You sat down. The phlebotomist tied the tourniquet. Then the room went sideways and your last clear memory was the ceiling tile pattern.
Table of Contents
If that’s happened to you, you have a lot of company. Roughly one in three Americans will have a vasovagal fainting episode in their lifetime, according to NIH StatPearls. The blood-draw chair is one of the most common places it strikes. Almost every faint is preventable once you know the playbook.

Quick Answer: Most blood-draw faints are caused by vasovagal syncope, a brief automatic drop in heart rate and blood pressure triggered by stress, the sight of blood, dehydration, or low blood sugar. Prevent it by drinking 16 to 20 ounces of water beforehand, eating a complex-carb plus protein snack, lying down during the draw, and using applied muscle tension. Tell your phlebotomist about past faints.
At a Glance
- Vasovagal syncope causes about 50% of all US fainting episodes (NIH StatPearls)
- Lifetime prevalence in adults: 33 to 42%
- Roughly 25% of US adults report fear of needles (McLenon & Rogers, J Adv Nurs 2019)
- The applied tension technique cuts blood-draw faints by 50 to 90% in needle-phobic patients
- LabCorp, Quest, and most US labs will let you lie down if you ask
- Eating a balanced snack 1 to 2 hours before stabilizes blood sugar and pressure
- Home and mobile phlebotomy removes most environmental triggers
What Actually Happens When You Faint at a Blood Draw
Fainting during bloodwork isn’t weakness, drama, or a personality flaw. It’s a hardwired reflex called vasovagal syncope, and your nervous system runs the show whether you give permission or not.
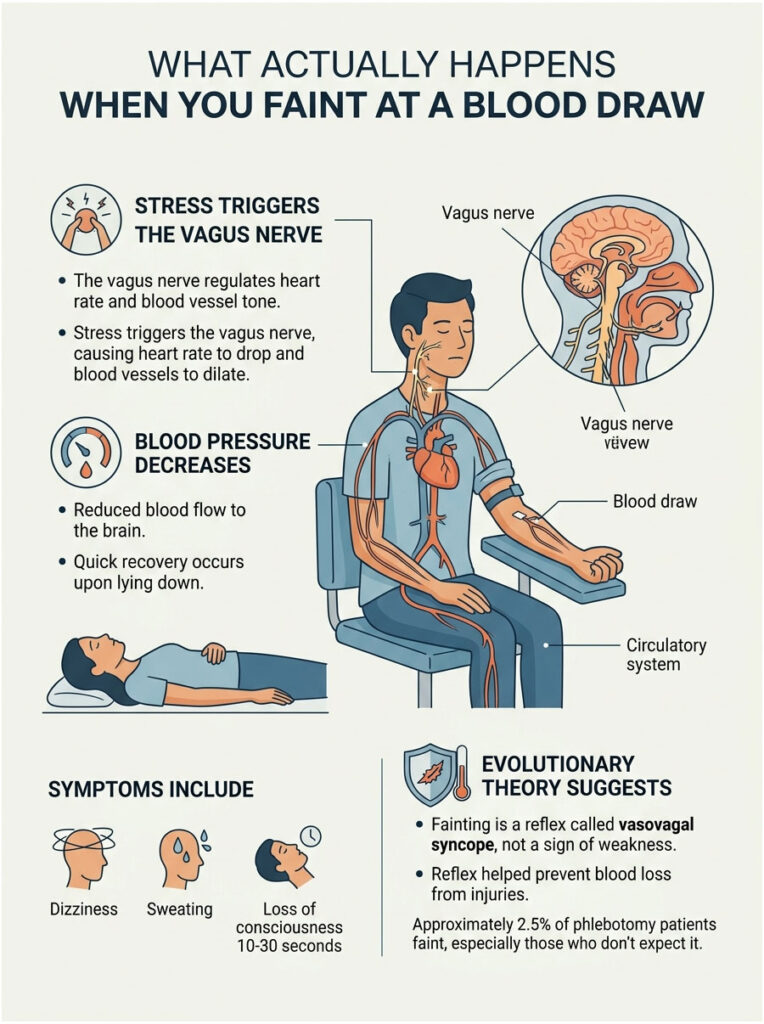
The Vagus Nerve Slams the Brakes
Your vagus nerve helps regulate heart rate and blood vessel tone. When something stresses you (pain, the sight of blood, even just thinking about a needle), the vagus nerve can overreact.
It drops your heart rate and dilates your blood vessels at the same time. Blood pressure tanks. Less blood reaches your brain. You feel dizzy, hot, sweaty, then cold, then the lights go out for 10 to 30 seconds.
Recovery is usually quick once you’re horizontal again.
Why Evolution May Have Wired You This Way
One leading theory: in our ancestors, an injury that drew blood could be life-threatening. A sudden drop in blood pressure may have helped reduce blood loss and clot wounds faster. Your body interprets a needle stick as the start of an “injury,” and obliges by playing dead.
I’ve worked alongside mobile phlebotomists across the US for years. The patients who faint most often are the ones who didn’t think they would. The reflex doesn’t care about your willpower.
How Common Is This, Really?
