You wake up at 6 a.m., swing your legs over the bed, and the room tilts. Within seconds, you’re sprinting to the bathroom. Welcome to the first trimester, where roughly 7 out of 10 American women spend their mornings (and afternoons, and evenings) wondering if they’ll ever feel human again.
Table of Contents
Good news: morning sickness is treatable, the worst of it usually passes by week 14, and most remedies that work are sitting in your kitchen right now.
This guide walks through 17 of them, ranked by what OB-GYNs actually recommend in 2026.

Quick Answer: Morning sickness affects about 70% of US pregnant women, usually starting around week 6 and easing by week 14. The fastest relief: eat dry crackers before getting out of bed, sip ginger tea, and take 25 mg of vitamin B6 three times daily. For stubborn nausea, OB-GYNs add doxylamine (Unisom) at bedtime. Call your doctor if you can’t keep fluids down for 24 hours.
At a Glance
- Morning sickness peaks around week 9 and fades by week 14 for most women
- Vitamin B6 is the #1 ACOG-recommended first-line treatment
- Ginger (250 mg, 4x/day) has clinical evidence for reducing nausea
- Sea-Bands offer drug-free acupressure relief at any US pharmacy
- Hyperemesis gravidarum affects ~1.2% of US pregnancies and needs medical care
- Eating before getting out of bed prevents the worst morning waves
- 2024 Cambridge research links severity to a placental hormone called GDF15
What Is Morning Sickness, Really?
Let’s clear something up. “Morning” sickness is the worst-named condition in pregnancy.
For some women, the nausea hits at noon. For others, it’s a 9 p.m. wave that ruins dinner. For the unlucky, it’s all day, every day, for months.

The medical term is nausea and vomiting of pregnancy (NVP). It’s one of the most common pregnancy complications in the United States. A 2013 PubMed meta-analysis of 67,602 American women pegged the rate at 68.6%, which lines up with what most OB-GYNs see in practice.
In conversations I’ve had with new moms, the biggest shock isn’t the nausea itself. It’s how long it lasts. One mom told me she planned a baby announcement photoshoot for week 12, expecting to glow. She spent the morning vomiting in the photographer’s bathroom. She isn’t unusual.
Why “Morning” Is Misleading
The name comes from the fact that an empty stomach (overnight) often triggers the worst symptoms first thing. Once your hormones are surging, though, your stomach can revolt anytime: in traffic, at your desk, while brushing your teeth.
About 80% of women with NVP report nausea throughout the day, not just mornings. So if your symptoms hit at random hours, you’re typical.
When It Usually Starts and Ends
For most American women, the timeline looks like this:
Here’s the data side by side:
| Statistic | Value | Source |
| US women who experience NVP | ~70% | PubMed Meta-Analysis (67,602 women) |
| Women with severe form (HG) | 1.2% | NIH/PMC |
| Pregnancies with symptoms before week 9 | 89% | Cleveland Clinic |
| Women whose symptoms resolve by week 14 | ~70% | ACOG |
| Women with symptoms past week 22 | ~10% | March of Dimes |
| Annual US hospital admissions for HG | ~60,000 | American Pregnancy Association |
What the New GDF15 Research Means
Here’s something your mom probably didn’t know. In late 2023, researchers at the University of Cambridge identified a hormone called GDF15 as the likely main culprit behind pregnancy nausea.
The hormone is produced by the placenta and acts on the mother’s brain. Women who had naturally low GDF15 before pregnancy turn out to be more sensitive to the surge during pregnancy. That’s why severity varies so wildly from woman to woman.
This is real progress. Within a few years, we’ll likely see treatments targeting GDF15 directly. Until then, the playbook below is your best bet.
5 Diet Strategies That Stop Nausea Before It Starts
Most morning sickness battles are won (or lost) at the breakfast table. Or rather, before you even reach the breakfast table.

The Bedside Cracker Rule
Keep a sleeve of saltines on your nightstand. The moment you wake up, before sitting up, eat 2 or 3. Wait 15 minutes, then get out of bed slowly.
Why this works: empty stomach plus standing up plus low blood sugar equals nausea explosion. The crackers prime your stomach with bland carbs and absorb stomach acid before it churns.
I once spoke with a labor and delivery nurse who joked that this single trick saves more morning vomiting than anything else she recommends. It costs nothing and takes 30 seconds.
Small, Frequent Meals (The 2-Hour Rhythm)
Forget three big meals. Aim for 6 to 8 small ones, every 2 hours.
The goal: never let your stomach feel completely empty or completely full. Both extremes trigger nausea.
A “meal” can be a handful of almonds, half a banana, or a few cheese cubes. The constant trickle of food keeps blood sugar stable.
