You sat in the chair, the phlebotomist tapped your arm twice, frowned, switched sides, and tapped again. Round two ended with a bandage, an apology, and a bruise that lasted a week. If that scene sounds familiar, you’re not the problem and your veins aren’t broken. They’re hiding, and there’s a lot you can do in the 24 hours before your draw to coax them back into view.
Table of Contents
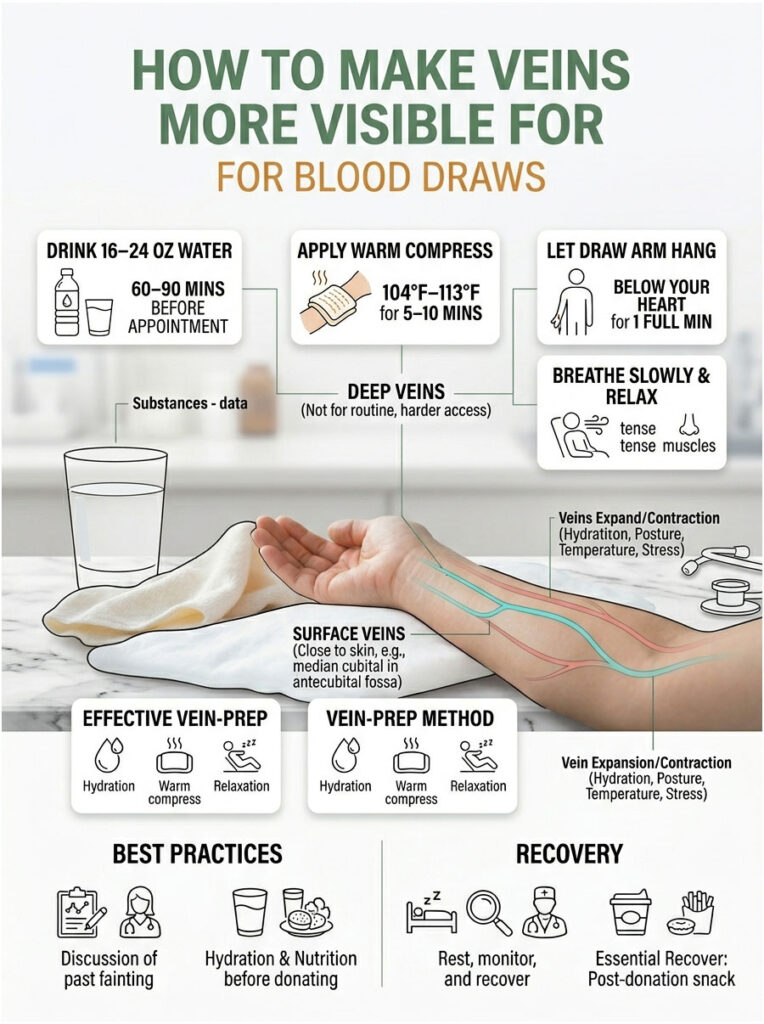
Quick Answer: To make veins bigger for a blood draw, drink 16 to 24 ounces of water in the 60 to 90 minutes before your appointment, apply a warm compress between 104°F and 113°F to your arm for 5 to 10 minutes, let your draw arm hang below your heart for one full minute, breathe slowly to relax tense muscles, and stay warm in the waiting room. These five steps dilate your surface veins, boost blood flow, and dramatically improve first-stick success rates.
At a Glance
- Difficult venous access affects 10% to 26% of hospitalized US patients per a recent meta-analysis
- Roughly 6 million peripheral IV insertions fail in US hospitals every year
- Hydration is the single highest-impact step you can take before a draw
- A warm compress for 5 to 10 minutes can noticeably increase vein visibility
- Caffeine and alcohol the night before measurably narrow your blood vessels
- Vein-finder devices like AccuVein are now used in many US hospitals
- You have the right to ask for a different phlebotomist after two failed sticks
Why Veins Hide During Blood Draws (The Real Reason)
Before you fix the problem, it helps to understand what is actually happening inside your arm. Veins are not static tubes; they expand and contract based on temperature, hydration, stress, and posture. In years of helping US patients prep for both lab and home blood collection, I have watched the same arm produce a “stick on the first try” vein at 9 a.m. and an invisible one at 4 p.m., simply because the patient skipped lunch and got chilled.
