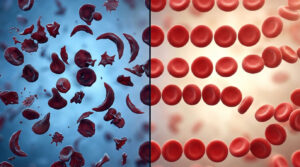
A newly pregnant patient I worked with last spring found out she had Type 2 diabetes at her first prenatal visit. She had no symptoms. No family history. Her A1C was 8.2. Because she called the day her home test turned positive, we caught it at 7 weeks, got her glucose under control, and she delivered a full-term, normal-weight baby. If she’d waited three months, the story would have ended differently. That’s prenatal care in one sentence: the thing you don’t know you need, until you really needed it.
Table of Contents
Quick Answer: Prenatal care is the medical care you get during pregnancy, covering regular checkups, lab work, ultrasounds, and vaccines. The CDC and ACOG recommend starting before 10 weeks. Babies of moms who skip it are three times more likely to be low birth weight and five times more likely to die, and US insurance (including Medicaid and ACA plans) covers it as a required benefit.

At a Glance
• Start prenatal care before 10 weeks; 6 to 8 weeks after your last period is ideal
• ACOG’s 2025 guidance permits 6 to 10 tailored visits for average-risk pregnancies
• Skipping prenatal care triples the risk of low birth weight and quintuples infant death
• Medicaid pays for about 41% of US births, often at $0 out of pocket
• 400 mcg of folic acid daily cuts neural tube defects by roughly 70%
• Call 1-800-311-BABY to find affordable care in your state
What Is Prenatal Care?
Prenatal care is every medical visit, screening, and conversation you have with a qualified provider from the moment pregnancy is confirmed through delivery. It’s not a single ultrasound or one big appointment. Think of it as a rolling relationship with an OB-GYN, certified nurse-midwife, or family medicine doctor who tracks your vitals, your baby’s growth, and the small changes that tell us whether everything’s on track.

In my work with first-time moms, I’ve noticed the biggest myth is that prenatal care is mostly ultrasounds. It isn’t. Blood pressure checks, urine dips, glucose screenings, and mental-health conversations usually carry more weight than any single scan.
What US Clinicians Actually Mean by “Prenatal Care”
According to ACOG, prenatal care has three jobs: medical screening and treatment, anticipatory guidance, and psychosocial support. Every visit should advance at least one of those. That’s why a ten-minute blood-pressure check still counts as real care, even if it feels short.
How the US Compares to Other High-Income Countries
The UK typically offers 7 to 10 antenatal visits for low-risk pregnancies. Canada runs about 10. The US traditionally pushed 12 to 14, a schedule built in 1930 and never seriously revised until recently. In April 2025, ACOG’s new Clinical Consensus allowed 6 to 10 visits for average-risk patients. Most OB practices I’ve spoken with are still easing into it.
Why Prenatal Care Matters (The US Data Is Blunt)
The case for showing up is straightforward: the earlier a provider sees you, the earlier they catch problems that are cheap to fix now and expensive or deadly later. I’ve had patients pushback (“I feel fine, do I really need this visit?”), and the honest answer is yes, because the whole point is to find what you can’t feel yet.

Maternal Mortality: The US Is an Outlier
Per CDC data for 2024, the US maternal mortality rate was 17.9 deaths per 100,000 live births. That’s down slightly from 18.6 in 2023, which is progress, but not the kind to celebrate. Black women faced a rate of 44.8 per 100,000, more than three times the rate for white women (14.2).
Most of these deaths are preventable. CDC reviews consistently find that hypertensive disorders, hemorrhage, infection, and cardiac events account for the majority. Almost all of them show warning signs at routine prenatal visits.
Low Birth Weight and Infant Mortality
The Office on Women’s Health reports that babies of moms who get no prenatal care are three times more likely to have low birth weight and five times more likely to die. Those numbers aren’t models. They come from decades of US vital-statistics data.
What a Routine First-Trimester Workup Actually Catches
A typical first-trimester visit flags anemia, hypothyroidism, hepatitis B, HIV, Rh incompatibility, ectopic pregnancy, elevated diabetes risk, and molar pregnancy, often before any symptoms appear. Each one has a cheap intervention if caught early and a terrible course if missed. I once saw a patient’s thyroid levels picked up at week 9 (she felt tired, which she’d chalked up to “just being pregnant”). A $12 daily pill kept the pregnancy completely normal.
