You did everything right. Skipped the late coffee, dimmed the lights, climbed into bed by ten. And still, at 3 a.m., you are wide awake, staring at the ceiling, doing math on how few hours are left. If that sounds familiar, here is the part most women are never told: this is not simply “getting older.” It is a measurable shift in your body’s chemistry, and one of the most studied tools for steadying it sits on every drugstore shelf.
Table of Contents
Quick Answer: Magnesium glycinate is a gentle, well-absorbed supplement that can help women over 40 sleep better by calming the nervous system, supporting GABA and melatonin, and easing muscle tension. Most women take 200 to 350 mg of elemental magnesium about 30 to 60 minutes before bed, with benefits building over one to three weeks. It is not a sedative and will not treat sleep apnea, so pair it with solid sleep habits and a clinician’s guidance.

At a Glance
- Sleep problems peak in perimenopause, when most women aged 40 to 59 sleep less than seven hours a night.
- Magnesium glycinate is magnesium bound to glycine, a calming amino acid, making it well absorbed and easy on the stomach.
- A 2025 clinical trial found magnesium bisglycinate measurably reduced insomnia severity, with most gains inside the first two weeks.
- Typical sleep dosing is 200 to 350 mg of elemental magnesium, taken in the evening.
- Results are gradual, not instant. Think nutritional support, not a knockout pill.
- Loud snoring, gasping, or morning headaches point to sleep apnea, which magnesium cannot fix.
Why Sleep Falls Apart for Women After 40
Sleep does not slowly fade with age in a straight line. For women, it tends to hit a wall, and that wall has a name: the menopause transition. Somewhere in the early to mid-40s, the ovaries begin producing estrogen and progesterone less predictably.

Those two hormones are not only reproductive signals. They also help run your sleep machinery. Progesterone has a mild sedative effect, and estrogen helps regulate body temperature and mood. When both start swinging, sleep is often the first thing to break.
Patients booking hormone panels with us often describe the same pattern. They fall asleep fine, then snap awake between 2 and 4 a.m., sometimes drenched in sweat, sometimes just alert for no reason at all.
The Hormone Shift Behind Midlife Insomnia
Declining progesterone removes a natural calming influence right when you need it most. Progesterone supports a soothing brain chemical, so when levels drop, that built-in calm goes with it.
Falling estrogen disrupts the body’s temperature control, which is why hot flashes and night sweats so often surface in the dark. Estrogen also influences mood-regulating chemicals, and when it dips, anxiety and low mood can creep in, both of which feed insomnia.
Add a cortisol system that grows more reactive with age, and your brain has a harder time switching off. Stress, caregiving for both kids and aging parents, and a slowing metabolism stack on top. Sleep starts to feel like a skill you somehow lost.
Night Sweats, Anxiety, and the 3 a.m. Wake-Up
The classic midlife complaint is not trouble falling asleep. It is trouble staying asleep. A night sweat can jolt you awake, and once estrogen-driven temperature swings collide with a racing mind, getting back to sleep can take an hour or more.
There is also the bladder factor. Many women over 40 wake at least once a night for the bathroom, and each trip is another chance for the mind to switch on. The result is sleep that is broken into pieces rather than truly restorative.
The numbers confirm this is not rare. According to the CDC’s National Center for Health Statistics, perimenopausal women are the group most likely to sleep under seven hours a night, well ahead of premenopausal and postmenopausal women. The Sleep Foundation reports that sleep disorders affect 39 to 47 percent of perimenopausal women and 35 to 60 percent of postmenopausal women.
Our medical reviewers note that many women arrive convinced they simply need more willpower at bedtime. The data tells a kinder story: this is biology, and biology responds to the right support.
| Sleep Statistic (USA Women) | Figure | Source |
| Perimenopausal women sleeping under 7 hours per night | 56.0% | CDC NCHS Data Brief No. 286 |
| Women aged 40-59 not waking well rested 4+ days per week | 48.9% | CDC NCHS Data Brief No. 286 |
| Sleep disorders among perimenopausal women | 39-47% | Sleep Foundation |
| Sleep disorders among postmenopausal women | 35-60% | Sleep Foundation |
| Magnesium bisglycinate vs placebo insomnia score drop | 3.9 vs 2.3 pts | Nature and Science of Sleep, 2025 |
What Magnesium Glycinate Actually Is
Magnesium is a mineral your body cannot make, so it has to come from food or supplements. It runs an enormous share of your internal chemistry. The Mayo Clinic notes that magnesium is essential for more than 300 enzyme systems involved in biochemical reactions throughout the body.
