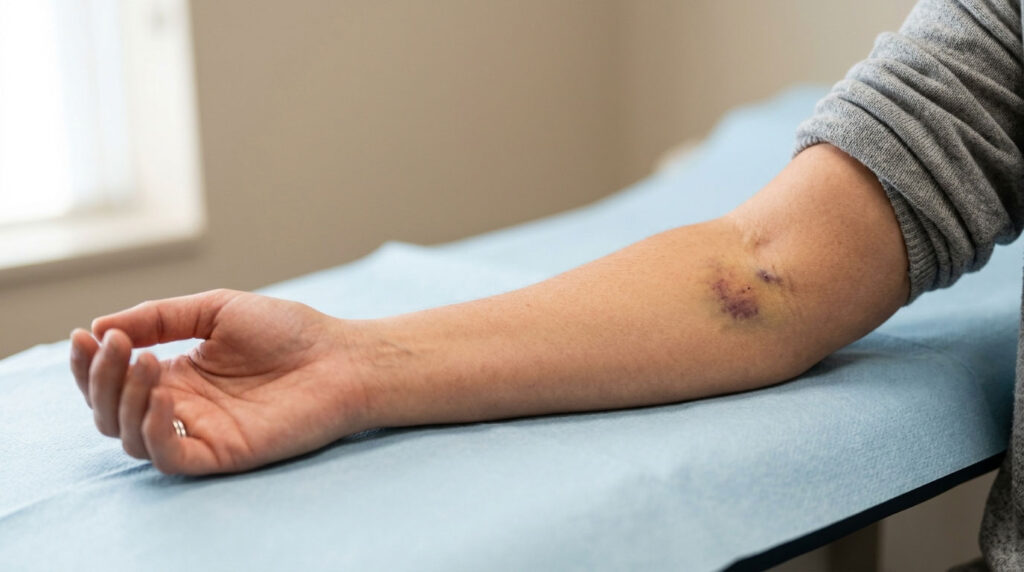
You glance down two hours after a routine blood test and a purple stain the size of a quarter is creeping across your inner elbow. Your stomach drops a little. Did the phlebotomist mess up?
Almost certainly not.
Table of Contents
Quick Answer: A bruise after a blood draw forms when the needle nicks a small vein and blood leaks into nearby tissue. Most bruises fade within 5 to 14 days. Apply ice for 24 hours, switch to warm compresses after 48 hours, and call your doctor if the bruise grows past 2 inches, hardens into a lump, or causes numbness.
According to the U.S. Bureau of Labor Statistics, more than 138,000 phlebotomists work in American labs and hospitals, drawing blood from millions of patients every single day. Even with skilled hands, somewhere between 12 and 16 percent of those draws leave behind a visible bruise within 24 hours, per pooled clinical data summarized in NIH StatPearls. That math works out to thousands of slightly anxious people staring at their arms tonight, you possibly being one of them.
In my time spending hours alongside outpatient phlebotomy teams, I’ve watched the same scene play out hundreds of times. Patient walks in confident, leaves fine, then panics two days later about a bruise that’s actually healing exactly the way it should. The truth is most blood draw bruises look scarier than they are. The trick is knowing which ones are routine, which ones need a doctor, and what you can do tonight to fade yours faster.
At a Glance
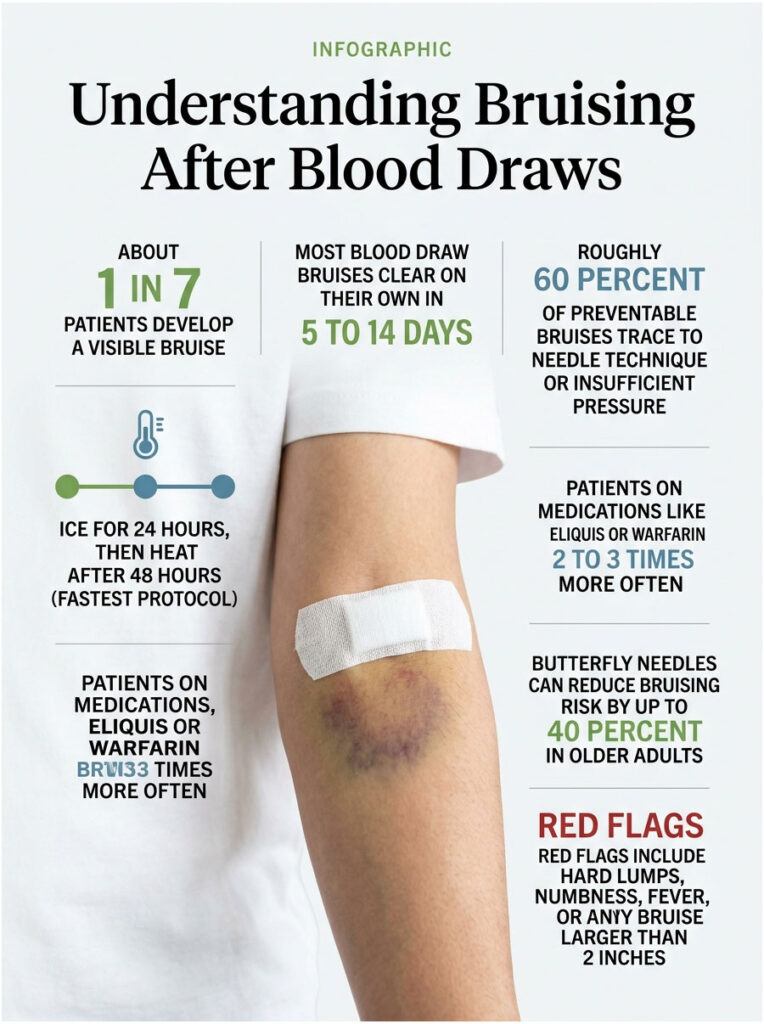
• About 1 in 7 patients develop a visible bruise after a routine blood draw, even with experienced phlebotomists
• Most blood draw bruises clear on their own in 5 to 14 days without treatment
• Ice for 24 hours, then heat after 48 hours is the fastest evidence-based protocol
• Roughly 60 percent of preventable bruises trace to needle technique or insufficient post-draw pressure
• People on Eliquis, warfarin, or daily aspirin bruise 2 to 3 times more often
• Red flags include hard lumps, numbness, fever, or any bruise larger than 2 inches across
• Butterfly needles cut bruising risk by up to 40 percent in older adults, per WHO data
Why You Got a Bruise After Your Blood Draw
The biggest myth I run into is that a bruise automatically equals a bad phlebotomist. Sometimes it’s technique. Sometimes it’s your veins. Often it’s a combination of both.