Table 1: Early Prenatal Care vs. No Prenatal Care — US Outcomes
| Outcome Metric | With Early, Regular Care | With No Prenatal Care | US Source |
| Low birth weight (under 5 lbs 8 oz) | Baseline risk | 3x higher risk | Office on Women’s Health |
| Infant mortality (first year) | Baseline risk | 5x higher risk | Office on Women’s Health |
| Preterm birth rate | ~10% | 18 to 20% | CDC MMWR |
| Gestational diabetes caught before 28 weeks | ~95% of cases | Often diagnosed at delivery | ACOG |
| Postpartum depression screened | Routinely | Rarely screened | ACOG Committee Opinion |
When Should You Start Prenatal Care?
I tell every new patient the same thing: call the day your home test is positive. Good OB offices schedule an intake within 1 to 3 weeks, sometimes sooner.
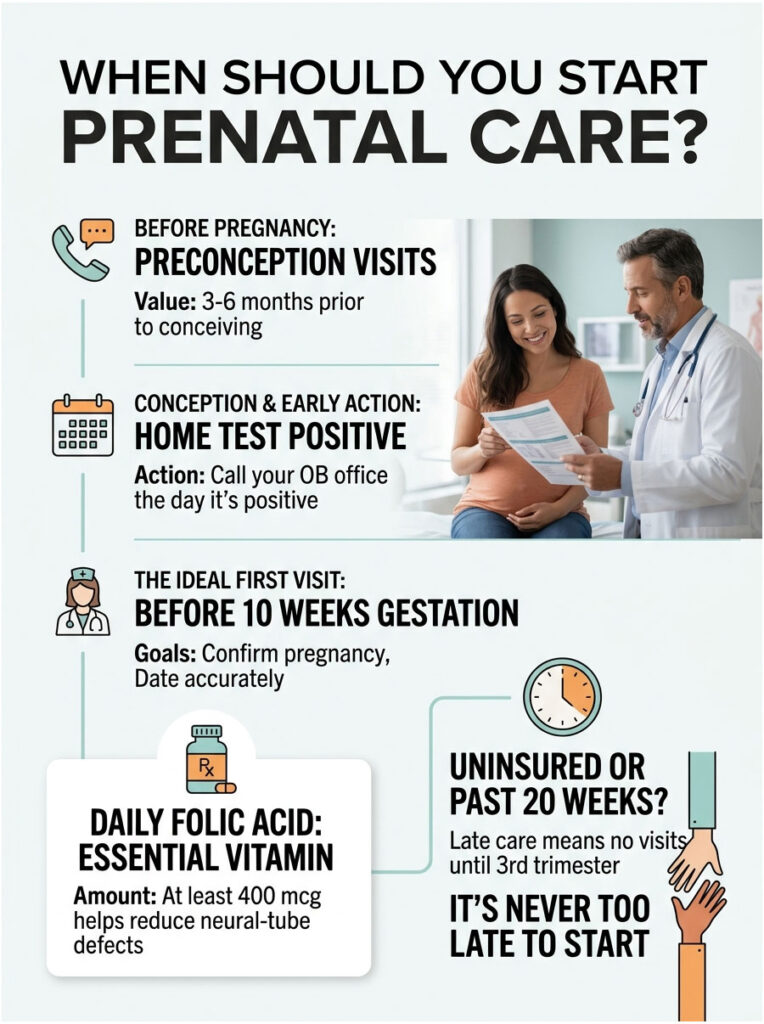
The Ideal: Before 10 Weeks
ACOG’s goal is a first in-person visit before 10 weeks of gestation, counted from the first day of your last menstrual period. That window lets your provider confirm the pregnancy, date it accurately, start or adjust folic acid, and run the big first-trimester lab panel while it still matters.
Preconception Visits
If you’re actively trying, a preconception visit three to six months before stopping birth control is one of medicine’s highest-value appointments. NICHD research shows at least 400 mcg of folic acid daily, started before conception, cuts neural-tube defects by about 70%. That single detail alone is worth the visit.
What “Late Prenatal Care” Means
In US vital statistics, late care means no visits until the third trimester (or none at all). It’s more common than people think, and self-pay and uninsured moms are far more likely to end up in that group. If you’re reading this past 20 weeks without any care yet, call today anyway. Something is always better than nothing, and catch-up testing can still flag gestational diabetes, Group B strep, and growth restriction in time to act.
The Prenatal Care Schedule (Average-Risk Pregnancy)
This is the section readers usually come here for, so I’ll be specific.