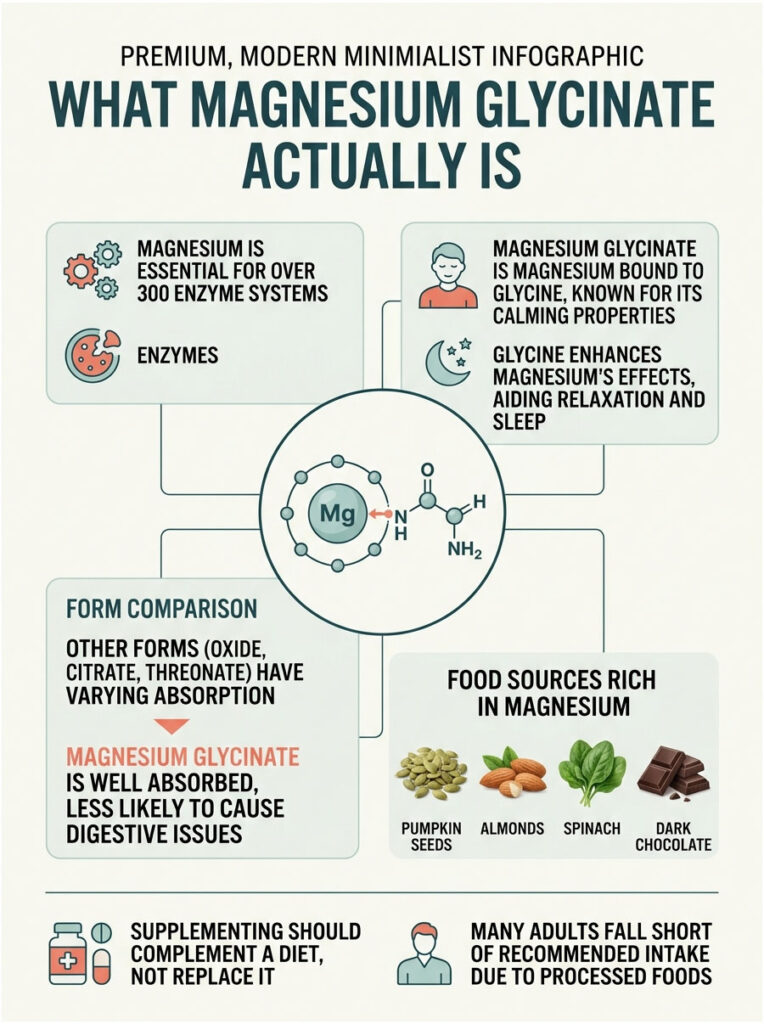
Magnesium glycinate is one specific form: the mineral chemically bound to glycine, an amino acid. You may also see it labeled “magnesium bisglycinate,” which means two glycine molecules per magnesium atom. For practical purposes, treat the two names as the same product.
Magnesium Plus Glycine, and Why the Pairing Matters
That pairing is the whole point. Glycine is not filler. It is a calming neurotransmitter in its own right, one that supports a slight drop in body temperature and helps quiet the brain at night.
So magnesium glycinate works on two fronts at once. The magnesium relaxes muscles and steadies the nervous system, while the glycine adds its own gentle, sleep-friendly effect. Few other forms give you that built-in second ingredient.
Why This Form Over Oxide, Citrate, and Threonate
Not all magnesium is built for sleep. The drugstore shelf holds several forms, and they behave very differently once they reach your gut.
Magnesium oxide is cheap but poorly absorbed, and it is mostly used for occasional constipation. Magnesium citrate absorbs better but tends to loosen stools, which is the opposite of restful. Magnesium threonate is marketed for brain health, though the evidence is still thin.