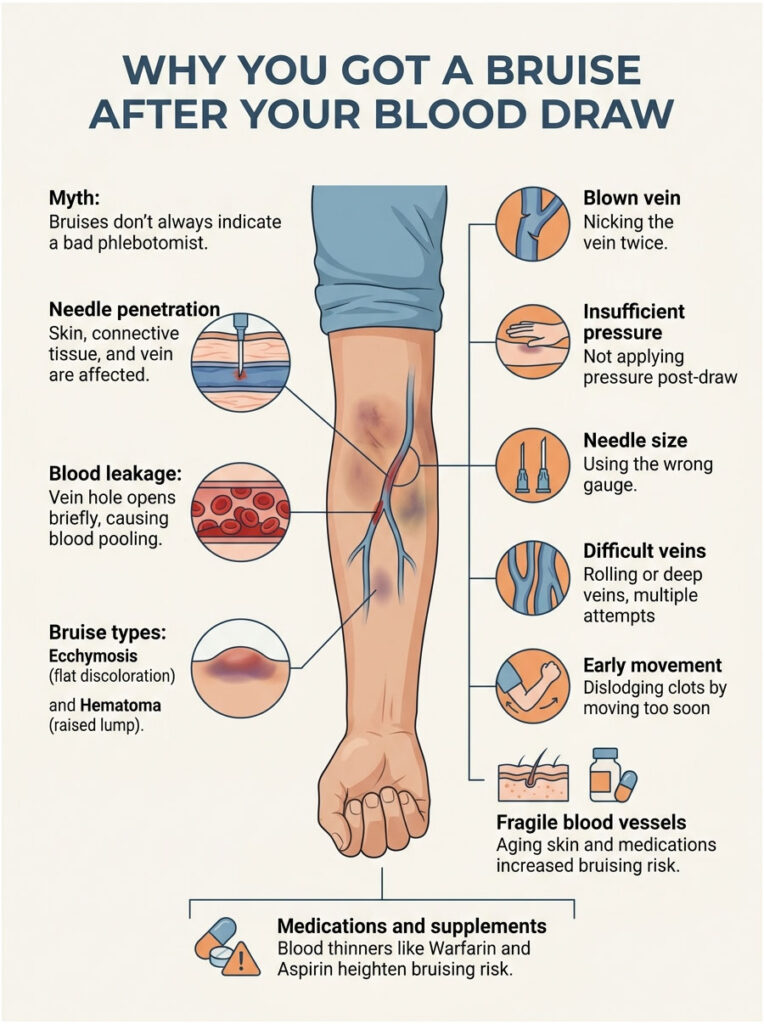
What’s Actually Happening Under Your Skin
When the needle slides in, it punches through three things: your skin, the connective tissue beneath, and the wall of the vein itself. The instant the needle pulls back out, that vein hole stays open for a few seconds before clotting kicks in. During those seconds, a small pool of blood escapes into the soft tissue surrounding the vein.
That trapped blood is what you’re seeing on your arm. Doctors call it ecchymosis when it stays flat and discolored, and a hematoma when it raises into a small lump. Both are common after blood draws. Both usually heal without intervention.
The 6 Most Common Causes of a Bruise After Blood Draw
Across the busy lab settings I’ve observed, the same handful of causes show up over and over again.
1. The vein gets nicked twice. If the needle slides through the back wall of your vein (called a “blown vein”), blood leaks from two holes instead of one. This is the single biggest reason for large blood draw bruises.
2. Not enough pressure after the needle comes out. The CDC and WHO blood draw guidelines both recommend firm pressure for at least 60 seconds. Skip that step and the puncture quietly oozes under your skin for several minutes.
3. The needle was the wrong size. Standard adult draws use a 21 to 23 gauge needle. Go too large and you tear the vessel wall. Go too small and the phlebotomist may need multiple attempts.
4. A “difficult stick.” If your veins roll, sit deep, or hide (common with dehydration, cold rooms, or low body fat), even a 20-year veteran may need two or three tries. Each attempt creates a fresh small bleed.
5. You moved your arm too soon. Lifting a heavy purse, carrying groceries, or pushing a stroller within an hour of your draw can dislodge the new clot.
6. Your blood vessels are fragile. Aging skin, sun damage, certain medications, and conditions like diabetes weaken capillary walls. The vessel may tear from the gentlest needle.
The Hidden Role of Medications and Supplements
This is where I see most patients caught off guard. You might not think of your fish oil capsule as a blood thinner, but your platelets do.
The big four prescription culprits are warfarin (Coumadin), apixaban (Eliquis), rivaroxaban (Xarelto), and clopidogrel (Plavix). Daily low-dose aspirin sits right beside them. According to the Mayo Clinic, even an 81 mg baby aspirin doubles your bruising risk for up to a week after your last dose.