The Anatomy: Surface Veins vs. Deep Veins
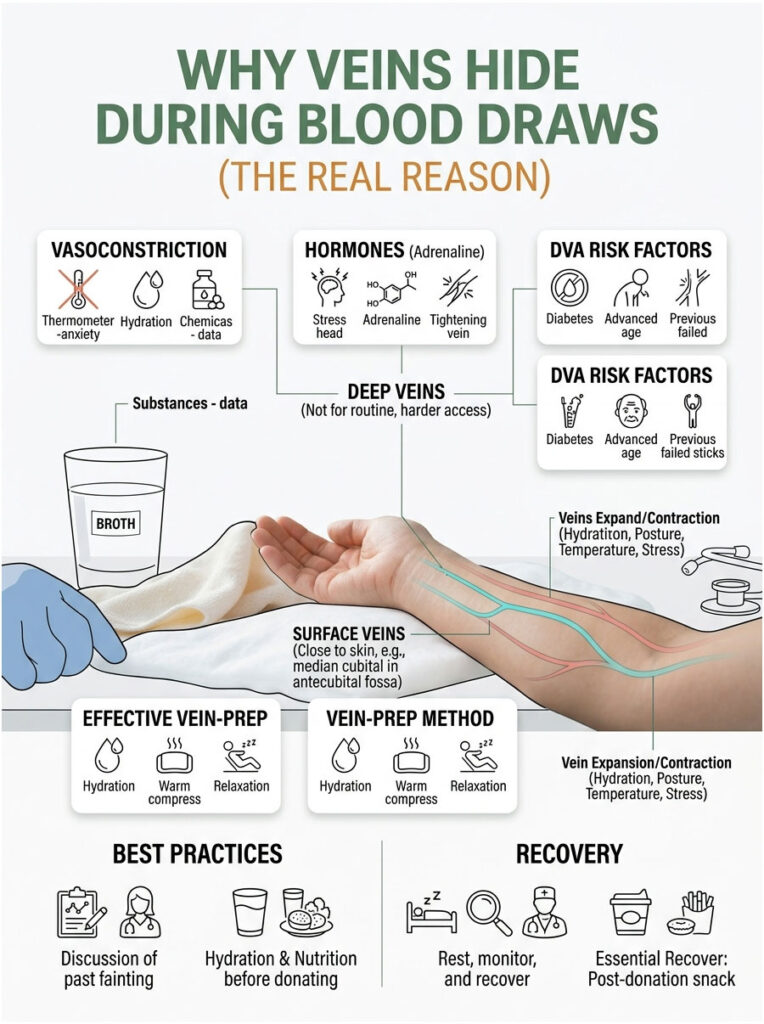
The veins your phlebotomist is hunting for live close to the skin’s surface, mostly in a small triangle on the inside of your elbow called the antecubital fossa. The three big targets there are the median cubital, cephalic, and basilic veins.
Deep veins (femoral, subclavian) are protected by tissue and not used for routine bloodwork. When your surface veins shrink, the tech does not switch to deeper ones; they start hunting smaller alternatives in your hand or wrist, which hurt more and bleed slower.
What Causes Vasoconstriction
Vasoconstriction is the medical term for “your veins just got skinnier.” Cold air, dehydration, anxiety, low blood pressure, caffeine, nicotine, and certain blood pressure medications can all shrink the diameter of your surface veins by a measurable amount.
Stress hormones like adrenaline tighten the smooth muscle around your blood vessels in seconds. That is why your veins seem to vanish the moment you sit in the chair, even if they were perfectly visible an hour earlier.
Who Is Most Affected
A study in the Journal of Clinical Nursing found that difficult venous access (DVA) reaches 59.3% in highly complex hospitalized patients. In a typical urban US emergency department, about 1 in every 9 to 10 adults qualifies as DVA on any given visit.
Risk factors that USA clinical research consistently identifies include diabetes, sickle cell disease, prior IV drug use, history of chemotherapy, advanced age, very young age (under 5), and a history of multiple past failed sticks.
Table 1: Common Vein-Prep Methods Compared
| Method | Time Required | Effectiveness | Evidence Source | Best For |
| Drinking 16 to 24 oz water | 60 to 90 min before | High | MedlinePlus / NIH | Everyone, including fasting patients |
| Warm compress (104°F to 113°F) | 5 to 10 min before | High | Hemophilia Federation guidance | Cold weather, small veins |
| Arm dangle below heart | 60 to 90 seconds | Moderate | Phlebotomy clinical practice | Rolling or shallow veins |
| Slow controlled breathing | 2 to 5 min | Moderate | Stress-physiology research | Anxious patients, kids |
| Light walking pre-arrival | 10 to 15 min | Moderate | SUNY Upstate guidance | Non-fasting patients |
| Avoiding caffeine 24 hours prior | 24 hours | Moderate to High | Cleveland Clinic patient education | Coffee drinkers, frequent draws |
12 Proven Ways to Make Your Veins Bigger Before a Blood Draw
These twelve tips stack on top of each other. You do not need to do all twelve to get a good stick, but the more you layer, the better your odds. I have personally walked patients through this list when they had failed three blood draws in a row, and the first four steps usually turn things around.
