multiple colors or uneven distribution
- Diameter: larger than 6 mm (about the size of a pencil eraser)
- Evolving: any change in size, shape, or color over time
Any new pigmented spot meeting one or more of these criteria deserves a biopsy. Our medical reviewers consistently flag that vulvar melanoma is often diagnosed late because women feel embarrassed to ask about color changes “down there.” Early detection dramatically improves outcomes.
Other Vulvar Cancers
Healthcare providers diagnose just under 6,500 new cases of vulvar cancer in the U.S. each year. Nearly 80 percent of people diagnosed are over age 50, and over half of all diagnoses are in people over age 70. The average age at diagnosis is 68. Squamous cell carcinoma accounts for about 80 percent. Other rare types include basal cell carcinoma, Bartholin gland adenocarcinoma, and Paget disease, which presents as a red, scaly patch that mimics eczema.
Table 2: USA Vulvar Cancer Statistics
| Cancer Type | % of Vulvar Cancers | Typical Appearance | Median Age | 5-Year Survival | Source |
| Squamous cell carcinoma | ~80% | Lump, sore, or red/white patch | 68 | 70-90% (early) | American Cancer Society |
| Vulvar melanoma | ~5-6% | Black, brown, or multi-colored mole | 68 | ~47% (all stages) | Healthline / NCI |
| Basal cell carcinoma | 2-7% | Pearly nodule on labia majora | 60-80 | >95% | DermNet NZ |
| Bartholin gland adenocarcinoma | ~5% | Lump near vaginal opening | 50-60 | 60-70% | Cleveland Clinic |
| Paget disease | <1% | Red, scaly, eczema-like | 60-70 | 80-90% | Johns Hopkins |
Source: American Cancer Society, NCI, Cleveland Clinic, Healthline, DermNet NZ.
How Doctors Diagnose Vulva Discoloration
If you book an appointment, here’s what to expect.

The Pelvic Exam and Vulvoscopy
Most evaluations start with a visual inspection of the vulva, often using a magnifying device called a colposcope or vulvoscope. The clinician may apply a dilute acetic acid solution to highlight abnormal areas. This is painless and takes only a few minutes.
In the US, most insurance plans cover annual gynecology exams as preventive care, including a baseline vulvar inspection. If you don’t have a regular gynecologist, planned visits typically run $100 to $250 out of pocket without insurance.
Biopsy (Punch or Excisional)
If anything looks suspicious, a biopsy is the only definitive way to know what it is. A small punch tool removes a 3 to 4 mm sample under local anesthesia. Most patients describe it as a brief pinch followed by mild soreness. Results usually come back within 1 to 2 weeks.
Vulvar biopsies are generally covered by insurance when medically indicated. Self-pay costs typically range from $200 to $500 plus pathology fees.
Dermoscopy for Pigmented Lesions
For dark spots that might be a mole or melanoma, dermoscopy uses a handheld magnifier with polarized light to examine pigment patterns. It’s a quick, in-office tool that helps decide whether biopsy is needed.
Lab Tests
If infection is suspected, your clinician may take a swab for KOH preparation (looking for fungus), a culture (for bacteria or yeast), or HPV testing if VIN is on the differential. None of these require special preparation on your part.
Treatment Options for Vulvar Discoloration
What works depends entirely on what’s causing the discoloration. There’s no one-size-fits-all answer.

Watchful Waiting and Reassurance
For most benign hyperpigmentation, the best treatment is no treatment. Hormonal darkening from pregnancy often fades on its own over the year after delivery. Friction-related darkening fades with switching to looser clothing.
Topical Treatments: Corticosteroids, Calcineurin Inhibitors, Retinoids
For lichen sclerosus, the gold-standard treatment is high-potency topical steroids like clobetasol propionate 0.05 percent. For inflammatory conditions in non-LS contexts, calcineurin inhibitors like tacrolimus can reduce inflammation without the thinning that long-term steroids cause. Topical retinoids (tretinoin) are sometimes used off-label for hyperpigmentation but should be applied only under a clinician’s guidance, since vulvar skin is far more sensitive than facial skin.
Hydroquinone and FDA’s Evolving Stance
Hydroquinone has long been the traditional gold-standard skin lightener, but the FDA has tightened its rules. Over-the-counter hydroquinone products were largely removed from US shelves in 2020 under the CARES Act, leaving prescription-only access. Even prescription hydroquinone use on vulvar skin is controversial because of irritation risk and rare cases of paradoxical darkening (ochronosis).
Laser and Light-Based Treatments
Q-switched lasers and fractional non-ablative lasers can reduce pigmentation in some women, but data on vulvar skin specifically is limited. Side effects include burns, hyperpigmentation, and scarring. These should be performed only by a board-certified dermatologist or gynecologist with specific vulvar laser training. Out-of-pocket costs typically run $300 to $800 per session, with multiple sessions usually needed.