Syncope causes roughly 740,000 emergency department visits and 250,000 hospital admissions in the US every year, costing about $2.4 billion annually (NIH StatPearls).
Among people under 40, more than 85% of fainting episodes are vasovagal in origin. Approximately 2.5% of all phlebotomy patients pass out or come close to it. Across the thousands of blood draws happening at LabCorp, Quest, and hospital labs every day, that adds up to a lot of pale faces and ice packs.
Why Some People Are More Likely to Faint Than Others
Two people sit in the same chair, with the same phlebotomist, on the same morning. Only one goes down. The lottery isn’t random.
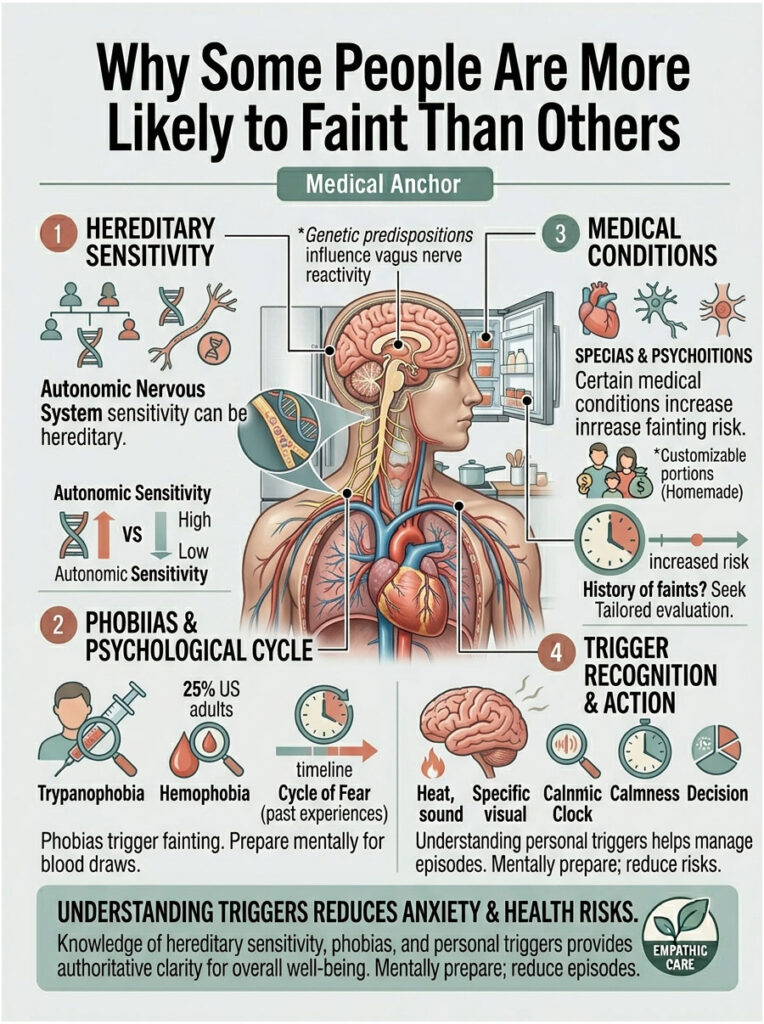
Your Autonomic Nervous System Is Just More Sensitive
Some people have a more reactive vagus nerve baseline. If your parents or siblings faint at blood draws, you’re statistically more likely to as well.
Genetic studies have flagged differences in autonomic regulation that run in families. It’s a hand-me-down trait, like flat feet or curly hair.
Needle Phobia (Trypanophobia) and Blood Phobia (Hemophobia)
About 25% of US adults report meaningful fear of needles. Roughly 1 in 10 has clinically significant trypanophobia, per the 2019 systematic review in the Journal of Advanced Nursing.
These phobias are unusual because they’re the only ones where the typical anxiety response (high heart rate, high BP) flips into the opposite (low heart rate, low BP) within seconds. That biphasic response is exactly what makes you faint instead of just panic.
The “One Bad Experience” Cycle
Fainted once at a draw? Your brain logs it as a threat. The next time you sit down, your body starts the vasovagal cascade before the needle is anywhere near you.
I’ve seen patients who can describe their first faint from 20 years ago in cinematic detail. Their nervous system never let it go. One man told me he could still smell the alcohol swab from his sixth-grade physical.
Medical Conditions That Stack the Deck
Several conditions raise your baseline risk:
- Anemia (low hemoglobin reduces oxygen delivery to the brain)
- Dehydration (less blood volume to begin with)
- Low blood pressure (you don’t have much room to drop)
- POTS (postural orthostatic tachycardia syndrome)
- Pregnancy, especially first and second trimester
- Recent illness, surgery, or fasting beyond 12 hours
If you have any of these and you’ve fainted before, treat your next blood draw like a planned event, not a quick errand.
Warning Signs You’re About to Faint (the prodrome window)
Most blood-draw faints don’t happen out of nowhere. Your body sends a 30 to 90 second warning called the prodrome. Catch the signals early and you can almost always head off the actual blackout.

What the Prodrome Feels Like
The classic combo: lightheadedness, a wave of warmth, a sudden cold sweat on your forehead or upper lip, ringing ears, tunnel vision, nausea, and the urgent feeling that you need to lie down right this second.