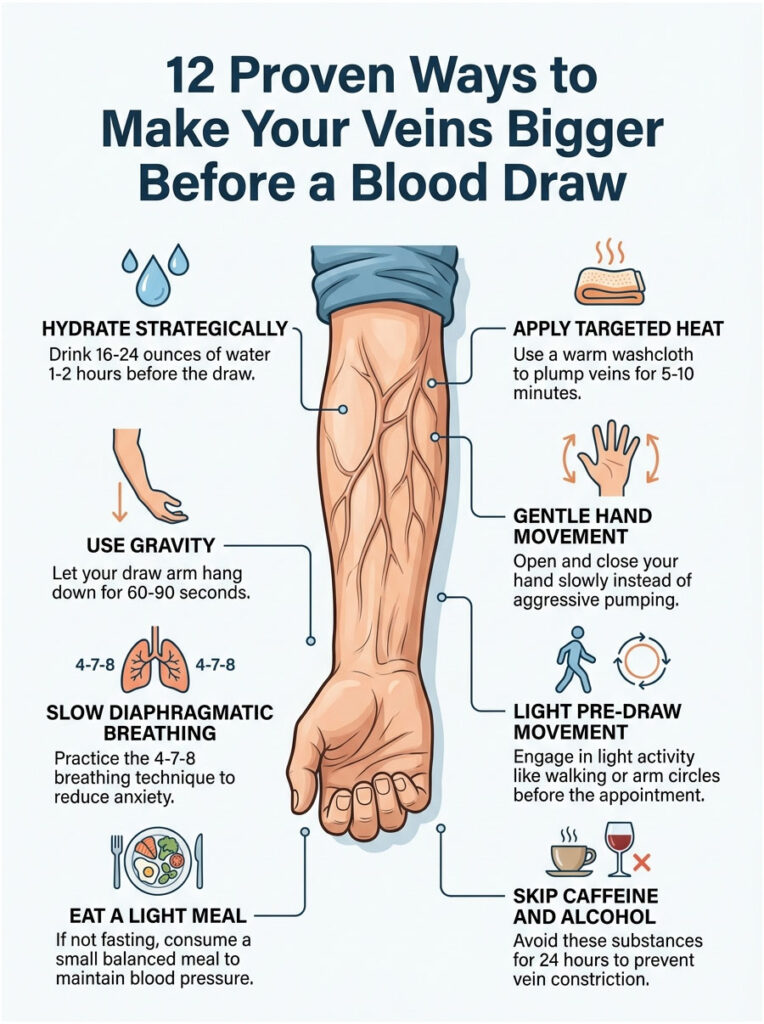
Tip 1: Hydrate Strategically (Not Just Right Before)
Water is the single most powerful tool you have. Your blood is more than half water, and even mild dehydration shrinks your blood volume, which collapses your surface veins. The goal is steady hydration, not a panicked chug in the parking lot.
Aim for 16 to 24 ounces (about 2 to 3 standard glasses) of plain water in the 60 to 120 minutes before your appointment, and start sipping the day before. If you are fasting, plain water is almost always allowed; MedlinePlus confirms this for nearly all standard tests.
Tip 2: Apply Targeted Heat
Warmth opens veins almost immediately. A warm washcloth held against the inside of your elbow for 5 to 10 minutes can noticeably plump your median cubital vein.
A few quick options that work in any US household: a microwaved damp washcloth (15 to 20 seconds; test the heat on your wrist first), a heating pad on the lowest setting, or running warm tap water over your forearm for 3 to 5 minutes. Aim for comfortable warmth, not heat that could burn.
Tip 3: Use Gravity (The Arm-Dangle Method)
Sit up straight and let your draw arm hang loose at your side, fingers pointing down toward the floor, for a full 60 to 90 seconds. Gravity pulls blood into your forearm, and your veins fill like a balloon.
This is the trick I see experienced US phlebotomists quietly suggest when a patient’s veins look flat. It costs nothing, takes a minute, and often saves a stick.
Tip 4: Gentle Hand Movement, Not Aggressive Pumping
You have probably been told to “make a fist.” That is fine, but do not pump it like a stress ball. Aggressive pumping can skew certain blood test results by releasing potassium from your muscles into your bloodstream.
Instead, slowly open and close your hand 4 or 5 times, then hold a relaxed soft fist while the tourniquet goes on. That is enough to push blood toward your antecubital fossa without affecting your lab numbers.
Tip 5: Slow Diaphragmatic Breathing
Anxiety triggers vasoconstriction in seconds. The simplest counter is a breath pattern called 4-7-8: inhale through your nose for 4 seconds, hold for 7, exhale through your mouth for 8. Three rounds is usually enough.
In practice, I have watched anxious patients’ veins visibly fill within 90 seconds of starting this breathing pattern. It works because slow exhalation activates your parasympathetic nervous system, which dilates your blood vessels.
Tip 6: Light Pre-Draw Movement (Walking, Arm Circles)
A short brisk walk 10 to 15 minutes before your appointment raises your heart rate and pushes more blood into your peripheral veins. SUNY Upstate’s patient guide recommends a quick walk for the same reason, with the caveat that you skip this if you are fasting and prone to lightheadedness.
If walking is not your thing, swing your draw arm in slow windmill circles 10 to 15 times. The centrifugal motion forces blood into your forearm faster than the dangle method.
Tip 7: Eat a Light Meal (When Not Fasting)
If your test does not require fasting, eat. A small balanced meal (whole-grain toast with peanut butter, Greek yogurt with berries, or a banana with a handful of almonds) keeps your blood sugar and blood pressure steady.
Low blood sugar drops your blood pressure, which collapses surface veins and can cause fainting in the chair. The American Red Cross recommends a light snack before blood donation for the same reason.
Tip 8: Skip Caffeine and Alcohol for 24 Hours
Caffeine is a vasoconstrictor; alcohol is a diuretic. Both work against you. Coffee, energy drinks, strong tea, and alcohol consumed within 24 hours of your draw can measurably shrink your veins by reducing blood volume and tightening vessel walls.
If you cannot skip your morning coffee, at least pair it with extra water (8 ounces of water per cup of coffee). For fasting tests, black coffee is not allowed anyway because caffeine itself can affect glucose readings.
Tip 9: Moisturize for Days Before
This one surprises most patients. SUNY Upstate’s blood-draw guide recommends moisturizing your hand and arm 4 times a day in the days leading up to a procedure to reduce skin sensitivity and pain.
Soft skin also produces a cleaner puncture, which means less bruising. Any standard US drugstore lotion works (CeraVe, Cetaphil, Eucerin); fragrance-free is ideal because some lab tests are sensitive to skin contaminants.