ACOG’s 2025 “Tailored Prenatal Care” Model
The April 2025 ACOG Clinical Consensus replaced the rigid one-size-fits-all schedule with a tailored plan. For an average-risk patient, that usually means 6 to 10 visits, mixing in-person and telehealth, with home blood-pressure monitoring between appointments.
Traditional Schedule vs. New Tailored Approach
Most US practices are still running a hybrid. You’ll see your OB roughly the same number of times, but some “check-in” visits are now virtual. The trimester structure below still holds for the majority of pregnancies, even under the new model.
Table 2: US Prenatal Care Schedule by Trimester
| Trimester | Weeks of Pregnancy | Visit Frequency | Core Tests & Screenings | Key Milestones |
| First | 4 to 13 | Intake + 1 to 2 visits | Blood type, Rh, CBC, HIV, hep B, syphilis, urine, dating ultrasound, NIPT (optional) | Confirm pregnancy, set due date |
| Second | 14 to 27 | Every 4 weeks | Quad screen or NIPT follow-up, anatomy ultrasound at 18 to 22 weeks, glucose tolerance test at 24 to 28 weeks | Anatomy scan, first kicks |
| Early Third | 28 to 35 | Every 2 weeks | Tdap vaccine at 27 to 36 weeks, maternal RSV vaccine, hemoglobin recheck, Rh immunoglobulin if Rh-negative | Vaccines, fetal growth check |
| Late Third | 36 to delivery | Every week | Group B strep swab at 36 to 37 weeks, cervical check (if indicated), non-stress tests if high risk | Labor prep, position check |
Sources: ACOG Prenatal Care FAQ, CDC Vaccines During Pregnancy, NICHD.
When Visits Become Weekly
Starting at 36 weeks, you’ll almost always shift to weekly visits. Your provider is watching fetal position, screening for preeclampsia, and checking whether the cervix is changing too early. This is also when most moms start discussing their birth plan in real detail, which I’d encourage you to take seriously. I’ve seen patients arrive in labor genuinely unsure what they’d agreed to; the prep conversation matters.
What Happens at Each Prenatal Visit?
The structure stays pretty consistent. What changes is what your provider is looking for.
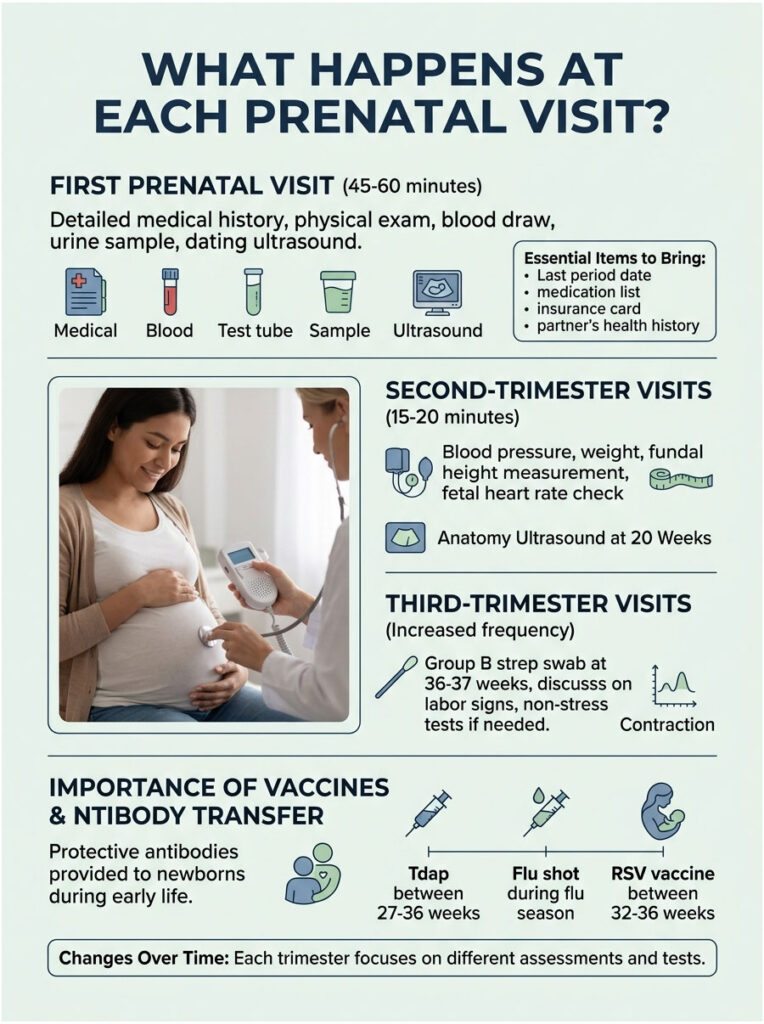
Your First Prenatal Visit, Step by Step
The intake visit runs 45 to 60 minutes. Expect a detailed medical and family history, a physical exam (including a pelvic exam and Pap if you’re due), a large blood draw, urine sample, and often a dating ultrasound.