Protein at Bedtime Plus Complex Carbs
A small protein-rich snack right before bed (string cheese, hard-boiled egg, peanut butter on toast) keeps blood sugar steady through the night. That alone often takes the edge off morning waves.
Pair it with a complex carb like whole-grain toast or oatmeal. The combo slows digestion and prevents the dawn blood sugar dip.
Cold Food Advantage
Hot foods give off stronger smells. Smell is the #1 nausea trigger in pregnancy.
Cold sandwiches, salads, smoothies, yogurt, fruit, popsicles: all winners. Many women find they can stomach a cold turkey sandwich when grilled chicken makes them gag.
If cooking smells trigger you, ask your partner to handle dinner for a few weeks. Order in. Use the microwave. This isn’t laziness. It’s strategy.
Hydration the Smart Way
Sip fluids between meals, not with them. A full stomach of food plus liquid equals pressure plus nausea.
Try cold water with lemon, ginger ale, coconut water, or popsicles if drinking feels impossible. Aim for at least 64 ounces (eight 8-ounce glasses) per day.
Dehydration makes nausea dramatically worse. Track it on a water bottle if you have to.
7 Foods That Calm Pregnancy Nausea Fast
When the nausea hits, you need food that won’t make it worse. Here’s the lineup OB-GYNs and registered dietitians recommend most:

| Food | Form/Dose | Best Time | Evidence Strength |
| Ginger | 250 mg capsules, 4x/day OR 8 oz tea, 4x/day | Throughout day | Strong (multiple RCTs) |
| Saltines / plain crackers | 2-3 pieces | Before getting out of bed | Strong (clinical consensus) |
| Lemon (smell or taste) | Fresh slice or essential oil sniff | When nausea spikes | Moderate (aromatherapy) |
| BRAT foods (banana, rice, applesauce, toast) | Small portions | Anytime nausea hits | Strong (GI evidence) |
| Cold protein (string cheese, eggs, peanut butter) | 1 oz portions | Bedtime + every 2 hours | Strong (blood sugar) |
| Peppermint tea | 1 cup, 2-3x/day | After meals | Moderate |
| Watermelon and citrus | Small bowl | Anytime, especially mornings | Moderate (hydration) |
Ginger: The Workhorse Remedy
Ginger isn’t folk medicine. It’s been studied in dozens of randomized trials, and the evidence is solid.
The active compounds (gingerols and shogaols) appear to interrupt the brain-gut nausea signal. The OB-recommended dose is 250 mg, four times a day, taken as capsules.
If you prefer food forms, brewed ginger tea (one teaspoon fresh grated ginger steeped in 8 oz hot water, four times daily) works similarly. Ginger candies, real ginger ale, and crystallized ginger all count.
One caveat: ginger can thin blood slightly. If you’re on blood thinners or have a clotting disorder, talk to your OB first.
Lemon and Citrus
A 2014 study in the Iranian Red Crescent Medical Journal found that pregnant women who sniffed lemon essential oil reported significantly less nausea than the placebo group.
You don’t need fancy oils. A fresh lemon, sliced and held under your nose, works just as well.
Some women keep a small jar of lemon zest in their purse. When nausea strikes in public, a quick sniff can buy you 20 minutes of relief.
BRAT Diet Basics
Banana, Rice, Applesauce, Toast.
These bland, low-fiber foods have been a stomach-upset standby for decades, and they work in pregnancy too. When everything else seems impossible, BRAT foods almost always go down.
Foods to Avoid Completely
Some foods reliably make morning sickness worse. Skip these during your worst weeks:
- Spicy foods (curry, hot sauce, chili)
- Greasy or fried foods (fast food, fried chicken, doughnuts)
- Strong-smelling foods (fish, onions, garlic-heavy dishes)
- Very sweet foods (candy, ice cream, soda)
- Coffee (the smell alone is a trigger)
- Anything with artificial sweeteners
Vitamin B6 + Doxylamine: The OB-Approved Combo
If diet changes aren’t cutting it, this is what your OB will reach for next.
ACOG lists vitamin B6 as the first-line pharmacological treatment for NVP. The evidence is strong.