Some people yawn repeatedly. Others feel a strange detachment, like they’re watching themselves from outside their body.
The 30-Second Rule for Speaking Up
If you notice any of these signs, tell your phlebotomist immediately. Don’t wait. Don’t try to tough it out. Don’t worry about being dramatic.
In my work with home-blood-draw teams, the patients who say something at the first whisper of dizziness almost never lose consciousness. The ones who try to ride it out often end up on the floor.
Table 3: Warning Sign Decision Guide
| Warning Sign | What It Means | What to Do Right Now |
| Lightheaded, room spinning | Blood pressure dropping fast | Say “I feel faint” and lower your head between your knees, or recline if possible |
| Cold sweat on forehead, upper lip, or back of neck | Vasovagal cascade has started | Tell phlebotomist to pause; start applied tension immediately |
| Tunnel vision, dimming sight | Brain perfusion dropping critically | Get horizontal NOW, raise your legs above heart level |
| Nausea, sudden hot flush | Vagal response peaking | Pause draw, breathe slowly through your nose, sip water if available |
| Ringing in ears, muffled hearing | Pre-syncope, faint imminent within 30 seconds | Lie back, raise legs, stay still until vision clears |
How to Stop Fainting During a Blood Draw: 11 Proven Tips
Here’s the playbook I give every patient who tells me they have a fainting history. Work through it as a sequence, not a buffet. The “before” steps matter as much as the “during” steps.

Before the Draw (5 Tips)
1. Hydrate for 24 Hours, Not 24 Minutes
Drink at least 64 ounces of water the day before your draw. Add another 16 to 20 ounces in the two hours leading up to it. Better hydration means more blood volume and more cushion when your blood pressure dips.
If you’re fasting for the test (cholesterol, glucose, comprehensive metabolic panel), water is still allowed and actively encouraged.
2. Eat the Right Pre-Draw Meal (when you’re not fasting)
Pair a complex carbohydrate with a protein source 1 to 2 hours before. Think oatmeal with peanut butter, a turkey sandwich on whole-grain bread, or Greek yogurt with berries and granola.
Skip sugary cereals, donuts, and fruit juice. They spike blood sugar fast then crash it, and a crash mid-draw is exactly what you don’t want.
3. Sleep Well the Night Before
Sleep deprivation lowers your vasovagal threshold. Your nervous system overreacts more easily on 4 hours of sleep than 8.
Aim for 7 to 8 hours. Mayo Clinic and the American Academy of Family Physicians both flag poor sleep as a syncope risk factor.
4. Schedule Strategically
Book the earliest morning appointment you can get. You’ll be less anxious from a long wait, the lab is cooler and quieter, and you can eat right after instead of stewing all day.
Avoid back-to-back stressful events. A blood draw stacked with a job interview or school drop-off scramble loads your nervous system before the needle ever appears.
5. Tell Your Phlebotomist (the single highest-impact step)
Walk in and say one sentence: “I have a history of fainting during blood draws. I’d like to lie down for this one.” Every reputable US lab will accommodate that request.
I’ve seen patients who avoided routine bloodwork for years finally get it done because someone simply asked if they could lie down. The accommodation is free, takes no extra time, and prevents the vast majority of faints.
During the Draw (5 Tips)
6. Choose Your Position: Lie Down or Recline
Sitting upright is the default in most US patient service centers, but it’s also the position with the highest fainting risk. If you’ve fainted before, ask for a draw bed or a fully reclining chair.
If neither is available, recline as far as the chair allows and prop your feet up on a second chair. The goal: keep blood flowing easily to your brain.
7. Use the Applied Tension Technique
This is the most underused tool in fainting prevention. Tense your leg, glute, and core muscles for 10 to 15 seconds, release for 20 to 30 seconds, then repeat. The muscle contractions push blood back toward your heart and brain, raising your blood pressure.
Start the cycles when you sit down and continue throughout the draw. (Full step-by-step in the next section.)
8. Look Away From the Needle
For visual triggers, line of sight matters. Turn your head toward your other shoulder. Watch a video on your phone. Stare at a poster on the wall. The phlebotomist doesn’t need you to supervise.
If looking away isn’t enough, close your eyes and picture a calming scene (the beach, your kitchen, your dog’s face). Mental imagery genuinely lowers vagal reactivity.
9. Use Controlled Breathing (the 4-7-8 method)
Inhale through your nose for 4 seconds, hold for 7 seconds, exhale slowly through your mouth for 8 seconds. Repeat three to four cycles. This activates your parasympathetic system in a slow, controlled way that competes with the chaotic vasovagal cascade.
Cleveland Clinic recommends this technique for general anxiety and pre-procedure jitters too.
10. Distract Your Brain Hard
Talk to the phlebotomist about literally anything (the weather, your weekend, the worst movie you’ve seen recently). Put on a playlist with earbuds. Count backward from 100 by 7s. Your conscious mind has limited bandwidth.
I once watched a patient sing the entire chorus of “Bohemian Rhapsody” through a 4-tube draw without flinching. It worked.