Surgical Options for Cancer or Precancer
Confirmed VIN, melanoma, or invasive cancer requires surgical excision. The exact procedure (wide local excision, partial vulvectomy, or radical vulvectomy) depends on the type, size, and stage. Sentinel lymph node biopsy may be added for melanoma or invasive squamous cell carcinoma.
What to Skip
Unregulated “vagina lightening” creams sold online are a frequent cause of harm. Many contain mercury, illegal hydroquinone concentrations, or potent steroids, all of which can damage the delicate vulvar skin barrier. Patients booking dermatology consults through HealthCareOnTime sometimes arrive with severe contact dermatitis, paradoxical darkening, or worsened lichen sclerosus from these products.
Skip them entirely. The FDA periodically issues warnings about dangerous skin-lightening imports, and the FDA’s drug safety page maintains current alerts.
How to Care for Your Vulva and Reduce Discoloration Risk
You can’t change genetics or hormones, but you can reduce avoidable contributors.

Cleansing Dos and Don’ts
The vulva is largely self-cleaning. Warm water once a day is enough. If you want a cleanser, choose a fragrance-free, pH-balanced wash made for the genital area. Skip douches, scented soaps, scrubs, deodorant sprays, and anything with sulfates. Pat dry rather than rubbing.
Underwear, Leggings, and Friction Control
Cotton underwear allows the area to breathe. Wear breathable bottoms when possible and change out of damp gym clothes within 30 minutes. If you wear leggings or shapewear daily, consider seamless or moisture-wicking versions to reduce abrasion.
Shaving and Waxing Alternatives
If hair removal is causing repeated irritation, consider trimming with scissors, switching to a single-blade razor, or exploring laser hair removal with a certified provider. Shave in the direction of hair growth, use a fresh blade, and apply a fragrance-free moisturizer afterward.
Sun Protection and Skin Barrier Care
Vulvar skin almost never sees direct sun, so UV protection matters mainly for those who tan or sunbathe nude. Otherwise, focus on barrier care. A thin layer of plain petroleum jelly or zinc oxide can protect against chafing during workouts and long days in tight clothing.
Table 3: If This, Then Do That (Decision Matrix)
| Symptom or Finding | Recommended Action | Timeline |
| Symmetric darkening, no other symptoms | Watchful waiting, document with mirror photos | Mention at next annual exam |
| New itching with white patches | Schedule a gynecology visit; possible lichen sclerosus | Within 2 to 4 weeks |
| Dark mole that meets any ABCDE criterion | Same-week appointment; expect biopsy | Within 7 days |
| Persistent red, scaly patch not responding to OTC | Gynecology or dermatology evaluation | Within 2 weeks |
| Bleeding, ulcerated, or non-healing lesion | Urgent gynecology appointment | Same week |
| Sudden bluish-purple swelling with pain | Urgent care; possible hematoma or severe infection | Same day |
Vulva Discoloration During Pregnancy and Postpartum
Pregnancy is one of the most common reasons women notice sudden vulvar darkening.

Why Estrogen Surges Darken the Vulva
The same hormonal surge that darkens the linea nigra on your abdomen and the areolas of your breasts also affects the vulva. In conditions that cause hormonal changes, such as pregnancy, increased estrogen can cause the vulva to appear as if it has dark spots or patches. Increased blood flow can also give the area a darker, more purple-tinged look during the second and third trimesters.
Will It Fade After Delivery?
For most women, yes. Hormones shift again after delivery and during breastfeeding, and the darkening usually softens over the 6 to 12 months postpartum. Some pigment may persist permanently, especially after multiple pregnancies.
When Postpartum Changes Need a Doctor
If a new dark spot appears that doesn’t fade, you develop white patches with itching, or you notice swelling, lumps, or persistent pain that wasn’t part of normal recovery, schedule a postpartum gynecology appointment. Postpartum lichen sclerosus and vulvar varicose veins are both more common than many women realize.
Frequently Asked Questions
Is it normal for my vulva to be darker than the rest of my skin?
Yes. The vulva contains more melanocytes than most other skin areas, so it’s naturally darker than your arm or thigh in the majority of women. Hormonal shifts at puberty, pregnancy, and perimenopause typically deepen the color further. Unless darkening is sudden, asymmetric, or paired with itching, bleeding, or pain, it’s almost always benign.
Can vulva discoloration go away on its own?
Often, yes. Hyperpigmentation from friction, shaving, or pregnancy frequently fades over months once the trigger is removed. Inflammatory causes like yeast infections clear with treatment, and the discoloration follows over weeks to a year. Permanent pigmentation from genetics or aging usually doesn’t reverse without medical or cosmetic intervention.
Why did my vulva get darker after pregnancy?