Tip 10: Dress Warm and Bring Layers
Cold body, cold veins. If you are driving to the lab in winter, keep the heat in your car cranked and wear short sleeves under a warm jacket so you can roll up the sleeve quickly without getting a chill.
In the waiting room, leave your coat on. I have seen patients walk in with arms so cold the phlebotomist literally could not find a vein, then return 10 minutes later (after holding a warm cup of water) to a textbook stick.
Tip 11: Communicate Your Vein History Out Loud
Tell the phlebotomist before they touch you which arm has worked best in the past, whether you have had luck with a butterfly needle, and whether your wrist or hand veins were used previously.
US labs encourage this. Phlebotomists at LabCorp, Quest Diagnostics, and most US hospital labs are trained to ask, but if they do not, speak up. Saying “my left arm always works better” can save you a stick.
Tip 12: Ask for a Butterfly Needle or Vein Finder
A butterfly needle (typically 21 or 23 gauge with flexible “wings”) is gentler on small or rolling veins than a standard straight needle. Many US labs use them by default for elderly and pediatric patients but will switch on request for any adult.
Vein-finder devices like AccuVein and VeinViewer project a real-time map of your veins onto your skin using harmless near-infrared light. They are now available in many US hospitals and outpatient clinics. Ask if your facility has one if your draws are routinely difficult.
Table 2: USA Statistics on Blood Draws and Difficult Venous Access
| Statistic | Number / Rate | Source | Year |
| US ED visits resulting in IV placement | 35.2 million per year | NHAMCS / ScienceDirect | 2014 (latest available) |
| Annual US peripheral IV insertion failures | ~6 million | ClinicalTrials.gov AccuCath study | 2024 update |
| DVA prevalence in urban US emergency dept | 11.8% | PubMed / Annals of EM | 2014 |
| DVA prevalence in highly complex inpatients | 59.3% | Journal of Clinical Nursing / PubMed | 2017 |
| DVA range across hospitalized patient meta-analysis | 10% to 26% | MDPI Medicina meta-analysis | 2026 |
| DVA in patients with recent injection drug use | 77% reported difficulty | SAGE Journals / 2025 study | 2025 |
What Not to Do Before a Blood Draw (5 Mistakes That Make Veins Hide)
Some popular tips you will see on TikTok and Reddit actually backfire. Avoiding these mistakes is just as important as following the tips above.
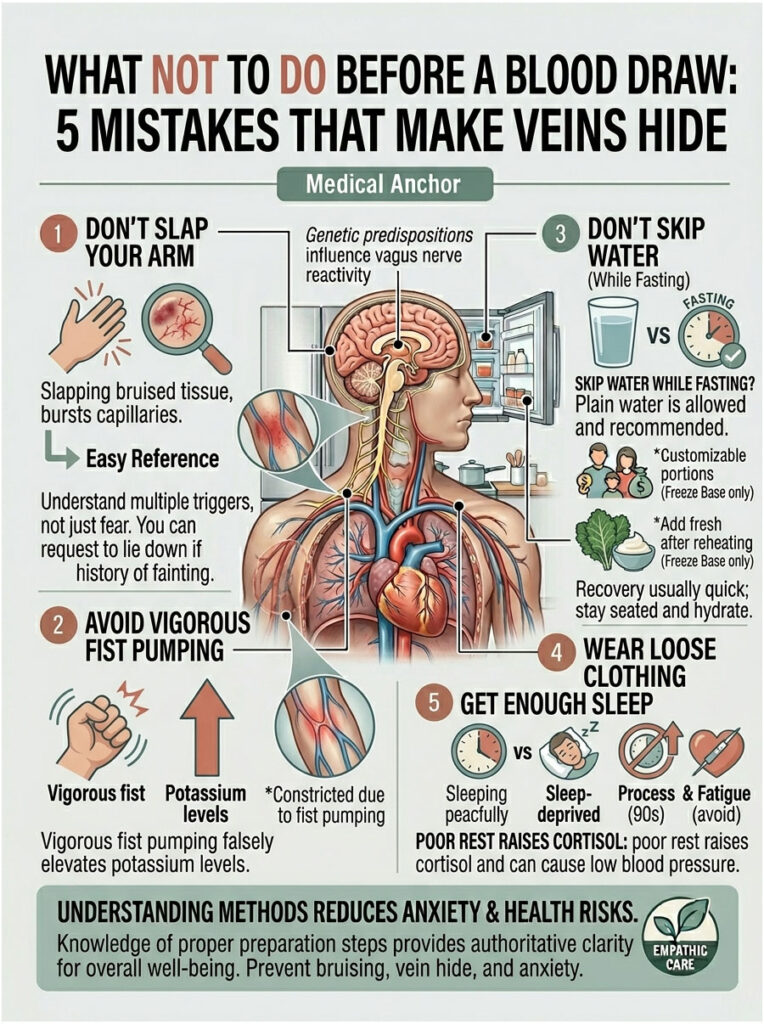
Don’t Slap Your Arm
You have seen it in movies; it does not work in real life. The Hemophilia Federation explicitly warns against slapping the skin to raise a vein because it can bruise the tissue and burst small capillaries. Gentle massage is fine. Slapping is not.