After the Draw (1 Tip)
11. Stay Seated for 5 Minutes and Rehydrate
Don’t leap up and walk to your car. Your blood pressure can drop again the moment you stand (orthostatic hypotension). That’s when people faint in parking lots and hit their heads on concrete.
Sip water or juice. Eat a small snack if you brought one. Wait until you feel completely steady before standing, and stand slowly. If the lab offers cookies or juice (many do, especially after multi-tube draws or donations), accept them.
The Applied Tension Technique, Step by Step
The applied tension technique was developed by Swedish psychologist Dr. Lars-Goran Öst in the 1980s. It remains the gold-standard non-drug intervention for blood-injury-injection phobia.
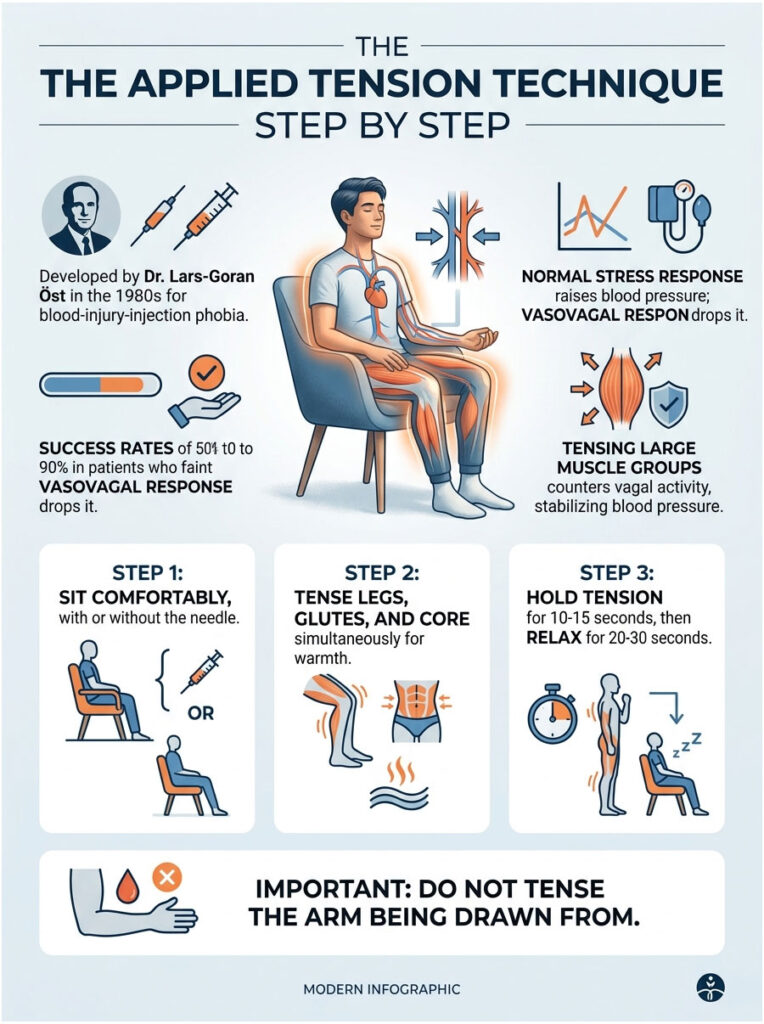
Multiple randomized trials show success rates of 50 to 90% in patients who used to faint regularly.
Why It Works
A normal stress response raises your blood pressure. The vasovagal response inverts that, dropping it. Tensing large muscle groups mechanically squeezes blood out of your legs and torso back toward your heart and brain.
It props up the pressure that vagal activity wants to drop. It’s a counter-attack at the exact physiological level where the problem lives.
The 10 to 15 Second Protocol
Step 1: Sit or recline in a comfortable position. You can do this with the needle already in.
Step 2: Tense the muscles in your legs (quads and calves), glutes, and core all at the same time. Squeeze hard but not painfully. You should feel warmth rise into your face within 10 seconds.
Step 3: Hold the tension for 10 to 15 seconds, then release for 20 to 30 seconds.
Step 4: Repeat the cycle 5 times, or for as long as you feel any lightheadedness.
Important rule: do not tense the arm being drawn from. You’ll move the needle. Tense the other arm if you want, plus everything from the waist down.
When to Start and When to Stop
Begin the cycles as soon as you sit down, before the tourniquet even goes on. Continue through the draw and for 1 to 2 minutes after.
If you start to feel faint at any point, immediately do a hold and ask the phlebotomist to pause. I’ve seen first-time users get genuinely surprised at how well it works. The flushed warm feeling in your face is the tell that your blood pressure has come back up.
What to Do If You Faint Mid-Draw
Even with prep, faints happen. Knowing the response steps prevents the secondary problem (a fall, a head injury, a needle still in your arm).
