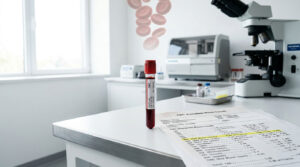
A Cardiologist’s Evidence-Based Guide to Raising HDL Without Medication
After twenty-plus years in clinical cardiology, I can tell you that one question comes up more than almost any other. Patients sit across from me, stare at their lab results, and ask: how do I boost my good cholesterol naturally? It is a great question, and one that most people don’t ask soon enough.
Table of Contents
The truth is, while most of us obsess over lowering bad cholesterol, we completely overlook the role of HDL, our body’s built-in cardiovascular cleanup crew. Raising your HDL is not just about nudging a number on a lab report. It is about improving the actual biological function of your lipid particles so they can scrub plaque from your arteries and lower your long-term risk of heart disease.
For decades, mainstream cardiology put all its energy into driving down LDL. Today, we know that optimizing your protective lipids matters just as much for a long, healthy life.
Quick Answer
Boosting HDL cholesterol naturally requires a full lifestyle approach. Focus on enhancing reverse cholesterol transport through specific dietary fats, consistent aerobic exercise, and targeted weight management. Incorporating monounsaturated fats, anthocyanin-rich foods, and Zone 2 cardio can meaningfully improve your good cholesterol levels and upgrade your heart health, all without relying solely on drugs.
Key Statistics on Cardiovascular Health in the USA
- Nearly 31.5 percent of American adults have suboptimal HDL levels, according to the American Heart Association (2023).
- Low HDL is clinically defined as below 40 mg/dL for men and below 50 mg/dL for women.
- Just 8 weeks of consistent aerobic activity can produce a measurable 5.3 percent increase in HDL markers.
- Losing 5 to 10 percent of excess body weight significantly improves good cholesterol by reducing systemic inflammation.
- Smokers who quit see up to an 11 percent rise in HDL within 4 to 6 weeks of stopping.
- Consuming 3 tablespoons of extra virgin olive oil daily is linked to a 7 percent improvement in macrophage cholesterol efflux capacity.
In this guide, I will walk you through the science of lipidology, help you decode your lab results, and give you practical, natural strategies to raise your HDL safely. These are the same methods I have used to help high-risk patients transform their cardiovascular health.
What HDL Actually Does Inside Your Body
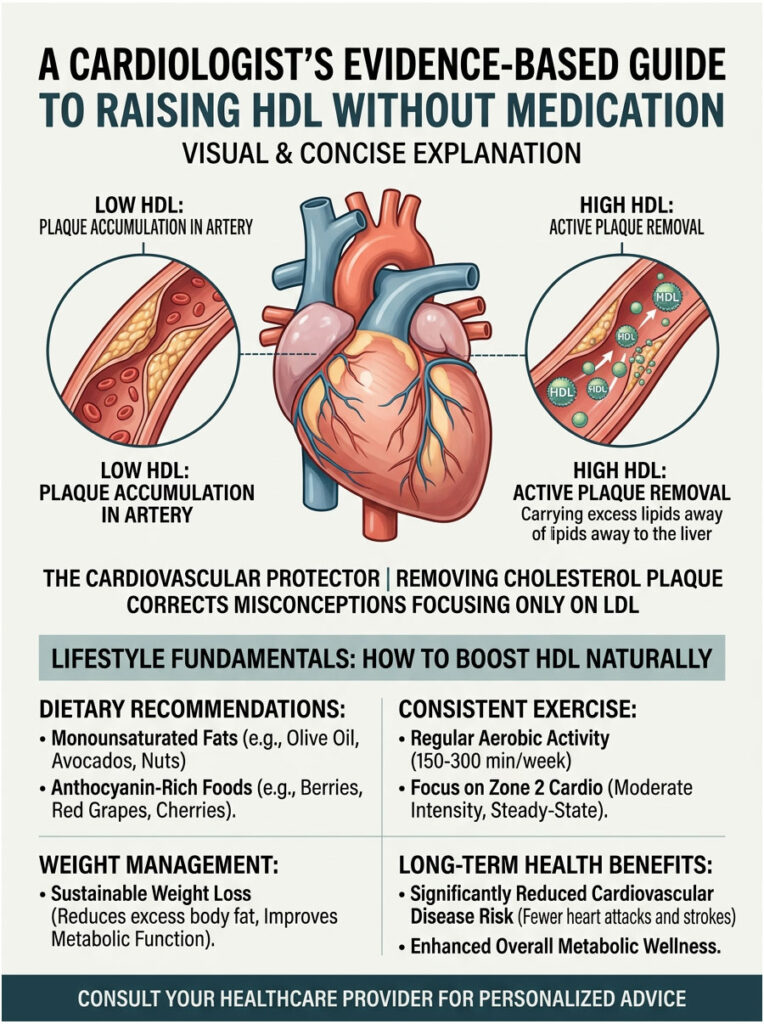
Before we talk about how to raise HDL naturally, let’s clear up what this molecule actually does. Most people picture it as a floating blob of “good fat.” In reality, HDL is a highly complex protein structure that works like a microscopic scavenger in your bloodstream.