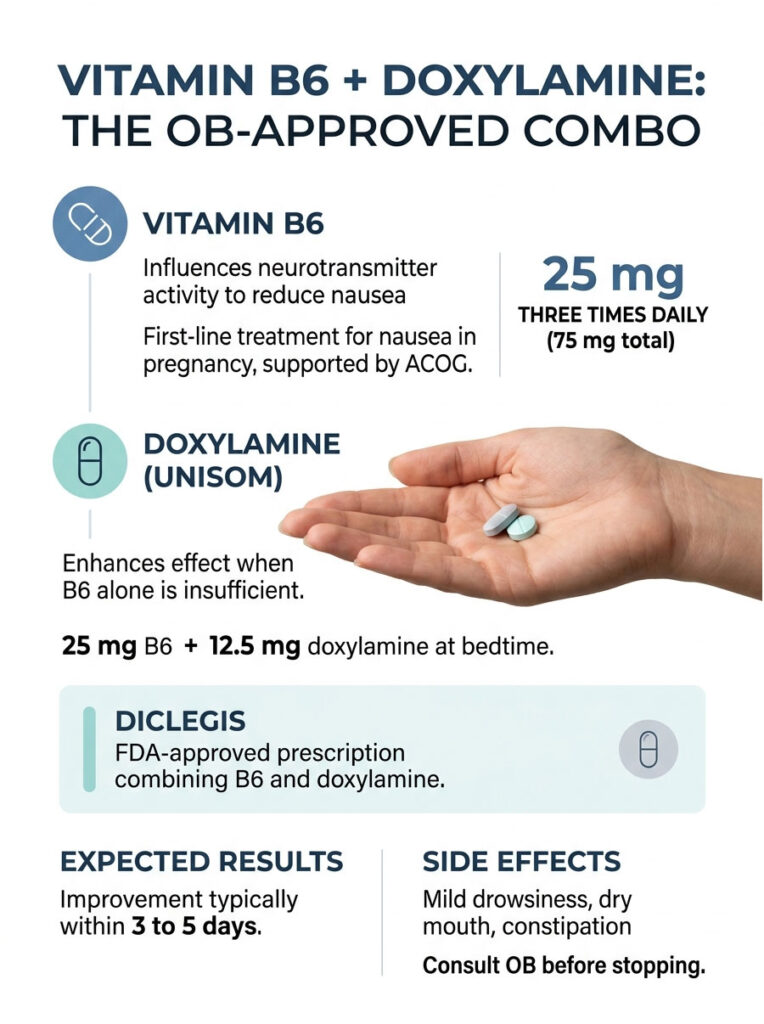
How Vitamin B6 Works (The 25 mg Sweet Spot)
Vitamin B6 (pyridoxine) reduces nausea by influencing neurotransmitter activity in the brain’s vomiting center. A landmark 1995 randomized trial of 342 women showed 30 mg daily significantly reduced nausea scores compared to placebo.
The standard OB recommendation today: 25 mg of vitamin B6, three times daily (75 mg total per day).
It’s available over the counter at any US pharmacy: CVS, Walgreens, Target, Walmart. Look for “Pyridoxine HCl 25 mg.” Don’t exceed 100 mg per day without your doctor’s okay. Mega-doses can cause nerve issues over time.
Adding Unisom (Doxylamine) for Stronger Cases
If B6 alone isn’t enough, ACOG recommends adding doxylamine (the active ingredient in Unisom SleepTabs).
The combo of 25 mg B6 + 12.5 mg doxylamine at bedtime works for the majority of women whose nausea isn’t responding to lifestyle changes alone.
Important: use Unisom SleepTabs (the round blue pills), not Unisom SleepGels or SleepMelts. Only the SleepTabs contain doxylamine.
Doxylamine causes drowsiness, which is why bedtime dosing makes sense. You sleep through the side effect and wake up with less nausea.
Diclegis: The Only FDA-Approved Prescription
If you’d rather not piece together OTC supplements, ask your OB about Diclegis.
It’s the only prescription medication specifically FDA-approved for nausea and vomiting of pregnancy in the US. It’s essentially the same B6 + doxylamine combo, but in a delayed-release tablet that times itself to your symptoms.
The catch: it’s expensive without insurance ($500+ per month in some markets). Many insurance plans cover it. Call your provider ahead of time.
What to Expect and Side Effects
Don’t expect overnight miracles. Most women see meaningful improvement within 3 to 5 days.
Side effects (when they happen) are usually mild: drowsiness, dry mouth, mild constipation. None of these should make you stop taking it without talking to your OB first.
Lifestyle Hacks That Make a Real Difference
Beyond food and supplements, small daily changes add up. These cost little and have real evidence behind them.

Sea-Bands and Acupressure
Sea-Bands are stretchy wristbands with a small plastic stud that presses on the P6 acupressure point on the inside of your wrist.
They’re sold at most US pharmacies (CVS, Walgreens, Target) for about $10 to $15. Used for motion sickness for decades, several studies show modest benefit for pregnancy nausea too.