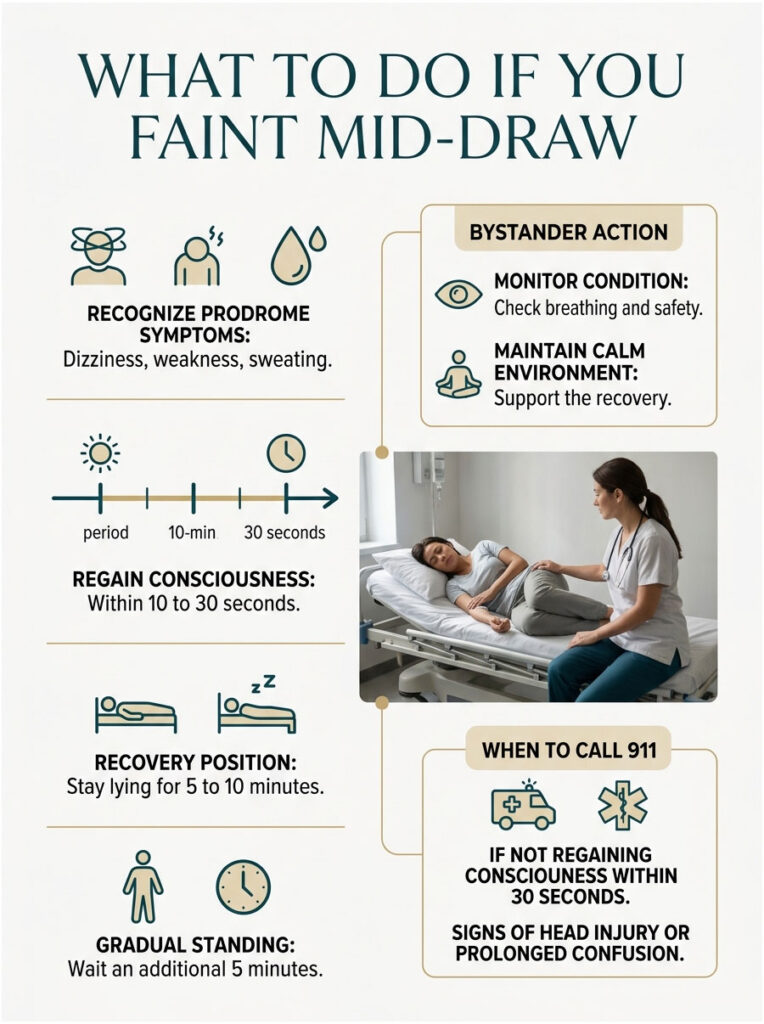
If You’re the Patient
If you feel the prodrome coming on:
- Say “I feel faint” or “stop” loudly. Don’t whisper.
- Get horizontal. If you’re in a chair, lean back as far as you can and slide down so your legs are higher than your head.
- Don’t try to walk it off. Standing up makes it worse.
If you actually lose consciousness, you’ll wake up in 10 to 30 seconds confused but recovering. Stay where you are for at least 5 to 10 minutes before sitting up, and another 5 minutes before standing.
If You’re the Bystander or Caregiver
- Stay calm. Most faints look terrifying and are medically minor.
- Lower the person to the floor or a flat surface. Raise their legs 8 to 12 inches above their chest using a coat, a bag, or your knees.
- Loosen any tight clothing around the neck (collar, scarf, tie).
- Do not put anything in their mouth. The old “bite a stick” advice is wrong and dangerous.
- Once they’re conscious, offer water or juice and have them stay flat until they feel normal.
When to Call 911
Call emergency services if any of these are present:
- Loss of consciousness lasts more than 1 minute
- Chest pain, irregular heartbeat, or shortness of breath
- Head injury occurred during the fall
- Confusion that doesn’t clear within a few minutes
- Seizure-like movements during the faint
- Person is on blood thinners or has a known heart condition
- Person is pregnant
Does Where You Get Your Blood Drawn Matter?
Yes, more than most patients realize. The setting, wait time, room temperature, and accommodations available all change your fainting risk. Here’s how the main US options stack up.

Table 1: Blood Draw Setting Comparison for Fainting Risk
| Setting | Avg Wait Time | Fainting Risk Factors | Accommodations Available | Best For |
| Hospital outpatient lab | 20 to 60 min | Long waits, crowded waiting room, fluorescent lights | Draw beds available, trained staff, on-site emergency response | Patients with known fainting history or complex orders |
| LabCorp / Quest Diagnostics PSC | 15 to 45 min | Standard chair, brief wait, often standing-room-only | Will accommodate lying-down request if asked, no draw bed at most locations | Routine draws for most healthy adults |
| Urgent care | 30 to 90 min | Stressful environment, sick patients nearby, variable phlebotomist skill | Exam tables available for reclining | One-off draws when other options are closed |
| Doctor’s office (in-network) | 5 to 20 min | Familiar setting, less anxiety, exam table available | Exam table for reclining, your own physician available | Patients with anxiety who feel safer at their PCP |
| Mobile / home phlebotomy | 0 min (they come to you) | Your own home, your own couch or bed, no waiting room | Total control of position, lighting, temperature, distractions | Severe needle phobia, post-faint anxiety, immunocompromised, mobility issues |
I had a patient in Phoenix who fainted three times in a row at her local Quest PSC during August (the building’s AC was struggling and the waiting room hit 84 degrees). She completed a 6-tube draw at her kitchen table the following month without a single problem. Environment is half the battle.