Bring the first day of your last period, a list of every medication and supplement you take, your insurance card, and your partner’s health history if you can get it. That one medication list changes management more than any single test, in my experience. I’ve had patients casually mention a “harmless” supplement that turned out to be contraindicated in pregnancy, and we swapped it that day.
Second-Trimester Visits
These are shorter, often 15 to 20 minutes. Your provider checks blood pressure, weight, fundal height (the bump measurement), and fetal heart rate. The anatomy ultrasound around 20 weeks is the big one, scanning roughly 30 different fetal structures. Block out the morning; it takes time.
Third-Trimester Visits
Visits get more frequent and more targeted. Expect a Group B strep swab at 36 to 37 weeks, conversations about labor signs, and possibly non-stress tests if you have risk factors like advanced maternal age, high blood pressure, or diabetes.
Vaccines During Pregnancy (Tdap, RSV, Flu)
The CDC recommends Tdap between 27 and 36 weeks of every pregnancy, a flu shot during flu season at any gestational age, and the maternal RSV vaccine (Abrysvo) between 32 and 36 weeks if you’ll deliver during RSV season. These vaccines pass protective antibodies to your baby for the first months of life, which matters most before the baby’s own immune system is up and running.
Prenatal Tests by Trimester: The Full List

First-Trimester Screenings
- Blood type, Rh factor, CBC
- Hepatitis B, HIV, syphilis, rubella immunity
- Urinalysis and culture
- Pap smear if due
- Dating ultrasound
- Optional: NIPT (non-invasive prenatal testing), CVS, first-trimester combined screen
Second-Trimester Tests
- Quad screen (if NIPT wasn’t done)
- Anatomy ultrasound at 18 to 22 weeks
- Glucose challenge test at 24 to 28 weeks
- Optional: amniocentesis at 15 to 20 weeks
Third-Trimester Tests
- Group B streptococcus (GBS) swab at 36 to 37 weeks
- Hemoglobin recheck
- Antibody screen if Rh-negative
- Non-stress tests and biophysical profile for high-risk pregnancies
Genetic Testing: Screening vs. Diagnostic
NIPT, which analyzes fetal DNA fragments in mom’s blood, can be drawn as early as 10 weeks. It screens for Down syndrome, trisomy 18, trisomy 13, and sex chromosome issues with high accuracy. CVS (11 to 13 weeks) and amniocentesis (15 to 20 weeks) are diagnostic, not screening, and carry a small miscarriage risk. Your provider should walk you through which option makes sense for your age, family history, and earlier screening results. There’s no universally “right” answer here; it’s personal.
High-Risk Pregnancy: When You Need Extra Care
A pregnancy is labeled high-risk when something about you, the baby, or the pregnancy itself raises complication odds. Common triggers include age 35 or older, age under 17, BMI over 30, prior preterm birth, chronic hypertension, Type 1 or Type 2 diabetes, lupus, thyroid disease, or a multiple pregnancy (twins or more).

If you’re high-risk, your OB usually adds a maternal-fetal medicine (MFM) specialist to your team and schedules you more often, often every two weeks from 24 weeks on. Extra monitoring typically includes growth scans, Doppler studies, and non-stress tests.
The March of Dimes documented that in 2024, Black moms faced a maternal mortality rate of 44.8 per 100,000 live births versus 14.2 for white moms. American Indian and Alaska Native women faced rates of 60.8 per 100,000 during 2019 to 2021. These disparities are partly clinical and partly structural, which is why self-advocacy at every single appointment matters. I’ve seen patients save their own lives by insisting on a second opinion when something felt off, and I’ll say this plainly: trust your gut.
What Prenatal Care Costs in the US (and How to Afford It)
The biggest gap between top-ranking articles and what patients actually ask me is money. So here it is, in plain numbers.

