You flush, glance back, and stop cold. The bowl is green. Not a slight olive tint, but the kind of green that makes you wonder if something inside you just declared war. Take a breath. In the vast majority of cases, green stool is your gut quietly telling you what you ate yesterday, how fast things are moving today, or that a new pill or supplement is doing its job. The few times it matters more, the signal almost always arrives with company, like cramps, fever, or blood.
Table of Contents
Quick Answer: Green stool usually means food moved through your gut faster than normal and didn’t give bile enough time to break down into brown stercobilin, or your meals contained chlorophyll-rich greens, blue or green food dyes, or iron supplements. Most cases resolve within 24 to 48 hours. Persistent green stool or green diarrhea with fever, mucus, blood, or weight loss can signal infection or a digestive condition and deserves a doctor’s visit.

At a Glance
- Stool is brown because gut bacteria convert green bile pigment into brown stercobilin during normal transit.
- The most common cause of green stool in healthy US adults is diet (spinach, kale, matcha, blue or green food dyes, iron).
- Fast transit (diarrhea) is the second most common cause, since bile stays green when there isn’t time for the color change.
- The CDC estimates 1.35 million Salmonella, 1.2 million Giardia, and 19 to 21 million Norovirus infections per year in the US, all of which can cause green diarrhea.
- Newborn meconium is normally dark green for the first 24 to 48 hours after birth.
- Green stool lasting more than three days, or paired with fever, blood, or severe pain, warrants medical evaluation.
- Stool culture, ova and parasites testing, and GI PCR panels are the standard US diagnostic workup.
Why Stool Has Color, in Plain English
Brown is not the natural color of digested food. It’s the end product of a chemistry experiment your liver, gallbladder, gut bacteria, and small intestine run dozens of times a day. The starring molecule is bilirubin, which forms when your body breaks down old red blood cells. Your liver packages bilirubin into bile, which is naturally a yellow-green fluid.
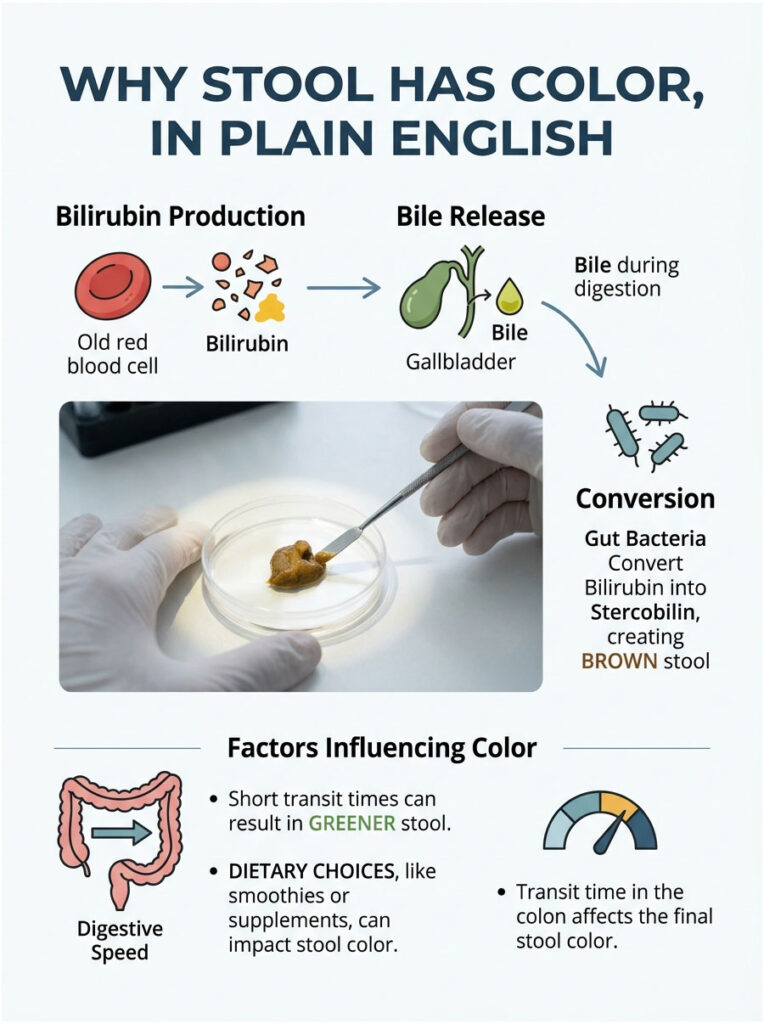
Bile gets stored in your gallbladder and released into your small intestine after meals to help digest fats. As it travels through your gut, bacteria progressively convert bilirubin into stercobilin, the brown pigment that gives healthy stool its color. The longer that journey takes, the browner the output. Cut the journey short, and what comes out is closer to the original green of bile.