Special Situations
The general advice covers most adults. But certain populations need a tailored approach.

Children
Kids faint less often than adults from blood draws (their nervous systems are usually less sensitized). But anxiety runs sky-high. Use distraction tools (a tablet, a favorite toy, a parent’s lap).
Numbing cream like EMLA or lidocaine 4% applied 30 to 60 minutes ahead helps with pain. The American Academy of Pediatrics recommends caregiver presence during pediatric draws, which both calms the child and makes faints more recoverable.
Pregnancy and Postpartum
Pregnant patients faint more easily because of expanded blood volume distribution and lower baseline blood pressure. Always lie down for draws during pregnancy, especially second and third trimester.
Side-lying (on your left side) is ideal in late pregnancy to avoid pressure on the inferior vena cava. Stay extra hydrated, and never skip meals before a draw unless your OB specifically tells you to fast.
I’ve seen second-trimester patients pass out from a routine glucose tolerance test simply because they sat upright in a warm waiting room for 45 minutes. Lying down for the draw itself takes the risk down to almost zero.
Older Adults (65+)
Vasovagal syncope still happens in older adults, but cardiac causes also rise. If you’re over 65 and you faint during a draw, talk to your doctor about ruling out arrhythmias, aortic stenosis, or medication interactions.
ACE inhibitors, diuretics, and beta-blockers can all amplify a vasovagal drop. Lie-down draws are wise. So is bringing someone with you to drive home.
Frequent Draws (Cancer Patients, IVF, Chronic Disease)
If you’re getting bloodwork weekly or biweekly, the cumulative anxiety can build into a conditioned vasovagal response. Ask for the same phlebotomist each time when possible. Use port-a-cath access if your oncologist has placed one.
In my work with chronic-care patients, switching from a clinic chair to home draws often breaks the conditioned cycle within 3 to 4 visits.
Blood Donors at the American Red Cross
Whole-blood donation removes about 470 mL (a pint) of blood, which is way more than a typical lab draw (5 to 50 mL across all tubes). American Red Cross donor reaction data shows roughly 1 in 30 donors experiences some form of reaction, and faints account for the majority.
Eat a salty meal beforehand, drink an extra 16 ounces of water, do calf raises during donation, and accept the cookies after. The post-donation snack isn’t a perk; it’s clinical care.
When Fainting Means Something More Serious
Most blood-draw faints are benign vasovagal episodes. But syncope can occasionally signal something cardiac, and you don’t want to miss the difference.
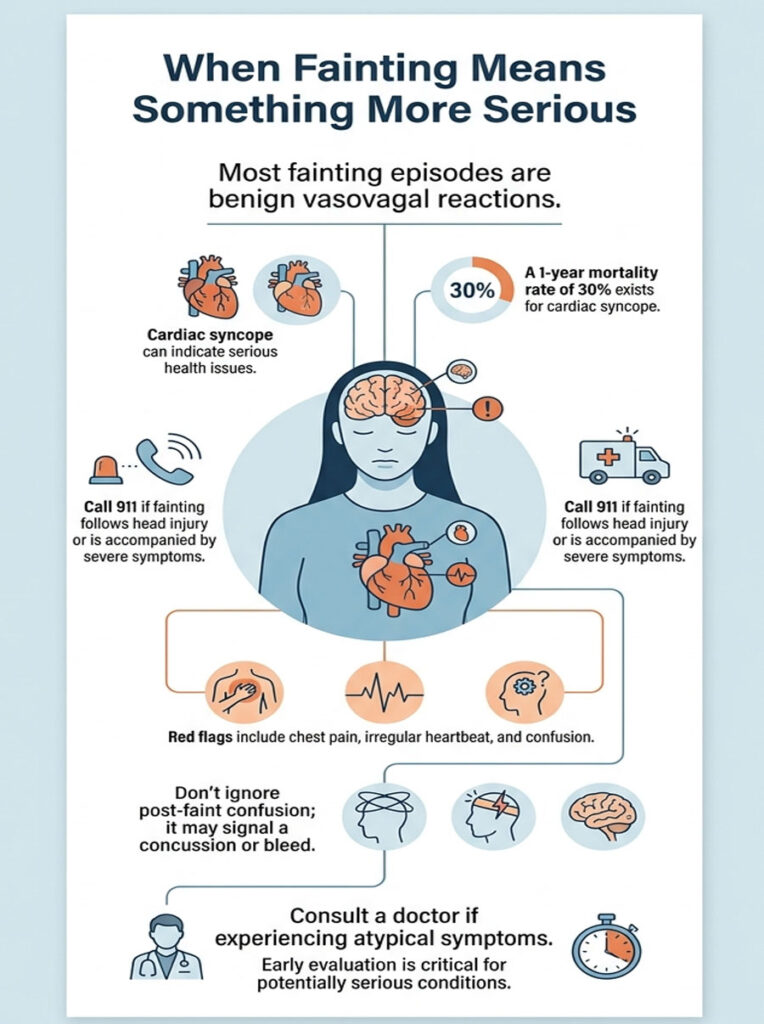
Red Flags That Warrant a Doctor Visit
Talk to your primary care physician (and ideally a cardiologist) if you experience any of these alongside or instead of typical vasovagal symptoms:
- Fainting without any warning prodrome (sudden blackout)
- Chest pain or palpitations during or before the faint
- Fainting while exercising or lying down
- Family history of sudden cardiac death
- Recurrent faints (more than 2 in a year)
- Confusion or weakness that lasts longer than 5 minutes after recovery
When to Call 911
Cardiac syncope carries a 1-year mortality rate of about 30%, per NIH StatPearls. Don’t downplay it.