Magnesium glycinate sits in the sweet spot. As Banner Health explains, it is well absorbed, may support sleep and relaxation, and is less likely to cause digestive issues like diarrhea. For a woman who wants calm without a midnight bathroom trip, that profile is hard to beat.
Food First: Magnesium-Rich Choices
Before reaching for a bottle, it helps to know that food is the foundation. A large share of American adults fall short of recommended magnesium intake, often because processing strips the mineral from packaged foods.
Magnesium-rich options are easy to add to a daily routine: pumpkin seeds, almonds, cashews, spinach, black beans, edamame, whole grains, and even dark chocolate. Building these into meals raises your baseline, and a supplement then fills whatever gap is left rather than doing all the work alone.
How Magnesium Helps You Sleep: The Science
It helps to know why a supplement works before you trust it. Magnesium is not sedating in the way a sleeping pill is. It works upstream, by helping your nervous system do its own job of winding down.

The GABA and Off-Switch Connection
GABA is your brain’s main calming chemical. It is the signal that tells an overactive mind to power down. Magnesium helps GABA bind to its receptors, so low magnesium can leave that off-switch sticky and slow.
This is why a magnesium shortfall so often shows up as a brain that will not stop narrating at midnight. Restoring adequate levels gives GABA a better chance to do its work, which is exactly the support a wired midlife brain needs.
Melatonin and Cortisol Regulation
Magnesium also plays a supporting role with melatonin, the hormone that anchors your sleep-wake cycle. And it appears to help blunt cortisol, the stress hormone that should be low at night but often is not in midlife.
When cortisol stays elevated into the evening, your body reads it as a signal to stay alert. Magnesium’s calming effect on the stress response helps tip the balance back toward rest.
If you feel physically tense at bedtime, or your legs feel restless, magnesium’s muscle-relaxing effect adds another layer. Across the patients HealthCareOnTime serves, that “wired but tired” feeling is one of the most common sleep complaints we hear in the 40-plus age group.
What the 2025 Clinical Trial Actually Found
For years, the magnesium-and-sleep story leaned on small studies and theory. That changed with a 2025 randomized, double-blind, placebo-controlled trial published in Nature and Science of Sleep.
The study enrolled 155 adults aged 18 to 65 who reported poor sleep quality. Participants were randomly assigned to either magnesium bisglycinate (250 mg of elemental magnesium daily) or a matching placebo, and sleep was tracked with the Insomnia Severity Index over four weeks.
The result was modest but real. The magnesium group saw a greater reduction in insomnia scores than placebo (a 3.9 versus 2.3 point drop), and most of that improvement showed up within the first 14 days and held steady. The supplement was also well tolerated, with fewer adverse events than the placebo group.
Two details matter for women over 40. The benefit appeared fast, inside two weeks, and it was strongest in people who started with lower dietary magnesium intake. If your diet is light on leafy greens, nuts, and beans, you are exactly the person this kind of supplement tends to help most.
It is worth keeping the honesty intact here. The effect was meaningful but not dramatic, which is precisely why magnesium belongs in a sleep plan rather than as the whole plan.
Magnesium Glycinate vs Other Sleep Options
Magnesium glycinate is one tool, not the only tool. Knowing how it stacks up against the alternatives helps you build a plan that actually fits your situation.