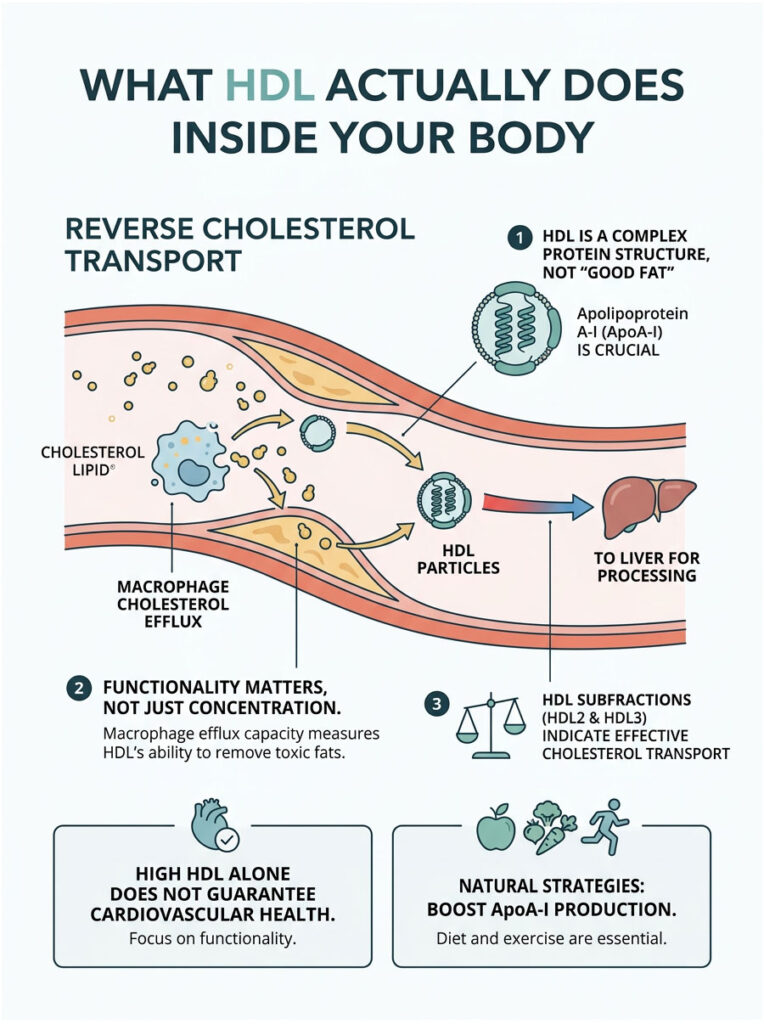
Concentration vs. Function: Why Your Number Alone Isn’t Enough
When you look at your annual blood work, you see a total HDL concentration measured in milligrams per deciliter (mg/dL). But here is what many patients don’t realize: having a high count of HDL particles does not automatically guarantee cardiovascular protection. Those particles also need to work properly.
This is where a concept called macrophage cholesterol efflux capacity comes in. In plain terms, it measures how well your HDL particles pull toxic, oxidized fats out of your artery walls.
Think of it this way. Imagine you have a fleet of 100 garbage trucks, but every engine is busted. The trash still piles up. Now picture 50 trucks that run perfectly. Your streets stay clean. That is the difference between HDL quantity and HDL quality.
A properly functioning HDL particle actively reduces inflammation in your blood vessels. A dysfunctional particle, often damaged by high blood sugar or oxidative stress, just drifts through without doing anything useful. This is exactly why the best natural strategies for raising HDL focus heavily on diet and exercise: they protect the structural integrity of the molecule itself.
How Reverse Cholesterol Transport Works
If you want to truly understand how to improve good cholesterol levels, you need to understand reverse cholesterol transport. This is the primary biological process that keeps your arteries clear of dangerous blockages.
Think of your HDL particles as highly absorbent molecular sponges. As they circulate through your blood, they run into peripheral tissues and atherosclerotic plaques. During reverse cholesterol transport, each sponge absorbs excess lipids and toxic fats from the walls of your arteries. Once the sponge is full, it travels back to the liver through your venous system.
Your liver then extracts these fats, converts them into bile acids, and pushes them out through the digestive tract. This entire cycle is essential for preventing heart attacks and strokes. When you boost HDL through healthy habits, you are directly strengthening this transport system, giving your body more sponges and making each one more absorbent.
If we can maximize reverse cholesterol transport, we can theoretically slow down, halt, or even reverse early-stage plaque buildup in the arteries. That is the ultimate goal of preventive cardiology today.
The Role of Apolipoprotein A-I (ApoA-I)
At the structural core of every HDL particle is a key protein called Apolipoprotein A-I. Think of it as the engine of the garbage truck. Without enough ApoA-I production, your body simply cannot build functional HDL particles.
Research published in the Journal of the American College of Cardiology highlights the powerful cardioprotective properties of ApoA-I. People with high levels of this protein have significantly lower rates of sudden cardiovascular events. When we talk about natural ways to raise HDL, we are really talking about how to stimulate your liver to produce more of this protein.
Certain dietary fats and specific exercise protocols directly signal your liver to ramp up ApoA-I production. On the flip side, artificial trans fats and prolonged inactivity send the opposite signal, telling the liver to shut down production. Understanding this gives you a real edge in your personal HDL optimization journey.
HDL Subfractions: HDL2 vs. HDL3
Not all HDL particles are the same size or have the same function. In advanced lipidology, we break them into subfractions, mainly HDL2 and HDL3.
HDL3 particles are small, dense, and freshly produced by the liver. They act as empty sponges, ready to absorb plaque from your arteries. As they pick up cholesterol, they swell and transform into the larger, more buoyant HDL2 particles.
Cardiologists want to see a healthy transition from HDL3 to HDL2 because it proves that reverse cholesterol transport is actively happening. If your blood only contains small HDL3 particles, it means the sponges aren’t collecting any debris. Effective natural strategies target this maturation process, helping particles grow large, buoyant, and highly protective.