What Changes the Timing
The final color depends on how much bile gets released (driven mostly by how fatty your last meal was), how much chlorophyll or food dye is competing for the spotlight, and how fast everything moves through your colon. Healthy adult transit time in the US runs between 12 and 72 hours. Anything that speeds that clock up, from a stomach bug to a strong cup of coffee, tilts the color toward green.
Patients booking stool analysis panels through HealthCareOnTime often arrive convinced something is seriously wrong, when the answer turns out to be the kale smoothie they drank Tuesday plus the iron supplement they started Wednesday. Two innocent inputs, one alarming output.
The Common Causes of Green Stool, Ranked
Our medical reviewers organized the typical USA causes from most to least common, based on what shows up in real outpatient case notes. Most of these are completely benign. A few aren’t.

Cause 1: Leafy Greens and Chlorophyll
Spinach, kale, arugula, Swiss chard, broccoli, matcha, and wheatgrass all contain heavy concentrations of chlorophyll, the green pigment plants use for photosynthesis. Eat enough of them, and the pigment passes through your digestive tract intact, tinting stool anywhere from olive to bright green. A single large salad usually won’t shift things much. A few days of green smoothies almost always will.
Cause 2: Green, Blue, or Purple Food Dyes
Artificial colors in sports drinks, frozen flavored ice pops, fruit punch, jello, frosted cookies, blue Gatorade, and birthday cake icing often pass through the gut unabsorbed. Blue and purple dyes are especially sneaky, because they mix with naturally yellow bile to produce a vivid green output. Kids’ party leftovers are a classic culprit in pediatric clinics.
Cause 3: Iron Supplements
Iron supplements and prenatal vitamins containing ferrous sulfate or ferrous fumarate can turn stool dark green, dark olive, or even black. The effect is dose-dependent and harmless. If you started a new iron pill in the past week and the color shifted, the timing is your answer. The Harvard Health Publishing team confirms this as one of the most frequent over-the-counter triggers.
Cause 4: Antibiotics Changing Gut Bacteria
Antibiotics kill the gut bacteria that convert bile pigments to brown, which can leave stool greenish for a few days after starting a course. Amoxicillin, clindamycin, and broad-spectrum cephalosporins are common offenders. If green stool is paired with watery diarrhea more than a week into an antibiotic course, talk to your prescriber, because that pattern can sometimes signal C. difficile infection.
Cause 5: Rapid Intestinal Transit (and Green Diarrhea)
This is the single biggest non-dietary cause. When stool moves through the colon too fast, bile pigments stay green because there isn’t time for the bacterial conversion to brown. The result is often what people call green diarrhea: watery, urgent, and noticeably green. Anything that causes diarrhea, from a stomach bug to lactose intolerance to sorbitol in sugar-free gum, can produce this pattern.
Cause 6: Gastrointestinal Infections
Bacterial, viral, and parasitic gut infections almost always produce diarrhea, and that diarrhea is frequently green. The major US culprits are Salmonella, E. coli, Shigella, Campylobacter, Norovirus, Rotavirus, Giardia duodenalis, and Clostridioides difficile. These usually arrive with cramps, fever, urgency, nausea, or vomiting, separating them from a benign dietary green.