If you faint and have chest pain, irregular heartbeat, persistent confusion, or hit your head on the way down, call 911. If a faint follows a head injury (even a “mild” one), get evaluated. Concussions and intracranial bleeds can mimic post-syncope confusion.
How to Make Your Next Blood Draw Easier
You’ve got the framework. Now make it stick. Print or screenshot this checklist before your next draw, share it with whoever is going with you, and run the prep on autopilot.
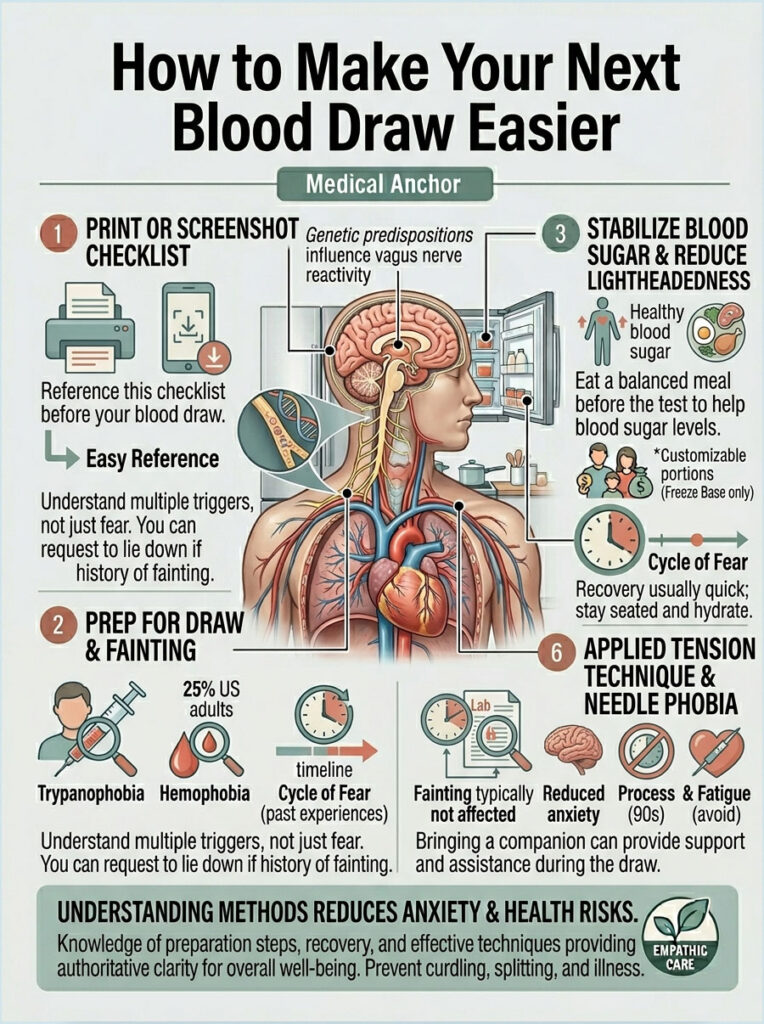
Table 2: US Vasovagal Syncope Statistics at a Glance
| Statistic | Number | Source |
| US ED visits for syncope per year | 740,000 | NIH StatPearls 2025 |
| US hospital admissions for syncope per year | 250,000 | NIH StatPearls 2025 |
| Annual US healthcare cost of syncope | $2.4 billion | NIH PMC, syncope epidemiology review |
| Lifetime prevalence of vasovagal syncope (US adults) | 33 to 42% | NIH StatPearls 2023 |
| Share of all US syncope cases that are vasovagal | ~50% | NIH StatPearls 2025 |
| US adults with significant needle fear | ~25% | McLenon & Rogers 2019, J Adv Nurs |
| Phlebotomy patients who experience syncope | ~2.5% | Clinical phlebotomy literature |
| Applied tension technique success rate (needle phobia) | 50 to 90% | Öst et al, Behaviour Research & Therapy |
Frequently Asked Questions
Why do I feel faint when I get blood drawn even if I’m not scared?
You can have a vasovagal response without conscious fear. Pain, the sight of blood, low blood sugar, dehydration, or just standing in a warm waiting room too long can trigger it. The reflex is automatic; your nervous system doesn’t ask your conscious brain for input. Treat it like any other physical reaction (allergies, motion sickness) and prep accordingly.
Can I ask to lie down at LabCorp or Quest?
Yes. Both LabCorp and Quest Diagnostics train phlebotomists to accommodate lie-down requests when patients have a fainting history. Most patient service centers don’t have actual draw beds, but they’ll let you recline as far as the chair goes and prop your legs up. Just say it at check-in so they can plan around it.