Decoding Your Lipid Panel: Ratios and Risk Factors
Many patients walk into my office and panic over a single number on their lab results. But to properly assess your actual cardiovascular risk, you need to look at the full metabolic picture.

Clinical Targets for Men and Women
In the United States, cardiovascular guidelines set distinct targets based on biological sex, largely because of the powerful cardioprotective effects of estrogen. For men, HDL levels need to stay above 40 mg/dL. Anything below that signals a severe lack of reverse cholesterol transport and a dangerously elevated risk for cardiac events.
For women, the threshold is higher. Women need their HDL above 50 mg/dL to maintain cardiovascular safety. Before menopause, estrogen naturally helps keep HDL elevated and blood vessels flexible. After menopause, estrogen levels drop sharply, and many women watch their HDL plummet almost overnight. This makes HDL optimization especially important for women in their fifties and sixties.
Ideally, both men and women should aim for 60 mg/dL or higher. At that level, the medical community considers your HDL to be highly protective against ischemic heart disease. Reaching that target takes daily commitment to the lifestyle strategies we will cover.
The Triglyceride-to-HDL Ratio: Your Most Important Number
Your HDL number does not exist in isolation. It interacts constantly with your triglycerides, the primary storage form of fat in your blood.
The first thing I calculate on every new patient’s chart is their Triglyceride-to-HDL ratio. This single ratio is one of the best clinical markers for hidden insulin resistance and looming metabolic syndrome. When you eat too many refined carbohydrates, your body rapidly converts them into triglycerides. High triglycerides degrade your HDL particles in the bloodstream, stripping away the crucial ApoA-I protein and leaving the particle small, dense, and useless.
To calculate your ratio, divide your total triglycerides by your HDL number. For example, triglycerides at 150 and HDL at 50 gives you a ratio of 3.0. The clinical ideal is below 2.0. If your ratio climbs above 3.0, you are likely dealing with meaningful insulin resistance that needs immediate lifestyle changes.
Fasting vs. Non-Fasting Lipid Panels
Patients often wonder whether they really need to fast before getting their cholesterol checked. Traditionally, a strict 12-hour fast was required to make sure triglycerides were not inflated by a recent meal. But modern cardiology has evolved.
Non-fasting panels actually give a more realistic picture of your everyday metabolic state. You spend most of your life in a fed state, after all. If your triglycerides spike wildly after eating and crush your HDL, your cardiologist needs to see that reaction. That said, if your non-fasting triglycerides come back abnormally high, your doctor will likely order a fasting panel to confirm the baseline.
| Biomarker | Optimal Target | High Risk Level | Clinical Significance |
| HDL (Men) | 60 mg/dL or higher | Below 40 mg/dL | Compromised reverse cholesterol transport |
| HDL (Women) | 60 mg/dL or higher | Below 50 mg/dL | Loss of estrogen-derived cardioprotection |
| Triglycerides | Below 100 mg/dL | Above 150 mg/dL | High levels actively degrade HDL particles |
| TG/HDL Ratio | Less than 2.0 | Greater than 3.0 | Strong indicator of insulin resistance |
Evidence-Based Dietary Strategies for Raising HDL
When patients ask me how to increase HDL cholesterol, my first prescription is always written for the grocery store. Food is biological information for your cells. The specific fats and antioxidants you eat directly determine how well your liver produces functional HDL particles.

Monounsaturated Fats and the Mediterranean Approach
Shifting from a standard American diet to a Mediterranean-style eating pattern is the single most important dietary change for HDL optimization. The typical American diet leans heavily on processed seed oils and inflammatory saturated fats. The Mediterranean approach, by contrast, puts monounsaturated fats (MUFAs) front and center, and clinical research consistently shows they improve good cholesterol levels.
Extra virgin olive oil is the gold standard here. High-quality olive oil contains oleocanthal, a phenolic compound that protects your HDL particles from oxidative damage while they circulate. I tell my patients to aim for two to three tablespoons of raw, unheated extra virgin olive oil each day. Drizzle it over salads, toss it with roasted vegetables, or simply use it as a finishing oil.
Other excellent MUFA sources include fresh avocados and raw macadamia nuts. Eating half an avocado daily provides exactly the type of fatty acids your liver needs to sustain high ApoA-I production. These dietary changes are not just effective; they are sustainable and genuinely enjoyable.
The Purple Effect: Anthocyanins and Heart Health
Here is something most people don’t know about. Anthocyanins are the natural plant pigments responsible for the deep colors in blueberries, blackberries, and purple cabbage. From a cardiology standpoint, these compounds are incredibly powerful.
When you eat anthocyanin-rich foods, you directly reduce oxidative stress in your blood vessels. Oxidative stress is the biggest enemy of macrophage cholesterol efflux capacity. If your bloodstream stays inflamed, your HDL particles get oxidized and lose their ability to transport fats effectively.
Research shows that consuming just one cup of wild blueberries daily can significantly improve HDL function. The antioxidants bind to your HDL particles like a biological shield, preserving their structural integrity so they can keep doing their cleanup work. Adding raw purple cabbage to your regular meals is another cost-effective way to improve good cholesterol levels.
Omega-3 Fatty Acids (EPA/DHA) for Triglyceride Reduction
You cannot successfully raise HDL without also tackling your triglycerides. This is where marine-sourced Omega-3 fatty acids become essential.