Cause 7: Bile-Related Issues
Bile acid malabsorption (BAM), a condition where the small intestine fails to reabsorb bile salts, dumps extra green bile into the colon and causes chronic green or yellow watery stool. Patients who’ve had gallbladder removal surgery (cholecystectomy) sometimes experience this for weeks or months while the body adjusts to constant bile drip rather than gallbladder-controlled release.
Cause 8: IBS, Crohn’s, Celiac, and Other GI Conditions
Irritable bowel syndrome (IBS) affects 10 to 15% of US adults, according to the American College of Gastroenterology, and frequently produces alternating stool colors and consistencies. Crohn’s disease, ulcerative colitis, and celiac disease can also generate green stool, usually as part of a larger pattern of cramping, weight loss, or bloody diarrhea.
Cause 9: Pregnancy Hormones and Prenatal Vitamins
Pregnancy slows some parts of digestion while prenatal vitamin iron speeds up the color change. Many expecting mothers report greenish stool, especially in the first trimester. In cases reviewed across our diagnostic network, this is rarely cause for concern unless paired with severe nausea, weight loss, or bleeding.
Cause 10: Stress and High-Fat Diets
The gut-brain axis is real. Acute stress speeds intestinal motility through the vagus nerve, shortening transit time and producing greener stool. Keto and other high-fat diets prompt the liver to release more bile to digest fats, sometimes more than gut bacteria can chemically convert, leaving a green tint behind.
Table 1: Green Stool Causes vs Symptoms vs Urgency
| Cause | Typical Stool Look | Common Symptoms | Urgency |
| Leafy greens, matcha, kale | Olive to forest green, formed | None | Watch and wait; resolves in 24 to 48 hours |
| Food dyes (blue, green, purple) | Bright neon green | None | Watch and wait; resolves in 24 hours |
| Iron supplements | Dark green to black, formed | Mild constipation possible | Watch and wait; expected side effect |
| Antibiotics | Greenish, sometimes loose | Mild bloating | Monitor; call doctor if diarrhea worsens past day 7 |
| Stomach bug (Norovirus) | Watery, bright green | Cramps, nausea, vomiting, low fever | Watch 48 to 72 hours; ER if dehydration |
| Salmonella, Giardia, C. diff | Green diarrhea, possibly bloody or mucus-coated | Fever, severe cramps, urgency | See doctor within 24 to 48 hours |
| Post-gallbladder surgery (BAM) | Green to yellow watery | Urgent diarrhea after fatty meals | Schedule a GI follow-up |
| IBS, Crohn’s, celiac | Variable, sometimes green | Bloating, pain, weight loss, blood | See doctor for full workup |
| Pregnancy + prenatal iron | Dark green, formed | Possible constipation, nausea | Routine; mention at next OB visit |
| Stress, high-fat / keto diet | Green to olive, loose | Anxiety symptoms, bloating | Watch and wait; lifestyle adjustment |
Green Stool in Adults vs Infants
The rules genuinely differ across age groups. What’s alarming in an adult may be perfectly normal in a newborn, and vice versa.