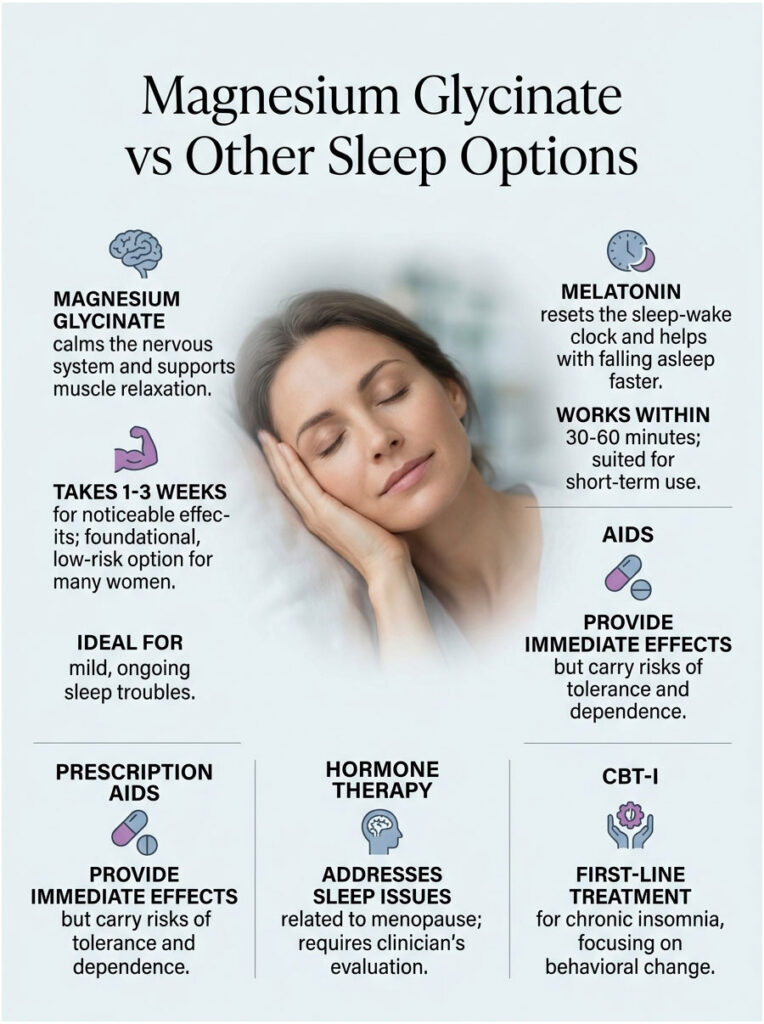

Magnesium Glycinate vs Melatonin
Melatonin is a hormone that tells your body it is nighttime. It is genuinely useful for shifting a sleep schedule, such as after travel or a shift change, and it helps you fall asleep faster.
Magnesium glycinate is a mineral, not a hormone. It does not force sleep on a schedule. Instead, it lowers the background noise so sleep can arrive and hold. Because they work through different pathways, some women use both.
One caution is worth flagging. A recent observational analysis raised questions about long-term nightly melatonin use and heart health, an association that researchers stress is not proof of cause. Patients commonly ask us whether melatonin is “safe forever,” and the honest answer is that it is best suited to short-term, occasional use rather than every single night for years.
Magnesium Glycinate vs Prescription Aids and Hormone Therapy
Prescription sleep medications work, and quickly, but they carry tolerance, grogginess, and dependence risk. They are a clinician’s call, not a casual choice. Hormone therapy can be genuinely effective when hot flashes and night sweats are the root cause, and it deserves a real conversation with a menopause-informed provider.
Cognitive behavioral therapy for insomnia, or CBT-I, is considered the first-line treatment for chronic insomnia and outperforms pills over the long run. Magnesium glycinate is not a competitor to any of these. It is the low-risk foundation many women build on first.
| Sleep Option | How It Works | Typical Onset | Best For | Key Drawback |
| Magnesium glycinate | Calms nervous system, supports GABA and muscle relaxation | 1-3 weeks of daily use | Mild, ongoing midlife sleep trouble; low magnesium intake | Gradual; not a quick fix |
| Melatonin | Signals nighttime to reset the sleep-wake clock | 30-60 minutes | Jet lag, shift work, trouble falling asleep | Best for short-term use only |
| Magnesium citrate | Magnesium in a more laxative-prone form | 1-3 weeks | Sleep plus occasional constipation | Loose stools disrupt rest |
| CBT-I | Retrains thoughts and habits around sleep | 4-8 weeks | Chronic insomnia, first-line therapy | Requires time and consistency |
| Hormone therapy | Replaces declining estrogen and progesterone | Weeks | Sleep driven by hot flashes, night sweats | Needs clinician evaluation |
| Prescription sleep aids | Sedate the brain directly | Same night | Short-term, severe insomnia | Tolerance and dependence risk |
How to Take Magnesium Glycinate for Sleep After 40
Getting the dose and timing right is what separates “this did nothing” from “this actually helped.” The good news is that the rules are simple.