EPA and DHA, the key Omega-3s found in cold-water fish, have a synergistic relationship with HDL. When you eat wild-caught salmon, mackerel, or sardines, the Omega-3s signal your liver to dial back triglyceride production. As triglycerides drop, your HDL particles finally have room to grow larger and more buoyant. A bigger particle has a much greater efflux capacity, meaning it can pull significantly more plaque from your artery walls.
For patients who will not eat fish, chia seeds and flaxseeds offer a plant-based alternative. However, the conversion rate of plant Omega-3s to usable EPA and DHA is quite low. For maximum results, I recommend marine sources or a high-quality, pharmaceutical-grade fish oil supplement.
Foods That Destroy Your HDL: Trans Fats and Refined Carbs
You cannot supplement your way out of a bad diet. If you seriously want to improve good cholesterol levels, you need to cut the foods that actively destroy HDL.
Artificial trans fats, often listed as partially hydrogenated oils, are the single most destructive ingredient for your lipid profile. They directly inhibit your liver’s ApoA-I production at a cellular level, telling your body to stop building the very particles that protect your heart. Even small amounts lurking in commercial baked goods and fried foods can wreck your lab results for weeks.
Refined carbohydrates and added sugars are nearly as damaging. When you consume sugary drinks or pastries, your blood sugar spikes rapidly. That spike triggers a process called glycation, where sugar molecules physically latch onto your HDL proteins and permanently damage them. A glycated particle cannot perform reverse cholesterol transport. It becomes biological dead weight.
The Overlooked Power of Soluble Fiber
Many patients skip right past dietary fiber when working on their HDL, and that is a mistake. Soluble fiber, found in oats, beans, and psyllium husk, plays a surprisingly important dual role in your gut.
When you eat soluble fiber, it forms a thick gel in your digestive tract that slows carbohydrate absorption and prevents the blood sugar spikes that trigger glycation. By stabilizing blood sugar, fiber directly protects your HDL particles from damage.
Fiber also feeds your gut microbiome, which produces short-chain fatty acids like butyrate. Butyrate travels to the liver and helps regulate overall lipid metabolism. Aiming for 30 to 40 grams of total fiber daily is non-negotiable if you want to improve your HDL naturally.
Expert Insight: Don’t fall for the outdated low-fat diet myth. In my practice, patients who adopt strict low-fat diets almost always see a dangerous drop in HDL. Your liver needs healthy dietary fats to manufacture these particles. Replace processed carbs with healthy fats, rather than eliminating fats entirely.
| Food Category | Best Sources | Impact on HDL | How It Works |
| Healthy Fats (MUFAs) | Olive oil, avocados | Increases HDL particles | Enhances ApoA-I production |
| Anthocyanins | Blueberries, purple cabbage | Improves particle function | Reduces oxidative stress |
| Refined Sugars | Soda, pastries | Crushes HDL levels | Spikes triglycerides, causes glycation |
| Trans Fats | Hydrogenated oils | Destroys HDL particles | Directly blocks ApoA-I production |
Exercise and Lipid Metabolism: The Aerobic Threshold
Diet gives your body the raw building blocks. Exercise provides the metabolic engine. If you want to meaningfully raise HDL, you need to move your body strategically, and not all exercise is equal when it comes to lipid health.

Zone 2 Training: The Sweet Spot for HDL
Cardiologists frequently recommend Zone 2 training for lipid optimization. Zone 2 refers to steady-state, moderate-intensity aerobic exercise where your heart rate stays elevated but stable, roughly 60 to 70 percent of your maximum. You should be breathing hard but still able to hold a short conversation.
Why does Zone 2 work so well? It comes down to mitochondrial density. Consistent Zone 2 cardio builds more mitochondria inside your muscle cells. These tiny cellular powerhouses burn fat for fuel, clearing it from your blood. As your aerobic capacity improves, your body becomes incredibly efficient at processing circulating lipids, which directly translates to larger, more buoyant, and more protective HDL particles.
The physical stress of blood pumping through your arteries also stimulates nitric oxide release. Nitric oxide repairs the endothelial lining, making reverse cholesterol transport easier and more efficient.
The 5 Percent Rule for Beginners
Many patients feel overwhelmed by the idea of starting an exercise program. They assume they need to train for a marathon to see any benefit on their labs. That is not the case.
The American Heart Association guidelines support what I call the 5 percent rule. Clinical data shows that just 8 weeks of consistent, moderate aerobic activity produces a 5 percent increase in HDL markers. For someone starting at a dangerously low 40 mg/dL, 5 percent may not sound dramatic. But in preventive cardiology, every single milligram counts.
Consistency matters far more than extreme intensity. A 30-minute brisk walk after dinner every day will improve your HDL more reliably than one brutal workout per week. Keep the metabolic engine running smoothly, day after day.
Resistance Training for Metabolic Syndrome Reversal
While aerobic exercise is the primary driver for HDL optimization, resistance training plays a powerful supporting role. Lifting weights builds metabolically active skeletal muscle, which acts as your body’s largest glucose disposal system.
When you build muscle, you increase the number of GLUT4 receptors on your cell membranes. These receptors pull excess sugar from your blood, improving insulin sensitivity. Better insulin sensitivity leads directly to a lower Triglyceride-to-HDL ratio.
By reversing metabolic syndrome markers through strength training, you indirectly boost your entire lipid profile. The less insulin your pancreas has to pump out, the more efficiently your liver can focus on making ApoA-I. I recommend combining Zone 2 aerobic work with two days of full-body resistance training for the best results.
What About HIIT?
Younger patients often ask if high-intensity interval training works better than Zone 2. HIIT involves short, explosive bursts of maximum effort followed by brief recovery periods. While HIIT is excellent for improving VO2 max, its effects on HDL are somewhat different.