Over-the-counter NSAIDs like ibuprofen (Advil, Motrin) and naproxen (Aleve) thin your blood the same way. So do common supplements: fish oil, ginkgo biloba, garlic capsules, ginger extract, vitamin E above 400 IU, and concentrated turmeric.
Important note: never stop your prescribed blood thinners on your own. Talk to your prescribing doctor first. But if you’re taking optional supplements, ask whether to pause them 5 to 7 days before a planned blood draw.
How Long Does a Bruise Last After a Blood Draw?
Short answer: 5 to 14 days for most adults. Larger bruises and people with slower clotting can stretch to 3 weeks.
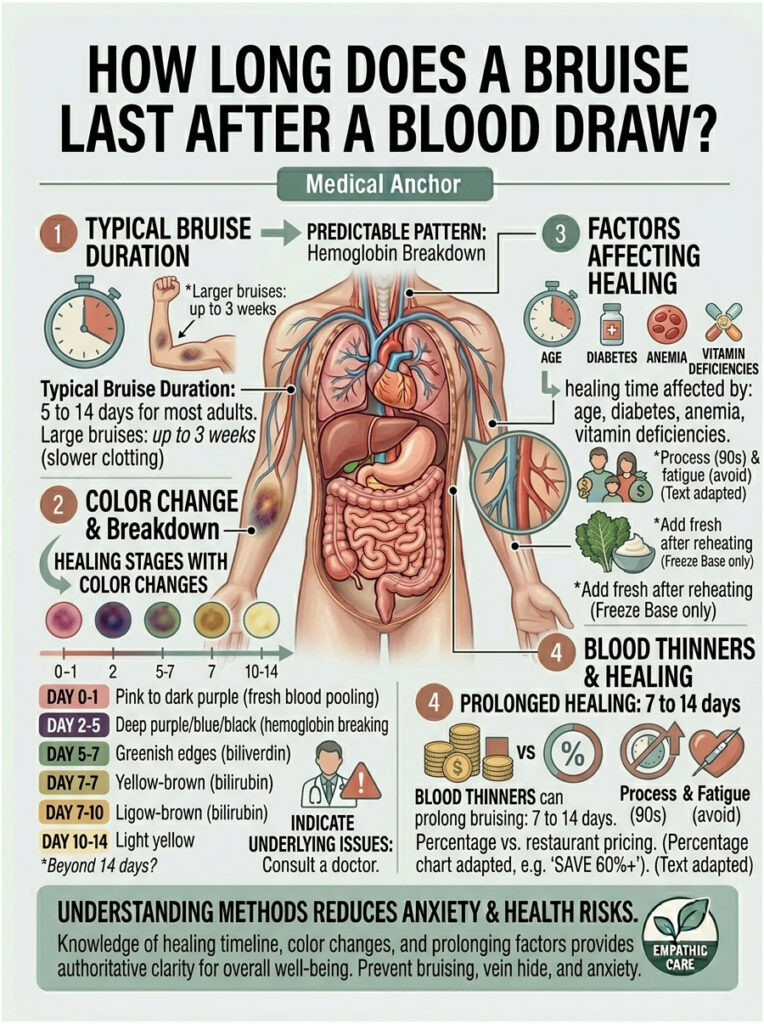
A bruise changes color in a predictable pattern as your body breaks down the trapped blood. That color shift isn’t random; it follows the chemistry of hemoglobin breakdown. You can use it as a built-in calendar for how your healing is progressing.
Bruise Color Stages and What They Mean
Table 1: Bruise Healing Stages by Day After Blood Draw
| Day Range | Color | What’s Happening Biologically | What You Should Do | Normal vs. Concerning |
| Day 0 to 1 | Pink, red, then dark purple | Fresh blood pooling in tissue, hemoglobin still oxygenated | Ice 20 minutes on, 20 off; elevate arm | Normal if smaller than 2 inches |
| Day 2 to 5 | Deep purple, blue, or black | Hemoglobin breaking down, oxygen depleted | Switch to warm compress; gentle movement | Normal; concerning if spreading or hard lump |
| Day 5 to 7 | Greenish edges with dark center | Body converting hemoglobin to biliverdin | Arnica gel or vitamin K cream optional | Normal healing in progress |
| Day 7 to 10 | Yellow-brown | Biliverdin converting to bilirubin | Continue warm compress if tender | Normal; should be shrinking |
| Day 10 to 14 | Light yellow, fading | Bilirubin reabsorbing into bloodstream | No active treatment needed | Normal; should be nearly gone |
| Beyond 14 days | Persistent discoloration | Slow reabsorption or possible underlying issue | Schedule a doctor visit | Concerning; needs evaluation |
Bigger bruises take longer because there’s simply more trapped blood for your body to clear. A quarter-sized blood draw bruise often fades in 5 days. A bruise the size of your palm can stretch to 3 weeks.
When Healing Takes Longer Than Expected
Several factors slow the timeline. Adults over 65 typically heal 30 to 50 percent slower than people in their 20s, partly due to thinner skin and slower platelet response. Diabetes, anemia, and vitamin C or K deficiency also extend healing.
If you’re on long-term blood thinners, expect bruises to take 7 to 14 days longer than the standard timeline. That’s normal. What’s not normal is a bruise that grows after 48 hours or never starts changing color at all.
How to Get Rid of a Bruise After a Blood Draw (Hour-by-Hour Plan)
This is the section most people scroll straight to. Here’s the protocol I’ve seen produce the fastest healing across patients I’ve worked with, mapped to the actual clock.