Don’t Pump Your Fist Hard
As mentioned earlier, vigorous fist-pumping can release potassium from your muscle cells, which falsely elevates your potassium reading and forces a redraw. Slow, gentle hand opening and closing is the right amount.
Don’t Skip Water Just Because You’re Fasting
This is one of the biggest myths in US patient prep. “Fasting” almost always means no food and no caloric drinks; plain water is allowed and encouraged. Cleveland Clinic explicitly recommends water during fasting for this reason.
Don’t Wear Tight Sleeves to the Lab
A tight sleeve rolled up on your bicep acts like a second tourniquet, blocking blood flow and making veins below it collapse. Wear loose short sleeves or a button-down shirt that opens fully.
Don’t Stay Up Too Late the Night Before
Poor sleep raises cortisol and blood pressure, then drops blood pressure in the morning. Patients who sleep less than 5 hours often arrive with low BP, smaller veins, and a higher chance of feeling lightheaded during the draw.
Special Situations That Need a Different Approach
Standard tips work for most people, but certain conditions and life stages call for adjustments. If you fall into one of these categories, share it with your phlebotomist before they pick a site.
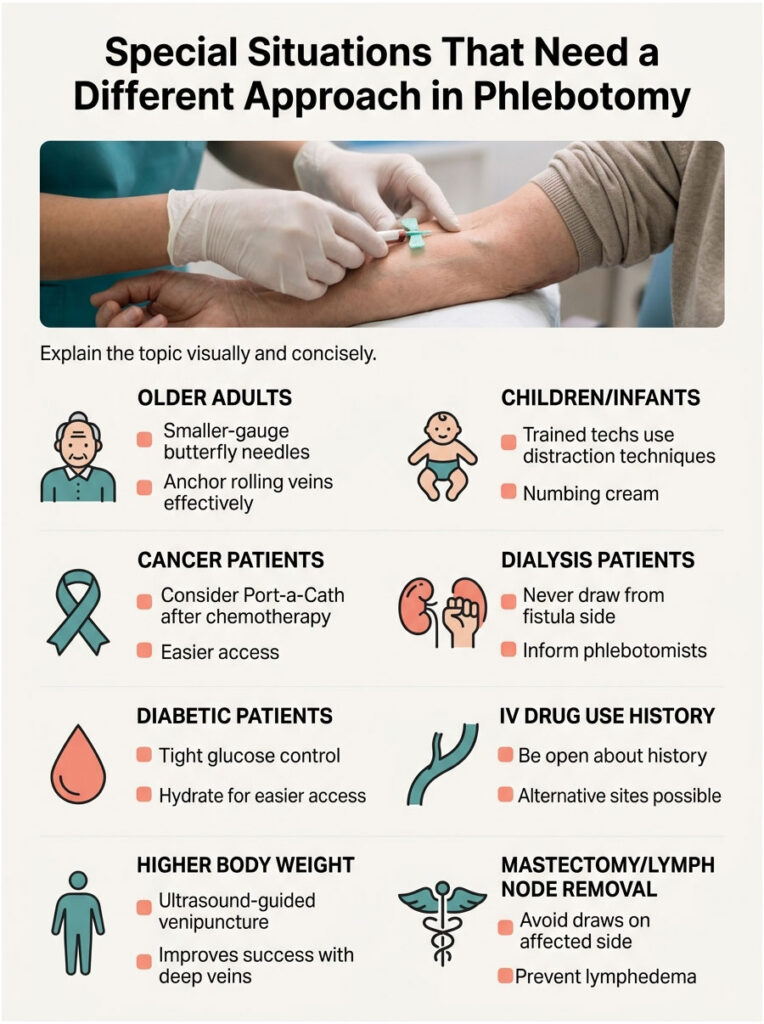
Older Adults and Fragile, Rolling Veins
Veins lose elasticity with age, becoming more likely to “roll” sideways under the needle. A skilled tech anchors the vein with their thumb below the puncture site and uses a smaller-gauge butterfly needle. Ask for one if it is not offered.
Children and Infants
Pediatric blood draws should be done by techs trained in pediatric phlebotomy. The dorsal hand or scalp veins are sometimes used in infants. Distraction (a tablet, song, or favorite toy) plus a numbing cream like LMX 4% applied 30 minutes before can make a huge difference.
Cancer and Chemotherapy Patients
Repeated chemo damages peripheral veins. If you have had chemo, ask whether your provider can use a port (a Port-a-Cath surgically implanted under the skin) for routine draws instead of sticking your arm again. The American Cancer Society supports port use for frequent bloodwork.
Dialysis Patients (Fistula Side Warning)
If you have an arteriovenous fistula or graft for dialysis, never let anyone draw blood from that arm. The fistula side is reserved for dialysis access only. Tell every phlebotomist before they put a tourniquet on you.
People with Diabetes
Diabetes is one of the strongest risk factors for difficult venous access in US studies. Tight glucose control, careful hydration, and warming your arms longer than usual all help. If you are on insulin, time your draw and meals carefully.
History of IV Drug Use
A 2025 SAGE Journals study of US patients with injection drug use history found 77% reported difficulty with venous access. Be honest with your phlebotomist; this is a clinical fact, not a moral judgment, and it changes their site selection. Hand and foot veins may work better than arm veins.
Higher Body Weight and Deep Veins
If your veins sit deeper under tissue, ultrasound-guided venipuncture is now the gold standard. Ultrasound guidance has been shown to dramatically improve first-stick success when veins are not visible or palpable. Many US ED departments use it routinely.