HIIT burns through glycogen quickly, forcing your body to become highly insulin sensitive in the hours after the workout. That insulin sensitivity helps crush triglycerides fast. However, for the specific goal of boosting ApoA-I production, steady-state Zone 2 training still has the edge.
My recommendation: use a hybrid approach. Do Zone 2 cardio three days a week, and add one short, 15-minute HIIT session to keep your metabolism adaptable.
Lifestyle Shifts: Weight Management, Stress, and Sleep
Your daily habits and body composition have a profound effect on blood chemistry. To truly optimize reverse cholesterol transport, you need to address the hidden lifestyle factors that quietly undermine your heart health.

Visceral Fat and Insulin Resistance
How does weight loss actually affect HDL cholesterol? The answer depends on the type of fat you are carrying. Subcutaneous fat, the soft layer just under your skin, is relatively harmless. Visceral fat, the hard belly fat wrapped tightly around your organs, is a different story entirely.
Visceral fat is metabolically active and behaves like an unwanted endocrine organ. It constantly pumps inflammatory cytokines into your bloodstream. These chemicals travel straight to your liver, where they suppress HDL production and ramp up triglyceride synthesis. This is why people with large waist measurements almost always have low HDL numbers.
The good news: losing just 5 to 10 percent of your total body weight, specifically targeting visceral fat, can transform your lipid panel. As inflammation decreases, your liver gets back to normal ApoA-I production.
The Immediate Impact of Quitting Smoking
Let’s be blunt. If you smoke, every other strategy we have discussed is fighting an uphill battle. Tobacco smoke is loaded with toxic chemicals that directly interfere with lipid metabolism.
The carbon monoxide and oxidative stress from smoking physically damage your HDL particles, rendering them useless for reverse cholesterol transport. A smoker’s HDL particles are essentially broken trucks clogging the arterial highways.
But your body is remarkably resilient. Clinical data shows a rapid 10 to 11 percent increase in HDL following complete smoking cessation, often within just 4 to 6 weeks. Once you stop flooding your bloodstream with toxins, your liver quickly ramps up ApoA-I production to repair the damage. Quitting smoking is an absolute prerequisite for anyone serious about improving their HDL.
Stress, Cortisol, and Lipid Disruption
We cannot talk about HDL optimization without addressing chronic stress. In today’s fast-paced world, chronic stress has become a silent cardiovascular risk factor.
When you are constantly stressed, your adrenal glands flood your system with cortisol. Cortisol was designed for short-term emergencies. It spikes your blood sugar so you have quick energy to escape danger. But when cortisol stays elevated chronically, it drives insulin resistance. Rising insulin means rising triglycerides, and falling HDL. This vicious cycle destroys your Triglyceride-to-HDL ratio.
Daily stress management through deep breathing, mindfulness, or any practice that lowers your sympathetic nervous system activity is a clinical necessity, not a luxury.
Sleep: The Silent Variable in Lipid Health
Sleep is not optional if you care about your lipids. During deep sleep, your body performs essential metabolic maintenance. Your liver uses this downtime to package and distribute lipid particles efficiently.
Patients with sleep apnea or chronic insomnia experience fragmented sleep that keeps their fight-or-flight system activated all night. This nocturnal stress prevents the liver from optimizing reverse cholesterol transport.
Prioritizing seven to eight hours of uninterrupted, quality sleep per night consistently produces better lipid panels. Fixing your sleep hygiene is one of the most underrated strategies for raising HDL.
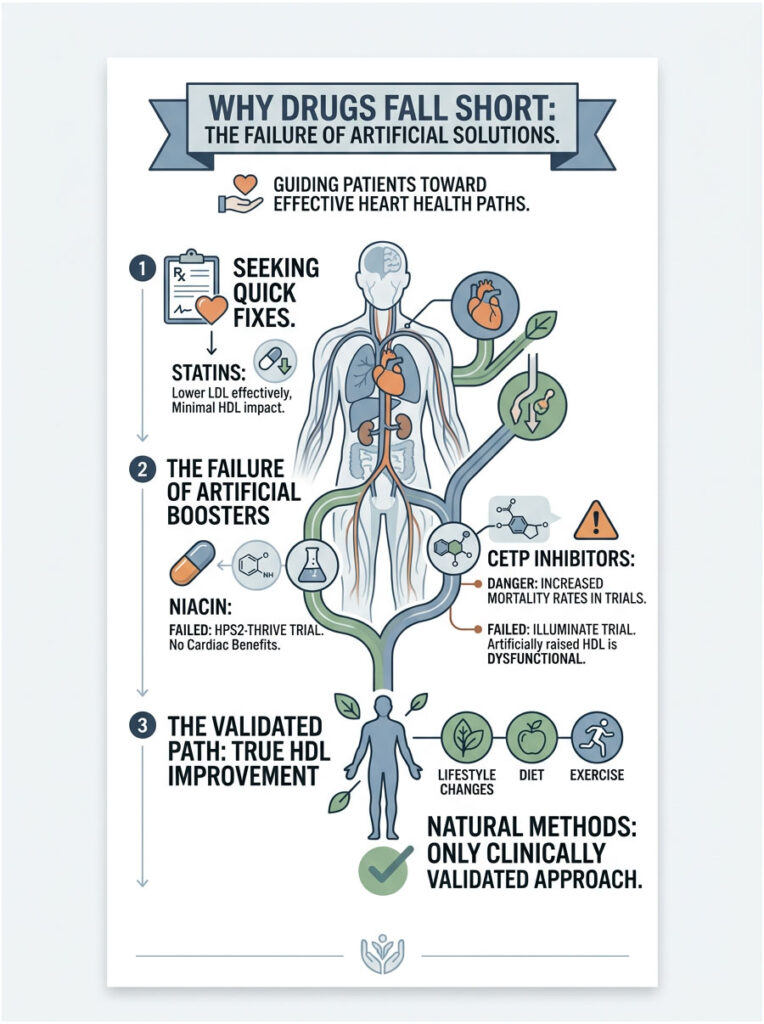
Why Drugs Fall Short: The Failure of Artificial Solutions
Many patients hope I will just write a prescription to fix their low HDL. They want a pill that instantly raises the number without any effort. Unfortunately, cardiovascular pharmacology has repeatedly proven that artificially boosting HDL does not work.