The evidence isn’t as strong as for ginger or B6. But they’re cheap, safe, and drug-free. Many women find them especially helpful for situational nausea (car rides, work meetings, grocery shopping).
Avoiding Trigger Smells
Make a list of every smell that triggers your nausea, then aggressively avoid them. Common offenders: coffee, cooked meat, perfume, scented candles, garbage, gasoline, cigarette smoke, certain laundry detergents.
Practical moves: switch to unscented soap and laundry detergent, take out the trash twice a day, ask your partner to brush their teeth before kissing you, and decline invitations to restaurants serving heavy-smelling food.
Sleep, Stress, and the Nausea Link
Exhaustion makes nausea worse. Stress makes it worse.
Skipping rest because you “have too much to do” is a losing strategy in the first trimester. Aim for 8 to 10 hours of sleep per night. Take naps when possible.
Say no to non-essential commitments. This isn’t being lazy. It’s giving your body what it needs to handle a hormonal upheaval.
Brushing Your Teeth Without Gagging
Toothpaste flavor is a sneaky trigger. If your usual minty paste makes you gag, switch to a kid’s toothpaste (mild fruit flavors) or a baking soda paste.
Use a smaller toothbrush head. Brush gently and slowly. If brushing still triggers vomiting, rinse with mouthwash and brush later in the day when nausea has eased.
When to Call Your OB-GYN (Don’t Wait Too Long)
Most morning sickness is uncomfortable but not dangerous. Some symptoms cross the line from “miserable” to “medically serious.”

Here’s when to pick up the phone:
| Scenario | Recommended Action | Urgency |
| Mild nausea, occasional vomiting, can keep fluids down | Try diet/lifestyle remedies + B6 | Routine |
| Persistent nausea despite B6 for 3+ days | Call OB to discuss adding doxylamine | Within 1 week |
| Vomiting more than 3 times per day | Schedule OB appointment | Within 48 hours |
| Can’t keep fluids down for 24 hours | Call OB same day | Same day |
| Weight loss of 5%+ from pre-pregnancy weight | Go to OB or urgent care | Same day |
| Signs of dehydration (dark urine, dizziness) | Go to ER or urgent care | Immediate |
| Vomiting blood or severe abdominal pain | Go to ER | Immediate |
Warning Signs of Dehydration
Dehydration is the most common reason morning sickness becomes a medical emergency. Watch for:
- Dark yellow or amber-colored urine
- Urinating less than every 8 hours
- Dizziness when standing up
- Racing heart or pounding pulse
- Dry mouth and cracked lips
- Extreme fatigue or confusion
If you check 2 or more boxes, call your OB or head to urgent care for IV fluids. This is common and easily treated.
Hyperemesis Gravidarum Red Flags
About 1.2% of US pregnancies progress to hyperemesis gravidarum (HG), the severe form of NVP. HG is the second most common reason for first-trimester hospitalization in the US.
You may have HG if you have:
- Vomiting more than 3 to 4 times per day
- Inability to keep food or fluids down
- Weight loss of 5% or more
- Ketones in your urine (your OB will test for this)
- Symptoms that don’t respond to standard treatment
HG isn’t something to tough out. Treatment ranges from prescription antiemetics (like Zofran or Reglan) to IV fluids and, in severe cases, a brief hospital stay. With proper care, most women with HG go on to have healthy pregnancies and babies.
I once heard from a young mom from Texas who lost 14 pounds in her first trimester before her OB diagnosed HG. After three days of IV fluids and Zofran, she gained back 6 pounds in a week. She wished she’d called her doctor a month earlier.
What Treatment Looks Like at the Clinic
If you end up in the OB office or ER for severe nausea, expect:
- A urine test for ketones and dehydration markers
- Bloodwork to check electrolytes
- Possibly an IV bag of fluids and anti-nausea medication
- A prescription for stronger antiemetics if needed
Most women feel dramatically better within a few hours of IV treatment. Don’t feel embarrassed to seek help. This is what your OB is there for.
A Quick Note for Partners and Family
If you’re the partner reading this: your support matters more than you know.
Morning sickness can be physically and emotionally exhausting. Many women feel guilty for “complaining” or being unable to function normally.

Practical Ways to Help
- Keep crackers stocked on her nightstand
- Take over cooking (especially anything with strong smells)
- Handle the grocery shopping (she may not tolerate the produce aisle)
- Drive her to OB appointments
- Take on extra household chores without being asked
- Pick up her prenatal vitamins and B6 from the pharmacy
What NOT to Say
Avoid these phrases at all costs:
- “It’s just morning sickness, it’ll pass”
- “My friend’s wife wasn’t this sick”
- “Have you tried [random remedy]?”