Adult Patterns
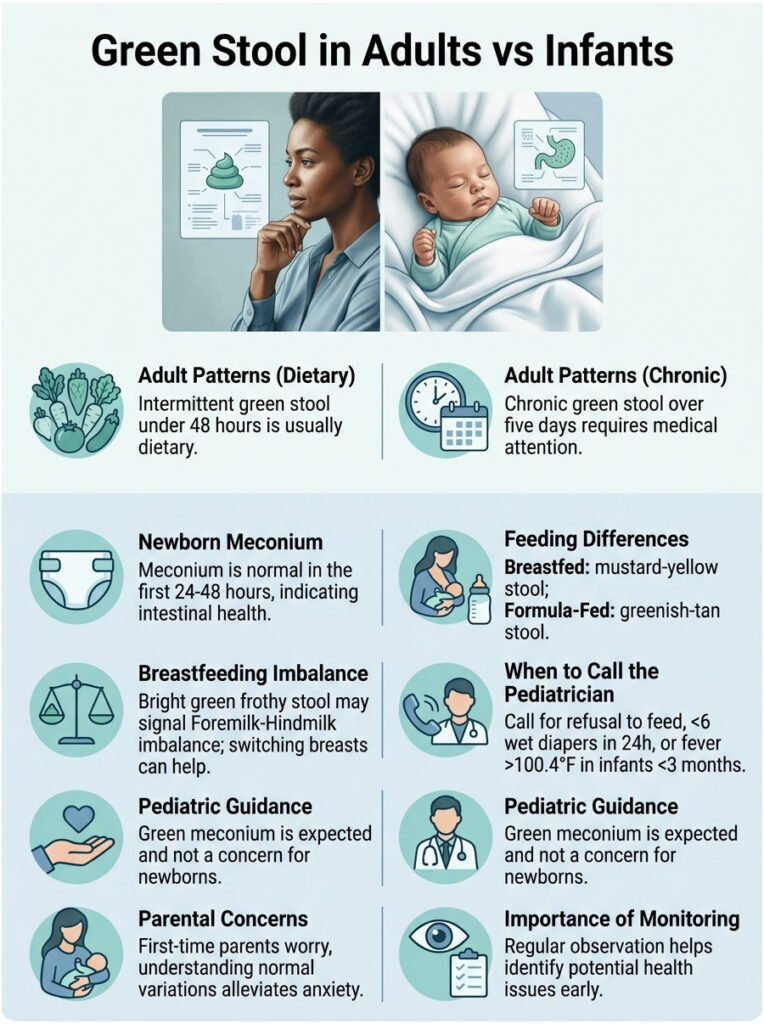
In healthy US adults, intermittent green stool that lasts under 48 hours and doesn’t come with pain, fever, or blood is almost always dietary or transit-related. Chronic green stool (more than five days running, especially with diarrhea) is the form that deserves medical attention.
Newborn Meconium
Every newborn passes meconium, a sticky, tar-like dark green to black stool, during the first 24 to 48 hours after birth. This is normal. Meconium is made of intestinal cells, mucus, amniotic fluid, and bile, and clearing it is a baby’s first major milestone. Pediatric guidance from the American Academy of Pediatrics treats green meconium as expected, not a red flag.
Breastfed vs Formula-Fed Infants
After meconium clears, breastfed babies typically produce soft, mustard-yellow stool, occasionally yellow-green. Formula-fed babies tend to produce darker, more formed stool, sometimes greenish-tan. Persistent bright green frothy stool in a breastfed baby can indicate a foremilk-hindmilk imbalance (the baby is getting too much low-fat foremilk and not enough fat-rich hindmilk), which often resolves by letting the baby finish one breast before switching.
When Parents Should Call the Pediatrician
Our medical reviewers see this pattern most often in worried first-time parents. Call the pediatrician if green stool in an infant comes with refusing feeds, fewer than six wet diapers in 24 hours, fever above 100.4 degrees Fahrenheit (rectal) in babies under three months, visible blood, mucus, or a baby who seems unusually sleepy or limp.
Green Diarrhea: When the Color and Consistency Both Matter
A formed green stool is one signal. Green diarrhea is a louder one. The combination almost always means rapid transit, and rapid transit has a short list of causes worth taking seriously.

Rapid Transit Physiology
When food moves through the colon faster than usual, several things happen at once. Water doesn’t get absorbed, leaving stool watery. Bile pigment doesn’t get converted, leaving stool green. And electrolytes (sodium, potassium, chloride) don’t get reabsorbed, raising dehydration risk. In the US, this combination sends about 5 million adults to outpatient clinics or ERs every year.
Common Viral and Bacterial Culprits
Norovirus is the most common cause of acute green diarrhea in adults nationally. The CDC estimates 19 to 21 million Norovirus illnesses per year in the United States, with the typical episode running 24 to 60 hours. Salmonella, Campylobacter, Shigella, and pathogenic E. coli are the bacterial heavy hitters, frequently linked to undercooked poultry, raw eggs, contaminated produce, or restaurant outbreaks.