Average Total Pregnancy Cost
Total pregnancy-related care in the US averages around $18,865, including prenatal visits, delivery, hospital stay, and postpartum follow-up. Insured parents pay roughly $2,655 to $3,214 out of pocket on average. The spread is wide: the same vaginal delivery that costs an insured family $8,000 in Arkansas can run $19,000 in California.
What the ACA Guarantees
Under the Affordable Care Act, all Marketplace and Medicaid plans must cover maternity and newborn care as one of ten essential health benefits, even if your pregnancy started before your coverage did. HealthCare.gov spells out the rules. Routine prenatal screenings and well-woman visits must be provided with no cost-sharing.
Medicaid, CHIP, and Presumptive Eligibility
Medicaid finances roughly 41% of all US births, per CMS data. Pregnant women with incomes at or below 138% of the federal poverty level must be covered in every state, and 47 states extend coverage that meets minimum essential coverage standards.
Presumptive eligibility is one of the most underused programs I’ve come across. It lets a qualified provider start your prenatal care the same day you apply, paid by Medicaid for up to 60 days while your full application processes. Call 1-800-311-BABY to reach your state’s program. Don’t wait on paperwork; start care now.
FQHCs and Sliding-Scale Options
Federally Qualified Health Centers operate in every US state and charge on a sliding scale based on income. Many offer prenatal care for $20 to $50 per visit for uninsured patients, which is roughly one-tenth of a private-practice cash rate. Community health centers are the only reason some of my patients got any care at all. Zero shame in using them; the quality is often excellent.
Nutrition, Lifestyle, and Safety

Prenatal Vitamins and Folic Acid
The FDA and NICHD recommend 400 to 800 mcg of folic acid daily, starting at least one month before conception if possible. Most US prenatal vitamins also contain iron, iodine, DHA, choline, and vitamin D at pregnancy-appropriate levels.
Don’t double up with a general multivitamin. Excess vitamin A (especially as retinol) can harm the fetus. One prenatal is enough for most moms.
Weight Gain Recommendations
Per Institute of Medicine guidelines that ACOG uses, underweight women (BMI under 18.5) should gain 28 to 40 lbs, normal-weight (BMI 18.5 to 24.9) should gain 25 to 35 lbs, overweight (BMI 25 to 29.9) should gain 15 to 25 lbs, and women with obesity (BMI 30+) should gain 11 to 20 lbs. These ranges assume a singleton pregnancy.
Foods, Medications, and Activities to Avoid
Skip raw fish (sushi, oysters), unpasteurized cheeses and juices, deli meats unless heated to steaming, high-mercury fish like swordfish and king mackerel, more than 200 mg of caffeine per day, and any alcohol at any stage. Always tell your provider about every prescription, over-the-counter drug, and herbal supplement you take.
Mental Health Screenings
ACOG now recommends screening for perinatal depression and anxiety at least once during pregnancy and once postpartum. Around 1 in 7 US women experiences perinatal depression. If your OB doesn’t screen you, bring it up yourself. It’s a normal, treatable part of modern prenatal care, and I’ve had patients tell me the mental-health conversation changed their whole pregnancy.
Red Flags You Should Never Ignore
Some symptoms mean a same-day call to your provider. Others mean skip the call and drive straight to the ER.

Table 3: Pregnancy Symptoms — Normal vs. Call OB vs. Go to ER
| Symptom | Probably Normal | Call Your OB-GYN Same Day | Go to the ER Now |
| Bleeding | Light spotting in early weeks after sex | Any bleeding past 12 weeks | Heavy bright-red bleeding, soaking a pad in an hour |
| Headache | Mild, relieved by rest and water | Persistent headache in third trimester | Severe headache with blurred vision, chest pain, or confusion |
| Swelling | Mild foot / ankle swelling late in pregnancy | New hand or face swelling | Sudden swelling with headache or right-upper-belly pain |
| Baby movement (after 28 weeks) | Quiet moments, usually hungry after eating | Less than 10 kicks in 2 hours after a kick count | No movement at all after cold water and an hour lying down |
| Contractions | Irregular Braxton-Hicks that stop with rest | Regular contractions before 37 weeks | Painful contractions every 5 minutes, water breaking, severe back pain |
Source: ACOG Urgent Maternal Warning Signs.