Dosage by Life Stage
The NIH Office of Dietary Supplements sets the recommended dietary allowance for women aged 31 and older at 320 mg of magnesium per day, counting food and supplements together. The upper limit for supplemental magnesium specifically is 350 mg per day for adults.
For sleep, a common starting point is 200 mg of elemental magnesium in the evening, with room to move toward 300 to 350 mg if your body tolerates it well. Perimenopausal women with active symptoms often land in the middle of that range. Postmenopausal women may do well at a steady, lower maintenance dose, since the goal shifts toward keeping stores topped up.
Here is the simple logic in practice. Start low for a week and watch how you feel and how your digestion responds. If sleep is improving and your stomach is fine, you can hold there. If you want a little more support and tolerate it well, step up gradually, never past the supplemental upper limit without medical guidance.
The phrase to watch is “elemental magnesium.” A capsule may list a large compound weight, but the elemental number is the dose that counts. More is not better here, and exceeding the limit invites side effects rather than deeper sleep.
Timing and Pairing With Food
Take it 30 to 60 minutes before bed if your main goal is sleep. Consistency matters more than perfect timing, because magnesium works by rebuilding your body’s stores over weeks, not by sedating you on the spot.
Splitting the dose, with part earlier in the day and part at night, can improve absorption and reduce any stomach upset. Taking it with a small amount of food helps too. Our lab partners report that women who treat it as a nightly habit, rather than an occasional rescue, see the steadiest results.
Reading the Label
Choose a product that clearly says “magnesium glycinate” or “magnesium bisglycinate” and lists the elemental magnesium per serving. Because the FDA does not review supplements for effectiveness before sale, third-party testing is your quality signal.
Look for a seal from USP, NSF, or ConsumerLab on the bottle. Brands such as Thorne, Pure Encapsulations, and Doctor’s Best are commonly cited as third-party tested, though many solid options exist. Avoid blends padded with magnesium oxide, which dilute the gentle, well-absorbed form you actually want.
What to Expect: Timeline and Realistic Results
Honest expectations protect you from quitting too soon. Magnesium glycinate is not a sleeping pill, and judging it like one sets you up for disappointment.

The One to Three Week Window
Some women notice a calmer, heavier sleep within a few nights. For most, the meaningful change builds over one to three weeks of consistent nightly use. That timeline matches what the 2025 trial showed, with gains landing inside the first two weeks and holding steady.
If you have taken it nightly for a month with no change at all, that is useful information rather than a failure. It may mean your sleep problem has a different root, which is worth investigating instead of doubling the dose.
Support, Not Sedation
Think of magnesium glycinate as nutritional groundwork for your nervous system. It removes a common obstacle to good sleep; it does not override every other one. Stress, an irregular schedule, late screens, alcohol, and untreated sleep disorders can all still keep you awake.
In cases reviewed across our diagnostic network, the women who get the most from magnesium are the ones who pair it with a steady wind-down routine rather than expecting the capsule to carry the entire load.
Safety, Side Effects, and Who Should Avoid It
For most healthy women, magnesium glycinate is one of the lower-risk supplements available. Its gentler profile is precisely why it gets recommended for sleep over harsher forms.

Common Side Effects and How to Prevent Them
The most likely side effect is mild digestive upset or loose stools, and even that is less common with glycinate than with other forms. Starting low, taking it with food, and splitting the dose almost always solves it.
Very high doses can cause nausea or next-day drowsiness. Staying at or below the 350 mg supplemental limit keeps you well clear of trouble in nearly all cases. Magnesium glycinate is not habit-forming, so there is no withdrawal concern if you stop.
Medication Interactions and Kidney Concerns
This is where caution genuinely matters. Magnesium can affect how some medications are absorbed, including certain antibiotics and thyroid medication, so doses may need to be spaced several hours apart.