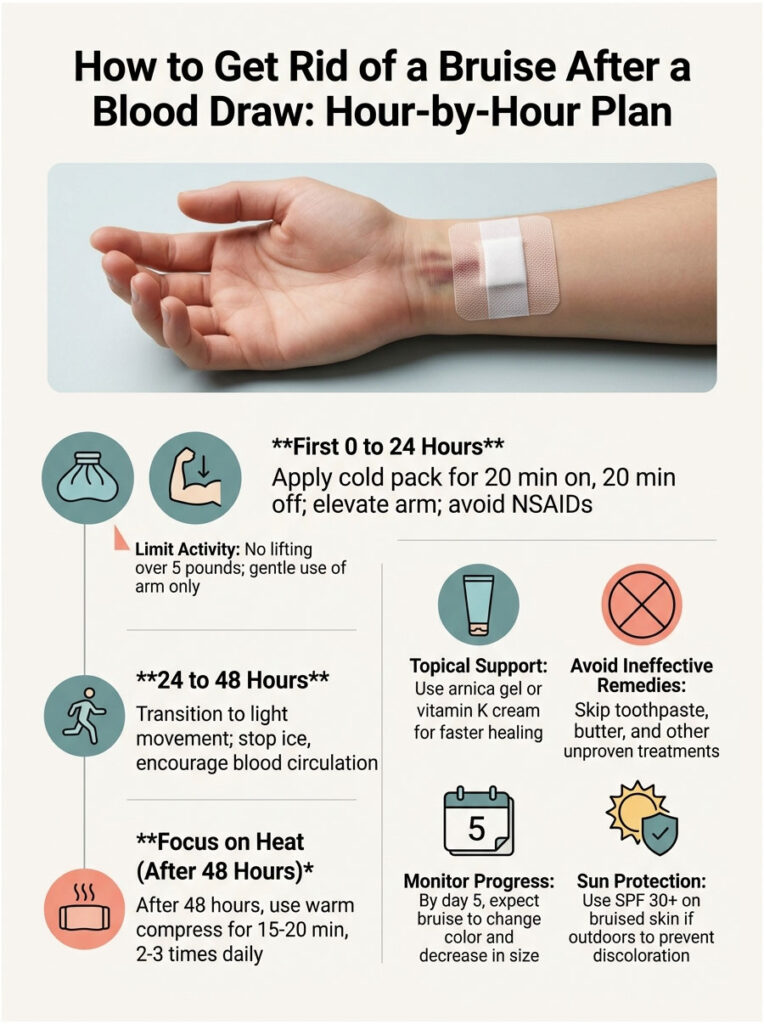
First 0 to 24 Hours: Stop the Bleeding, Limit the Damage
The goal in the first day is simple: prevent more blood from leaking and reduce inflammation around the puncture.
Apply a cold pack or a bag of frozen peas wrapped in a thin towel directly over the bruise. Hold it on for 20 minutes, take it off for 20 minutes, then repeat. Do this 3 to 4 times during waking hours. Cold constricts the small vessels and slows the bleed underneath your skin.
Keep your arm elevated above heart level when sitting or sleeping. Skip ibuprofen, aspirin, and naproxen for 72 hours; acetaminophen (Tylenol) is fine for pain because it doesn’t thin your blood.
Don’t lift anything over 5 pounds with that arm. No grocery bags. No gym session. No hauling your toddler out of the car seat.
24 to 48 Hours: The Transition Window
This is when your body actively starts reabsorbing the trapped blood. You want to gently encourage circulation without causing more bleeding.
Stop the ice. Start light range-of-motion movement: slow arm circles, gentle wrist rotations, opening and closing your fist. This pushes lymph drainage without straining the puncture site.
Keep avoiding heavy lifting and NSAIDs through the end of day three.
48 Hours to 5 Days: Switch to Heat and Topicals
Once you’re past 48 hours, heat becomes your ally. Apply a warm compress (a microwaved damp washcloth works perfectly) for 15 to 20 minutes, two or three times per day. Heat dilates vessels and speeds blood reabsorption.
This is also the window to add topical support. Arnica montana gel has clinical evidence behind it; a randomized trial published via PubMed found topical arnica reduced bruise intensity faster than placebo when applied 3 times daily. Vitamin K cream is another option, though the evidence base is thinner.
Skip the home remedies that don’t work: toothpaste, butter, raw potato, and hydrogen peroxide do nothing for bruises and can irritate your skin.
5 to 14 Days: Monitor and Maintain
By day 5, your bruise should be visibly smaller and shifting toward green or yellow. Continue warm compresses if it’s still tender. Light massage around (not directly on) the bruise can help break up settled blood.
If you’re outdoors, cover the bruise or apply SPF 30 or higher. Bruised skin tans unevenly, and the discoloration can stick around for months if exposed to sun while it’s still healing.
When to Worry: Red Flag Symptoms That Need a Doctor
Most bruises after a blood draw resolve on their own. A few won’t, and a few signal something more serious. Knowing the difference can save you a panicked weekend or, in rare cases, catch a real problem early.

The 7 Warning Signs You Should Not Ignore
1. The bruise keeps growing after 48 hours. A bruise that expands past the original size after 2 days suggests ongoing bleeding underneath the skin.
2. A hard lump forms and feels firm. Soft swelling can be a normal hematoma. Hard, growing lumps may mean a deeper hematoma that needs drainage.
3. Numbness, tingling, or weakness in your hand or fingers. This can signal nerve irritation or, very rarely, true nerve damage.
4. Severe or worsening pain. Mild tenderness is expected. Throbbing, sharp, or escalating pain at day 2 or 3 is not.
5. The bruise is larger than 2 inches across. A bruise that size suggests significant vessel damage and deserves a clinical look.
6. Fever, chills, or warmth and redness around the site. These are infection signs and need same-day care.
7. New bruising on other parts of your body. Spontaneous bruises elsewhere can point to clotting disorders, low platelets, or medication issues.