Hydration and Timing
A short bout of green diarrhea (under 24 hours, no fever, no blood) usually clears on its own with fluids and electrolyte drinks. Patients commonly ask us when to switch from home care to clinic care, and the simple rule is: more than three days, blood or mucus in stool, fever above 102 degrees Fahrenheit, severe abdominal pain, signs of dehydration (dry mouth, dizziness, dark urine, no urination in eight hours), or unintentional weight loss.
Red Flags
Specific signs that flip a routine bout into a same-day doctor visit include bloody or tar-black stool, projectile vomiting that won’t stop, fever above 102.5 degrees Fahrenheit, severe localized abdominal pain (especially right lower quadrant or right upper quadrant), confusion or lethargy, or diarrhea lasting more than seven days.
USA Statistics: How Common Is This?
Green stool itself isn’t tracked nationally, but the conditions that cause it are. The numbers help put your own situation in context.

Table 2: US Conditions That Commonly Produce Green Stool
| Condition | Annual US Burden | Notes | Source |
| Norovirus illnesses | 19 to 21 million per year | #1 cause of acute gastroenteritis | CDC Norovirus Burden Data |
| Salmonella infections | ~1.35 million per year | ~26,500 hospitalizations, ~420 deaths | CDC Salmonella Estimates |
| Giardia duodenalis infections | ~1.2 million estimated per year (13,829 reported in 2022) | Most common US intestinal parasite | CDC NNDSS Giardiasis Summary 2022 |
| IBS prevalence (adults) | 10 to 15% of US adults (~25 to 45 million) | Chronic alternating stool patterns | American College of Gastroenterology |
| Crohn’s disease | ~780,000 Americans diagnosed | Often produces green undigested bile in diarrhea | Crohn’s and Colitis Foundation |
| Celiac disease | ~1 in 133 Americans (~2.4 million) | Often undiagnosed; can cause loose green stool | NIDDK |
| Gallbladder surgeries (cholecystectomy) | ~700,000 per year | Bile acid changes common post-op | American College of Surgeons |
Same color symptom, very different conditions. A 48-hour viral bug, an autoimmune disease, and a post-surgical adjustment can all produce green stool. Patient history, timing, and accompanying symptoms (not color alone) drive the right diagnosis.
How Doctors Diagnose Green Stool Concerns
A primary-care visit for persistent green stool follows a predictable path. Knowing it ahead of time helps you bring the right information to the appointment.

Patient History and Food Diary
Your doctor will ask what you ate in the past three to seven days, what medications and supplements you take, your travel history, whether anyone in your household has similar symptoms, and your typical bowel pattern. A two- to three-day food diary often resolves the question without testing.
Stool Culture and GI PCR Panel
A stool culture or, more commonly today, a multi-target GI PCR panel checks for the major bacterial and viral pathogens at once. Modern PCR panels can identify 22 or more pathogens from one sample within 24 hours, with sensitivity above 95% for most targets. Our diagnostic network supports stool culture, GI PCR, and ova and parasites testing with home-collection options across major US cities.
Stool Ova and Parasites (O&P)
If travel history, well water exposure, or a freshwater outdoor activity is in the picture, doctors order an O&P exam to look for Giardia, Cryptosporidium, Entamoeba histolytica, and other protozoa. Three separate samples on different days are sometimes needed because parasite shedding is intermittent.
Calprotectin and Lactoferrin
These stool markers measure intestinal inflammation. Elevated fecal calprotectin (above 50 micrograms per gram in most US labs) points toward inflammatory bowel disease (Crohn’s, ulcerative colitis) rather than IBS, and helps decide whether colonoscopy is warranted.
Blood Tests
A CBC checks for anemia (from chronic blood loss) or elevated white blood cell count (infection). A CMP evaluates liver and kidney function. CRP and ESR measure systemic inflammation. Vitamin B12, folate, ferritin, and tissue transglutaminase IgA (celiac screen) round out a typical workup.