Mastectomy or Lymph Node Removal
If you have had lymph nodes removed (most often after breast cancer surgery), avoid blood draws on that side because of the increased lymphedema risk. Tell every phlebotomist; this is one of the most commonly missed details in US outpatient labs.
Tools US Phlebotomists Use for Hard Veins
If standard prep is not enough, your phlebotomist has technology and techniques designed exactly for hard sticks. Knowing what is available means you can ask for it.
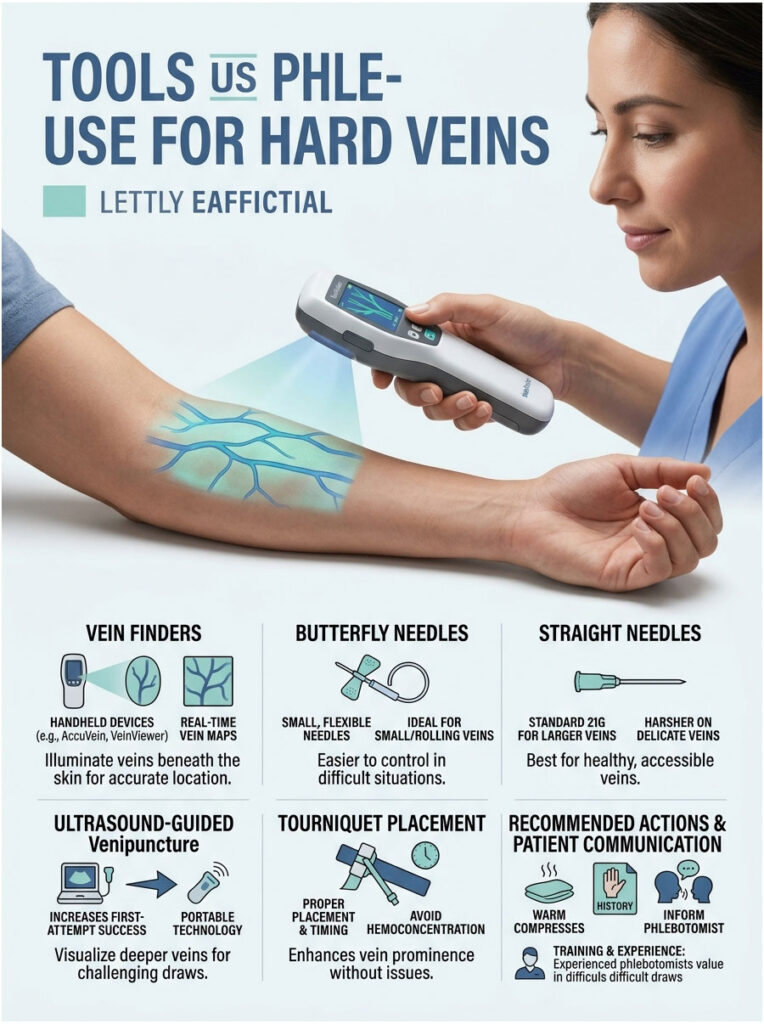
Vein Finders (AccuVein, VeinViewer)
AccuVein AV500 and Christie Medical’s VeinViewer Flex are the two most common handheld vein-finder devices in US healthcare. They project a real-time vein map onto your skin in green or red light. No needle, no contact, no radiation, just a flashlight-style scan that takes a few seconds.
Butterfly Needles vs. Straight Needles
A butterfly (winged infusion set) uses a smaller, more flexible needle attached to short tubing. It is easier to anchor on small or rolling veins. Standard 21G straight needles are faster for big visible veins but harsh on tiny ones. A 23G butterfly is a typical choice for delicate veins.
Ultrasound-Guided Venipuncture
Portable ultrasound is now common in US emergency departments and increasingly in outpatient settings for difficult sticks. The phlebotomist sees the vein on a small screen and guides the needle in real time. First-attempt success rates jump significantly with this approach.
Tourniquet Placement and Timing
A tourniquet should sit 3 to 4 inches above the puncture site and stay on for no more than 60 seconds. Longer than that causes hemoconcentration, which can falsely elevate certain lab values. If you have been waiting more than a minute with the tourniquet on, it is reasonable to ask the tech to release and re-tie.
Table 3: Scenario / Recommended Action Quick Reference
| Your Situation | Recommended Action | Why It Works |
| Cold and shivering on arrival | Hold a warm cup of water for 5 minutes; ask for warm compress | Heat dilates surface veins quickly |
| Fasting since last night | Drink 16 to 24 oz water 60 min before; ask for slow seated draw | Water keeps blood volume up; sitting prevents fainting |
| Past 2+ failed sticks at same lab | Request butterfly needle; ask if vein finder is available | Smaller needle and visualization improve first-stick success |
| Naturally small or “rolling” veins | Ask for senior phlebotomist plus butterfly needle plus warm compress | Experienced techs anchor better; smaller needles bend less |
| Severe needle phobia | Tell tech to lay you down; do 4-7-8 breathing; ask for distraction | Reduces vasovagal response and vasoconstriction |
| History of chemo or frequent draws | Ask provider about a port; mention any tender or scarred sites | Ports protect remaining peripheral veins |
| Mastectomy or lymph node removal | Speak up before tourniquet goes on; use opposite arm only | Reduces lymphedema risk on affected side |
Your Pre-Blood-Draw Checklist (Night Before to Walking In)
If you only remember one thing from this guide, make it the timeline below. Following it has helped many patients I have personally coached through home-collection visits turn a dreaded draw into a 90-second non-event.