The Niacin Paradox
For decades, doctors prescribed high-dose Niacin (Vitamin B3) to raise HDL. Niacin was remarkably effective at pushing the number up on a lab report. Patients would watch their HDL jump from 35 to 60 mg/dL and assume they were protected.
Then came the HPS2-THRIVE trial, a massive clinical study testing whether artificially raised HDL actually prevented heart attacks. The results shocked the medical community. Despite dramatic HDL increases, patients on Niacin did not have fewer cardiac events than those on placebo. They actually experienced more side effects, including liver damage.
The lesson was humbling. Forcing the number higher with supplementation does not improve macrophage cholesterol efflux capacity. The particles Niacin created were dysfunctional. To gain real protection, you must improve HDL naturally through diet and exercise.
The CETP Inhibitor Disappointments
After the Niacin failure, pharmaceutical companies poured billions into developing CETP inhibitors, drugs designed to block cholesterol transfer from HDL to LDL. Early trials showed HDL numbers rising by as much as 100 percent. It looked like the holy grail of lipid therapy.
Then the ILLUMINATE trial tested Torcetrapib in thousands of high-risk patients. The trial was halted early because patients on the drug were dying at higher rates. The drug had created massive, bloated HDL particles that could not perform reverse cholesterol transport. These repeated failures reinforce that natural methods remain the only clinically valid approach to raising HDL.
Statins and Their Limits
Statins are the most prescribed cardiovascular drugs in the world, and they are excellent at lowering bad LDL cholesterol. They save countless lives by stabilizing plaque and reducing inflammation.
However, statins do very little for HDL. At best, a high-intensity statin might raise your HDL by 2 to 4 percent. Statins simply are not designed to stimulate ApoA-I production. That is why I tell my patients: statins handle the bad guys, but you have to build the good guys yourself through daily lifestyle work.
Advanced Nutritional Strategies for HDL Optimization
Once you have the Mediterranean diet and Zone 2 cardio locked in, you can explore these advanced nutritional interventions for an extra edge.
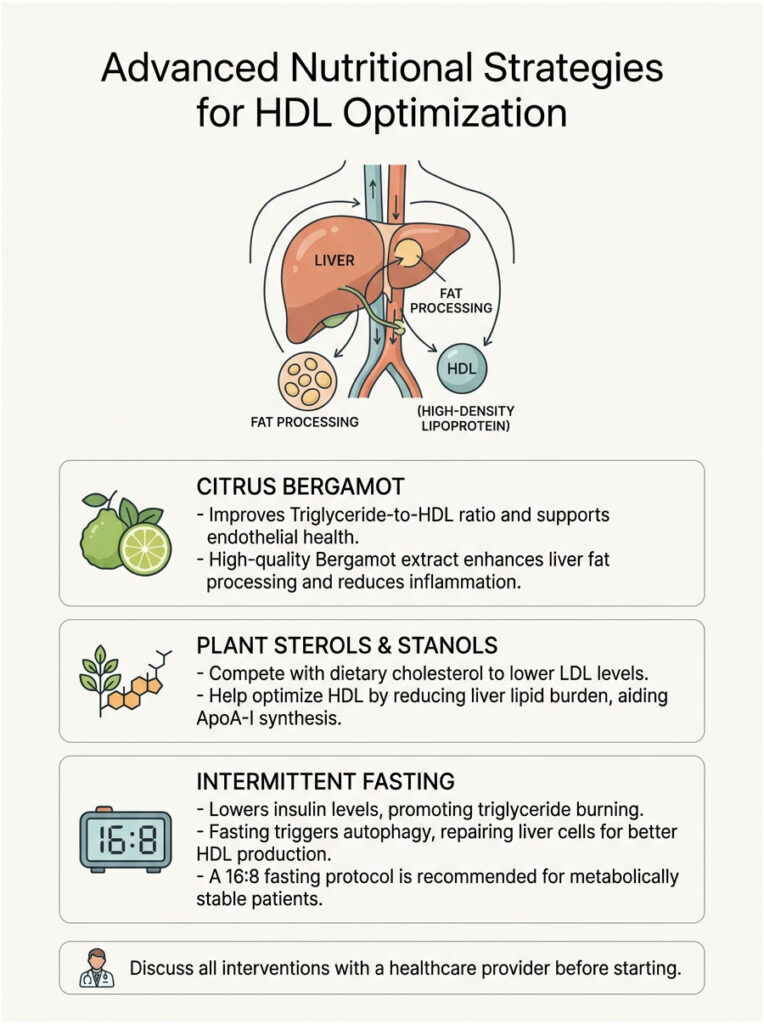
Citrus Bergamot and Endothelial Repair
Citrus Bergamot is a fruit extract sourced primarily from the Calabria region of Italy that has gained serious attention in preventive cardiology. It contains a unique polyphenol profile that acts similarly to a mild statin, with a bonus: it also directly improves the Triglyceride-to-HDL ratio.