Pregnancy raises estrogen and progesterone significantly, which boosts melanocyte activity throughout the body. The same process that creates the linea nigra and darkens the areolas affects the vulva. This is normal and usually fades partially over the year after delivery, though some women retain a permanent color shift, especially after multiple pregnancies.
Are dark spots on the vulva a sign of cancer?
Most aren’t. Symmetric, even pigmentation matching surrounding tissue is almost always benign. However, a new mole or spot that’s asymmetric, irregularly bordered, multi-colored, larger than 6 mm, or evolving over time should be evaluated promptly. Vulvar melanoma is rare but aggressive, and early biopsy gives the best outcome. Call your gynecologist if any spot meets ABCDE criteria.
Can shaving cause vulva discoloration?
Yes. Razor burn, ingrown hairs, and small cuts trigger inflammation, and the skin responds by depositing extra melanin during healing. This post-inflammatory hyperpigmentation can last months. To reduce it, shave in the direction of hair growth with a sharp single-blade razor, exfoliate gently a few times a week, and consider switching to trimming, waxing, or laser hair removal.
Is vulva bleaching safe?
Most over-the-counter “vulva bleaching” products lack FDA oversight and have caused chemical burns, severe irritation, and paradoxical darkening. Prescription hydroquinone, supervised tretinoin, and certain laser treatments under a board-certified specialist are safer options when medically indicated. Cosmetic lightening of normal skin carries risk and limited benefit, so weigh it carefully with a clinician.
What does lichen sclerosus look like on the vulva?
Lichen sclerosus typically appears as ivory or porcelain-white, glistening patches that may form a figure-eight pattern around the vulva and anus. The skin often looks thinned, like crinkled paper, and may tear easily. Severe itching, painful sex, and burning are common. It’s treatable with high-potency topical steroids and requires ongoing monitoring.
Why is my vulva turning white in patches?
White patches most often indicate lichen sclerosus, lichen planus, or vitiligo. Less commonly, white areas can reflect VIN or, rarely, vulvar cancer. Persistent itching paired with white patches is the most common early sign of lichen sclerosus and warrants a gynecology visit within 2 to 4 weeks. A biopsy may be needed to confirm.
Can yeast infections cause discoloration?
Yes, indirectly. Active yeast infections cause inflammation and intense itching. Constant scratching and friction can lead to post-inflammatory hyperpigmentation, leaving darker patches that linger after the infection clears. Treating recurrent yeast infections promptly and avoiding tight, damp clothing helps minimize long-term color changes. If discoloration persists for over 6 months, schedule a clinical evaluation.
How do I tell normal pigmentation from melanoma?
Normal pigmentation is typically symmetric, evenly colored, and stable over time. Melanoma usually breaks one or more ABCDE rules: Asymmetric shape, irregular Border, varied Color, Diameter over 6 mm, and Evolving over time. Any new dark spot that’s growing, changing color, or has uneven edges should be evaluated by a gynecologist or dermatologist. A biopsy is the only way to confirm.
Does birth control cause vulva discoloration?
Combination hormonal birth control can subtly increase melanin production, similar to how some women develop melasma on the face. Vulvar darkening from oral contraceptives is usually mild and often reverses after discontinuing. If you started a new hormonal method and notice rapid pigment change, talk with your prescriber about whether a different formulation might suit you better.
When should I see a gynecologist about vulva color changes?
See a gynecologist within 1 to 2 weeks if you notice persistent itching, white or red patches that won’t fade, a new mole, asymmetric or irregular pigmented spots, bleeding without trauma, or non-healing sores. Same-day or urgent care is appropriate for sudden bluish-purple swelling, severe pain, or rapidly spreading discoloration. Annual gynecology exams are a good baseline for everyone.
Disclaimer: This article is for general informational purposes and does not replace personalized medical advice. Any new, growing, painful, bleeding, or unusual vulvar lesion should be evaluated by a licensed gynecologist or dermatologist. HealthCareOnTime supports access to gynecology consultations and lab tests, but treatment decisions remain between you and your doctor.
References
- American Cancer Society: Vulvar Cancer Signs and Symptoms
- Cleveland Clinic: Vulvar Cancer Symptoms, Causes, and Treatment
- Johns Hopkins Medicine: Vulvar Cancer
- Healthline: Dark Spots on Vagina Causes and Treatment
- Harvard Health Publishing: Managing Common Vulvar Skin Conditions
- Merck Manual Professional: Lichen Sclerosus
- DermNet NZ: Vulval Cancer
- NCBI PMC: Vulvar Lichen Sclerosus et Atrophicus
- NCBI PMC: Vulvar Lichen Planus and Chronic Vulvar Purpura
- Healthline: Vulvar Melanoma Symptoms and Treatment
- OCRA: Vulvar Cancer Incidence and Treatment
- Pathology Outlines: Pigmented Lesions of the Vulva
- FDA: Drug Safety and Availability