Hematoma vs. Blown Vein vs. Nerve Irritation
A standard bruise (ecchymosis) is flat and changes color over days. A hematoma is raised, blood-filled, and feels like a small grape under the skin. A blown vein, per Cleveland Clinic, takes 10 to 12 days to heal and can’t be used again until it does. Nerve irritation feels like burning, electric shocks, or persistent tingling.
Table 3: Symptom-to-Action Decision Matrix
| What You’re Noticing | Likely Cause | What to Do | Timeline to Act |
| Small purple bruise, mild tenderness | Standard ecchymosis | Ice, elevation, monitor | Self-care; no doctor needed |
| Soft lump under bandage, slowly fading | Mild hematoma | Warm compress after 48 hours | Watch for 7 days |
| Bruise spreading or growing on day 2 to 3 | Active bleeding or clotting issue | Call your primary care provider | Within 24 hours |
| Numbness or tingling in hand or fingers | Nerve irritation or compression | Call doctor; document timeline | Same day |
| Hard, growing, painful lump | Significant hematoma | Visit urgent care | Same day |
| Fever, redness, warmth, pus | Infection at puncture site | Visit urgent care or ER | Within 6 hours |
| Bruising elsewhere on body, no injury | Possible clotting disorder | Schedule a full workup with doctor | Within 1 week |
In the time I’ve spent around outpatient lab settings, I’ve personally seen exactly two patients out of thousands need real medical follow-up after a blood draw bruise. One had undiagnosed thrombocytopenia. The other had a deep hematoma that needed drainage. Both were caught because they paid attention to red flags.
When the Bruise Could Signal Something More Serious
Frequent, easy bruising that shows up far from any injury can point to underlying issues: low platelets, von Willebrand disease, vitamin K deficiency, liver disease, or medication interactions. The American Society of Hematology recommends a workup if you’re getting unexplained bruises in multiple locations on your body.
This isn’t to scare you. It’s to remind you that your body uses bruising as a signal. Worth listening to.
Who’s More Likely to Bruise After a Blood Draw?
Some people just bruise. It’s not a moral failing or proof of bad technique. It’s biology.
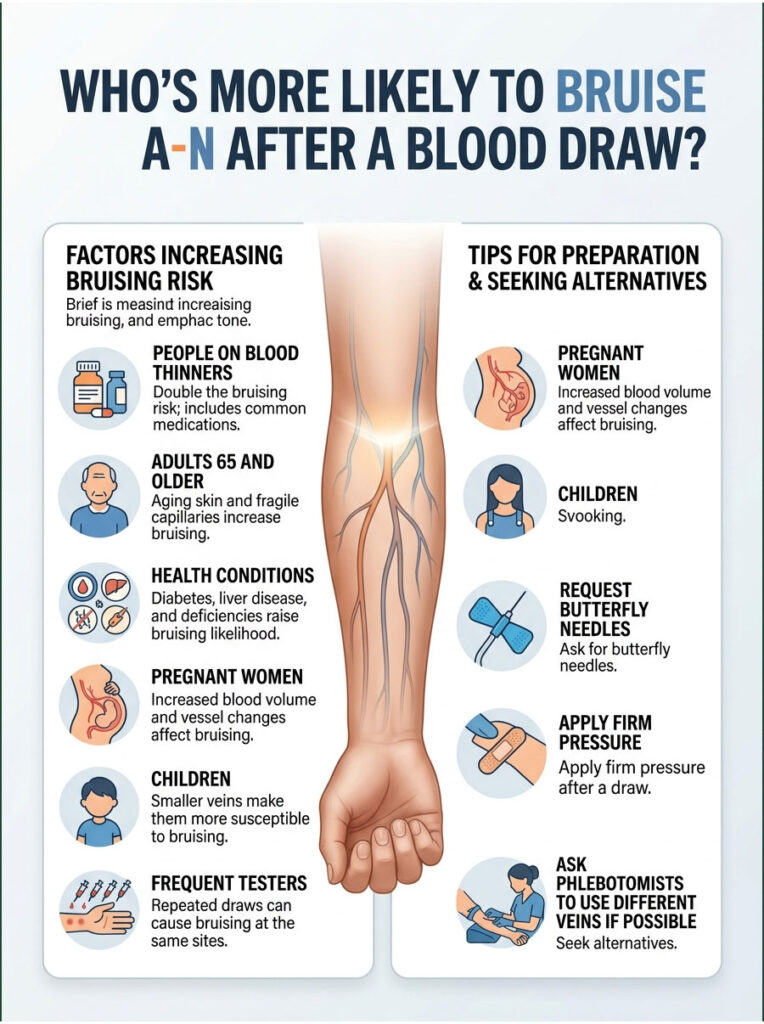
People on Blood Thinners
If you take Eliquis, Xarelto, warfarin, Plavix, or daily aspirin, your bruising risk roughly doubles. According to CDC data, about 6.1 million American adults take prescription anticoagulants, and another 25 million take low-dose aspirin daily. That’s almost 1 in 10 US adults walking around with thinned blood at any given moment.
Don’t stop these medications before a blood draw unless your doctor specifically tells you to. But you can prepare differently: ask for a butterfly needle, request a smaller-gauge size, and apply firm pressure for a full 5 minutes after the draw instead of the usual 60 seconds.
Adults 65 and Older
Aging skin loses collagen and the protective fat layer that cushions blood vessels. Older adults also develop senile purpura, where capillaries become so fragile they break from minor pressure. The Cleveland Clinic confirms this is harmless but cosmetically frustrating.
People With Specific Health Conditions
Diabetes, liver disease, chronic kidney disease, and any clotting disorder all raise bruising likelihood. Vitamin C and vitamin K deficiencies do too. People undergoing chemotherapy may bruise dramatically because chemo lowers platelet counts.