Clinical studies show that high-quality Bergamot extract helps the liver process circulating fats more efficiently while reducing systemic inflammation. By calming the endothelium (the inner lining of your blood vessels), Bergamot allows your HDL to function at its best. I frequently use a 500mg daily dose of standardized Citrus Bergamot for patients struggling with stubborn ratios.
Plant Sterols and Stanols
Plant sterols and stanols are natural compounds found in certain plant cell membranes. Structurally, they look almost identical to human cholesterol. When you eat them, they compete with dietary cholesterol for absorption in your gut.
Their main claim to fame is lowering LDL, but they indirectly help HDL optimization too. By blocking bad fat absorption, they reduce the lipid burden on your liver, freeing up resources for ApoA-I synthesis. You can find plant sterols naturally in nuts, seeds, and legumes. For therapeutic doses, fortified foods or specific supplements are available. Always discuss these with your cardiologist before starting.
Intermittent Fasting and Insulin Dynamics
Intermittent fasting has become wildly popular, but does it actually improve good cholesterol? The clinical data says yes, primarily through its effect on insulin.
When you restrict your eating window to roughly 8 hours, your insulin levels drop to baseline for the remaining 16 hours. This extended period of low insulin forces your body to burn stored triglycerides for fuel. As triglycerides drop, your HDL particles have room to thrive. Fasting also triggers autophagy, a cellular cleaning process that repairs damaged liver cells, resulting in higher-quality HDL production.
I typically recommend a gentle 16:8 fasting protocol for metabolically stable patients. It is a no-cost, highly effective method to enhance reverse cholesterol transport.
Your Personal Action Plan: How to Boost Good Cholesterol Naturally
Knowledge without action is useless. Here is the exact three-week protocol I use to help patients transition into a heart-healthy lifestyle.

Week 1: Dietary Reset
Start by going through your kitchen and removing any product containing partially hydrogenated oils or high-fructose corn syrup. These are HDL’s worst enemies.
Next, pick up a high-quality, cold-pressed extra virgin olive oil in a dark glass bottle. Commit to two tablespoons per day on salads or mixed into vegetables. Add one cup of wild blueberries to your morning routine for those critical anthocyanins.
Finally, swap two of your weekly meat-heavy dinners for fatty fish like wild-caught salmon or sardines. The Omega-3 influx will start driving down your triglycerides within days. Lock in this dietary foundation before we add metabolic stress.
Week 2: Building Your Aerobic Engine
In week two, we fire up the metabolic engine. Schedule four 45-minute sessions of Zone 2 cardio into your weekly calendar. Whether you choose brisk walking, cycling, or swimming, keep your heart rate in that moderate, conversational zone.
Don’t push too hard. Excessive physical stress can temporarily spike cortisol and undermine your progress. Consistency is your strongest weapon here. After each session, your muscles act like sponges, soaking up excess glucose from your blood. Treat these sessions like non-negotiable medical appointments.
Week 3: Sleep and Stress Optimization
In the third week, we tackle the silent killers of cardiovascular health. You need to regulate cortisol levels to protect your newly formed HDL particles.
Establish a strict sleep routine, aiming for eight hours in bed every night. Turn off all blue-light screens an hour before bed to let natural melatonin production peak. Add a simple 10-minute deep breathing exercise to your morning to keep your sympathetic nervous system calm.
Lower stress means lower triglycerides, which means higher HDL. This three-week ramp-up prevents overwhelm and helps these changes become permanent habits.
Summary and Key Takeaways
The answer to how to boost good cholesterol levels naturally is clear: adopt a multi-faceted lifestyle approach that prioritizes biological function over artificial lab numbers. Your goal is to enhance reverse cholesterol transport, clear arterial plaque, and optimize your metabolic health.

Natural strategies for raising HDL are the most effective, evidence-based tools available in modern medicine. Drugs are great for lowering LDL, but they do very little for HDL. You hold the power to upgrade your internal cleaning crew.
5 Steps You Can Start Today
- Swap Your Cooking Oils: Ditch processed seed oils and commit to high-quality extra virgin olive oil daily to support ApoA-I production.
- Calculate Your Ratio: Divide your total triglycerides by your HDL. Aim for a Triglyceride-to-HDL ratio below 2.0.
- Start Zone 2 Cardio: Commit to 45 minutes of moderate, steady-state aerobic exercise four times a week.
- Eat the Rainbow: Add wild blueberries and raw purple cabbage to your weekly grocery list for powerful anthocyanins.
- Target Visceral Fat: Focus on sustainable weight loss. Dropping just 5 percent of your body weight can dramatically improve your lab results.
Take control of your cardiovascular health today. By putting these evidence-based strategies into practice, you will build a resilient, highly functional metabolic system that protects your heart for decades to come.
Frequently Asked Questions
Why is my HDL function more important than the actual number on my lab report?
As a cardiologist, I look beyond the concentration measured in mg/dL. Having a high volume of particles doesn’t guarantee protection if those particles are ‘broken.’ We focus on macrophage cholesterol efflux capacity, which is the ability of your protective lipids to actually ‘scrub’ toxic fats from arterial walls. You want highly functional particles that actively perform reverse cholesterol transport, rather than just a high concentration of dysfunctional ones.
What is the clinical significance of my Triglyceride-to-HDL ratio?