Choosing Your Prenatal Provider

OB-GYN vs. Certified Nurse-Midwife vs. Family Medicine
OB-GYNs handle every risk level including surgical deliveries. Certified nurse-midwives (CNMs) are advanced-practice nurses who manage average-risk pregnancies, often with lower cesarean rates and longer appointment slots. Family medicine doctors can manage average-risk pregnancies too, with the bonus of caring for your baby after birth.
Maternal-Fetal Medicine Specialists
MFM specialists are OB-GYNs with three extra years of high-risk training. If you have a chronic condition or a fetal anomaly is found, you’ll likely be co-managed by one.
Questions to Ask at Intake
Ask about the practice’s cesarean rate, how many providers you may see in labor, whether they offer VBAC (vaginal birth after cesarean), how after-hours calls work, and which hospital they deliver at. Also ask how they manage your specific condition if you have one. I’ve seen moms switch practices in the first trimester and be so much happier; the intake visit is the right time to decide if the fit is real.
Quick Checklist for Your First Prenatal Visit
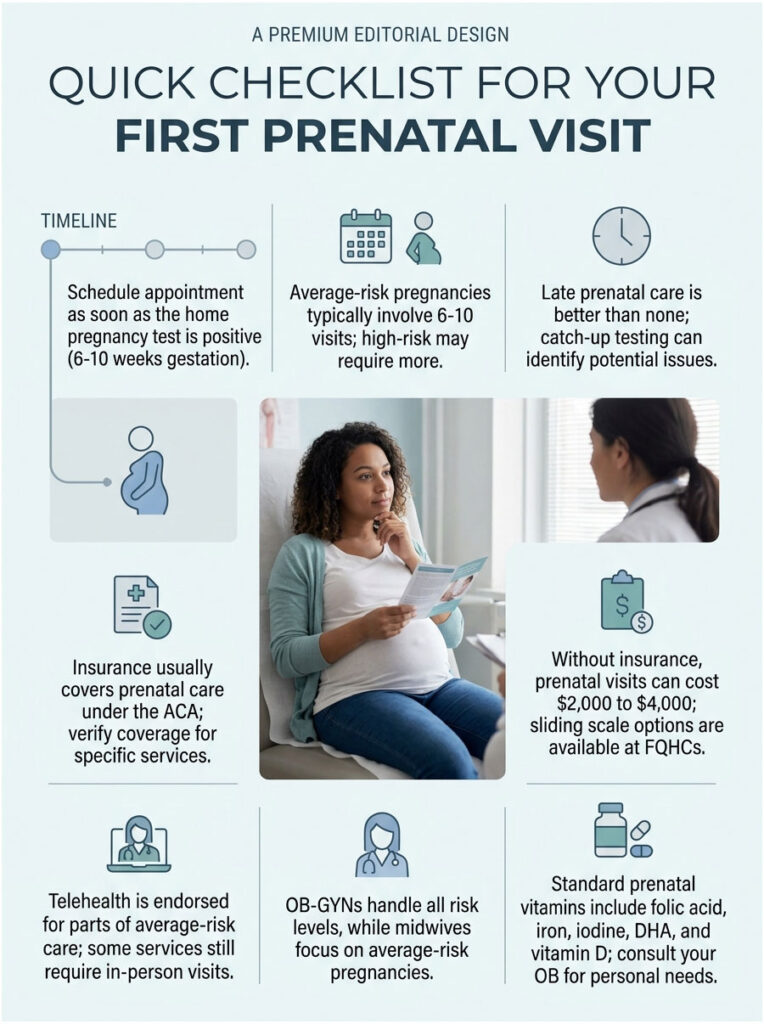
- First day of your last menstrual period
- A list of every medication, vitamin, supplement, and herbal remedy
- Personal medical history, including surgeries and chronic conditions
- Family history for both biological parents (diabetes, heart disease, genetic conditions)
- Insurance card and photo ID
- List of questions you want answered
- A partner or support person, if you want one there
- Comfortable clothing and a light snack
Frequently Asked Questions
When should I schedule my first prenatal appointment?
Call the day your home pregnancy test is positive. Most US practices aim for a first visit between 6 and 10 weeks of gestation (counted from the first day of your last period). Scheduling early helps you secure a spot with the OB or midwife you want, confirm dating, and start prenatal vitamins if you haven’t already.
How many prenatal visits will I have?