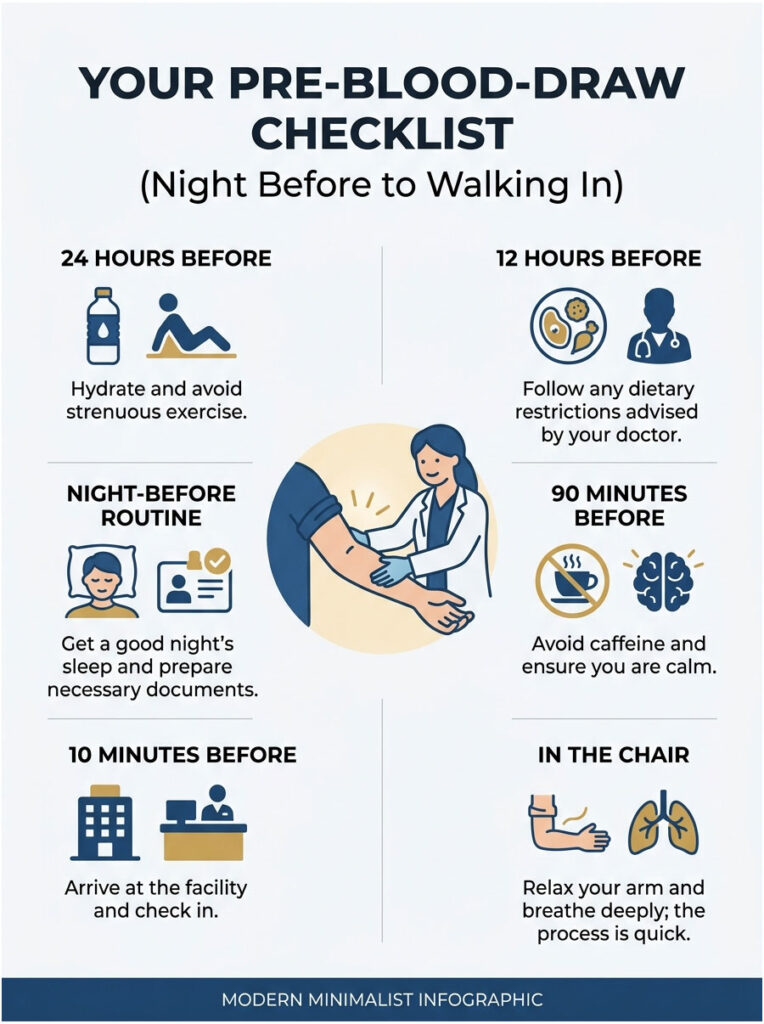
24 Hours Before
- Skip alcohol entirely
- Cut caffeine to one cup max, or zero if possible
- Drink water steadily through the day, aiming for half your body weight in ounces
- Begin moisturizing your draw arm
- Get to bed at a reasonable hour
12 Hours Before (Night-Before Routine)
- Eat a balanced dinner if you are not yet fasting
- Lay out loose, short-sleeved or button-down clothing
- Set water by your bed for first thing in the morning
- Begin fasting now if your test requires it (water still allowed)
90 Minutes Before
- Drink 16 to 24 ounces of plain water
- Take a warm shower if possible
- Apply moisturizer to your hand and forearm
10 Minutes Before
- Walk into the building rather than rushing
- Keep your jacket on; warm beats cool
- Apply a warm washcloth to the inside of your elbow if you brought one
- Do three rounds of 4-7-8 breathing in the waiting room
In the Chair
- Tell the tech which arm has worked best
- Mention any history (mastectomy, fistula, chemo, drug use, fainting)
- Let your arm hang for a moment before extending it
- Breathe out slowly as the needle goes in
When to Ask for a Different Phlebotomist (The Two-Stick Rule)
Most US labs have an unofficial “two-stick rule”: after two failed attempts, the current tech should hand you off to a senior colleague. You do not have to wait for them to volunteer. You can ask.

Your Patient Rights in US Labs
Under standard patient-rights frameworks adopted by major US healthcare systems, you have the right to refuse further attempts and request a different provider. CLSI Standard GP41 (the blood specimen collection standard followed by US labs) recommends limiting attempts to two per provider before reassessing.
How to Ask Without Awkwardness
A polite phrase that works: “I really appreciate you trying. Is there a senior tech who could give it a fresh look? My veins have been tough today.” Most phlebotomists are relieved by the request because they do not enjoy missed sticks any more than you do.
When to Request a Pediatric or NICU-Trained Tech
If you are an adult with very small veins, a pediatric phlebotomy specialist often has the lightest touch and the right small-gauge equipment. Most US hospitals will accommodate this request from outpatient labs upon a polite ask.
Frequently Asked Questions
How long before a blood draw should I drink water?
Start drinking water steadily the day before, then have 16 to 24 ounces (about 2 to 3 glasses) in the 60 to 90 minutes before your appointment. Sip rather than chug. According to MedlinePlus, plain water is allowed even during fasting tests and helps keep your veins fuller.
Can I drink water before a fasting blood test?