Imaging and Procedures
Abdominal ultrasound checks the gallbladder and bile ducts. CT scans assess for abscess, bowel obstruction, or appendicitis. Colonoscopy and upper endoscopy let gastroenterologists directly visualize the GI tract and biopsy suspicious areas. These are reserved for cases where stool and blood tests don’t give a clear answer.
At-Home Triage and When to Call a Doctor
Most green stool episodes never need a clinic visit. A few absolutely do. The table below maps the decision logic patients commonly ask us to clarify.
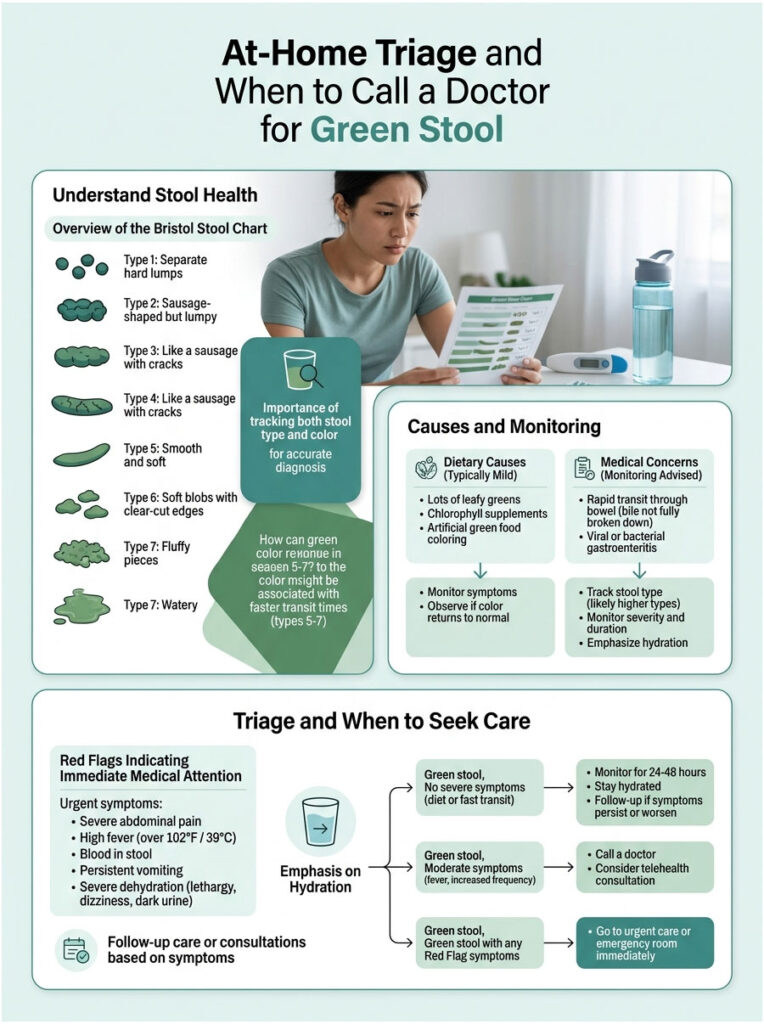
Bristol Stool Chart Context
The Bristol Stool Chart, developed at the University of Bristol and used widely in US clinics, classifies stool into seven types from hard pellets (Type 1) to entirely liquid (Type 7). Healthy formed stool sits at Types 3 and 4. Types 5, 6, and 7 indicate softer stool and faster transit, which is when green color most often shows up. Tracking your type along with color gives your doctor a much clearer picture than color alone.