Average-risk US pregnancies now involve 6 to 10 visits under ACOG’s 2025 tailored-care model, though many practices still use the traditional 12 to 14. High-risk pregnancies usually add several visits, especially in the third trimester. The exact number depends on your health, the baby’s growth, and whether your provider offers telehealth between in-person appointments.
What if I start prenatal care late?
Late care, meaning no visits until the third trimester, is still much better than no care. Catch-up testing can still flag gestational diabetes, Group B strep, and growth restriction in time to act. If cost or access is the barrier, call 1-800-311-BABY for your state’s pregnancy-care hotline, or look up a nearby FQHC for same-week availability.
Does insurance always cover prenatal care?
Under the ACA, all Marketplace plans, employer plans, and Medicaid must cover maternity care as an essential health benefit. Routine prenatal screenings should have no cost-sharing. You may still owe deductibles and copays for delivery and some tests, so request an itemized estimate from your OB’s billing office early.
How much does prenatal care cost without insurance?
Cash prices at private OB practices run roughly $2,000 to $4,000 for prenatal visits alone, before delivery. FQHCs charge $20 to $80 per visit on a sliding scale. Medicaid (including presumptive eligibility) can bring the entire pregnancy cost to $0 out of pocket if you qualify. HealthCare.gov and 1-800-318-2596 are the fastest paths to check eligibility.
Can I do prenatal visits via telehealth?
Yes, and ACOG’s 2025 guidance formally endorses it for parts of average-risk care. Telehealth works well for mental-health check-ins, medication reviews, counseling, and some blood-pressure monitoring if you have a home cuff. Anatomy scans, Group B strep swabs, and physical exams still need in-person visits.
What’s the difference between an OB-GYN and a midwife?
OB-GYNs are surgically trained medical doctors who handle every risk level, including cesareans. Certified nurse-midwives are registered nurses with advanced training who manage average-risk pregnancies, typically in hospitals or birth centers. Many US patients see both, which is a legitimate collaborative model.
How many ultrasounds are standard in a US pregnancy?
Most average-risk US pregnancies include two ultrasounds: a dating scan around 8 to 12 weeks and an anatomy scan at 18 to 22 weeks. Additional scans are added for high-risk pregnancies, suspected growth issues, placenta previa, or multiples. Insurance usually covers medically indicated scans, but “keepsake” 3D/4D scans are rarely covered.
What vitamins should I take during pregnancy?
A standard prenatal with 400 to 800 mcg of folic acid, 27 mg of iron, 150 mcg of iodine, 200 to 300 mg of DHA, and 600 IU of vitamin D covers most needs. Your OB may add extra iron if you’re anemic, extra vitamin D if deficient, or magnesium for leg cramps. Stop any herbal supplement without checking first.
What’s the 28-week glucose test for?
The glucose challenge test screens for gestational diabetes, a pregnancy-onset form of diabetes that affects roughly 8% of US pregnancies. You drink a sweet 50-gram glucose drink and get blood drawn an hour later. If the result is high, a longer 3-hour confirmatory test is ordered. Catching gestational diabetes early protects both mom and baby from delivery complications.
Is prenatal yoga safe?
Prenatal yoga is one of the safest and most studied pregnancy exercises when taught by a certified prenatal instructor. Avoid hot yoga, deep twists, and positions flat on your back after 20 weeks. Clear any new exercise plan with your OB, especially if you have placenta previa, a history of preterm labor, or high blood pressure.
What if I miss a prenatal appointment?
Call your OB office the same day to reschedule. Missing one routine mid-pregnancy visit is rarely dangerous, but skipping a Group B strep swab, glucose test, or a weekly third-trimester visit can matter. Repeat no-shows can also affect your ability to deliver at some hospitals, so stay in touch with your team.
Medical Disclaimer: This article is for general educational purposes only and does not replace medical advice from a licensed clinician. Always discuss your specific health situation with your OB-GYN, midwife, or family-medicine provider before making decisions about prenatal care, testing, medications, or lifestyle changes.
References
• ACOG: Tailored Prenatal Care Delivery for Pregnant Individuals (2025 Clinical Consensus)
• CDC: Maternal Mortality Rates in the United States, 2024
• CDC: Vaccines During Pregnancy
• NICHD: Pre-pregnancy and Prenatal Care
• Office on Women’s Health: Prenatal Care
• March of Dimes: CDC Data on Maternal Mortality Rates in the US
• HealthCare.gov: Health Coverage Options for Pregnant Women