Yes. Plain water is allowed and recommended for almost all fasting blood tests. Cleveland Clinic and MedlinePlus both confirm this. Avoid flavored water, sparkling water with sweeteners, lemon water, coffee, tea, or juice; these can affect your results. Stick to plain still water.
Does drinking coffee make veins shrink?
Yes, somewhat. Caffeine is a mild vasoconstrictor and a diuretic, meaning it both narrows blood vessels and pulls water from your body. For 24 hours before a draw, limit coffee to one cup or skip it entirely. For fasting tests, coffee (even black) is not allowed because it can affect glucose readings.
How much water should I drink before a blood draw?
About 16 to 24 ounces of plain water (2 to 3 standard glasses) within 1 to 2 hours of your appointment is the sweet spot for most adults. Larger people may need more. Do not try to compensate for skipping water all day with one giant chug right before; your body needs time to absorb it.
Why do my veins roll when getting blood drawn?
Rolling veins move sideways under the needle instead of staying in place. They are more common in older adults, very thin people, and patients with frequent draws. Ask your phlebotomist to anchor the vein with their thumb below the puncture site, and request a smaller butterfly needle for better control.
Does massaging my arm help veins show up?
Gentle massage along the inside of your forearm in the direction of your heart can help blood flow into the antecubital area. Use light circular motions for 30 to 60 seconds. Skip slapping or aggressive rubbing; both can damage capillaries and bruise the area, which actually makes the draw harder.
Can exercise help my veins for a blood draw?
Light movement helps. A 10 to 15 minute brisk walk before your appointment raises your heart rate and pushes blood into peripheral veins. Skip strenuous exercise; vigorous workouts can affect lab values like creatine kinase, liver enzymes, and white blood cell counts, which may force a redraw.
What foods help make veins more visible?
Foods rich in water, potassium, and nitrates support blood volume and circulation. Cucumber, watermelon, oranges, leafy greens, beets, and bananas are all good choices the day before. Skip very salty foods, which can cause bloating that masks veins. Always follow your provider’s fasting instructions when applicable.
Why are my veins harder to find in cold weather?
Cold causes vasoconstriction, where surface blood vessels narrow to conserve heat. This is your body’s normal protective response, not a problem with your veins. Stay warm in the waiting room, keep your jacket on, and ask for a warm compress on your arm before the draw if your veins look flat.
Can I refuse a second needle stick?
Yes. You have the right to ask for a different phlebotomist or to pause and reschedule. The unofficial “two-stick rule” in US labs limits attempts per provider to two before handing off. A polite request like “Could a senior tech try next?” is appropriate and almost always honored.
Does age affect how easy it is to draw blood?
Yes. Children under 5 and adults over 70 often have smaller, more fragile, or more mobile veins. Older adults’ veins also lose elasticity and are more prone to bruising. Smaller butterfly needles, slower draws, and longer warming time help in both age groups.
How do mobile phlebotomists handle difficult veins at home?
Mobile phlebotomy services in the US (including HealthCareOnTime’s home collection options) bring trained techs, butterfly needles, warm compresses, and sometimes vein-finder devices directly to your house. Comfort, warmth, and unhurried timing in your own environment often produce better stick rates than a busy lab.
Medical Disclaimer: This article is for general educational purposes only and does not replace personalized medical advice. Always follow the specific instructions provided by your healthcare provider or laboratory. If you experience repeated difficulty with blood draws, persistent bruising, or symptoms of dehydration, consult a licensed clinician. Information about medications, devices, and procedures reflects general US clinical practice and may not apply to your specific situation.
References
- Cleveland Clinic, Fasting Before Blood Work. https://my.clevelandclinic.org/health/articles/fasting-for-blood-work
- MedlinePlus (NIH), Fasting for a Blood Test. https://medlineplus.gov/lab-tests/fasting-for-a-blood-test/
- SUNY Upstate Medical University, How Patients Can Improve Blood Draws. https://www.upstate.edu/whatsup/2017/0929-how-patients-can-improve-blood-draws.php
- PubMed, Risk Factors Associated with Difficult Venous Access in Adult ED Patients. https://pubmed.ncbi.nlm.nih.gov/25171796/
- PubMed, Prevalence of Difficult Venous Access in Highly Complex Hospitalised Patients. https://pubmed.ncbi.nlm.nih.gov/28165645/
- MDPI Medicina, Strategies to Address Difficult Venous Access in Blood Sampling Meta-Analysis. https://www.mdpi.com/1648-9144/62/3/604
- ClinicalTrials.gov, Ultrasound-Guided Peripheral Venous Access Using AccuCath. https://clinicaltrials.gov/study/NCT02469038
- Hemophilia Federation of America (HemAware), Tips & Tricks for Accessing Problem Veins. https://hemaware.org/mind-body/tips-and-tricks-accessing-problem-veins
- SAGE Journals, Correlates of Difficult Venous Access Among People Who Inject Drugs (2025). https://journals.sagepub.com/doi/10.1177/29767342251389739
- Hospital Procedures Consultants, Most Common Techniques for Difficult Venous Access. https://hospitalprocedures.org/techniques-for-difficult-venous-access/
- Centers for Disease Control and Prevention (CDC), Hydration Guidance. https://www.cdc.gov/
- ScienceDirect (Annals of Emergency Medicine), Difficult Venous Access Risk Factors. https://www.sciencedirect.com/science/article/abs/pii/S0735675714005014