This ratio is perhaps the most critical marker for hidden insulin resistance. To calculate it, divide your total triglycerides by your HDL level. In my clinical practice, I look for a ratio strictly under 2.0. A ratio above 3.0 suggests that high levels of insulin and triglycerides are actively stripping away the vital Apolipoprotein A-I proteins from your ‘good’ cholesterol, leaving you at higher cardiovascular risk.
Which dietary fats are most effective for increasing good cholesterol levels naturally?
Monounsaturated fats (MUFAs) are the biological foundation for HDL optimization. I recommend consuming two to three tablespoons of raw, high-quality extra virgin olive oil daily. Olive oil contains oleocanthal, which protects your lipid particles from oxidative damage. Other excellent sources include fresh avocados and macadamia nuts, which provide the liver with the raw materials needed to synthesize more Apolipoprotein A-I.
How do anthocyanins in berries help improve my lipid profile?
Anthocyanins are the pigments found in wild blueberries and purple cabbage that act as a biological shield for your heart. These compounds reduce oxidative stress within the blood vessels, which preserves the structural integrity of your HDL particles. By preventing these particles from becoming oxidized, anthocyanins ensure your internal ‘garbage trucks’ stay functional and capable of transporting plaque to the liver.
What is the best exercise protocol for boosting HDL cholesterol?
Zone 2 aerobic training is the gold standard for lipid metabolism. This involves steady-state, moderate-intensity exercise—like a brisk walk or stationary cycling—where you maintain 60 to 70 percent of your maximum heart rate. This specific intensity increases mitochondrial density in your muscles, making your body more efficient at clearing circulating fats and stimulating the production of larger, more buoyant protective lipids.
How does losing visceral fat specifically impact my good cholesterol?
Visceral fat, the deep belly fat surrounding your internal organs, acts like an inflammatory organ. it releases cytokines that travel to the liver and suppress the production of protective lipids. In my experience, losing just 5 to 10 percent of your body weight—specifically targeting that midsection—reduces systemic inflammation enough to allow your liver to resume healthy Apolipoprotein A-I synthesis and raise your HDL naturally.
Can quitting smoking really raise my HDL levels in just a few weeks?
Yes, the impact is remarkably rapid. Tobacco smoke introduces toxins that physically damage the protein structure of your protective lipids, rendering them useless for reverse cholesterol transport. Clinical data shows that within 4 to 6 weeks of complete cessation, patients often experience an 11 percent rise in protective lipids as the liver upregulates production once the toxic interference is removed.
What is the difference between HDL2 and HDL3 subfractions on advanced tests?
Think of HDL3 as a small, newly formed ’empty sponge’ produced by the liver. As it circulates and absorbs cholesterol from your arteries, it swells and matures into the larger, buoyant HDL2 particle. As a cardiologist, I want to see a healthy transition from HDL3 to HDL2, as this confirms that the reverse cholesterol transport process is actively and effectively clearing your blood vessels.
Why shouldn’t I just take high-dose Niacin to raise my HDL?
The Niacin Paradox, highlighted in the HPS2-THRIVE trial, taught us a vital lesson: artificially raising the number on a lab report with supplements does not equate to heart protection. Niacin can increase the concentration of HDL, but it often creates dysfunctional particles that cannot perform their cleaning duties. To gain real cardiovascular benefits, you must improve particle function through diet and exercise.
Why are the clinical targets for good cholesterol different for men and women?
Biological sex plays a role due to the profound cardioprotective effects of estrogen, which naturally helps improve good cholesterol levels. For men, we look for a minimum of 40 mg/dL, while women require at least 50 mg/dL to maintain safety. After menopause, when estrogen levels drop, women often see a sharp decline in protective lipids, making natural optimization strategies like Zone 2 cardio even more critical.
Does intermittent fasting help with HDL cholesterol optimization?
Intermittent fasting is highly effective because it improves insulin dynamics. By extending the period where insulin remains at baseline, you force your body to metabolize stored triglycerides for energy. Since high triglycerides are a primary driver of low HDL, this metabolic shift allows your protective lipid particles to grow larger and more efficient at clearing arterial plaque.
Should I follow a low-fat diet if I want to improve my good cholesterol?
Actually, a strict low-fat diet is often counterproductive. In my clinical practice, I frequently see protective lipids plummet in patients who avoid all fats. Your liver requires healthy dietary fats to manufacture these particles. The key is to replace processed carbohydrates and trans fats with high-quality monounsaturated fats and marine-sourced Omega-3s, rather than eliminating fat entirely.
Disclaimer
This article is for informational and educational purposes only and does not constitute formal medical advice, diagnosis, or treatment. The content is written from the perspective of a board-certified cardiologist but should not replace a one-on-one relationship with a qualified healthcare professional. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition or before beginning any new diet, exercise, or supplement program.
References
- American Heart Association (AHA) – 2023 Statistical Update – Provides the foundational data on suboptimal lipid levels among American adults.
- Journal of the American College of Cardiology (JACC) – 2021 Clinical Publication – Research regarding the role of Apolipoprotein A-I in macrophage cholesterol efflux capacity.
- New England Journal of Medicine (NEJM) – PREDIMED Study – Authoritative source on the cardiovascular benefits of the Mediterranean diet and olive oil.
- New England Journal of Medicine (NEJM) – HPS2-THRIVE Trial – The landmark study identifying the “Niacin Paradox” and the failure of artificial HDL boosting.
- The Lancet – ILLUMINATE Trial – Clinical data regarding the safety and failure of CETP inhibitors like Torcetrapib.