Pregnant Women, Children, and Frequent Testers
Pregnancy increases blood volume and changes vessel elasticity. Kids have smaller veins that are easier to nick. People who get monthly or weekly blood draws (chemo patients, transplant recipients, blood disorder patients) often have repeated bruising at preferred draw sites because those veins haven’t fully healed.
If you’re in any of these groups, ask the phlebotomist to use a different vein each visit when possible.
Hematoma vs. Bruise vs. Blown Vein: Knowing the Difference
These three terms get used interchangeably, but they describe different things with different healing timelines.
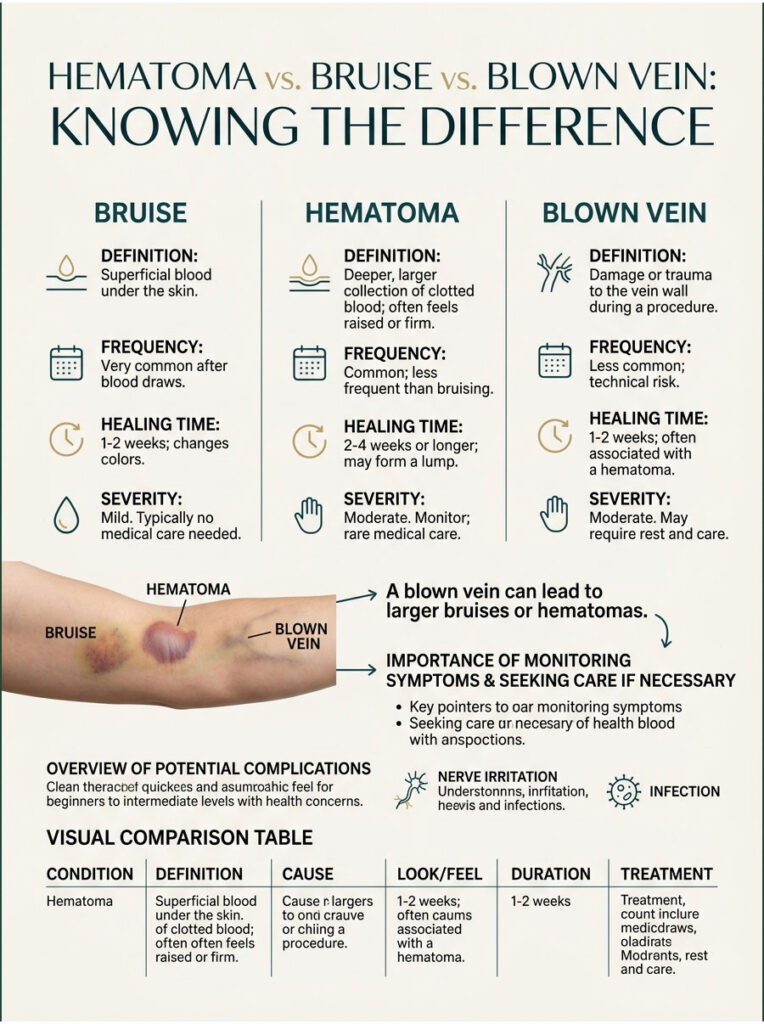
Table 2: Bruise vs. Hematoma vs. Blown Vein USA Comparison
| Condition | Estimated Frequency After US Blood Draws | Typical Healing Time | Severity | Source |
| Standard bruise (ecchymosis) | 12 to 16 percent of draws | 5 to 14 days | Mild, no medical care needed | NIH StatPearls |
| Hematoma | 2 to 4 percent of draws | 7 to 21 days | Mild to moderate, monitor | WHO Phlebotomy Guidelines |
| Blown vein | 3 to 5 percent of draws | 10 to 12 days | Mild but can’t reuse vein | Cleveland Clinic |
| Nerve irritation | Less than 1 percent | Days to weeks | Variable; needs evaluation if persistent | NIH/PubMed |
| Infection at puncture site | Less than 0.1 percent | Requires antibiotics | Moderate to serious | CDC |
A bruise is purely cosmetic blood under the skin. A hematoma is a localized blood pool you can feel as a lump. A blown vein is the actual injury that often causes the larger bruise or hematoma.
If you’ve ever had a phlebotomist say “your vein blew,” that’s why a much bigger bruise showed up than usual.
How to Prevent Bruising at Your Next Blood Draw
Some bruising is unavoidable, but you can stack the odds in your favor with smart prep.