Table 3: Green Stool Scenario to Recommended Action
| Scenario | What It Likely Suggests | Recommended Action |
| One or two green bowel movements after a kale smoothie, salad-heavy day, or party with blue frosting | Dietary chlorophyll or food dye | Watch and wait; expect normal color within 24 to 48 hours |
| Dark green or near-black stool after starting an iron pill or prenatal vitamin | Iron supplement effect | Continue supplement; mention at next visit if it bothers you |
| Loose green stool for 1 to 3 days, no fever, no blood, mild cramps | Mild viral gastroenteritis or stress | Hydrate with electrolyte drinks; rest; recheck in 48 hours |
| Green diarrhea more than 3 days, OR with fever above 102 degrees Fahrenheit, mucus, or visible blood | Possible bacterial or parasitic infection | See doctor within 24 hours; request stool GI PCR panel |
| Sudden bright green watery stool with vomiting, severe cramps, signs of dehydration | Possible food poisoning or severe gastroenteritis | Same-day urgent care or ER; rehydration may be required |
| Chronic green or yellow watery stool after gallbladder surgery | Bile acid malabsorption | Schedule a gastroenterology consult |
| Green stool with weight loss, night sweats, or chronic abdominal pain | Possible IBD, celiac, or other GI disease | Book full GI workup; consider colonoscopy |
Red flags requiring the nearest US emergency room: confusion or fainting, signs of significant dehydration (no urination in eight hours), severe localized abdominal pain, bloody or tarry stool with weakness, or stool changes in someone immunocompromised.
How to Get Your Stool Color Back to Normal
If the cause is benign, a few practical steps speed recovery and lower the chance of a repeat.

Hydration and Electrolyte Balance
Green diarrhea drains fluids fast. Pedialyte, Gatorade (in moderation, watching the dye), or homemade oral rehydration solution (six teaspoons of sugar plus a half teaspoon of salt per liter of water) restores electrolytes. Plain water alone isn’t enough for sustained diarrhea.
Dietary Reset
The BRAT diet (bananas, rice, applesauce, toast) is the traditional US recovery plan and still works. Add boiled potatoes, plain crackers, and broth-based soups. Hold off on raw vegetables, dairy, caffeine, alcohol, and fatty foods for 48 to 72 hours.
Probiotics and the Gut Microbiome
After antibiotic-associated green stool, probiotic strains like Saccharomyces boulardii and Lactobacillus rhamnosus GG have peer-reviewed evidence for restoring normal gut flora. Plain yogurt with live cultures works for milder cases. Talk to your doctor before starting probiotics if you’re immunocompromised.
Reviewing Supplements and Medications
If iron pills are causing the color, ask your doctor whether a lower dose, an every-other-day schedule, or a different formulation (ferrous bisglycinate is often easier on the gut) would still meet your needs. Don’t stop prescribed medications without checking first.
Stress Management
Chronic stress speeds gut transit and worsens IBS-pattern symptoms. Sleep, regular exercise, mindfulness practices, and treatment of underlying anxiety all help normalize bowel patterns over weeks.
Frequently Asked Questions
What does it mean if your poop is suddenly bright green?
Sudden bright green stool usually means recent intake of green or blue food dye, a chlorophyll-heavy meal, or rapid transit from mild diarrhea. If you can identify a food or supplement trigger within the past 24 to 48 hours, the explanation is almost always benign. Persistent bright green stool past three days deserves medical evaluation.
Can stress cause green stool?
Yes. Acute stress activates the vagus nerve and speeds intestinal transit, which is why anxious people often experience looser, greener stool before a stressful event. Chronic stress can also disrupt the gut microbiome, lowering the bacterial conversion of bile pigments. Stool color usually returns to normal once the stressor resolves or is managed.
How long does green stool typically last?
Most dietary or transit-related green stool clears within 24 to 48 hours after the trigger stops. Antibiotic-related green stool can last a few days into the course and a week or two after. Green stool from infection generally lasts as long as the infection (24 hours to 14 days). Persistent green stool beyond five days warrants a doctor’s visit.
Is green poop a sign of liver problems?
Generally no. Liver problems more commonly cause pale, clay-colored, or yellowish stool, not green. The exception is bile acid malabsorption, where excess bile reaches the colon (sometimes after gallbladder surgery). If green stool comes with yellowing skin or eyes, dark cola-colored urine, or right upper abdominal pain, see a doctor promptly to evaluate liver function.
Does Pepto-Bismol turn stool green?