Anyone with reduced kidney function should not start magnesium supplements without medical clearance, because impaired kidneys cannot clear excess magnesium efficiently. The same goes for women who are pregnant or taking diuretics or heart medications. The Mayo Clinic advises talking with your healthcare team before starting magnesium, especially with kidney disease, pregnancy, or other medications in the picture.
| Your Situation | What It Might Mean | Recommended Action |
| Mild trouble staying asleep, diet low in greens and nuts | Possible low magnesium intake | Try 200 mg elemental magnesium glycinate nightly; reassess in 3 weeks |
| Loose stools after starting | Dose too high or taken on empty stomach | Lower the dose, take with food, split it across the day |
| No change after 4 weeks of consistent use | Sleep issue may have another cause | Stop guessing; ask a clinician about testing and CBT-I |
| Loud snoring, gasping, or morning headaches | Possible sleep apnea | See a doctor for a sleep evaluation; magnesium will not treat this |
| Taking thyroid meds, antibiotics, or heart medication | Risk of absorption interaction | Space doses several hours apart; confirm with your pharmacist |
| Known kidney disease or pregnancy | Higher risk from excess magnesium | Do not self-supplement; get medical clearance first |
When Magnesium Isn’t Enough: Red Flags and Next Steps
Magnesium glycinate is a fair first step, but it is not a diagnosis. Some sleep problems need medical attention, and treating them as a supplement issue only delays relief.

Signs It Could Be Sleep Apnea or Another Disorder
Sleep apnea becomes more common in women after menopause, and it is widely underdiagnosed. Warning signs include loud snoring, choking or gasping awake, waking with a headache, and crushing daytime fatigue despite a full night in bed.
Restless legs syndrome, thyroid disorders, anxiety, and depression can also masquerade as ordinary insomnia. No supplement corrects these conditions. They need a proper workup and, often, a targeted treatment plan.
When to Ask for Testing
If poor sleep has lasted more than a few weeks, or it is dragging down your mood, focus, and daily function, that is the signal to investigate rather than self-treat. A simple blood panel can check magnesium status, thyroid function, vitamin D, and hormone levels, which together explain a large share of midlife sleep complaints.
Patients booking lab work with us often find that one quiet, fixable factor, low vitamin D or an underactive thyroid, was part of the puzzle all along. Knowing your numbers turns guesswork into a plan, and it tells you whether magnesium is the right tool or only a piece of a larger picture.
Building a Sleep Routine That Works With Magnesium
A supplement performs best inside a routine that respects how sleep actually works. These habits cost nothing and multiply whatever benefit magnesium provides.

Sleep Hygiene Basics That Multiply the Benefit
Keep a consistent wake-up time, even on weekends, since that anchor sets your whole sleep-wake rhythm. Make the bedroom cool, dark, and quiet, which matters even more when night sweats are in play. A lower room temperature works with magnesium and glycine rather than against them.
Cut caffeine after noon and be honest about alcohol. A nightcap may help you fall asleep, then fragments the second half of your night, exactly the stretch midlife women already struggle to hold. Daylight in the morning and movement during the day both strengthen the same internal clock.
A Simple Evening Checklist
Aim to dim screens an hour before bed, or at least switch on night mode. Take your magnesium glycinate with that wind-down. Add a calm ritual: a warm shower, light stretching, reading on paper, or slow breathing.
Keep the bedroom for sleep, not for scrolling or work. If you are awake for more than 20 minutes, get up, do something dull in low light, and return when sleepy. Done nightly, these steps and a steady magnesium habit give your body its best shot at the rest it has been missing.
Frequently Asked Questions
How much magnesium glycinate should I take for sleep?
Most women start at 200 mg of elemental magnesium in the evening and may move toward 300 to 350 mg if well tolerated. Keep total supplemental magnesium at or below 350 mg per day unless a clinician advises otherwise. Always read the label for the elemental dose.
How long does magnesium glycinate take to work?