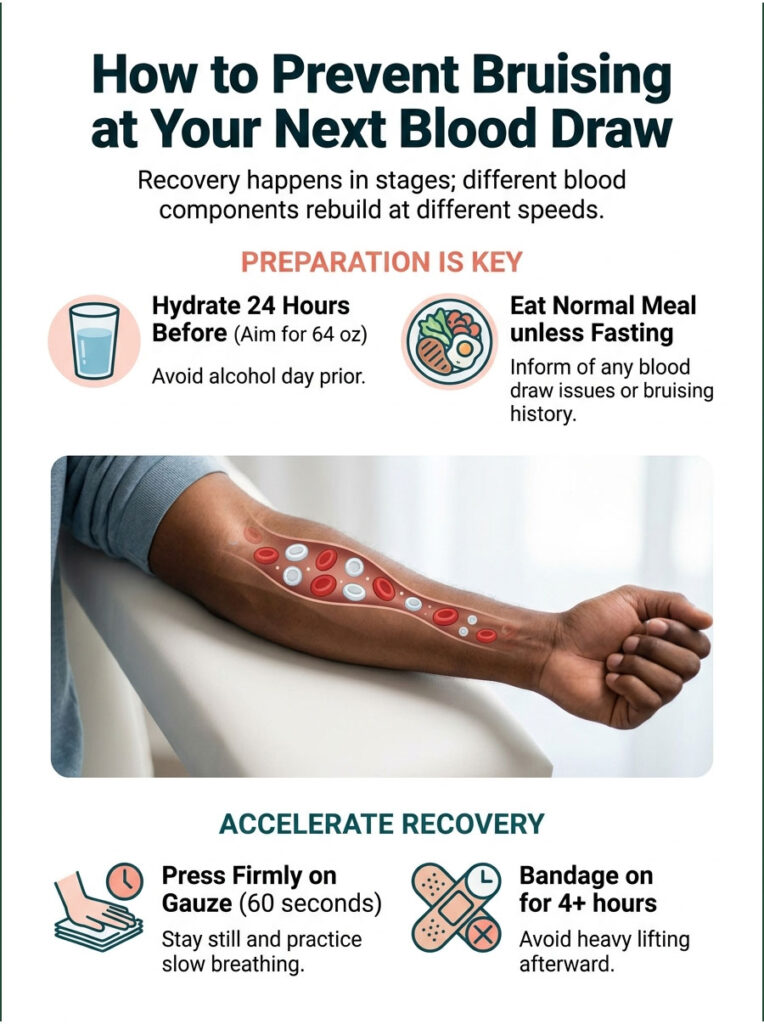
Before Your Appointment
Hydrate hard for 24 hours before your draw. Aim for at least 64 ounces of water. Plump, well-hydrated veins are easier to find and less likely to roll or collapse. Skip alcohol the day before; it dehydrates and thins your blood.
Eat a normal meal unless your test requires fasting. Low blood sugar can leave you lightheaded and increase the chance you’ll flinch during the draw.
Wear a short-sleeve shirt or one with loose, easy-to-roll sleeves. Tight cuffs act like tourniquets and increase venous pressure, which raises bruising risk.
During the Draw
Tell the phlebotomist if you’re a difficult stick or have a history of bruising. They can pick your best arm, use a smaller needle, or grab the butterfly setup, which the WHO blood drawing guidelines note reduces vessel damage by roughly 40 percent in elderly patients.
Stay still. Don’t watch if it makes you tense up. Take slow breaths through your nose. The more relaxed your arm, the cleaner the draw.
If you feel a sharp shooting pain (not the normal pinch of needle entry), say something immediately. That can signal a nerve hit.
After the Needle Comes Out
This is where most preventable bruising happens. Press firmly on the gauze pad for at least 60 seconds. If you’re on blood thinners, press for a full 5 minutes. Don’t peek. Don’t keep lifting the pad to check; that breaks the clot every single time.
Keep the bandage on for at least 4 hours, longer if you’re on anticoagulants. Skip heavy lifting, gym workouts, and stressful arm movements for the rest of the day.
I’ve watched plenty of patients undo a clean draw by hauling a 30-pound briefcase out the door 90 seconds later. That’s almost always when the bruise shows up the next morning.
What to Put on a Bruise After a Blood Draw (Evidence-Backed Remedies)
The drugstore aisle has dozens of options. Most don’t work. Here’s what does, and what to skip.
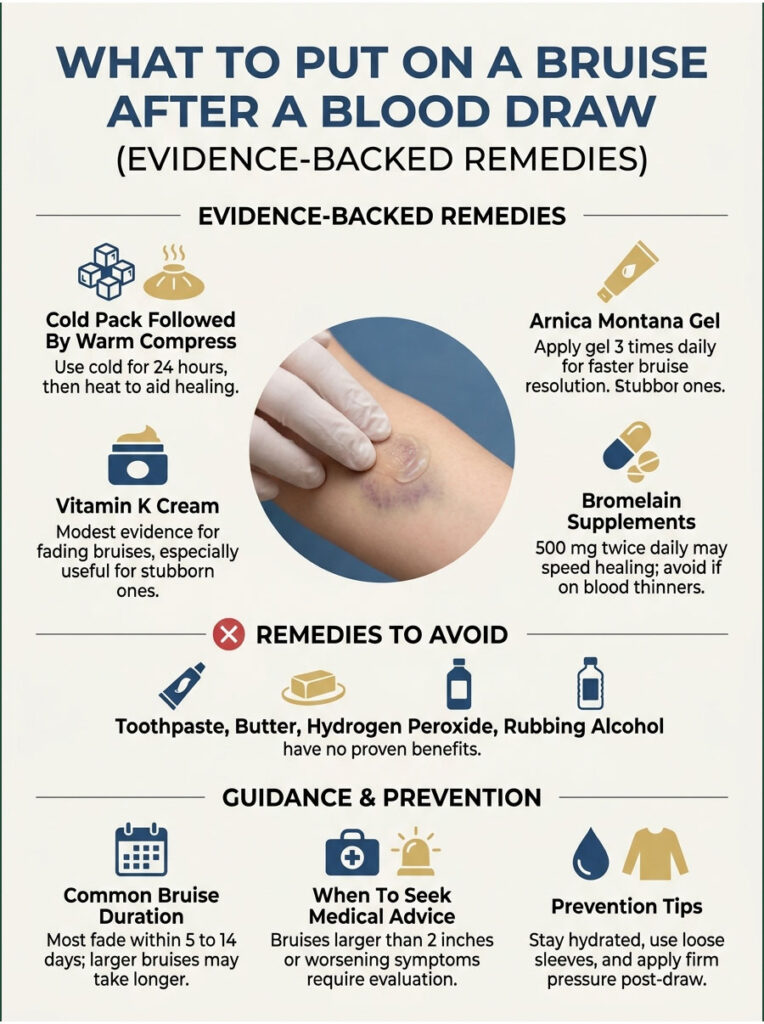
Cold Pack Then Warm Compress (Free, Most Effective)
Cold for the first 24 hours, heat after that. Nothing beats the cost-to-benefit ratio. Use a thin towel between your skin and the cold or warm source to prevent burns or frostbite.