Does eating before a blood test prevent fainting?
Yes, when you’re allowed to eat. A complex-carb plus protein meal 1 to 2 hours before stabilizes blood sugar and supports blood pressure during the draw. If your test requires fasting (lipid panel, glucose, comprehensive metabolic), water is still allowed and you should drink plenty. Don’t fast longer than your provider specifies.
How long does it take to recover after fainting at a blood draw?
Most people are conscious again within 10 to 30 seconds and feel mostly normal within 5 to 15 minutes. Lingering tiredness, mild headache, or “off” feeling can last a few hours. Stay seated for at least 10 minutes after a faint, sip water, eat a snack, and don’t drive for at least 30 minutes (longer if you still feel hazy).
Will fainting affect my lab test results?
Not for most common tests. The needle was already drawing blood when you fainted, so your sample reflects your pre-faint physiology. Some specialized tests (cortisol, catecholamines) can be affected by acute stress, so mention the faint to your ordering provider. They may want to redraw if the stress markers matter for your diagnosis.
Is the applied tension technique scientifically proven?
Yes. Dr. Lars-Goran Öst’s original 1980s research showed it reduced fainting in 73% of blood-injury phobic patients within 5 sessions. Follow-up studies have replicated success rates of 50 to 90%. It’s recommended by the NHS, the American Red Cross, and major US blood banks. The technique is free, drug-free, and works fast.
Can I take anti-anxiety medication before a blood draw?
Sometimes. Talk to your prescribing physician. Short-acting benzodiazepines (lorazepam, alprazolam) are occasionally prescribed for severe needle phobia. They can lower anxiety but don’t always prevent the vagal drop, so still use the physical techniques. Never take someone else’s prescription, and arrange a ride home if you do take a sedative.
Why do I feel dizzy hours after a blood test?
Mild post-draw dizziness usually traces back to dehydration, low blood sugar, or residual vagal activity. Drink fluids, eat a snack with carbs and protein, and rest for an hour. If dizziness lasts more than 4 to 6 hours or comes with chest pain, palpitations, or weakness on one side of your body, contact your doctor or seek urgent care.
Can dehydration alone cause me to faint at a blood draw?
Absolutely. Dehydration shrinks your blood volume, so even a small drop in pressure during a draw can tip you into syncope. Aim for at least 64 ounces of water in the 24 hours before, plus 16 to 20 more ounces in the 2 hours leading up. Hot weather, exercise, alcohol the night before, and caffeine all worsen baseline hydration.
Should I bring someone with me if I tend to faint?
Yes. A companion can drive you home, advocate for accommodations at check-in, hold your hand during the draw, and respond if you actually pass out. They don’t need to watch the needle. They just need to be present. Many US labs let companions sit in the draw room; ask when you book.
Is it dangerous to faint during a blood draw?
The faint itself is almost always benign and self-limiting. The danger is the fall (head injury, broken wrist, dental damage). That’s why “lie down before you might fall down” is the most important safety rule. Damage from secondary falls causes the bulk of syncope-related ER visits, not the faint itself.
What if my child faints every time? When should I see a doctor?
One faint is usually nothing. Two or more is worth a pediatrician visit, especially if your child also faints during exercise, has a family history of cardiac problems, or faints without warning. Most pediatric vasovagal syncope is harmless and outgrown by late teens, but a quick EKG and history can rule out the rare cardiac causes that need treatment.
Disclaimer: This article is for educational purposes only and does not substitute for professional medical advice, diagnosis, or treatment. If you have recurrent fainting episodes, chest pain, irregular heartbeat, or other concerning symptoms, contact your healthcare provider or call 911 in an emergency. Always consult a licensed clinician before changing how you prepare for medical procedures.
References
- NIH StatPearls, Vasovagal Episode: https://www.ncbi.nlm.nih.gov/books/NBK470277/
- NIH StatPearls, Syncope (epidemiology and US ED data): https://www.ncbi.nlm.nih.gov/books/NBK442006/
- NIH StatPearls, Cardiac Syncope: https://www.ncbi.nlm.nih.gov/books/NBK526027/
- McLenon J, Rogers MAM, “The fear of needles: A systematic review and meta-analysis,” Journal of Advanced Nursing, 2019: https://pubmed.ncbi.nlm.nih.gov/30109720/
- Öst LG, “Applied tension: a specific behavioral method for treatment of blood phobia,” Behaviour Research and Therapy, 1991: https://pubmed.ncbi.nlm.nih.gov/2016083/
- Cleveland Clinic, Vasovagal Syncope overview: https://my.clevelandclinic.org/health/diseases/23325-vasovagal-syncope
- MedlinePlus, Fainting first aid: https://medlineplus.gov/fainting.html
- American Academy of Family Physicians: https://www.aafp.org/
- American Red Cross, Donor experience and reactions: https://www.redcrossblood.org/
- NIH PMC, Global prevalence of vasovagal syncope (2024 meta-analysis): https://pmc.ncbi.nlm.nih.gov/articles/PMC10821537/
- NIH PMC, Vasovagal syncope therapies review: https://pmc.ncbi.nlm.nih.gov/articles/PMC11659707/