Yes, sometimes. Bismuth subsalicylate (the active ingredient in Pepto-Bismol and Kaopectate) reacts with trace sulfur in your digestive tract and saliva, producing bismuth sulfide. This compound can darken stool to green, gray, or black. The effect is harmless and resolves within a few days of stopping the medication.
Can green stool indicate cancer?
Green stool alone is rarely a cancer sign. Colorectal cancer more typically causes red, dark red, or tarry-black stool from bleeding, along with weight loss, persistent abdominal pain, or change in bowel habits. If green stool comes with any of those red flags, or you’re over 45 (the current US screening threshold), schedule a colonoscopy discussion with your doctor.
What does green stool with mucus mean?
Mucus in stool can indicate intestinal inflammation from infection, IBS, or inflammatory bowel disease (Crohn’s or ulcerative colitis). Small amounts of clear mucus occasionally are normal. Green stool with persistent mucus, especially with cramping or blood, warrants a stool GI PCR panel, fecal calprotectin test, and a primary-care or gastroenterology visit.
Why is my newborn’s poop green?
The first stool a newborn passes (meconium) is normally dark green to black for 24 to 48 hours. After that, green stool can come from formula switches, maternal diet in breastfed babies, foremilk-hindmilk imbalance, or mild infection. Call the pediatrician if green stool comes with fever, refusing feeds, fewer than six wet diapers daily, or blood.
Can antibiotics turn stool green?
Yes. Antibiotics kill gut bacteria that convert bile pigments to brown, leaving stool greener than usual for the duration of the course and a few days after. Watery diarrhea more than five to seven days into an antibiotic course can signal C. difficile infection, which is more serious and needs medical evaluation.
Is green stool a sign of food poisoning?
It can be. Food poisoning from Salmonella, Campylobacter, E. coli, or Norovirus often produces green diarrhea because the infection speeds gut transit. Food poisoning typically also brings cramps, fever, nausea, vomiting, or urgency. Onset is usually within 6 to 48 hours of eating the suspected food. Most cases resolve in 24 to 72 hours with hydration.
Should I get tested for parasites if I have green stool?
Testing makes sense if green stool lasts more than seven days, you’ve traveled internationally or to areas with untreated water in the past month, you’ve swum in freshwater lakes or rivers, you drink from a private well, or you have other GI symptoms like bloating, weight loss, or greasy stool. A stool ova and parasites exam plus a Giardia antigen test is the standard US workup.
Does HealthCareOnTime offer stool testing?
Yes. Our diagnostic network supports stool culture, GI PCR multi-pathogen panels, ova and parasites exams, Giardia and Cryptosporidium antigen tests, fecal calprotectin, fecal occult blood, and H. pylori stool antigen testing. Home-collection options are available across major US cities, with results typically returned within 24 to 72 hours depending on the panel.
Medical Disclaimer: This article is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Symptoms that resemble simple green stool can sometimes mask serious conditions including inflammatory bowel disease, colorectal cancer, parasitic infection, and acute bacterial illness. Always consult a licensed US healthcare provider if your symptoms persist, worsen, or are paired with fever, blood, severe pain, dehydration, or unintentional weight loss. If you experience confusion, fainting, severe abdominal pain, or bloody stool with weakness, seek emergency care immediately.
References
- Harvard Health Publishing: Green poop and stool color meaning
- Mayo Clinic via Beacon Health System: Green stool causes
- Northwestern Medicine: Green Poop, What’s Going On?
- Healthline: Why Is My Poop Green? 6 Possible Causes
- CDC: Norovirus Burden in the United States
- CDC: Salmonella Information
- CDC: Giardiasis NNDSS Summary Report 2022
- American College of Gastroenterology: Irritable Bowel Syndrome
- NIDDK: Symptoms and Causes of Diarrhea
- Crohn’s and Colitis Foundation: Crohn’s Disease Facts
- American Academy of Pediatrics: Bowel Movements in Babies
- GoodRx: Why Is Your Poop Green and Should You Be Concerned?