Arnica Montana Gel
Arnica is a plant extract used in homeopathic and herbal medicine. Multiple clinical trials cataloged on PubMed show topical arnica gel applied 3 times daily speeds bruise resolution by 1 to 2 days. Look for products with at least 5 percent arnica concentration.
Vitamin K Cream
Topical vitamin K (often labeled K1 or phytonadione) shows modest evidence for fading bruise discoloration. Less proven than arnica but worth trying for stubborn bruises that linger past day 7.
Bromelain Supplements
Bromelain, an enzyme from pineapple, has anti-inflammatory effects. Some clinical research suggests 500 mg taken twice daily on an empty stomach can speed bruise healing. Skip if you’re on blood thinners or about to have surgery.
What NOT to Put on a Blood Draw Bruise
Toothpaste does nothing despite TikTok claims. Butter, lard, and meat tenderizer are old wives’ tales with zero evidence. Hydrogen peroxide can damage healing skin and isn’t appropriate unless there’s an open wound. Rubbing alcohol stings and dries the skin without helping the bruise.
If a remedy sounds suspicious, it probably is.
Frequently Asked Questions
How long does a bruise last after a blood draw?
Most bruises after a blood draw fade within 5 to 14 days, depending on size and your individual healing speed. Smaller bruises clear faster, often within a week. Larger ones, or bruises in people taking blood thinners or those over 65, can take up to 3 weeks to fully disappear.
Is a big bruise after a blood draw normal?
A bruise up to 2 inches across is generally normal, especially if you’re on blood thinners, are older, or had a difficult draw. Bruises larger than 2 inches, or any bruise that keeps growing after 48 hours, deserve a call to your primary care doctor for a quick check.
Why does my arm hurt a week after a blood draw?
Mild tenderness for up to a week is common as the bruise heals. Persistent throbbing, burning, or shooting pain can signal nerve irritation, a deep hematoma, or rarely, infection. If pain is worsening rather than improving by day 7, contact your doctor for evaluation.
Can I take ibuprofen for a bruise after a blood draw?
Skip ibuprofen, aspirin, and naproxen for the first 72 hours after your draw because they thin your blood and can worsen the bruise. Acetaminophen (Tylenol) is the better choice for pain relief because it doesn’t affect clotting. Resume your usual NSAIDs after 3 days if needed.
What is the lump under my skin after blood draw?
A small soft lump is usually a hematoma, which is a pocket of pooled blood from the punctured vein. Most hematomas resolve in 7 to 21 days with warm compresses after the first 48 hours. A hard, growing, or painful lump warrants a same-day visit to urgent care for evaluation.
Should I put heat or ice on a bruise after a blood draw?
Use ice for the first 24 hours to slow bleeding and reduce swelling, applied 20 minutes on and 20 off. Switch to a warm compress after 48 hours to boost circulation and help your body reabsorb trapped blood faster. Don’t apply heat in the first 24 hours; it can make the bruise worse.
Can I exercise with a bruise after a blood draw?
Skip strenuous exercise, weight lifting, and arm-heavy workouts for at least 24 hours after a blood draw, even without a bruise. With visible bruising, wait 48 to 72 hours before resuming arm workouts. Light cardio like walking is fine. Heavy activity can dislodge the clot and make the bruise much worse.
Why do I bruise so easily after blood tests?
Easy bruising can come from blood thinners, daily aspirin, fish oil supplements, age-related skin thinning, vitamin C or K deficiency, diabetes, liver disease, or low platelet counts. If you bruise easily from minor injuries elsewhere on your body, ask your doctor for a complete blood count and clotting workup.
Can a blood draw cause nerve damage?
Permanent nerve damage from a blood draw is extremely rare, occurring in less than 1 in 21,000 venipunctures according to clinical literature. Temporary nerve irritation is more common and feels like burning, tingling, or electric shocks during the draw. If symptoms last beyond a few days, see your doctor.
How can I prevent bruising on my next blood draw?
Hydrate well for 24 hours before, wear loose sleeves, ask for a butterfly needle if you bruise easily, apply firm pressure for 60 seconds (5 minutes if on blood thinners), keep the bandage on for 4 hours, and skip heavy lifting for the rest of the day. Tell your phlebotomist about any past bruising history.
Does drinking water before a blood draw prevent bruising?
Yes, hydration helps significantly. Well-hydrated veins are larger, plumper, and easier for the phlebotomist to find on the first try. That cuts the need for multiple needle attempts, which is one of the biggest causes of bruising. Aim for 64 ounces of water in the 24 hours before your draw.
When should I see a doctor about a blood draw bruise?
Call your doctor if the bruise is larger than 2 inches, keeps growing after 48 hours, develops into a hard lump, causes numbness or weakness in your hand, comes with fever or warmth, or hasn’t started fading by day 14. Also seek care if you notice unexplained bruises elsewhere on your body.
Disclaimer: This article is for educational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always consult a qualified healthcare provider with any questions about your medical condition or symptoms after a blood draw. Never delay seeking medical care because of something you read online. If you’re experiencing severe pain, significant swelling, numbness, fever, or signs of infection, contact your healthcare provider or visit an urgent care clinic right away.
References
- National Institutes of Health (NIH) StatPearls: Phlebotomy
- World Health Organization: WHO Guidelines on Drawing Blood
- Cleveland Clinic: Blown Vein
- Mayo Clinic: Aspirin Drug Information
- Centers for Disease Control and Prevention (CDC)
- American Society of Hematology
- PubMed Clinical Studies on Arnica Montana for Bruising
- U.S. Bureau of Labor Statistics: Phlebotomist Occupational Data