- “Are you sure you’re eating enough?”
Instead, try: “What sounds good right now?” or “What can I do to help?” or simply, “I’m sorry you feel awful.”
Frequently Asked Questions
When does morning sickness usually start and end?
Morning sickness typically starts between weeks 4 and 6 of pregnancy, peaks around weeks 8 to 10, and resolves for about 70% of women by week 14. Roughly 10% of women experience symptoms throughout the entire pregnancy, though usually milder after the first trimester.
Is morning sickness a sign of a healthy pregnancy?
Some research suggests women with morning sickness may have a slightly lower risk of miscarriage, possibly because nausea correlates with strong placental hormone production. However, not having morning sickness is also completely normal and doesn’t mean anything is wrong. Both groups have healthy babies at similar rates.
How much vitamin B6 is safe during pregnancy?
ACOG recommends 25 mg of vitamin B6 (pyridoxine) three times daily, totaling 75 mg per day, for nausea relief. This dose is well within the safe range during pregnancy. Don’t exceed 100 mg daily without your OB’s approval, as very high doses can cause nerve damage over time.
Can ginger really stop pregnancy nausea?
Yes. Ginger has solid clinical evidence for reducing pregnancy nausea. Multiple randomized trials show 250 mg capsules taken four times daily significantly reduce nausea symptoms. Ginger tea, candies, and crystallized ginger work similarly. Avoid ginger if you’re on blood thinners.
What does morning sickness at night mean?
Despite the name, “morning” sickness can hit anytime, including evening. Nighttime nausea often happens because of low blood sugar after a long stretch without eating. A small bedtime snack with protein and complex carbs (like cheese and crackers) often prevents nighttime waves.
Is it normal to throw up every day in early pregnancy?
Vomiting once or twice daily during the first trimester is common and usually not concerning. However, vomiting more than 3 times daily, inability to keep fluids down, or weight loss are signs you need medical evaluation. Don’t try to tough it out.
What foods make morning sickness worse?
Common triggers include spicy foods, fried/greasy foods, strong-smelling foods (fish, onions), very sweet foods, coffee, and foods with artificial sweeteners. Hot foods are usually worse than cold ones because of stronger smells. Each woman’s triggers are different, so track yours.
Can prenatal vitamins cause nausea?
Yes. The iron in prenatal vitamins is a frequent nausea trigger. Try taking your prenatal at bedtime with a snack instead of in the morning. If that doesn’t help, ask your OB about switching to a gentler formula or splitting the dose. Don’t skip prenatals entirely without medical guidance.
When should I worry about dehydration?
Call your OB the same day if you can’t keep fluids down for 24 hours, your urine is dark amber, you’re dizzy when standing, or your heart races. Severe dehydration in pregnancy can lead to electrolyte imbalances and may require IV fluids at the clinic or ER.
Does morning sickness mean I’m having a girl?
This is a popular myth with limited evidence. Some studies have found a slight association between severe nausea and female babies (possibly due to higher hCG levels), but the difference is small and unreliable as a gender predictor. Wait for the ultrasound or NIPT for accuracy.
Can morning sickness hurt the baby?
Mild to moderate morning sickness has no harmful effect on the baby. Even with significant vomiting, your baby gets nutrients from your body’s reserves. The exception is severe hyperemesis gravidarum with significant weight loss, which can affect birth weight if untreated. Early treatment matters.
What’s the difference between morning sickness and hyperemesis gravidarum?
Regular morning sickness is uncomfortable but lets you keep some food and fluids down. Hyperemesis gravidarum (HG) is severe: vomiting more than 3 to 4 times daily, weight loss of 5% or more, dehydration, and ketones in the urine. HG affects about 1.2% of US pregnancies and requires medical treatment, sometimes hospitalization.
Disclaimer: This article is for educational purposes only and is not a substitute for professional medical advice. Always consult your obstetrician or healthcare provider before starting any new supplements, medications, or treatments during pregnancy. If you experience severe symptoms or signs of dehydration, seek medical care immediately.
References
- American College of Obstetricians and Gynecologists (ACOG): Morning Sickness FAQ
- Cleveland Clinic: Morning Sickness Overview
- Mayo Clinic: Morning Sickness Diagnosis and Treatment
- PubMed: Prevalence of NVP in the USA Meta-Analysis
- NIH/PMC: Optimal Management of Nausea and Vomiting of Pregnancy
- March of Dimes: Morning Sickness Resource
- American Pregnancy Association: Morning Sickness Remedies
- University of Cambridge: GDF15 Pregnancy Sickness Research
- NIH/PMC: Emerging Progress in NVP and Hyperemesis Gravidarum