Some women feel calmer sleep within a few nights, but the meaningful change usually builds over one to three weeks of consistent nightly use. The 2025 trial found most improvement landed inside the first two weeks. If nothing shifts after a month, the cause may lie elsewhere.
Is it safe to take magnesium glycinate every night?
For most healthy women, nightly use at recommended doses is considered safe and is not habit-forming. Magnesium glycinate is among the gentler forms. The exceptions are women with kidney disease, pregnancy, or interacting medications, who should get medical clearance before starting.
Magnesium glycinate vs melatonin, which is better after 40?
They do different jobs. Melatonin resets the sleep-wake clock and helps you fall asleep, ideal for jet lag or short-term use. Magnesium glycinate calms the nervous system over time and suits ongoing midlife sleep trouble. Some women use both, ideally with a clinician’s input.
Can magnesium glycinate help with menopause night sweats?
Magnesium does not directly stop hot flashes or night sweats, which are driven by declining estrogen. It can ease the anxiety, muscle tension, and restlessness that surround them, making the disruption less severe. For frequent, intense night sweats, ask a provider about hormone therapy options.
What is the best time to take magnesium glycinate?
If sleep is your goal, take it 30 to 60 minutes before bed. Consistency matters more than exact timing, since magnesium works by rebuilding your stores over weeks. Splitting the dose, part earlier and part at night, can improve absorption and reduce any stomach upset.
Magnesium glycinate vs citrate, which is better for sleep?
Magnesium glycinate is generally the better sleep choice because it is well absorbed and gentle on digestion. Magnesium citrate also absorbs well but has a stronger laxative effect, which can disturb sleep. Citrate suits people who want help with occasional constipation alongside magnesium support.
Can magnesium glycinate cause weight gain?
No. Magnesium glycinate does not cause weight gain. By supporting better sleep and a calmer stress response, it may even help, since poor sleep is itself linked to weight gain. Any supplement claiming dramatic weight effects should be treated with healthy skepticism.
Are there side effects for women over 50?
Side effects are uncommon at recommended doses and usually limited to mild digestive upset. Women over 50 are more likely to take medications and to have changing kidney function, so a quick check with a doctor or pharmacist before starting is a sensible precaution.
Can I take magnesium glycinate with my blood pressure medication?
Sometimes, but not without checking first. Magnesium can affect blood pressure and interact with certain heart and diuretic medications. Some blood pressure drugs also alter magnesium levels. Confirm with your prescribing clinician or pharmacist before combining them.
Should I get my magnesium levels tested first?
Standard blood tests do not always reflect total-body magnesium well, since most of it sits inside cells and bone. Still, a blood panel checking magnesium alongside thyroid, vitamin D, and hormones can reveal fixable causes of poor sleep. Testing is especially worthwhile if sleep problems persist.
Does magnesium glycinate help with anxiety-related insomnia?
It may. Magnesium supports GABA, the brain’s calming signal, and the glycine component adds its own soothing effect. Many women report a quieter mind at bedtime. It is supportive rather than a treatment for an anxiety disorder, which deserves its own care if symptoms are significant.
Disclaimer: This article is for general educational purposes and is not medical advice. It does not diagnose, treat, or replace care from a licensed healthcare professional. Dietary supplements are not reviewed by the FDA for effectiveness, and individual needs vary. Talk with your doctor or pharmacist before starting magnesium glycinate, especially if you are pregnant, have kidney disease, or take other medications.
References
- CDC, National Center for Health Statistics, Data Brief No. 286: Sleep Duration and Quality Among Women Aged 40-59 by Menopausal Status
- Sleep Foundation: Sleep Statistics, Facts and Data About Sleep
- Nature and Science of Sleep (2025): Magnesium Bisglycinate Supplementation in Healthy Adults Reporting Poor Sleep, A Randomized, Placebo-Controlled Trial
- NIH Office of Dietary Supplements: Magnesium Fact Sheet for Health Professionals
- Mayo Clinic Press: Magnesium Glycinate, Is This Supplement Helpful for You?
- Banner Health: What Is Magnesium Glycinate? Health Benefits and Safety
- U.S. Food and Drug Administration: Information for Consumers on Using Dietary Supplements